Abstract
New York City (NYC) Health + Hospitals implemented a nutrition program making plant-based meals the primary lunch and dinner options for patients at its 11 hospitals. Plant-based and culturally diverse meals are prepared and distributed by a central culinary center, managed by Sodexo. Food service associates visit patient rooms and verbally introduce the featured meals each day. To ensure alignment among all staff members, staff are educated about the health benefits of plant-based nutrition and about the new menu items. The plant-based meals have been well received, with patient acceptance over 95% and patient satisfaction above 90%. Per-tray food costs for plant-based entrees cost $0.59 less compared to trays including animal products. Furthermore, the hospital system has achieved a 36% reduction in calculated carbon emissions as a result of the new plant-based menu. Because dietary choices contribute significantly to health and may influence the likelihood of hospital readmissions, prioritizing plant-based meals and nutrition education during the hospital stay may help improve patient outcomes.
“90% of patients who received the plant-based meals reported being satisfied with their choice.”
NYC Health + Hospitals is the nation’s largest public hospital system, providing health care to New Yorkers regardless of ability to pay or immigration status. The system serves 1.1 million patients annually at more than 70 locations, including 11 hospitals, five post-acute facilities, and more than 38 diagnostic centers, with 43,000 health care providers and with more than 200 languages spoken by its patients.
Because nutrition plays an important role in recovery from illness and in preventing recurrence,1-3 NYC Health + Hospitals developed an innovative nutrition program. In this program, healthful plant-based meals are the default inpatient meal option, and nutrition information is provided to patients and their families, encouraging them to make healthier dietary choices both in the hospital and after discharge. Here we describe the development and implementation of the program and share the corresponding outcomes.
Program Development
In 2019, a Meatless Mondays program was initiated as a test of a weekly meatless options for inpatients, starting with lunch. Dishes were designed to be familiar and appealing in taste and texture. Acceptability of these new dishes, defined as the number of patients who chose the offered plant-based options and did not request an alternate meal, was 95%. The success of this program led to its expansion to the dinner menu, and additional meatless meals were introduced. In 2021, the culinary team began the development of a plant-based default program, in which plant-based meals would become the primary option, based on three strategic pillars: • Research foundation: The program was based on research showing the benefits of plant-based diets in chronic disease prevention, management, and in some cases, reversal.1-3 • Culinary center innovation: The culinary team was trained in fundamental techniques of plant-based cooking and in creating new dishes. • Employee and patient engagement: Engagement with stakeholders, from hospital administration to nursing staff and patients, ensured that all had a common understanding about food, nutrition, and the program’s goals.
Recipe Development
Plant-Based Menu Items for Inpatients at NYC Health + Hospitals.
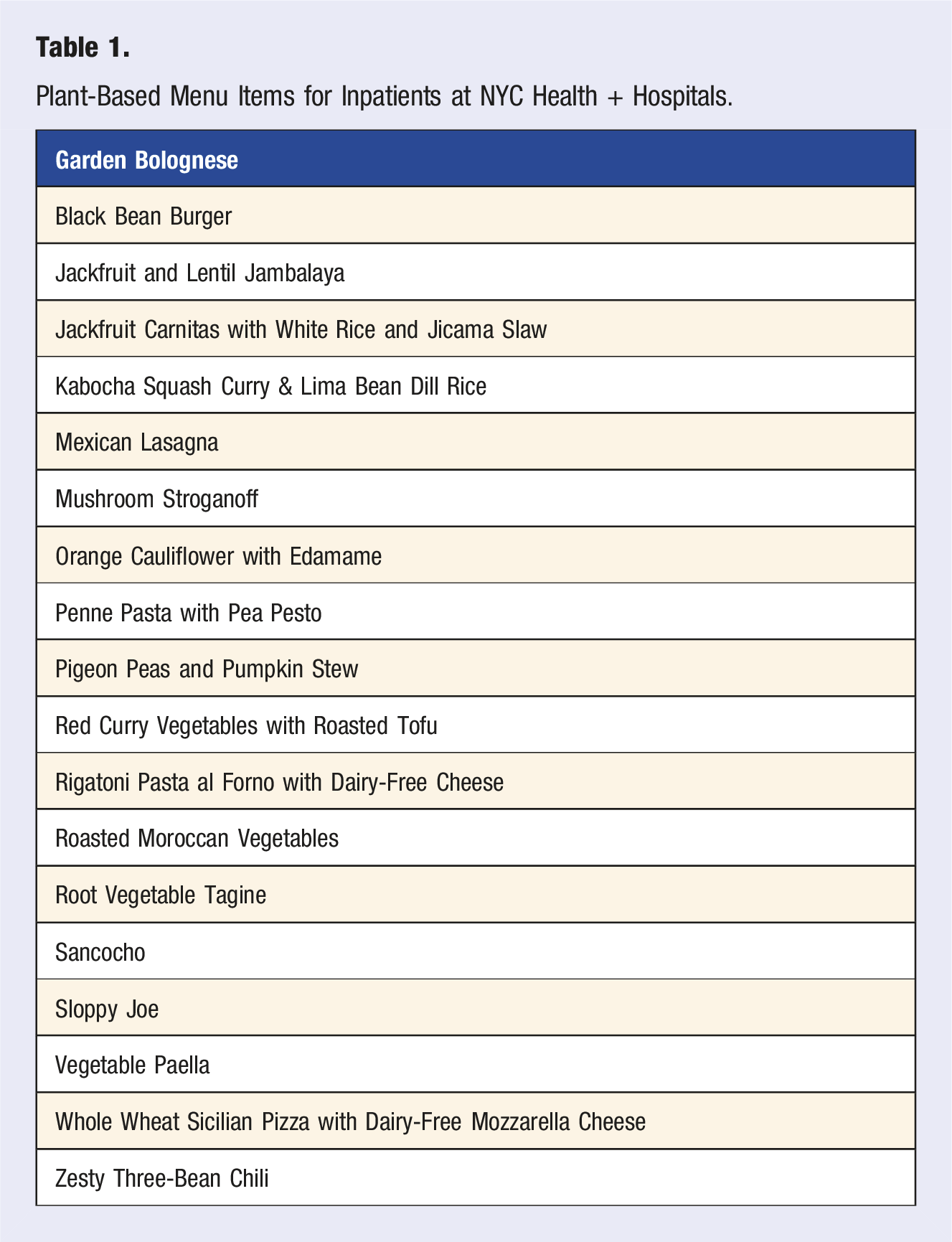
Recipes have evolved over time. For example, the Garden Bolognese was first made with soy crumbles, but in an effort to reduce reliance on processed foods, the recipe evolved to use mushrooms as its high-protein ingredient. Since some patients may have reduced appetite during hospitalization, the use of meals with familiar flavors and textures was deemed important to help increase dietary intake.
In addition to developing plant-based, culturally diverse recipes, changes were made in food preparation techniques. Rather than boiling and stewing, chefs began braising, sauteing, and adding various flavor profiles based on spices from the diverse cultures of NYC.
The management team ensured that leaders explained to the frontline staff the importance of these menu changes. Frontline staff then served as ambassadors to promote plant-based nutrition to the patients.
Technical Considerations
All meals are prepared at the NYC Health + Hospitals Culinary Center using a Cook-Chill system, in which meals are prepared and chilled before delivery to their respective facilities. The Cook-Chill system has a hot/cold tray delivery cart, which slowly heats the meals over 45 to 50 minutes, allowing the meals to be held at a proper temperature. On the opposite side from the hot food, the tray cart maintains cold food at 40 degrees Fahrenheit or below, allowing food prepared off-site to be delivered at an appropriate temperature. Disposable dinnerware was replaced with more appealing serving sets. While some patients will require disposable trays for various reasons, most can use reusable dinnerware.
Implementation
In advance of the initiation of the program, program leaders held educational meetings at each of the 11 hospitals to update hospital staff regarding the upcoming menu changes and provide an opportunity to taste the new recipes and learn techniques for communicating the importance of nutrition to patients.
The plant-based program began at lunch, with educational campaigns designed to engage staff and patients coinciding with National Nutrition Month activities.
A food service associate program was implemented, including servers dedicated to taking the patients’ orders, explaining the benefits of the healthful foods, and placing orders for alternative meals when requested. Eventually, the plant-based meals then expanded to include dinner service. In addition to the program in the 11 hospitals, plant-based entrees were also introduced in all five post-acute care facilities.
Patient Experience
The patient meal experience begins with the therapeutic diet ordered by the physician. Regardless of a patient’s diet order, plant-based options are available and can be adjusted as needed.
In the patient’s room, a food service associate presents the menu verbally and places the meal order on an iPad. The first item offered is the chef’s recommendation of the day, which is always plant-based. If this is not accepted, the patient is offered an alternate plant-based meal. If the patient chooses neither plant-based option, many other options are available. While the goal is to offer the most healthful meal first, patients are not restricted in their options.
After meals, food service associates collect feedback on the menu items, allowing the culinary staff to adjust recipes. Food service associates also work closely with registered dietitians, discussing any challenges encountered with patients, and registered dietitians are available to provide additional education to patients.
On-Site Promotion
To communicate the value of plant-based meals, patients receive branded educational material at admission with information about the meals, including QR codes leading to recipes, as well as answers to frequently asked questions. Screensavers cycled on all hospital computers and televisions, including an appealing photograph of plant-based foods and the following text:
A plant-based diet has been shown to … • Decrease risk of heart disease. • Lower cholesterol. • Lower blood pressure. • Reduce inflammation. • Improve blood sugar. • Support weight management.
Additionally, tray carts are wrapped in imagery promoting plant-based meals as the carts are pushed through hospital halls. Food service staffers wear pins that read: Ask me about plant-based menus. At discharge, patients receive a plant-based recipe book collected from hospital staff submissions.
Outcomes
During the initial year after implementation, data were available on acceptance, uptake, and satisfaction. • Acceptance: 95% of eligible patients chose plant-based options and did not request alternate meals. • Uptake: 50% of the full patient population chose plant-based entrees. Included in this number were patients who were ineligible for the plant-based chef’s special based on diet orders (such as renal and texture-modified diets); therefore, these patients were not offered the primary plant-based meal. • Satisfaction: 90% of patients who received the plant-based meals reported being satisfied with their choice.
The carbon emissions and cost for each meal was examined. • Carbon emissions: The meal program led to an estimated 36% reduction in carbon emissions from all meals served compared to the prior year when the program was not yet fully implemented. • Cost savings: Cost of individual meals varied, but cross-sectional data collection revealed that plant-based entrees were, on average, $0.59 less expensive than meals containing animal products. For example, a meat-based chili may cost roughly $1.38 per serving while a plant-based version may cost roughly $0.47 per serving.
The program minimizes processed foods and meat alternatives, focusing instead on raw ingredients which brings substantial cost savings. In total, the program served almost 800,000 plant-based meals in 2023, with savings of $318,000. Projections suggest that the number of plant-based meals offered will continue to increase annually, leading to further cost savings. NYC Health + Hospitals is currently considering expanding the program to include patients who were not included in the initial rollout, such as behavioral health patients, and increasing outreach to the broader community.
Conclusion
The plant-based initiative at NYC Health + Hospitals yielded strong acceptance and satisfaction among patients, reduced carbon emissions, and substantial cost savings. Keys to success included working with key stakeholders, including government and hospital leadership, education for all levels of employees, cross-departmental engagement and cooperation, stepwise introduction of the program, menu modification based on patient feedback, and the use of food service associates to interact with patients. Plant-based meals have proved a major advantage for NYC Health + Hospitals, ensuring that nutrition is an integral part of the healing process.
Footnotes
Declaration of Conflicting Interests
Samantha Morgenstern, RD, MS, CDN, is an employee of Sodexo, a hospital food service provider. Mercedes Redwood, MS, is an employee of NYC Health + Hospitals. Anna Herby DHSc, RD, CDE, is an employee of the Physicians Committee for Responsible Medicine, an organization conducting research and educational programs on nutrition.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
