Abstract

“These findings offer hope for expanding lifestyle medicine interventions and pave the way for larger LSMSMA studies with longer time frames that will be necessary for the lifestyle medicine and LMSMA fields to grow.”
Shared Medical Appointments (SMAs) are receiving increased attention for chronic disease management.1-3 Although SMAs are widely considered to be a promising care delivery tool, 4 SMA research to date has focused on short-term outcomes alone. As a result, there is uncertainty about the effectiveness of SMA programming to prevent and/or treat chronic disease over the long term. The absence of such studies demonstrating beneficial outcomes of SMA interventions—including biometrics, medication utilization, and total cost of care—has likely inhibited wide-scale SMA implementation in clinics and health systems. Investments in sustainable SMA programming will thus first require re-focusing SMA research on long-term outcome assessments, like many studies of medications and surgeries, investigating SMA effectiveness for chronic disease care.
We previously reported several promising short-term outcomes of a virtual, primary care-based, four-part Lifestyle Medicine SMA (LMSMA) series on hypertension. 5 In additional to hypertension education and individualized medical care, this intervention also included home blood pressure monitoring (HBPM) and group-based health and wellness coaching. In our preliminary study of 23 patients who completed the series, we observed an estimated reduction in both systolic and diastolic blood pressure of −5.4/−2.9 mmHg on HBPM. In addition, 59% of patients on antihypertensive medications had a reduction in dosages during the series, including four patients (18%) who were taken off antihypertensive medications completely. In the 180 days following the LMSMA series, eight of the remaining 18 patients (44%) on antihypertensive medication had their dosage reduced or discontinued as part of usual care. The study, like other hypertension-focused SMA research,6-8 investigated only short-term outcomes.
The current study is a long-term follow-up analysis of the aforementioned hypertension-focused LMSMA cohort. The study period was between 180 days and two years after completing the LMSMA series. Unfortunately, due to technical difficulties, HBPM data were not available for analysis after the LMSMA series. Antihypertensive medication regimens were assessed in the electronic medical record (EMR) two years after finishing the LMSMA series. The presence of at least one in-person primary care visit, where a blood pressure was taken, during the study period was also determined using the EMR.
Of the 23 patients in the original study, two patients were lost to follow-up two years after completing the LMSMA series. All other patients had at least one in-person primary care visit during the study period. As a result, there were 21 patients included in the analysis, including 20 patients who started the LMSMA series on medication. As a result of usual care between the 180-day and two-year timepoints after the LMSMA series, there were no changes in antihypertensive medication regimens in 15 patients (71%), including 10 patients who were deprescribed during (n = 5) and/or in the 180 days after (n = 5) the LMSMA series (Figure 1). Between the 180-day and two-year timepoints, there was an antihypertensive medication reduction in one patient (5%), increase in two patients (10%), and switch in medication classes in three patients (14%). Sunburst chart of antihypertensive medication changes (n) at three timepoints: (1) the end of the series, compared to the start of the series (inner circle); (2) 180 days after the end of series, compared to the end of the series (middle circle); and (3) two years after the end of the series, compared to 180 days after the end of the series (outer circle). Reductions in medication doses are coded green, with subsequent reductions or no subsequent changes in medications additionally coded green. An increase in medication doses is coded red, with subsequent increases or no subsequent changes in medications additionally coded red. Gray is used to denote (1) no change in medication regimen after starting the LMSMA series, (2) switching antihypertensive medication classes (“Switch”), and (3) lost to follow-up at the two-year timepoint (“N/A”).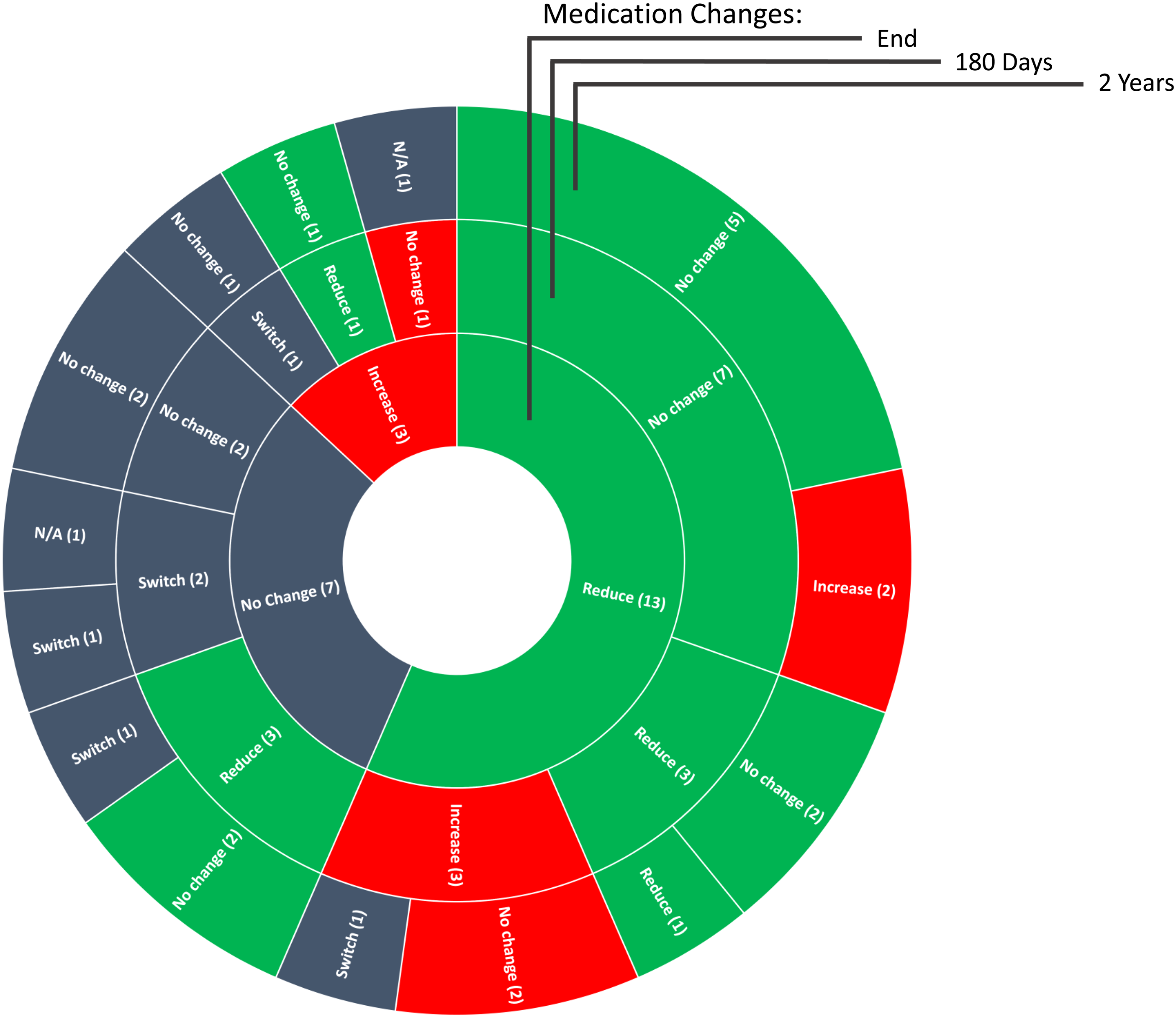
Of the 20 patients included in the study who started the LMSMA series on at least one medication, 10 patients (50%) were on lower antihypertensive medication regimens, if any, two years after finishing the LMSMA series. In a sub-group analysis of the 13 patients who had medication reductions during the LMSMA series, eight patients (62%) had sustained (n = 5), if not further reduced (n = 3), lower medication doses two years after the LMSMA series. One patient had medication reductions during the LMSMA series and during both interval periods after the series.
This study is significant because it includes the longest LMSMA follow-up period (i.e., two years) to date. As lifestyle medicine gains traction in health systems, demonstrating long-term impact—especially regarding improved health outcomes, reduced medication burden, and lower cost of care—will be critical. Although HBPM results were not available in this analysis, the sustained and/or further reduction in antihypertensive medications for 50% of patients who entered the LMSMA series on medications is very promising. Moreover, the observation that 62% of patients who had a medication reduction during the LMSMA series were still on lower doses two years later gives hope for leveraging relatively short-term LMSMA programming for long-term impact.
This study has several limitations. Primarily, without HBPM data, it is difficult to assess the direct impact of the LMSMA series on long-term blood pressure control. Given the reliance on medication prescriptions as a surrogate, there are several additional limitations. First, it is possible that some patients at the two-year timepoint were on inappropriately low medication regimens (i.e., despite elevated blood pressure that was either undetected during clinic visits or not acted on), leading to an overestimation of the impact of the LMSMA series. Conversely, given the general lack of deprescribing of antihypertensive medications in the primary care setting,9,10 the impact of the LMSMA series could be underestimated by patients who remained on higher medication regimens despite well-controlled blood pressures at home and/or in the clinic setting. Additionally, without interrogation of medication adherence, it’s also difficult to assess the direct relationship between prescriptions and hypertension control. Finally, as with the original study, the lack of a control group also limits the interpretation of the findings.
Future analyses of this and other LMSMA series should include sustained HBPM as the gold-standard for assessing both blood pressure changes over time as well as the appropriateness of antihypertensive medication regimens. In addition, future studies should assess other markers of importance to health systems and insurers given the move towards value-based care, including medication costs, emergency room and hospital utilization, and total cost of care. Finally, it is imperative that future LMSMA studies include larger sample sizes with control groups to accurately assess efficacy.
In conclusion, this follow-up analysis of the long-term impact of a virtual four-part LMSMA series suggests sustained reductions in antihypertensive medication regimens two years after completion. These findings offer hope for expanding lifestyle medicine interventions and pave the way for larger LMSMA studies with longer time frames that will be necessary for the lifestyle medicine and LMSMA fields to grow.
Footnotes
Authors’ Contribution
All authors substantially contributed to the manuscript, meet journal guidelines for authorship, and gave consent for submission.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Jacob Mirsky MD MA DipABLM is the founder and owner of Lifestyle Medicine Consulting LLC.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
