Abstract
There is no longer any serious doubt that daily habits and actions profoundly impact on both short- and long-term health and quality of life. An overwhelming body of scientific and medical literature supports this contention. Thousands of studies support the concept that regular physical activity, healthy nutrition and maintaining a healthy body weight, not smoking cigarettes, obtaining healthy sleep, reducing stress and maintaining positive connections with other individuals all profoundly impact on health. The scientific literature the supports the health impact of these daily habits and actions is underscored by its incorporation into virtually every evidence-based clinical guideline in the area of metabolic diseases. Thus, the scientific basis for lifestyle medicine rests on an enormous body of evidence-based literature. The key issue in lifestyle medicine is to provide an overall framework where these studies, which are often spread over scientific literature in multiple disciplines, can be made accessible to the medical community and to the public at large. This is the essence of the field of lifestyle medicine. The academic basis of lifestyle medicine is robust and needs to be emphasized by all practitioners of lifestyle medicine. This is the key to moving this field forward into the future.
Keywords
“The Western diet in particular has been associated with dysbiosis by favoring gut bacteria that create adverse health consequences.”
Introduction
There is no longer any serious doubt that the practices and habits that individuals adopt in their daily lives profoundly affect their short- and long-term health and quality of life. An overwhelming body of scientific and medical literature supports this contention. 1 Literally, thousands of studies support the concept that regular physical activity, 2 healthy nutrition, 3 maintaining a healthy body weight,3–5 not smoking cigarettes, 6 obtaining healthy sleep,2,7 reducing stress, 8 and maintaining positive connections with other individuals 9 all profoundly impact on health.10,11
Sampling of Guidelines That Incorporate lifestyle Recommendations for the Threat or Prevention of Chronic Disease.
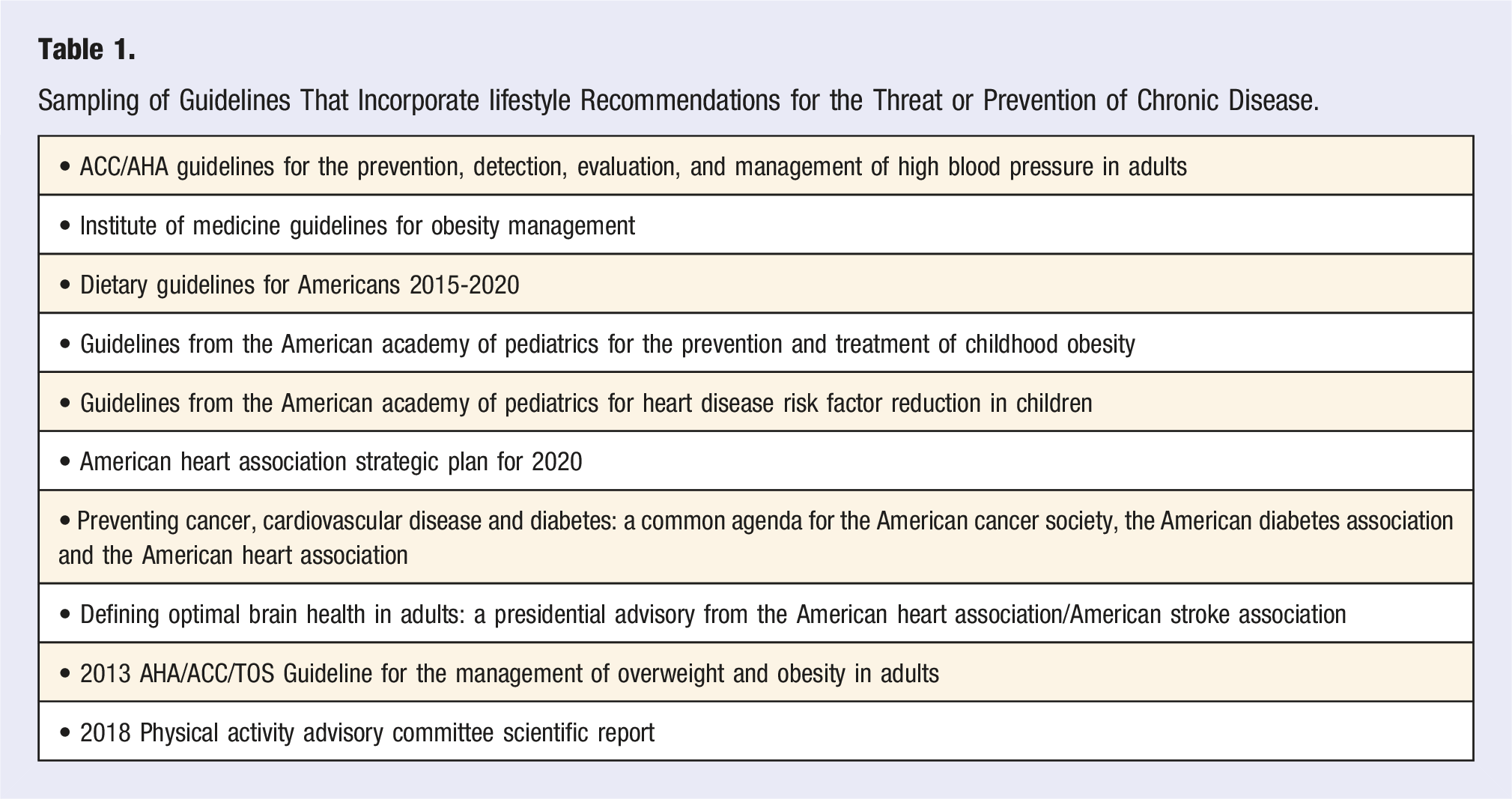
Despite widespread recognition of the important role of lifestyle measures and overall habits and actions as key components of preventing and treatment metabolic diseases, it has been frustratingly difficult to actually change factors for the American public. An example of the extent of this problem may be found in the Strategic Plan released by the American Heart Association (AHA) in 2020 13 which estimated that only 5% of the adult population in the United States practices all of the positive lifestyle measures known to significantly reduce the risk of developing cardiovascular disease (CVD).
In addition, it has been frustratingly difficult to provide adequate education for physicians in the areas of physical activity, nutrition, weight management and other important lifestyle parameters. This, despite the fact that there is overwhelming evidence to support the important role that these habits and actions play and even a strong consensus amongst physicians concerning the value of positive lifestyle factors. Indeed, virtually every physician would agree with the premise that regular physical activity, weight management, sound nutrition, and not smoking tobacco yield significant health benefits. Yet, the actual application of this knowledge has been woefully inadequate.
The purpose of this review is to provide a summary of the literature that supports the benefits of positive health promoting habits and issue a strong call for increased emphasis on recommending lifestyle medicine practices amongst physicians and other healthcare providers. The focus of this review will be to summarize research and knowledge in the area that has now been called “lifestyle medicine” and suggest some remediation related to existing practice gaps.
The History of Lifestyle Medicine
Literally thousands of studies have been conducted over many decades demonstrating that regular physical activity, healthy nutrition, weight management, avoiding tobacco, stress reduction, healthy sleep and positive connections with others are all associated with decreased risk of chronic disease. These research studies have been spread in the scientific literature in multiple different disciplines. The result has made it very difficult for physicians to have access to this literature in one convenient place. That is the essence of the field of lifestyle medicine.
I had the privilege of editing the first multiple authored academic textbook in this area. In fact, this textbook, which was published in 1999, coined the term “lifestyle medicine” in the academic literature. 14 We defined lifestyle medicine as “the discipline of studying how daily habits and practices impact on both the prevention and treatment of disease often in conjunction with pharmaceutical or surgical therapy to provide an important adjunct to overall health.”
Subsequent to this initial definition, a number of different constructs have evolved offering slightly different definitions of lifestyle medicine but observing the essential core concept that daily habits and practices profoundly impact on both the likelihood of developing disease or, if present, in its treatment.15,16 Various researchers have made significant contributions not only in these individual areas but also in the overall discipline of lifestyle medicine. While different frameworks for this body of work have evolved, it is clear that the field will coalesce around the term “lifestyle medicine.”
As one of many examples, the American Heart Association (AHA) changed the name of one of its councils from the “Council on Nutrition, Physical Activity and Metabolism” to the “Council on Lifestyle and Cardiometabolic Health.” 17 In 2013, the AHA and ACC joined forces to issue practice guidelines which also utilized the phrase “lifestyle” as a key recommendation for lowering the risk of CVD in their statement entitled “2013 AHA/ACC Guidelines on Lifestyle Management to Reduce the Cardiovascular Risk.” 18 In addition, guidelines that were jointly released by AHA and ACC both for lipid management 19 and control of high blood pressure, 20 which also strongly emphasized the central role of lifestyle practices and decisions to ameliorate these risk factors.
Of note, both the American College of Preventive Medicine (ACPM) and the Academy of Family Practice (AFP) have established working groups and/or educational tracks in the area of lifestyle medicine. The AHA also published in its major academic journal Circulation, a series articles entitled “Recent Advances in Preventive Cardiology and Lifestyle Medicine.” 21
A summary of competencies physicians should possess to practice lifestyle medicine was published in the Journal of the American Medical Association. 22 Significantly, a new health care organization was formed in 2004 named the American College of Lifestyle Medicine (ACLM) which is devoted to providing a professional home for individuals who wish to emphasize lifestyle medicine in their practices. 16 ACLM has doubled its membership each year for the past 5 years and has now enrolled over 10,000 physicians and other health care professionals making it the most rapidly growing health care discipline in the United States.
In addition, ACLM founded the American Board of Lifestyle Medicine (ABLM) which offers certification boards in lifestyle medicine which over 2000 health care professionals have taken to receive certification from the ABLM. 23 Lifestyle medicine has also now blossomed into an international movement with the development of the Lifestyle Medicine Global Alliance (LMGA). 24 Over 40 countries have now established individual branches of lifestyle medicine which are part of LMGA.
Additional academic endeavors have been launched which are designed to continue to build and expand the academic footprint of lifestyle medicine. For example, the fourth edition of my Lifestyle Medicine textbook will be published in 2024. 1 In addition, a peer reviewed academic journal has been established, the American Journal of Lifestyle Medicine (AJLM), which was established in 2007 with the stated purpose of providing a forum for individuals interested in changing academic information in this growing field. 25 This journal currently has over 21,000 subscribers and in 2022 experienced over 200,000 downloads of academic papers. I have the honor of serving as the Editor in Chief of AJLM.
To further enhance the academic credibility of lifestyle medicine and further embed it within mainstream medicine, a series of single topic books, the Lifestyle Medicine Series, 26 has been established and has published books in the areas of cardiovascular medicine, weight management, counseling and behavior change, women’s health, diabetes, pre-diabetes and the metabolic syndrome, nursing, and psychiatry and mental health. I have been pleased to be the Editor in Chief of this Series. In the next 2 years we plan to publish additional volumes in geriatrics, primary care, brain health, and health equity. Thus, there are multiple reasons why the term “lifestyle medicine” has emerged as the centerpiece for what this academic discipline will be called.
The term lifestyle medicine seems particularly appropriate for this discipline. First of all, the field focuses on daily habits and actions which are essential components of lifestyle and its relationship to health. Secondly, it is clearly “medicine” based on a wide range and large volume of evidence supporting the health benefits of positive daily habits and actions.
The Power of Lifestyle to Promote Good Health
Multiple lifestyle practices have been demonstrated to lower the risk of chronic disease as well as serve as important adjuncts to treatment. These include regular physical activity, healthy nutrition, weight management, avoidance of tobacco products and other addictive substances, strategies to reduce stress, anxiety, and depression, obtaining healthy regular sleep, and developing positive interpersonal connections. These habits and actions have been lumped together as an overall framework entitled “The Pillars of Lifestyle Medicine.” Each will be discussed in this section.
Physical Activity
Physical Activity has been shown in literally thousands of studies to promote overall good health and serve as a key component of prevention and treatment of various diseases. The 2018 Physical Activity Guidelines Advisory Committee Scientific Report emphasized that physical activity carries multiple benefits for people of all ages from infancy through old age. 2 Regular physical activity has specifically been demonstrated to reduce the risk of CVD, type 2 diabetes (T2DM), the metabolic syndrome, obesity, and certain types of cancer while enhancing cognition and mental health. In addition, the Physical Activity Guidelines for Americans 2018 Scientific Report (PAGA 2018) 2 corroborates that regular physical activity enhances quality of life, improves sleep and results in general feelings of enhanced well-being and improved daily functioning. Some of these benefits of physical activity occur immediately and almost all of the benefits become even more significant with ongoing and regular performance of moderate or vigorous physical activity.
Physical activity decreases the likelihood that a woman will gain excessive weight during pregnancy. 27 It also yields a decrease in the likelihood of post-partum depression. Physical activity has been shown to improve cognitive functioning and lower the risk of dementia. These are particularly important areas since dementia represents a significant health problem in the United States with more than 4.9 million individuals suffering from Alzheimer's Disease or other forms of dementia. 28 In addition, physical activity has been shown to decrease the likelihood of falls and lower the risk of sarcopenia in older individuals by helping to preserve lean body mass. 29
As will be discussed later in this review, numerous studies have shown that physicians own physical activity behavior predicts the likelihood that they will recommend physical activity to their patients. Unfortunately, it has been estimated that less than 40% of physicians regularly counsel their patients on the importance of increasing physical activity. In order to try to improve this likelihood of exercise prescription, the American College of Sports Medicine launched the “Exercise is Medicine” (EIM) initiative which provides a variety of tools to simplify and improve the likelihood that physicians will provide physical activity recommendations. 30 The EIM program also has urged health care providers to report level of physical activity as a “vital sign” during all patient visits.
Nutrition
Healthy nutrition plays a key role in daily lifestyle habits and practices that affect virtually every chronic disease. The critically important role of nutrition has been emphasized in multiple consensus statements, by numerous professional organizations and is further codified in the Dietary Guidelines for Americans 2020-2025 (DGA 2020-2025) Scientific Report. 4 Consensus statements which support the role of nutrition in reducing the risk of CVD, T2DM, obesity, cancer, and many other conditions, are quite similar to each other. 31 These Consensus Statements consistently recommend dietary patterns that are higher in fruits and vegetables, whole grains (particularly high fiber), non-fat dairy, seafood, legumes, and nuts. These guidelines are also consistent in recommending diets lower in red and processed meats, refined grains, sugar sweetened foods and beverages, and saturated and trans fats. All of the guidelines emphasize the importance of combining proper nutrition with regular physical activity and balancing calories as strategies to maintain a healthy weight and further reduce the risk of chronic diseases.
Dietary guidelines, over the past 2 decades, have moved from recommending specific nutrients and foods to greater emphasis on dietary patterns. There has also been an increased emphasis on strategies to enhance adherence to known healthy nutritional guidelines. Despite the consistency of dietary recommendations, a distinct minority of Americans follow these guidelines. For example, less than 12% of individuals eat the recommended daily servings of fruit and less than 7% consume the recommended daily number of servings of vegetables. 32 In the area of hypertension, for example, less than 20% of individuals with high blood pressure follow the DASH diet which has been shown to contribute to significantly lowering blood pressure. 33
The field of nutrition has changed dramatically over the past 2 decades. In the 1990s a strong recommendation was made particularly for those at risk of cardiovascular disease, to consume a low-fat diet. This did not appear to be an unreasonable recommendation, but the scientific data to support this dietary recommendation has changed. Several research studies have now demonstrated that a low-fat diet does not reduce the risk of heart disease any more than the standard American diet. 34 What has emerged, however, is that diets which contain increased fruits and vegetables and whole grains along with other healthy foods substantially reduce the risk of CVD and many other chronic diseases. This was clearly demonstrated in the PREDIMED study 35 which provided the scientific underpinnings for the Mediterranean Diet.
The Mediterranean Diet as well as the Dietary Approach to Stop Hypertension (DASH) and the Healthy US Eating Pattern recommended by DGA 2020-2025, as well as multiple diets from the AHA in their most recent nutritional guidance, 3 have all been demonstrated to substantially lower the risk of heart disease. The basic underlying hypothesis now for the health benefits of these diets is that they lower inflammation in the body which is a key component inciting various chronic diseases.
Unfortunately, many physicians find it daunting to keep up with the rapidly emerging field of nutrition science. Recent surveys have indicated that over 80% of physicians do not feel that they are adequately trained in nutrition. 36 Even in the subspecialty of cardiology, over 90% of cardiologists feel that they do not have adequate training to provide patients with the most up to date nutritional guidance. It is reassuring, however, that 95% of cardiologists feel that recommending healthy nutrition to their patients is imperative for their subspecialty. 37 Clearly, efforts need to be made to enhance physician education in all aspects of lifestyle medicine and, in particular, nutrition.
Obesity and Weight Management
Obesity is a pandemic representing one of the most significant public health challenges to world health in recent history. It is currently estimated that over 2.1 billion people in the world are currently obese. 38 In many ways, obesity represents the quintessential lifestyle disease.
It has been well established that obesity results from energy imbalance and may also have a genetic or epigenetic component. Thus, both nutrition and physical activity are important components in lifestyle interventions. These are important not only for short-term weight loss but also long-term maintenance of healthy body weight.
In 2013, obesity was recognized by the American Medical Association (AMA) as a disease. Multiple research studies further support that obesity increases the risk of many other chronic diseases including CVD, T2DM, cancer, chronic kidney disease, the metabolic syndrome, and many musculoskeletal diseases. 39 It may appear simple that a decreased caloric intake or increased physical activity would contribute to weight loss; however, the process is more complicated. The consensus statement on metabolism from the American Society of Nutrition emphasized that metabolism consists of multiple factors including percentage of body fat and also is related to a host of environmental factors. 40
Current research supports the concept that obesity leads to a condition of total body inflammation which may be why it is linked to so many chronic diseases. Obesity is a condition characterized by accumulation of excess adipose tissue. Adipose tissue has been shown to be highly metabolically active.
While there are many potential causes of obesity, the leading ones are the following: • Energy imbalance—On the most fundamental level weight changes are associated with an imbalance between energy intake and energy expenditure.
41
When energy intake exceeds energy expenditure excess energy is stored as fat which leads to increased adiposity. • Genetics and Epigenetics—While obesity is typically considered a consequence of prolonged energy imbalance, there is increased evidence that inherited factors also contribute in significant ways.42,43 It is estimated that 30%–50% of variation in the likelihood of obesity can be explained by inherited genetic susceptibility. A particular area of recent interest has been in the area of epigenetics. In this area, DNA methylation is thought to result in inflammation which can further result in changes in insulin signaling and lipid metabolism. The American diet is thought to be one of the main culprits responsible for both obesity and DNA methylation.
Additional evidence also implicates other potential causes for obesity including infections, smoking, inadequate sleep, and changes in gut microbiota (see subsequent section). Multiple other factors are currently being researched for potential linkages to obesity including pharmaceutical agents, temperature control and endocrine disruptors. 44 While these are all under investigation, clear evidence does not exist for these additional underlying factors at the current time.
Tobacco Products
Smoking is a leading preventable cause of death and disease in the United States and the single most important risk factor for coronary heart disease (CHD).45,46 Over 20 million premature deaths are attributable to smoking exposure and secondhand smoke in the United States as documented in the 2014 Surgeon General’s Report. 47 In addition, within this number, 2.5 million deaths are among non-smokers who died from diseases caused by exposure to secondhand smoke. Despite years of decline in the prevalence of smoking, cigarette consumption still counts for approximately 480,000 deaths attributed to smoking related diseases in the United States each year. For example, smoking causes 32% of CHD. 48 The economic costs attributable to smoking are also substantial. It has been estimated that over 30 billion US dollars were spent between 2009 and 2012 including direct health care expenditures and loss of productivity because of smoking. Cigarette smoking is not only a major risk factor for CVD, but also multiple other atherosclerotic diseases such as stroke, erectile dysfunction, and chronic kidney disease as well as chronic obstructive pulmonary disease (COPD) and asthma.49,50
Cigarette smoking is also associated with a variety of cancers including cancer of the lung, bladder, cervix, oral cavity, larynx, esophagus, stomach, kidney, uterus, and pharynx.49,50 For all of these reasons, it is imperative that lifestyle medicine physicians assess smoking status in every patient and offer advice and programs to help individuals cease smoking at the earliest possible time. It should be emphasized that smokers who quit reduce their excess risk of a coronary event by 50% in the first 2 years after smoking cessation. 49 The risk of former smokers developing CHD becomes the risk of never smokers after 3-5 years.
Stress, Anxiety, and Depression
Anxiety, depression, and stress are all endemic in the modern fast paced world. Lifestyle interventions have been demonstrated to play an effective role in ameliorating all three of these conditions.51,52
Within mental health disorders, anxiety is the most common. 53 The overall prevalence of anxiety disorders in the population has been reported as over 30%. Regular physical activity has been demonstrated in multiple studies to lower both acute anxiety (state anxiety) and trait anxiety (longitudinal anxiety). Studies exploring lifestyle strategies to reduce anxiety have typically utilized 30 minutes of moderately intense physical activity per session.
Depression is also quite common with a lifetime risk of significant depression of 10% in the US population. 54 Even without significant symptoms of depressive disorders, levels of depression can adversely influence both health and quality of life. Physical activity has been repeatedly shown to decrease symptoms of depression. Once again, studies have typically employed 30 minutes of moderate or intense physical activity performed on a regular basis as a strategy to reduce depression.
Stress is also common in modern society. It has been estimated that more than 30% of individuals have sufficient stress in their daily lives to hinder their performance at home or at work. Multiple lifestyle medicine modalities are effective in stress reduction including physical activity, mindfulness meditation and others. 55 Multiple mind/body therapies have also been demonstrated as helpful in managing stress. These include the relaxation response and multiple mind/body therapies including meditation, self-awareness, body scanning, contemplation, prayer, and love and kindness. Some movement practices can also result in lowering levels of stress. The most prominent in this area are yoga and tai chi.
Sleep
Sufficient sleep is essential for optimal health and life itself.56-59 Sleep plays a significant role in virtually every aspect of living including metabolism, brain function, systemic physiology, appetite regulation and function of the cardiovascular immune and hormonal systems.
Lifestyle factors play a significant role in maintaining healthy sleep. Normal healthy sleep is characterized by good quality, sufficient duration, appropriate timing and regularity and the absence of sleep disorders. Despite the importance of sleep, 70 million people in the United States have a chronic sleep disorder which impacts on daily functioning and health. 59
There are over 100 sleep disorders. 60 These are typically manifest by failure to obtain the necessary amount or quality of sleep, chronic sleep deprivation, inability to maintain sleep continuity (disrupted sleep), difficulty maintaining sleep (insomnia), and disordered sleep, for example, sleep apnea, and restless leg syndrome. 61
Sleep disruption is very common. The National Sleep Foundation in a 2014 survey recorded that 35% of American adults rated their sleep quality as “poor” or “one fair.” Disrupted sleep at least night per week was reported by 45% of respondents while 53% of respondents had trouble staying asleep 1 night in the previous week and 23% of respondents had trouble staying asleep on five or more nights in a week. Snoring is also common and reported by 40% of respondents.
Sleep Disordered Breathing (SDB) is a subset of the general category of sleep disruption and is a significant risk factor for CVD. 62 One of the most prominent types of SDB is obstructive sleep apnea (OSA) which may be found in 40%–80% of patients with hypertension, heart failure, coronary heart disease and cerebrovascular disease. It is thought that the underlying etiology of OSA is ischemia.63,64 A more general underlying cause for SDB is the triggering of the sympathetic nervous system and the release of proinflammatory proteins.
It should also be noted that quality and duration of sleep change as people grow older. As many of 50% of older adults complain of sleep problems including disturbed or “light” sleep.65-67 For all of these reasons, the AHA lists sleep as one of the key components of their overall framework for reducing the risk of heart disease called “Life’s Essential 8.” 68 All lifestyle medicine clinicians should assess the level of sleep and potential disruptions in every patient but particularly those over the age of 65.
Positive Interpersonal Connections
Positive interpersonal connections represents one of the six key pillars of lifestyle medicine. The issue of problems with interpersonal connections has recently come to the foreground. It was particularly exacerbated by isolation required related to COVID-19. A recent book by the US Surgeon General, Vivek Murthy, 69 quoted a Kaiser Permanente Foundation study that found that 22% of individuals regarded themselves as “lonely.” On the positive side, a recent book by Daniel Buettner indicated that positive social connections was a hallmark of most societies which he called “Blue Zones” where individuals lived to long periods of healthy life. 70 In addition, a recent book published related to the ongoing Harvard Student Study which has now been in progress for 80 years, cited positive interpersonal connections as the simple most important component of living a healthy and “good life.” 71 Dr Murthy reports that loneliness carries the equivalent risk of consuming 6 alcoholic beverages a day or smoking 15 cigarettes. He states that loneliness carries a greater health risk than obesity.
Lifestyle medicine clinicians should assess levels of interpersonal connections in every clinical encounter. Oftentimes, loneliness is hidden because individuals feel ashamed to admit that they are lonely. The mere fact that the clinician asks about social connections indicates that a clinical encounter is a safe place to have this type of discussion.
Lifestyle Medicine Approaches in the Treatment and Prevention of Chronic Diseases
Lifestyle medicine modalities have been demonstrated in numerous studies to play significant roles in both the prevention and treatment of many chronic diseases and conditions. This section will explore some of the most common disease or conditions where lifestyle modalities have been studied.
Cardiovascular Disease
The strength of the literature supporting lifestyle medicine modalities as key components of the treatment and prevention of heart disease is underscored by its inclusion of numerous documents and guidelines from the AHA and the ACC.3,18-20 Despite overwhelming evidence that positive lifestyle measures lower the risk CVD, it has been difficult to translate this information into the habits and actions of individuals. It should be noted that between 1980 and 2000 mortality rates from CHD in the United States fell by 40%. 72 Almost half the reduction in CHD between 1980 and 2000 was attributed to improvement in such lifestyle risk factors as smoking cessation, increased physical activity, and better control of cholesterol and blood pressure. Unfortunately, however, the increase in obesity and T2DM and glucose intolerance levels during this period of time has the potential to wipe out all the gains in other lifestyle related risk factors.
Despite significant progress in lifestyle measures and CVD, it still remains the leading cause of mortality in the United States resulting in 37% in all annual deaths. 73
Various lifestyle strategies are critically important for reducing the risk of cardiovascular disease. For example, in the area of physical activity, guidelines from the PAGA 2018 to obtain 30 minutes of moderate physical activity at least 5 times per week results in reducing the risk of CVD and all-cause mortality by 70%.
2
This relationship is depicted in Figure 1. As also shown in this Figure, even one 30-minute episode of physical activity per week decreases the risk of heart disease by 20%. From the 2018 Physical Activity Guidelines Advisory Committee. 2018 Physical Activity Guidelines Advisory Committee Scientific Report. Washington, DC: U.S. Department of Health and Human Services, 2018.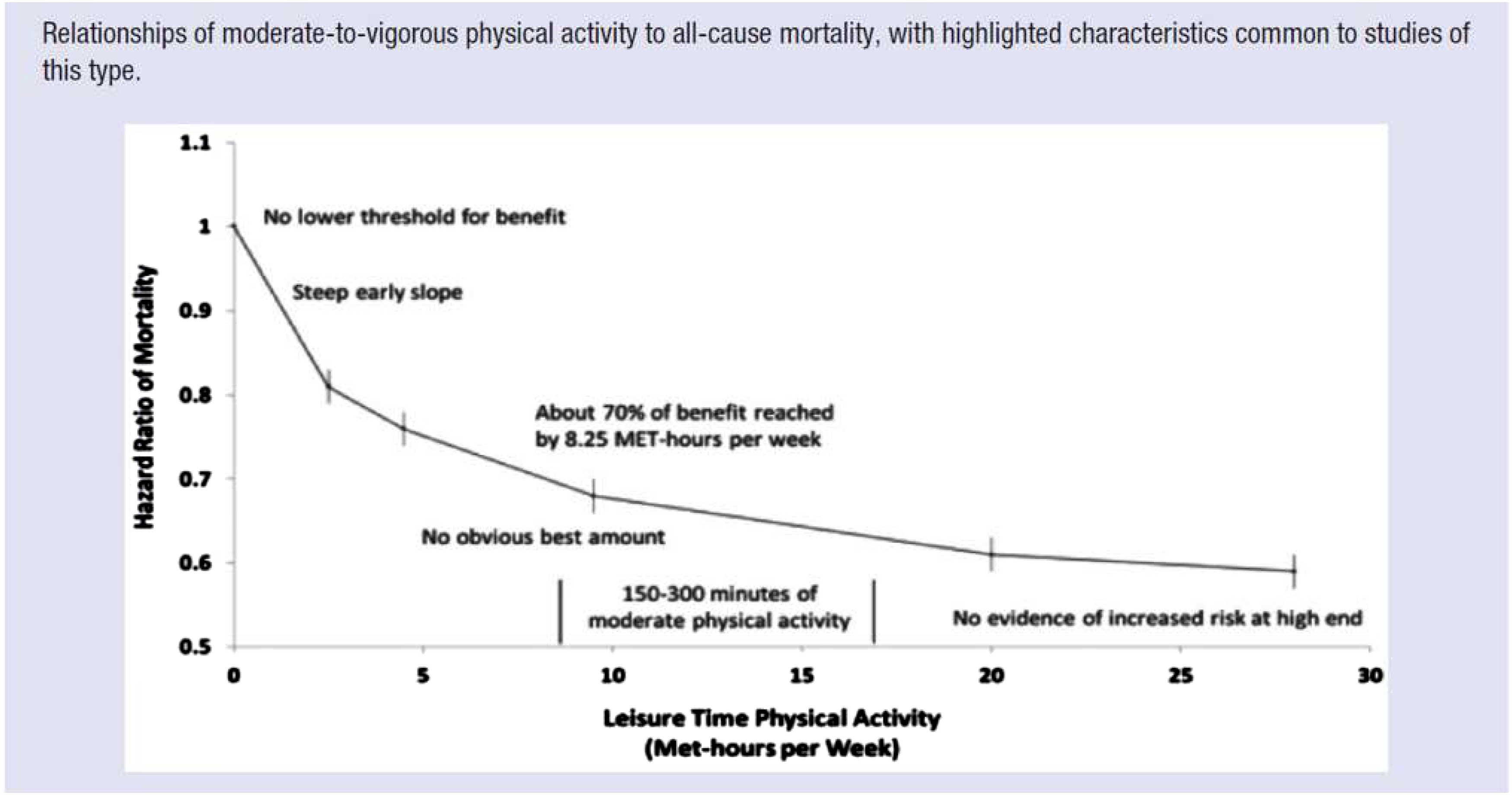
Unfortunately, most physicians do not encourage their patients to exercise enough. Studies have demonstrated that less than 40% of physicians routinely recommend physical activity for patients. 74 In one survey of 175 primary care physicians, only 12% were aware of the recommendations from the American College of Sports Medicine and the PAGA 2018 for regular amounts of physical activity. 75
Nutritional factors also play an important role in lowering the risk of CVD and CHD. Multiple documents from the AHA as well as the DGA 2020-2025 all recommend dietary intervention to lower the risk of CVD.2-4 The diets that are recommended are very similar to each other and include an increased amount of fruits and vegetables and whole grains as well as decreased consumption of saturated fats, red meat, sugar sweetened beverages and trans fats. Among the multiple healthy diets emphasized are the US Healthy Diet Pattern, 4 the Mediterranean Diet, 35 the DASH Diet, 33 the vegetarian diet, 34 and other plant-based diets.
Being overweight or obese also increases the risk of heart disease as does smoking and exposure to tobacco products. It should be noted that lifestyle measures such as regular physical activity, proper nutrition, weight management and avoidance of tobacco products are also important to control blood pressure and lipids as well as playing a major role in control of blood glucose.18-20
Diabetes, Pre-Diabetes, and the Metabolic Syndrome
Lifestyle modalities are also critically important to lower the risk and assist in the treatment of T2DM, pre-diabetes and the metabolic syndrome. In the United States the prevalence of T2DM has increased dramatically over the past 30 years. 76 As of 2015, the Centers for Disease Control and Prevention reported more than 100 million US adults who are living with T2DM and/or pre-diabetes. These include 30.3 million US residents (9.4% of the population) who have T2DM and another 100 million individuals with pre-diabetes (33.9% of adults).
Lifestyle therapies including medical nutrition therapy (MNT), physical activity and/or education counseling all play critical roles in both the prevention and management of T2DM. 77 Multiple studies have also shown that lifestyle interventions implemented in individuals with pre-diabetes can effectively prevent or delay T2DM in some instances by up to 15-20 years. 78
A recent framework for approaching these conditions focused on glycemia has been developed. This is called Dysglycemia-based Chronic Disease (DBCD) which emphasizes the primacy of treating elevated glucose levels at the earliest possible time utilizing lifestyle measures. 79
Obesity
Obesity is a pandemic representing a significant public health challenge around the world. It is currently estimated that 2.1 billion people in the world are obese. In the United States, over 72% of the adult population is either overweight or obese. 80 Obesity is associated with multiple chronic diseases such as CVD, T2DM, many different cancers, osteoarthritis, and multiple other medical conditions. In addition, a gain of as little as 10-12 pounds increases the risk of multiple chronic diseases. 81 Both regular physical activity and attention to proper nutrition are key lifestyle modalities for both lowering the risk of developing overweight or obesity and also in treating obesity and preventing weight gain.
Cancer
Cancer is the third leading cause of death in the United States behind only CVD and stroke. In 2016, it was estimated that 1,685,215 cases of cancer were diagnosed in the United States and 595,690 individuals died from the disease. 82 Lifestyle measures play a significant role in both the prevention and treatment of cancer. In addition, lifestyle measures play an important role in the ongoing health of cancer survivors. These measures include regular physical activity, proper nutrition, and weight management.83-85 These factors were underscored by the joint statement issued by the American Cancer Society (ACS), the American Diabetes Association (ADA) and the AHA on the prevention and early detection of cancer, cardiovascular disease, and diabetes. 86
Brain Health/Dementia/Cognition
A healthy brain is essential for a fulfilling life. Many lifestyle measures are essential for maintaining brain health. Strong links exist between brain health and cardiovascular health. This fact was underscored by the Presidential Advisory from the AHA and the American Stoke Association (ASA) on “Defining Optimal Brain Health in Adults.” 25 Lifestyle measures such as maintaining a healthy body weight, controlling blood pressure, lowering the risk of T2DM, increasing physical activity, and not smoking are all factors to enhance or preserve brain health which can be treated by lifestyle modalities.
These issues are particularly important as the population in the United States and other advanced countries continues to age. The United States has an estimated 5.1 million individuals over the age of 65 with Alzheimer’s disease which is the most common form of dementia. Recent evidence has suggested that early adoption of positive lifestyle measures can significantly lower the risk of Alzheimer’s disease. It should also be noted that lifestyle modalities such as regular physical activity are also highly effective in treating anxiety, depression and also ameliorating stress. These issues are very important, not only to quality of life, but also for brain health.
Lifestyle Medicine and Physician Education
The level of physician education in lifestyle medicine modalities is woefully inadequate. For example, in 1985, the National Academy of Science recommended that all medical schools devote at least 25 hours to nutrition education. 87 Now, almost 40 years later, only 27% of medical schools meet that minimal criteria. Moreover, many of those medical schools list courses in biochemistry as their offerings in the area of nutrition education and not a more broad-based approach to nutrition and disease prevention. This is unfortunate since in recent surveys over 90% of medical students indicate that they are interested in diverse areas of lifestyle medicine such as physical activity and nutrition upon entry to medical school but this declines over the course of their four-year experience. 87 Shockingly, only 6% of medical schools offer a formal course in exercise physiology! 88
In the area of cardiology, over 90% of cardiologists feel that they do not have adequate background education in the area of nutrition to counsel patients. 37 A positive sign, however, is that 95% believe that healthy nutrition is an essential part of the practice of cardiovascular medicine and would support further education in this area for cardiologists at all levels of training. Of note, when cardiologists are asked to rate the importance of various modalities in the prevention of CVD, healthy nutrition scores higher than statins or blood pressure control! 37
Some recent efforts have been undertaken to enhance the education of physicians in the areas of nutrition and physical activity. In September, 2022, the Biden administration convened the “White House Conference on Hunger, Nutrition and Health.” 89 Many initiatives have grown out of this seminal event largely focusing on both the areas of nutrition and physical activity. It is hoped that these initiatives will yield higher levels of physician knowledge in these critically important areas. Other initiatives include the American College of Sports Medicine with their program on Exercise is Medicine which offers physicians practical tools to increase the likelihood of prescribing exercise. At the very least, it is essential that physicians have at least read the executive summaries of the Dietary Guidelines for Americans 2020-2025 and the Physical Activity Guidelines for Americans 2018 and keep the key concepts from these evidence-based documents in their toolbox.
Following the White House Conference on Nutrition and Physical Activity, a number of organizations stepped forward to help address the relative paucity of physician education in nutrition and physical activity. For example, ACLM made available to 1400 physicians in healthcare facilities around the country a five-hour educational program on nutrition and lifestyle medicine free of charge. A number of other organizations made significant contributions to assisting in the area of physician education and nutrition.
Other initiatives include the American Board of Lifestyle Medicine (ABLM) which was founded in 2016. As of 2023, over 2445 physicians have been certified in lifestyle medicine through the ABLM. In addition, 729 non-physician, healthcare professionals and 217 other U.S. practitioners have also been certified through the ABLM. 23 A Lifestyle Medicine Residency Curriculum (LMRC) was piloted in 2018 and has now been implemented in 207 residency programs across more than 100 sites and currently has 5560 enrollees. 23 In addition, an International Board of Lifestyle Medicine (IBLM) has been established to provide registration hubs and offer exams generated by the ABLM. These organizations are all part of the Lifestyle Medicine Global Alliance.
There is also considerable ferment in undergraduate medical education. Over 130 lifestyle medicine student interest groups have been founded in medical schools throughout the United States. 87 Thus, there are continued educational efforts through multiple organizations in the area of lifestyle medicine.
The next breakthrough will come when lifestyle medicine is fully accepted by the certifying organizations for both undergraduate and graduate medical education.
Lifestyle Medicine, Personal and Planetary Health
A strong relationship exists between lifestyle medicine modalities to be adopted for personal health and their impact on planetary health. A number of prestigious commissions have concluded that unless major changes occur in the dietary practices of people around the globe, at some point in the future the planet will no longer be able to provide the human race with adequate food. 90 For example, Western dietary habits have made a significant impact on global warming. 91 Over 70% of fresh water in the world is now used for agricultural purposes. Animal husbandry generates significant pollution. Methane gas generated from cow manure is one of the most potent factors in global warming (over 30 times as polluting as carbon dioxide from internal combustion engines). In fact, agricultural practices are the leading cause of pollution responsible for global warming and far surpass issues such as automobile emissions. 91 Thus, it is essential that lifestyle medicine physicians become knowledgeable, not only about the personal health impacts of lifestyle practices and habits but also the strong association between these habits and practices and health of the planet.
Health Equity
Understanding disparities in health has become a major topic in American medicine. While significant disparities in health equity have existed for many decades, these were exacerbated during the COVID-19 pandemic. Individuals with hypertension, obesity, and diabetes were 3-4 times more likely to suffer morbidity and mortality than individuals who did not have these conditions. 92
Many of these adverse consequences can be traced back to poor nutritional habits. These disparities were particularly prominent in Black and Hispanic populations. These populations were 3-4 times more likely to require hospitalizations and ultimately die from COVID-19 than were members of the Caucasian race.
A number of medical organizations including the American College of Physicians (ACP) 93 and the AHA have issued policy statements emphasizing the critical importance of addressing issues related to health equity and its effects on health parameters. 94 Certainly, lifestyle medicine modalities such as physical activity, nutrition, weight management, and avoid tobacco products can play significant roles in helping to address the current significant problem of health disparities in the United States.
The Microbiota
There has been a recent surge in interest in the relationship between the gut microbiota and various health issues. 95 The human gut contains literally trillions of bacteria, viruses, fungi, etc. which can either serve to enhance health or create adverse health consequences. 96
The Western diet in particular has been associated with dysbiosis by favoring gut bacteria that create adverse health consequences. These changes in the gut microbiota may contribute to “leaky gut syndrome,” dyslipidemia and immune dysfunction. Dysbiosis caused by the Western diet can increase the likelihood of inflammation which underlies a variety of chronic diseases. In contrast, plant-based diets generally support more favorable bacterial growth in the gut and help generate beneficial short chain fatty acids such as butyrate. The health effects of the microbiota is an area of active investigation but there is no question that human health interacts with the gut. This is an area where lifestyle medicine can and will play a very significant role particularly in the area of nutrition.
Atherosclerosis
A substantial advance has occurred over the past 20 years concerning how we regard the process of atherosclerosis.97-99 This carries significant implications for practitioners of lifestyle medicine. The view of atherosclerosis which has emerged in the past 2 decades involves the interactions between the inner lining of the arteries (endothelium), lipids, and how inflammatory cells can invade below the endothelium. Both the lipid component and the inflammatory component are extremely important processes within atherosclerosis, and both are thus highly relevant to practitioners of lifestyle medicine. 100 Lifestyle medicine modalities can be utilized not only to lower lipids within the arteries but substantially reduce inflammation which has become increasingly the hallmark of the modern understanding of atherosclerosis. Atherosclerosis is a systemic condition which involves not only CHD, but also stroke, hypertension, peripheral artery disease, erectile dysfunction, and chronic kidney disease.
Modalities such as regular physical activity, plant-based eating and stress reduction have all been demonstrated to decrease inflammation in atherosclerotic plaques allowing them to stabilize. Lifestyle treatments for both CHD and T2DM carry significant implications for the development of atherosclerosis. Lifestyle modalities not only impact established risk factors such as dyslipidemia, obesity, and diabetes but they may also interact with underlying genetic changes that can result in decreased inflammatory markers.
Inflammation
In the past 2 decades, a unifying hypothesis has emerged linking multiple chronic diseases such as CVD, obesity, T2DM, and cancer to underlying inflammatory processes. These inflammatory processes, as already indicated, is also central to the initiation of atherosclerosis.
It used to be thought that fat cells, for example, were largely passive storage sites. Now it is clear that adipocytes are highly active generators of metabolically active compounds which can stimulate inflammation. Recent evidence has also emerged that the Western diet is highly inflammatory which provides another reason why it contributes to multiple chronic diseases. In contrast, plant-based diets such as the Mediterranean Diet, DASH diet and the US Healthy Eating Pattern are non-inflammatory which may be a major reason for why they have been shown to lower the risk of CVD so profoundly.
The Future of Lifestyle Medicine
The original intent for the field of lifestyle medicine, which was articulated back in 1999 with my initial, multi-authored textbook in this field, was to provide evidence of the benefits of multiple components of lifestyle medicine in one place where physicians could conveniently access the evidence. This goal remains a key issue for the field of lifestyle medicine moving forward.
There is no longer any serious doubt that what individuals do in their daily lives profoundly impacts on their short- and long-term health and quality of life. This is the fundamental concept behind the WHO initiative to combat non-communicable diseases. The WHO has stated that 71% of all annual mortality relates to non-communicable diseases. 101 Thus, the role of lifestyle habits and practices to both lower the risk of chronic disease and assist in its treatment is now well established by virtually every professional organization involved in metabolic disease. This underscores a very powerful position and opportunity for lifestyle medicine.
The future of lifestyle medicine will depend on adopting a dual strategy. First, the field needs to embrace important research in virtually every field of mainstream medicine. This includes significant research in CVD, T2DM, cancer, weight management and obesity, and many others. While embracing these studies, the field of lifestyle medicine can advance health care by bringing this information together in one understandable and accessible framework.
The future of lifestyle medicine will hinge also on continuing education efforts. In this regard the numerous lifestyle medicine student interest groups will play a major role. In addition, the American Board of Lifestyle Medicine must continue to develop educational materials and offer board certification in lifestyle medicine. The ultimate goal, however, will be for the field of lifestyle medicine to become embedded in both undergraduate and graduate medical education curricula in medical schools throughout the United States and in many other countries.
It must be emphasized that the evidence base for lifestyle medicine is incredibly powerful. Despite claiming to be evidence-based, mainstream medicine has largely ignored the enormous evidence available for how daily habits and actions impact on health. It is important for the field of lifestyle medicine to continue to articulate these profound connections and continue to educate medical professionals at all levels about the role of daily habits and actions in overall health.
Conclusion
The field of lifestyle medicine, which is based on the connection between daily habits and actions and short- and long-term health and quality of life has rapidly expanded in the United States and in many other countries around the world in the past 20 years. This achievement is based on the enormous scientific literature that supports the concepts that daily habits and actions such as physical activity, healthy nutrition, weight management, avoidance of tobacco products, the role of healthy sleep, and the power of interpersonal connections are all related to overall enhanced health and well-being. These habits and actions which have been utilized as a framework developed by the American College of Lifestyle Medicine entitled the “Six Pillars of Lifestyle Medicine.” All 6 pillars are deeply evidence-based. 16 They also are connected to central approaches to reducing the risk of or managing multiple chronic diseases including CVD, T2DM, obesity, cancer, and dementia. The central focus and opportunity for lifestyle medicine is to bring disparate bodies of high-level evidence together in one readily acceptable place to help physicians understand and utilize the power of daily habits and actions to promote good health. This synthesis has remained the central goal of lifestyle medicine over the past 25 years and is never more important than today.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
