Abstract
Lifestyle education is a key component of healthcare, particularly primary care. Multiple studies have shown that dedicated patient education on lifestyle topics, in addition to medication management, creates the most positive outcomes. Improving knowledge on health topics is critical for eliciting positive change in health behaviors. However, education takes time, and access to focused education outside of the office visit can be a challenge. We discuss here a quality improvement initiative to increase value-based care by utilizing telehealth to improve access to Lifestyle Medicine education during the COVID-19 pandemic. We focused on 4 primary objectives including creating a Lifestyle Medicine Virtual Referral Clinic (LMVRC) embedded within our Family Medicine Residency, determining payor mix of referred patients, utilizing a telehealth platform to provide lifestyle medicine education, and finally determining the influence of our services on patient’s perceived health. There were many key findings in the development, implementation, and evaluation of the LMVRC that could serve to assist others and our clinic in further development of lifestyle medicine education in the primary care setting. In our experience, a LMVRC embedded in a primary care setting proved to be an effective approach to provide access for patients and advancing value-based care.
“When analyzing the population referred to the LMVRC, the average patient had a BMI of 38 and weight loss was one of the primary goals noted.”
Introduction
Lifestyle education is a key component of healthcare, particularly primary care. Multiple studies have shown that dedicated patient education on lifestyle topics, in addition to medication management, creates the most positive outcomes. Studies have successfully shown that lifestyle medicine can help in preventing and treating non-specific low back pain and decreasing distress from chronic disease in adolescents.1,2 Nutrition education is the first line treatment for diabetes prevention and reducing glucose-related outcomes and diabetes self-management education (DSME) programs have been shown to reduce hospitalizations and readmissions.3,4 Focused, longitudinal programs addressing lifestyle factors are vital in achieving improved knowledge and behavior change. A program for youth with obesity implemented nutrition classes and exercise sessions and found significant improvements in insulin sensitivity, BMI, and waist circumference compared to controls who received only general health information. 5
Improving knowledge on health topics is critical for eliciting positive change in health behaviors. However, education takes time, and access to focused education outside of the office visit can be a challenge. Medical Nutrition Therapy (MNT) is a great example of a service that provides focused, lifestyle education. Unfortunately, lack of insurance coverage can be a barrier to access, especially for patients of low socioeconomic status, and Medicaid does not cover MNT in most states. 6 Multiple studies and primary care physician surveys have also shown office visit time to be a recurring barrier.7-9 In 2004, a study found that less than 1 min was spent in patient encounters reviewing lifestyle medicine topics such as diet, exercise, and smoking. 10 Per a 2012 study only 32% of patients reported their physician counseled them on physical activity recommendations. 11 While changes in the healthcare system, such as the Affordable Care Act have tried to prioritize primary preventative care, the actual clinic operations for lifestyle medicine as preventative care remain to be optimized.
Since the commencement of the COVID pandemic, access has also been a major barrier to lifestyle education and telehealth has since become a cornerstone for healthcare delivery. Telehealth has been shown to be an effective delivery method for management of chronic disease states such as diabetes, arthritis, hypertension, and chronic pain. A systematic review of 35 studies also found that telehealth improves access in terms of time to service and comprehensiveness of service. 12 These studies showed reduced wait times, reduced time to treatment, and an increase in the number of patients receiving indicated diagnostic tests or treatments. We discuss here a quality improvement initiative to increase value-based care by utilizing telehealth to improve access to Lifestyle Medicine education during the COVID-19 pandemic.
Methods
Objectives
Our quality improvement project focused on 4 primary objectives. Our first primary objective was to create a Lifestyle Medicine Virtual Referral Clinic (LMVRC) embedded within the primary care setting, to offer personalized education and goal setting with patients.
At the time of implementation, we were aware of 2 main lifestyle medicine-focused programs in our institution: Cardiopulmonary Rehabilitation and the Diabetes Prevention Program. While these programs have shown significant benefits in patient outcomes and disease burden reduction, lack of insurance coverage for these services is a barrier for some patients. A second primary objective was to determine the payor mix of referred patients to ensure open access.
As the COVID pandemic had significantly reduced in-person visits and increased staffing shortages, pivoting to a virtual method of delivery allowed us to bypass these barriers. Our third primary objective was to utilize a telehealth platform for providing lifestyle medicine education.
Although the benefits of lifestyle medicine education have been well documented in literature and associated with long-term positive health outcomes, we wanted to better understand the short-term impact and satisfaction among our patients. Our fourth primary objective was to determine the influence of our service on a patient’s health.
The quadruple aim framework was considered in the development of this project. Telehealth was used to increase access during COVID pandemic restrictions which also served as a cost consideration. After initial consultation, subsequent Lifestyle Medicine visits were centered around each patient’s unique medical problems, knowledge, and resources to enhance the patient’s experience. Schedule templates, length of visit and the development of educational videos addressed both the patient and clinician experiences.
Implementation Strategy
Setting
The LMVRC was established within our Family Medicine Residency clinic. The referral base included over 200 family medicine and specialty providers. The electronic medical record used was EPIC which had previously integrated Zoom technology for telehealth. A steering committee that included representation from primary care, specialty services, clinic leadership, information technology, referral management, and lifestyle medicine specialists was created to support buy-in and implementation.
Staff
Staff for the LMVRC during pilot integration included: • A lifestyle medicine board-certified provider • A medical assistant (MA) for intake scheduling, rescheduling, and patient education for virtual platform integration. • An administrative assistant to send and receive the patient questionnaires and upload to the EMR. • A clinic manager assigned to lead the steering committee and oversee implementation including new processes to support the clinic, lead data development and collection, platform troubleshooting, team coordination, marketing, and liaison to leadership.
Marketing
The LMVRC was initially marketed to all family medicine providers in the 11 primary care clinics in our region, starting 2 months prior to clinic opening (June 2021). After receiving requests from specialty services, select groups were also included. The Medical group leadership guided the marketing process, and no direct-to-consumer marketing was utilized for the LMVRC. Internal marketing materials were developed using American College of Lifestyle Medicine (ACLM) resources that explained the process to referring providers to maintain consistency in messaging and advocacy for lifestyle medicine.
Patient Encounters
The referral process offered each patient 10 visits with a lifestyle medicine provider within a 6-month period. Each visit was 40 min in length. The initial intake was used to gauge existing lifestyle practices and develop a plan for future visits. Subsequent visits were focused on one of the following lifestyle pillars per visit: healthy eating, movement, connection and stress management, sleep hygiene and risky substance use. Some lifestyle pillars required multiple visits. Medical history and medications were reviewed in conjunction with Lifestyle Medicine education, and, at the end of every visit, creation of Specific, Measurable, Achievable, Relevant and Time-Bound (SMART) goals was strongly encouraged; goals were reviewed periodically for troubleshooting and motivation.
In February 2022 (7 months after LMVRC initiation), due to patient request for audio-visual (AV) material, pre-recorded educational videos were created by the provider and offered using an open online platform prior to scheduled visit. This was initiated in February 2022.
Questionnaires
Pre-/post-survey
Development of patient pre-/post-surveys to assess lifestyle practices involved utilization of ACLM resources and revision from lifestyle medicine subject matter experts. The questionnaires included evaluating a patient’s motivation and confidence in each lifestyle medicine pillars (nutrition, sleep, stress, connection, physical activity, and substance use) to determine their stage of change. Participants rated their confidence level from 0-10 and these numbers were assigned to a stage of change based on the Transtheoretical Model. 13 A level of 0-3 was assigned “Pre-contemplative,” 4-6 was assigned “Contemplative,” 7 was assigned “Preparation,” 8-9 was assigned “Action,” and 10 was assigned “Maintenance.” 14 These categories were then combined to create 3 groups, with Group 1 including Pre-contemplative, Group 2 including Contemplative and Preparation, and Group 3 including Action and Maintenance.
Multi-Symptom Questionnaire
The Multi-Symptom Questionnaire (MSQ) was utilized to guide patient assessment as well as a symptom-based tool to capture changes in health. We recognized that biometrics changes using lifestyle techniques requires long-term follow-up, so the MSQ was used as a tool to capture short-term improvements.
Results
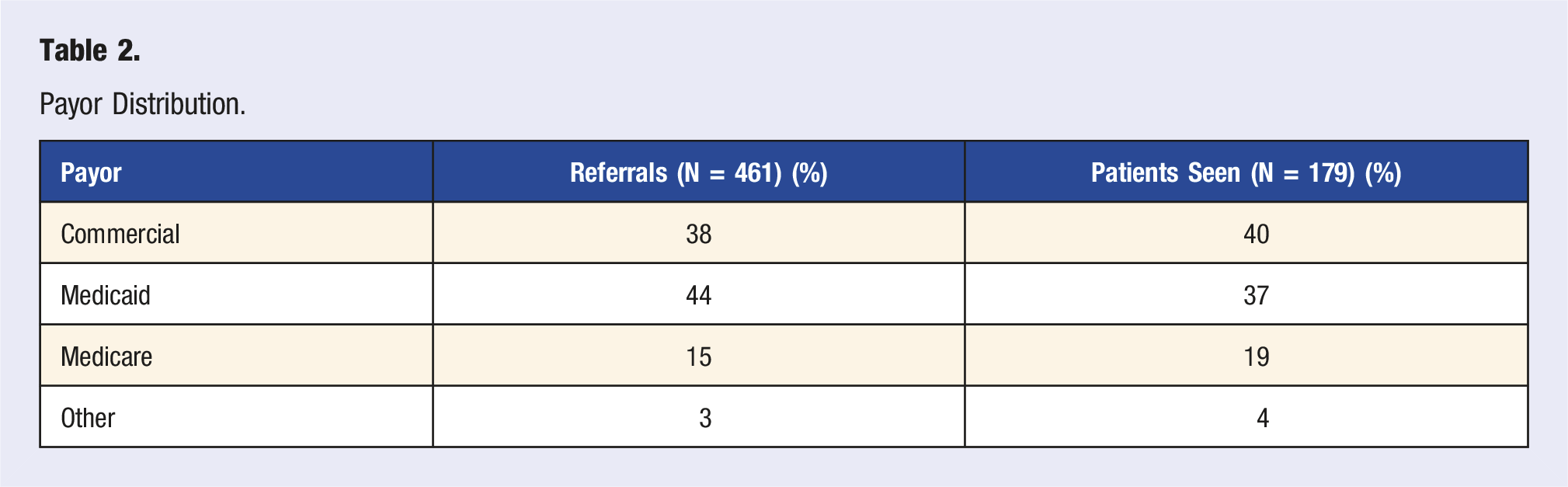
Between July 2021 and March 2022, 461 referrals were placed. Approximately 39% of all referrals translated into an initial Lifestyle Medicine consultation, 36% of patients referred declined to schedule and 25% of patients either scheduled for an intake and then canceled before being seen or did not respond to 3 outreach scheduling attempts.
Of the 461 patients referred to the LMVRC, 179 patients (39%) completed an initial consultation. Of those 179 patients seen, 20% were seen for initial consultation (intake only), 40% had 2-4 visits, 26% had 5-7 visits, and 14% had 8-10 visits. However, only 39 patients (22%) received education on all lifestyle pillars over an average of 7 visits and within a timeframe of 2 to 7 months.
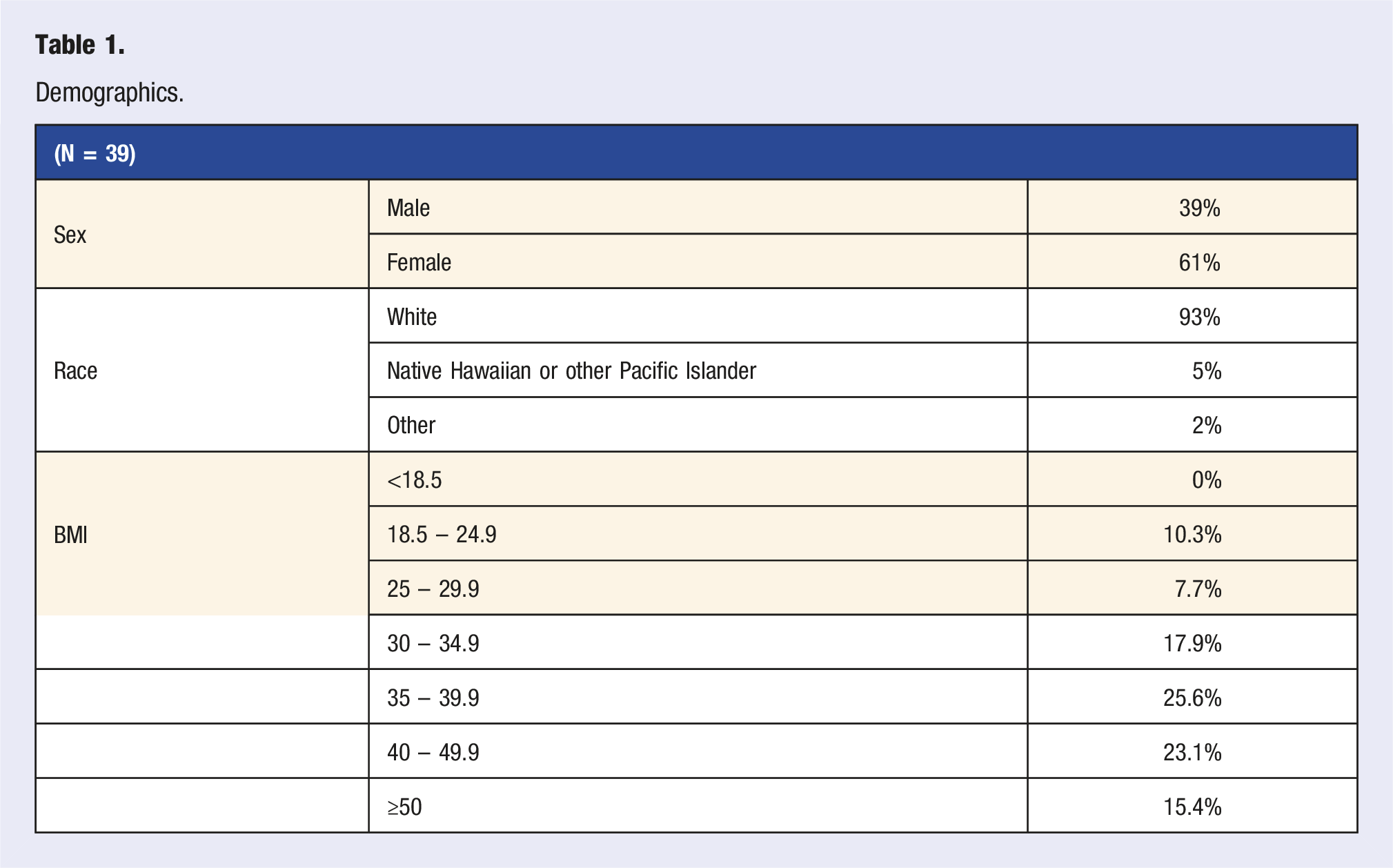
Demographics.

Payor Distribution.
Our third primary objective was to utilize a telehealth platform for lifestyle medicine education. To evaluate our virtual service, we looked at the following process measures in a monthly distribution (Figure 1): number of total patient visits, number of intakes (initial consultation), number of referrals, number of empty slots and number of no-shows. We used the process measures to determine the impact of three Plan-Do-Study-Act (PDSA) cycles during our intervention. Monthly LMVRC volumes.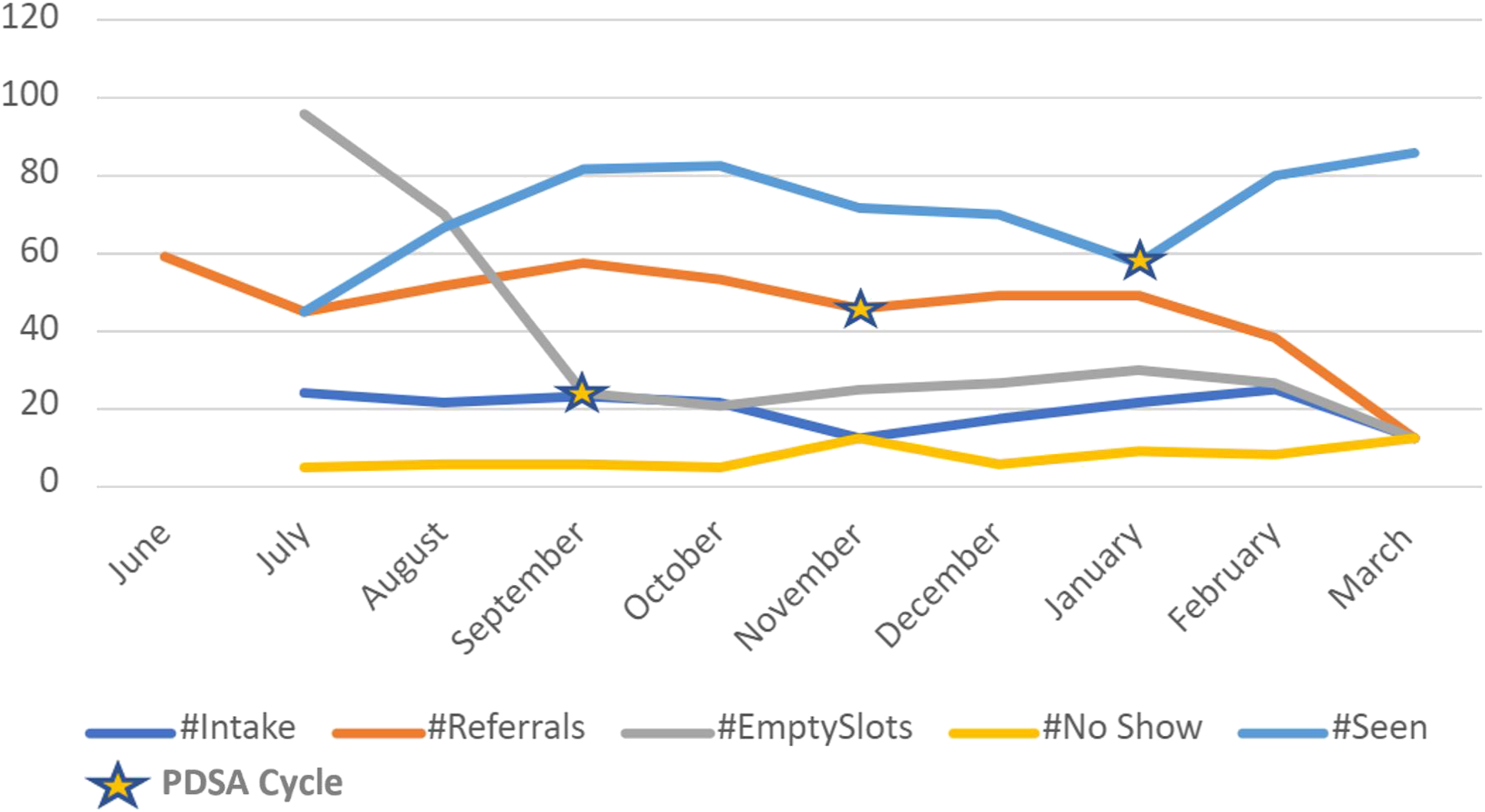
For our first PDSA cycle (September 2021), we changed our schedule from 40-minute visits to 60-minute visits. While our no-show rate remained the same, the number seen increased, and the number of empty slots decreased.
During PDSA Cycle #2 (November 2021), 2 changes were made. First, due to popular demand, we began accepting Lifestyle Medicine referrals from specialty clinics including neurosurgery and cardiology. Second, the Lifestyle Medicine MA educated referring clinic MAs on the process for directly scheduling referred patients into the LMVRC for initial consultation. This led to an increase in the number of referrals.
During PDSA Cycle #3 (February 2022), audio-visual materials were created to standardize the education of lifestyle medicine fundamentals. With this change, the number of empty slots decreased, and the number seen increased.
Data for our fourth primary objective, the outcome measures, came from the results of patient questionnaires including a repeat MSQ, confidence levels per pillar and overall satisfaction rating.
Of our 39 participants, 12 patients completed both pre- and post-MSQs. As noted in Figure 2, overall MSQ scores decreased in 8 out of 12 patients (67%). Percentage change for Multi-Symptom Questionnaire (MSQ).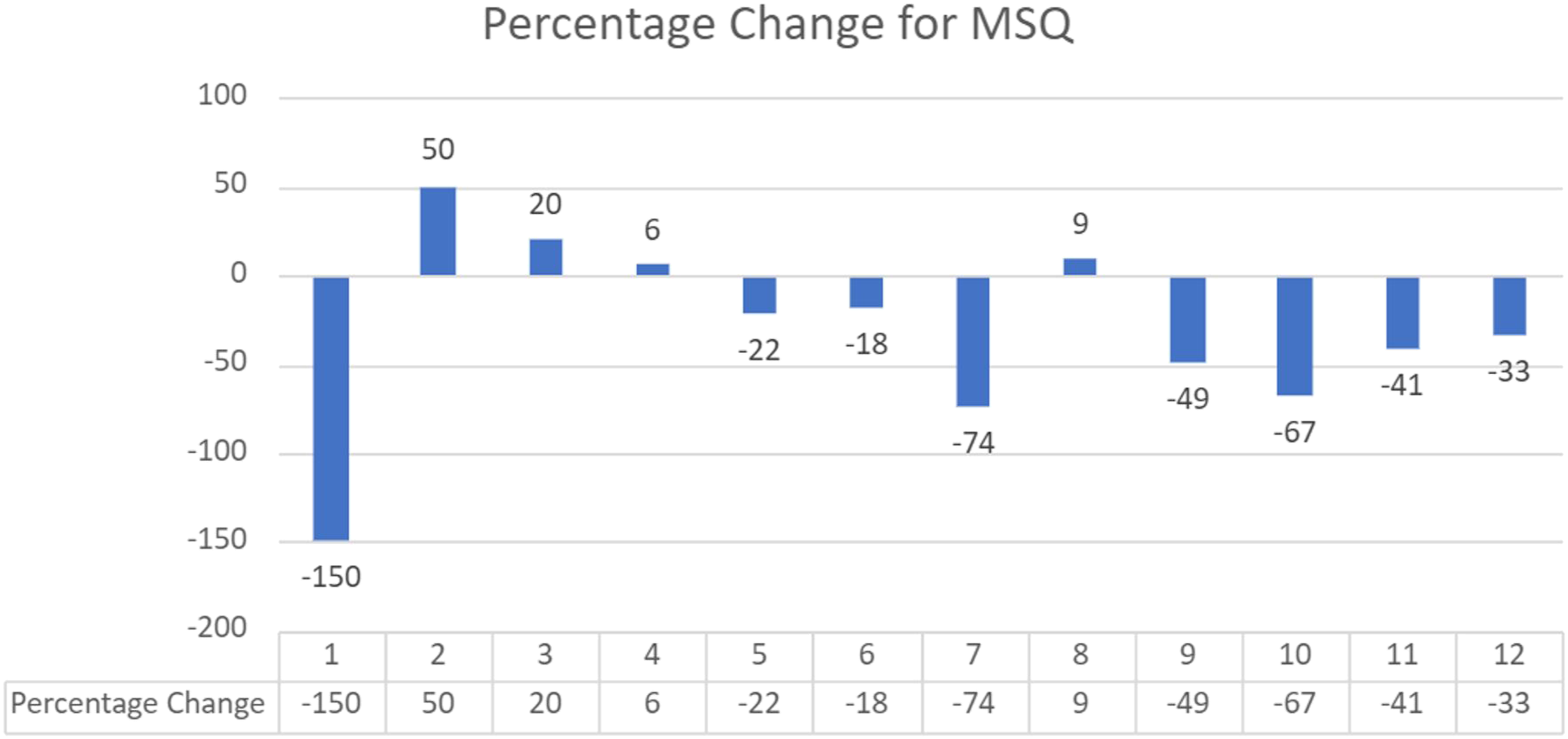
In analysis of Stage of Change and confidence levels across all 5 pillars (Figure 3), there were fewer participants in Group 1 (pre-contemplative) compared to both Group 2 and Group 3. Post-program surveys showed progression in stage of change increase among participants for Activity, Healthy Eating, Mental Health, and Social Connection. Stage of change before and after series of lifestyle medicine visits.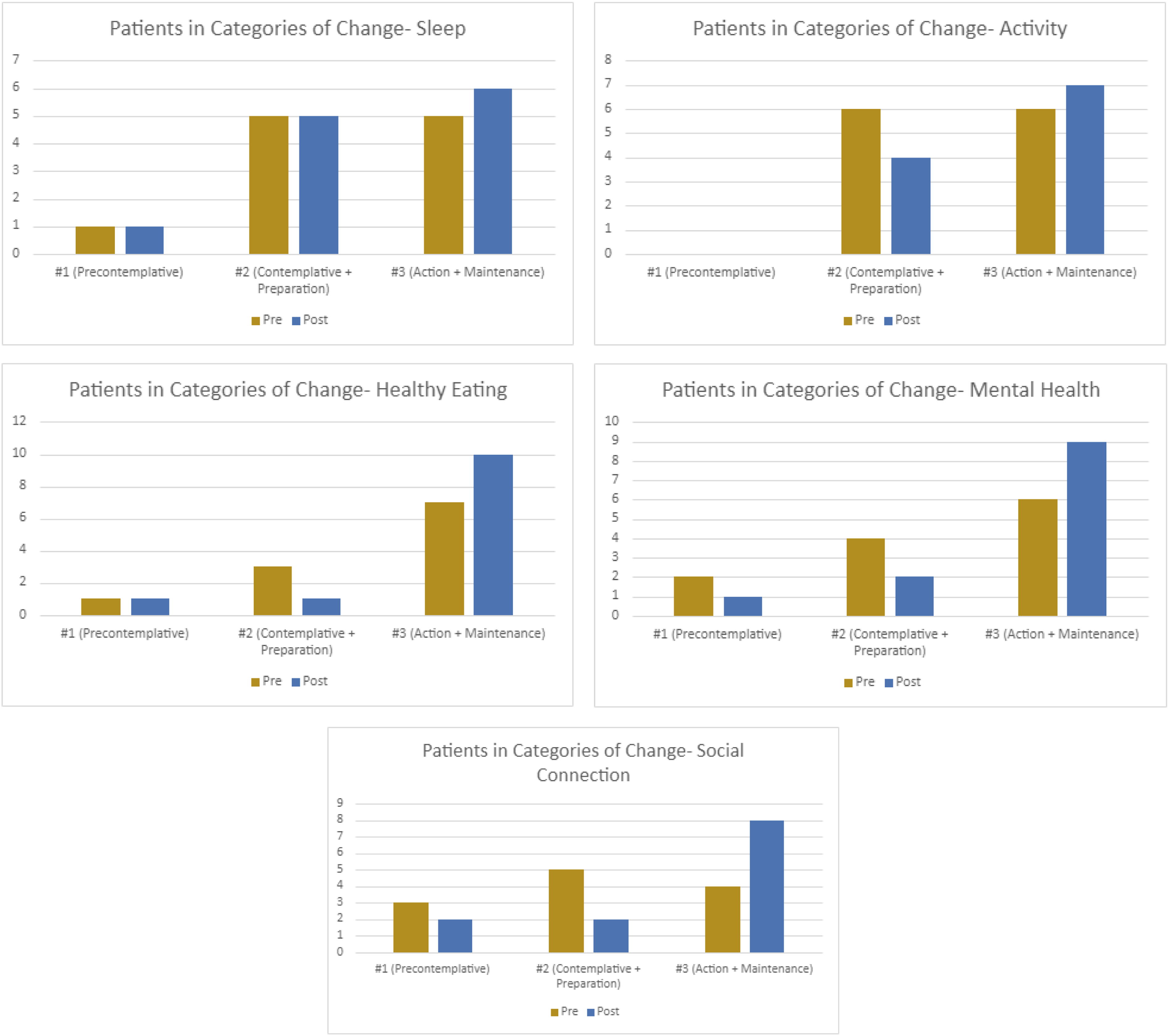
Discussion and Next Steps
There were many key findings in the development, implementation, and evaluation of the LMVRC that could serve to assist others and our clinic in further development of lifestyle medicine education in the primary care setting.
Addressing the need for increased availability of intensive lifestyle medicine programs that are accessible regardless of payor was the goal for developing the LMVRC. One of the key drivers for embedding the Lifestyle Medicine Referral Clinic within the Primary Care Clinic was to overcome the barrier of insurance coverage limitations preventing referral of Primary Care patients to outside LM entities. The largest volumes of referrals came from a Federally Qualified Health Center (FQHC) and a Family Medicine Residency training program which serve a proportionately higher percentage of Medicaid-insured and less resourced patients in our community. These two clinics accounted for 20% of the referral base and 80% of the referrals. Next steps include creating processes to address the sustainability of the LMVRC such as patient volumes, financial benchmarks, and other patient specific factors.
For successful implementation, direct scheduling privileges to ancillary staff of referring clinics were found to increase referrals. We also found that a simplified, consistent schedule, ideally with 30- or 60-min time slots increased patient volume and pre-reviewed, standardized audio-visual educational content is believed to increase patient empowerment and shift focus to maximize time spent on problem list, medication management, and disease prevention or reversal.
When analyzing the population referred to the LMVRC, the average patient had a BMI of 38 and weight loss was one of the primary goals noted. We intend to use this information to tailor lifestyle medicine education to the referred patient population in future studies.
In review of the patient MSQ scores, 67% of patients saw a decrease in their symptomatic complaints but 33% saw an increase. We hypothesize this increase could be secondary to an increase in awareness leading to heightened symptomatic experience or due to poor understanding of the pre-/and post-survey questionnaire. This is an important finding to improve communication processes with patients during the lifestyle medicine education process.
We also would like to address the difficulty in encouraging completion of all lifestyle tenets once the intake was completed. Of the 179 initial intake consultations performed, only 39 patients (22%) completed all of the lifestyle tenet education visits. One hypothesis could be a misunderstanding of what lifestyle medicine education included and the goal expectations set in each visit. Another could include limitations like access, cost, or time to implement lifestyle factors which deter the patient from attending further clinic visits.
In review of the patient surveys, we found that confidence levels overall increased and patients progressed upwards in the stages of change after completing the LMVRC intervention. Our findings suggest that the patients most likely to engage in the LMVRC are those that are already in the contemplative-preparation or action-maintenance stages thus confirming that assessing for stage of change is a useful tool to screen patients for likelihood of success. Other reasons could include access to audio-visual educational material and increased engagement during the consultations. Furthermore, we strongly believe that SMART goals, which were set in every virtual visit, were perceived steps to motivate patients towards action and increase confidence in the patient’s ability to achieve their goals. We suggest SMART goals should be used frequently during lifestyle medicine education and interventions.
Limitations
The small sample size of patients who completed lifestyle medicine visits was a limitation for quality data analysis. Selection bias by the referring provider could have also contributed to the demographics (Ex: BMI) and initial stage of change of patients seen in the LMVRC.
Conclusion
In our experience, a LMVRC embedded in a primary care setting proved to be an effective approach to provide access for patients and advancing value-based care.
Footnotes
Acknowledgments
Marcus Heisler, MD, MPH, DipABLM, for review of the article and editorial recommendations.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
