Abstract
More than one in three adults age ≥65 fall each year, and fall-related deaths are increasing in the United States. Falls risks can be reduced when older adults are able to engage in series of behavior changes to reduce their high fall risk factors. However, older adults perceive their fall risks to be lower than clinically indicated and adherence rates for fall prevention recommendations are suboptimal. Motivational interviewing (MI), a validated patient-centered behavior change communication approach, is ideal for addressing these gaps and facilitating older adults’ engagement in fall prevention. The goal of this paper is to present practical tips to apply MI for fall prevention for clinicians who may not be familiar with MI. We draw on our experience from providing MI sessions to high fall risk older adults within a randomized controlled trial. We describe how we delivered MI sessions and practical lessons learned from this experience. We present how basic MI skills can be used for fall prevention using a case study, how an older adult may move through Stages of Change for fall prevention, and how to address strongly held beliefs about fall prevention.
“Physiologic and behavioral fall risks such as loss of balance control and strength, orthostatic hypotension, vision impairment, or tendencies to hurry are developed over time.”
Introduction
Falls lead to significant negative physical and emotional trauma. One in three adults age ≥65 fall every year, and falls are the number one reason older adults lose their independence. 1 Falls are caused by biologic, behavioral, and environmental factors. Although biologic factors for fall prevention are well studied, there is a lack of effort and knowledge to improve behavioral fall risk factors. The Centers for Disease Control and Prevention (CDC) recommends talking to providers to identify fall prevention strategies and to implement balance exercises, environmental modifications for safety, and adjustment of high fall risk medication. 1 However, only half of older adults report their falls to their providers, 1 and only 18-50% of older adults adhere to these fall prevention recommendations.2,3 Older adults do not perceive fall prevention as relevant to them 4 and view fall prevention strategies as too intensive or inconvenient. 5 Strategies to overcome older adults’ resistance with fall prevention are necessary to enhance their engagement in fall prevention behaviors.
Motivational interviewing (MI) has immense potential to be applied to fall prevention. MI is a validated communication strategy to promote individual health behavior change.6–8 MI can be delivered in-person, virtually, and in brief formats (i.e., 15-30 minutes). There is emerging evidence to support the use of MI to address fall prevention.9,10 However, there is limited literature on practical application of MI with older adults in healthcare settings to address fall prevention.
In this paper, we draw on our experience from providing MI sessions to high fall risk older adults within a randomized controlled trial. We describe how we delivered MI sessions and practical lessons learned from this experience. We present how basic MI skills can be used for fall prevention using a case study, how an older adult may move through Stages of Change for fall prevention, and how to address strongly held beliefs about fall prevention.
Overview of Motivational Interviewing
Abundance of literature exists for MI.6–8 With clinicians who may not be familiar with MI in mind, we briefly describe elements of MI that pertains to facilitating patient-centered conversations for fall prevention. The fundamental elements of MI include: (1) MI specialist’s core communication skills; (2) a distinctive way of being called Spirit of MI 6 and (3) the four processes of MI. We use the term MI specialist as someone who utilizes MI. The core communication skills of MI include utilizing open-ended questions, affirmations, reflections and summary statements (OARS) to effectively move client’s behaviors toward change in conversations. 6 These skills are built on the MI specialist’s Spirit of MI, meaning that there’s constant recognition that each patient has absolute worth and autonomy in their life choices, and this unwavering respect is expressed through collaboration, evocation, compassion, and acceptance. 6
Equipped with these fundamental elements of MI, the MI specialist will facilitate MI conversations through four processes of MI known as engagement, focusing, eliciting (evoking), and planning. 6 Engagement refers to building trust and safety. As the MI specialist and the patient build a trusting relationship (engagement), the MI specialist will facilitate the conversation to provide clarity in a target behavior for change and potential outcomes (focusing). The MI practitioner will also facilitate forward movement in behavior change (elicit), meaning developing the momentum to shift the client toward change talk, commitment statement to adopt new behavior, rather than sustain talk, statements to indicate desire to remain at status quo. Finally, the MI specialist will facilitate conversations around planning next steps when the client is ready to adopt new behaviors (planning). Application of four processes of MI to fall prevention is illustrated in Table 2.
In order for these MI processes to take place, it is helpful for the MI specialist to understand where the patient is at for behavior change using the Stages of Change model 11 to facilitate behavior change. Stages of Change is a helpful conceptualization of how individuals move through series of stages—precontemplation, contemplation, preparation, action, and maintenance—as they adopt various health behaviors for fall prevention. Centers for Disease Control and Prevention (CDC) has been successful exemplifying how providers may respond to patients at various Stages of Change. 12 However, comprehensive description on how Stages of Change may shift toward change for fall prevention does not exist.
Motivational Interviewing for Fall Prevention (MI-FP) Study
As a study intervention for a federally funded study, Motivational Interviewing for Fall Prevention (MI-FP) was developed. In the MI-FP study, MI sessions were provided to older adult participants recruited from an internal medicine clinic at an academic medical center. Patients were eligible if they are age 65 or older, at high fall risk using the CDC’s Stopping Elderly Accidents, Death, and Injuries (STEADI) fall risk assessment questionnaire in which a score of ≥4 is considered high fall risk, 13 and received fall prevention recommendations from their providers. We conducted chart reviews and excluded patients with diagnosis of dementia or low scores on cognitive screening tests (Montreal Cognitive Assessment [MOCA] < 16; Saint Louis University Mental Status [SLUMS] <19.5 no high school education, <21.5 with high school education; Mini-Mental Status Exam [MMSE] <26.5 no high school education, <27.5 with high school education). Details are described elsewhere (in review).
Once participants were consented and randomly assigned to the intervention group, older adults received eight strike monthly MI sessions over 6-months over phone or video call (baseline, 1-week booster session, then monthly for 6 months). The study was approved by Oregon Health and Science University Institutional Review Board (IRB #8993) and registered as Clinical Trial # NCT04612842.
Delivery and Fidelity of Motivational Interviewing Sessions
Five MI specialists with basic or proficient skills of MI provided the MI sessions. These MI specialists have attended an MI workshop or one-to-one MI training prior to joining the study. The proficiency levels of MI skills were identified using Motivational Interviewing Training Integrity (MITI) 4.2.1 coding manual. 14 MI specialists included a mental health counselor, three nurses (two were inducted to Motivational Interviewing Network of Trainers [MINT] during the study), and a nursing student who was a health navigator at a primary care clinic. Overall quality of MI sessions was supervised by the consultant to the study, a MINT member (KNS). The MITI coding scheme was used by individual MI specialists to code individual MI sessions and during the monthly MI specialist meeting for ongoing MI training throughout this project. A random selection of MI sessions was quarterly assessed by four MITI coding experts external to the study who were Motivational Interviewing Network of Trainers (MINT) members who had completed MITI training program.
Description of Motivational Interviewing Sessions
The MI sessions were semi-structured to capture participants’ response to specific open-ended questions for research purposes. For example, the Menu of Options for Fall Prevention, 4 one-page document outlining potential topics for fall prevention (e.g., goals, risks, prevention strategies), was introduced during the first three sessions to engage and guide older adults’ fall prevention conversations. The first session started with the specialist describing the nature of MI sessions and asking “What do you think about the meeting today to talk about fall prevention?” and “What comes to your mind when you hear ‘fall prevention?’” to gauge older adults’ level of engagement with fall prevention. Typically, while the first session was aimed at building rapport and an engaged relationship with the participant, the second session was aimed at identifying the focus of fall prevention behavior change. In later sessions, MI specialists elicited health behavior change using OARS skills to reduce sustain talk and to encourage change talk.
Key Lessons Learned
All MI specialists participated in the monthly MI specialist meeting led by the MINT trainer (KNS) and the principal investigator (HKT) from September 2020 to July 2022. Total of 74 participants had completed at least two MI sessions. Thirty-nine participants had completed all eight MI sessions. Participants were mean age of 80, 32% male, 91.5% White, 92.5% Non-Hispanic, and 76.5% had Medicare insurance. During these meetings, MI specialists exchanged ideas about how to incorporate geriatric fall prevention strategies in 15-30 minute phone or video MI sessions, use Menu of Options for Fall Prevention, how to effectively move participants through four processes of MI, and how to address older adults’ sustain talk about fall prevention, and what worked to facilitate change talk.
Using the meetings notes, and further discussion among the MI specialists, we identified three key lessons to skillfully navigate brief, repeated, phone or video MI sessions about fall prevention with older adults. These lessons were about: how basic MI skills can be used for fall prevention, how an older adult may move through Stages of Change for fall prevention, and how to address strongly held beliefs about fall prevention.
Lesson 1: Application of Basic MI Skills for Fall Prevention
Fall prevention case study using motivational interviewing skills.
Case. Peggy, 75-year-old female, is identified as high fall risk. Balance exercise and use of cane are recommended by her provider to enhance stability. 6 months later, she is back at the clinic, and you (as provider or clinician) have 10 minutes to talk about fall prevention. You observe that she walks slow and use the wall more often to stabilize herself. However, she reports that she does not need to use the cane and does not have a cane with her. What do you think is going through Peggy’s head? How would you respond to the situation?
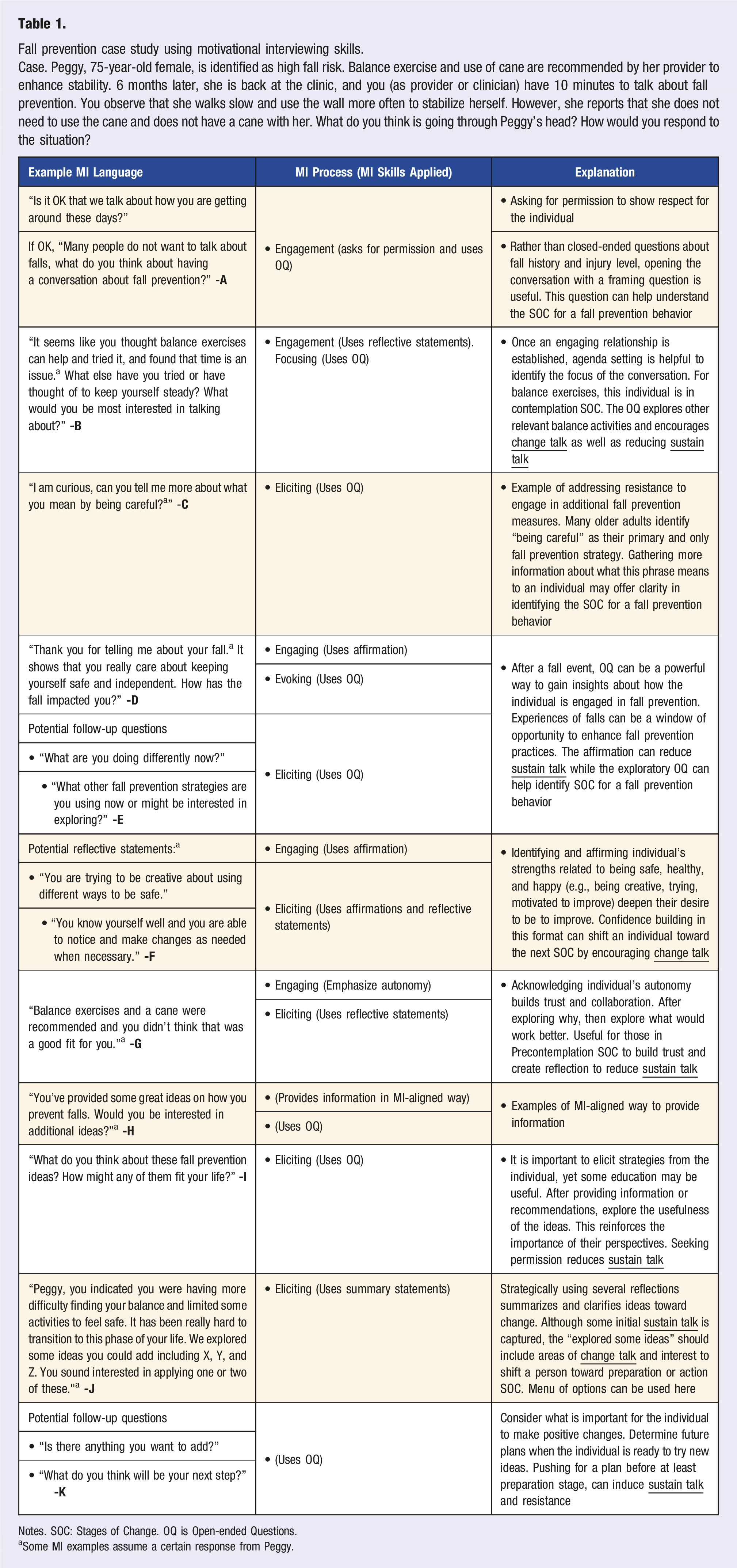
Notes. SOC: Stages of Change. OQ is Open-ended Questions.
aSome MI examples assume a certain response from Peggy.
MI Spirit is demonstrated throughout, and is highlighted by how the request for permission is embedded in the conversation (Table 1-A) and how information is shared about fall prevention (Table 1-H). MI adherent way of information giving includes asking permission to share information and exploring the individual’s thoughts after the information is shared. 6 This approach allows participants to gain knowledge while retaining their autonomy to choose.
Open-Ended Questions.
• Explore the common strategy of “being careful” by asking, “I am curious, can you tell me more about what you mean by being careful?” (Table 1-C) • After a fall event, exploring with “How has the fall impacted you?” or “What are you doing differently now?” can be powerful ways to gain insights about how the individual is engaged in fall prevention. Not all individuals see experiencing a fall as a window of opportunity to enhance fall prevention practices. (Table 1-D) • Explore the usefulness of information or recommendations by asking “What do you think about these fall prevention ideas?” This will reinforce the importance of their perspectives. (Table 1-I) • Open-ended questions aimed to elicit meaning and value were essential to move the conversation forward in 15-30 minute conversations. (Table 1-C, E-J) • The Menu of Options for Fall Prevention can be used for focusing the conversation, finding the goal behavior to explore, or open the discussion possibilities. This tool is useful for covering various risk factors for falls in limited time. Examples include: “We have X, Y, Z options to focus on today, which do you see as the priority?” Or to explore next steps: “There are many options for preventing falls including ___, which do you believe you can work on for now?” (Table 1-J)
Affirmations
Because many older adults believe that they are not at risk for falling or are defensive about fall risk, affirming their abilities and skills to stay independent and capable are critical to gain their trust in early stages of MI sessions. (Table 1-D, F) • Recognizing that older adults “know themselves” or “are intuitive about what works” supports desires to try new strategies.
Reflections
Reflections to capture older adult’s inner thoughts and feelings and to empathize with uncertainty, ambivalence, and grief were crucial. Meaningful reflective statements lead to building engaging relationships in a short amount of time. Reflective statements may also be valuable to demonstrate that you are actively listening when participants cannot see your facial or body expressions over the phone. (Table 1-B, F,G) • Accepting an older adults’ autonomy builds trust and collaboration: “Your doctor recommended you do X, and you didn’t think that was necessary for you.” From here one can explore why or what would work better for the older adult. (Table 1-G)
Summary
Providing balanced or change talk focused summary is an effective way to tie in key elements of the conversation or redirect the conversation to focus on “potential” for change. (Table 1-J)
Lesson 2: Stages of Change Varies for Fall Prevention Topics and Health Behaviors
Examples of fall prevention topics and behaviors and Stages of Change.
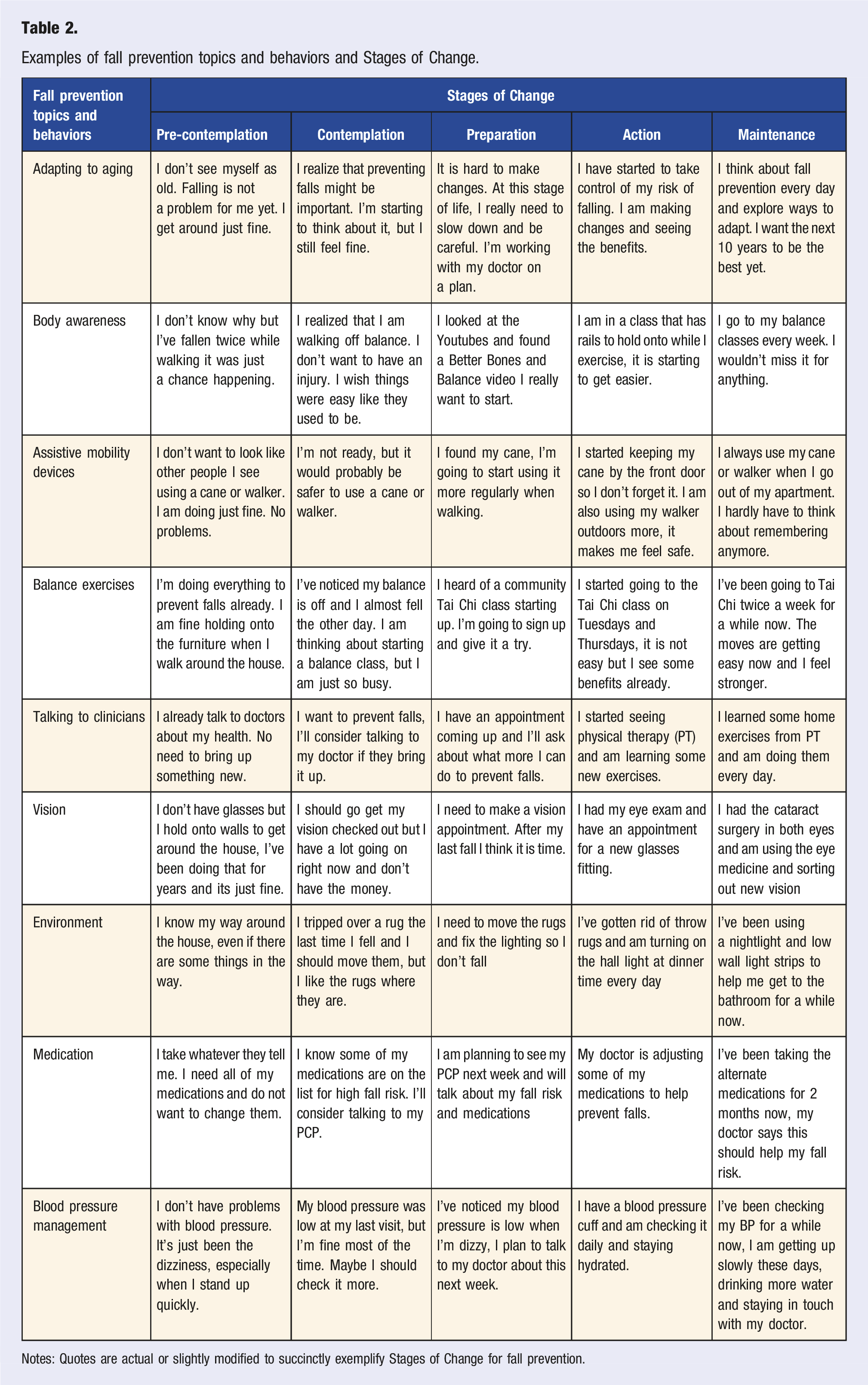
Notes: Quotes are actual or slightly modified to succinctly exemplify Stages of Change for fall prevention.
Lesson 3: MI Spirit is Essential to Find Common Ground
MI specialists found that participants make choices that may not line up with provider recommendations, reflecting their autonomy. Participants had strong opinions about how they prefer to engage with fall prevention. For example, participants have stated “I’m not there yet to use the walker” or “I’ve tried Tai Chi and I don’t like it,” referring to what they had been recommended to do by their provider. In addition, many participants verbalized that “being careful” was sufficient to reduce their chances of falling. Fall prevention recommendations from their providers such as balance exercise, vision checks, and maintaining ideal blood pressure were often mentioned as afterthoughts or not at all when asked about what they are interested in discussing during MI sessions. Clinicians must be well prepared for these opinions that may not align with evidence-based practices. There may even be some emotional response from the clinician to correct the patient if they are deviating from evidence-based practice (e.g., righting reflex 8 ); however, it may not be the right approach for behavior change. An alternative to correcting the patient is to embrace the MI Spirit. Stepping back to realize that this conversation is for the patient helps to tame this reflex. Shifting the focus from correcting to being genuinely curious about participant’s experience may ultimately help identify fall prevention strategies that align with participants’ priority.
Discussion
This manuscript described how we structured and implemented MI sessions to facilitate older adults’ engagement in fall prevention, and to share our learning about MI for fall prevention. We presented examples of how open-ended questions, affirmations, reflections, and summaries helped navigate MI sessions on fall prevention in a short amount of time and by phone or video call. We illustrated how older adults may be at different Stages of Change for a specific fall prevention topic or behavior and that MI Spirit is essential when working with strongly held beliefs.
As we write this manuscript, we understand that conversations about fall prevention may not be a common practice for clinicians. In this context, we would like to offer ideas so that behavior change approaches like MI can be utilized with high fall risk individuals. First, reframing fall prevention as a chronic condition with multiple risk factors can strongly impact the supports that older adults may receive. Physiologic and behavioral fall risks such as loss of balance control and strength, orthostatic hypotension, vision impairment, or tendencies to hurry are developed over time. Once fall prevention is viewed as a chronic health condition, clinicians, public health professionals, healthcare and social systems can approach fall prevention as something that needs lifestyle and behavior change. It takes time and multiple opportunities to reduce each of the fall risks. Lastly, reframing fall prevention as a chronic condition will help encourage a team-based approach for fall prevention, which may include MI-trained personnel in a care manager or community health navigator role.
MI is a learned communication skill ideally suited to address multiple factors to address chronic risks, used within a clinical setting, and can applied by any team member. 15 The topic of focus for MI will differ depending on the clinical role of the individual using MI. It will be most suited for prescribing clinicians and pharmacists to discuss high fall risk medication. Conversely, many fall risks can be addressed by non-licensed personnel to address health promoting activities such as exercise or behavior tendencies. MI can be viewed as a foundational skill to promote behavior change and to have satisfying conversations. 16 We support that all clinicians be equipped with MI skill, starting with small communication changes, and taking another step as described in this manuscript to explore new skills while conversing with older adults to address fall risks. These first-hand experiences, and the immediate results one may receive from patients will encourage the continuation of an MI approach, as many of us in the authorship team have done.
We hope that sharing real-world experiences of organizing and conducting MI sessions would help clinicians to trial and implement aspects of MI in their clinical practice to address fall prevention. Case study examples were provided so that elements of MI can be applied to clinical practice if the whole package of MI seems daunting. Asking open-ended questions to assess older adults’ Stages of Change is a great place to start patient-centered conversations about fall prevention. If resistance is met, which is not uncommon, embrace the MI spirit and explore why. We hope these lessons offer practical MI strategies to move beyond patients’ resistance, and to stimulate older adults’ interest in fall prevention.
Footnotes
Acknowledgments
We deeply thank participants of the study and would like to acknowledge Tiffany Caldwell, M.S.N., R.N. and Yanira Perez, B.S. for their important contribution to the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute of Nursing Research and the National Institutes of Health Office of Directors under Award Number K23NR018672. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
