Abstract
Introduction: Teaching kitchens have emerged as strategies to deliver lifestyle medicine principles and practices. However, a better understanding of their implementation, delivery cost, and potential benefits are needed. This article provides a comprehensive analysis of the costs associated with the development, deployment, and evaluation of the Emory Healthy Kitchen Collaborative (EHKC) teaching kitchen clinical trial.
Methods: The actual number of hours spent and costs incurred to develop and deploy the EHKC teaching kitchen were recorded and broadly categorized into 1 of 4 areas: program development, course delivery, research, and optional enhancements. Costs of each item were assigned as fixed or variable, enabling calculation of the marginal per participant program cost.
Results: Total costs were US$123,898, with 3/4 incurred for program development, research, and optional enhancements. Delivery of the course alone (not including program development costs, research, or any optional enhancements) cost US$30,194. The total cost per participant for the course was US$755, with a marginal participant cost of US$141.
Conclusion: Teaching kitchens represent viable options to deliver lifestyle medicine interventions. However, more research and cost analyses are needed to better understand the value teaching kitchens provide to determine if they are an effective and economical way to deliver lifestyle medicine.
Teaching kitchens represent novel ways to deliver lifestyle medicine principles, and understanding the cost associated with delivering teaching kitchens is needed to gain further adoption.
Introduction
The United States (US) spent US$3.8 trillion on healthcare in 2019, 90% of which was spent on chronic and mental health conditions.1,2 The majority of healthcare expenditures are accounted for through employment, as employers provide insurance for 55% of the US population. 3 Thus, in 2016, 46% of all employers offered workplace health promotion (WHP) programs. 4 In a 2010 meta-analysis, these programs were shown to decrease medical costs by US$3.27 for every dollar spent and reduce absenteeism costs by US$2.73 per dollar spent. 5
In addition to cost savings, programs focusing on lifestyle medicine principles such as the Complete Health Improvement Project (CHIP) have been shown to reduce the risk of cardiovascular disease, treat type 2 diabetes mellitus, reduce body weight, and improve depression scores.6-9 Intensive lifestyle programs like the Diabetes Prevention Program (DPP) have demonstrated superior outcomes with lifestyle intervention as compared to medication in preventing progression from pre-diabetes to diabetes. 10 More recently, teaching kitchens have been studied as a WHP intervention. A feasibility pilot study of 40 participants over 14-16 weeks revealed significant decreases in body weight (−2.8 kg), systolic and diastolic blood pressure (−7.7 and −6.3 mmHg, respectively), and total cholesterol (−7.5 mg/dL) post-program. 11
The Emory Healthy Kitchen Collaborative (EHKC) sought to build on the preliminary teaching kitchen research by conducting a year-long teaching kitchen clinical trial. The clinical trial design and rationale of the EHKC have been described previously. 12 Briefly, this was a 12-month program (August 2019–September 2020) that included a 10-week course comprising 5 4-hour classes held every other Saturday. It combined didactic and experiential material. The course curriculum was specifically developed and led by Emory University faculty and staff in the disciplines of nutrition, culinary skills, yoga, physical activity, stress resilience, mindfulness-based eating, and ethnobotany. This course was followed by continued access to weekly yoga classes, the Full Plate Living online platform, health coaches (for an additional fee), and periodic check-ins. Forty benefits-eligible employees were recruited to participate in the program, with preference given to those with comorbidities and high levels of motivation to adopt healthier lifestyles. Physical and mental health data were collected using biometrics and survey instruments at baseline, 3 months, 6 months, and 12 months.
As with other WHP programs, one of the main barriers to the implementation of this program and other teaching kitchens was cost.11,13 As noted by Eisenberg et al, culinary instruction, food cost, utensils, and proper kitchen facilities have raised concerns about the feasibility of these programs. 11 However, given the potential economic savings and health improvements documented from other WHP, exploring the upfront cost of teaching kitchens is warranted. The purpose of this article is to provide a comprehensive analysis of the costs associated with the development and deployment of the EHKC teaching kitchen clinical trial.
Methods
An initial budget was drafted in 2018 as part of a grant proposal. This document was subsequently adjusted to reflect the actual number of hours worked and the cost of various aspects of the program post-hoc. Costs were then broadly categorized into 1 of 4 areas: program development, course delivery, research, and optional enhancements.
Program development costs were considered necessary expenditures to create the program from scratch and would not need to be incurred for future offerings. Course delivery costs were specific to delivering the actual course. These items represent expenses needed to offer this program again. The research category included costs for activities pertaining to conducting the clinical trial and would not typically be part of future offerings. Optional enhancements included discretionary costs that were not critical to the deployment of the program, though they provided additional benefits to participants or the program.
Recognizing that the cost of some items spanned multiple categories (i.e., personnel), actual costs were attributed based on the relative contribution to each category. In the case of personnel, actual hours were used when available. If a detailed hour summary was not available, the percentage of the cost was agreed upon via discussion by the co-authors (i.e., 80% of the content expert’s costs were attributed to the development of their material and 20% was allocated to the delivery). Personnel costs were calculated as a percentage of annual salary and fringe benefits based on the time commitment to the program.
Additionally, costs were denoted as fixed or variable and calculated for 40 participants. While adding participants would not impact fixed costs, substantial changes to this number (i.e., 10 participants or 80 participants) would necessitate a “scaling” effect to cover the cost of a more appropriately sized space, or dramatically different amounts of food for the group meals during the sessions.
The variable costs would change with adding or subtracting an individual participant. In situations where variable costs were related to adding additional personnel (i.e., adding another facilitator), the variable cost for 1 participant was estimated based on a specified number of additional participants to collectively cover the total cost of hiring the additional staff person. The marginal cost of adding 1 participant was calculated by summing the variable costs. Costs were aggregated and combined as appropriate using Microsoft Excel (2018).
Results
Itemized Costs of the Emory Healthy Kitchen Collaborative Teaching Kitchen by Category.
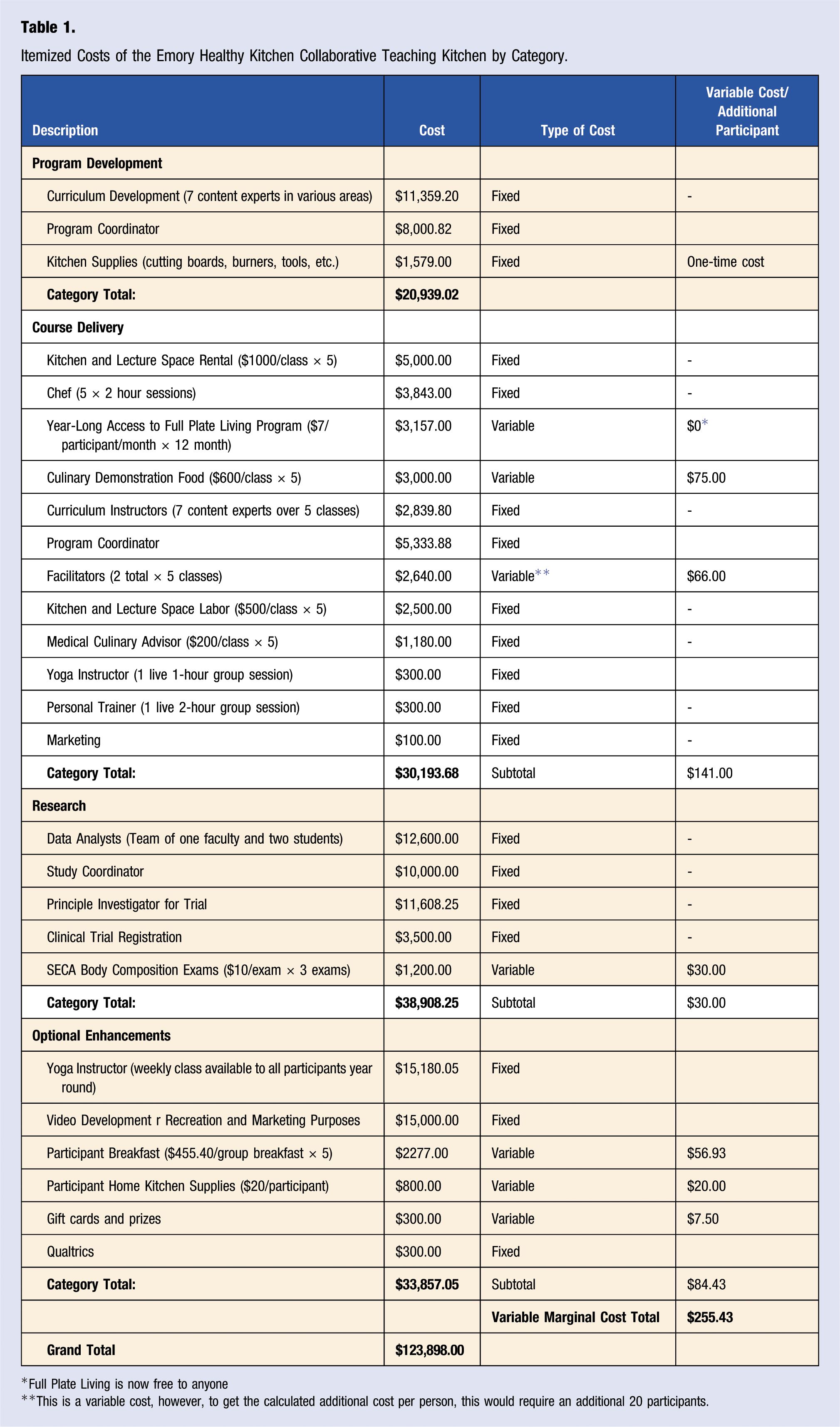
Full Plate Living is now free to anyone
This is a variable cost, however, to get the calculated additional cost per person, this would require an additional 20 participants.
Individual Participant Costs.
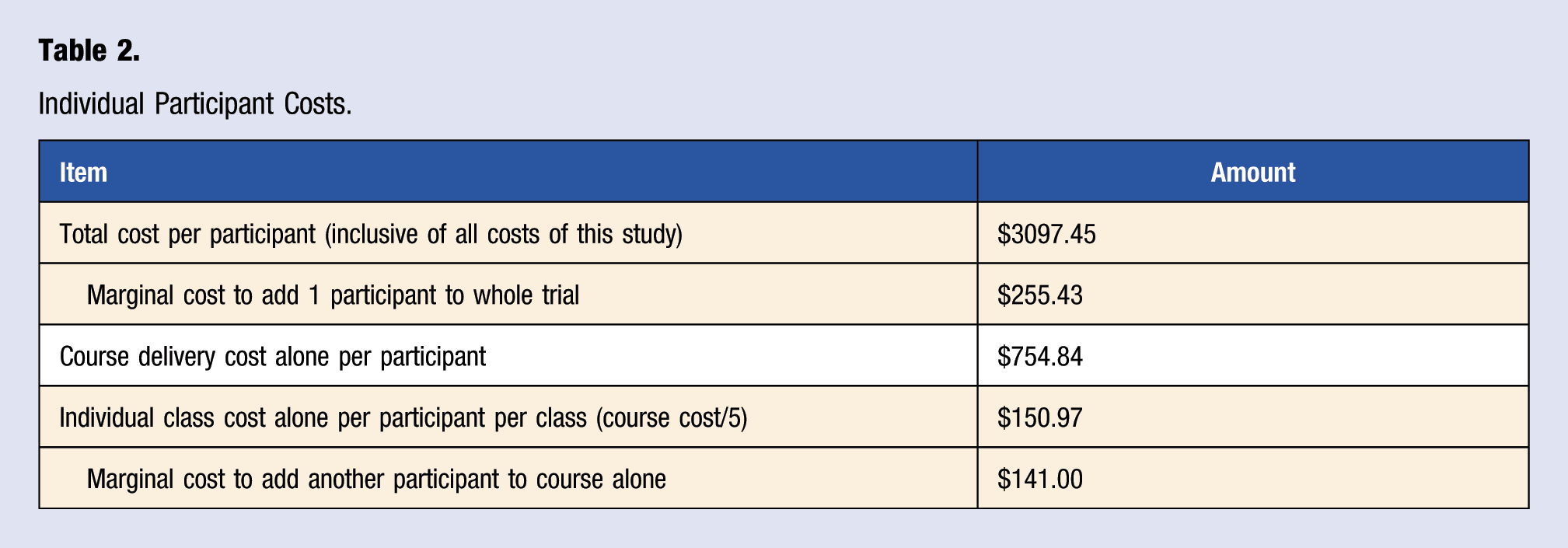
The total cost per participant for the 10-week course alone (not including program development costs, research, or any of the optional enhancements) was US$755. Dividing this by 5 for each of the classes yielded an average participant cost of US$151 for each 4-hour class. The marginal cost of adding 1 additional participant to the 10-week course alone was US$141.
Number of Hours Spent Before, During, and After the 10-Week Course to Develop the Program, Deliver the Course, Conduct Research, and Provide Optional Enhancements.
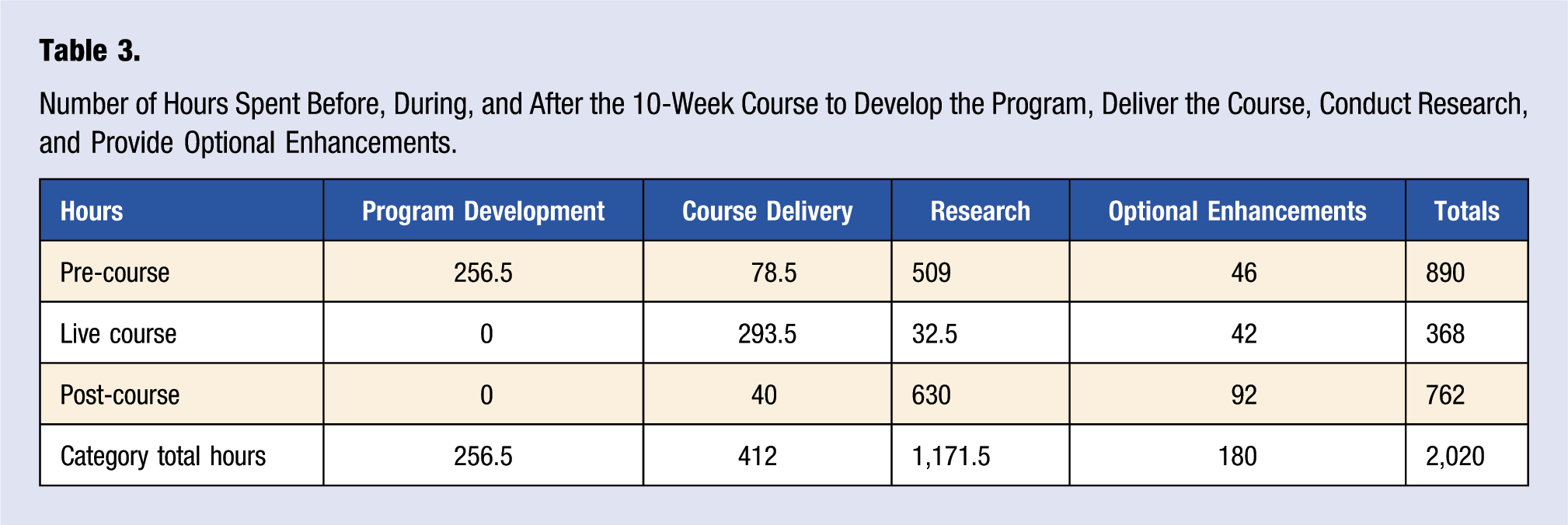
Discussion
Our detailed cost analysis offers valuable insight into the actual costs required to develop and deploy a comprehensive WHP program. While the overall cost of the entire clinical trial was US$123,898, more than half of the clinical trial budget funded the research portion and optional enhancements. Development costs made up the smallest portion. These 3 categories collectively made up nearly 3/4 of the total cost and could theoretically be markedly reduced when offering this program again using the same curriculum.
Importantly, the cost to deliver the actual teaching kitchen course was much more affordable. The per-participant cost of US$755 included the 10-week comprehensive course, access to the Full Plate Living platform over the year, and periodic check-ins. Interestingly, much of this US$755 went toward covering fixed costs, as the marginal cost of adding 1 additional participant to the 40-participant course was only US$141. This suggests that expanding and scaling this type of intervention would be beneficial in reducing costs and increasing access to the course.
For context, the non-research cost of the 3-year DPP trial was an additional US$2,780 per participant for the intensive lifestyle intervention group and US$2,542 per participant for the medication group. Compared to the control group, the DPP lifestyle intervention and metformin groups reduced the risk of developing diabetes by 58% and 31%, respectively. Staff time comprised 45%-55% of the direct medical cost of the DPP intervention. 14
Another study investigated the total cost of monthly outreach motivational interviewing over a year for smoking cessation and relapse prevention among 156 low-income pregnant women. Delivering this program cost US$312.00 per participant in comparison to US$4.82 when usual care was involved. The main cost components were intervention delivery, travel time, scheduling, and training. 15 The motivational interviewing intervention was found to be cost saving in preventing smoking relapses but provided no additional benefit beyond usual care for smoking cessation. 16
These examples suggest that health promotion program costs seem to correlate with the duration, intensity, and the health outcomes of the studies. They suggest that the costs associated with the EHKC clinical trial and program deployment are reasonable. Personnel costs are consistently the largest driver of cost, and similar to the DPP trial, 14 65% of our costs went toward personnel. The higher cost of the DPP trial is accounted for by the 3-year trial duration and more intensive lifestyle intervention, as well as their impressive reduction in the risk of developing diabetes. The lower cost of the motivational interviewing study reflects a less intensive intervention overall, involving only a monthly phone call to participants, as well as lower rates of smoking cessation. This suggests more comprehensive interventions may lead to better health outcomes. As the results become available from our clinical trial, further cost-benefit analysis will be possible to determine its true value.
A large part of the advancement of the field of lifestyle medicine is contingent on financially viable strategies to implement these principles into practice. As teaching kitchens grow in popularity, a better understanding of their cost and benefit is crucial to their advancement. We feel that the reported costs associated with delivering this program are reasonable, though could also be adapted to less resource-intensive settings as well. For example, if a suitable space could be borrowed or rented for a lower cost than the US$5000 allocated in our study, this would reduce the overall course delivery cost by nearly 17%. The challenge with any cost reductions is retaining the integrity and effectiveness of the program. We hope our itemized costs will serve as a guide to help future teaching kitchen programs forecast costs and budget appropriately.
Limitations
This financial analysis is specific to the EHKC and would vary if the program were recreated at another institution. Factors influencing costs include institutional policies, procedures, and resources available. While we attempted to provide an accurate assessment of the number of hours worked and the exact allocation of funds, there are inevitably some inaccurate attributions. Some personnel hours were likely underreported, and if exact costs were not available, the grant allocation estimates were used.
While we provided marginal cost estimates per participant, this assumed a 40-participant program. A significantly smaller program would change some of the estimates due to the relatively higher fixed costs. Conversely, greatly expanding the program would allow for some savings related to scale. The other challenge with estimating marginal costs of individual participants is that some costs require lump-sum payments. For example, to maintain the same facilitator-to-participant ratio, adding or subtracting a handful of participants would require paying the entire salary of another facilitator. For our estimates, we split this salary expense across an assumed additional 20 participants, as this would maintain the 20:1 participant-to-facilitator ratio. Depending on the ratios of faculty to participants programs wish to maintain, these costs could be higher or lower.
One of the challenges in comparing this study to other lifestyle intervention programs is the significant variability in the content, structure, frequency, and delivery of programs. Moving toward more consistent programming options would allow for the aggregation and comparison of data from disparate teaching kitchen interventions.
Conclusion
Teaching kitchens represent novel ways to deliver lifestyle medicine principles. Understanding the cost associated with delivering teaching kitchens is needed to gain further adoption. The cost to deliver the EHKC course was US$755 per participant. More research, course offerings, and cost analyses are needed to refine this estimate, better understand the value teaching kitchens provide, and determine if they are an economical and efficient way to deliver lifestyle medicine.
Footnotes
Acknowledgments
We would like to acknowledge the Ardmore Institute of Health who provided grant funding and support for the EHKC teaching kitchen clinical trial, as well as the in-kind support from Emory University, the Seavey Clinic, and the faculty and staff who contributed to this program.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Grant funding to conduct this clinical trial was provided by the Ardmore Institute of Health.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
