Abstract
Objective:
Chronic Pancreatitis (CP) is a multifactorial disease. It was characterized by severe inflammation and acinar cell destruction. Thus, the present study was initiated to evaluating the ability of bone marrow-based mesenchymal stem cell (MSCs) combined with Icariin to restore and regenerate acinar cells in the pancreas of rats suffering chronic pancreatitis.
Methods:
Chronic pancreatitis was induced in rats via both L-arginine plus radiation, repeated L-arginine injection (2.5g/Kg body-weight, 1, 4,7,10,13,16,19 days), then, on day 21, rats were exposed to a single dose of gamma-radiation (6 Gy), which exacerbate injury of pancreatic acinar cells. One day after irradiation, rats were treated with either MSCs (1 × 107 /rat, once, tail vein injection) labeled PKH26 fluorescent linker dye and/or Icariin (100 mg/Kg, daily, orally) for 8 weeks.
Results:
Icariin promotes MSCs proliferation boosting its productivity in vitro. MSCs, and/or icariin treatments has regulated molecular factors TGF-β/PDGF and promoted the regeneration of pancreatic tissues by releasing PDX-1 and MafA involved in the recruitment of stem/progenitor cell in the tissue, and confirmed by histopathological examination. Moreover, a significant decrease in IL-8 and TNF-α cytokines with significant amelioration of myeloperoxidase activity were noted. As well as, reduction in MCP-1 and collagen type-1 levels along with Hedgehog signaling down-regulating expression in such cells, Patched-1, Smoothened, and GLi-1.
Conclusion:
The potent bioactive therapeutic Icariin combined with MSCs induces a significantly greater improvement, compared to each therapy alone.
Introduction
Chronic pancreatitis (CP) is an inflammatory, progressive disease of the pancreas which leads to the progressive destruction of the pancreatic acinar cells. This leads on to the development of pancreatic fibrosis, characterized by changes in the pancreatic morphology, gland destruction and eventually loss of exocrine and endocrine functions. 1,2 One of the accepted theories is that chronic pancreatitis results from oxidative stress and repeated episodes of acute pancreatitis (AP). CP may also develop complications, such as chronic abdominal pain syndrome, metabolic bone disease and pancreatic cancer. 3
The impact of ionizing radiation (IR) on human health is becoming a concern. A wide variety of peoples and societies; particularly workers in the radiation sector and the nuclear industry, patients undergoing routine diagnostic and/or radiotherapy procedures and medical personnel are exposed to certain doses of gamma radiation. 4 Besides, nuclear and radiological accidents represent a threat to all living organisms around the world. Ionizing radiation induces tissues damage through amplified endogenous signaling and culmination of reactive oxygen species (ROS) and nitrous oxide in a coordinate series of molecular events that are damaging many cellular macromolecules such as DNA, lipids and proteins. 5 Also, ionizing radiation alters the number and function of immune system cells like increasing macrophages and lymphocytes-T secretion that stimulates several inflammatory factors such as NF-κB and SMAD2/3, as well as cytokines, for example, interleukin’s (IL-1, 2, 6, 8, and 33), tumor necrosis factor-alpha (TNF-α), interferon-gamma (IFN-α), transforming growth factor-β1(TGF-β) and platelet-derived growth factor (PDGF). 5
Throughout recent years, mesenchymal stem cells (MSCs) have played an effective role all over inflammatory damage, regeneration and healing. 6 The stem cell therapy serves as a possibility for the recovery and regeneration of the damaged tissues. It was found in previous studies, that infused MSCs could effectively relieve injury of pancreatic acinar cells and small intestinal epithelium, promote the proliferation of enteric epithelium, repair of the mucosa and attenuate systemic inflammation in rat chronic pancreatic model. 7 Many studies confirmed that recovery of the pancreatic β-cells and regulation of the blood glucose level in cases of diabetes could be achieved by transplantation of MSCs. 8,9
Despite the large interest on acute pancreatitis, only a few studies have explored the therapeutic potential of MSCs on chronic pancreatitis in which the persistence of inflammation and its molecular consequences lead to the formation of large fibrotic area due to the transition of pancreatic stellate cells from a round shape to a fibroblast-like morphology. The development of a fibrosis rather than glandular parenchyma affects and restricts the pancreatic functions. 10
Icariin (IC), a traditional Chinese medicine that possesses major bioactive therapeutic properties, is extracted from potent Horny Goat Weed (Ying Yang Huo). 11 Early in vivo and in vitro studies have shown that, icariin acts as a natural anti-inflammatory drug which targets pro-inflammatory cytokines TNF-α and IL-6, and inflammatory mediators. 12 -14 Moreover, icariin activates the phosphoinositide 3-kinase (PI3 K)/protein kinase B (AKT) signaling pathway to ameliorate lipopolysaccharide (LPS)-induced acute inflammatory responses. 15 Icariin was found to have many neuroprotective effects such as, improving the survival and functioning of neurons as well as triggering their self-renewal through neural stem cells. 16 Mesenchymal stem cells’ potential therapeutic role in CP has attracted great attention but the underlying mechanisms remain unknown. Therefore, this work aims to study the possible role of Icariin and mesenchymal stem cells (MSCs) treatment in pancreatic injury. The evaluation includes molecular, biochemical analysis and histopathological examination.
Material and Methods
Reagents
Icariin purity 98%, L-Arginine and PKH26 used in this study were purchased from Sigma–Aldrich® (St. Louis, Missouri, USA).
Collection and Culture of Bone Marrow-Derived Mesenchymal Stem Cells (MSCs)
Using Caplan’s process, bone marrow was flushed out of the femurs and tibiae of 6 weeks old male albino rats and were isolated and cultured in vitro. 17
In Vitro Study
MTT cell proliferation assay
Cell proliferation of MSCs incubated with Icariin compared with MSCs was determined using the MTT (3-[4,5-dimethyl thiazol-2-yl]-2.5-diphenyl tetrazolium bromide) cell proliferation kit (Trévien Inc., Gaithersburg, MD, USA) as per manufacturer’s protocol. Cells were placed in tissue culture plates about 3000 cells/well in a final volume of 100 µL of medium and allowed to attach for the 24 h of the experimental duration. The MTT reagent was added (10 µL per well) and the plate incubated for 2 h to allow for an intracellular reduction of the soluble yellow MTT to the insoluble purple formazan dye, each sample was put in a microplate reader at 570 nm. The extent of cell proliferation was assessed by comparing the percentage of cell proliferation in case of the treated cells (MSCs +IC) to the untreated cells (MSCs).
Phonotypical characterization with flow cytometry of BM-MSCs
Surface CD markers monoclonal rat anti-antibodies CD34 FITC, CD105 PE, CD29 and CD90 APC (Cat # 11-0341-81, # 12-1051-82, # 17-0291-82, and # 17-0900-82), from BioScience™, Thermo Fisher Scientific Inc, USA. Antibodies used for the identification in the fourth stage, by using Flow Cell Cytometer analysis (CYTOMICS FC 500, Beckman colter, FL, USA) and measured by CXP version 2.2 Software. 18
Induction of Chronic Pancreatitis
Methods
Chronic pancreatitis was induced in rats by repeated L-arginine injection hydrochloride (250 mg/100 gm. wt. /1, 4,7,10,13,16,19 days day) in normal saline, 19 then, on day 21, rats were exposed to a single dose of gamma-radiation (6 Gy).
Irradiation Procedure
Rat’s whole body irradiation was performed in Cesium
Animals and Experimental Protocol
Thirty-six of 6 weeks old young male albino rats, of an average weight of 170-200 gm were maintained in an air-conditioned animal house with specific pathogen-free conditions and subjected to a 12:12-h daylight/darkness and allowed unlimited access to chow and water. All the ethical protocols for animal treatment followed by the National Institutes of Health guide for the care and use of Laboratory animals (NIH Publications No. 8023, revised 1978) were followed and supervised by the animal facilities, National Center for Radiation Research and Technology, Atomic Energy Authority.
Rats of the present study were divided into 6 equal groups (6 rats/group) as follows:
At the end of the experiment, rats were anesthetized with ether and then euthanized. Pancreas was directly separated and weighed then a known mass of the pancreas tissue was homogenized in a suitable buffer solution using a homogenizer, then the cell debris was removed by centrifugation at 1589.796 g for 10 min, the supernatant was used for the estimation of the molecular, and biochemical analysis. Other dissection samples taken from the pancreas were fixed in 10% formalin for histopathological examination.
Biochemical Assay
Analysis of lipase and amylase
Serum lipase and amylase activities were evaluated with a spectrophotometric technique, performed according to a previously described method. 21
Determination of cytokines pro-inflammatory
In pancreatic tissues, tumor necrosis factor-alpha (TNF-α) was estimated using ELISA kit (Abcam, Cambridge, MA, USA), monocyte chemoattractant protein-1 (MCP-1) and myeloperoxidase (MPO) enzymatic activity were measured by ELISA kit (R&D Systems, Minneapolis, MN) according to manufacturer’s description. In the serum, interleukine-8 (IL-8), transforming growth factor-β1 (TGF-β1), platelet-derived growth factor (PDGF), were measured using ELISA kit (R&D Systems, Minneapolis, MN) according to manufacturer’s description. Samples were evaluated using the ELISA plate reader (Biotek, USA).
Real-time quantitative polymerase chain reaction determination of the gene expression of PDX-1, MafA, and Collagen-1
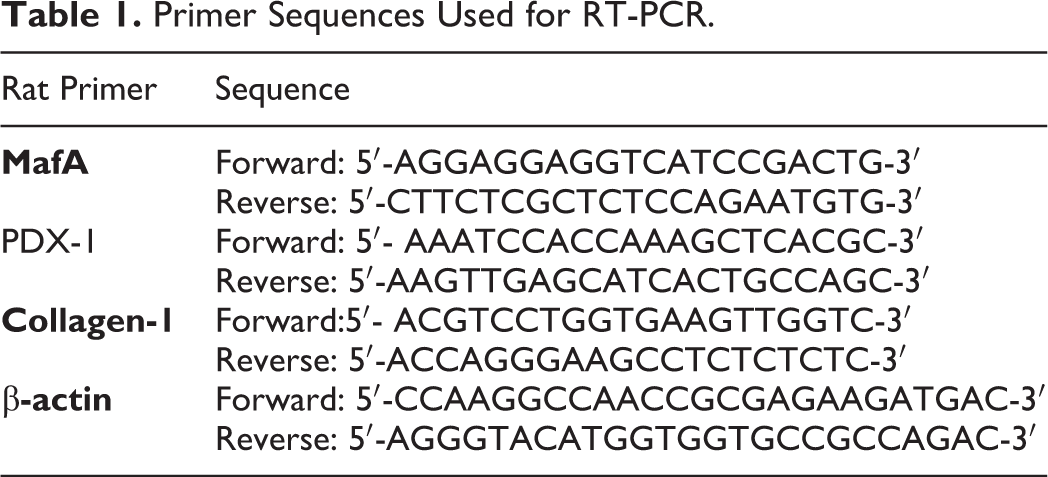
Real-time, quantitative RT-PCR was performed, 22 using the StepOne Real-Time PCR System Instrument (Life Technologies) with the QuantiTectTMSYBR Green PCR Kit (Qiagen, Valencia, CA). The whole RNA was isolated from rat exocrine pancreas using the TRIzol reagent (Invitrogen Ltd., Carlsbad, CA) to process the RNA extraction. Data analysis was performed using the ABI Prism sequence detection system software and quantified using the v1 Sequence Detection Software from PE Biosystems (Foster City, CA). The relative expression of the studied gene was calculated using the comparative threshold cycle method. The Primer sequences are shown in Table 1.
Primer Sequences Used for RT-PCR.

Western blot analysis to identify the PTCH-1, SMO, and (GLi-1) protein expression
A piece of the pancreas tissue was homogenized with RIPA buffer, and then centrifuged at 23182 g for 20 min at 4°C. The concentration of protein was determined with a (BCA) protein assay kit (Thermo Fisher Scientific Inc., USA), each sample was overloaded with sodium dodecyl sulfate-polyacrylamide gel electrophoresis (PAGE) 8% and moved to membrane nitrocellulose (Amersham Bioscience, Piscataway, NJ, USA) by a semi-dry transfer apparatus (Bio-Rad, Hercules, CA, USA). The membranes were incubated with 5% milk blocking buffer, washed with TBST and incubated with a 1:100 dilution of anti- Ptch-1(patched), anti- SMO (smoothened) and anti-GLi-1 (glioma-associated oncogene) (Thermo Fisher Scientific Inc., USA) overnight on a shaker roller at 4°C. The filters were washed and subsequently probed with horseradish peroxidase-conjugated goat anti-mouse immunoglobulin (Amersham Life Science Inc., USA). Chemiluminescence detection was performed using the Amersham detection kit, according to the manufacturer’s protocols and exposed to X-ray film. Protein levels were quantified by densitometric analysis of the auto-radiograms using a scanning laser densitometer (Biomed Instruments). Results were determined after normalization of β-actin protein expression as the housekeeping protein
Homing of stem cells detection
A fluorescent microscope (Olympus BX50F4, no. 7M03285, Tokyo, Japan) was used to identify and trace the cells stained with PKH26 in the pancreas.
Histopathological examinations
Pancreas tissue specimens were fixed in 10% neutral buffered formalin, trimmed, washed and dehydrated in ascending grades of alcohol, cleared in xylene, embedded in paraffin, sectioned at the 4-6 µm thickness and stained with hematoxylin and eosin. 24
Statistical analysis
Statistical analysis and tests of significance was performed using the statistical package SPSS (Statistical Program for Social Science) version 15.0 by applying a 1-way ANOVA test followed by a post hoc test (LSD) for multiple comparisons. All data are expressed as a mean of 6 values; SE and difference between means were considered significant at P < 0.05.
Results
Engraftment of MSCs Morphology
The MSCs were extracted, isolated and cultured from six-week-old male rats. On day 14, undifferentiated BM-MSCs reached 70–80% confluence. MSCs as shown in Figure 1A-D, were identified by their adhesiveness and fusiform shape which exhibited a similar heterogeneous fibroblast (long spindle) morphology.
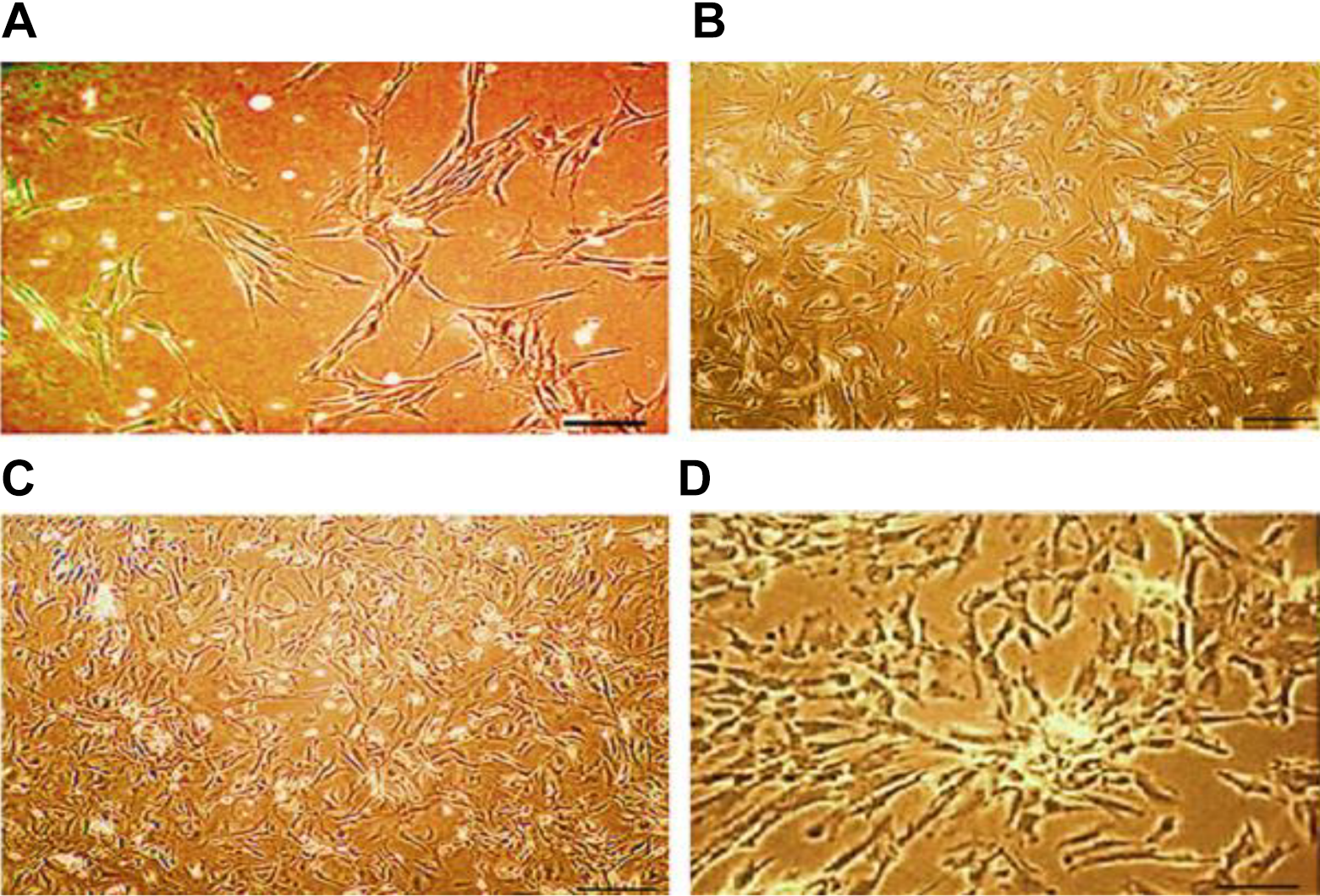
The morphological fibroblast-like appearance of MSCs. Isolation and culture first day (A), cultured (MSCs) derived from rats morphologically defined by a fibroblast-like appearance at passage 1, 3, and 5 days respectively (B-D) and MSCs with plate adherence and fibroblast-like morphology (spindle shape) (scale bar: 100 μm)
Homing of MSCs
Groups of Control, AP, CP and CP+IC sections revealed the lack of PKH26 labeled stem cells (Figure 2A-D). Sections of the CP+MSCs (Figure 2E) and CP+MSCs+IC treated groups (Figure 2F) indicates the existence of PKH26 labeled stem cells in the islets of Langerhans and some pancreatic acini.

Photomicrographs of sections in the pancreas of albino rats. (A) The fluorescent microscopic image of a rat pancreas from the control group shows a negative immune fluorescent reaction 1 islet (blue arrow) surrounded by many pancreatic acini, (B) L-Arg (AP) group (C) CP group (D) CP+IC group no fluorescent visible as the control groups. (E) Some immunofluorescent PKH-26-labeled MSCs (white arrows) in the pancreas of the CP+MSCs group. (F) Numerous PKH-26-labeled MSCs (white arrows) and some pancreatic acini (yellow arrows) in the pancreas of the CP+ MSCs+ IC group (Fluorescent microscope image, X 200).
Assessment of the Role of Icariin in MSCs Proliferation
As shown in Figure 3, the MTT assay revealed that Icariin significantly increased the proliferation of MSCs as compared with the untreated control group.

MTT proliferation assay in the MSCs treated with Icariin group (MSCs+IC) compared to (MSCs) the control group: *P < 0.05 compared to the control group.
MSCs Characterization by Flow Cytometer
The expression of cell surface markers of MSCs were evaluated by flow cytometry. As shown in Figure 4, the MSCs weakly expressed CD34 (≤4%), which is a specific cell surface markers of hematopoietic stem cells. However, MSCs cells strongly expressed CD90, CD29CD105 and (≥ 90%), which are specific cell surface markers of MSCs.

The expression of surface MSC specific markers characterization. The surface MSCs specific markers including CD90, CD29, and CD105 were positive in isolated cells but negative for CD34, which is a hematopoietic stem cell marker. The red area represents isotype control IgG expression, while the black line depicts the marker expression.
Effect of Bone Marrow Derived Mesenchymal Stem Cell (MSCc) and/or Icariin (IC) on Serum Lipase and Amylase Activities
To investigate the effect of MSCc and/or Icariin on pancreatic dysfunction, the activity of lipase and amylase was measured in the serum of all the studied groups. As shown in Table 2, acute pancreatitis (AP group) resulted in pancreatic injury manifested by a significant increase in serum lipase and amylase activities compared to control groups. The exposure of AP rats to gamma radiation (CP group) has intensified the increase of both enzymes, which was significantly attenuated by MSCs, IC and MSCs +IC treatments.
Effect of Mesenchymal Stem Cells (MSCs) and/or Icariin on Serum Lipase and Amylase Activities.

Each value represents the mean of 6 records ± S.E. The values with different superscripts in the same row are significantly different at P ≤ 0.05.
Effect of Bone Marrow Derived Mesenchymal Stem Cell (MSCc) and/or Icariin (IC) on the Inflammatory Markers
The results presented in Table 3 show that the exposure of rats to L-arginine induced a significant increase in the level of serum IL-8 and pancreatic TNF-α compared with their respective values in the control group. The increase was more severe when AP rats were exposed to radiation (CP group). Meanwhile, treatment with MSCs and/or Icariin displayed a reduction in the proinflammatory markers, and serum IL-8 & pancreas tissue TNF-α reached nearly their normal levels in case of MSCs combined with IC (CP+ MSCs+ IC group).
Effect of MSCs and/or IC on Inflammatory Mediators and Profibrotic Markers.

Each value represents the mean of 6 records ± S.E. The values with different superscripts in the same row are significantly different at P ≤ 0.05.
Effect of Bone Marrow Derived Mesenchymal Stem Cell (MSCc) and/or Icariin (IC) on Profibrotic Markers
The results presented in Table 3 show that the highest increase in serum TGF-ß1 & PDGF was recorded in the CP pancreatitis model exposed to radiation (CP group). MSCs and/or Icariin treatment has significantly attenuated this elevation. PDGF nearly reached the control value. In addition, the highest increase in the tissue level of monocyte chemoattractant protein 1 (MCP-1), which is a vital chemokine in the pathogenesis of pancreatitis, and MPO activity is recorded in CP group. A significant amelioration was recorded by MSCs and/or IC treatment with the best results obtained by the combined treatment (CP+MSCs+IC group) and MCP-1 levels reached the control value.
Effect of Bone Marrow Derived Mesenchymal Stem Cell (MSCc) and/or Icariin (IC) on the Gene Expressions of PDX-1, MafA and Collagen-1 in Pancreatic Tissue
The transcriptional factors, PDX1, and MafA share key functions as beta-cell specific regulators. To identify which transcriptional regulator(s) contribute to stem cell and/or Icariin regeneration of pancreas injury, we monitored the gene expression levels of PDX1, and MafA in pancreatic tissue. PDX1, and MafA mRNA levels were decreased significantly in AP and CP groups compared to the corresponding normal control Figure 5) with a more decline in the CP group when compared to the AP group. The effects of MSCs and/or Icariin treatment on the regeneration in primary islets was identified by the increase in the transcriptional factors, PDX1, and MafA. Transplanted (1×107) stem cells or treatment with icariin induced both basal levels of PDX1, and MafA (Figure 5A and B). The highest increase was reached by MSCs+ IC treatment. Also, as shown in Figure 5C, the mRNA levels of collagen-1 in pancreatic tissue were up-regulated by L-arginine treatment, but the group subjected to both L-arginine and 6 Gy γ-rays strikingly accumulated collagen-1 mRNA levels, meanwhile treatment with Icariin and/or stem cells down-regulated the expression level of collagen-1 mRNA with the best results obtained by the combined treatment.
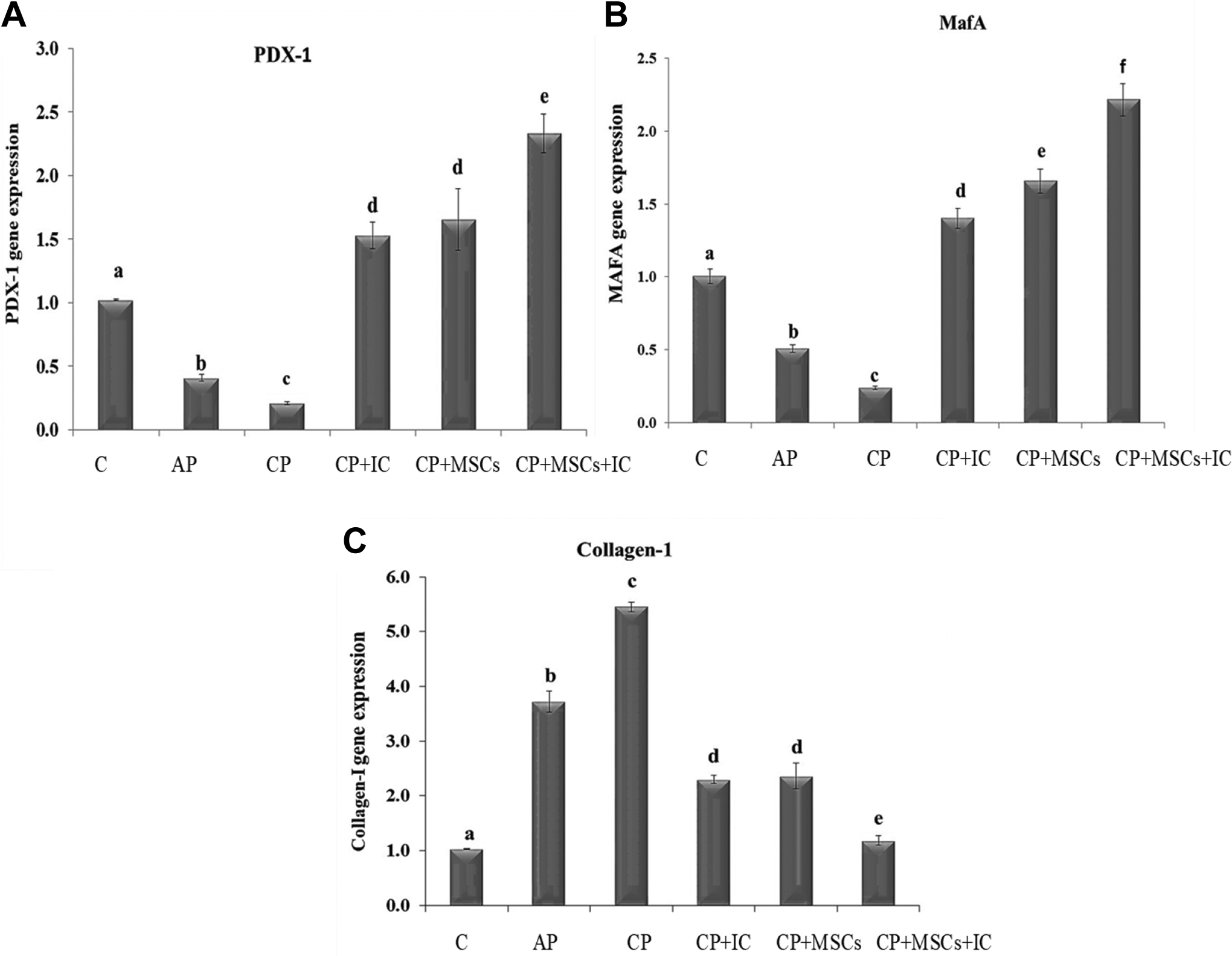
Effect of MSCs and/or Icariin on gene expressions fold change of PDX-1 mRNA, MafA mRNA C AP CP CP+IC CP+MSCs CP+MSCs+IC C AP CP CP+IC CP+MSCs CP+MSCs+IC C AP CP CP+IC CP+MSCs CP+MSCs+IC MSCs and/or Icariin on gene expressions fold change of PDX-1 mRNA, MafA mRNA and collagen-1mRNA. Each value represents the mean of 6 values ± SE. The values with different superscripts are significantly different at P ≤ 0.05.
Effect of Bone Marrow Derived Mesenchymal Stem Cell (MSCc) and/or Icariin (IC) on the Protein Expression of PTCH-1, SMO, and GLi-1 in Pancreatic Tissue
The effect of MSCs and/or IC on the expression of pivotal Hh signaling molecules, including PTCH-1, SMO, and Gli-1 was assessed by western blot. We found that in AP and CP groups the expression pattern of pivotal Hh signaling molecules was upregulated, which was significantly more intense in the CP group (Figure 6A-C). Conversely, treatment with MSCs, Icariin, and their combination has significantly regulated the PTCH-1, SMO and GLi-1 pancreatic protein expression.

Western Blot analysis of signaling growth factors: A) PTCH-1, B) SMO, and C) GLi-1 protein expressions, and PAGE of PTCH-1, SMO, and GLi-1 protein expression normalized to β-actin of pancreas tissues. Each value represents the mean of 6 values ± SE. The values with different superscripts are significantly different at P ≤ 0.05.
Histological Results
Sections of the normal control group showed the normal architecture of the pancreas. The pancreatic tissues revealed the normal histological structure of both exocrine and endocrine tissues. The pancreatic lobules were of different sizes and shapes. The islets of Langerhan’s showed a normal arrangement of cellular constituent and the acinar structure revealed normal proteineous eosinophilic materials. The islets appeared lightly stained than the surrounding acinar cells. The acinar cells consisted of pyramidal cells with basal nuclei and apical acidophilic cytoplasm. The exocrine component forms of pancreas were closely packed by acinar cells and arranged into small lobules. Pancreatic lobules were separated by intact intra-lobular and interlobular connective tissue septa (Figure 7A

Pancreatic tissue section showing (A) Control group: normal histological structure of both exocrine and endocrine tissues, (B, C) AP group: apoptosis of Langerhan’s cells, loss of lobular architecture with vacuolation of acinar cells, (D, E) CP group: loss of some Langerhan’s cells and vacuolation of acinar cells (F) CP+MSCs group: Some acinar cells showing deeply stained pyknotic nuclei, (G) CP+IC group: Hyperplastic proliferation of Langerhan’s cells, (H) CP+MSCs+IC group: vacuolation of acinar cells. H&E x400.
The sections of acute pancreatitis (AP) group showed apoptosis of Langerhans cells, which appear as eosinophilic apoptotic bodies’ in-between cells (Figure 7B
Sections of acute pancreatitis
On the other side, sections of acute pancreatitis and radiation exposure (CP) treated with mesenchymal stem cells (MSCs) CP+MSCs group showed good improvement of pancreatic lobules and islets of Langerhan’s histological picture. Some acinar cells showed deeply stained pyknotic nuclei, whereas the majority of acinar cells appeared with vesicular nuclei. The inflammatory reaction and vascular congestion completely disappeared (Figure 7F).
Sections of acute pancreatitis
Sections of acute pancreatitis
Discussion
The primary source of all pancreatic cells are pancreatic progenitor cells such as beta cells and thus, the proliferation and differentiation of pancreatic progenitor cells into islet-like cell clusters open the way for regenerating islets. Furthermore, finding potential drugs prompting the differentiation of bone marrow-derived mesenchymal stem cells (MSCs) into pancreatic progenitor cells may be a promising strategy for beta cell regeneration. 25 In the current study, we explore the efficiency of MSCs and/or Icariin to renew, repair and differentiate acinar-like cells in acute pancreatitis rat’s model exposed to radiation leads to chronic pancreatitis. Acute and especially late toxicity-related radiation consequences, is a major and well-established problem in radiation oncology practice for certain organs and tissues. The pancreas is one of the most radiosensitive organs and it can have serious damages due to the loss of function caused by chemotherapy with radiotherapy. 26
It is well documented that the administration and excessive concentrations of L-arginine causes an imbalance of amino acids that can trigger pancreatitis. It is the conversion of L-arg to L-ornithine which represent the most important step in the induction of pancreatitis by L-arginine. 27 Furthermore, previous studies stated that calcium-independent mitochondrial injury precedes other early events in the induction of pancreatitis by L-lysine, L-ornithine, and L-arginine. 28 However, in some reports the ultrastructure changes in response to toxic doses of amino acids (L-arginine) are detected earlier in the endoplasmic reticulum (ER), rather than mitochondrial abnormalities. 29 , 30 L-arginine is a G-protein-coupled receptor for the family C, (or class 3), which includes CaSR (calcium-sensing receptor) and G-PRC6A, (G-Protein-coupled receptor family C group 6 member A). 31 , 32 These 2 receptors expressed in the pancreas cause mutations that leads to acute pancreatitis. 33
In the current study, the administration of L-arginine to rats in repeated doses has induced acute pancreatitis demonstrated by a significant increase in serum amylase and lipase enzymes activity indicating deterioration in the pancreas functions, accompanied by an elevation in myeloperoxidase (MPO) activity, which was associated with high levels of the pro-inflammatory cytokines IL-8 and TNF-α. Moreover, L-arginine causes depression in pancreatic PDX-1 and MafA mRNA gene expression levels. Moreover, acute pancreatitis caused a significant increase of the angiogenic molecular factors TGF-β and PDGF levels along with a marked deposition of type I collagen and MCP-1. Besides, a disturbance in the Hedgehog (Hh) molecular signaling pathway which affects the fibrogenic pancreas up-regulation via increasing protein expression levels; Patched1 (PTCH-1), Smoothened (SMO), and GLi-1 (glioma-associated oncogene).
The exposure of AP rats to γ-radiation has intensified the damage through the amplified endogenous signals cascaded mediated by reactive oxygen species overproduction and activation of inflammatory mediators. 34 , 35 This is in agreement with the previous findings that γ-radiation has cytotoxic and genotoxic effects. 36 Transplanted MSCs alone or in combination with IC has significantly improved the key digestive enzymes amylase and lipase levels indicating a curative effect. The improvement of serum amylase and lipase levels was in line with the normalization of pancreatic histopathology.
It is well documented that IL-8 promotes pancreatitis, which activates pancreatic stellate cells, 37 - 39 and this explains the inflammatory response induced by L-arginine and γ-radiation exposure as acinar cell necrosis, followed by the release of the digestive enzymes lipase and amylase (Table 2), cytokines production and fibrogenesis (Table 3), which is the fundamental process underlying the diagnosis of extreme severe pancreatitis (Figures 4, 5, & 7). L-arginine is as a substrate for nitric oxide synthase and potentiates its pro-oxidant capacity by enhancing nitrosative stress and oxidative stress.
Exposure to γ-radiation elevates the level of inflammatory mediators which is linked with the release of prostaglandins and the production of free radicals, including ROS and nitric oxide (NO). Under these conditions, such as exposure to high doses of ionizing radiation, oxidative damage, chronic inflammation and its consequences, a disruption may occur in pancreatic functions, which explains the dramatic increase in lipase and amylase enzymes in AP plus irradiated rats. Our results exhibited that Icariin, and Icariin + MSCs improve the damage induced by L-arginine + Radiation. Supporting our study, Icariin acts by chelating free radicals involved in oxidative stress pathways which shows a strong antioxidant efficacy and therapeutic capabilities as neuroprotective effect, cardiovascular protective outcome, anti-tumor, anti-inflammatory, immune-modularity, and improved reproductive function. 40 A microenvironment can repair pancreas injuries which leads to differentiation into β-cell by the secretion of a variety of bioactive factors by MSCs. 41 A previous study suggests that the hippocampal neurogenesis of APP / PSI transgenic mice cerebral cortex inhibiting IL-6, IL-1β, and TNF-α was reduced by icariin (120mg/kg). 42
Meanwhile, the TGF-β and platelet-derived growth factor (PDGF) have the main role in the regulation of hedgehog signaling, which is an essential pathway of mesenchymal stem cells osteogenic. 43 Furthermore, TGF-β1 and PDGF released from pancreatic injured tissue activate collagen type-I mRNA which induces high production of proinflammatory cytokines and collagen deposition. 44 In agreement with the above, our results illustrated that TGF-β and PDGF levels are overexpressed accompanied with the up regulation of MCP-1 and collagen-I mRNA levels.
In the current study, Icariin combined with MSCs treatment restored PDGF, MCP-1 and collagen-I back to their basal levels and modulated TGF-β, which suggests that IC+MSCs play a vital role in the healing of fibrosis (Figure 4). Like our findings, the injection of rat Umbilical cord MSCs healed an injury to acinar cells by lowering the expression of monocyte chemoattractant protein 1 (MCP-1). 45 MSCs improves the excessive secretion of the extracellular matrix and its degradation during fibrosis, MSCs also reduces the collagen deposition as a principal constituent of the extracellular matrix. 46
Gamma rays-mediated ROS production effects senescence or autophagy induction has been associated with many signaling pathways. The initiation of senescence and autophagy led the cells to apoptotic cell death, which is the malignant diversion, or may revert them into the cell cycle. 35 Hedgehog signaling considerably over-expression leads to stimulated fibroblasts in pancreatic fibrosis. 39 In several embryonic patterning events, hedgehog signals are implicated and have an essential role. The Hedgehog (Hh) family of proteins control cell growth, survival, fate and pattern in almost every aspect of the vertebrates, and was found to play similar vital roles in controlling tissue patterning, as well as cellular differentiation and proliferation both during embryonic development and in the control of stem cell behavior and homeostasis in adults. Hh factors overexpression is also linked to pancreatic adenocarcinoma, moreover, the Hh pathway inhibition at the level of SMO can consequently result in proliferation obstacles and induce cell death in pancreatic cell lines. 47 Interestingly, some aspects of development and endocrine functions required a low-level of Hh signaling, where overt activation prevents organogenesis. In our study, we found that some hedgehog signaling markers were significantly exaggerated in L-arginine/irradiation rats group with a high level, however, the PTCH-1, SMO and GLi-1 overexpression protein levels were normalized by IC+MSCs treatment.
Interestingly, the role of MafA in pancreatic β-cells is to regulate their specification, maturation and possibly survival/proliferation of those cells. Furthermore, a study by Nagasaki and groups exhibited that MafA transduction in combination with PDX1 and Ngn3 in the liver of transgenic mouse-insulin luciferase promoter leads to a major stimulation of the insulin gene. 48 Thus according to our results, we could conclude that IC+MSCs transplantation activates β-cell functions along with the increased expression of pancreatic duodenal homeobox protein 1 (PDX-1) and v-maf musculoaponeurotic fibrosarcoma oncogene homolog A (MafA) gene expression, which are involved in the regeneration of islets and pancreatic beta-cell development. Besides its involvement in β-cell maturation, the strong evidence confirms MafA’s position as a central transcriptional regulator of β-cell function. 49
In brief, a marked antioxidant potential of IC plus MSCs replenishes and promotes the regeneration of pancreatic tissue by releasing PDX-1 and MafA transcription factors involved in the regeneration of islets and pancreatic repair that binds specifically to the insulin gene promoter and act as a crucial regulator for pancreatic beta-cell differentiation and improves the mature beta-cell functioning of the injured pancreas and regulating molecular intracellular signaling.
Icariin
MSCs therapy prohibits the progression of chronic pancreatitis. 51 In our study, we attempted to intensify the MSC’s capacity to home and survive into the injured pancreas tissue and to enhance their renewing tissues through combination with icariin, which has a potent antioxidant activity that can mediate tissue repair against cell death and inflammation caused by the chronic pancreas disease. Icariin has a great potential for ROS elimination. 52 Furthermore, icariin preserved the proliferative power of MSCs and decreased their senescence and dysfunction. 53 The ex-vivo icariin treatment behaves like a preconditioning agent that increases the secretion of favorable MSCs paracrine activity and decreases the risk of the early death of the engrafted MSCs in damaged tissue.
Conclusion
It is plausible to propose that MSCs co-transplantation with IC can impressively improve the function of pancreatic stellate cells by enhancing the key β-cell markers PDX1 and MafA. This is an important finding, as earlier studies have shown that PDX1 and MafA progenitor cells are the sources for functional beta-like cells. These findings shed light that a fuller understanding of new drugs to increase the growth and differentiation of bone marrow derived mesenchymal cells is essential. Also, further clinical studies are required.
Footnotes
Acknowledgment
Sincerely the authors acknowledge sincerely Dr. Ahmed Othman (Professor of Histopathology, Faculty of Medicine, Cairo University) for accomplishing the Histopathological examination in the present study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
All the ethical protocols for animal treatment were followed by the National Institutes of Health guide for the care and use of Laboratory animals (NIH Publications No. 8023, revised 1978) and supervised by the animal facilities, National Center for Radiation Research and Technology, Atomic Energy Authority.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
