Abstract
Radiographic imaging for scoliosis screening, diagnosis, treatment, and management is the gold standard assessment tool. Scoliosis patients receive many repeat radiographs, typically 10-25 and as many as 40-50, equating to a maximum 50 mGy of cumulative exposure. It is argued this amount of radiation exposure is not carcinogenic to scoliosis patients for 5 main reasons: 1. Estimated theoretical cumulative effective doses remain below the carcinogenic dose threshold; 2. Scoliosis patient x-rays are delivered in serial exposures and therefore, mitigate any potential cumulative effect; 3. Linear no-threshold cancer risk estimates from scoliosis patient cohorts are flawed due to faulty science; 4. Standardized incidence/mortality ratios demonstrating increased cancers from aged scoliosis cohorts are confounded by the effects of the disease entity itself making it impossible to claim cause and effect resulting from low-dose radiation exposures from spinal imaging; 5. Children are not more susceptible to radiation damage than adults. Radiophobia concerns from patients, parents, and doctors over repeat imaging for scoliosis treatment and management is not justified; it adds unnecessary anxiety to the patient (and their parents) and interferes with optimal medical management. X-rays taken in the evidence-based management of scoliosis should be taken without hesitation or concern about negligible radiation exposures.
Introduction
Over the last 20 years there has been a drastic movement throughout healthcare to restrict the use of radiological imaging due to carcinogenic concerns. This is due to reports, in the early 2000s, of projected increased cancers from CT scans 1,2 (that have continued to be published 3 ) and the release of the National Council on Radiation Protection and Measurements (NCRP) report 160 (2006) 4 concluding the near doubling of public exposures to medical radiation (mostly due to CT scans). This was then followed by more recent long-term studies of children cohorts who had received CT scans finding increased cancers in adulthood. 5,6 Throughout this timespan, the media has continued to amplify the carcinogenic concerns and propagated fears over medical exposures to radiation (i.e. radiophobia). 7 -11 Simultaneously, these reports motivated the initiation of several medical radiation reduction/limiting campaigns including Image Gently (pediatrics), 12 Image Wisely (adults), 13 Choosing Wisely (various disciplines), 14 and ACR Appropriateness Guidelines. 15
The movement to reduce medical radiation exposures have been criticized for being a “double-edged sword,” as many harms initially not realized have come to light. Real harms as well as presumed harms (i.e. increased radiation exposures) from medical radiation reduction campaigns include propagating radiophobia, 7 increased patient refusal for medically warranted X-rays, 11,16 increased burden to medical professionals attempting to deliver high-quality medical care, 17 reduced image quality, 18,19 increased potential missed diagnoses, 20,21 increased radiation exposures (via retakes due to too little exposure or gonadal shielding covering targeted anatomy), 17,18,22,23 increased use of alternate imaging methods that presents other unique risks (e.g. sedation for MRI), 18,24 and increasing liability to physicians. 17
Despite medical radiation reduction campaigns, there are conditions that warrant routine radiological imaging, this includes the condition of scoliosis. Scoliosis is a spinal deformity or curvature in the coronal plane as viewed on the antero-posterior (AP) or posterior-anterior (PA) spinal radiograph and is diagnosed as a curve greater than 9° as measured by the Cobb angle—the gold standard assessment method. 25 Most of the research focus on scoliosis is in the treatment of pediatrics and adolescents (i.e. adolescent idiopathic scoliosis: AIS), though it can affect patients of any age. Patients diagnosed with scoliosis are often exposed to repeated spinal X-rays during the medical management of the disorder, which may include “watchful waiting” (no treatment), spinal exercise programs, posture modification methods, spinal braces, spine traction, and/or eventual surgery. 26
Several studies have documented the total number of spinal radiographs as typically ranging from 10-25 images over the history of care of a given patient 27 -29 ; though some patients may receive upward of 40-50 or more spinal radiographs over several years. 30 Generally, the greater the progression of the spinal curve, the greater the number of X-rays the patient will receive during treatment and follow-up. 30
The radiation dose per X-ray image varies by spinal region, however a typical AP thoracic spine x-ray may be up to 0.5-1 mGy, roughly corresponding to a small pediatric, and a larger adolescent patient. The actual effective dose, however, varies according to the specific thickness and density of the patient as well as the variation between different x-ray machines. Thus, estimated theoretical cumulative effective doses that typical scoliosis patients receive may range from about 10 mGy to a maximum of 50 mGy (from plain films), and this of course depends on the age of initial diagnosis (size of patient) and number of radiographs taken (Table 1).
Estimated (Theoretical) Cumulative Effective Radiation Doses From Repeated Spinal Radiographs in Scoliosis Patients.
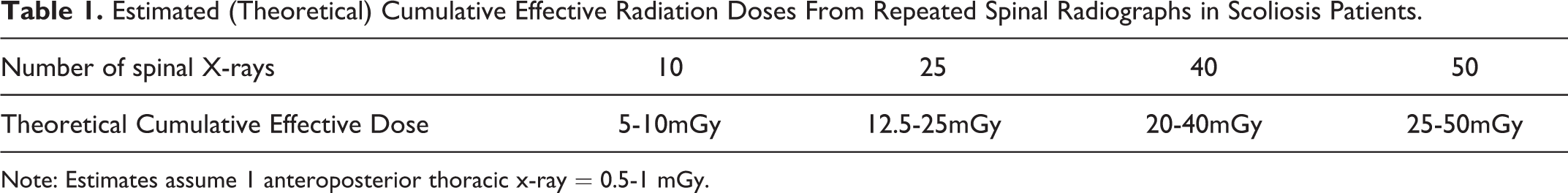
Note: Estimates assume 1 anteroposterior thoracic x-ray = 0.5-1 mGy.
Recently, there has been a substantial emergence of literature on the Estimated theoretical cumulative effective doses remain below carcinogenic dose thresholds. Scoliosis patient X-rays are fractionated and therefore mitigate potential cumulative effects. Linear no-threshold cancer risk estimates from scoliosis patient cohorts are a falsehood. Relative risk ratios demonstrating increased cancers in aged scoliosis cohorts show the effects of the disease entity and not radiation effects. Children are not more susceptible to radiation damage than adults.
The purpose of this article is to discuss the rationale underlying 5 main reasons why radiography as used in the treatment and management of spinal disorders, specifically scoliosis should not be feared or avoided due to unwarranted radiophobia by patients or their providers in daily clinical practice.
Estimated Theoretical Cumulative Effective Doses Remain Below Carcinogenic Dose Thresholds
Recently, Cuttler illustrated that the radiogenic dose threshold for leukemia, in nearly 100,000 atomic bomb survivors, is about 1100 mGy, (Figure 1). 37 Since the blood-forming stem cells of bone marrow are more radiosensitive than most other cell types (i.e. leukemia), other cancers would likely result from greater doses. 36 -38 Vaiserman et al. 39 argue the most accurate information on health effects from low-dose radiation exposures are found in studies on medical and technical personnel who are occupationally exposed. In their review, they noted that although in the early part of the last century (prior to 1920) there were increased cancers in radiologists, radiologic technologists, radiation and nuclear workers, this excess mortality disappears after 1920 (e.g. Yoshinaga; 40 Doll 41 ) when the first radiation limits were set in place at 0.2 R/d (equivalent to about 500 mGy/y).

1958 UNSCEAR data indicates a threshold of about 1.1 Gy (1100 mGy; assuming RBE = 1) for radiogenic leukemia in 95,819 persons exposed to A-bomb radiation from Hiroshima (Cuttler, 2019 37 ).
It is also documented that the data from multiple studies has shown less cancers in those occupationally exposed to low-doses of radiation, 39 suggesting low-dose exposures as having a protective effect, and to prevent cancers. 42 As discussed recently, 43 there is actually much evidence not only showing no harm from seemingly large radiation exposures (up to 500-800 mSv), but increased protective effects and less cancers. Calabrese et al. for example demonstrated in the early and mid 1900s, many human ills were treated by radiotherapy where patients were exposed to doses ranging from about 30-100 roentgen (∼263-877 mSv), which resulted in success rates of 75-90%. 44 Further, Cuttler and Pollycove 45 demonstrated that doses up to 300 mGy were protective against breast cancer, and Tubiana 46 showed doses up to 500 mGy were protective against secondary malignancies. In fact, radiotherapy which delivers radiation doses much higher than X-rays, has been used to successfully treat many human diseases including neurodegenerative and inflammatory conditions, infections, and cancers (Table 2). 44,47 -69
The question is, how can low-dose radiation exposures be harmful when they are proven to be beneficial? We contend, based on the data, low-dose radiation exposures are beneficial. Whatever the actual radiogenic dose threshold is (e.g. 500-1100 mGy), there is certainly no valid evidence of harm from doses below 500 mSv. 70 Thus, as demonstrated in Table 1, even for the scoliosis patient being diagnosed at a young age and receiving up to 50 spinal radiographs, this would still be at least an order of magnitude less than a conservative 500 mSv carcinogenic dose threshold estimate. Thus, there is no harm to the typical scoliosis patient, even for the patient receiving up to 50 X-rays, in terms of future potential radiogenic cancer induction.
Scoliosis Patient X-rays Are Fractionated and Therefore Mitigate Potential Cumulative Effects
Scoliosis patients receive spinal X-rays spread over time (i.e. a series of fractions delivered over time), approximately every 3-6 months depending on different clinical scenarios (i.e. age of patient, magnitude of spinal curve, receiving treatment or not, risk of progression, etc.). Therefore, the body has ample time for physiological repair of any damage done (DNA alterations) from singular X-ray events occurring during each assessment.
Radiation hormesis is the phenomenon where low doses have a beneficial health effect on living organisms, and only higher levels may produce harm. 71 Studies on patients receiving CT scans, for example, demonstrate that the genetic damage (DNA double-strand breaks) resulting immediately following low-dose CT scans do induce damage, however, as soon as 24 hours after exposure the damage is over-repaired, resulting in a net loss of damage (more repair) than prior to receiving the scan in the first place. 72 Thus, cumulative effective dose calculations for scoliosis patients receiving serial X-ray exposures are not valid as any potential harm is mitigated, and therefore, are theoretical and manufactured. 73
Linear No-Threshold Cancer Risk Estimates From Scoliosis Patient Cohorts Are a Falsehood
Several studies have used the linear no-threshold (LNT) model to calculate theoretical cancer incidence from estimating cumulative doses in scoliosis cohorts. 27,28 Essentially this is the application of a linear assumption that all radiation exposures are harmful, and that each exposure is cumulative in a linear fashion. 39,74
Using data from a cohort of 13 scoliosis females receiving 22 X-rays, treated with a brace over a period of 3 years, dosimeters measured actual radiation exposures. 27 Using the National Academy of Sciences data, carcinogenic risks to various internal organs were calculated. It was determined that the increase in organ carcinogenic risk due to radiation from 22 X-rays ranged from 3.4-15 per million, and for breast cancer ranged from 140-290 per million. 27 In a cohort of 2039 scoliosis patients referred to a large pediatric hospital between the years 1965-1979, Levy et al. calculated the theoretical lifetime cancer risks from dose-response models from the National Academy of Sciences 5th committee on the Biological Effects of Ionizing Radiation. 28 They determined a total lifetime excess cancer risk to range from 42-238/100,000 and 14-79/100,000 for women and men, respectively.
Critical assessment of these data 27,28 is needed as these theoretical risk estimates are inflated compared to today’s technology because of the greater radiation exposures associated with older X-ray technology. More importantly, this point becomes moot as this type of extrapolation using the LNT model is not applicable for low-dose exposures. 74 -77 Previous literature has not provided sufficient support to show low-dose radiation exposures from X-rays cause cancers, but there is data showing that low-doses prevents them. 44 -46,70 Also, as discussed, any damage caused by serial exposures to low-dose X-rays are mitigated. The extrapolations of estimated or measured radiation exposures to theoretical carcinogenic risks leads to public fear and dissuades the use of essential medical X-rays. 17,78
Relative Risk Ratios Demonstrating Increased Cancers in Aged Scoliosis Cohorts Show the Effects of the Disease Entity and Not Radiation Effects
Standardized mortality ratios (SMRs) and standardized incidence ratios (SIRs) are simple ratios of observed cases in a specific cohort to expected cases as determined from natural background incidence. These are used as a surrogate for the measure of association between radiation exposure and risk of cancer incidence (SIR) or mortality (SMR).
In the US scoliosis cohort study, several papers have been published showing increased SIRs and SMRs for scoliosis patients who received x-rays during childhood and adolescence. Hoffman et al. 30 reported on 1030 females with scoliosis who received an average of 41.5 X-rays over 8.7 years, and who were contacted by mail questionnaire or telephone interview an average of 26 years after initial diagnosis. They found 11 patients had reported breast cancer vs. an expected number being 6; this resulted in an SIR of 1.82 (90% CI = 1.0-3.0), and 2.4 (90% CI = 0.9-5.0) for those followed for over 30 years. Expanding on this dataset, Doody et al. 29 reported on 5573 female scoliosis patients who had an average of 25 X-rays and were followed-up an average of 40 years after diagnosis. There were 77 breast cancer deaths observed in the scoliosis cohort vs. only 45.6 expected; this gave an SMR of 1.69 (95% CI = 1.3-2.1). A re-analysis of this sample by Ronckers et al. 79 reported on the 47-year mean follow-up and reported an SMR of 1.68 (95% CI = 1.38-2.02) for breast cancer mortality in the scoliosis cohort.
As discussed above, low doses of radiation exposure given by repeat medical x-rays are not cumulative and do not likely induce cancer. Further, too often there is a failure to acknowledge the notion that low-dose radiation upregulates the body’s physiological adaptive protection systems. As mentioned, Cuttler and Pollycove
45
demonstrated that females treated for tuberculosis by chest X-rays, as examined in the Canadian breast fluoroscopy study,
80
having cumulative radiation exposures within 50-300 mGy exhibited breast cancer rates up to one-third less than the expected incidence. The question arises, therefore:
It should be noted that Ronckers et al.
79
found unexpected
Most scoliosis cohorts that have been followed or re-contacted years later are confounded by the exposures to X-rays in their youth, however, there are cohorts similar to scoliosis patients, those having thoracic hyperkyphosis spinal hunchback deformity who are not confounded by a history of previous X-rays. 85 -90 Many studies assessing the health status in these cohorts have found spine deformity patients have increased rates of cancers and also shorter lifespans. 85 -90 Kado et al., 87 for example, found relative to older people with good posture, thoracic hyperkyphosis hunched patients had a relative hazard of 1.44 for overall mortality (95% CI = 1.12 -1.86, P = .005), 2.03 for death from pulmonary causes (95% CI = 0.9-4.56), 1.86 for death from atherosclerosis (95% CI = 1.03-3.38), and 1.74 for death from cancers (95% CI = 0.8-3.81).
Increased cancer incidence in scoliosis cohorts may be explained by understanding physiological aging that is associated with spinal deformity. In studies that examined gene knockout mouse models, even though these mice showed normal development, they exhibited premature aging and spinal deformity (i.e. hyperkyphosis).
91
In other studies, mutations involving tumor suppressor genes
It becomes evident that the scoliosis disease entity itself hinders the functions of normal anatomy and over time, leads to pathophysiological consequences. The worsening of spine deformity with aging, therefore, biomechanically leads to detrimental consequences in terms of insidiously affecting a patient’s long-term health and longevity via the corresponding effects on the internal organs and spinal tract and nervous system.
Children Are Not More Susceptible to Radiation Damage Than Adults
A long-held notion is that children are more susceptible to the effects of radiation than adults because they are younger (more time for mutations to develop into cancers) and their immune systems are immature (i.e. less able to repair DNA damage). Disregarding scoliosis studies, long-term data on children exposed to low-dose radiation exposures do
Nasopharyngeal radium irradiation (NRI) treatment was practiced from the 1920s to the early 1970s for mostly children to shrink swollen lymphoid tissue in the area of the head and neck. Several studies have evaluated long-term risks of potential cancers resulting from this treatment. 94 -96 In all cases, there were no clear statistical findings of increased cancers in NRI-treated children versus controls; in fact, a National Cancer Institute report on NRI concludes: “A clear link between NRI exposure and cancer risk…has not been established.” 97
Another example for pediatric exposures to radiation is in the treatment of asthma in the earlier half of the 20th century. Calabrese et al. 49 summarized many studies showing the effective application of radiation in the treatment of bronchial asthma. The radiation doses from this treatment included an X-ray dose to the chest that was in the range of 0.01 to 1.0 skin erythema dose (SED). The SED is nominally 600 rad (6 Gy), which seems quite high for a chest X-ray considering that the whole-body lethal dose for humans (LD50) is about 450 rad or 4.5 Gy. 98 This is strong medicine that was given to children too. We could not locate any articles documenting the long-term carcinogenic effect of this asthma treatment.
For a brief few years from 1923-1936, pertussis (i.e. whooping cough) was treated with the use of radiation therapy. 54 Calabrese et al. reported on 20 articles showing the treatment of 1500 patients where the majority of cases were under the age of 3 years. Most cases showed dramatic symptomatic recovery (85% success rate) after 1-3 treatments totaling less than 0.5 erythema dose. There was also greater than a 90% reduction in childhood mortality in those less than 3 years. 54
In assessing the carcinogenic effects of radiation treatment for cancer in childhood in a sample of 5000 survivors, Tubiana et al. 46 reported on risks of secondary malignant neoplasms (SMN), specifically sarcomas and carcinomas as a function of initial radiation dose received from the original radiation treatment during childhood. The results indicated no increase in risk of SMN for doses lower than 1 Gy as calculated by a conventional case control method. Additionally, the authors found less cancer incidence for those having dose ranges from 0.0-0.5 Gy as calculated by the integral dose method 46 ; hence supporting the previously discussed hormesis effect. 71
Although there are well-known reports of increased thyroid cancers in children exposed to low-dose radiation (<10 mGy) after the Fukushima accident,
99
this turned out to be the result of the scientifically acknowledged problem of “thyroid cancer over-diagnosis.”
100
In fact, due to better diagnostic ability massive thyroid screening programs showed a 30-60 fold increased incidence of thyroid cancers in both exposed
Long-term cohort studies have reported increased cancers in adults who were exposed to CT scans during childhood (e.g. Pearce, 5 Matthews 6 ); although initially concerning, have been debunked for many methodological short-comings. 102,103 The most compelling criticism to these types of studies is the concept of protopathic bias (i.e. “reverse causation”). This implies that the children who were required to get the CT scans in childhood had underlying issues that would predispose them to future cancers versus the assumption that the radiation from the images had caused their future cancers. 104 This exact concept was shown to occur in the well-designed study by Journy et al. who determined that in assessing the relative risk of cancer incidence to adults who previously received CT scans prior to age 10, when controlling for known cancer pre-disposing risk factors, found that “no significant excess risk (for cancer) was observed in relation to CT exposures.” 105
Cancer is associated more with the aged and is likely associated with a less efficient immune function. 106 Thus, it can be argued that children have much more active immune systems and would be more protected from the damage from radiation exposures, regardless of source. As evidenced, children and adolescents can well tolerate low-dose level radiation exposures.
Discussion
In presenting 5 valid arguments why low-dose radiation exposures to scoliosis patients would not likely lead to future cancers, it is noteworthy to point out that even assuming LNT model validity, excess cancers in this cohort of patients would be negligible relative to the current approximate 40% background cancer incidence. 107 For example, assuming a maximum cumulative dose of 50 mSv in a scoliosis patient, the ICRP estimate of a 5% increased cancer risk per Sv 108 indicates a mere 0.25% (.05 Sv x 5%) increased cancer incidence. The potential benefit for a scoliosis patient who may have a higher quality of life by getting the appropriate medical treatment (and repeated X-rays) for their condition far outweighs any potential calculated population risk; that is, the individual risk is quite trivial.
Since repeated X-rays in scoliosis patients are mitigated by endogenous adaptive protection systems, the collective dose concept as presented in Table 1 is merely theoretical. Thus, as Oakley et al. have pointed out, scoliosis patients at most must be evaluated for harmful exposure from the total dose received from a single X-ray examination procedure, or about 1-3 mGy. 109 This makes the above aforementioned 0.25% increase above a 40% background cancer incidence all the more irrelevant (i.e. 0.005-0.015% added to background). Further, Socol et al. argue that for low-dose exposures, risks should more accurately be communicated at 2.5% increased cancer risk per Sv, not 5%. 110 Thus, this would half these predictions (i.e. 0.0025-0.0075% added to background), making them indistinguishable from background cancer incidence—and this is assuming LNT has validity for low-dose radiation risk estimates—which it does not.
Since the risks of radiocarcinogenicity from medical X-rays is low, if not non-existent, why are there such enthusiastic movements to reduce these exposures (e.g. American Chiropractic Association’s adoption of Choosing Wisely 111 )? The answer lies in the underlying assumptions regarding radiation carcinogenicity models. During the 1950s and formally adopted by the NCRP in 1977 112 the LNT model has been the foundation for all radiation risk analysis by national and international bodies. 110,113 This model is simple and as mentioned, has the inherent assumptions of all radiation being harmful and also cumulative. Both these assumptions are false. 75,76,114
The basis of the LNT model is the dataset from the Life Span Study (LSS) comprising the survivors of the atomic bombings of Hiroshima and Nagasaki. 113 Occurring 75 years ago, long-term follow-up of the survivors has given important insights as to the true extent of health outcomes resulting from this event. A recent analysis by Ozasa et al. 115 indicates that when the data are corrected for a “likely negative bias” in baseline cancer mortality rate, the data are more consistent with a linear-quadratic radiation hormesis model; that is, lower exposures reduced mortality. 113,116 Indeed, overall, the bomb survivors outlived controls. 117 Others have criticized the LSS data underpinning the LNT model on the basis of not being valid. 110,118 After performing a Monte-Carlo simulation of possible LSS outcomes, Socol et al. demonstrated there is insufficient statistical power for the LSS to support the LNT. 110 Sutou argues that because the residual radiation exposures from fallout occurred from contaminated rain (i.e black rain), this led to both an underestimation of exposure to the LSS, and the inappropriate use of a contaminated control group that was also irradiated by the rain. These discoveries led the author to conclude that LNT based on LSS data is invalid and stated “Major revision of the radiation risk assessment paradigm is required.” 118
As mentioned, the early studies projecting future cancers from CT scans (e.g. Brenner 1 ) and the NCRP report 160 4 created information that was amplified by the media and also fueled the launch of several medical radiation reduction campaigns. This “snowball effect” was based on invalid LNT projections. It should be noted that even if the LNT were valid, “the calculation of the number of cancer deaths based on collective effective doses from trivial individual doses should be avoided.” 108 This is because individual effective dose effects has great uncertainty (±40%) due to age, gender, mass, etc. 119,120 thus, “Risk is always a population-based metric and as such, its ascription to an individual patient should never be interpreted deterministically.” 121
If the LNT model is not valid for estimating health risks from low-dose exposures to radiation as from medical X-rays, why is it still used by the major regulatory bodies for risk assessment? This question is difficult to answer. One possible answer for the establishment to continued endorsement of the LNT as the prevailing model is for convenience and to continue its
Those LNT proponents who argue there is evidential support for the contention that X-rays cause cancers often cite the LSS study, the Oxford study of Childhood Cancers (OSCC) or large epidemiological studies. 128 In examining the evidence of these citations, however, Ulsh 128 found that there was no credible support. For the LSS study, for example, it is pointed out that in the Figure presented by Preston et al. 129 (2007) on the excess relative risk (ERR) for all solid cancers in LSS survivors from 1958-1998, that several of the data points below 0.2 Gy had central estimate values of about zero and stated “If this interpretation is correct, and the ERR from zero to approximately <150 mGy are not statistically significantly elevated, it means that the LSS study does not support the assertion that even doses more than 20 times higher than an adult chest CT have been shown to be associated with increased cancer risk.” 128
Examination of the OSCC study (e.g. Doll et al. 130 ; Boice et al. 131 ) it can be determined that there were significant short-comings including selection bias (used only fatal cancers as opposed to incident cases to avoid selection bias related to fatality), information biases (interviewers were aware of interviewee as control or study subject), uncertainties in dose estimates (reliance on memory for number of X-rays if missing from files), and was inconsistent with many other studies showing no increase in cancers of pediatric populations exposes to very low doses of radiation (e.g. shulze-rath et al. 132 ). 128
Large epidemiological studies have been published and claimed to show evidence of cancers caused from radiologic imaging, for example Pearce et al. 5 This study and others like it (Mathews et al. 6 ) have been criticized for several methodological flaws, the most significant being reverse causation. 103 As discussed, the study by Journey et al. proved reverse causation and showed children receiving CT scans in childhood are not a comparable population to children who do not get CT scans. 104 Further, a recent study by Shibata et al. who assessed why 763 children received CT scans, determined that 32% had congenital anomalies, and since the normal incidence of congenital anomalies is less than 2.5% they concluded “the population of children undergoing CT is completely different from that not undergoing CT. The 2 groups should not be compared.” 133 Thus, these types of studies are not an appropriate approach to support carcinogenicity caused from medical imaging.
The fact is, today’s current understanding of the scientific evidence shows that higher quality studies do not show increased cancer risks from low-dose radiation exposures. 134
Even if the LNT model were correct, which it is not, UNSCEAR has shown that overall, in only about 25% of cancer types,
128
children
Conclusion
The assessment of low-dose radiation exposures in cancer risk estimates using LNT modeling are misguided. Cancer incidence or mortality ratios from long-term studies of scoliosis patient cohorts are more likely documenting the pathologic consequences resulting from the disease entity of scoliosis of the spine rather than from negligible radiogenic effects from low-dose radiation exposures that likely prevent cancers. Although scoliosis patients receive many repeat radiographs, the equivalent radiation exposure remains at least 2 orders of magnitude lower than the dose threshold for developing leukemia, the cancer most likely to first occur. Radiographic imaging as used for scoliosis screening, diagnosis, treatment, follow-up, and management is not harmful to the patient. Ethical concerns for improving pediatric health should be directed at the diagnosis and treatment of the disease entity rather than wasting time, energy, and resources propagating erroneous associations between low-dose radiation exposures and non-existent radiogenic cancer risks.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: P.A.O. is a paid research consultant for CBP NonProfit, Inc.; D.E.H. teaches spine rehabilitation methods and sells products to physicians for patient care that require radiography for biomechanical analysis.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by funds from CBP NonProfit, Inc.

