Abstract
Objective:
Atherosclerosis is a pathological condition of fat deposition in the arteries, which causes cardiovascular disorders. Management of atherosclerosis remains a challenge and conventional drugs used for its management have several limitations. This study evaluated the protective effect of tabersonine against atherosclerosis and assessed its molecular mechanism of action.
Methods:
Atherosclerosis was induced by feeding apolipoprotein E (ApoE)-deficient mice a high-fat diet. Mice were treated with 20 or 40 mg/kg of tabersonine intraperitoneally for the 12-week duration of the study. Atherosclerosis markers and nitric oxide were measured in the sera of ApoE-deficient mice. Mediators of inflammation and markers of oxidative stress were assessed using enzyme-linked immunosorbent assays. Western blotting, quantitative reverse transcriptase polymerase chain reaction, and immunohistochemistry analyses were conducted to determine the protein expression in aortic tissue.
Results:
The tabersonine-treatment groups had an improved lipid profile and enhanced liver function, compared to the ApoE treatment group. Tabersonine treatment resulted in reduced levels of nitric oxide, cytokines, and oxidative stress, compared to the ApoE group. The altered expression levels of protein inhibitor activated STAT-3 (PIAS3), signal transducer and activator of transcription-3 (STAT-3), and nuclear factor of kappa light polypeptide gene enhancer in B-cells inhibitor, alpha (IkBα) in ApoE-deficient mice were ameliorated by tabersonine treatment. Moreover, cAMP-response-element-binding (CREB) expression was elevated in aortic tissue of tabersonine treatment groups, compared to the ApoE group.
Conclusion:
These results suggested that tabersonine ameliorates the expression of STAT-3 by activating CREB protein in atherosclerotic ApoE-deficient mice.
Introduction
Atherosclerosis is a pathological condition of fat or atheroma deposition in the arteries, which causes cardiovascular disorders. 1 Inflammation reportedly plays an important role in the initiation and development of atherosclerosis. 2 Several inflammatory mediators, such as interferon-γ and interleukin 6 (IL-6), have been shown to increase the incidence of aortic lesions. 3 The results of prior studies suggest that these inflammatory cytokines stimulate the JAK/STAT pathway, which promotes the migration, proliferation, inflammation, and adhesion of vascular cells. 4 Several factors including inflammatory mediators, mechanical stress, vascular stress, and angiotensin II activate the JAK/STAT pathway. 5 In the presence of elevated levels of IL-6, JAK is activated and phosphorylates STAT3; this modification leads to further stimulation of the immune response, cell survival, and cell proliferation through activation of gene expression. 6 Previous studies have reported elevated levels of IL-6 among patients with inflamed myocardial tissue. 7 In addition, vascular smooth cells, endothelial cells, T cells, and macrophages exhibit elevated levels of IL-6. 8
Several factors contribute to the formation and progression of atherosclerotic plaques, including oxidized low-density lipoprotein (ox-LDL), which causes smooth muscle cell proliferation and migration, foam cell formation, and inflammation. 9 The results of prior studies suggest that ox-LDL causes alterations in the levels of growth factors and cytokines, which activate STAT1 and STAT3. 10 Activation of the JAK/STAT pathway induces inflammatory damage and causes immune disorders. Activation of cAMP-response-element-binding (CREB) protein contributes to the regulation of immunological functions through inhibition of the STAT3 pathway. 11
Tabersonine is a terpene indole alkaloid present in several plants, including Catharanthus roseus (Apocynaceae). 12 Catharanthus roseus is used as a traditional Chinese medicine for the management of various conditions, such as cancer, malaria, and diabetes. 13 Tabersonine has been reported to exhibit strong anticancer and neuroprotective effects. 13 Previous studies have shown that tabersonine has strong anti-inflammatory properties and protects against lung injury by regulation of the nuclear factor (NF)-κB and p38/MK2 pathways. 14 Building on these prior findings, this study investigated the protective effects of tabersonine against ox-LDL-induced cell responses during atherosclerosis and examined the underlying molecular mechanism of action.
Materials and Methods
Animals
Eight-week-old, genetically modified (apolipoprotein E [ApoE]− / −) C57BL/6 J male mice were housed under the standard conditions of 12-hour light/dark cycles at 25°C ± 3°C and 60% ± 5% humidity. The study protocol was approved by the Institutional Animal Ethical Committee of Affiliated Hospital of Southwest Medical University, China (approval no. IAEC/AH-SMU/2018/09).
Chemicals
Tabersonine was purchased from Sigma-Aldrich (St. Louis, Missouri) and enzyme-linked immunosorbent assay kits were purchased from R&D Systems, Inc (Minneapolis, Minnesota). Antibodies for Western blotting were obtained from Abcam (Cambridge, Massachusetts). Kits used for the measurement of serum concentrations of aspartate transaminase (AST), alanine transaminase (ALT), LDL, high-density lipoprotein (HDL), and total cholesterol were purchased from Roche Diagnostics (Shanghai, China).
Experimental Protocol
Animals were fed a high-fat chow diet (21% fat and 0.15% cholesterol, wt/wt) for the 12-week study duration. Animals were separated into 4 separate groups of 10 animals per group: (1) a control group; (2) an ApoE group, in which animals received ApoE in a saline solution; (3) a 20 mg/kg tabersonine group; and (4) a 40 mg/kg tabersonine group. Tabersonine was administered intraperitoneally for 12 weeks. After 12 weeks, mice were killed by decapitation. Blood samples were collected and aortas were isolated for analysis.
Assessment of serum markers
Mice were anesthetized and blood samples were collected from the retro-orbital plexus. Serum was isolated by centrifugation at 13 000 rpm for 10 minutes at 4°C. An auto-analyzer was used to measure the serum concentrations of AST, ALT, LDL, HDL, and total cholesterol.
Assessment of nitric oxide
A nitrite/nitrate assay kit was used to investigate nitric oxide (NO) metabolites in plasma, in accordance with the experimental protocol provided by the kit manufacturer.
Assessment of cytokines
The levels of inflammatory mediators (ie, NF-κB, IL-1β, IL-6, and TNF-α) in aortic tissue homogenate were measured using enzyme-linked immunosorbent assays, in accordance with kit protocols.
Assessment of oxidative stress
The riboflavin sensitized method was used to assess the activity of superoxide dismutase and the absorbance was measured at 460 nm. The levels of lipoperoxidation in aortic tissue were determined using the method developed by Ohkawa. Malondialdehyde levels in aortic tissue were measured at 523 nm.
Assessment of immunohistochemical and histopathology analysis
Aortic tissue was isolated from each animal and fixed in formalin solution (4%) at 4°C for 24 hours. The tissue was sectioned at a thickness of 7 µm and neutral lipids in the plaques were detected using 0.5% Oil Red O stain. For immunohistochemical analysis of aortic tissue, samples were stained with primary antibodies and incubated for 12 hours, prior to incubation with secondary antibodies. A light microscope was used to analyze the stained sections.
Western blotting
Western blotting was used to investigate the expression levels of inducible nitric oxide synthase (iNOS) (1:200 dilution), p65 (1:500 dilution), protein inhibitor activated STAT-3 (PIAS3) (1:500 dilution), signal transducer and activator of transcription-3 (STAT-3) (1:200 dilution), nuclear factor of kappa light polypeptide gene enhancer in B-cells inhibitor, alpha (IkBα) (1:500 dilution), extracellular signal-regulated kinase 1/2 (ERK1/2) (1:200 dilution), p-ERK1/2 (1:1000 dilution), CREB (1:200 dilution), p-CREB (1:1000 dilution), α-tubulin (1:500 dilution), and β-actin (1:500 dilution) in isolated aortic tissue. Protein content in tissue homogenate was determined using a bicinchoninic acid assay kit, and protein separation was achieved by 10% sodium dodecyl sulfate–polyacrylamide gel electrophoresis. The proteins were transferred to blotting membranes and 5% blocking reagent was applied to prevent nonspecific binding. Membranes were incubated with primary antibodies overnight at 4°C. After membranes had been washed with phosphate-buffered saline, they were incubated with goat secondary antibodies conjugated to horseradish peroxidase. A chemiluminescence kit was used to assess protein expression.
Quantitative reverse transcriptase polymerase chain reaction
SYBR green-based quantitative reverse transcriptase polymerase chain reaction (qRT-PCR) was used to determine the messenger RNA (mRNA) expression levels of STAT-3, IL-6, PIAS3, and Monocyte chemoattractant protein-1 (MCP-1). Total RNA was isolated using TRIzol reagent and mRNA levels were analyzed using TaqMan MicroRNA assays. Moloney murine leukemia virus reverse transcriptase was used to synthesize the complementary DNA, applying 2 µg of total RNA to the reverse transcriptase reaction (20 µL). Primers (listed below) were mixed with reverse transcriptase 2 SYBR Green Mastermix and gene expression was determined using the Quantitative SYBR Green PCR assay. The relative target gene expression levels were determined using the 2−ΔΔCq equation.

Statistical analysis
The results were expressed as means ± standard errors of the mean (n = 12). All statistical analyses were performed using Prism 5.0 software (Graph Pad, La Jolla, California). Experimental groups were compared using Dunnett post hoc test. P values <.05 were considered statistically significant.
Result
Tabersonine Improved the Levels of Serum Markers
Serum markers of atherosclerosis including ALT, AST, total cholesterol, LDL, and HDL were measured in ApoE-deficient mice (Table 1). In the ApoE group, the total serum levels of cholesterol and LDL increased to 251.9 and 1206 mg/dL, respectively; the serum HDL levels decreased to 8.46 mg/dL. Moreover, AST and ALT activities in the ApoE group increased relative to those activities in the control group. The tabersonine treatment groups had reduced total cholesterol and LDL levels, as well as elevated HDL levels, compared to the ApoE group. Tabersonine treatment resulted in statistically significant dose-dependent reductions in ALT and AST activities, compared to the ApoE group.
Tabersonine Attenuates Serum Markers of Atherosclerosis in ApoE-Deficient Mice.a
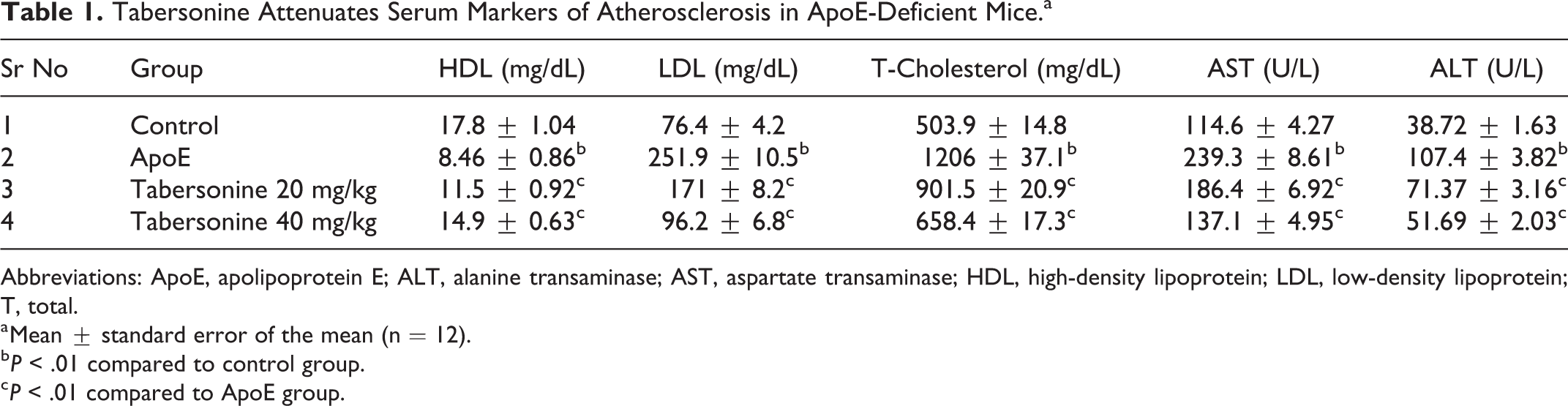
Abbreviations: ApoE, apolipoprotein E; ALT, alanine transaminase; AST, aspartate transaminase; HDL, high-density lipoprotein; LDL, low-density lipoprotein; T, total.
a Mean ± standard error of the mean (n = 12).
b P < .01 compared to control group.
c P < .01 compared to ApoE group.
Tabersonine Improved the Level of NO
The effects of tabersonine on plasma NO levels in ApoE-deficient mice are shown in Figure 1. The ApoE group exhibited elevated plasma levels of NO, compared to the control group. Tabersonine treatment significantly reduced the plasma levels of NO, compared to the ApoE group.

Tabersonine attenuates the level of nitric oxide (NO) in the plasma of apolipoprotein E (ApoE)-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group.
Tabersonine Improved Levels of Inflammatory Mediators
Cytokine levels were measured in aortic tissue homogenate of ApoE-deficient mice by enzyme-linked immunosorbent assay. The ApoE group had elevated cytokine levels in aortic tissue, compared to the control group. Tabersonine treatment improved the altered cytokine levels in ApoE-deficient mice (Figure 2).

Tabersonine attenuates the level of cytokines in the aortic tissue homogenate of apolipoprotein E (ApoE)-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group.
Tabersonine Improved Markers of Oxidative Stress
Markers of oxidative stress, including superoxide dismutase activity and malondialdehyde levels, were assessed in aortic issue homogenate of ApoE-deficient mice. Aortic tissue of ApoE-deficient mice exhibited elevated malondialdehyde levels (8.5 µM/mg) and reduced superoxide dismutase activity (0.3 U/mg). Tabersonine treatment improved markers of oxidative stress in aortic tissues of ApoE-deficient mice (Figure 3).
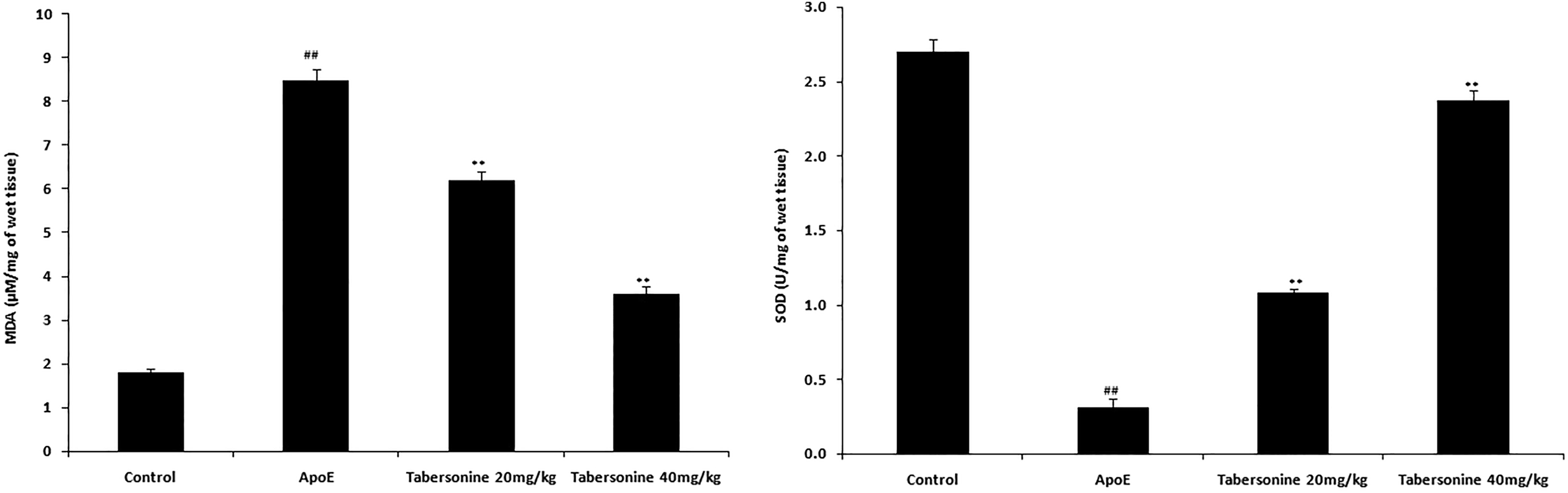
Tabersonine attenuates the markers of oxidative stress in the aortic tissue homogenate of apolipoprotein E-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group.
Tabersonine Improved Histopathological and Immunohistochemical Alterations
The effects of tabersonine were studied with respect to the histopathology and expression of iNOS in aortic tissue of ApoE-deficient mice (Figure 4A and B). The ApoE group had elevated lipid deposition in the aorta, compared to the control group. Tabersonine treatment reduced the level of lipid deposition in aortic tissue of ApoE-deficient mice (Figure 4A). In addition, aortic tissue of the ApoE group exhibited elevated iNOS expression, compared to the control group. The tabersonine treatment groups had reduced iNOS expression in aortic tissue, compared to the ApoE treatment group (Figure 4B).

Tabersonine attenuates histopathological changes in aortic tissue homogenate of apolipoprotein E-deficient mice. (A) Histopathology of aortic tissue; (B) Expression of iNOS in aortic tissue (immunohistochemical analysis). Mean ± standard error of the mean (n = 12).
Tabersonine Improved Protein Expression Levels of iNOS, p65, PIAS3, STAT-3, and IkBα
The protein expression levels of iNOS, p65, PIAS3, STAT-3, and IkBα were measured in aortic tissue of ApoE-deficient mice by Western blotting. The ApoE group had elevated protein expression levels of iNOS, p65, PIAS3, STAT-3, and IkBα, compared to the control group. The tabersonine treatment groups showed dose-dependent reductions in protein expression levels of iNOS, p65, PIAS3, STAT-3, and IkBα, relative to the ApoE group (Figure 5).

Tabersonine attenuates expression of iNOS, p65, PIAS3, STAT-3 and IkBα protein in aortic tissue homogenate of apolipoprotein E (ApoE)-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group.
Tabersonine Improved mRNA Expression Levels of STAT-3, IL-6, PIAS3, and MCP-1
The effects of tabersonine on mRNA expression levels of STAT-3, IL-6, PIAS3, and MCP-1 in aortic tissue of ApoE-deficient mice were evaluated by qRT-PCR. In the ApoE group, mRNA expression levels of STAT-3, IL-6, PIAS3, and MCP-1 were elevated (P < .01), compared to the control group. Tabersonine treatment resulted in dose-dependent reductions in mRNA expression levels of STAT-3, IL-6, PIAS3, and MCP-1 (Figure 6).

Tabersonine attenuates mRNA expression of iNOS, p65, PIAS3, STAT-3, and IkBα in aortic tissue homogenate of apolipoprotein E (ApoE)-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group. mRNA, messenger RNA.
Tabersonine Improved the Expression of CREB Protein
Both CREB and ERK1 protein expression levels were measured in aortic tissue of ApoE-deficient mice. The ApoE group had reduced protein expression levels of p-CREB/CREB and p-ERK1/ERK1, compared to the control group. The tabersonine treatment groups exhibited dose-dependent increases in protein expression levels of p-CREB/CREB and p-ERK1/ERK1, compared to the ApoE group (Figure 7).

Tabersonine attenuates expression of CREB and ERK1 protein in aortic tissue homogenate of apolipoprotein E (ApoE)-deficient mice. Mean ± standard error of the mean (n = 12); ## P < .01 compared to control group; **P < .01 compared to ApoE group. CREB indicates cAMP-response-element-binding.
Discussion
Atherosclerosis is a pathological condition of fat deposition in the arteries, which causes cardiovascular disorders. Inflammation reportedly plays an important role in the initiation and development of atherosclerosis. 2 The management of atherosclerosis remains a challenge and conventional atherosclerosis therapies have several limitations. This study evaluated the protective effect of tabersonine against atherosclerosis and investigated its molecular mechanism of action. Atherosclerosis was induced by feeding a high-fat diet to ApoE-deficient mice. Subsets of mice were treated with tabersonine 20 or 40 mg/kg intraperitoneally for the 12-week duration of the study. Markers of atherosclerosis were measured in the sera of ApoE-deficient mice. Markers of inflammation and oxidative stress were assessed by enzyme-linked immunosorbent assays. Western blotting, qRT-PCR, and immunohistochemistry analyses were conducted to assess expression levels of mRNA and protein in aortic tissue.
Atherosclerosis is often associated with changes in lipid profile and liver function, because lipid deposition in arteries leads to atherosclerosis. 15 This study revealed that tabersonine treatment ameliorated the alterations in lipid profile and liver function. Furthermore, mediators of inflammation and oxidative stress are considered important in the development of atherosclerosis. 16 Previous studies have shown that cytokines (eg, IL-1β and IL-6) are elevated following aortic tissue injury, thereby leading to further arterial fat deposition. 17 These changes in cytokine levels occur due to the degradation of IκBα and activation of NF-κB. 18 The results of this study showed that tabersonine treatment reduced cytokines levels and NF-κB in aortic tissue.
Previous studies have shown that elevated NO levels reduce the expression of PIAS3, thus promoting atherosclerosis. 19 In addition, oxidative stress is higher in atherosclerosis, which leads to increased protein expression levels of iNOS and p65. 20 This study demonstrated that tabersonine treatment resulted in reduced levels of NO. Tabersonine ameliorated the altered protein expression levels of iNOS and p65 in ApoE-deficient mice. The results of prior studies suggest that STAT3 mediates IL-6 expression by downregulation of NF-κB in atherosclerosis. 21 The present study showed that tabersonine treatment reduced PIAS3 expression, thereby negatively regulating the JAK/STAT pathway.
Lastly, the ERK-CREB signaling pathway is involved in several vascular disorders. Given the role of CREB protein in regulation of immunological function, the findings in previous studies suggested that this protein may constitute a novel target for the treatment of atherosclerosis. 22 Several factors, including inflammation mediators and CREB inhibition, contribute to the development of atherosisclerosis. 23 This study showed that tabersonine treatment activates CREB protein in aortic tissue of ApoE-deficient mice.
Conclusion
This study showed that treatment with tabersonine ameliorated the expression of STAT3 by activation of CREB protein in atherosclerotic ApoE-deficient mice. In addition, treatment with tabersonine reduced cytokine levels and oxidative stress markers associated with atherosclerosis in aortic tissue of ApoE-deficient mice. Based on these findings, tabersonine is a potential treatment for atherosclerosis.
Footnotes
Acknowledgments
All the authors of this manuscript are thankful to National Natural Science Foundation of China, China (grant no: 81500643) for providing funding to conduct this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Received financial support for this work from National Natural Science Foundation of China, China (grant no. 81500643).
