Abstract
We reported that low-dose radiation (LDR) alleviated cardiotoxicity of doxorubicin (DOX) via inhibiting myocardial cell apoptosis and oxidative stress in vivo. Here, we tested whether LDR could enhance chemotherapeutic effect of DOX and alleviate myocardial injury induced by DOX by observing cell proliferation, apoptosis, and metastasis of heterotopic tumor in vivo. Mice implanted with 4T1 breast carcinoma cells were given 7.5 mg/kg DOX or 0.9% NaCl solution 72 hours after LDR (0 or 75 mGy). The histology of tumor tissue was observed by hematoxylin and eosin staining, the apoptosis was determined by terminal deoxynucleotidyl transferase–mediated dUTP nick-end labeling, and the expression of Ki67, Bcl-2, Bax, cleaved caspase3, matrix metalloproteinase 2 (MMP2), MMP9, and CD34 was detected by Western blot. Expression of Ki67 and CD34 was also detected by immunohistochemistry. Results showed that cell proliferation of the breast tumor and protein expression of the metastasis-related molecules were significantly reduced and the apoptosis of tumor cells was significantly increased in the LDR + DOX-treated tumor-bearing mice. Pretreatment with LDR significantly prevented DOX-induced cardiotoxicity likely through preventing DOX-induced mitochondrial Bcl2/Bax dyshomeostasis-induced caspase-3 cleavage-dependent apoptosis. These results suggested that LDR not only enhances DOX antitumor effect but also reduces DOX cardiotoxicity, which may potentially overcome the limitation for DOX clinical usage.
Introduction
Breast cancer is the most common cancer and also a major cause of death in women worldwide. 1 Doxorubicin (DOX, Adriamycin), an anthracycline that suppresses tumor progression via inducing apoptosis and inhibiting metastasis of tumor cells, is a traditional curative chemotherapy (CTX) for breast cancer. 2 However, the clinical application potential of DOX was immensely limited by its profound cardiotoxicity and acquired drug resistance. The myocardial damage induced by DOX might relate to the increase in apoptosis. 3 The drug resistance may account for the excessive tumor cell damage, metabolic dysregulation, and autophagy induced by DOX. 4 Thus, seeking a new approach that can sensitize DOX’s antitumor effect with less side effects on heart is urgently needed.
In recent years, low-dose radiation (LDR)-induced adaptive response has attracted the attention of radiation biologist and oncologist. 5 Dey et al found that LDR delivered in fractionations sensitized CTX drug toxicity in tumor cells in vitro. 6 In contrast, LDR also reduced the chemotherapeutic damage on the immune system, stimulated the antitumor immune reaction, and then promoted the CTX efficiency in tumor-bearing mice. 7 These findings were separately consistently evidenced in other studies, 8 including our own 9 : LDR combined with CTX significantly delays tumor growth by promoting apoptosis and blocking cell cycle in vivo 8 ; LDR prevented DOX-induced cardiac damage in BALB/c mice. 9 These preclinical research indicated that LDR could not only sensitize CTX effects in vitro and in vivo but also exhibit a potential protection against CTX side toxicity on normal tissues. Nevertheless, whether LDR enhances antitumor effect of DOX and also alleviated the cardiac side toxicity induced by DOX in the same animal model as well as what potential mechanisms remains unclear yet.
In this study, therefore, we established the subcutaneous heterotopic breast tumor-bearing mice to test whether 75 mGy LDR could enhance the chemotherapeutic effect of DOX with a simultaneous protection of cardiac tissue from DOX through the analysis of tumor cell growth, proliferation, apoptosis, and metastasis-related protein expressions. Mechanistically, mitochondrial Bcl-2 and Bax expression-mediated caspase 3 cleavage status was also examined in the xenograft breast tumor tissue and the cardiac tissue. We demonstrated that pre-LDR treatment enhanced DOX antitumor effects and also reduced DOX cardiac damage, which may be associated with the differential regulation of mitochondrial Bcl2/Bax caspase-3 cleavage pathway between tumor and cardiac tissues.
Materials and Methods
Cells and Animals
The murine 4T1 breast carcinoma cell line was obtained from Cell Lines Bank, Shanghai Institute of Biological Sciences (Shanghai, China). Cells were maintained in RPMI-1640 medium (Gibco, Thermo Fisher Scientific, USA) supplemented with 10% fetal bovine serum (Gibco) and antibiotics (100 IU/mL of penicillin and 100 IU/mL of streptomycin) and incubated at 37°C in a humidified atmosphere of 95% air and 5% CO2.
Female BALB/c inbred strain mice, weighing 18 to 22 g and 8 weeks of age, were purchased from Animal Experiment Centre of Basic Medical Sciences, Jilin University. All experimental procedures were approved by the Institutional Animal Care and Use Committee of the Jilin University, which was in compliance with the Guide for the Care and Use of Laboratory Animals published by the National Institutes of Health (NIH Publication No. 85-23, revised 1996). All mice were housed at constant temperature, constant humidity, and specific pathogen-free with free access to food and water. The paddings were replaced regularly.
Establishment of Subcutaneous Heterotopic Breast Tumor-Bearing Model in BALB/c Mice
In brief, 0.1 mL (2 × 106 per mL) 4T1 cell suspension was subcutaneously inoculated into the right-side axilla area of BALB/c mice to form breast tumor xenograft mouse model. A total of 24 female BALB/c mice were used in this experiment. The subcutaneous tumors were monitored, and when tumors of 3 to 5 mm in diameter formed in the axilla, mice were grouped randomly into 4 groups: (1) Control group (vehicle treatment)—mice were treated with 0.9% NaCl solution through intraperitoneal injection and irradiated with 0 mGy (n = 6); (2) LDR group—mice were irradiated in whole body with LDR 72 hours before the injection of 0.9% NaCl solution (n = 6), and a deep X-ray machine model was used to give the LDR whole-body irradiation at a dose of 75 mGy (LDR) with a dose rate of 12.5 mGy/min; (3) DOX group—mice were sham-irradiated with X-rays and then injected with DOX at 7.5 mg·kg−1 (n = 6); (4) LDR + DOX group—the mice were irradiated with 75 mGy X-rays and 72 hours later given the injection of DOX at 7.5 mg·kg−1 (n = 6), based on a previous study. 10 Five days after injection, mice were weighed and then anesthetized by injection of 0.1 mL pentobarbitone (1%) and killed for collecting tumors and hearts, both of which were excised, weighed, and photographed. Portions of the tumor tissue and heart were fixed in 4% paraformaldehyde for morphological assay, immunohistochemical staining, and terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) staining, while the remaining tissue was used for Western blot analysis.
Histological Examination
After fixation with 4% paraformaldehyde, tumor tissues were embedded in paraffin and sectioned at a thickness of 4 μm. These sections were deparaffinized with dimethylbenzene and rehydrated with graded alcohols for staining. Then the sections were stained with hematoxylin and eosin and examined under a microscope for the morphology of tumor cells.
Immunohistochemistry
After rehydration with graded alcohols, antigen retrieval was performed by treating the slides with sodium citrate buffer and heating in a microwave oven at 98°C for 15 minutes each. Endogenous peroxidase activity was blocked with 3% hydrogen peroxide solution at 37°C for 25 minutes. Nonspecific binding was prevented by blocking with normal goat serum at room temperature for 20 minutes. Immunostaining of Ki67 and CD34 was performed using murine anti-Ki67 and CD34 monoclonal antibody (Proteintech, Wuhan, China). Goat antimouse immunoglobulin G conjugated with horseradish peroxidase (HRP) was used as the secondary antibody. The staining procedure was carried out manually at 37°C for 30 minutes, using HRP-avidin complex method. Reactive products were visualized with 3,3′-diaminobenzidene as the chromogen, and the slides were counterstained with hematoxylin. The stained slides were analyzed and photographed under a microscope, and cellular brownish staining was scored as positive.
The TUNEL Assay
The TUNEL assay was performed using the TUNEL System kit (Promega, Madison, Wisconsin), according to the manufacturer’s protocol. Briefly, the slides were permeabilized with proteinase K (20 μg/mL) at 37°C for 2 minutes followed by TUNEL in the dark at 37°C for 1 hour. The localized green fluorescence of the apoptotic cells was visualized by fluorescence microscopy. 11
Western Blot Analysis
Total proteins were extracted in the presence of complete protease and PhosSTOP phosphatase inhibitors (Roche Applied Sciences, Indianapolis, Indiana) and subjected to sodium dodecyl sulfate polyacrylamide gel electrophoresis. Separated proteins were electrophoretically transferred onto polyvinylidene difluoride membranes (Thermo Fisher, Rockford, Maryland) and immunoblotted with anti-Bcl-2, Bax, β-actin, total and cleaved caspase 3, matrix metalloproteinase 9 (MMP-9), MMP-2, vascular endothelial growth factor (VEGF), N-cadherin, and E-cadherin (Proteintech), as described previously. 11,12 Immunoreactive proteins were visualized using the Odyssey Infrared Imaging System (Li-Cor, Lincoln, Nebraska) following the guidelines of the manufacturer. 11
Results
Low-Dose Radiation Slightly Ameliorated the Body Weight Loss of DOX-Treated Tumor-Bearing Mice
In order to assess the effects of LDR on the health of these mice, we monitored their body weight daily after treatment. As shown in Figure 1A, there was no difference in the body weights between control (vehicle treated tumor-bearing mice) and LDR groups; DOX-treated mice had a lowest body weight compared to other groups, while pretreatment of the tumor-bearing mice with LDR showed less body weight loss in DOX-treated mice (Figure 1A). These results suggested that LDR inhibited DOX-induced body weight loss, which may mirror the less systemic toxicity of DOX, including cardiotoxicity.

Analysis of the effect of low-dose radiation (LDR) preirradiation in vivo. A, Daily body weight of the 4T1 xenograft tumor-bearing mice following different treatments. B and C, Tumor sizes and average weight among different groups following different treatments. D, Representative images of histological changes, examined by hematoxylin and eosin (H&E) staining, in different groups are presented. The damage of cell structure was significantly intensified in tumors of LDR + doxorubicin (DOX) group compared to those of DOX group. E, Representative images of Ki67 expression in the tumors of different groups examined by immunohistochemistry were provided. F, Semiquantitative analysis of Ki67 expression among groups was presented as mean density (MD) value. The data represented the mean ± standard deviation (SD) for 6 animals in each group (n = 6). *P < .05 versus control group; **P < .01 versus control group; # P < .05 versus DOX group.
Low-Dose Radiation Enhanced DOX Antitumor Effect
The effect of LDR on breast tumor growth was examined by measuring tumor sizes (Figure 1B) and weight (Figure 1C) from all groups. Compared to control group, LDR did not change tumor size and weight, but DOX significantly reduced tumor size and weight. Pretreatment with LDR enhanced the inhibitive effects of DOX in LDR + DOX group compared to DOX group (P < .05).
Hematoxylin and eosin staining showed no significant changes such as reddish cytoplasm, karyopyknosis, or karyorrhexis in the control group; however, these changes were observed in the LDR or DOX group (Figure 1D). Moreover, those histopathological changes were intensified in the LDR + DOX group even with more karyolysis and destroyed cell structures (Figure 1D).
Immunohistochemistry analysis of Ki67 expression, index of cell proliferation (Figure 1E and F), showed the inhibitive effect of LDR or DOX alone on tumor cell proliferation, while LDR + DOX showed the most inhibitive effect on tumor cell proliferation among groups. Taken together, this study implies that LDR could enhance DOX effect on inhibiting tumor growth in breast tumor-bearing mouse model.
Low-Dose Radiation Enhanced DOX-Induced Tumor Cell Apoptosis
The TUNEL staining in the tumor tissues revealed that apoptosis rates of tumor cells in the groups of mice treated by LDR or DOX alone and LDR + DOX were all significantly elevated (P < .05) compared to that of control group, with the highest rate in LDR+DOX group (Figure 2A and B).
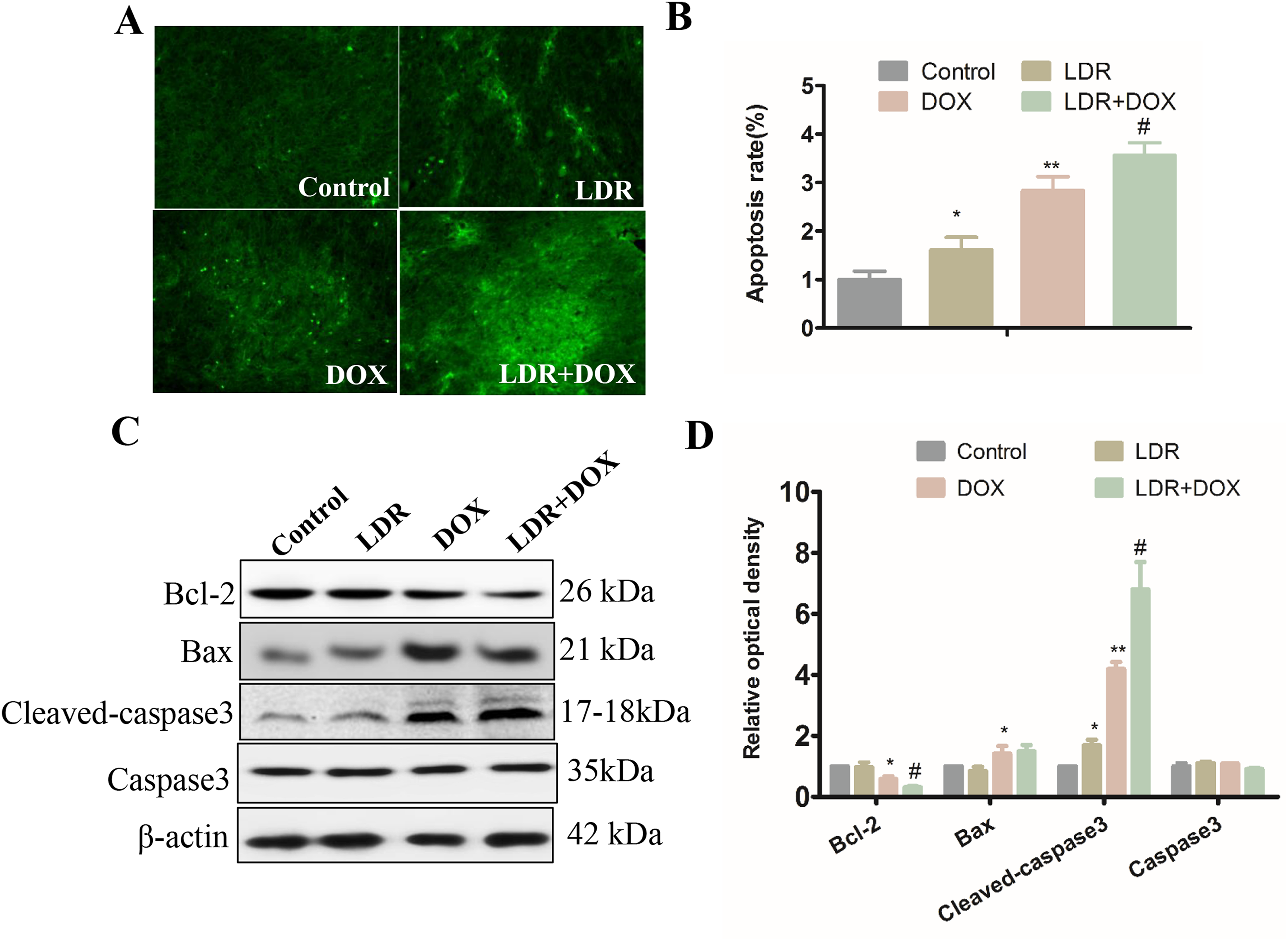
Low-dose radiation (LDR) enhanced apoptotic effect of doxorubicin (DOX) in xenograft breast tumor. A, Apoptosis in 4T1 xenograft tumors was examined by terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) fluorescent staining, where green fluorescence indicates apoptosis, representative images of which from each group were presented. B, Semiquantitative analysis of TUNEL-positive cells by relative optical density (OD) value was presented. C, Representative Western blotting profiles for the protein expression of Bcl-2, Bax, total, and cleaved caspase3 in the tumors of different groups. D, Relative OD values of Western blots in panel C were compared to their loading control (β-actin). Data represented the mean ± standard deviation (SD; n = 6). *P < .05 versus control group; **P < 0.01 versus control group; # P < .05 versus DOX group.
To further confirm the enhanced apoptosis by preexposure to LDR, expression of Bax, Bcl-2, and cleaved caspase-3 was detected by Western blots (Figure 2C and D). Results showed that the expression of antiapoptotic protein Bcl-2 in tumor tissues was significantly downregulated in the DOX group and further downregulated in the LDR + DOX group compared to the control group. Moreover, both DOX with and without LDR significantly (P < .05) increased proapoptotic protein Bax expression. Neither LDR nor DOX affected noncleaved caspase 3 expression in the tumor tissue, but both LDR and DOX increased and LDR + DOX synergistically increased cleaved caspase-3 expression. Taken together, we showed that LDR pretreatment could promote tumor cell apoptosis in DOX-treated tumor-bearing mice (Figure 2C and D).
Low-Dose Radiation Enhanced DOX-Inhibiting Expression of Tumor Metastasis-Related Proteins
To evaluate whether LDR enhances the inhibitive effects of DOX on metastasis-related proteins in the tumor tissues, the immunohistochemistry assay was employed to detect the expression of CD34, an index of endothelia cells. As shown in Figure 3A and B, the expression of CD34 in tumors was significantly (P < .05) downregulated in the LDR group, more downregulated in the DOX group, and most significantly downregulated in the LDR + DOX group compared to the control group. Expression of VEGF by Western blotting assay was slightly low in the DOX group (but P > .05) and significantly low in the LDR + DOX group (P < .05).

Low-dose radiation (LDR) enhanced the antimetastasis effect of DOX in xenograft breast tumor. A, Representative images of CD34-positive staining that was analyzed by immunohistochemistry in the tumors of different groups are presented. B, Microvessel density (MD) values of CD34 staining in each group were semiquantitatively analyzed. C, Western blot assay of matrix metalloproteinase 9 (MMP9), MMP2, vascular endothelial growth factor (VEGF), E-cadherin, and N-cadherin expression in each group. D, Optical density (OD) values of Western blot in each group were compared to their loading control (β-actin). The data represented the mean ± standard deviation (SD; n = 6). *P < .05 versus control group; **P < .01 versus control group; # P < .05 versus doxorubicin (DOX) group.
In addition, expression of other metastasis-related proteins including MMP9, MMP2, and E-cadherin was also examined by Western blotting assay. Compared to the control group, expression of MMP9 and MMP2 in the tumors was significantly downregulated in DOX-treated mice and further downregulated in LDR + DOX-treated mice (P < .05; Figure 3C and D). Low-dose radiation slightly decreased MMP9 expression but did not affect the expression of MMP2, N-cadherin, and E-cadherin (Figure 3C and D). It was noted that DOX alone did not affect N-cadherin expression but remarkably increased E-cadherin expression. Low-dose radiation further worsened DOX-decreased N-cadherin expression effect but did not affect DOX-increased E-cadherin expression effect. These results indicated that LDR might enhance the inhibitive effect of DOX on breast tumor metastasis possibility through decreasing expression of MMP9, MMP2, and N-cadherin proteins.
Low-Dose Radiation Prevented DOX-Induced Cardiotoxicity in Breast Tumor-Bearing Mice Probably Through Preserving Bcl2-Mediated Inhibition of Caspase-3 Cleavage
To test our hypothesis that LDR not only enhances DOX antitumor effect but may also protect the heart from DOX-induced cardiotoxicity, Western blot was employed to detect the expression of Bcl-2, Bax, and cleaved caspase 3 in heart tissues. We found that the level of cleaved caspase 3 was reduced in the LDR group and increased in the DOX group, but not changed in the LDR + DOX group, compared to the control group (Figure 4). Expression of Bcl-2 was significantly downregulated in the heart of DOX-treated mice (P < .05) but was significantly increased in the LDR group and even in the LDR + DOX group (Figure 4). In contrast, although LDR did not affect cardiac level of Bax level compared to control, it significantly prevented DOX-increased Bax level in the heart of LDR+DOX-treated mice compared to DOX-treated mice.

Low-dose radiation (LDR) protected heart from doxorubicin (DOX) probably via preserving Bcl2-mediated inhibition of caspase 3 cleavage. A, Western blot assay for protein expression of Bcl-2, Bax, and cleaved caspase 3 in cardiac tissues from each group. B, Optical density (OD) values of these target proteins, shown in panel A, from all groups were compared to their loading control (β-actin). The data represented the mean ± standard deviation (SD; n = 6). *P < .05 versus control group; **P < .01 versus control group; # P < .05 versus DOX group.
Discussion
A previous study concluded that organ weight changes were often attributable to CTX side effects. 13 Similarly, a consensus research confirmed the negative impact by DOX on the body weight gain in mice. 14 However, an adaptive response protection could be induced by LDR pretreatment, 15 leading to a protection of the normal tissue from DOX. Consistent with this concept, the present study showed that mice in the LDR + DOX group were relatively heavier than those in the DOX group. This may relate to the improvement in systemic toxicity, including cardiac toxicity, by LDR in DOX-treated breast tumor-bearing mice.
Yu et al found that LDR could stimulate the growth of normal cells but not tumor cells in vitro and in vivo. 16 They also reported that pretreatment of S180 sarcoma-bearing mice with whole-body X-rays at 75 mGy significantly enhanced antitumor effect of cyclophosphamide on the inhibition of both tumor growth. 8 Low-dose radiation also reduced sphere formation and self-renewal ability and prevented cancer metastasis in breast cancer. 17 In the present study, we used DOX as CTX reagent and also provided evidence that pretreatment of breast tumor-bearing mice with whole-body X-rays at 75 mGy enhanced the antitumor effect of DOX on tumor growth. Although we did not have direct evidence to show less metastasis of the tumors, we showed the enhanced effect of LDR on DOX-induced inhibition of metastasis-related protein expressions. In terms of tumor cell growth, the nuclear antigen Ki67, a nuclear proliferation marker, is an important index of cell proliferation in the breast cancer, prostate cancer, and malignant pleural mesothelioma. 18 -21 The immunohistochemistry evaluation of cell staining for Ki67 has been widely applied to comparing proliferation between tumor samples, which is also potentially used for predicting the resistance to CTX and as a biomarker of treatment efficacy in samples. 22 We showed here that LDR or DOX could inhibit tumor growth via reducing Ki67-positive cells, but combined LDR with DOX showed more significantly reduction in Ki67-positive cells in tumor tissue which was in good agreement with the morphological changes (Figure 1E and F). These results indicated the cytotoxicity of DOX in xenograft breast tumor was potentiated by LDR pretreatment.
One of mechanisms by which LDR inhibits tumor growth may be related to its antitumor immune function that may increase antibody formation, natural killer activity, secretion of interferon, and other cytokines which all are able to inhibit tumor growth, 23 which, in fact, also negatively regulated tumor cell metastasis by inhibiting metastasis-associated proteins. 23 Tumor metastasis and invasion were complex processes mediated by various proteins, such as CD34, MMP2, and MMP9. The expression of CD34 promoted the formation of pathological, invasive vessels during neovascularization. 24 Both MMP2 and MMP9 reportedly contributed to the metastasis and invasion of gastric carcinomas and colorectal cancer. 25,26 In the present study, we showed that LDR treatment followed by DOX further decreased, compared to DOX alone, the expression of CD34, MMP2, and MMP9. These findings suggested that DOX combined with LDR pretreatment may have more sufficient inhibition of tumor metastasis compared to DOX treatment alone.
For any CTX or radiotherapy, activation of apoptosis in tumor cells plays a crucial role in the antitumor effect. Here, we showed that treatment with DOX combined with LDR significantly promoted tumor apoptosis process (Figure 2A and B). It was reported that LDR could increase the apoptosis of tumor cells through lowering the level of antiapoptosis protein Bcl-2 in the S180 sarcoma-bearing mice, 27 resulting in mitochondria-related caspase 3 cleavage-mediated apoptosis. 28,29 Our experiment revealed that LDR pretreatment promoted DOX-induced apoptosis in tumor tissues by increasing Bax–Bcl-2 ratio and cleaved caspase-3, supporting the involvement of the mitochondria apoptosis pathway.
What’s more, our previous study has defined that LDR pretreatment could protect cardiac tissue from DOX-induced cardiotoxicity via suppressing apoptosis and oxidative stress. 9 In the present study, LDR pretreatment with DOX could significantly prevent DOX-induced decrease of Bcl-2 expression and increase of Bax expression and cleaved caspase-3 in cardiac cells (P < .05), further confirming that pretreatment with LDR could lighten cardiac damage by DOX treatment in breast tumor-bearing mice (Figure 4).
In summary, this study concluded that LDR enhanced the effect of CTX. The combination therapy of LDR and DOX significantly blocked the growth and metastasis possibility of xenograft breast tumor-bearing mice and meanwhile also significantly decreased DOX side toxicity in cardiac, and probably other normal tissues. Different responses of breast tumor and normal tissues, especially the heart, to LDR were the fundamental phenomenon with the great potential for clinical application in breast cancer CTX.
Footnotes
Author Contribution
Xin Jiang and Yanwei Du are equal contributors.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China, NSFC [grant number: 81272471].
