Abstract
Background:
Dental trauma is caused by fracture(s) in the vertical plane and the horizontal plane of roots. The objective of this study is to perform multiple diagnostic modalities for the diagnosis of horizontal root fracture(s) of the tooth.
Methods:
A total of 250 patients with dental complaints were subjected to intraoral radiography, multidetector helical computed tomography (MDHCT), and limited cone beam computed tomography (LCBCT). The suspected tooth was extracted, visually inspected, and subjected to microcomputed tomography (micro-CT). Images were observed in the lightbox, and a fracture was considered if it had been directly visualized as radiolucent line traversing tooth root. Wilcoxon test/Tukey post hoc test was performed at 99% of confidence level.
Results:
With respect to visual inspection, for LCBCT, intraoral radiography, MDHCT, and micro-CT, sensitivities were 0.988, 0.972, 0.967, and 0.979; accuracies were 0.956, 0.785, 0.905, and 0.888; false-positive values were 5, 21, 12, and 11; and false-negative values were 3, 24, 3, and 11, respectively. The area of the image visible at one time was in the order of treatment without radiography < intraoral radiography < MDHCT < micro-CT < LCBCT.
Conclusion:
The LCBCT had the highest sensitivity and accuracy for diagnosis of horizontal tooth root fracture(s).
Level of Evidence:
I.
Trial Registry:
researchregistry3647, dated December 31, 2016 (www.researchregistry.com).
Keywords
Introduction
Dental trauma mainly causes fractures in the horizontal plane of the root. Moreover, the horizontal tooth root fracture is hardly detectable by intraoral radiography. 1 Diagnosis of fracture of tooth root is a vital method to determine the appropriate treatment and to assess prognosis for the dental trauma. 2 Intraoral radiography is a well-established imaging modality for detection of tooth root fracture. However, it has low accuracy and is slightly problematic, where the displacement of the fragments does not occur and is not characterized by granulation of tissues or oral edema. 3,4 At present, the computed tomography (CT) methods for 3-dimensional images have been employed to compensate for the drawbacks (eg, distortion, anatomic superimposition, and magnification) of intraoral radiography. Limited cone beam computed tomography (LCBCT) has been established for regional dentomaxillofacial small field-of-view imaging, 5 with high-resolution scans at the same low-dose radiation as that of intraoral radiography. 6 Moreover, LCBCT and helical computed tomography (HCT) are well-established methods for detecting vertical root tooth fracture(s). 7
There is enough empirical evidence that radiation is harmful and can cause cancer. 8 However, oral and maxillofacial surgeons ignored linear no-threshold hypothesis (LNTH) and as low as reasonably achievable (ALARA) principles for diagnosis of rare horizontal tooth root fracture(s) and performed multiple radiological diagnoses, because the low-dose radiation of the imaging modalities has no reported to harm. However, LNTH and ALARA do in an assured manner . 9 Both principles stated that low-dose responses are the mother of high-dose effects and that it yields cumulative harm throughout life, irrespective of how low the dose rate is. 10 However, these hypotheses are not protective at all. 9 In everyday life, people have face low-dose radiation from the sky, their bodies, and land. Average annual natural background exposure is 1 to 260 mSv in some areas, yet no associated toxic health effects have been reported. 11
The primary aim of the study was to use multiple diagnostic modalities for diagnosis of horizontal root fracture(s) of the tooth in humans ignoring LNTH and ALARA principles. The secondary end point of the study was to compare sensitivity and accuracy of intraoral radiography, multidetector helical computed tomography (MDHCT), LCBCT, and micro-CT for diagnosis of horizontal tooth root fracture(s) considering a visual inspection of tooth (after extraction) as “reference standard” at the level I of evidence (Table 1) without conflict of interest.
Level of Evidence.

Methods
Ethical Consideration and Consent to Participate
The study had been registered in research registry (www.researchregistry.com), UID no.: researchregistry3647, dated December 31, 2016. The protocol (BR/XCH/DR/13/17, dated December 29, 2016) had been granted by the Xiangyang Central Hospital review board. The study had adhered to the law of China. A written informed consent for radiographic images, surgeries, to have additional procedures done purely for research purposes, and patient information and images (if any) to be published in all formats (hard and/or electronics) irrespective of time and language were provided by the patients or their relatives (legally authorized representatives).
Inclusion criteria
All patients admitted to the oral and maxillofacial department of the Xiangyang Central Hospital, Affiliated Hospital of Hubei University of Arts and Science, Hubei, China, and Xiangyang City Dental Hospital, Xiangyang, Hubei, China, during January 2017 to January 2018, with complaints of tenderness, mobility, and/or dental trauma due to some orofacial injuries in the upper left, lower left, upper right, lower right, or central incisor were included in the study. Patients who were aged 18 years and older and signed informed consent form were included in the study. All patients who had been subjected to all types of radiological images were included in the study. The demographic characteristics of enrolled patients are reported in Table 2.
The Demographic Characteristics of Patients.a,b

aAll data were represented as number (percentage).
bAll patients had the origin of PR China.
cWho had faced an accident and the remaining had faced oral injuries.
Exclusion criteria
Patients who were aged younger than 18 years and not signed informed consent form were excluded from the study. Patients who had a psychiatric problem or neuropathic pain in the oral cavity but not any endodontic problems were excluded from the study. The patients whose only intraoral radiography, MDHCT, or LCBCT scan or combination of these 2 diagnostic modalities, which led to intraoral surgery for extraction of the tooth were excluded from the study.
All the tooth examined were traumatized central incisors per Association of Surgical Technologists standards of practice for ionizing radiation exposure in the perioperative setting. 12 The study had adhered to Standard for Reporting of Diagnostic Accuracy (STARD) guidelines and 2013 Declarations of Helsinki. 13 The work is reported in line with Strengthening the Reporting of Cohort Studies in Surgery criteria. 14 A total of 250 patients were subjected to nonexperimental, nonrandomized, cross-sectional study. The STARD flow diagram of the study is presented in Figure 1.

STARD flow diagram of the study. All the tooth examined were traumatized central incisors as per AST. STARD indicates Standard for Reporting of Diagnostic Accuracy; AST, Association of Surgical Technologists.
Intraoral radiography
All patients were subjected to intraoral radiography using standardized X-ray exposure (GE Healthcare, Chicago, Illinois, USA). The instrument was operated at 19.9 mA, 66 kV, 0.0999 seconds exposure time, and 40 cm of a focus-film distance. Images were obtained by the bisecting technique at an angle of +54.5° to the occlusal plane and phosphor plate (Prestige Dental Products, Inc, Canada) was used as the image detector. 2
Multidetector helical computed tomography
All patients were subjected to Somatom Emotion 6, MDHCT (Siemens, Erlangen, Germany). The instrument was operated at 79.9 mA and 129 kV. The axial scan, parallel to the occlusal plane was recorded at 2-slice thickness settings: 0.629 mm detector (0.5 mm) and 0.629 mm slice thickness. The collimation detector was used. The images were reconstructed to 0.2-mm-interval images. 2,15
Limited cone beam computed tomography
All patients were subjected to LCBCT (PSR 9000N; Asahi Roentgen, Kyoto, Japan). The instrument was operated at 8 mA, 70 kV, and 1 second, with a slice thickness of 0.099 mm. Patients were positioned so that the occlusal plane had been paralleled with the floor. Imaging had produced 39.9 mm height and 40 mm diameter cylindric field of view. 2,16
Tooth extraction
The suspected tooth was extracted using forceps under local anesthesia (lidocaine) by the oral maxillofacial surgeon. 17 All extracted teeth were visually inspected. The presence of pulp, cementum, and/or the dentine was considered as root fracture. The visual inspection was considered as “gold standard” or reference standard. 18
Micro-computed tomography
Micro-CT provides enhancement in forensic diagnostic accuracy. Therefore, all extracted teeth were subjected to the micro-CT device (SkyScan 1278, Brucker, Germany). The instrument was operated at 100 µA and 65 kV, and 0.013 mm slice thickness with radiation of <1 µSv/h at 10 cm from the instrument surface and reconstruction time of 45 seconds. 2,19
Image analysis
Radiographical scans were performed per protocols (protocol 1: field of view: 41 × 41 and voxel: 0.079 mm; protocol 2: field of view: 99 × 99 and voxel: 0.19 mm; protocol 3: field of view: zoom and voxel: 0.079 mm). Twelve radiologists including the authors observed the radiographs in the lightbox. Data of MDHCT and LCBCT had been reconstructed to provide images (cross-sectional coronal) perpendicular to the fracture lines by Digital Imaging and Communications in Medicine (DICOM) viewer software (postDICOM, UK). A fracture was confirmed if it was directly visualized as radiolucent line traversing the tooth root. The interpretation of DICOM files had a response of either yes or no to the question as “Is a fracture line present?.” 20 The benefit score (the difference between the expected benefit and the expected harm) for diagnosis of horizontal tooth root fracture of each modality was derived by decision curve analysis method (Equations 1 and 2) 21 :
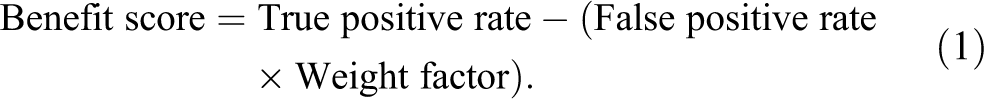

Statistical Analysis
InStat (Windows version, GraphPad Software, CA, USA ) was used for statistical analysis of the study. Wilcoxon test 22 following Tukey post hoc test (considering critical value q > 4.418 as significant) 23 was performed for predictive values between the 4 diagnostic modalities. The results were considered significant at a 99% confidence level. DeLong test was used to compare the area under the curve values (AUCs) for different diagnostic modalities. Results by 12 radiologists were evaluated by κ statistics to check intra- and interobserver reproducibility (where κ coefficient = 0—indicated random chances in agreements between the raters and 1—indicated perfect agreements between the raters). 18 For statistical analysis, true results were considered as 1, and false and inconclusive results were considered 0. Per protocol method of analysis was preferred.
Results
Only 55 patients had faced accident that led to dental trauma. However, remaining enrolled patients had small injuries related to oral cavity before enrollment.
Three, 7, 2, and 9 patients were not subjected to intraoral radiography, MDHCT, LCBCT, and micro-CT, respectively. Results of 247 patients for intraoral radiography, 243 patients for MDHCT, 248 patients for LCBCT, 250 patients for visual inspection (reference standard), and 241 patients for micro-CT were used in the statistical analysis.
There were perfect agreements between the raters for image analysis (κ > .81; Table 3). With respect to the visual inspection, .972, .967, .988, and .979 were sensitivities (radiolucent line traversing the tooth root was considered as root fracture for radiographic images, and the presence of pulp, cementum, and/or the dentine was considered as root fracture for visual inspection) of intraoral radiography, MDHCT, LCBCT, and micro-CT, respectively, for the presence of horizontal root fractures. The LCBCT (P = .0005; q = 2.729) had higher diagnostic accuracy than intraoral radiography (P < .0001, q = 11.756), MDHCT (P < .0001, q = 6.298), and micro-CT (P < .0001, q = 7.758). Intraoral radiography, MDHCT, LCBCT, and micro-CT had 0.623, 0.723, 0.813, and 0.745 AUC values, respectively (Figure 2). There were high true fracture line rate and low false-positive fracture line rate observed with LCBCT. Moreover, inconclusive results were higher in the case of intraoral radiography and MDHCT than LCBCT (Table 4).
Intra- and Interobserver Reproducibility for Image Analysis.a-d

aTotal 12 radiologists were involved in image analysis.
bκ: kappa coefficient. κ = 0: Random chances in agreements between the raters, κ = 1: Perfect agreements between the raters.
cA fracture was considered if it was directly visualized as radiolucent line traversing the teeth root for radiological images.
dThe presence of pulp, cementum, and/or the dentine was considered as root fracture for visual inspection.

Diagnostic parameters of imaging modalities. Visual inspection of the tooth after extraction was considered as “reference standard.” A fracture was considered if it was directly visualized as radiolucent line traversing the tooth root. All the tooth examined were traumatized central incisors as per AST. Blue-colored bars show the area under the curve values, saffron-colored bars show the diagnostic accuracy, and the slate-colored bars show the diagnostic sensitivity. AST indicates Association of Surgical Technologists.
Interpretation of Results of Different Diagnostic Modalities.a-e

aAll data were represented as a number (percentage).
bA fracture was considered if it was directly visualized as radiolucent line traversing the teeth root.
cVisual inspection of teeth considered as “reference standard.”
dAll the teeth examined were traumatized central incisors as per AST.
eRadiography of upper left, lower left, upper right, lower right, and central incisor.
The area of the image visible at 1 time available per modality with respect to threshold probability (a state of diagnostic confidence above it the tooth extraction could be performed) was in the order of treatment without radiography < intraoral radiography < MDHCT < micro-CT < LCBCT (Figure 3).

Decision curve for the benefit score of individual modality. Visual inspection of the tooth after extraction was considered as “reference standard” for comparison purpose only. A fracture was considered if it was directly visualized as radiolucent line traversing the teeth root for radiological images. The presence of pulp, cementum, and/or the dentine was considered as root fracture for visual inspection. All the tooth examined were traumatized central incisors as per AST. AST indicates Association of Surgical Technologists.
Discussion
The first-ever human diagnostic study ignored LNTH and ALARA principles on dental trauma demonstrated that LCBCT had higher diagnostic accuracy among available diagnostic modalities for diagnosis of horizontal tooth root fracture(s). The LNTH and ALARA principles prescribe strictly adhered radiation dose optimization in imaging. However, there is no evidence for the carcinogenicity of radiation imaging modalities. 9 Both principles lack suggested guidelines. 10,24 Applying this to the protocol for the study, the trial is a justified use of multiple diagnostic modalities for diagnosis of horizontal tooth root fracture.
The study reported a sensitivity of 0.972, 0.967, 0.988, and 0.979 for intraoral radiography, MDHCT, LCBCT, and micro-CT, respectively, for horizontal tooth root fracture(s). Single horizontal root fracture in the apical or middle third tooth of the root is the usual result after trauma to the tooth. 25 To detect the horizontal root fracture, intraoral radiography is widely used as it is cheap, has high resolution, and is convenient. 26 While interpreting radiographic images, a radiolucent line demonstrating discontinuity of dentine, which is not a shadow of the periodontal ligament, can be diagnostic of root fracture, 27 but subtle fissures in a very early stage without separation of the fragments may not be quantifiable by intraoral radiography. 28 The results of the study suggest that intraoral radiography is not an exact method for detection of horizontal root fracture.
The study showed the highest diagnostic accuracy for LCBCT among all diagnostic modalities. The difference in accuracy for the diagnostic modalities was due to the difference in slice thickness. 29,30 Radiographic films have higher resolution than MDHCT, LCBCT, and micro-CT, 31 but intraoral X-ray images are distorted by the vertical angle between film and the axis of the tooth leading to inaccurate images of horizontal root fractures. 18 However, LCBCT gives a 3-dimensional view of tooth root without overlap of images, which provides a detailed evaluation of horizontal tooth root fracture. 32 The study suggested that intraoral radiography and MDHCT imaging modalities were less effective in the diagnosis of horizontal root fracture than vertical root fracture.
This cross-sectional human study showed the superiority of LCBCT for diagnosis of horizontal root fracture. All previous studies of diagnostic modalities for horizontal root fracture are simulated studies only. 2,3,17 -20,33 The simulated study has a major limitation in generalizing results in the clinics, for example, separation of the fragments and subsequent union and gluing of the fragments is carried out, which results in large fracture lines that might be easy to diagnose. 20 The simulated fracture is not an event that happens like a dental trauma. 17 The effect of patient movement on the scans cannot be taken into account, which has a significant effect on the resolution of images 34 and also has the issue of root fillings or various types of post that affect diagnosis. 27 In respect to the selection of an object in the trial, the current study is first research on humans and provides valuable state-of-art research results in the field of Endodontists.
Some limitations of the study are, for example, that the interpreters were not blind to the study, and all diagnostic modalities have attenuation problems. Zoom images have greater noise than the original images and have a higher chance of false positives. While original images have lower chances for the masking of fracture lines in the images. The study was not performed specifically for diagnosis of horizontal root fractures. The study was performed for the prospect of research not for patients’ treatment purpose. The MDHCT had a 5× higher slice thickness at acquisition and 10× higher slice thickness at reconstruction for viewing than LCBCT. The ethical considerations and patients consent for 4 different radiographic modalities just for the detection of horizontal tooth root fracture was difficult to obtain. The study did not compare the diagnostic parameters with the gold standard modality of magnetic resonance imaging.
The study is describing some reflections of the role of CT scan in dental trauma. Some more explanation must be done to explain the radiation hazard. The optimization process deals with risk and benefit and not only damage. The knowledge of the damage is not fully known yet which must be taken notice of. The LNTH and ALARA principles have contributed to developing new diagnostic modalities with lower radiation to the patients. The LNTH and ALARA principles have had great importance in getting lower radiation doses. The radiation dose for the different modalities ought to be given. So, the study can be helpful in advising which modality can be used to give the best diagnoses with little radiation to the patient, which is the most important part of the finding.
Conclusion
This nonexperimental, nonrandomized, cross-sectional study with level I of evidence concluded that LCBCT had higher diagnostic accuracy than intraoral radiography, MDHCT, and micro-CT. The LCBCT should be used for the detection of horizontal root fracture.
Footnotes
Author’s Note
Feng Li and Jun Li contribute to this work equally. All authors read and approved the manuscript for publication. Feng Li and Jun Li had performed conceptualization, data curation, and formal analysis. Deming Zhang performed an investigation, methodology, and project administration. Feng Wu drafted, reviewed, and edited the manuscript for intellectual content.
Acknowledgments
Authors are thankful for the radiological and nonradiological staff of Xiangyang Central Hospital, Affiliated Hospital of Hubei University of Arts and Science, Hubei, China and Xiangyang city dental Hospital, Xiangyang, Hubei, China.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
