Abstract
Presenteeism, defined as attending work despite physical or mental health issues that impair full productivity, is a prevalent concern with significant implications for workplace efficiency and employee well-being. Testosterone, the primary male sex hormone, plays a vital role in sustaining physical energy, cognitive function, and emotional stability—key factors for optimal work performance. This study explores the association between late-onset hypogonadism (LOH) and presenteeism, emphasizing how LOH-related symptoms such as fatigue, reduced libido, erectile dysfunction, and mood disturbances may contribute to reduced workplace productivity. Data from 96 male patients aged 27 to 76 years, who sought treatment at a university hospital for LOH-related symptoms, were analyzed using blood tests and validated questionnaires, including the Aging Males’ Symptoms (AMS) scale, Work Functioning Impairment Scale (WFun), and Sexual Health Inventory for Men. Significant correlations were observed between AMS scores and both work functioning impairment and erectile dysfunction, indicating a strong link between LOH symptoms and presenteeism. In addition, symptoms such as fatigue, diminished motivation, and poor sleep quality were identified as exacerbating factors for work-related impairments. The greatest strength of this study lies in its focus on clinically diagnosed LOH patients, a factor that significantly distinguishes it from prior research on presenteeism in general working populations. This study underscores the potential benefits of testosterone replacement therapy, lifestyle modifications, and workplace wellness programs in addressing presenteeism among employees with LOH. Further research is necessary to assess the efficacy of these interventions in mitigating presenteeism and improving employee well-being.
Introduction
Presenteeism is defined as the phenomenon where individuals attend work despite physical or mental health issues that hinder their ability to perform at full capacity. Unlike absenteeism, which is the complete absence from work, presenteeism is more subtle but can have significant impacts on productivity, workplace dynamics, and employee well-being (Fujino, 2018). The term has gained prominence in occupational health research due to its implications for individual productivity and organizational performance. Presenteeism is a widespread issue in modern workplaces, often associated with chronic health conditions, mental health problems, and workplace stress. Studies estimate that the economic cost of presenteeism can surpass that of absenteeism due to its pervasive and persistent nature (Brouwer et al., 2023). Presenteeism affects nearly 50% of employees in developed nations at some point in their careers, and its prevalence continues to rise as job demands increase (Aronsson et al., 2000).
Testosterone, the primary male sex hormone, plays a significant role in maintaining both physical and mental health, which may directly influence workplace productivity and presenteeism (Ide, 2023; Okawara et al., 2024). Testosterone contributes to muscle mass, energy levels, bone density, and overall physical vitality. Low testosterone levels (a condition known as hypogonadism or, in aging men, late-onset hypogonadism [LOH]) can result in various symptoms such as fatigue, weakness, reduced physical stamina, erectile dysfunction (ED; Ide et al., 2023). These factors impair an individual’s ability to meet workplace demands, contributing to presenteeism. Individuals experiencing fatigue are more likely to attend work despite being unproductive, as they may not perceive fatigue as a legitimate reason to take leave. This behavior contributes to presenteeism, as their output at work is suboptimal.
Testosterone plays a crucial role in cognitive function and emotional well-being. LOH has been linked to decreased focus and attention, poor memory, mood disorders, such as depression and anxiety, and sleep disturbances (Ide, 2023). These mental and emotional impairments can diminish an individual’s ability to perform tasks effectively, increasing the likelihood of presenteeism.
The association between sexual function and LOH has been well-documented. Research has indicated that a substantial proportion of men with LOH experience sexual dysfunction. For example, the European Male Aging Study revealed that men with testosterone deficiency are more likely to report symptoms such as reduced libido and difficulty achieving or maintaining erections compared to men with normal testosterone levels (Corona et al., 2011). Sexual dysfunction, including ED and reduced libido, can significantly impact an individual’s quality of life (QOL), self-esteem, and overall mental health. These factors, in turn, influence work performance and productivity (Elterman et al., 2021). The association between sexual function and presenteeism has been a growing area of interest in scientific research.
While direct studies linking LOH to presenteeism are limited, this study stands out by specifically targeting clinically diagnosed LOH patients rather than relying on self-reported symptoms in general working populations. Evidence suggests that addressing the symptoms associated with low testosterone can improve workplace productivity and reduce presenteeism. Indeed, a previous study found that men with higher testosterone levels demonstrated better physical function and energy levels, which are critical for workplace efficiency (Snyder et al., 2016). Additionally, studies targeting employees in general corporations suggest a significant association between LOH symptoms and work dysfunction (Okawara et al., 2024). Although several studies have investigated presenteeism in general working men (Okawara et al., 2024; Yoshimoto et al., 2020), no research has specifically focused on cases with LOH symptoms. While previous studies on presenteeism have mainly involved general working male populations or relied on self-reported symptoms, our study specifically targets patients with confirmed LOH diagnoses. This approach provides a more accurate assessment of the relationship between LOH-related symptoms and presenteeism by minimizing misclassification bias and enhancing clinical relevance.
In this study, we investigated whether LOH serves as a contributing factor to presenteeism by conducting a detailed evaluation using various validated questionnaires for patients presenting with LOH symptoms. By focusing on clinically diagnosed patients, this study provides robust data that contribute to a more comprehensive understanding of the relationship between LOH and presenteeism. Addressing LOH, including sexual dysfunction, particularly through medical interventions such as testosterone replacement therapy (TRT), counseling, and lifestyle modifications, may alleviate presenteeism and improve both personal and professional well-being. This targeted approach opens a new avenue for improving workplace efficiency and employee QOL by addressing the specific challenges faced by individuals with clinically confirmed LOH.
Materials and Methods
Subjects
This study was based on data from 135 men who visited the Department of Urology at Juntendo University Hospital with complaints of symptoms related to LOH, between 2022 and 2024. Thirty-nine individuals with missing blood test data or incomplete questionnaire responses were excluded, leaving a total of 96 subjects. Specifically, patients with severe psychiatric disorders, systemic chronic diseases, or those who were experiencing acute occupational overload were excluded from the final analysis based on clinical interviews and medical history. While sleep quality and depression were assessed via the Pittsburgh Sleep Quality Index (PSQI) and the Self-rating Depression Scale (SDS), respectively, we did not apply these as exclusion criteria but rather analyzed their relationship with presenteeism. Ages ranged from 27 to 76 years. For each patient, blood test data and questionnaire results from the initial consultation were used. Body mass index was measured based on the patient’s height and weight. Approval was obtained from the Hospital Research Ethics Board (Approval number: H22-0403).
Blood Collection
Blood samples were collected in a fasted state in the morning. Blood for serum luteinizing hormone (LH) and follicle-stimulating hormone (FSH) concentrations was collected in plain tubes and then centrifuged at 3,000 rpm for 5 min. Blood for serum testosterone was collected in plain tubes and then centrifuged at 3,000 rpm for 10 min. Total testosterone levels were measured by chemiluminescent immunoassay using an Architect i2000SR (Abbott Japan, Minato City, Japan). A Modular EEE or cobas e 801 (Roche Diagnostics, Basel, Switzerland) was used for measuring LH and FSH levels by electrochemiluminescence immunoassay.
Questionnaire
In this study, participants were asked to respond to the Aging Males Symptoms (AMS) score (Heinemann, 1999), which assesses the severity of LOH symptoms, the Work Functioning Impairment Scale (WFun; Tokutsu et al., 2019), which evaluates work function impairment, the Sexual Health Inventory for Men (SHIM; Rosen et al., 1999), which evaluates ED, PSQI (Buysse et al., 1989), which assesses sleep quality, and SDS (Jokelainen et al., 2019), which evaluates depression. All questionnaires were completed by the patients themselves using a tablet device.
Statistical Analysis
Pearson’s correlation analysis was used for the statistical analysis of the AMS score and each questionnaire. Analysis of variance was used for the statistical analysis of the AMS score and WFun. The significance level was set at p < .05. Statistical Package for Social Sciences (SPSS) version 29.0.0 (IBM Corp., Armonk, NY, USA) was used to analyze the data.
Results
Basic Characteristics
Patient characteristics are presented in Table 1. The target patients were over 20 years old, and all underwent blood sampling and self-administered questionnaires.
Patients Characteristics

Note. AMS = Aging Males Symptoms; BMI = Body mass index; FSH = follicle-stimulating hormone; LH = luteinizing hormone; PSA = Prostate Specific Antigen; PSQI = Pittsburgh Sleep Quality Index; SDS = Self-rating Depression Scale; SHIM = Sexual Health Inventory for Men; WFun = Work Functioning Impairment Scale.
Comorbidities included mental disorders in approximately 30% of cases, hypertension and dyslipidemia in about 20% of cases, and diabetes in 7% of patients. The most common reason for visiting the hospital was a referral from a primary care physician, accounting for approximately 50%. Approximately 40% of patients learned about the concept of LOH syndrome through media outlets such as television and radio, prompting them to seek medical consultation. Referrals from other departments within the hospital accounted for 7%, while cases where patients were encouraged to seek medical consultation by family members or occupational physicians were less common, at 2% each.
Subjective Symptoms
All target patients responded regarding the presence or absence of symptoms they were aware of (Figure 1). Multiple answers were allowed for the responses. The most common subjective symptom was a decline in sleep quality, followed by decreased motivation and decreased concentration. Sexual function symptoms, such as decreased libido, reduced morning erections, and ED, were observed in approximately 60% to 80% of the patients. Hot flashes and sweating, which are common menopausal symptoms in women, were observed in only about 40% of the patients (Figure 1).
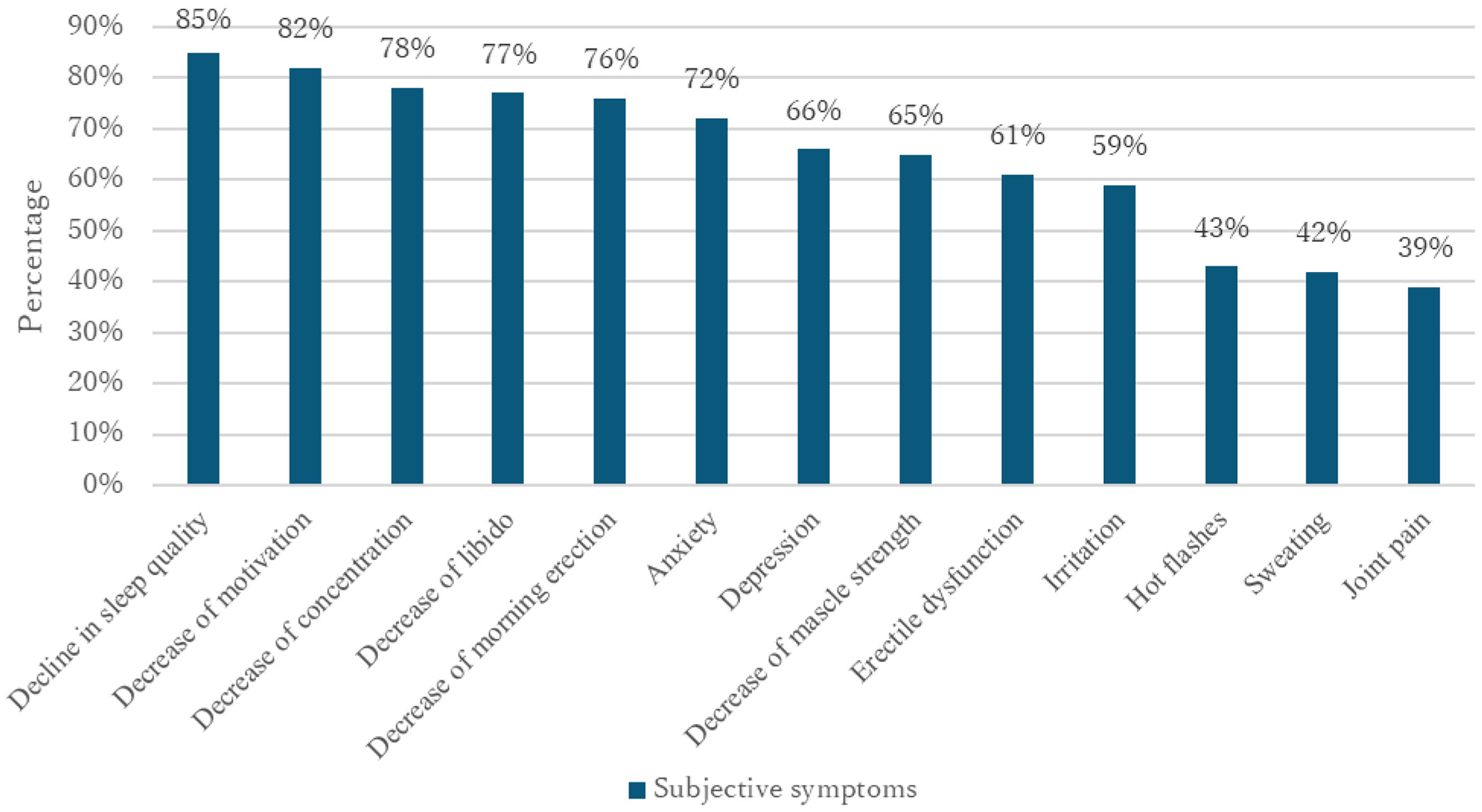
Percentage of Subjective Symptoms
Correlations Between AMS Score and Other Questionnaires
We found a significant correlation (p < .001) between the AMS score and WFun. AMS score positively correlates with WFun (Figure 2a). The effect size for this correlation was calculated as r = .62, indicating a moderate to strong association. Similarly, a significant correlation (p < .001) was also found between the AMS score and SHIM. AMS score negatively correlates with SHIM (Figure 2b). The effect size for this correlation was r = −.59, also suggesting a clinically meaningful relationship. No significant correlations were found between AMS scores and SDS, or AMS scores and PSQI.

(a) AMS Score and WFun. This Shows the Correlation Between the Total AMS Score and the Total WFun Score. “r” Represents the Correlation Coefficient, and “p” Indicates the Significance Probability. (b) AMS Score and SHIM. This Shows the Correlation Between the Total AMS Score and the Total SHIM
Relationship Between Symptoms and the Severity of WFun
The AMS score can be classified into three categories: physical symptoms (Questions 1–5, 9, 10), psychological symptoms (Questions 6–8, 11, 13), and sexual function symptoms (Questions 12, 14–17). In addition, WFun can be categorized into four levels: no problems, mild, moderate, and severe. An analysis of the severity of WFun and each AMS symptom revealed significant differences between severity levels (Table 2). As the severity of WFun worsens, the AMS scores for physical, mental, and sexual function also deteriorate. The symbols listed in the table indicate whether there are significant differences between severity levels. Notably, significant differences are particularly pronounced in the AMS scores for physical and mental functions, depending on the severity of WFun (Table 2).
Symptoms and WFun Severity

Note. AMS = Aging Males Symptoms; WFun = Work Functioning Impairment Scale;
p < .05 versus No.
p < .05 versus Mild.
p < .05 versus Moderate.
Specifically, AMS score questions 1, 4, 5, 6, 7, 8, 9, 10, 11, 12, and 13 are significantly associated with the four severity groups of WFun. In other words, symptoms such as a general decline in physical condition, insomnia, irritability, nervousness, anxiety, decreased motivation, fatigue, muscle weakness, depression, and a sense of helplessness were associated with the severity of WFun.
Discussion
Testosterone and Its Role in Energy, Vitality, and Workplace Productivity
Testosterone is essential for energy, vitality, and both physical and mental health. Its levels naturally decline with age, especially after 30 to 40 years. Chronic stress further accelerates this decline (Zitzmann, 2020). This decline is often associated with symptoms of LOH, such as fatigue, reduced libido, and mood disturbances—issues frequently observed in the workplace. Research suggests that these symptoms of testosterone deficiency may explain why middle-aged and older male workers are more prone to presenteeism, defined as attending work despite not being fully productive due to health issues (Bielecky et al., 2015). Low testosterone levels not only contribute to fatigue and reduced libido but are linked to mood disturbances such as depression and irritability (Schlich & Romanelli, 2016; Tenover, 1997). In fact, our study revealed that fatigue, mood disturbances, and irritability (Questions 1, 6, and 9 of the AMS score) are significantly associated with the severity of WFun.
Testosterone and Sleep Quality: Implications for Productivity
Sleep disorders are a prominent symptom of LOH and are closely associated with testosterone levels. Research in Japanese men has shown that testosterone levels positively correlate with sleep quality (Hirokawa et al., 2022). Similarly, studies by Agrawal et al. (2024) indicate that sleep disorders are linked to low testosterone levels and ED (Agrawal et al., 2024). Declines in sleep quality are the most commonly reported subjective symptom in men with LOH in this study and also questions 4 and 9 related to sleep quality are associated with the severity of WFun. There is growing evidence that sleep disorders directly impact presenteeism, and addressing these issues through medical interventions may contribute to improved workplace productivity (Furuichi et al., 2020; Tezuka et al., 2022).
Testosterone, Sexual Function, and Presenteeism
Our results are supported by prior findings, including Wu et al. (2010), who identified reduced morning erection, ED, and low libido as core symptoms of LOH. Testosterone deficiency is associated with reduced penile blood flow and decreased erectile function (Aversa et al., 2000; Petrone et al., 2003). Studies have shown that ED, a common symptom of LOH, correlates with AMS scores, which assess LOH symptoms (Molina-Vega et al., 2020). This study found that the worsening of sexual function symptoms is associated with WFun severity, and men with ED are reported to have significantly higher rates of presenteeism and reduced activity levels compared to those without ED, suggesting that sexual dysfunction can significantly impact workplace productivity (Goldstein et al., 2019).
Interestingly, no significant correlation was found between serum testosterone levels and presenteeism, as measured by the WFun score.
This suggests that subjective symptoms—such as fatigue, low motivation, and emotional instability—may play a more critical role in perceived work impairment than hormonal levels alone.
Previous studies have also noted that self-reported symptom severity often shows stronger associations with functional outcomes than do isolated biochemical values (Snyder et al., 2016; Wu et al., 2010).
These findings underscore the need for clinicians to evaluate patient-reported symptoms in addition to laboratory results when considering interventions for LOH.
The observed correlations between AMS scores and both WFun and SHIM were not only statistically significant but also demonstrated moderate to strong effect sizes.
These findings suggest that LOH-related symptoms, as assessed by the AMS, may have a substantial and clinically relevant impact on both work functioning and sexual health, further reinforcing the importance of early recognition and intervention.
The Broader Context: Aging, Comorbidities, and Presenteeism
Japan, with 28.7% of its population aged 65 and over, is one of the fastest-aging countries in the world. Employment among the elderly has also reached record highs, with individuals aged 65 and over comprising 13.3% of the workforce (Statistics Bureau, Ministry of Internal Affairs and Communications; https://www.stat.go.jp/data/handbook/index.html).
Serum testosterone is a biomarker that reflects multiorgan function (Shirakawa et al., 2024) and is a crucial factor in maintaining homeostasis in middle-aged and older men.
Chronic conditions associated with aging, such as metabolic syndrome, obesity, and cardiovascular disease, exacerbate fatigue, physical discomfort, and emotional distress, which further impair workplace performance.
Frailty, often linked to LOH, leads to declines in QOL due to cognitive impairment, depression, and reduced physical and sexual function. Ensuring healthy aging has become a critical social and medical issue, making the evaluation and management of LOH increasingly important. Strategies to address LOH-related presenteeism may include workplace wellness programs, lifestyle interventions, and TRT.
TRT can improve energy, mood, and QOL in men with LOH. These effects may help reduce presenteeism by improving work performance (Snyder et al., 2016). Improved motivation and job efficiency through TRT may prevent presenteeism, providing tangible benefits for both individuals and organizations. In addition, workplace wellness programs that incorporate health screenings for testosterone deficiency and related conditions could help identify employees at risk of presenteeism.
Although TRT is mentioned as a potential intervention to alleviate LOH-related presenteeism, it is important to emphasize that this study was observational and cross-sectional in nature.
Therefore, no causal conclusions can be drawn from our findings.
Further research using randomized controlled trials or longitudinal study designs is warranted to determine whether TRT can directly reduce presenteeism and improve work functioning in men with LOH.
Study Limitations and Future Directions
We acknowledge that a formal a priori power analysis was not conducted before initiating this study.
As this was an exploratory, cross-sectional study based on available clinical cases from a university hospital setting, we utilized all eligible patients during the designated study period (n = 96). For future studies, we plan to perform a priori sample size calculations based on the effect sizes observed in the current study to ensure adequate power for hypothesis testing. We acknowledge that conducting this study at a university hospital may introduce selection bias, as the patients included may not fully represent the broader working male population. In this study, the AMS score was used to measure the severity of LOH symptoms. While the AMS score has high sensitivity, its low specificity makes it less useful for diagnostic purposes. In addition, no significant correlations were observed between testosterone levels and the questionnaire results in this study. Increasing the sample size in future research may uncover new findings and provide further insights into the relationship between testosterone, presenteeism, and related symptoms.
Conclusions
Testosterone is essential for maintaining physical energy, cognitive function, and emotional stability, all of which are critical for optimal workplace performance. Low testosterone levels contribute to presenteeism through symptoms such as fatigue, mood disturbances, and reduced cognitive ability. Addressing testosterone deficiency through clinical interventions, lifestyle changes, and workplace wellness programs has the potential to mitigate presenteeism and improve productivity. Further research is needed to directly evaluate the impact of TRT on presenteeism metrics, enabling a more comprehensive understanding of its role in enhancing workplace efficiency. In addition to medical interventions such as TRT, workplace-based strategies should be considered.
These may include routine screening for testosterone deficiency among aging male workers, implementation of lifestyle modification programs (e.g., exercise, nutrition, and sleep), and access to mental health support.
Such comprehensive interventions may enhance employee well-being and productivity while reducing the burden of presenteeism associated with LOH.
Footnotes
Ethical Considerations
The present study protocol was reviewed and approved by the institutional review board of Juntendo University Hospital (Approval number: H22-0403). Informed consent was submitted by all subjects when they were enrolled.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Health Care Committee of Japan Society of Obstetrics and Gynecology and the Ministry of Health, Labour and Welfare, Japan (Grant number: 22FB1001).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The authors confirm that the data supporting the findings of this study are available within the article and its supplemental materials.
