Abstract
Men’s health has often been overlooked in health care, with traditional gender norms and societal expectations significantly shaping men’s health behaviors and attitudes. The MANifest Health Theory (MHT) offers a comprehensive framework to address cis-gender men’s unique health needs by considering the complex interplay of biological, psychological, and social factors. Rooted in four interconnected core concepts—Biopsychosocial Model, Health Optimization, Health Synchronicity, and Ethnocultural Expression—MHT provides a holistic understanding of men’s health. This article explores how MHT integrates inductive and deductive reasoning, describing, explaining, predicting, and controlling aspects of men’s health. Key components such as Gender-Sensitive Care, Health Empowerment, Supportive Environments, and Interdisciplinary Collaboration are discussed in relation to practical strategies for health care delivery. The limitations of MHT, including its developmental status, cultural applicability, and inclusivity of diverse gender identities, are acknowledged. Future steps for validating and refining the theory through empirical research, cultural adaptation, and inclusion of diverse gender experiences are outlined. By applying MHT, health care professionals can deliver more holistic and culturally competent care, promoting healthier lifestyles and reducing health care disparities among men.
Introduction
Men’s health is a critical but often overlooked aspect of health care. Traditional gender norms and societal expectations have shaped cis-gender men’s health behaviors and attitudes, influencing their willingness to seek care and adopt healthier lifestyles. Acknowledging the imperative need for a comprehensive framework to address men’s unique health needs while considering the complex interplay of biological, psychological, and social factors, the MANifest Health Theory (MHT) is proposed. This theory guides health care professionals, particularly nurses, in delivering holistic care, prioritizing cis-gender men’s health and well-being. MHT is rooted in four interconnected core concepts: the Biopsychosocial Model, Health Optimization, Health Synchronicity, and Ethnocultural Expression. These concepts collectively create a roadmap for understanding and addressing the multifaceted nature of men’s health.
The MHT incorporates elements of both inductive and deductive reasoning in its development. Inductive reasoning is evident as MHT draws from observations, research findings, and empirical evidence about men’s health. MHT recognizes real-world experiences and disparities that exist among men in health care. For example, epidemiological data show that men, on average, have higher mortality rates for various health conditions compared with women (Murphy et al., 2021; Smith et al., 2013). Studies indicate that men are less likely than women to seek regular medical check-ups and are more likely to delay seeking health care until their conditions become advanced (Courtenay, 2000; Mursa et al., 2022). Behavioral research involving surveys, interviews, and qualitative studies provides valuable insights into the factors influencing men’s health-related decisions, validating the real-world experiences that MHT seeks to address.
The MHT was developed in 2023, drawing from research findings and theoretical frameworks primarily from the late 20th and early 21st centuries. MHT integrates established theoretical frameworks to create a comprehensive approach tailored to men’s health, applying inductive and deductive reasoning. MHT integrates the Biopsychosocial Model, developed by George L. Engel in 1977, which posits that health and illness are products of biological, psychological, and social factors. This model emphasizes that to fully understand an individual’s health status, one must consider the complex interactions between these factors rather than focusing solely on biological symptoms (Engel, 1977).
MHT also incorporates the Gender-Sensitive Care approach by Margaret Miers, introduced in 2002. This approach underscores the importance of considering gender differences in health care, recognizing that societal and cultural norms about gender can significantly impact health behaviors and outcomes. Gender-sensitive care addresses these differences by providing tailored interventions that resonate with men’s specific health needs and experiences (Miers, 2002). In addition, MHT includes the Health Promotion Model (HPM) developed by Nola Pender in 1982. This model focuses on helping individuals achieve higher levels of well-being by encouraging health-promoting behaviors. The HPM assumes that people will take actions to improve their health if they believe the benefits outweigh the barriers, they feel capable of implementing the behaviors (self-efficacy), and they are supported by their environment and community (Aqtam & Darawwad, 2018; Pender, 2011).
The Mind-Body Medicine (MBM) framework, initially developed by Dr. Herbert Benson in the 1970s, emphasizes the connection between mental and physical health. This approach, combined with Tobias Esch’s BERN framework, highlights the physiological and psychological benefits of stress reduction techniques and holistic health practices. The MBM framework recognizes that psychological states can significantly influence physical health, advocating for integrated care approaches that address mental and physical health needs (Esch & Stefano, 2022).
Furthermore, MHT incorporates the concept of cultural humility described by Melanie Tervalon and Jann Murray-Garcia in 1998. Cultural humility involves self-reflection and self-critique, recognizing and challenging power imbalances in the patient-provider relationship, and developing mutually beneficial community partnerships. Cultural humility emphasizes the importance of understanding and respecting cultural differences in health care settings to provide effective and equitable care (Tervalon & Murray-Garcia, 1998). By synthesizing these frameworks, MHT creates a holistic and nuanced approach to men’s health, addressing the biological, psychological, social, gender-specific, cultural, and holistic dimensions of health. This comprehensive approach ensures that health care providers can develop more effective and personalized interventions, ultimately promoting better health outcomes for men.
Goals of Theory Development
MHT serves various goals associated with theory development, including describing, explaining, predicting, and controlling aspects of men’s health. In describing men’s health, MHT provides a comprehensive framework that outlines the various factors, behaviors, and dynamics that influence men’s health. MHT represents the interconnected nature of biological, psychological, social, and cultural factors and their impact on men’s well-being (Engel, 1977; Evans et al., 2011; Smith et al., 2013).
In explaining men’s health, MHT offers insights into why specific health disparities exist among men. The theory identifies and describes the influence of traditional gender norms, masculine identity, cultural diversity, and other factors on men’s health behaviors and outcomes (Courtenay, 2000; Mahalik et al., 2007; Wilfred, 2021). In predicting health outcomes, health care providers and researchers can use the insights provided by MHT to predict potential health outcomes or trends among specific groups of men. By understanding the impact of masculine health identity, health behavior change, supportive environments, and cultural competence, it becomes possible to make informed predictions about how interventions or changes in health care practices may influence men’s health behaviors and outcomes (Bandura, 1997; McGraw et al., 2021; Prochaska & DiClemente, 1982; Wilfred, 2021).
In controlling health disparities, MHT emphasizes the importance of cultural competence, tailored interventions, supportive environments, and interdisciplinary collaboration to improve men’s health outcomes. By implementing MHT-based strategies and interventions, health care providers can work toward reducing health care disparities and promoting healthier behaviors among men (Betancourt et al., 2003; Abualhaija, 2022; Reeves et al., 2017).
Several vital assumptions underpin the MHT framework in addressing men’s health. MHT assumes that health is not solely a physical state but a multidimensional concept encompassing biological, psychological, and social aspects (Engel, 1977; Galdas et al., 2023). Literature suggests societal norms, cultural beliefs, and traditional gender expectations significantly impact men’s health behaviors and attitudes (Courtenay, 2000; Reis de Sousa et al., 2023). The theory assumes that conventional notions of masculinity, characterized by emotional restraint and self-reliance traits, often discourage men from seeking help or discussing health concerns openly (Mahalik et al., 2007; Reis de Sousa et al., 2023). MHT assumes that behavior change is possible and that understanding the factors influencing health behavior change is crucial (Baldwin et al., 2022; Bandura, 1997). Betancourt et al. (2003) and Lindinger-Sternart (2015) mention that men come from diverse cultural backgrounds and that culture significantly influences health beliefs and practices.
MHT assumes a spiritual or existential dimension by recognizing that physical conditions do not solely determine men’s health but are also significantly influenced by their gender/sexual identities within societal and cultural norms (Kirmayer, 2012; Melder, 2023). MHT assumes that men’s health is multifaceted, requiring expertise from various health care disciplines (Abualhaija, 2022; Reeves et al., 2017). Men have unique health concerns influenced by their individual and gender identities (Nutbeam, 2000; Robertson & Kilvington-Dowd, 2019). MHT assumes that creating supportive health care settings and community environments is essential for reducing barriers to care and encouraging men to seek help and communicate openly about their health (Abualhaija, 2022; Schofield et al., 2016). The theory assumes that preventive care and patient education are fundamental to empowering individuals to make informed health choices (Glanz et al., 2008; Abualhaija, 2022). Finally, MHT assumes that by recognizing and addressing the factors that contribute to health care disparities among men, such as gender norms and delayed health care seeking, it is possible to bridge the gap and reduce these disparities in terms of morbidity and mortality (Robertson & Kilvington-Dowd, 2019; Truong et al., 2014).
Reasons for the Theory
Men’s health has often been overshadowed by the spotlight on women’s health issues. Research has shown that men are more likely to engage in risky behaviors, have higher mortality rates, and are less likely to seek medical care when needed (Abualhaija, 2022). These disparities stem from a complex interplay of biological, psychological, and social factors, including traditional gender norms that discourage men from expressing vulnerability or seeking help (Courtenay, 2000; Palmer et al., 2024). Research has consistently shown significant gender disparities in health outcomes. Men, on average, have a shorter life expectancy and a higher prevalence of certain health conditions, such as cardiovascular disease and specific types of cancer (Abualhaija, 2022). These disparities are influenced by complex interactions between gender roles, societal expectations, and health care utilization patterns (Palmer et al., 2024; Smith et al., 2013). Traditional notions of masculinity often discourage men from seeking help or discussing health concerns openly. The reluctance to appear vulnerable or weak can deter men from seeking timely medical care, resulting in delayed diagnoses and poorer health outcomes (Mahalik et al., 2007; Palmer et al., 2024). Health is a multidimensional concept encompassing physical, mental, and social well-being. While many existing theories focus primarily on physical health, MHT takes a more holistic approach. It recognizes that men’s health outcomes are shaped by biological, psychological, and social factors (Engel, 1977; Palmer et al., 2024).
One size does not fit all when it comes to health care interventions. Existing theories may not adequately account for men’s diverse needs and preferences from various backgrounds and cultures. MHT emphasizes cultural competence and tailoring health care to align with men’s health beliefs and values (Betancourt et al., 2003; Lindinger-Sternart 2015). The development and application of MHT aim to reduce health care disparities among men. By recognizing and addressing the factors contributing to these disparities, such as delayed health care seeking and adherence to unhealthy behaviors, MHT offers a roadmap for health care providers to bridge the gap (Abualhaija, 2022; Truong et al., 2014).
Definition of Masculinity
Masculinity, as framed by MHT, refers to the beliefs, attitudes, behaviors, and expectations traditionally associated with being a man within a specific cultural or societal context. This concept acknowledges that masculinity is not a static or universally defined trait but rather a dynamic construct influenced by cultural, social, and historical factors (Courtenay, 2000; Palmer et al., 2024). Critical components of masculinity framed by MHT may include characteristics such as emotional restraint, self-reliance, physical strength, and the avoidance of vulnerability or the expression of emotions perceived as “weakness.” These traditional notions of masculinity can influence how men perceive and approach their health and well-being (Mahalik et al., 2007; Oliffe, 2023).
In the context of MHT, masculine health identity refers to the unique and individualized health concerns, behaviors, and attitudes that are influenced by a person’s gender identity and societal expectations of masculinity. Oliffe (2023) recognizes that men, based on their gender identity and the cultural norms associated with masculinity, may have specific health needs and approaches to health care. Masculine health identity encompasses several vital aspects. Traditional notions of masculinity may influence men’s beliefs and perceptions about health, such as self-reliance, emotional restraint, and the avoidance of vulnerability (Courtenay, 2000; Oliffe, 2023). Masculine health identity acknowledges that men may be less inclined to seek medical care or openly discuss health concerns due to societal expectations (Mahalik et al., 2007; Palmer et al., 2024). MHT recognizes that men’s health concerns are not uniform but can vary based on their unique experiences, lifestyles, and values. Masculine health identity encourages men to explore and understand their individual health needs within the context of their gender identity (Courtenay, 2000; Palmer et al., 2024). Effective health care interventions should consider how they align with men’s masculine values and identities. This may involve tailoring health care approaches to resonate with men’s beliefs and expectations (Mahalik et al., 2007; Abualhaija, 2022).
Core Concepts
The core concepts of MHT include the Biopsychosocial Model, Health Optimization, Health Synchronicity, and Ethnocultural Expression. Each concept is crucial in holistically understanding men’s health (see Figure 1). The Biopsychosocial Model posits that health and illness are products of biological, psychological, and social factors (Engel, 1977). This model integrates physical health, mental health, and social well-being. Wade and Halligan (2017) and Palmer et al. (2024), emphasize a holistic approach to health, recognizing that men’s health can only be fully understood by considering the interplay of these factors. Health care providers use this model to assess and treat patients by considering all three dimensions of health rather than focusing solely on biological symptoms (Leone et al., 2021; Smith et al., 2013).
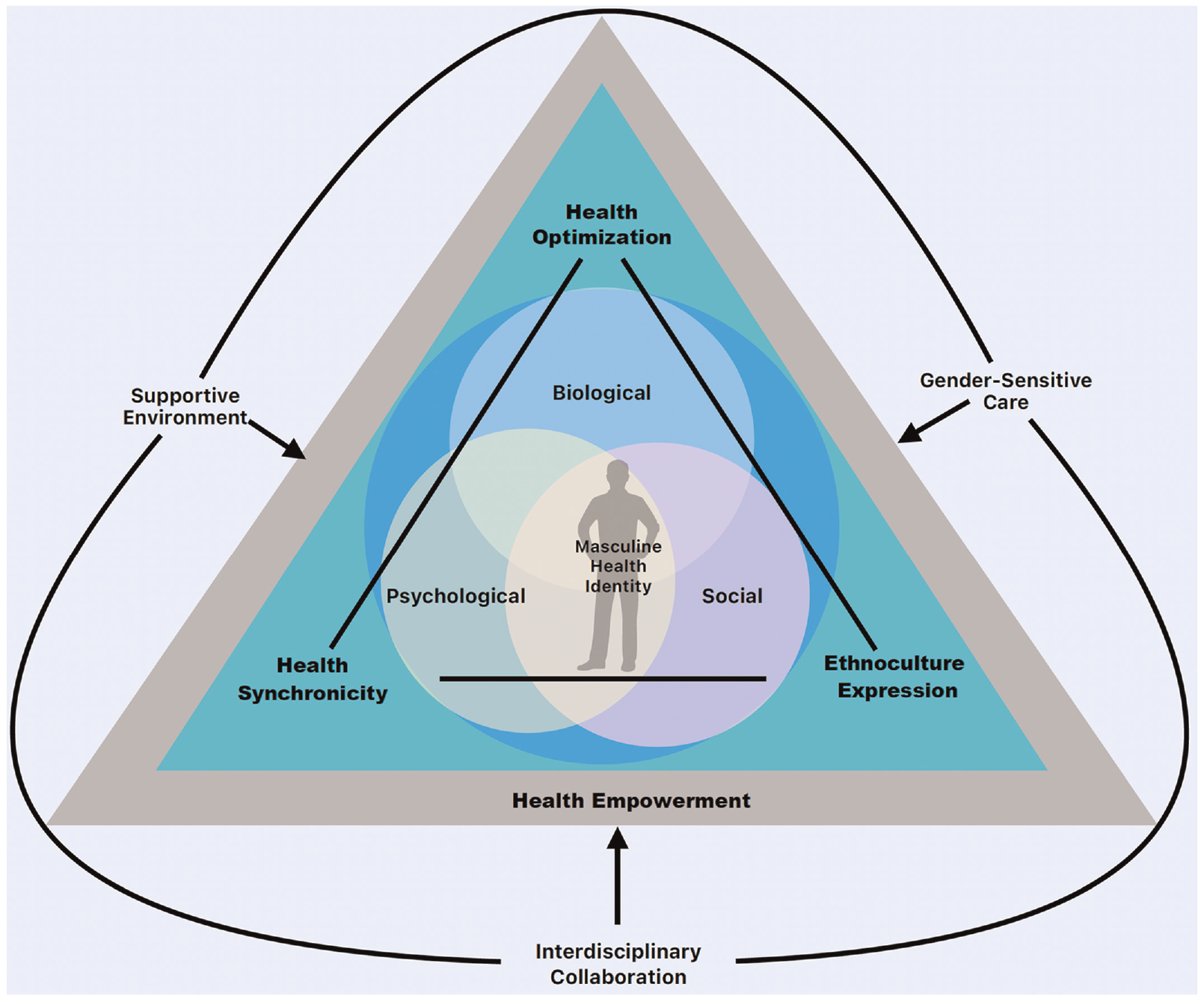
The MANifest Health Model
Health Optimization improves health outcomes through strategic health behavior changes and maintenance (Hayman, 2022; Prochaska & DiClemente, 1982). This involves health promotion, disease prevention, and health maintenance. Health Optimization highlights the importance of proactive health measures and the role of behavior change in achieving optimal health outcomes (Glanz et al., 2008; Hayman, 2022). Interventions and programs are designed to encourage and support men in adopting healthier lifestyles, including regular physical activity, balanced nutrition, and routine medical check-ups (Hayman, 2022; Koh et al., 2010).
Health Synchronicity is the seamless integration and interdependence of mental, emotional, and physical health. MHT acknowledges the continuous interaction between different health aspects, where changes in one area can significantly impact the others. Health Synchronicity promotes the understanding that mental and physical health are deeply interconnected, requiring integrated care approaches (Groeneveld et al., 2013; Parent & Sánchez, 2019). Health care strategies and interventions are developed to address psychological and physical health simultaneously, ensuring a comprehensive approach to treatment and care (Bishop et al., 2014; Parent & Sánchez, 2019).
Ethnocultural Expression refers to the influence of cultural and ethnic identity on health beliefs and practices. Stubbe (2020) recognizes the diversity of health behaviors and perceptions influenced by cultural values and traditions. This concept ensures that health care is culturally competent, respectful, and tailored to men’s diverse backgrounds and values (Stubbe, 2020; Truong et al., 2014). Health care providers are trained to deliver culturally sensitive care, acknowledging and incorporating the cultural context of each patient in their treatment plans (Kirmayer, 2012; Stubbe, 2020).
Key Components
The critical components of MHT are Gender-Sensitive Care, Health Empowerment, Supportive Environments, and Interdisciplinary Collaboration. These components translate the core concepts into practical strategies for health care delivery.
Gender-sensitive care involves tailoring health care to meet the specific health needs of men, considering the influence of traditional gender norms and societal expectations (Courtenay, 2000; Friend & Alden, 2024). This component focuses on men’s unique experiences and challenges in health care settings. Gender-sensitive care addresses the barriers created by traditional notions of masculinity, which often discourage men from seeking help or discussing health concerns openly (Mahalik et al., 2007; Friend & Alden, 2024). Developing health care interventions and communication strategies that resonate with men’s health beliefs and values can make engaging in health-promoting behaviors easier (Galdas et al., 2023; Yousaf et al., 2015).
Health Empowerment provides men with the knowledge and tools to make informed health choices and take control of their health. This component emphasizes education, prevention, and self-management (Friend & Alden, 2024; Nutbeam, 2000). Health Empowerment encourages proactive health-seeking behaviors and fosters a sense of agency and responsibility in managing one’s health (Bandura, 1997; Friend & Alden, 2024). Creating educational programs and resources that empower men to understand their health risks and adopt healthier lifestyles is a crucial application of this component (Friend & Alden, 2024; Galdas et al., 2023; Glanz et al., 2008).
Supportive Environments refer to creating health care settings and community environments that encourage men to seek care and communicate openly about their health. This component focuses on reducing stigma and barriers to care (Galdas et al., 2023; Wang et al., 2017). Supportive Environments ensure that men feel comfortable and supported when accessing health care services, promoting better health outcomes (Galdas et al., 2023; Smith et al., 2013). Designing health care facilities and community programs that provide a welcoming and non-judgmental atmosphere for men is essential (Friend & Alden, 2024; Schofield et al., 2016).
Interdisciplinary Collaboration encourages teamwork among health care providers from various disciplines to deliver holistic care for men. This component involves collaboration between physicians, psychologists, social workers, and other health care professionals (Bookey-Bassett et al., 2022; Reeves et al., 2017). Interdisciplinary Collaboration ensures a comprehensive approach to men’s health, addressing physical and psychological aspects (Bookey-Bassett et al, 2022; Sturmberg & Martin, 2013). Developing integrated care plans and collaborative treatment approaches that draw on the expertise of multiple health care professionals is a practical application of this component (Bookey-Bassett et al., 2022; Mitchell et al., 2012).
Interconnectedness of Core Concepts and Key Components
The core concepts and critical components of MHT are interconnected, each supporting and enhancing the others to provide a comprehensive approach to men’s health. The Biopsychosocial Model provides the theoretical foundation for Gender-Sensitive Care by emphasizing the need to consider the biological, psychological, and social factors that influence men’s health. Gender-sensitive care translates this model into practice by addressing how societal norms and gender expectations impact men’s health behaviors and attitudes (Courtenay, 2000; Engel, 1977; Stone, 2020).
Health optimization focuses on improving health outcomes through behavior change and maintenance, closely tied to health empowerment through education and promotion. Empowering men with the knowledge and tools necessary for behavior change is essential for optimizing their health (Bandura, 1997; Hayman, 2022; Prochaska & DiClemente, 1982). Health Synchronicity emphasizes the interconnectedness of mental, emotional, and physical health. Supportive Environments facilitate this interconnectedness by creating spaces where men feel comfortable discussing and addressing both their psychological and physical health needs (Friend & Alden, 2024; Groeneveld et al., 2013; Wang et al., 2017). Ethnocultural Expression recognizes the impact of cultural and ethnic backgrounds on health behaviors and perceptions. Interdisciplinary Collaboration is essential for providing culturally competent care, ensuring that health care strategies are sensitive to the diverse needs of men from different cultural backgrounds (Betancourt et al., 2003; Bookey-Bassett et al., 2022; Reeves et al., 2017).
Discussion
The MANifest Health Theory (MHT) represents a groundbreaking and all-encompassing framework designed to comprehend men’s health concerns and address them thoroughly. This innovative theory intertwines the Biopsychosocial Model, Health Optimization, Health Synchronicity, and Ethnocultural Expression, offering a holistic approach that fully recognizes the multifaceted nature of men’s health. This comprehensive examination thoroughly compares MHT to other well-established health theories, shedding light on its distinct contributions and potential avenues for enhancement.
Strengths and Limitations of the Theory
The MANifest Health Theory (MHT) possesses several strengths that make it a valuable framework for addressing men’s health. One of its primary strengths is its holistic and integrative approach, combining elements from various theories and models to create a comprehensive framework that addresses men’s health’s biological, psychological, and social dimensions. This integrative approach enables health care providers to develop more effective and tailored interventions by considering the complex interplay of factors influencing men’s health behaviors and outcomes.
Another strength of MHT is its emphasis on cultural competence. The theory promotes culturally competent care by recognizing the diversity of men’s health experiences and the influence of cultural and societal norms. This focus is essential for addressing health disparities and improving health outcomes among men from diverse backgrounds. In addition, MHT includes the concept of gender-sensitive care, which involves tailoring health care to meet the specific health needs of men while considering the influence of traditional gender norms and societal expectations. This component addresses the barriers created by conventional notions of masculinity, which often discourage men from seeking help or discussing health concerns openly.
Furthermore, MHT emphasizes the creation of supportive health care settings and community environments that encourage men to seek care and communicate openly about their health. By reducing stigma and barriers to care, this approach promotes better health outcomes by ensuring that men feel comfortable and supported when accessing health care services.
Despite its strengths, the MANifest Health Theory also has some limitations. One significant limitation is its developmental status. As a work in progress, the concepts and components of MHT require further refinement and validation through empirical research. This ongoing development means the theory may not be fully robust or universally applicable.
Another limitation is the theory’s cultural applicability. MHT may not fully capture the complexity and diversity of men’s health experiences across different cultures and socioeconomic backgrounds. More research is needed to explore its applicability in various cultural contexts and to adapt the theory to address the unique health needs of diverse cultural groups.
Moreover, while MHT focuses on cis-gender men, it may overlook the experiences of men who do not conform to traditional gender norms, including transgender and non-binary individuals. Expanding the theory to include these experiences is necessary to ensure it is inclusive and relevant to all men. Finally, the practical application of MHT in clinical settings may face challenges due to varying levels of cultural humility and interdisciplinary collaboration among health care providers. Ensuring that health care providers are adequately trained and capable of implementing MHT-based strategies is crucial for the theory’s success.
Next Steps for Validation of the Theory
To validate and refine MHT, the following steps are recommended: conducting empirical studies to test the core concepts and critical components of MHT in diverse populations and settings to establish the reliability and validity of the theory; exploring the applicability of MHT across different cultural contexts and adapting the theory better to address the unique health needs of diverse cultural groups; expanding MHT to include the experiences of transgender and non-binary individuals, ensuring that the theory is inclusive and relevant to all men; developing training programs to enhance the cultural competence and interdisciplinary collaboration skills of health care providers, facilitating the practical implementation of MHT in clinical settings; and conducting longitudinal studies to examine the long-term impact of MHT-based interventions on men’s health outcomes.
Conclusion
The MANifest Health Theory (MHT) offers a comprehensive framework for addressing men’s health needs by recognizing the interconnectedness of biological, psychological, and social factors and considering the influence of gender norms and cultural diversity. By applying MHT, health care professionals can deliver holistic care that respects men’s identities and values, promotes healthier lifestyles, and reduces health care disparities among men. However, as a work in progress, MHT requires further research and refinement to realize its full potential. This concept analysis clarifies the core concepts and critical components of MHT, providing a foundation for further study and practical application in health care settings.
Footnotes
Acknowledgements
I would like to thank Dr. Karen Foli for providing guidance in developing this theory.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
