Abstract
Male first responders face high occupational stress and health risks, influenced by structural barriers and masculine norms. This cross-sectional study examined men’s health knowledge, perceived barriers to care, traditional masculinity norms, and health behaviors among 102 male first responders. Descriptive statistics were computed, and nonparametric tests and Spearman correlations evaluated associations with key outcomes, including omission of pertinent health information during clinical encounters. Scale reliability was strong (men’s health knowledge α = 0.92; barriers α = 0.77; masculinity norms α = 0.78). Mean age was 44.9 years (SD 13.5); mean BMI was 30.8 (SD 5.6, n = 84), with 53.6% classified as obese/severely obese. A total of 22.0% (n = 91) endorsed Yes/Maybe to having omitted pertinent health information from a provider. Men endorsing omission reported higher overall barriers (Mann–Whitney, p = .0268, r = .325), driven by lack of time (pFDR = .0055, r = .453) and limited awareness of services (pFDR = .0467, r = .332). Traditional masculinity norms differed by occupation (Kruskal–Wallis, p = .00211, ε2 = .117), with police scoring higher than firefighters and EMS. Provider satisfaction was inversely associated with barriers (ρ = −.273, pFDR = .0206) and masculinity norms (ρ = −.295, pFDR = .0142). Diet and exercise correlated positively with self-rated health and body image, whereas BMI correlated negatively. Findings support MANifest Health Theory: selective disclosure is shaped by “maintenance friction” (time/awareness barriers) interacting with masculinity-aligned identity needs. Interventions reducing access friction and framing care as readiness maintenance may improve disclosure.
Keywords
Introduction
First responders, including firefighters, police officers, and emergency medical services (EMS) professionals, face a unique constellation of occupational stressors that place them at elevated risk of a wide range of mental and physical health concerns (Substance Abuse and Mental Health Services Administration, 2018; Tiesman et al., 2021). Daily, these individuals are confronted with traumatic events, unpredictable hazards, and high-pressure decision-making environments, all of which can have profound effects on psychological well-being and long-term physical health. Exposure to traumatic incidents is known to increase the likelihood of depression, anxiety, substance use, post-traumatic stress disorder (PTSD), and cardiovascular disease among first responder populations. Despite these well-documented risks, there remains a persistent pattern of underutilization of health care services by male first responders (O’Dare et al., 2024).
Multiple intersecting factors contribute to this underutilization. Cultural expectations within first responder communities often promote resilience, toughness, and an ethos of self-reliance, discouraging expressions of vulnerability or emotional distress (Heward et al., 2024; Odom, 2021). These occupational norms are further reinforced by broader societal beliefs about masculinity, specifically, traditional masculinity ideology, which values stoicism, independence, and physical strength (Odom, 2021). For many men in these roles, acknowledging health concerns or seeking help may be perceived as a sign of weakness or a threat to their professional identity. This can create significant barriers to open communication with health care providers, delay preventive care, and result in poorer health outcomes.
Systemic barriers also play a role. Shift work, long hours, and the unpredictable nature of emergency response can limit opportunities to seek care, while concerns about confidentiality or potential impacts on job security may further discourage disclosure of health issues (O’Dare et al., 2024; Smetana, 2024). These cultural, systemic, and gender-related influences interact in complex ways, shaping the health behaviors and attitudes of male first responders (O’Dare et al., 2024). Understanding how these factors intersect is critical for designing effective interventions and improving health engagement within this vital workforce.
Literature Review
Research consistently demonstrates that men, especially those in high-risk or hyper-masculine professions, are less likely to seek preventive or mental health care, leading to higher rates of unaddressed morbidity and mortality (Baker et al., 2017; Courtenay, 2000). The gender gap in health engagement is attributed to socialized masculine norms that valorize endurance, emotional control, and autonomy (Addis & Mahalik, 2003). Such norms can foster a reluctance to disclose vulnerabilities, whether physical or psychological, with studies showing that men are more likely than women to delay seeking help even for serious symptoms (Tannenbaum & Frank, 2011). For first responders, these issues are compounded by occupational cultures that prioritize operational readiness and the suppression of emotional expression, which can further discourage care-seeking and open dialogue with health care providers (Smith et al., 2019).
The Male Role Norms Inventory–Short Form (MRNI-SF) conceptualizes traditional masculinity as a multidimensional construct, encompassing norms such as emotional restriction, self-reliance, and dominance, each with distinct implications for health behavior (Levant et al., 2013). Evidence suggests these dimensions do not operate uniformly; men’s discomfort with counter-stereotypical behaviors varies by specific masculinity endorsements and perceptions of gender norm change (Borinca et al., 2021).
Occupational identity shapes how masculinity is expressed within first responder roles, influencing patterns of health disclosure and engagement. Policing is often characterized by a militarized ethos that reinforces toughness and emotional control, whereas EMS work emphasizes relational competence and caregiving, potentially allowing greater openness to help-seeking (Courtenay, 2000; Smith et al., 2019). Cross-national research shows these masculinity-health mechanisms extend beyond the United States; masculine norms similarly shape men’s health behaviors across cultures, with anticipated sexual misclassification identified as a key psychological mechanism underlying avoidance of vulnerable care-seeking (Borinca et al., 2021; Gough & Novikova, 2020). Interventions that explicitly address these differentiated masculine norms, including gender-sensitive education and male-focused support strategies, have demonstrated potential to improve men’s health engagement (Borinca & Gkinopoulos, 2025; Robertson et al., 2015). Notably, exposure to alternative masculine role models and minority norms can reduce endorsement of traditional masculinity, highlighting the malleability of gender norms for intervention design (Borinca & Gkinopoulos, 2025).
This study was guided by the MANifest Health Theory (Gallegos, 2024), a conceptual framework developed to explore how masculine identity influences health engagement, particularly in populations like male first responders. The theory posits that traditional masculinity norms, such as emotional suppression, toughness, and reluctance to show vulnerability, can significantly shape men’s willingness to seek health care, especially for sensitive issues like mental health or sexual health. MANifest Health Theory integrates concepts of masculinity, cultural context, and health behavior to explain how men’s health decisions are made within the constraints and expectations of masculine identity. MANifest Health Theory builds upon established masculinity and health behavior frameworks, extending them to occupationally masculine contexts such as first responder work. Figure 1 illustrates the MANifest Health Theory pathway to health engagement among first responders.

MANifest Health Theory Pathway for Health care Engagement and Selective Disclosure Among Male First Responders
Study Aims
Aim 1: Describe sample demographics, health indicators, and distributions of men’s health knowledge, perceived barriers, masculinity norms, and provider relationship satisfaction.
Aim 2: Estimate prevalence of selective disclosure and test whether selective disclosure is associated with barriers to care and provider satisfaction.
Aim 3: Evaluate whether masculinity norms vary by occupational role and relate to barriers and provider satisfaction.
Aim 4: Explore associations among diet, exercise, BMI, self-rated health, and body image satisfaction in alignment with MANifest Health Theory’s readiness/maintenance framing.
Methods
Design and Setting
A quantitative cross-sectional design was employed to recruit participants residing in rural, suburban, and urban communities across the United States.
Inclusion and Exclusion Criteria
Inclusion criteria required participants to identify as male, be 18 years of age or older, reside in the United States, and currently or previously serve as a first responder (firefighter, law enforcement officer, EMS professional, or related public safety role). Exclusion criteria included non-male gender identity or inability to read English, as the survey was only available in English. Including multiple first responder roles enabled examination of how occupational subcultures differentially shape masculinity norms and health care engagement, strengthening interpretive depth rather than diluting specificity.
Sampling and Participants
Recruitment was conducted using a non-probability approach that combined convenience and snowball sampling techniques. Most of the flyers were shared through email distribution lists, professional first responder networks, and social media platforms linked to public safety groups. Other flyers were distributed in person to readily accessible participants, while social media platforms were used to facilitate snowball recruitment (snowball effect) by encouraging participants to share the study information with colleagues. These strategies were well suited for reaching first responders, a population that can be difficult to access (Frazer et al., 2021). Participants self-identified their occupational role (firefighter, police, EMS, other). The sample size of this study comprises of male first responders (N = 102).
Procedure for Data Collection
Data collection occurred between June and August 2025 using a de-identified survey dataset following institutional review board (IRB) approval. The authors conducted in-person recruitment visits to police, fire, and emergency medical services (EMS) departments, where flyers were distributed after explaining the study’s purpose and potential benefits. In some departments, organizational leaders approved the posting of flyers on physical notice boards and shared the study information through internal online platforms. Interested participants completed the survey using X Qualtrics platform. Survey completion required approximately 15–30 minutes on average. Participation was voluntary, anonymous, and were offered to be enrolled in a giveaway of a gift card if selected.
Measures
Data were collected using a custom Qualtrics survey composed of both original items and adapted, validated scales. Participants spent an average of 20 minutes completing the survey. The entire data-collection process took place over a period of 2 years (2023–2025). Of the total 220 participants who initially responded, 118 surveys were not completed, resulting in a final sample of 102 male first responders.
The survey included demographics, health indicators (height/weight for BMI), health behaviors (exercise frequency and modality; diet self-rating; alcohol, tobacco, and performance-enhancing drug use), and health care engagement variables (primary care provider type; provider relationship satisfaction, 1–5 scale; and an item assessing whether the participant had omitted pertinent health information from a provider [No/Yes/Maybe]). Composite scales were constructed for (a) men’s health knowledge (nine items), (b) health care access barriers (five items), and (c) traditional masculinity norms (five items). Higher scores indicated greater endorsement.
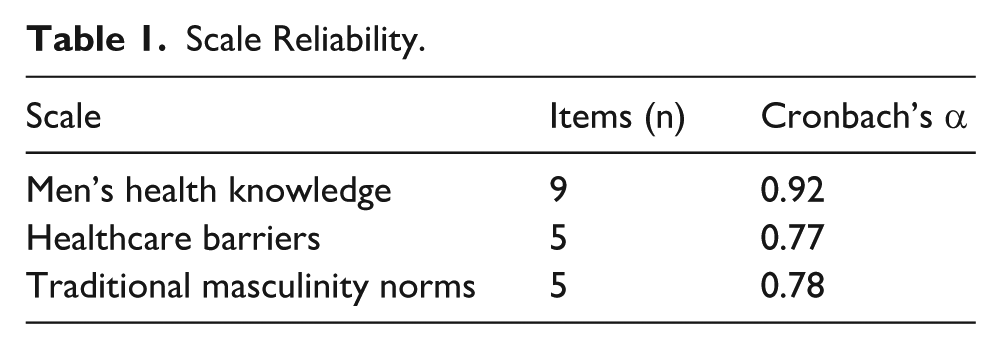
Scale Reliability
Internal consistency was excellent for men’s health knowledge (α = 0.92) and acceptable-to-good for barriers (α = 0.77) and masculinity norms (α = 0.78; Table 1).
Scale Reliability.
Ethical Considerations
The study was approved by Purdue University Institutional Review Board (IRB-2023-1835) on 2/25/2025. Participants provided informed consent electronically before accessing the survey. No identifying information was collected, and all responses were stored on encrypted, password-protected university servers.
Statistical Analysis
Descriptive statistics summarized the sample. Internal consistency was evaluated with Cronbach’s alpha. Given ordinal Likert-type responses and evidence of non-normality, group comparisons used Mann–Whitney U tests (two groups) and Kruskal–Wallis tests (≥3 groups) with effect sizes (rank-biserial r; epsilon-squared ε2). Associations were assessed with Spearman correlations. Within families of related tests, p-values were adjusted using the Benjamini–Hochberg false discovery rate (FDR). Analyses were conducted using Python.
Results
Demographics
Participant characteristics and behaviors are presented in Table 2. Mean age was 44.94 years (SD 13.47). Roles were predominantly firefighter (59.8%), followed by police (19.6%), EMS (9.8%), and other (10.8%). Residence was rural (48.0%), suburban (42.2%), and urban (9.8%).
Participant Characteristics and Key Indicators.

Health Indicators
Among those with complete self-reported anthropometric data (n = 84), mean BMI was 30.78 (SD 5.63), with 11.9% in the normal range, 34.5% overweight, 48.8% obese, and 4.8% severely obese. Exercise frequency averaged 3.15 days/week (SD 1.58; n = 89). Diet self-rating (n = 91) was good (36.3%), average (41.8%), and poor (22.0%). Alcohol use was endorsed by 62.6% (n = 91); tobacco and performance-enhancing drug use were each endorsed by 8.8%.
Selective Disclosure
Among respondents completing the omission item (n = 91), 22.0% endorsed Yes/Maybe. Men endorsing Yes/Maybe reported higher overall barriers than those endorsing No (p = .0268, r = .325). Barrier item analyses (FDR-adjusted) indicated higher endorsement of lack of time (pFDR = .0055, r = .453) and limited awareness of services (pFDR = .0467, r = .332) among those endorsing Yes/Maybe (Table 3).
Significant Inferential Findings.

Note. FDR = Benjamini–Hochberg false discovery rate adjustment within test families.
Masculinity Norms by Occupation
Traditional masculinity norms differed by occupation (H(2) = 12.32, p = .00211, ε2 = .117). Post hoc testing (FDR-adjusted) showed police endorsed higher norms than firefighters (pFDR = .00322) and EMS (pFDR = .0188).
Provider Satisfaction
Provider relationship satisfaction correlated negatively with barriers (ρ = −.273, pFDR = .0206) and masculinity norms (ρ = −.295, pFDR = .0142).
Rurality
Lack of time as a barrier differed by residence (p = .0282); rural respondents endorsed lack of time more strongly than urban respondents (pFDR = .0119).
Lifestyle Correlates
Diet and exercise were positively associated with self-rated health and body image satisfaction, whereas BMI was negatively associated. Key correlations were: diet with self-rated health (ρ = .547, pFDR < .001) and body image (ρ = .454, pFDR < .001); exercise days with self-rated health (ρ = .452, pFDR < .001) and body image (ρ = .485, pFDR < .001); BMI with body image (ρ = −.372, pFDR = .00210) and self-rated health (ρ = −.255, pFDR = .0222). Aerobic exercise and strength training were each associated with higher body image satisfaction (p = .00186 and p = .0158, respectively).
Discussion
This study extends prior masculinity and help-seeking research by identifying selective nondisclosure, not avoidance of care, as a critical and underrecognized mechanism shaping men’s health engagement in first responders. Using a MANifest Health Theory lens, the current findings suggest that health care engagement among male first responders is shaped by the intersection of identity, occupational expectations, and structural constraints. Consistent with scoping and exploratory applications of theory, this cross-sectional design was intended to examine whether observed patterns align with MANifest Health Theory constructs rather than to test causal pathways. Approximately one in five respondents (22%) reported selective nondisclosure to a clinician, and nondisclosure was most strongly linked to practical barriers (especially lack of time) and limited awareness of services, rather than demographic factors alone. These findings reinforce that men’s health care behavior is rarely explained by a single determinant; rather, it reflects a “readiness-maintenance” calculus in which health behavior must compete with role demands and masculine performance expectations.
Selective Nondisclosure as an Identity-Protective Strategy
Selective disclosure is increasingly recognized as common across health care settings. In a national U.S. sample, many patients reported withholding medically relevant information due to embarrassment, fear of judgment, or concern about how the clinician would respond (Levy et al., 2018). In first responder populations, these general mechanisms can be intensified by occupational stigma, fear of “appearing weak,” and concerns that disclosure may trigger consequences (e.g., fitness-for-duty evaluations, perceived career vulnerability), which aligns with evidence describing stigma-related barriers in first responders (Haugen et al., 2017). Within MANifest Health Theory, nondisclosure can be conceptualized as an adaptive, identity-protective maneuver, a way to preserve perceived competence, toughness, and readiness when health concerns might threaten one’s masculine self-appraisal or occupational identity (Gallegos, 2024).
Importantly, nondisclosure is also shaped by relational trust. Research shows that people who experience lower trust in health systems or perceive discrimination may be more likely to withhold information (Nong et al., 2022). In the context of first responders, this supports the idea that provider relationship quality is not merely “patient satisfaction” but a disclosure-enabling condition. Although provider satisfaction was inversely associated with both barriers and masculinity norms, selective disclosure clustered most strongly with structural barriers, suggesting nondisclosure is not reducible to dissatisfaction alone.
Masculinity Norms Vary by Role and May Influence Engagement
Traditional masculinity norms differed significantly across roles, with police respondents endorsing higher norms than firefighters and EMS. This aligns with gender-and-health scholarship demonstrating that hegemonic masculine expectations (stoicism, emotional restriction, self-reliance) shape health behavior and often discourage disclosure or help-seeking (Courtenay, 2000). Addis and Mahalik’s framework further explains that men frequently evaluate health-seeking through “masculinity-compatibility,” weighing whether help-seeking threatens or supports masculine identity (Addis & Mahalik, 2003). Reviews of masculinity and help-seeking have repeatedly found that stronger conformity to masculine norms is associated with lower likelihood of help-seeking, particularly for emotional or stigmatized concerns (Seidler et al., 2016).
From a MANifest perspective, occupationally reinforced masculinity norms (especially in policing cultures) may heighten the tendency to treat health as “maintenance only, when necessary,” and disclosure as something to minimize unless it clearly supports role performance. Masculinity norms did not operate independently but interacted with structural barriers such as time and access, supporting a multilevel interpretation rather than a purely identity-driven explanation.
Time Barriers and Rural Constraints as Structural Impediments
Time constraints emerged as a key barrier and appeared stronger among rural respondents. Rural health care access is commonly limited by workforce shortages, travel distance, fewer clinic hours, and competing work demands (Douthit et al., 2015). For first responders, shift schedules and overtime may exacerbate these limitations, producing a “care-access mismatch” that reinforces delayed preventive care. This is consequential because shift work and irregular schedules are also linked to adverse cardiometabolic outcomes across populations (Wu et al., 2022), meaning that the same occupational conditions that reduce access may also increase risk.
Lifestyle and Readiness: Prevention Framed as Performance
The sample showed elevated BMI patterns (mean BMI in the obese range; nearly half obese), consistent with firefighter cohort research documenting high prevalence of overweight/obesity (Poston et al., 2011). Strong associations between diet/exercise and self-rated health and body image satisfaction suggest that men may already perceive health behaviors through “performance” and “fitness” lenses. MANifest Health Theory uniquely supports leveraging this: if men view care as a readiness behavior rather than a vulnerability admission, engagement may increase (Gallegos, 2024). In practice, framing prevention as “routine maintenance” and “operational readiness checks” may reduce identity friction and increase disclosure. Lifestyle associations were examined to contextualize health engagement within a readiness and maintenance framework, reinforcing how physical self-perception may shape disclosure and care-seeking behavior.
Implications for Practice
The findings of this study carry several critical implications for improving health care delivery and engagement among male first responders. First, health care systems must adopt culturally responsive, gender-sensitive, and trauma-informed approaches that recognize how masculine norms and occupational culture influence health behaviors. Providers should be trained to create environments that encourage vulnerability and disclosure without fear of judgment or professional consequences, especially in areas like mental health, which remain stigmatized in this population.
Second, structural barriers such as cost, time, and distance were more frequently cited than relational factors like provider gender or service availability. This underscores the need for system-level interventions, such as mobile health units, on-site occupational health clinics, flexible scheduling, and telehealth, particularly for time-constrained and high-demand roles like firefighting. Health policies and employer practices must be aligned to ensure these men can access timely and comprehensive care without compromising their responsibilities or privacy.
Finally, the study supports the integration of masculinity-informed frameworks, such as the MANifest Health Theory, into both research and practice. Tailored interventions that frame help-seeking as a form of strength and resilience, rather than weakness, may be more effective in shifting attitudes and behaviors. Addressing workplace stigma, protecting confidentiality, and embedding peer support networks into emergency services can foster a more open and supportive culture around health, especially mental health, for male first responders.
Limitations
Limitations include the cross-sectional design, subgroup sample size constraints (e.g., EMS, urban), reliance on self-report, and item missingness that reduced analytic denominators. Future research should test longitudinal pathways predicted by MANifest Health Theory (masculinity norms + friction → selective disclosure → downstream outcomes) and evaluate pragmatic, department-embedded interventions designed to reduce friction and increase identity congruence. Selective disclosure was assessed using a single pragmatic item designed to capture clinically meaningful omission behavior. While this approach limits granularity, it reflects real-world screening questions used in patient–provider communication research. While self-selection and item missingness limit population-level inference, the use of nonparametric tests, effect sizes, and FDR correction supports internal validity and pattern detection appropriate for exploratory men’s health research.
While snowballing and convenience methods risk selection bias by engaging those more open to health research, efforts to promote snowball recruitment aimed to reach more reluctant individuals through trusted peer networks, helping to mitigate this limitation.
Conclusion
Male first responders in this study demonstrated meaningful barriers to preventive health care engagement, including elevated BMI patterns and a substantial rate of selective nondisclosure to clinicians. Nondisclosure clustered most strongly with practical barriers especially lack of time and limited awareness of services highlighting that engagement problems are not solely motivational but also structural.
Viewed through MANifest Health Theory, nondisclosure may represent an identity-protective strategy rooted in occupational readiness culture and masculinity expectations. Differences in masculinity norms across occupational groups further suggest that interventions must be role-sensitive, and provider strategies should emphasize identity-congruent framing (“maintenance,” “readiness,” “operational performance”) while strengthening trust and confidentiality.
Ultimately, improving men’s health engagement in first responders will require multi-level solutions: clinician communication changes, structural access improvements (especially for rural/shift workers), and organizational policies that reduce stigma-based fears and support preventive care as a component of readiness and longevity. Interventions that reduce access friction and frame preventive care as readiness maintenance may improve disclosure and engagement without challenging occupational identity.
Footnotes
Acknowledgements
We extend our sincere gratitude to the scholars whose work informed and guided this study.
Ethical Considerations
This study was approved by the Purdue University Institutional Review Board (IRB-2023-1835) on 2/25/2025.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
