Abstract
Previous studies have indicated that outdoor air pollution has a negative impact on semen quality; however, few studies have examined whether living in a recently renovated residence is one of the factors influencing semen parameters. We aimed to examine the association between household renovation and semen parameters among infertile men. Our study was conducted at the Reproductive Medicine Center, The First Hospital of Jilin University (Changchun, China) from July 2018 to April 2020. A total of 2267 participants were enrolled in the study. The participants completed the questionnaire and provided a semen sample. Univariate and multiple logistic regression models were used to estimate the association between household renovations and semen parameters. Of the participants, about one-fifth (n = 523, 23.1%) had undergone renovations in the last 24 months. The median progressive motility was 34.50%. There was a significant difference between participants whose residences had been renovated in the last 24 months and those whose residences had not been recently renovated (z = –2.114, p = .035). Compared with participants whose residences were not recently renovated, participants who moved into the residence within 3 months after renovation had a higher risk of abnormal progressive motility after adjusting for age and abstinence time (odds ratio [OR] = 1.537, 95% confidence interval [CI]: 1.088–2.172). Our findings indicated that progressive motility was significantly associated with household renovations.
Semen quality has decreased in the 21st century (Centola et al., 2016; Rolland et al., 2013). Environmental factors appear to have a significant impact on sperm quality (Storgaard et al., 2006). Some publications have reported that decreased semen quality is associated with environmental factors (Zamkowska et al., 2018). Since the 1990s, researchers have begun to focus on the impact of air pollution on semen quality. A meta-analysis of association between exposure to outdoor air pollution and semen quality suggested that high levels of air pollution exposure had a negative effect on semen quality (J. Zhang et al., 2020). Sperm morphology and concentration were the most sensitive parameters of dust pollution, and exposure to dust particles may influence sperm quantity in infertile men (Najafpour et al., 2020). Sperm morphology and concentration are also affected by exposure to ozone (Wdowiak et al., 2019; H. T. Zhang et al., 2019). Sperm motility decreases after exposure to particulate matter (PM) 2.5, especially 2 to 3 months after exposure (Hammoud et al., 2010). Furthermore, a decline in sperm count was significantly associated with exposure to ambient air pollutants (CO, NO2, O3, PM10, and PM2.5), especially during 10 to 14 lag days (G. Huang et al., 2020).
Compared to ambient air pollution, people may be exposed to more indoor air pollutants (Kumar et al., 2021). With the acceleration of urbanization, people are paying more attention to improvement in living conditions, and an increasing number of Chinese people have moved into new houses after renovation, especially young people of childbearing age. Household renovations have become a source of indoor air pollution (Motoki et al., 2019). Household renovation can produce many harmful chemical pollutants and heavy metals, including formaldehyde (S. Huang et al., 2017), volatile organic compounds (VOCs) (Brown, 2002; Järnström et al., 2008; Srivastava et al., 2000), carbonyl compounds (Ochs Sde et al., 2016), ammonia (Liu et al., 2008), and lead (Reynolds et al., 1999). Owing to the complexity and difficulty of quantifying indoor air, no research has been conducted on indoor air pollutants and semen quality. To the best of our knowledge, there has been only one epidemiological study on household decoration and semen quality. The epidemiological study only focused on the association between semen quality, which was assessed using the World Health Organization (WHO) criteria (1999), and household renovation, but did not study the association between semen parameters and household renovation (Miao et al., 2015).
Our study aimed to confirm whether semen parameters were associated with household renovation, determine the association between household renovation and semen parameters, and provide epidemiological basis and clues for indoor air pollution and semen quality.
Materials and Methods
Subjects
This study was conducted at the Reproductive Medicine Center, The First Hospital of Jilin University (Changchun, China) from July 2018 to April 2020. The research related to human use complied with all the relevant national regulations and institutional policies, in accordance with the tenets of the Helsinki Declaration, and was approved by the Ethical Committee of The First Hospital of Jilin University (No. 2020-555).
Male outpatients were recruited if they completed the questionnaire and provided qualified semen samples. The questionnaire collected information on age, education level, type of occupation, income per month, and abstinence time (days). The questionnaire included two questions about household renovation (Miao et al., 2015): (a) Is your residence recently renovated in the last 24 months? (definition of residence recently renovated was residence with at least two of the following items included: wall (with paint or wallpaper), floor (with ceramic tiles or wood), and furniture (recently bought or repainted)) (b) How many months after the house renovated did you move into your residence? Participants who spent an average of less than 8 hours per day in the renovated residence were excluded. Of the 2938 participants, 671 participants were excluded: 227 participants reported clinical conditions that could affect semen quality (cryptorchidism, varicoceles, and urogenital infections); 153 participants had immune diseases (thyroiditis and rheumatoid arthritis); 23 participants reported having genetic diseases (chromosomal disease and single gene disease); 87 participants reported having chronic diseases (tuberculosis, chronic renal failure, and hyperthyroidism); 30 participants had too short (<2 days) or too long (>7 days) duration of abstinence time; 59 participants had incomplete semen collection; and 92 participants did not complete the questionnaire. The final sample size for this study was 2267. Written informed consent was obtained from all individuals included in this study.
Samples Collection and Analysis
The subjects provided semen samples by masturbating into a sterile jar after a period of 2 to 7 days of sexual abstinence. Each participant was instructed to collect a complete ejaculate sample. The samples were immediately delivered to the laboratory and were incubated at 37°C until completely liquefied. Conventional semen analysis was then conducted. Semen samples were analyzed for volume, sperm concentration, motility, viability, and normal sperm morphology. We extracted 5-ml semen samples from well-mixed semen and examined sperm concentration, motility, viability, and normal sperm morphology through the computer-automated semen analysis system (CASA) (BEION S3, Beion Medical Technology Co. LTD, Shanghai, China). The remaining semen samples were transferred to a test tube with a precision scale to measure semen volume (ml). Total sperm count (million) was calculated as sperm concentration times semen volume. Semen parameters were classified according to the guidelines of the WHO Laboratory Manual (Cooper et al., 2010).
Statistical Analysis
Statistical analyses were performed using the SPSS software (version 23.0; IBM, Armonk, NY, USA). Quantitative variables are expressed as mean ± standard deviation (SD) or median (interquartile range [IQR]). Categorical data were expressed as frequencies (percentages). The Mann–Whitney U-test was used to compare the differences in semen parameters between groups of residents with and without recent renovation.
Univariate and multiple logistic regression models were used to estimate the association between household renovation and semen parameters. Associations were indicated using crude and adjusted odds ratios (ORs) with 95% confidence intervals (CIs). We set the classification of semen parameters according to the guidelines of the WHO Laboratory Manual as the dependent variable (normal semen parameters were coded as 0, abnormal semen parameters were coded as 1), set the household renovation independent variable (lived in residence without household renovation were coded as 0, lived in residence with recently renovated were coded as 1), and set factors that may affect semen parameters as potential confounding factors. Potential confounding factors that affect semen parameters, including age and abstinence time, were entered into multiple logistic regression models. P values <.05 for a two-tailed distribution were considered statistically significant difference.
Results
Characteristics of Study Population
A total of 2267 participants were included in this study. The general characteristics of the study population are summarized in Table 1. The mean (±SD) age was 32.15 (±4.71) years. Among the participants, the majority had an educational level of college or above (n = 1424, 62.8%). More than half (n = 1440, 63.5%) of participants were manual workers. Of the participants, 23.1% (n = 523) lived in residences that had been renovated in the last 24 months. The median month from house renovation to moving into residence was 6.00 (3.00, 10.00) months. The median abstinence time was 4 days. The median sperm concentration and total sperm count were 54.40 million/ml and 188.73 million, respectively. The median (IQR) value for progressive motility was 34.50 (22.40, 46.20).
General Characteristics of the Study Population
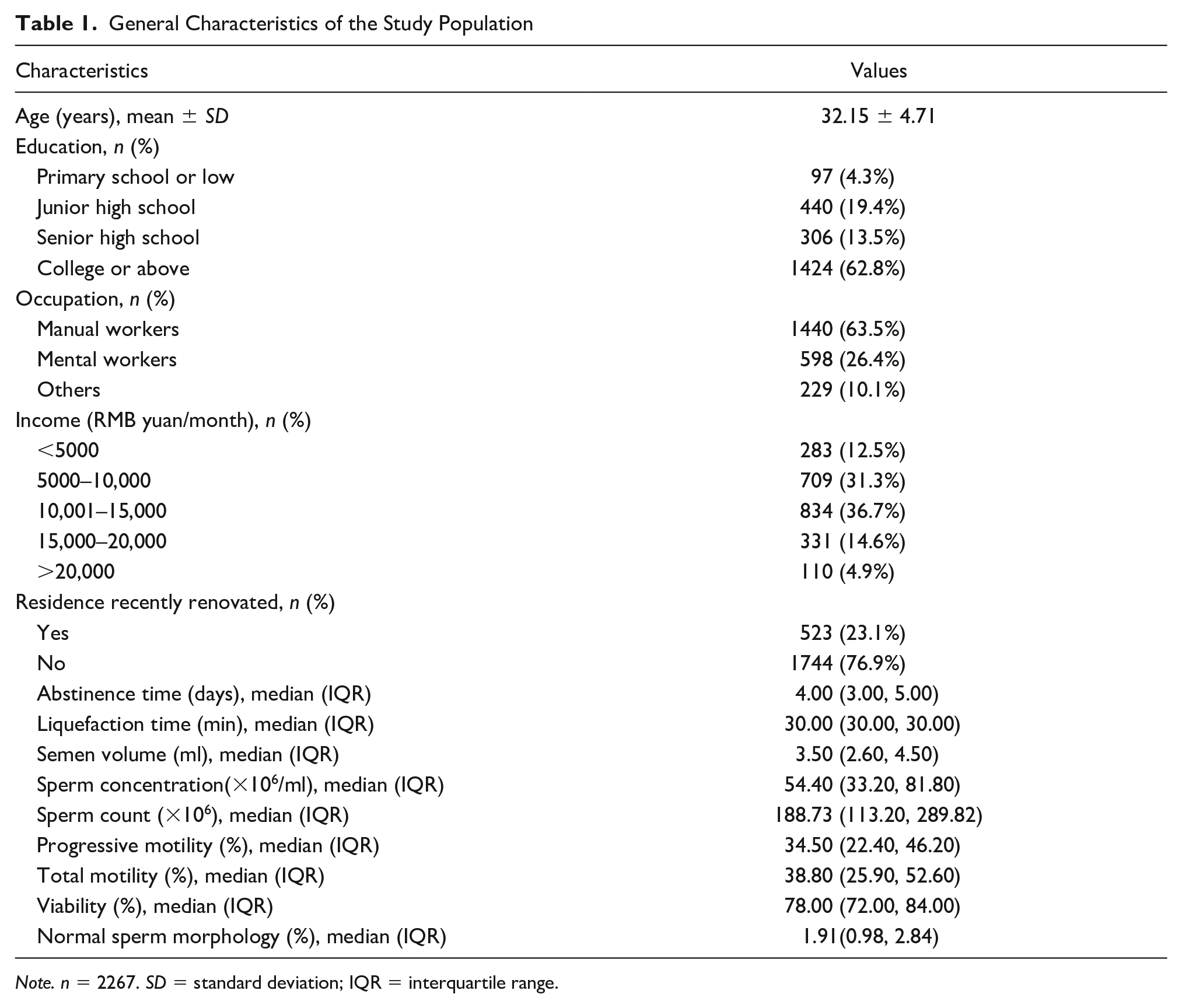
Note. n = 2267. SD = standard deviation; IQR = interquartile range.
Association Between Household Renovation and Semen Parameters
Table 2 presents the difference in semen parameters between the groups of residences with and without renovation in the last 24 months. There were no significant differences in semen volume, sperm concentration, sperm count, total motility, and normal sperm morphology between participants who lived in residences with recently renovated (in 24 months) and those who lived in residences that were not recently renovated (both p > .05). Progressive motility significantly differed between the groups with and without renovation in the last 24 months (z = –2.114, p = .035).
Comparison Between Semen Parameters and Household Renovation (n = 2267)

Table 3 and Table 4 present the logistic regression for semen parameters and household renovations. In univariate logistic regression analyses, household renovation had a significantly negative association with abnormal progressive motility (Wald χ2 = 5.479, p = .019). The OR of household renovation for progressive motility was 1.263 (95% CI: 1.039–1.537). In multiple logistic regression analyses, after adjusting age and abstinence time, participants who moved into the residence within 3 months after household renovation had a higher risk of abnormal progressive motility (OR = 1.537, 95% CI: 1.088–2.172) than those whose residences were not recently renovated.
Associations Between Semen Parameters and Household Renovation (n = 2267)

Associations Between Abnormal Progressive Motility and Household Renovation (n = 2267)

adjusting for age and abstinence time.
Discussion
In this study of male patients, we found that the recent household renovation group had a significantly lower progressive motility than the group without household renovation. Household renovation increased the risk of abnormal sperm progressive motility, especially for participants who moved into the residence within 3 months after household renovation.
The formaldehyde concentration and mean concentrations of BTEX (toluene, m/p-xylene, o-xylene, and ethylbenzene) emitted by products and materials in newly renovated apartments were significantly higher than those in old buildings (Dai et al., 2017; Guo et al., 2009; Hadei et al., 2018). Among them, formaldehyde concentration was not only high, but also decayed more slowly than other VOCs, and formaldehyde pollution of the building would persist for many years (Brown, 2002). Sperm vitality and sperm motility decrease in workers exposed to benzene, toluene, and xylene (Xiao et al., 2001). Workers occupationally exposed to formaldehyde observed decreased sperm progressive motility and total sperm motility (Wang et al., 2015). Workers exposed to high hydrocarbon concentrations in occupational air environment had more abnormal semen characteristics than those who are unexposed; exposed workers had alterations in viscosity, liquefaction capacity, sperm count, sperm motility, and the proportion of sperm with normal morphology (De et al., 2000). Exposure to renovation materials may result in a decrease in semen parameters in men. In 2007, a study in India confirmed that paint factory workers had lower sperm velocity, total motility, and progressive motility than nonoccupationally exposed groups (p < .001) (Naha & Manna, 2007). Occupational exposure to cement increases the risk of oligozoospermia (OR = 1.1; 95% CI: 0.9–1.4) (Daoud et al., 2017). A study of participants from wood processing industries and age-matched male volunteers reported that sperm progressive motility, total sperm motility, curvilinear velocity, straight-line velocity, and time-average velocity were significantly decreased in formaldehyde exposure workers compared to the referents (Wang et al., 2015). Miao et al. (Miao et al., 2015) reported that household renovation impaired semen quality; participants with a history of indoor renovation in the recent 1 year were more likely to have poor semen quality than participants with no such history (OR = 5.9; 95% CI: 2.3–25.1). Previous studies have focused on semen quality in men who had occupational exposure related to renovation, and few studies have investigated exposure to household renovation.
Renovation materials may affect semen parameters by affecting testicular function. Long-term exposure to formaldehyde has a harmful effect on male reproduction by inducing oxidative stress in rats; sperm quantity and quality, and testicular seminiferous tubular diameter were significantly decreased (Zhou et al., 2011). In vivo experiments in male ICR mice indicated that BDE-209(BDE-209 is a common flame retardant in furniture) results in damage to the testis structure, leading to cell apoptosis in the testis and decreased sperm number and motility, while sperm malformation was significantly increased (Li et al., 2019). Environmental exposure, rather than genetics, was the most important factor affecting male fertility observed trends (Skakkebaek et al., 2016). Exposure to solvents and painting materials in workplace increased the risk of male infertility (OR:3.88; 95% CI:1.50–10.03; El-Helaly et al., 2010).
To our knowledge, this study was the first observation study on household renovation and specific semen parameters. However, this study also had several limitations. First, this study was a cross-sectional study. We can only obtain an association between household renovation and semen parameters, but we cannot obtain causal inferences and explanations regarding this association. Second, all participants were men attending the Reproductive Medicine Center, and they may only represent the infertile population. Third, though all participants in the study were owners of residences, the information related to household renovation were obtained through self-reports. Imprecise recollection of household renovation might arise recall bias. Despite these limitations, the results of this study can provide clues to the etiology of the changes in semen parameters.
Conclusions
In summary, progressive motility is associated with household renovations. We do not recommend that men of childbearing age move to residences immediately after household renovation.
Footnotes
Acknowledgements
The authors would like to thank participants of this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Science and Technology Department of Jilin Province, China (grant no. 20200404186YY).
Data Availability Statement
The data presented in this study are available upon request from the corresponding author. The data are not publicly available because they contain information that can compromise the privacy of the research participants.
