Abstract
This study aims to explore how peer education influences men who have sex with men (MSM) to accompany friends to test and then affects their own testing, and to reveal the internal mechanism of peer education influencing HIV testing. A cross-sectional study among MSM in 11 cities in Shandong province, China was conducted to collect information on demographic characteristics, behavior, HIV-related knowledge, HIV testing history, and use of prevention services. Blood samples were tested for HIV status. Logistic regression was used for univariate and multivariate analyses, and R Mediation package was used for mediating effect analysis. Of 4,005 participants, 66.8% (2,674/4,005) had HIV testing in the last year, 50.6% (2,026/4,004) accompanied a friend for HIV testing, and 65.3% (2,614/4,005) received peer education in the last year. In multivariate logistic regression analysis, MSM who had anal sex with men in the past six months (adjusted odds ratio [AOR] = 1.772, 95% confidence interval [CI] = [1.438, 2.182]), had used drugs (AOR = 2.762, 95% CI = [2.264, 3.368]), received peer education in the past year (AOR = 2.412, 95% CI = [2.081, 2.796]), and accompanied a friend for testing in the past year (AOR = 3.077, 95% CI = [2.653, 3.569]) were more likely to take HIV testing. Receiving peer education in the past year could influence their own HIV testing in the past year by affecting their accompanying one’s friends to take the test in the past year (a*b = 0.889, 95% CI = [0.733, 1.053]). Peer education not only had a direct effect on HIV testing but also had an indirect effect on HIV testing by influencing accompanying friends for testing.
Introduction
AIDS is an important public health problem in the world. So far, the incidence of AIDS continues to rise in some countries in Europe, North America, and South America (Govender et al., 2021). Men who have sex with men (MSM) are the high-risk group and bridge group of AIDS, and are more likely to be infected with HIV than the general population (Wu et al., 2019; Zhang et al., 2020). As of October 2020, China had reported 1,045,000 live HIV/AIDS cases, of which 112,000 were newly reported nationwide from January to October 2020 (Chuai et al., 2020). Since 2010, the prevalence of HIV in MSM in China has increased significantly (Sun et al., 2021 Wu et al., 2019). The overall national prevalence of HIV among MSM from 2001 to 2018 was about 5.7% in China (Dong et al., 2019). Over the years, China has achieved remarkable achievements in HIV/AIDS prevention and control, keeping the epidemic at a low level. However, the transmission of HIV through sexual intercourse is difficult to be effectively controlled in the coming years, especially the uncontrolled transmission through sexual contact among MSM (Guo et al., 2020). Shandong is a coastal province in eastern China with a population of about 102 million. Since 2009, the number of HIV/AIDS cases in Shandong province has shown a rapid growth trend, and the annual average growth rate has exceeded the national average (Zhang et al., 2017). As of the end of December 2019, 66.8% of the living HIV cases in Shandong Province were transmitted through MSM (Liao et al., 2020). Since there is no cure and no effective vaccine (Waymack & Sundareshan, 2021), it is important to prevent AIDS by reducing high-risk behaviors and promoting safe behaviors.
Peer education refers to the sharing of HIV/AIDS information in small groups or one-on-one with peers who are matched with the target population through demographic characteristics or risk behaviors (Medley et al., 2009). Peer education can promote HIV testing in high-risk groups, promote condom use, and reduce unprotected sex (He et al., 2020) and has become an important strategy for health promotion in HIV-high-risk groups worldwide, including MSM (Jones et al., 2008; Kebede et al., 2021).
HIV testing is the first step toward the global 90-90-90 goal set by UNAIDS. HIV testing must be scaled up if 90% of people infected with HIV are to be diagnosed (Desai et al., 2020). Studies have reported that people with HIV who are aware of their infection status are more likely to take effective measures to prevent transmission of HIV to their partners than those who are unaware of their infection status (Pinkerton et al., 2008). Since 2013, the HIV testing rate of MSM in China has shown an upward trend (Wu et al., 2021). However, HIV testing in China’s MSM is still at a low level (Wang et al., 2020). About 50% to 60% of MSM had not been tested for HIV in the past year (Ren et al., 2017; Tang & Lyu, 2021; Wu et al., 2019). In 2013, the HIV testing rate of MSM in China was about 60%, rising to 77.3% in 2018 (Wu et al., 2021). There are still many MSM who have never been tested for HIV. So, it is necessary to take intervention measures to improve the rate of HIV testing among MSM.
Before a person makes a choice, he can engage in observational learning by watching what happen to other credible people, known as the observational learning in social cognitive theory (Lockwood & Klein-Flügge, 2021). Studies have found that HIV infection rates are as high as 3.6% to 5% for companions who accompany HIV-positive patients to medical institutions for testing or treatment (Bischof et al., 2015; LeViere et al., 2019). By testing these companions, we can enable more people who are already infected with HIV to know their infection status as early as possible. The reason why HIV testing based on medical institutions does not cover all MSM is because of the stigma of HIV testing, the insufficient confidentiality and privacy in medical institutions, and the low trust of MSM to medical institutions (Song et al., 2011; Yu et al., 2018). Accompanying one’s friends to take the test can make oneself have a general understanding of the testing environment and testing process, so as to eliminate the above concerns. This may increase the courage and confidence of those MSM who want to be tested but are afraid of testing for various reasons, and reduce the fear of testing stigma.
Although some studies have noted that peer education is a positive factor for HIV testing in MSM (He et al., 2020; Lin et al., 2021; Zhou et al., 2017), few studies have linked peer education, accompanying friends for testing and HIV testing. By combining the above three factors, this study aims to explore how peer education influences MSM to accompany friends to test and then affects their own testing, and reveals the internal mechanism of peer education influencing HIV testing. Elucidating this mechanism will enable the intervention of peer education to be more targeted to effectively increase HIV testing in the future.
Method
Recruitments and Participants
Cross-sectional surveys were conducted among MSM in 11 cities in Shandong Province, that is, Jinan, Qingdao, Zibo, Yantai, Weifang, Weihai, Liaocheng, Jining, Binzhou, Heze, and Dezhou, from April to June in 2019. The inclusion criteria were being biologically male, aged 15 to 65, self-reported ever had penetrative oral or anal sex with a man in the past year.
Multiple recruitment methods including venue-based recruitment, internet advertisement, community outreach, and peer referrals were used in this study. MSM were recruited from bars, night clubs, tea bars, saunas, bathhouses, public toilets and parks, non-venue-based grassroots communities, HIV testing sites, and internet advertisements.
Before starting a formal questionnaire survey, survey information was collected anonymously and remained confidential by trained investigators. All participants were invited for eligibility assessments and interviewed in community-based voluntary counseling and testing center. After completing the questionnaire, the investigator carefully checked each question for mistakes immediately.
Measures
Face-to-face interviews were administered to collect general demographic information (age, marital status, location of household registration, ethnicity, education level, sexual orientation), sexual and drug use behavioral information, history of HIV testing and HIV-related prevention services, and experiences of participating in health promotion activities in gay community, etc. HIV-related knowledge included a total of eight questions. Participants who answered six or more questions correctly were considered having sufficient AIDS knowledge. We asked the participants when they were tested last time, the frequency of testing in the last year by asking “In addition to this test, have you been tested for HIV in the last year?” and “How often have you been tested for HIV in the last year?.” Peer education experience in the past year was collected by the question “Have you received peer education on HIV prevention in the past year?.”
All participants were asked if they had heard of or participated in some activities that encourage HIV testing in the gay community. The participants were also asked if they had accompanied their friends or sexual partners to a regular testing site for HIV testing. Regular testing sites refer to institutions designated or authorized by the Centers for Disease Control and Prevention.
Finally, the investigators informed the participants that they needed to have their blood taken for testing. Blood samples were collected for HIV antibody testing. All participants were required to report the results of two HIV antibody tests, including initial screening and re-testing. All blood samples that were initially screened positive were retested using another enzyme-linked immunosorbent reagent-2 of a different principle or manufacturer. When both test results were positive, the HIV antibody could be determined to be positive.
Statistical Analysis
We used Epidata3.1 to enter the data, and used SPSS 24.0 and R 4.1.0 to analyze the data. Continuous variables were represented by median and interquartile range, and categorical variables were represented by frequency and proportion. In this study, Mann–Whitney U test (for continuous variable) and chi-square test (for categorical variable) were used to evaluate the univariate distribution of each variable in HIV testing behavior, and the significance level was set to 0.05. Then we took the non-tested group as the reference group and included the variables (p < .05) of the above two groups (HIV testing in the past year, Yes or No) into the multivariate logistic regression analysis to further analyze the differences between the populations with different test characteristics. We used univariate and multivariate logistic regression to analyze the possible influencing factors of peer education. In addition, we separately calculated the regression coefficients between “peer education” and “accompanying friends for testing,” between “accompanying friends for testing” and “HIV testing.” Since the three variables are all binary variables, we used the R Mediation package in R to analyze the mediation effect of the path of peer education-accompanying friends for testing-HIV testing (Tofighi & MacKinnon, 2011). We calculated the product of the above two regression coefficients and the 95% confidence interval (CI). If the 95% CI did not contain 0, there was a mediating effect between the variables.
Results
Characteristics of Participants and Correlates of HIV Testing
A total of 4,005 valid questionnaires were collected in the study. Age of the participants ranged from 15 to 74 years old. Among them, 66.8% (2,674/4,005) had been tested for HIV in the past year. About 89% (3,562/4,005) of the study participants had sufficient knowledge of AIDS, 65.3% (2,614/4,005) had received peer education in the past year, and 50.6% (2,026/4,004) had the experience of accompanying friends for HIV testing in the past year. The prevalence of HIV was 3.5% (142/4,005). HIV infection in MSM was significantly associated with HIV testing in the past year (χ2 = 12.911, p < .001). Univariate analysis showed that AIDS knowledge, having anal sex with men in the past 6 months, drug use, peer education, and accompanying friends for testing had statistically significant effects on the HIV testing status of MSM in the past year. MSM who had sufficient knowledge about AIDS (χ2 = 29.491, p < .001), had anal sex with men in the past six months (χ2 = 71.964, p < .001), had used drugs (χ2 = 186.957, p < .001), had received peer education in the past year (χ2 = 271.167, p < .001), and had accompanied friends for testing in the past year (χ2 = 328.277, p < .001) were more likely to receive HIV testing in the past year (Table 1).
Demographic, Risk Behaviors, HIV-Related Knowledge, and the Use of HIV-Related Prevention Services Among MSM Who Had HIV Testing and Those Who Did Not Have HIV Testing in the Past Year, in Shandong Province (N = 4,005).

Note. MSM = men who have sex with men.
Median and Quartile, Wilcoxon rank sum test.
The boldfaced values represent statistically significant variables.
Table 2 shows that MSM who have had anal sex with men in the past 6 months (AOR = 1.772, 95% CI = [1.438, 2.182]), have used drugs (AOR = 2.762, 95% CI = [2.264, 3.368]), have received peer education in the past year (AOR = 2.412, 95% CI = [2.081, 2.796]), and have accompanied a friend for testing in the past year (AOR = 3.077, 95% CI = [2.653, 3.569]) are more likely to be have been tested for HIV in the last year (Table 2).
Multivariate Analysis of MSM Who Were Tested for HIV and Who Were not Tested in the Past Year, in Shandong Province (N = 4,005).
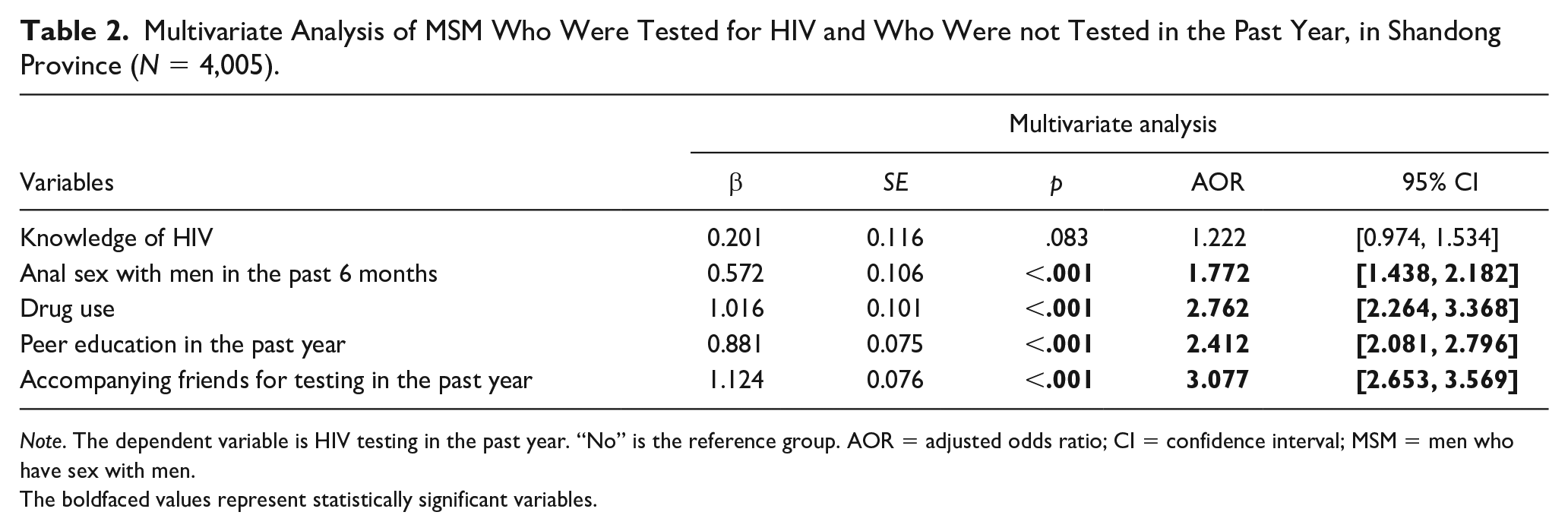
Note. The dependent variable is HIV testing in the past year. “No” is the reference group. AOR = adjusted odds ratio; CI = confidence interval; MSM = men who have sex with men.
The boldfaced values represent statistically significant variables.
Correlates of Peer Education
Univariate and multivariate analyses were performed on whether MSM had received peer education in the past year. Variables with p < .05 in univariate regression were included in multivariate regression analysis. Table 3 shows that MSM who are currently married to a woman (AOR = 1.513, 95% CI = [1.291, 1.772]), have used drugs (AOR = 1.863, 95% CI = [1.557, 2.229]), have been tested for HIV in the past year (AOR = 2.427, 95% CI = [2.093, 2.816]), and have accompanied a friend to be tested in the past year (AOR = 1.697, 95% CI = [1.469, 1.960]) are more likely to have received peer education in the past year. MSM who are currently cohabitating with a woman (AOR = 0.322, 95% CI = [0.172, 0.603]), have a junior high school degree (AOR = 0.542, 95% CI = [0.312, 0.942]), are less likely to have received peer education in the past year.
Factors Associated With Peer Education in Univariate and Multivariate Regression Among MSM in Shandong Province (N = 4,005).

Note. The dependent variable is peer education in the past year. “No” is the reference group. OR = odds ratio; AOR = adjusted odds ratio; CI = confidence interval; MSM = men who have sex with men.
The boldfaced values represent statistically significant variables.
Mediating Effect of Accompany Friends for Testing
Figure 1 and Table 4 display the mediation effect path and effect values of “Peer education → Accompanying friends for testing in the past year → HIV testing in the past year.” The results indicate that peer education not only has a direct effect on HIV testing (c’ = 0.881, p < .05), but also has an indirect effect on HIV testing by influencing accompanying friends for testing. Receiving peer education in the past year could influence MSM’s own HIV testing in the past year by affecting their accompanying one’s friends to take the test in the past year (a*b = 0.889, 95% CI = [0.733, 1.053]; Figure 1, Table 4).

Mediation Effect Diagram.
Mediation Effect of “Peer Education → Accompany Friends for Testing → HIV Testing in the Past Year”.

Note. CI = confidence interval.
Discussion
In this study, we analyzed and explored the association between peer education and HIV testing in MSM in Shandong Province, and found independent mediating effect of accompanying friends for testing.
In our study, 66.8% (2,674/4,005) of the participants had been tested for HIV in the past year. Multivariate analysis showed that MSM with high-risk behaviors such as anal sex with men in the last 6 months and drug use were more likely to have been tested in the past year, which was consistent with the results of many studies (Lorusso et al., 2017; Sun et al., 2020; Wong et al., 2017). A study reported that 51% of MSM living in the United States had been tested for HIV in the past year (Stephenson et al., 2015). A study of the MSM population in Changsha, China found that 62.3% of the study participants had been tested for HIV in the past year (Zhou et al., 2018). Although the proportion in this study is higher than that in the two studies above, there is still a gap to the target of 90% proposed by UNAIDS (Granich et al., 2017). Therefore, appropriate interventions are needed to increase the HIV testing in MSM.
Many studies have demonstrated that peer education could increase AIDS knowledge, reduce the occurrence of high-risk behaviors, promote HIV testing, and effectively prevent HIV transmission (Ceylan & Koç, 2021; He et al., 2020; Medley et al., 2009; Raker et al., 2020). Because the MSM is a hidden population with certain particularity, they are more willing to trust their peers compared with the mass media, so that they can discuss sensitive topics without concerns (Medley et al., 2009). Therefore, peer education is of great significance for HIV prevention. Our research confirmed this point in that 65.3% of MSM received peer education in the last year, and MSM who received peer education were 2.4 times more likely to undergo HIV testing in the last year than those who did not receive peer education. Thus, peer education should be promoted in AIDS prevention and control in the future. In particular, we should strengthen publicity and education for MSM who are cohabitating with women and those who have a junior high school degree or less.
This study found that peer education in MSM could influence their own HIV testing through the mediating effect of accompanying their friends for testing. MSM’s knowledge of AIDS increases after peer education, which may lead them to want to test for HIV. However, MSM may be afraid that their privacy will be discovered by others, or they may be afraid of being stigmatized by HIV, so MSM may choose to accompany their friends to get a test first, and then take the test by themselves after they have a certain understanding of the testing environment and process. Another explanation is that accompanying a friend who tested positive may prompt one to take the test himself to determine whether he is infected with HIV. Studies have proved that people who know their sexual partners or close friends have been tested are more likely to be tested regularly themselves (Cheng et al., 2020). MSM who have close partners or friends who have been tested for HIV are more likely to be tested for HIV. MSM who have friends living with HIV are also more likely to be tested for HIV. MSM are more likely to be tested for HIV if their social networks include other friends who are living with HIV or have been exposed to HIV prevention interventions. Having at least one friend who has tested HIV positive can encourage them to get tested themselves (Yamanis et al., 2017). MSM in the core of the social networks are more likely to be tested for HIV than MSM in the periphery of the networks, because they have more friends and can quickly contact many people in the networks, so they are more likely to accompany their friends to be tested for HIV. MSM are more likely to get tested when they go with friends or when friends suggest them to do test. Talking to friends about HIV can encourage them to get tested themselves (Kaneko et al., 2021). All of the above situations can occur when accompanying a friend for testing, so as to improve their courage and confidence for HIV testing and promote their own testing. For those MSM who have concerns and fears about being tested, it is advisable to encourage them to accompany their partners or friends to be tested to promote their own testing.
This study has some limitations. First, the MSM is a hard-to-reach population, and the research subjects we recruited cannot fully represent this group and there is a certain selection bias. Second, due to the particularity of the MSM, they may deliberately conceal something when answering sensitive questions, thus report bias might exist. However, in this study, anonymous questionnaires were used, and investigators assisted in filling in and quality control of the questionnaires, which improved the authenticity of the questionnaires to some extent. Third, the cross-sectional study design adopted in this study can only reflect the relationship between variables rather than causality. Further longitudinal data should be collected to explore its effect and mechanism.
Conclusion
In summary, peer education and accompanying friends for testing are important factors to promote MSM to take HIV testing themselves and are important intervention measures to prevent HIV transmission. Peer education not only directly affects HIV testing but also has an indirect effect through the mediating role of accompanying friends to test. Therefore, peer education should be vigorously carried out in the MSM. For MSM who are afraid of taking HIV test, they can be encouraged to accompany their friends to be tested first, so as to further improve the HIV detection rate in the MSM.
Footnotes
Acknowledgements
We would like to thank the study participants for sparing their time to respond to the data collection. We are grateful to the leadership of the local community-based organizations (CBOs) and Centers for Disease Control and Prevention (CDC) for their cooperation and support during data collection. Special thanks also go to the other investigators and staff for their invaluable effort during the implementation of the study.
Author Contributions
W.M. conceived and designed the study. L.W. and M.L. participated in investigation and data acquisition. Y.L. contributed to data analysis and interpretation, and drafted the manuscript. W.M., L.G., and M.L. made critical revisions of the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Key Research and Development Program of China under Grant (2017YFE0103800) and the National Science and Technology Major Project under Grant (2018ZX10721102-003-004).
Ethical Approval
This study was approved by the Ethical Review Committee (ERC) of School of Public Health in Shandong University (20190210).
Informed Consent
All participants provided their consent to participate in the study. Before the interview, interviewers explained the purpose and content of the study to the participants, and we promise to protect their privacy. The participants voluntarily decided to participate in this study after being informed.
