Abstract
Depression is one of the biggest health issues among men who have sex with men (MSM) living with HIV, where sexual identity might play an intricate role. Yet, findings of the relationship between sexual identity and depression were mixed and few studies explored its underlying mechanisms. This study aimed to examine the association between sexual identity and depression, and the potential mediating role of HIV-related stigma and moderating role of age. A cross-sectional survey was conducted among 203 MSM living with HIV in Guangxi, China. Participants provided information on sexual identity, depression, HIV-related stigma, and background information. Descriptive statistics, bivariate analysis, and path analysis were applied to examine our hypotheses. Bivariate analysis demonstrated that participants who self-identified as gay reported a lower level of HIV-related stigma and depression. Path analysis revealed an insignificant direct effect of identifying as gay on depression. Yet, the indirect pathway was significant, with identifying as gay being associated with a lower level of HIV stigma and thus a lower level of depression. This indirect effect was moderated by age. The conditional indirect effect was significant in the younger group yet ceased in the older group. The study provided information to better understand the effect of sexual identity on mental health among stigmatized sexual and gender minorities by highlighting the mediating effect of HIV-related stigma and the protective effect of age. Interventions targeting mental health of MSM living with HIV might consider placing greater emphasis on addressing HIV-related stigma among younger MSM.
Introduction
Despite the increasing efforts in HIV prevention and control, HIV infection among men who have sex with men (MSM) is still dramatically rising in China. According to a large-scale systematic analysis, the pooled national HIV prevalence among MSM ranged from 0% to 22.91%, with a tendency of increasing as time progressed from 2001 to 2018 (Dong et al., 2019). Guangxi Zhuang Autonomous Region (Guangxi) reported a total of 124,282 HIV/AIDS cases by 2018, representing a 78.70% increase since June 2011 (69,548 cases), placing Guangxi the third in terms of the documented HIV seropositive cases among China’s provinces (Guangxi Center of Disease Control and Prevention, 2018). From 2008 to 2017, the HIV prevalence among MSM is surprisingly surging in Guangxi, although the proportion of HIV cases accounted for by MSM is still lower than the national average level (Chen et al., 2019). In 2008, the annual cross-sectional survey among MSM in Guangxi demonstrated an HIV prevalence of 2.0%; however, such rate grew to 10.0% in 2017 (Guanghua et al., 2018) due to an increase in high-risk behaviors and wider use of the internet to search partners (He et al., 2012; Qin et al., 2016).
Depression is one of the biggest health issues among MSM living with HIV (Beyrer et al., 2013; Ferlatte et al., 2017). According to the minority stress theory, minority groups are exposed to both external stressors (e.g., discrimination) and internal stressors (e.g., concealment of identity), which in turn places them at risk of tremendous adverse mental health outcomes (Meyer, 2003). Being part of the sexual and gender minority (SGM) population, MSM were reported to be at higher risk of depression compared with their nonsexual minority counterparts in the predominantly heteronormative society (Heywood & Lyons, 2016; Meyer, 2003; Yan et al., 2014). A meta-analysis revealed that the pooled prevalence of depression among MSM living with HIV was 43% (Xiao et al., 2020), which is higher than heterosexual men living with HIV (Hatzenbuehler et al., 2008). Depression among MSM is reported to be associated with health behaviors and mental/physical outcomes, such as antiretroviral therapy (ART) adherence (Tao et al., 2017), responsiveness to ART (Carrico et al., 2011), viral suppression (Leserman, 2008), and CD4 count (Antoni et al., 2006).
HIV-related stigma might aggravate depressive symptoms among MSM living with HIV (Wohl et al., 2013; Yan et al., 2019; X. Yang et al., 2020). Although MSM living with HIV perceive and experience various types of stigma, the influence of HIV stigma has been revealed to overshadow the degree to which sexual identity–related stigma influences psychological distress for this population (Aunon et al., 2020). HIV-related stigma is pervasive (Li et al., 2016; Rao et al., 2008) and compromises people living with HIV’s (PLWH) mental health through social isolation (Courtenay–Quirk et al., 2006), lack of social support (Dowshen et al., 2009), self-blame, and impaired self-esteem (Dowshen et al., 2009; Kalichman et al., 2009). A cross-sectional study with 456 HIV-infected MSM demonstrated that 61% of the participants reported perceiving discrimination from the gay community because of their HIV serostatus, and such perceived HIV stigma was associated with higher levels of depression, anxiety, loneliness, avoidant coping strategies, and suicidal ideation (Courtenay–Quirk et al., 2006). Similar findings were demonstrated in younger MSM (Jeffries et al., 2015).
Such HIV-related stigma experienced by MSM living with HIV might vary across sexual identities—the self-identification in terms of to whom one is romantically or sexually attracted (Reiter, 1989). Carrillo and Hoffman (2016) highlighted the importance of considering the inconsistency between sexual identity and sexual behavior. Although maintaining same-sex relationships with males, part of MSM were more likely to self-identify as “straight” (Finlinson et al., 2006). Living in a society where strong social value is placed on heterosexuality, regardless of the achievements of lesbian, gay, bisexual, transgender, and queer or questioning (LGBTQ) movements, identifying with heterosexuality is still considered a better option for some MSM (Dean, 2014). MSM who were ashamed to self-identify as “gay” might experience worse HIV stigma because they were exposed to negative social beliefs such as “homosexuality is immoral and HIV is a disease caused by immoral behavior” (Jeffries et al., 2015, p. 66). By refusing to acknowledge their identity as a sexual minority, MSM who identified as “straight” distanced themselves from the LGBTQ community and inadvertently from the relevant support they could receive from it, which resulted in compromised psychosocial well-being and worse depressive symptoms (Kertzner et al., 2009). Although studies among MSM living with HIV have revealed the non-negligible influence of HIV stigma on depression (Wohl et al., 2013; Yan et al., 2019; X. Yang et al., 2020), and the potential association between HIV stigma and sexual identity (Jeffries et al., 2015), few empirical studies were conducted to describe the sexual identity–HIV stigma-depression pathway, not to mention potential moderators for these associations.
Given that age was often investigated as a moderator in stressors and coping studies (Folkman, 2011), we assume that the hypothesized sexual identity–HIV stigma-depression pathway might also be moderated by age. Older age could serve as a protector of mental well-being among MSM (Corboz & Corboz, 2008; Meanley et al., 2020). Studies have demonstrated that MSM younger than the age of 30 years were more likely to report psychological distress related to their sexual identity than older MSM (McAdams-Mahmoud et al., 2014). Demonstrated by a meta-analysis, age was negatively related to HIV-related stigma, with younger persons reporting greater HIV-related stigma (Logie & Gadalla, 2009). Meanwhile, younger MSM appeared to be at a higher risk of depression than their older counterparts (Corboz & Corboz, 2008). Such association was also identified under Asian culture (Logie et al., 2012).
Although the impacts of sexual identity, HIV-related stigma, and age on depressive symptoms among MSM were previously reported (Cho & Sohn, 2016; Hylton et al., 2017; Logie et al., 2012; Wohl et al., 2013), little is known about the potential mediating and moderating mechanisms behind the associations. We examined the underlying mechanisms of sexual identity, HIV-related stigma, and age on depressive symptoms among 203 MSM living with HIV recruited from Guangxi, China. Guangxi is a culturally and economically underdeveloped province with poor natural resources and lower average education attainment among the residents (Zhao et al., 2015). The conservative culture and social norms in Guangxi might be associated with a depraved mental well-being of MSM living with HIV (Sha et al., 2021). This study aimed to (a) examine the main effects of sexual identity, HIV-related stigma, and age on depression; (b) explore the mediating effect of HIV-related stigma on the relationship between sexual identity and depression among MSM living with HIV; and (c) investigate the moderating role of age in the mediation effect. As depicted in Figure 1, we hypothesized that (a) perceived HIV-related stigma would mediate the relationship between sexual identity and depressive symptoms and (b) the indirect effect of sexual identity on depression through HIV-related stigma would be moderated and buffered by age.

Hypothesized Moderated Mediation Model Among Sexual Identity, HIV-Related Stigma, Depression and Age
Method
Study Sites and Participants
Data were drawn from a cross-sectional study designed to explore psychosocial and behavioral factors related to mental and physical health. The study was conducted from March to July 2019 in Guangxi, China. In 2018, more than 86,000 HIV/AIDS cases were reported in Guangxi (Guangxi Center of Disease Control and Prevention, 2018), placing Guangxi third among China’s 31 provinces in terms of the documented seropositive cases (Wu et al., 2019). The top four cities (i.e., Nanning, Guizhou, Guilin, and Beihai) with the largest cumulative number of MSM living with HIV were selected as study sites. In collaboration with the local CDC, medical staff or case managers from each study site screened all the eligible MSM in their clinical record and invited all the prospective participants to join the study. Eligible participants were men who (a) had a confirmed diagnosis of HIV/AIDS and (b) self-reported having sex with men in the last 6 months. A purposive sampling method was used to recruit participants. After excluding the individuals who were not eligible, a total of 203 participants completed the survey.
Study Procedure
With the assistance and collaboration of Guangxi CDC, an interviewer-administered questionnaire was used for quantitative data collection. After obtaining participants’ written informed consent, local research team members conducted surveys in private offices in community health centers or HIV clinics where participants received regular medical care. The entire survey took around 30 min. Based on preexisting projects, each participant received cash of 50 Chinese Yuan (around US$7) upon the completion of the questionnaire (X. Yang et al., 2020a). The research protocol was approved by Institutional Review Boards at both the University of South Carolina and Guangxi CDC in China (Pro00100296).
Measures
Background Information
Participants were asked to provide information on their age, employment (i.e., full-time job vs. student, half-time job, or unemployment), marital status (i.e., married/remarried vs. others), education attainment (i.e., high school or below vs. college or above) and monthly income (i.e., less than 3,000 vs. 3,000 Chinese Yuan and above), sexual identity disclosure, HIV disclosure, HIV diagnosis duration, and ART use.
Sexual Identity
Participants’ sexual identity was assessed with one item, “What is your self-identified sexual identity?” Four options were provided as “gay,” “heterosexual,” “bisexual,” and “not sure.” Participants who reported themselves as gay were coded as 1. Otherwise, they were coded as 0.
HIV-Related Stigma
Eight items from the Negative Self-Image Scale (original Cronbach’s α = .96; Berger et al., 2001) were adapted to measure internalized HIV-related stigma. The Chinese version scale has been validated/used in various studies among Chinese PLWH (Li & Sheng, 2014; C.-H. Yu et al., 2019). Sample items were “I feel I’m not as good a person as others because I have HIV” and “HIV in my body makes me disgusted.” Responses of each item were rated from 1 (strongly disagree) to 4 (strongly agree). The scale exhibited good internal consistency in our study (Cronbach’s α = .95). For the purpose of data analysis, a sum score was first calculated and then recoded to a dichotomic variable (low vs. high) with a cut-off of the median.
Depression
Depression was assessed with a 10-item Center for Epidemiologic Studies Depression Scale (CES-D-10; original Cronbach’s α = .73–.86; Kohout et al., 1993). The Chinese version of CES-D-10 has been validated in both the clinical and nonclinical populations in China (S. C. Yu et al., 2013). The sum scores of CES-D-10 ranged from 10 to 40, with higher scores indicating more depressive symptoms. The scale exhibited an acceptable internal consistency in our study (Cronbach’s α = .81).
Data Analysis
First, descriptive statistics were presented to describe distributions of main study variables and key demographic variables, including frequencies for categorical variables and means and standard deviations for continuous variables. Second, Pearson correlation for continuous variables and point-biserial correlation for dichotomic variables (Gupta, 1960; Tate, 1954) were calculated on key variables and demographics. Finally, path analysis was conducted to examine the hypothesized moderated mediation model controlling for potential covariates (i.e., marital status, education attainment, employment, HIV disclosure, and sexual identity disclosure). Age as a moderator in the paths from HIV-related stigma to depression was integrated into an indirect effect model, whereby the relationship between sexual identity and depression was mediated by HIV-related stigma. If moderation analysis yielded a significant result, a simple slope analysis would be employed to provide the details of the moderation.
Among the 203 participants in the current study, each variable has less than 5% missing values. The expectation-maximization method was used to impute missing data (Dempster et al., 1977). Descriptive statistics and correlation analysis were performed with SPSS 26.0. Path analysis was conducted with Amos 26 to determine the overall fit of the proposed model, providing estimates of path coefficients (β) and bootstrapped 95% confidence intervals (95% CIs) based on 5,000 resamples. A p value of less than .05 was employed to indicate statistical significance.
Results
Descriptive Results
Among the 203 participated MSM, about two thirds (n = 129, 63.55%) of participants identified themselves as gay men, while others identified themselves as heterosexual, bisexual, or not sure. The average age of the sample was 32.43 (SD = 10.70, range = 16–67) years. Most of the participants were never married (n = 151, 74.38%), with a degree of college or above (n = 109, 53.69%), and having a full-time job (n = 132, 65.02%). The average length of HIV diagnosis duration was 32.33 (SD = 29.31, range = 1–145) months. Most participants were receiving ART (n = 169, 83.25%). Less than half of participants (n = 87, 42.86%) disclosed their HIV seropositive status to at least one of their parents, siblings, or friends, with even fewer participants (n = 60, 29.56%) disclosing their sexual identity to these recipients (Table 1).
Overall Descriptive Information and the Level of Depression by Demographic Groups Among MSM Living With HIV (N = 203).

Note. Categorical variables are reported with frequency and column percent; continuous variables are reported with mean and standard deviation (SD) for overall descriptions. Differences of depression across groups were calculated with ANOVA or two-group t tests as appropriate. MSM = men who have sex with men; ART = antiretroviral therapy; ANOVA = analysis of variance.
Associations Among Main Study Variables
As displayed in Table 2, for correlations among key variables, self-identified homosexual was negatively associated with HIV-related stigma (r = −.35, p < .01), age (r = −.15, p < .05), and depression (r = −.17, p < .05). HIV-related stigma was positively associated with age (r = .30, p < .01) and depression (r = .21, p < .01). For correlations between key variables and covariates, self-identified homosexual was positively associated with educational attainment (r = .28, p < .01) and sexual identity disclosure (r = .22, p < .01) while negatively associated with being married (r = −.35, p < .01). HIV-related stigma was positively related to being married (r = .34, p < .01) and negatively related to HIV diagnosis duration (r = −.20, p < .01). Age was positively related to HIV diagnosis duration (r = .35, p < .01). Depression was positively related to being married (r = .66, p < .01) while negatively related to educational attainment (r = −.32, p < .01), HIV disclosure (r = −.15, p < .01), and sexual identity disclosure (r = −.21, p < .01).
Correlation Matrix of Main Measures.

Note. Parameters reported in the table are Pearson correlations for continuous variables and point-biserial correlations for dichotomic variables. Sexual identity: 0 = heterosexual/bisexual/unsure, 1 = homosexual; HIV-related stigma: 0 = low, 1 = high; education attainment: 0 = high school or below, 1 = college or above; marital status: 0 = single, 1 = married/remarried; employment: 0 = student/half-time job/unemployment, 1 = full-time job; monthly income: 0 = <3,000, 1 = ≥3,000; HIV disclosure: 0 = no, 1 = yes; sexual identity disclosure: 0 = no, 1 = yes; ART use: 0 = no, 1 = yes. ART = antiretroviral therapy.
p < .05. **p < .01.
Path Analysis
The results of path analysis demonstrated good model fit: χ2/df = .89, p > .05; Tucker–Lewis index (TLI) = .93; comparative fit index (CFI) = .98; root mean square error of approximation (RMSEA) = .05; standardized root mean squared residual (SRMR) = .06. The finalized model (see Figure 2) explained a substantial portion of variance in the mediator (25.6% for HIV-related stigma) and dependent variable (16.6% for depression).

Moderated Mediation Model Among Sexual Identity, HIV-Related Stigma, Age, and Depression
In the mediation path (see Supplemental Material), the direct effects of sexual identity on HIV-related stigma (β = −.27, p < .01) and HIV-related stigma on depression were significant (β = .28, p < .01), whereas the direct effect of sexual identity on depression was not significant (β = −.03, p > .05). The indirect effect of sexual identity on depression through HIV-related stigma was significant (β = −.08, p < .01).
In the moderated mediation path (see Supplemental Material), the main effect of HIV-related stigma on depression was significant (β = .28, p < .01). The main effect of age was not significant (β = −.11, p > .05). The interactive effect of HIV-related stigma and age was significant (β = −.16, p < .05), indicating the relationship between HIV-related stigma and depression was diminished when age increases.
As presented in Figure 3, the simple slope analysis demonstrated an attenuate association between HIV-related stigma and depression as age increases. For the younger group (whose age is below the mean value), the association between HIV-related stigma and depression was significantly positive, b = 5.27, 95% CI = [3.03, 7.50], p < .01, whereas for the older group (whose age is above the mean value), the association between HIV-related stigma and depression was no longer significant, b = 1.53, 95% CI = [−1.70, 4.76], p > .05.
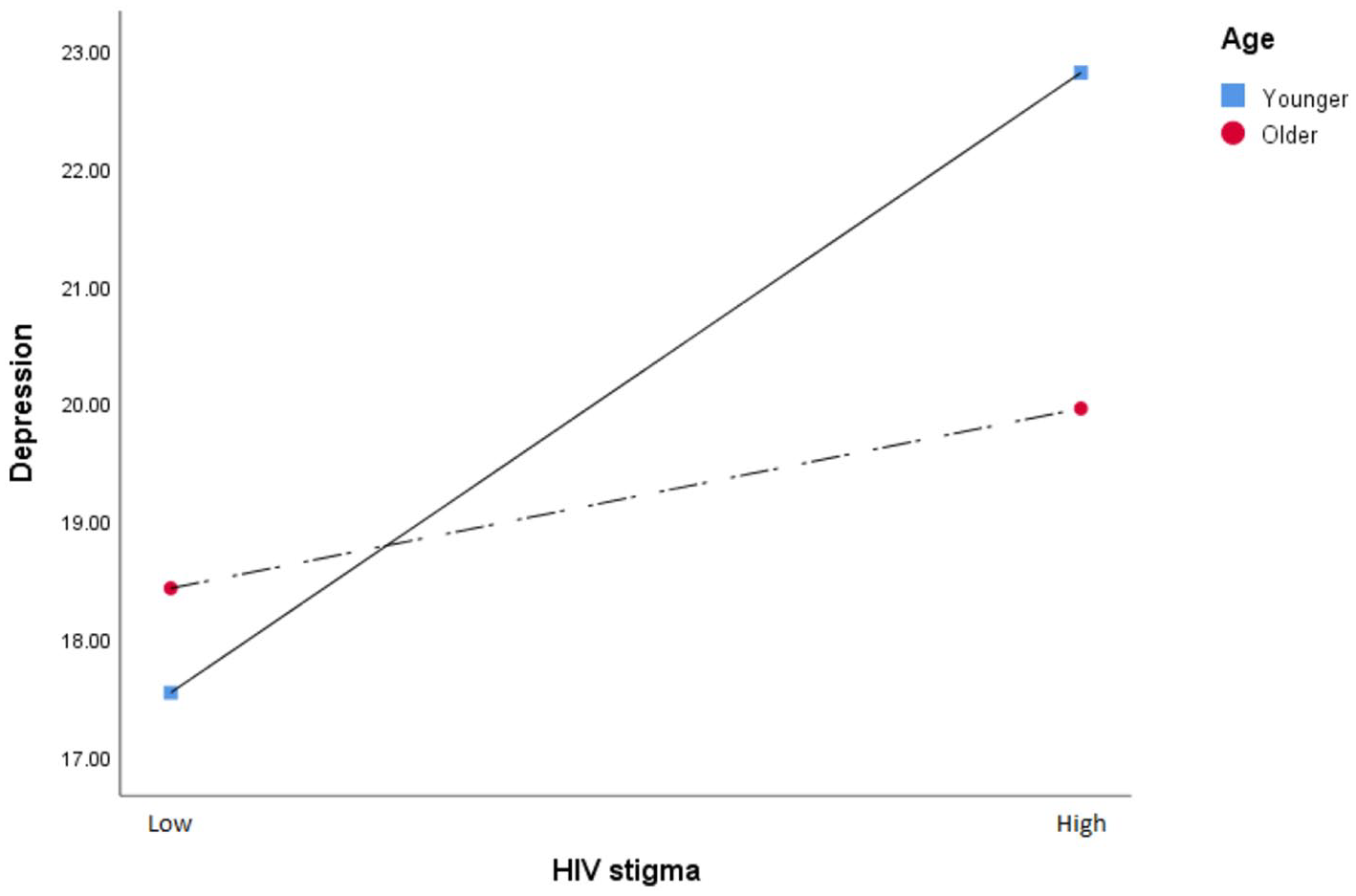
The Moderating Effect of Age on the Relationship Between HIV-Related Stigma and Depression
Conditional indirect effects were calculated based on age groups (see Supplemental Material). The indirect effect of sexual identity on depression through HIV-related stigma was significant in the younger group (β = −.17, p < .01). In comparison, it was not significant in the older group (β = .00, p > .05).
Discussion
The study is one of the first efforts to explore the relationship between sexual identity, HIV-related stigma, and depression in the MSM population across age groups. In the current sample, about two thirds of participants identified themselves as gay, and one third self-identified as heterosexual, bisexual, or not sure. The proportion of self-identified gay participants was lower than the rates reported in studies in the United States or Brazil (Fisher et al., 2018; Guimarães et al., 2018) but higher than another study previously conducted in China (Z. Yang et al., 2020). The results suggested that MSM who self-identified as gay were more likely to report lower HIV-related stigma, followed by fewer depressive symptoms. On the contrary, self-identified heterosexuality or bisexuality was associated with higher levels of HIV-related stigma and, in turn, worse depressive symptoms. The positive relationship between HIV-related stigma and depression could be moderated by age. Older MSM reported a smaller adverse effect of HIV stigma on depression, indicating that older age might act as a protector for mental health of MSM.
Our result revealed that the level of HIV-related stigma varied across MSM with different sexual identities. Such stigma disparity was further associated with the difference in mental health status. Interestingly, sexual identity was not directly related to depression in the current sample, which differs from previous studies among MSM living with HIV. Cho and Sohn (2016) illustrated that MSM who self-identified as gay reported significantly fewer depressive symptoms than those who were self-identified as bisexual/heterosexual and others. In contrast, Hylton et al. (2017) displayed that the odds of probable depression were significantly lower among MSM who self-identified as bisexual than those who self-identified as homosexual (Hylton et al., 2017). In line with previous studies (Amola & Grimmett, 2015), our results suggested that the sexual identity of MSM did not lead to psychological distress solely, but rather the depraved HIV-related stigma that negatively impacted mental health. As reported in previous studies among MSM living with HIV, 61% of the participants reported perceiving discrimination from the gay community because of their HIV serostatus, and such perceived HIV-related stigma was associated with higher levels of depression, anxiety, loneliness, avoidant coping strategies, and suicidal ideation (Courtenay–Quirk et al., 2006). Similar findings were demonstrated in younger MSM (Jeffries et al., 2015). The results propose a possibility that the inconsistency between sexual self-identity and sexual behavior might elicit stronger HIV-related stigma and, in turn, could exacerbate depression. As we are dedicated to achieving equal rights and dignity for lesbian, gay, bisexual, and transgender (LGBT) people, we have no reason to “intervene” sexual identity. With future efforts confirming the potential mechanism with longitudinal studies, interventions targeting the mental health of MSM living with HIV might consider placing greater emphasis on addressing HIV-related stigma and paying more attention to MSM who self-identified as heterosexual.
Results indicated that age could moderate the stigma-depression part within the pathway from sexual self-identity to depression through stigma. In the younger group, self-identified homosexuality had a significantly negative indirect effect on depression. Yet, such an indirect effect ceased in the older group. From a life span developmental perspective in health psychology (Spiro, 2007), individuals’ health behaviors and outcomes change through all phases of life as a synthesized result of biological factors, individual actions, and contextual influences. Older adults might be more efficient copers due to their greater experience in deciding which coping strategies work in which particular situations to achieve their goals (Aldwin et al., 1996). Such correlation of age and coping capacity was also reported in the PLWH (Brown & Grossman, 2014; Halkitis et al., 2017) and MSM populations (Brown & Grossman, 2014; Halkitis et al., 2017). The one-child policy in China initiated in the 1970s might expose young MSM to a more solemn “duty” of getting married and having children to coincide with the social norms (Z. Yang et al., 2020). We suggest mental health providers working with MSM living with HIV to pay more attention to younger MSM.
Limitations of the current study should be noted. First, sexual identity was measured with only one single item instead of a standardized scale (e.g., the Kinsey scale), preventing us from describing sexual identity comprehensively. Future studies are appreciated to mark participants’ sexual personhood with a flexible number on a scale rather than an arbitrary label (Drucker, 2012). Second, we did not consider other types of stigmas related to social status or identities (e.g., race, gender, sexual orientation, socioeconomic status) and examine the effect of intersectional stigma. Future studies might consider assessing different types of stigma and exploring the role of intersectional stigma in mental health among MSM. Third, causal relationships cannot be inferred from a cross-sectional design. The direction of the association between HIV-related stigma and depression remained unclear. Future longitudinal data are warranted to confirm and validate our findings. Fourth, the size of the indirect effects was small, despite significance. The variance of depression explained by the model was also limited (16.6%). These results suggested that other essential factors might exist besides HIV-related stigma that affects the mental health of MSM living with HIV.
Despite these limitations, the findings of the current study provide meaningful contributions in understanding the effect of sexual identity on mental health among stigmatized sexual and gender minorities by highlighting the potential mediating effect of HIV-related stigma and the protective effect of age. Our findings can inform future mental health interventions of considering the HIV-related stigma elicited by the inconsistency of sexual self-identity and sexual behavior, instead of focusing on the sexual identity itself among MSM. Future studies are also encouraged to consider socioeconomic status indicators and ethnic subgroup membership as potential moderators, which have been well documented to exacerbate risks for depression in this population (Hu et al., 2019). Further longitudinal research on the mental health of vulnerable populations with multiple stigmatized identities will allow a better understanding of strategies to reduce stigma, improve mental health, and achieve an overall better quality of life.
Supplemental Material
sj-docx-1-jmh-10.1177_15579883221087531 – Supplemental material for HIV-Related Stigma, Sexual Identity, and Depressive Symptoms Among MSM Living With HIV in China: A Moderated Mediation Modeling Analysis
Supplemental material, sj-docx-1-jmh-10.1177_15579883221087531 for HIV-Related Stigma, Sexual Identity, and Depressive Symptoms Among MSM Living With HIV in China: A Moderated Mediation Modeling Analysis by Tianyue Mi, Guanghua Lan, Xueying Yang, Xiaoming Li, Shan Qiao, Zhiyong Shen and Yuejiao Zhou in American Journal of Men's Health
Footnotes
Author Contributions
G.L., Z.S., and Y.Z. organized the study field and collected the data. X.L. and S.Q. contributed to the conceptual framework and variables construction. T.M. and X.Y. analyzed and interpreted the data and were major contributors in writing the manuscript. All authors read and approved the final manuscript.
Availability of Data and Material
The data sets used during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
The research protocol was approved by the Institutional Review Boards at both University of South Carolina in the United States and Guangxi CDC in China. All participants have given their written consent to participate in the survey.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was supported by National Institutes of Health (NIH)/National Institutes of Mental Health (NIMH) (Grant No. R01MH0112376). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH or NIMH.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
