Abstract
Gene polymorphism is one of the few factors that increases the risk of prostate cancer. T to C substitution in the 5’ promoter region of the CYP17 gene is hypothesized to increase the rate of gene transcription, increase androgen production, and thereby increase the risk of prostate cancer. Nevertheless, the inconsistencies originating from studies on CYP17 polymorphism and prostate cancer prompted this meta-analysis, to decipher the association between CYP17 polymorphism and prostate cancer. Most case-control studies addressing CYP17 polymorphism and prostate cancer were exhaustively searched from Web of Science, Google Scholar, and PubMed. The various genotype distributions as well as the minor allele distributions were retrieved. Pooled odds ratios (
Diet plays several roles that include but are not limited to protective, carcinogenic, and mutagenic agents. Enzymes of biotransformation metabolize the bioactive components of diets. When the expression or the function of these enzymes are altered through gene polymorphism, it increases the risk of cancer development. It is well documented that the susceptibility to carcinogenesis varies among individuals. Genetic polymorphisms play an important role and help to explain individual variations in cancer risk. Previous studies have been conducted to evaluate the prevalence of different gene polymorphic forms among cancer patients and normal control individuals (Rayner et al., 2004). The most studied polymorphisms of gene variants involved in carcinogenesis are mainly those that alter the bioavailability, metabolism, affinity, and behavior of several dietary constituents. Steroid hormones are suspected to play a role in the growth of several cancers (prostate and breast cancer), and the expressions of genes that regulate hormones may thereby affect disease risk (Elsamanoudy et al., 2016). One such gene is the CYP17. The conversion of 17-hydroxypregnenolone and 17-hydroxyprogesterone to dehydroepiandrosterone and androstenedione, respectively, is made possible by the CYP17 gene, which codes for cytochrome P450c17. A replacement of thymidine (T) with cytosine (C) at nucleotide 34 usually occurs in the 5’-untranslated promoter regions of the CYP17 gene as a result of gene polymorphism. This replacement is of scientific importance because the C variant allele (A2 allele), which is associated with higher levels of enzymatic activities, causes an increase in the circulating levels of androgen as compared to the T allele (A1 allele; Sharp et al., 2004). Association studies have been conducted to investigate a possible effect of CYP17 polymorphism on the risk of sporadic prostate cancer. Two studies reported elevated risk estimates (
Methods
Search Strategy
Most studies addressing the prevalence of CYP17 rs743572 polymorphism were exhaustively searched from PubMed, Web of Science, and Google Scholar. This study only considered studies that met the following inclusion criteria: (a) the study participants were male patients and the CYP17 rs743572 polymorphisms at the promoter region were determined; (b) the study reported the outcome (prostate cancer) as either incidence or prevalence; (c) the control groups used in the study were non-prostate cancer population and the study compared prostate cancer group versus control groups; (d) case control was used as the study design; and (e) the frequency distribution of the genotypes was provided. The exclusion criteria were: (a) not case-control studies; (b) review article or commentary; (c) duplicate studies; and (d) studies lacking relevant data.
Data Extraction
Information extracted from each article for this meta-analysis was: first author, year of publication, country, ethnicity, source of controls, number of cases and controls, and frequency of genotype distribution. To determine the association between gene polymorphism and prostate cancer, the reviewers extracted the following as additional data: the type of genotyping method used and the source of the control group.
Statistical Analysis
Using five genetic models, the role of CYP17 rs743572 polymorphism and prostate cancer susceptibility (Thakkinstian et al., 2005) were measured using odds ratios (
Results
From the literature search, a total of 85 studies or articles were screened from PubMed, Web of Science, and Google Scholar. After the removal of duplicates and evaluation of titles and abstract, 33 full text scripts were evaluated. After a secondary full text evaluation, 11 case-control studies reporting CYP17 rs743572 polymorphism and prostate cancer were finally included in this meta-analysis (Figure 1); each article’s characteristics for gene effect are detailed in Table 1. Except for four studies, all other studies were in agreement with the HWE. The minor A2 allele ranged from 31% to 48% among the various studies (Table 2). To estimate the pooled frequency (A2), we used data only from a non-prostate cancer population. There was high-pooled heterogeneity (

Prisma flow chart of study selection.
Characteristics of Studies Included in the Meta-Analysis.

Pooled Prevalence of A2 Allele.

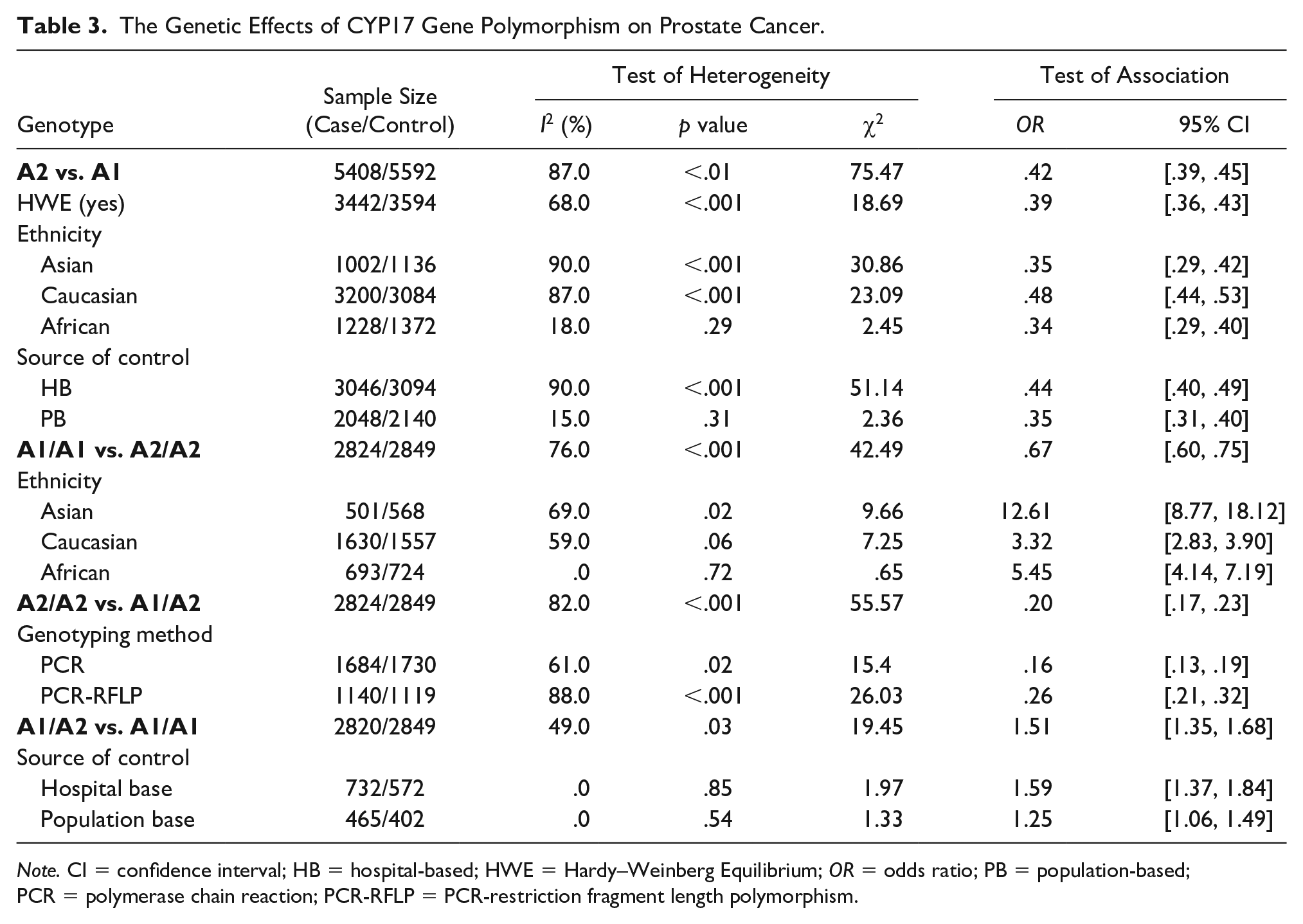
The Genetic Effects of CYP17 Gene Polymorphism on Prostate Cancer.
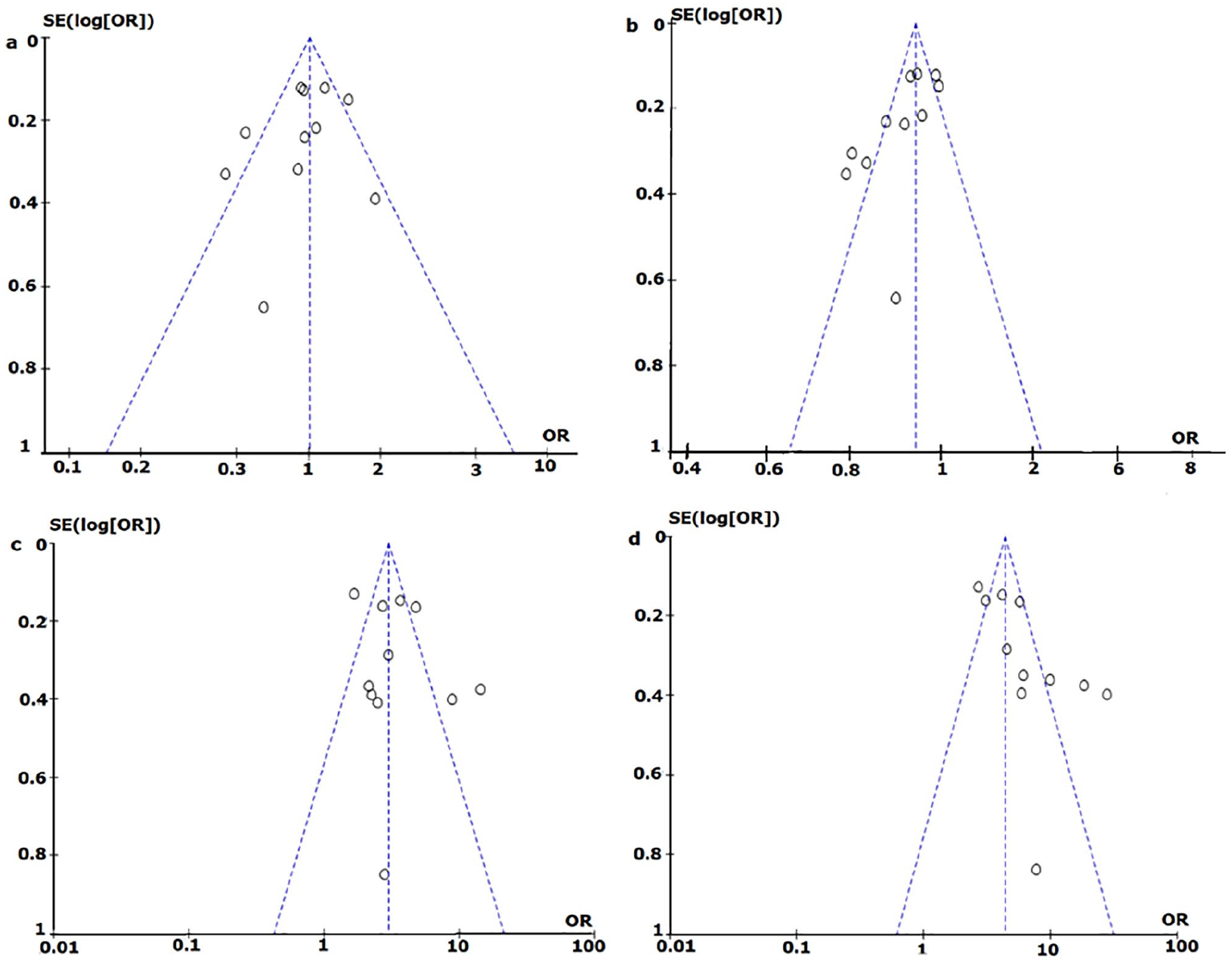
Begg’s funnel plot for (A

Forest plot of CYP17 rs743572 polymorphism in A1/A1 versus A1/A1 genotype models.

Forest plot of CYP17 rs743572 polymorphism in A1/A1 versus A1/A2 genotype models.

Forest plot of CYP17 rs743572 polymorphism in A1/A1 versus A2/A2 genotype models.
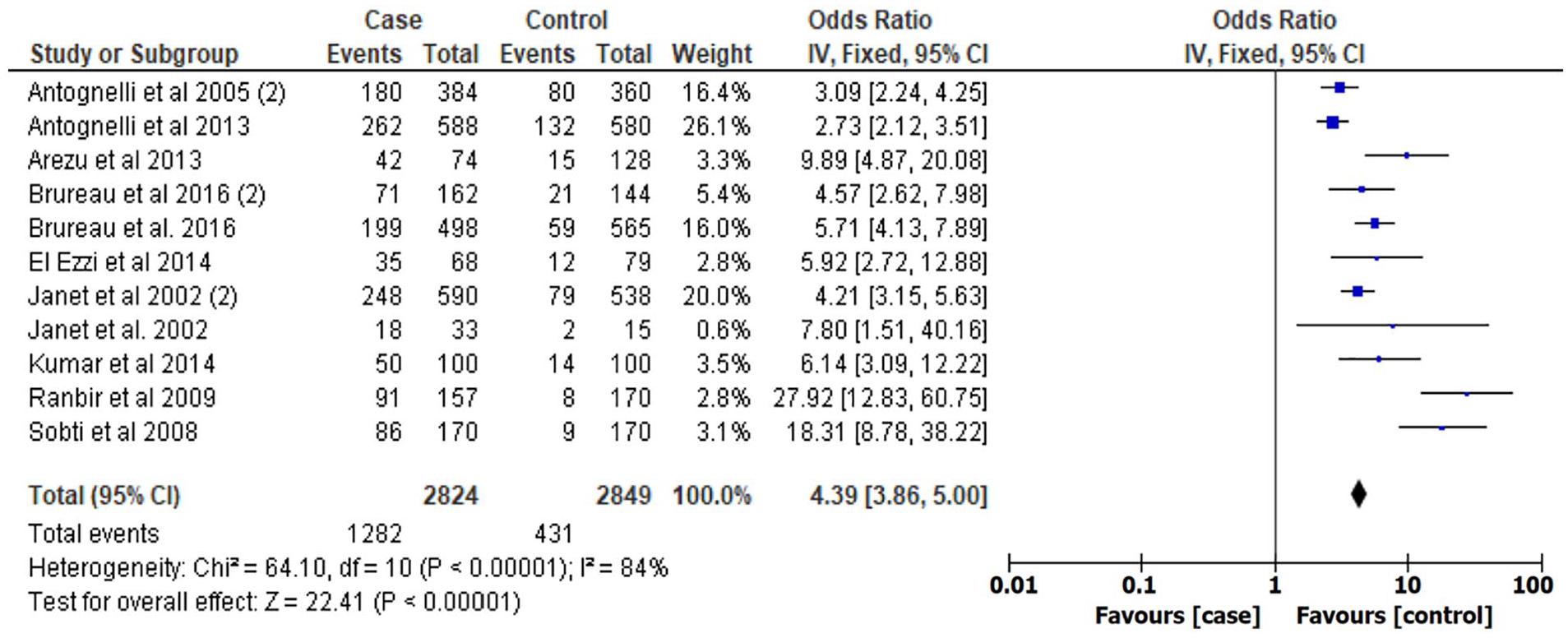
Forest plot of CYP17 rs743572 polymorphism in A1/A2 versus A2/A2 genotype models.
Discussion
The present meta-analysis, including 2824 cases and 2849 controls from case-control studies, explored the relationship between CYP17 rs743572 polymorphism and the risk for prostate cancer. Till now, there have been contradictory data concerning CYP17 risk allele and prostate cancer. This study realized some significant association between CYP17 rs743572 polymorphism and the risk of prostate cancer except for the A1/A1 versus A1/A2 and A1/A1 versus A1/A1 genotype models. With the subgroup analysis of the various genotype models, ethnicity was a major risk factor for prostate cancer. Several authors have reported the association between CYP17 rs743572 polymorphism and the risk of prostate cancer using African ancestry as a determinant (Lunn et al., 1999; Kittles et al., 2001; Stanford et al., 2002; Cicek et al., 2004; Sarma et al., 2008; Beuten et al., 2009; Dos Santos et al., 2002). This meta-analysis disagrees with a study by Wang et al. (2011), who reported no significant association between CYP17 rs743572 polymorphism and prostate cancer in Caucasians and Asians. Although there may be some differences in the genetic makeup and some differences in environmental conditions between the various ethnic groups, this did not translate into a protective factor for prostate cancer although there were some differences in the degree of the risk to prostate cancer. It is also likely that the observed ethnic similarities may be due to studies that had a moderate sample size, which may have provided sufficient statistical power to detect any slight effect changes. According to Lewis and Lee-Robichaud (1998), the A1/A1, A1/A2, and A2/A2 genotypes of CYP17 gene are known to mediate two key steps in sex steroid biosynthesis.
The presence of the CYP17 A2 allele has been described to be an independent risk factor for a subset of breast cancers. However, the present results indicate that the A2 allele is not a significant associative risk factor of prostate cancer per the allele model using the stratified analysis of HWE, ethnicity, and the source of control as variables. This is in agreement with studies by Wang et al. (2011) and Ragin et al. (2010) where the A2 allele was marginally, but not significantly, associated with prostate cancer risk. Other studies have reported conflicting results on the CYP17 genotype in prostate cancer patients, indicating either an increased risk of prostate cancer in the presence of the allele A2 or an increased risk with the A1A1 genotype (Wadelius et al., 1999).
The increased transcription efficiency of gene and the enhancement of enzymatic activity are considered to be improved by A2 allele, which in turn enhance the synthesis of androgen thereby increasing the risk of prostate cancer (Nedelcheva et al., 1999; Sharp et al., 2004). However, a study by Söderström et al. (2002) reported no significant differences in the levels of testosterone as well as androgens and their metabolites in men based on their CYP17 genotypes. Also, the A2 allele determines the synthesis of a less enzymatically active protein or fewer quantities of the protein and consequently to a block or at least to a reduction of the androgen biosynthesis pathway in which the cytochrome P450c17 gene seems to be the rate-limiting step.
In a study by Makridakis et al. (1997), it was suggested that there is no known proof to link the A2 allele to the strong and consistent increased androgen levels. As androgens partake in the causal pathway of prostate cancer, the nonsignificant associative effect of CYP17 polymorphism on androgen levels is consistent with the findings of this study.
The important role in mediating androgen biosynthesis makes the CYP17 polymorphism a compelling candidate for a susceptibility gene for prostate cancer. This is also proven by the fact that there is an increasing body of evidence suggesting that CYP17 polymorphism may be regarded as a biomarker for prostate cancer risk. New drug therapies developed to target the CYP17 enzyme in an effort to decrease local tumor production of androgens have rekindled the attention on CYP17 and prostate cancer-specific mortality. The treatment of advanced prostate cancer is usually by Ketoconazole, and this has nonspecific CYP17 inhibitory qualities. The introduction of Abiraterone acetate showed antitumor activity, which was considered as a selective and a precise drug for the inhibition of CYP17 in a Phase I trial that included 21 men facing castrate-resistant prostate cancer (Attard et al., 2008). We can attempt to increase prostate cancer-specific survival, through genetic variation of CYP17, which can be achieved through an alteration of enzymatic activity.
Limitations
This study admits the possibility of serious confounding bias, which may be as a result of lack of information. A more precise analysis could have been conducted if we had more information on individual studies. Therefore, the results of this study were unadjusted estimates instead of conducting adjusted estimates of some factors such as age. Several factors moderate the risk of prostate cancer, which may include: gene–gene interaction, gene–environment interaction, and the effect of different polymorphic loci of the same gene. The limitation of not obtaining the original information of the various studies impeded further evaluation of the effect of these factors on the risk of prostate cancer. The possibility of publication bias cannot be written off, although none was detected using the Begg’s funnel plot. The reliance on the available subjects of published papers may exaggerate the true effect due to publication bias. Meta-analyses are prone to numerous potential biases, such as measurement error and genotyping error, in addition to the aforementioned publication bias.
Conclusions
From this meta-analysis, it can be inferred that CYP17 polymorphism may be a risk factor for prostate cancer. Ethnicity is a major risk factor for prostate cancer. Although some genotype models were associated with the risk of prostate cancer, we should be mindful when interpreting the results of this study because of the limited number of studies used and the small sample size. The interplay of various factors such as gene–gene and gene–environment interactions should be researched to provide a better understanding and to ascertain a concrete association between the CYP17 polymorphism and prostate cancer risk.
Footnotes
Author Contributions
CYE and YW contributed to the conceptualization of the work, data retrieval, and analysis; LW contributed to the conceptualization of the work and analysis; CA, WW, EKD and SY contributed to the data retrieval and analysis. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of Data and Material
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request
