Abstract
The aim of this study was to investigate the frequency of nocturnal sperm emissions (NSE) in varicocele patients after varicocele surgery. A total of 127 patients, 96 varicocele (Group 1) and 31 patients with inguinal hernia (Group 2) were included in this study. Mean age, laterality of surgical procedures, spermiogram results, marital status, and postoperative serum hormone levels were noted for all patients. Two groups were compared in terms of Beck depression score (BDS) and anxiety scores (AS). The frequency of NSE and libido changes in the patients during 10 days postoperatively was evaluated. The number of the patients who had NSE and increased libido were significantly higher in the varicocelectomy group when compared with the control group. No significant difference was noted between the groups in terms of BDS, AS, and serum hormone levels. No association was reported between BDS, AS, and serum hormone levels and the presence of NSE in Group 1. The incidence of NSE was higher in younger men. Increased libido was significantly associated with NSE in Group 1. Cord dissection during surgery may be a factor on increased frequency of NSEs in varicocele patients.
Introduction
Varicocele can be defined as collection of abnormally dilated, tortious spermatic veins (Baazeem et al., 2011; Choi & Kim, 2013). The prevalence of varicocele is between 10% and 15% in the general population (Choi & Kim, 2013; Gorelick & Goldstein, 1993; Sabanegh & Agarwal, 2012; Stahl & Schlegel, 2011). The prevalence rate is increased in men with primary and secondary infertility (30% to 35% and 70% to 80%, respectively; Gorelick & Goldstein, 1993; Stahl & Schlegel, 2011). Varicocele is the most common surgically correctable cause of male infertility (Choi & Kim, 2013; Dubin & Amelar, 1971).
Various modalities have been defined for the surgical treatment of varicole, including embolization, open varicocelectomy, laparoscopic varicocelectomy, and microsurgical varicocelectomy (Choi & Kim, 2013). Among these treatment methods, microscopic inguinal or subinguinal varicocelectomy are mostly preferred techniques with relatively high success and low complication rates (Baazeem et al., 2011; Choi & Kim, 2013; Sabanegh & Agarwal, 2012).
Nocturnal sperm emission (NSE) is an autonomous reflex mediated by the sympathetic nervous system (Hovav, Dan-Goor, Yaffe, & Almagor, 1999). Although little is known about the actual cause of NSE, there are many potential hypotheses about how they are caused. The aim of this study was to determine the frequency of NSE in varicocele patients after varicocele surgery.
Materials and Methods
Following the ethical committee approval, a total of 96 varicocele patients (Group 1) and 31 control patients who had inguinal hernia (Group 2) were included in this study. All varicole patients underwent subinguinal microsurgical varicocelectomy, and tension-free mesh hernia repair was performed in all patients with inguinal hernia in the control group. Mean age, laterality of surgical procedures, spermiogram results, and marital status were noted for all patients.
Postoperative serum follicle-stimulating hormone, luteinizing hormone, and testosterone levels were noted for all patients included in the study. Two groups were compared in terms of Beck depression score (BDS) and anxiety score (AS). The frequency of NSE and libido changes of these patients was evaluated during the 10-day postoperative period. Statistical analyses were performed with SPSS 15.0, and a p value of <.05 was considered as statistically significant. Chi-square test was used to compare postoperative NSE frequency, libido, and serum hormone levels. Mann–Whitney U test was used to compare BDS and AS between the groups.
Results
The mean age of the patients in varicocelectomy group was 26.7 years, and mean age of the patients in inguinal hernia repair group was 30.5 years (p > .05). Seventy-one patients (74%) had left-sided varicocele and 25 patients (26%) had bilateral varicocele in Group 1. In Group 2, 12 patients (38.7%) underwent left-sided, 2 patients (6.5%) underwent bilateral, and 17 patients (54.8%) underwent right-sided inguinal hernia repair (p < .001). Thirty-eight patients (39.6%) were single, and 58 patients (60.4%) were married in Group 1. In Group 2, 9 patients (29%) were single, and 22 patients (71%) were married (p = .346). Preoperative spermiogram results revealed normospermia in 39 patients (40.6%), oligospermia in 55 patients (57.3%), and azoospermia in 2 patients (2.1%) in Group 1. 28 patients (90.3%) had normospermia, and 3 patients (9.7%) had oligospermia in Group 2. Spermiogram results revealed azoospermia in none of the patients in the control group (p < .001).
Incidence of NSE was evaluated in both groups presurgically. A similar presurgery NSE incidence was determined between Groups 1 and 2. No statistically significant difference was observed between the groups (p > .05). Data showing presurgical NSE incidence are reported in Table 1.
Presurgical Incidence of NSE in Groups 1 and 2.
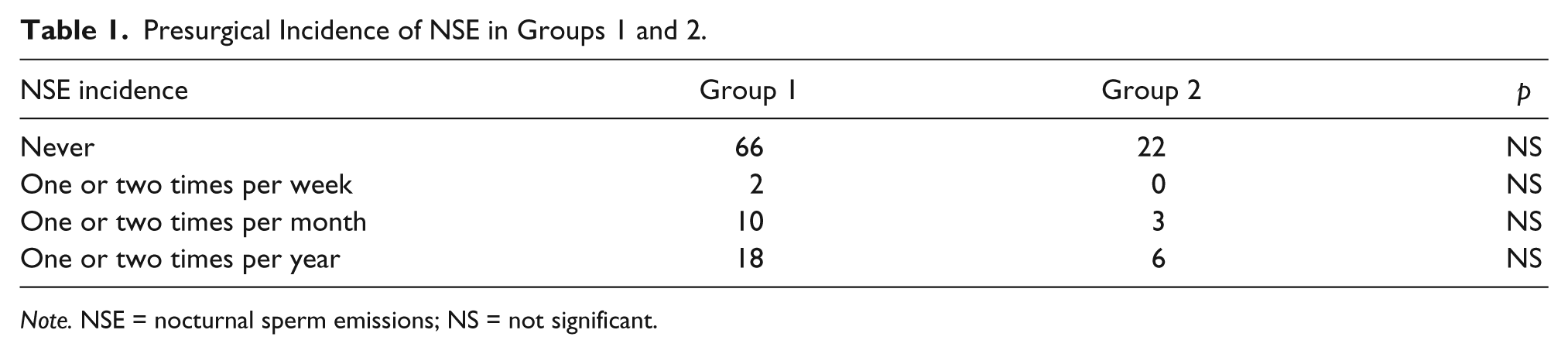
Note. NSE = nocturnal sperm emissions; NS = not significant.
In presurgical examination, there were 11 patients with libido decrease in Group 1 and 4 patients in Group 2 in the past 3 months. No statistically significant difference was observed in libido decrease between the two groups (p > .05).
In Group 1, 64 patients (66.7%) experienced NSE postoperatively, and no NSE was noted for 32 patients (33.3%). Two patients (6.5%) had NSE and 29 patients (93.5%) had no NSE postoperatively in Group 2. In the varicocelectomy group, 20 patients (20.8%) presented with increased libido postoperatively, whereas no change was noted in 76 patients (79.2%). In the control group, an increase in libido was noted in none of the patients postoperatively.
Number of the patients who had NSE and increased libido after surgery were significantly higher in the varicocelectomy group when compared with the control group (p < .001 and p = .006, respectively). No significant difference was noted between the two groups in terms of BDS, AS, serum testosterone, and follicle-stimulating hormone/luteinizing hormone levels (p > .05, p > .05, p = .195, p = .154, respectively). No association was reported between BDS, AS, and serum hormone levels and the presence of NSE in Group 1. The incidence of NSE was higher in younger men. Increased libido was significantly associated with presence of NSE in varicocelectomy group. Demographic characteristics and postoperative outcomes of all patients included in the study are summarized in Table 2. A dose of 75-mg diclofenac sodium was used intramuscularly in both groups with 12-hour interval for pain. A dose of 50 mg pethidine was used intramuscularly for chronic pain in seven patients in Group 1 and four patients in Group 2. When narcotics usage was considered, no difference was detected between the groups (p > .05). Diclofenac sodium was given orally for pain control after discharge.
Demographic Characteristics and Postoperative Outcomes of the Patients in Groups 1 and 2.

Note. NSE = nocturnal sperm emissions; FSH = follicle-stimulating hormone; LH = luteinizing hormone; BDS = Beck depression score; AS = anxiety score.
Discussion
Varicocele is the most common surgically correctable cause of male infertility (Choi & Kim, 2013; Dubin & Amelar, 1971). The majority of the men with varicocele are asymptomatic and fertile, with approximately 20% experiencing physical discomfort or problems associated with fertility (Goldstein, 2012; Mehta & Goldstein, 2013). Varicocelectomy is recommended in cases of a clinically palpable varicocele with abnormal semen parameters (Mehta & Goldstein, 2013). Previous studies identified an association between varicocele and abnormal sperm DNA quality, impaired testosterone production, testicular pain, and testicular hypotrophy (Choi & Kim, 2013; Goldstein, 2012; Mehta & Goldstein, 2013).
Varicocele has a progressive negative effect on testicular function (Choi & Kim, 2013; Mehta & Goldstein, 2013). Treatment alternatives for surgical correction of varicocele include inguinal, high retroperitoneal, laparoscopic surgery, and inguinal or subinguinal microsurgical varicocelectomy (Mehta & Goldstein, 2013). Potential postoperative complications include hydrocele formation, scrotal hematoma, infection, and testicular hypertrophy (Goldstein, 2012; Mehta & Goldstein, 2013). Microsurgical varicocele repair helps clinicians preserve lymphatics and testicular arteries during the surgical procedure (Mehta & Goldstein, 2013; Mirilas & Mentessidou, 2012). Microsurgical varicocelectomy is the gold-standard technique with significantly lower postoperative recurrence and complication rates compared with other surgical methods (Choi & Kim, 2013; Mehta & Goldstein, 2013; Mirilas & Mentessidou, 2012).
Subinguinal microsurgical varicocelectomy is routinely performed in our clinic. In our daily clinical practice, it was observed that majority of men who underwent varicocelectomy surgery presented with increased NSE postoperatively. Investigating the potential increase in postoperative NSE frequency in patients who underwent microsurgical varicocelectomy was aimed in the recent study. The frequency of NSE and libido changes between the patients who underwent varicocelectomy and tension-free mesh inguinal hernia repair was compared. The control group included the patients who underwent inguinal hernia repair since both procedures were similar in terms of surgical approach, operation time, anesthesia, postoperative follow-up, and possible surgical stress. In a previous study, Bulus, Dogan, Tas, Agladıoglu, and Coskun (2013) concluded that tension-free mesh hernia repair does not have any negative effect on testicular perfusion and sexual function and can be safely performed for the treatment of inguinal hernia (Bulus et al., 2013). To the best of our knowledge, this is the first study investigating the possible role of varicocelectomy procedure on the postoperative increase in NSE frequency and libido.
In the present study, the number of the patients who had NSE and increased libido after surgery were significantly higher in the varicocelectomy group when compared with the control group. The incidence of NSE was higher in younger men. Increased libido was significantly associated with presence of NSE in varicocelectomy group.
NSE is an autonomous reflex mediated by the sympathetic nervous system (Hovav et al., 1999). In a previous study, the authors reported that NSE is significantly correlated with a calculated free testosterone index in a nonclinical group of 9th- and 10th-grade Caucasian boys (Udry, Billy, Morris, Groff, & Raj, 1985). In a different study, Finkelstein et al. (1998) identified that increased testosterone may cause increases in NSE. In this study, there was no significant difference between the patients who underwent varicocelectomy and the control group in terms of serum hormone levels. There was also no association between serum hormone levels and the presence of NSE in Group 1.
It was hypothesized that the surgical stress might be a potential factor affecting postoperative NSE frequency and change in libido. No significant difference was noted between the groups for BDS and AS, and there was no association between BDS and AS and the presence of NSE in Group 1.
The findings of the current study revealed a significant increase in NSE frequency and libido following microsurgical varicocele repair. No association was demonstrated between the postoperative stress, serum hormone levels, and NSE frequency. Spermatic cord dissection during varicolectomy might be a potential factor on increased frequency of NSEs in varicocele patients. The limitations of the current study are short patient follow-up period and low number of patients in the control group.
Conclusion
NSEs and libido significantly increase after microsurgical varicocelectomy procedure. Cord dissection might be a possible factor that causes an increase in NSE frequency and libido following the surgery. New studies with a higher number of patients and more appropriate follow-up periods are required.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
