Abstract
The aim of this research was to compare the health and lifestyle behaviors between male and female nursing professionals. Biological, workplace, and lifestyle factors as well as health behaviors and outcomes are reported as different between male and female nurses. Although male nurses show distinct health-related patterns and experience health disparities at work, few studies have investigated health differences by sex in a large cohort group of nursing professionals. This observation study of Australian and New Zealand nurses and midwives drew data from an eCohort survey. A cohort of 342 females was generated by SPSS randomization (total N=3625), to compare against 342 participating males. Measures for comparison include health markers and behaviors, cognitive well-being, workplace and leisure-time vitality, and functional capacity. Findings suggest that male nurses had a higher BMI, sat for longer, slept for less time, and were more likely to be a smoker than their female nurse counterparts. Men were more likely to report restrictions in bending, bathing, and dressing. In relation to disease, male nurses reported greater rates of respiratory disease and cardiovascular disease, including a three times greater incidence of myocardial infarction, and were more likely to have metabolic problems. In contrast, however, male nurses were more likely to report feeling calm and peaceful with less worries about their health. Important for nurse workforce administrators concerned about the well-being of their staff, the current study reveals significant sex differences and supports the need for gender-sensitive approaches to aid the well-being of male nurses.
Introduction
The importance of workplace health is ever present and, in the context of health care providers, there is strong momentum toward optimizing the health of workers who are responsible for patient care Chan and Perry (2012). The nursing workforce is unique both in terms of being the largest subgroup of health care providers and for its longstanding gender disparity wherein women account for approximately 90% of nurses (Auebach, Staiger, Muench, & Buerhaus, 2012). Recognizing the need to support the health of nurses, there is strong interest in better understanding sex differences and health behaviors as a means to informing gender-sensitive targeted workplace health promotion programs (Oliffe & Han, 2014). The current study by detailing health behavior and outcome sex differences among female and male nurses offers empirical weight to prompt thoughtful consideration about the need for targeted gender-sensitive workplace health promotion programs.
Background
Sex, Gender, and Health
Johnson and Repta (2012) eloquently differentiate sex and gender in health to distil the biological origins of sex (e.g., genitalia, hormones) and the diversity and range of socially informed gendered health behaviors. Although there is inherent value to comparing health behaviors and outcomes by sex, there is also increasing interest in combining sex and gender analyses to contextualize the differences and similarities within and between men and women’s health (Galdas, Johnson, Percy, & Ratner, 2010). Most often cited are life expectancy differences between men and women wherein women live longer than men (Lipsky, Cannon, & Lutfiyya, 2014). This longstanding epidemiological profile in Western countries is often used to make the case for a focus on men’s health, which in turn garner biological sex (Dogan et al., 2014) and/or behavioral gender explanations (Courtenay, 2000). Upstream risk factors (e.g., alcohol overuse, unprotected sex) are also routinely chronicled to explain men’s poor health outcomes compared to women (Lyons, Emslie, & Hunt, 2014). For example, poor diets, sedentary lifestyles, and testosterone levels in males often foreground the fact that men are more likely than women to be overweight (two-thirds of adult males are obese, larger proportion of men are overweight compared to women based on BMI measures) (Saad & Gooren, 2011; Templeton, Sainsbury, & Thompson, 2011). In terms of gender, “toughness” is a prevailing masculine ideal, and competitiveness and avoidance of health care services are manly norms used to explain male heart disease and workplace injuries (Lipsky et al., 2014; Templeton et al., 2011). Inversely, feminine ideals are synonymous with care for oneself and looking after the health of others (vocationally as nurses and/or in caring for the health of the men in women lives) (Lee & Owens, 2002).
Gender and Nursing
Typically, nursing as an occupation is acknowledged as a demanding job in accounting for the high burnout within the profession (Erickson & Grove, 2007). Excessive workload, exposure to hazardous environments, and limited skill and knowledge development due to the routine nature of the work have also been cited as contributing to nurse recruitment and retention challenges (O. Evans & Steptoe, 2002; Hsu, Chen, Yu, & Lou, 2010; Walters et al., 1996). In terms of sex differences, both student attrition and burnout rates among men in nursing have been linked to gender role conflict fueled by the female-dominated nature of nursing, prevalent stereotypes, and gender bias in nursing education (Hsu et al., 2010). This may go some way to explaining the higher rates and episodes of sick leave compared to female nurses found in a study of UK-based men in nursing (O. Evans & Steptoe, 2002). Coupled with this are claims that male nurses reflect the wider men’s health literature wherein men have high self-perceived health despite engaging in risky behaviors including alcohol and tobacco overuse (Limiñana-Gras, Sánchez-López, Román, & Corbalán-Berná, 2013).
Discussions of gender in health have typically focused on women; yet conspicuously absent from the literature are sex comparisons and gender analyses detailing female nurse’s work and/or self-health behaviors. The few articles addressing gender and male nurses have detailed the specificities of men’s work-related experiences. For example, male nurses are often perceived as physically powerful, which situates them as having the strength to protect others (J. Evans, 2004). Mathews (2001) reported that when asked to describe the care they provide, male nurses tended to focus on technical aspects, including taking blood pressure and dispensing medications. Similarly, within acute care practice, many male nurses work in ICUs and emergency departments, and this high-adrenaline clinical work, though challenging, is understood to demand autonomy and draw respect from others (Schoonover-Schoffner, 2006). Although these studies detailed connections between masculinities and male nurse’s work, the health behaviors of male nurses, and for that matter female nurses, are poorly understood in sex and gender research.
Clearly, sex and gender analyses are vital to differentiating and developing nuanced understandings about the health practices of female and male nurses (O. Evans & Steptoe, 2002; Limiñana-Gras et al., 2013). The Australian and New Zealand Nurses and Midwifes e-Cohort study is a large, self-reported survey of practicing nurses across an array of workplaces. Using findings drawn from this data set, we compared the health and lifestyle behaviors between male and female nursing professionals in order to maximize thoughtful consideration to the need for developing targeted gender-sensitive workplace health promotion programs.
Methods
Setting
Data here were drawn from the Australian and New Zealand Nurses and Midwifes e-Cohort study (N = 3,968), a self-reported survey of practicing nurses and midwives across multiple working environments (Huntington et al., 2011; Tuckett et al., 2009). The e-cohort data set contains longitudinal, population-based information, making possible the examination of factors associated with the nurse and midwife workforce and health outcomes. In the primary round of delivery, Australia and New Zealand nurses and midwifes were recruited during 2006–2008, with participants completing a large survey based on a range of instruments, focused on two broad content themes. The sample, recruitment, and survey structure have been described in detail elsewhere (Huntington et al., 2001; Tuckett et al., 2009). In brief, the two broad content themes questioned the following:
Work–life balance to describe and quantify the factors associated with the retention of the existing workforce and patterns of employment; and
Staying healthy to measure the prevalence, incidence, and associated risk factors of physical, mental, and health behaviors, including musculoskeletal disorders and workplace injuries in the cohort.
The survey consisted of 108 questions based on validated tools (e.g., SF-36, International Physical Activity Questionnaire) and direct assessments of markers of workforce involvement and health (e.g., years of shift work, BMI, diagnosed disease) with participants requested to complete them all. Ethics approval was provided by the Human Research Ethics Committee, The University of Queensland, Australia. Of the 290,000 Australian and 44,400 New Zealand registered and enrolled nurses and midwives eligible for inclusion at the time, 8,247 participated in the survey (Turner et al., 2009) and 3,968 had data relevant to this analysis. Recruitment was by an online expression of interest and admittance to the survey web page following the submission of demographic data and contact details. On average, it took 40 min to complete the survey.
For the purpose of this research, total male participant numbers were aggregated and an equal number of female respondents were randomized from the remaining cohort for comparison. Specifically, of the eligible responders to the eCohort survey, 342 identified as male and 342 of the potential 3626 respondents who identified as female were randomized to the study through SPSS case randomization with unselected cases deleted and the male and female data sets merged.
Comparisons were made on items with an underlying theme of health and well-being that included health markers and behaviors, cognitive well-being, workplace and leisure time vitality, and functional capacity. Specifically, between-group differences for age, body mass index (BMI, kg/m2) and category (underweight: <18.5 kg/m2, normal: 18.6–24.9 kg/m2, overweight: 25.0–29.9 kg/m2, and obese: ≥30 kg/m2), MET min/week (total, sitting, walking, moderate and vigorous intensity), days off sick, years of shift work, and hours of sleep were compared. In addition, the presence of a diagnosed disease and capacity for daily activities (e.g., walking 1 km, bathing) were compared. Finally, a sex comparison was undertaken based on response to the SF-36 and used to inform physical and mental well-being over the previous 4 weeks.
Statistical Analysis
All data were processed in SPSS version 22.0 (SPSS Inc., Chicago, IL). Prior to grouping, data were extensively reviewed and outliers eliminated by case. Descriptive and frequency analyses were undertaken dependent on the variables status. Between-group comparisons on categorical data were by Pearson’s chi-squared test (χ2) and where applicable logistic regressions were undertaken on disease diagnosis to identify gender-specific odds ratio (r) and 95% confidence intervals (CIs). For continuous variables a between-group t test was conducted. An alpha of .05 was required for significance. All data are represented as mean ± standard deviation.
Results
Participant Demographic Characteristics
The cohort (n = 684) were 42.4 ± 10.3 years old, with 40% reporting shift work for 10 or more years. Shift work is defined as work performed primarily outside typical daytime hours and includes evening shifts, rotating shifts, irregular shifts, and flexitime (Greene-McKenzie & Scofer, 2006; Zhao, Bogossian, Song, & Turner, 2011). Women were more likely to be new to shift work (14.1% 1 year and 12.3% 2 years), but men more than twice as likely to have been doing shift work for 6 years (11.0%; χ2 = 17.177, df = 6, p = .009). Table 1 contains cohort and group characteristics for age, BMI, sitting and physical activity, and days off sick.
Group and Between Group Differences for Age, BMI, Sitting Time, and Days Off Sick.
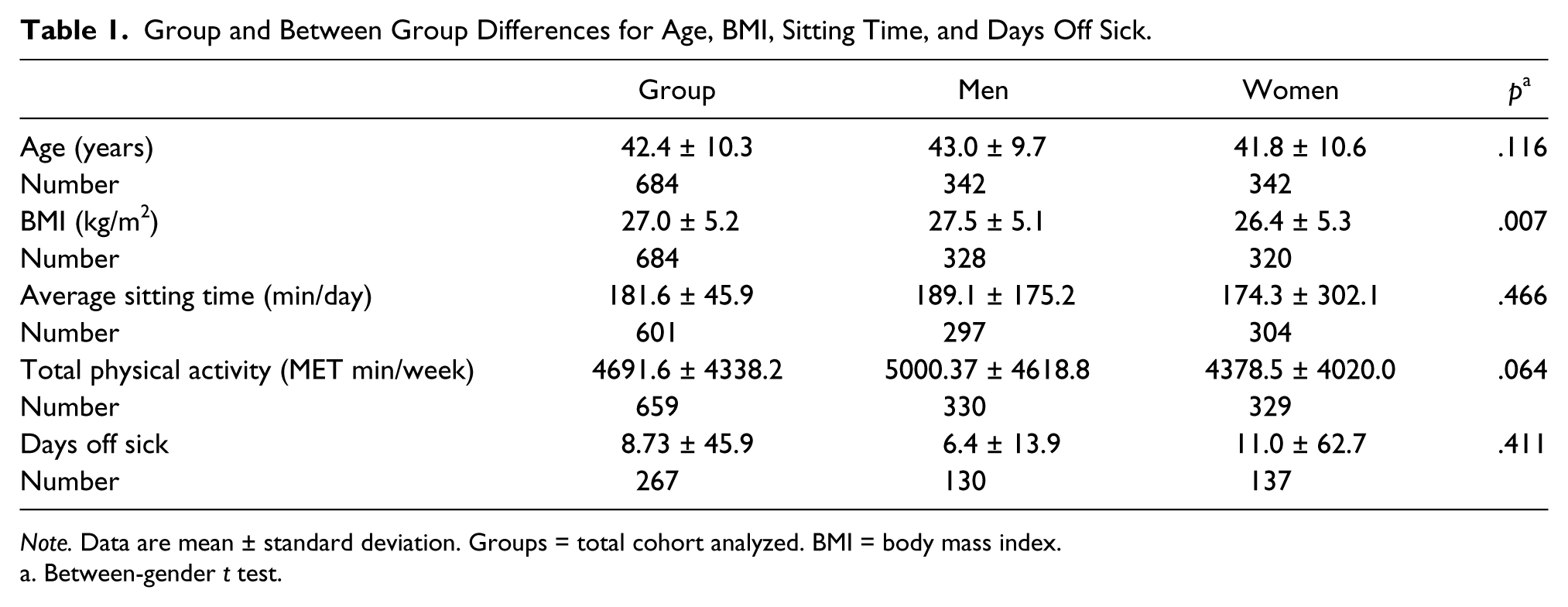
Note. Data are mean ± standard deviation. Groups = total cohort analyzed. BMI = body mass index.
Between-gender t test.
Clinical Measures
Male nurses had a significantly higher BMI than the women, 27.5 ± 5.0 kg/m2 versus 26.4 ± 5.3 kg/m2, respectively (p = .007; Table 1). Consequently, men were more likely to be overweight (BMI = 25.0–29.9 kg/m2) than their female nurse counterparts (47.9%; χ2 = 23.923, df = 3, p < .001; OR = 2.11, 95% CI = 1.53–2.91).
Men also reported greater presence of cardiovascular disease symptoms and risk factors. In brief, men were significantly more likely to have a diagnosis of Type 2 diabetes (χ2 = 4.097, df = 1, p = .043; OR = 2.18, 95% CI = 1.01–4.70), elevated serum triglyceride (χ2 = 9.547, df = 2, p = .002; OR = 2.31, 95% CI = 1.34–3.98), report having high blood pressure (χ2 = 3.895, df = 1, p = .048; OR = 1.58, 95% CI = 1.00–2.51), and have elevated serum cholesterol (χ2 = 13.708, df = 2, p < .001; OR = 2.14, 95% CI = 1.42–3.22) than women (Table 2 and Figure 1). Furthermore, men were significantly more likely to have been diagnosed with a basal cell skin cancer (χ2 = 4.968, df = 1, p = .026; OR = 1.98, 95% CI = 1.08–3.64) and to have experienced gout (χ2 = 4.641, df = 1, p = .031; OR = 2.74, 95% CI = 1.06–7.08) (Table 2 and Figure 1). In addition, the prevalence of myocardial infarction (χ2 = 4.597, df = 1, p = .032) and emphysema or chronic bronchitis (χ2 = 3.868, df = 1, p = .049) was higher in the men than the women.
Gender differences in diagnosed disease by Pearson’s χ2 test.
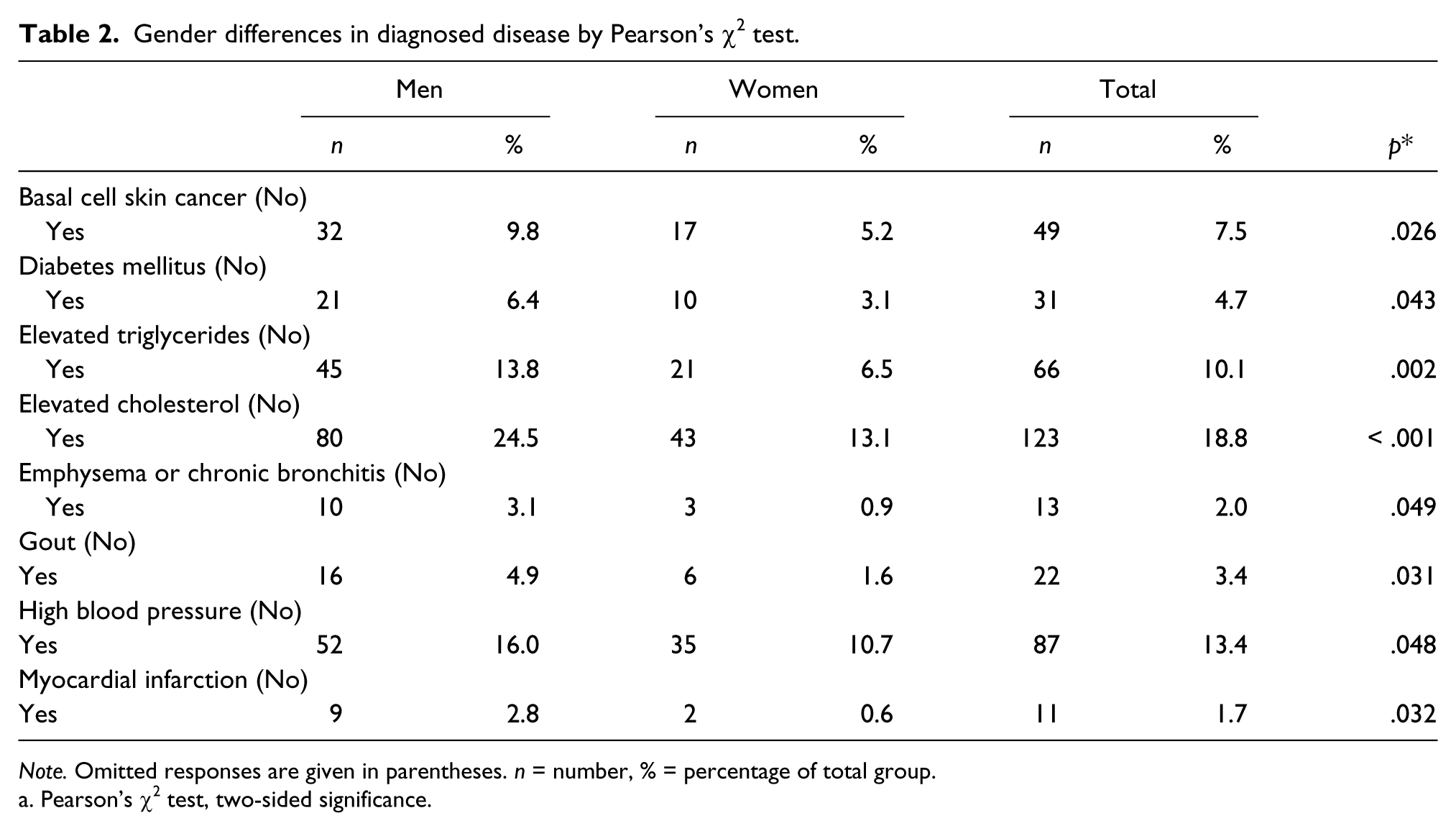
Note. Omitted responses are given in parentheses. n = number, % = percentage of total group.
Pearson’s χ2 test, two-sided significance.

The odds ratios (95% confidence interval) of male nurses experiencing diagnosed disease or poor clinical measures compared to female nurses.
Lifestyle Behaviors
Nurses reported 300.5 ± 214.1 min of at-work or leisure-time physical activity per day (range: 0–954 min/day) averaged across the week. Men were twice as likely to be categorized as having high sitting time (>490 min/day) (6.1%, χ2 = 6.353, df = 2, p = .042; Table 1) and report sleeping less than the 7–9 hours per night (41.2%, χ2 = 6.317, df = 2, p = .042). In addition, more men reported being a current smoker (21%) compared to women (χ2 = 8.622, df = 1, p = .003). Men were also more likely to report being restricted in bending, kneeling or stooping, and bathing and dressing activities “all of the time” (9.2% [χ2 = 7.975, df = 2, p = .019] and 5.2% [χ2 = 7.214, df = 2, p = .027], respectively).
Self-Reported Health Status and Mental Well-Being
Women were twice as likely to report they had accomplished less “some of the time” in the previous 4 weeks due to their physical health (17.8%) (χ2 = 14.620, df = 4, p = .006). Men were 3 times more likely than female nurses to report feeling full of life and calm and peaceful “all of the time” (6.4% [χ2 = 15.503, df = 4, p = .003] and 3.6% [χ2 = 13.918, df = 4, p = .008], respectively). Women were more likely to report feeling worn out and tired “all of the time” (4.2% [χ2 = 16.650, df = 4, p = .002] and 8.2% [χ2 = 18.786, df = 4, p = .001], respectively) but also that their health would “definitely not” be getting worse (34.0%, χ2 = 11.473, df = 4, p = .022). These data are summarized in Table 3.
Self-Reported Well-Being and General Health Markers by Pearson’s Chi-Squared Test (χ2).

Note. Omitted responses are given in parentheses. eCohort survey questions are based on/taken from validated tools. Measures presented here are from the SF-36 (Ware . . .) and ask the respondent to recall the 4-week period prior to survey participation. n = number, % = percentage of total group.
Pearson’s χ2 test, 2-sided significance.
Discussion
To expand upon the current study’s descriptive findings, and lobby for the transition of such insights toward interventions, three discussion points are shared in what follows: (a) the need to target male nurses, (b) supporting the health of female nurses, and (c) advancing nurse recruitment, retention, and patient care.
The findings drawn from the current study reveal male nurses’ health practices and outcomes as relatively poor in comparison to their female counterparts. For example, as a cohort male nurses are significantly more likely to be overweight, a finding consistent with Australian men’s health overall (Templeton et al., 2011). Male obesity is commonly linked to modifiable factors, including high sedentary time and poor diet, and directly implicated in male mortality and an array of morbidities (Ahn, Sharkey, Smith, Ory, & Phillips, 2010; Elwood et al., 2013). For example, adverse downstream outcomes were evident for the men in the current study wherein they had significantly higher incidence of Type 2 diabetes (118%), high blood pressure (58%), and myocardial infarction (364%) compared to female nurses. Although these results reflect wider population health trends (Naqvi, Davis, & Mukamal, 2010), one might reasonably ask why these sex differences prevail among nurses who work directly in the provision of health care?
Previous gender research with male nurses can provide some insights to the disjuncture between men’s willingness to provide quality health care amid neglecting their own health. For example, a study by Wu, Oliffe, Bungay, and Johnson (2015) suggested that male nurses distanced themselves from the more emotive aspects of care as a form of protection, objectively providing patient and family care. With this in mind, it may be that male nurses disregard within their own lives what they know and oftentimes teach others about health promotion and illness management. Although it is evidenced that male nurses both reject and rely on masculine norms (Dyck, Oliffe, Phinney, & Garrett, 2009; Wu et al., 2015), the current study findings may reflect how many male nurses’ alignment to masculine ideals distance men from self-health and their own mortality (Courtenay, 2000; Sabo, 2004). By comparison to their female colleagues, the male nurses in the current study were more likely to smoke, sit, be less able bodied, and get less than the recommended amount of sleep. When these factors are combined with long-term shift work, males nurses may be at risk for impaired driving performance and motor vehicle accidents in transit to and from work, as previously suggested by Ftouni et al. (2013).
Even in light of self-reported symptoms and diagnosed disease, male nurses described feeling full of life, and being calm and peaceful—and these findings also emerged in stark contrast to female nurses. Although men are known to overestimate their health (Robertson, 2007), the discord between male nurses’ illness profiles and self-reports in the current study may have been influenced by masculine norms around resilience and stoicism. Men are also characterized as less introspective, expressive, or inclined to admit to distress than women (O. Evans & Steptoe, 2002) and revered for embodying cultural norms synonymous with the easygoing and light-hearted Australian male (Templeton et al., 2011). Indeed, male depressive symptoms and anxiety are more often ineffectually self-medicated through drug overuse (Oliffe & Phillips, 2008) and the use of alcohol in this regard can be explained away as what men typically do despite heightening the risk for male suicide (Oliffe, Ogrodniczuk, Bottorff, Johnson, & Hoyak, 2012).
The move toward targeted workplace men’s health promotion has been slow (Oliffe & Han, 2014) though principles including the avoidance of shame or blame, using other men’s testimonials and providing explicit permission for men to engage in health behaviors are important program considerations (Oliffe, Bottorff, & Sarbit, 2012). By providing men-centered programs, self-health can be delinked from femininities and women’s health to more fully engage men. The workplace is known to be an acceptable place for men to engage in health promotion, especially under the guise of being fit to work wherein physicality and performance can bolster men’s efforts for optimizing one’s health. The use of male group based programs can also enable men to engage in friendly competition with one another in ways that may also reduce overestimations about one’s health (Creighton & Oliffe, 2010).
The female nurses by comparison reported overall better health amid sharing that they were tired and worn out, and challenged to accomplish all they wanted to do. This current study finding is consistent with previous work reporting women as having better health than men (Oliffe et al., 2010), yet as revealed in the current study, within the workplace and at home women consistently report higher stress levels than men (O. Evans & Steptoe, 2002; Fuhrer, Stansfeld, Chemali, & Shipley, 1999; Peterson, 2004; Walters et al., 1996). A number of gender-informed explanations can be offered for unraveling this. As health care providers, the female nurses may have strongly aligned to feminine ideals that women care for the health of others (DiGiacomo, Davidson, Zecchin, Lamb, & Daly, 2011), and are naturally attuned to their own health needs (Anonymous, 2014). Also reflected may be feminine norms around taking on the bulk of the work in domestic and child care spheres (DiGiacomo et al., 2011) along with ideals about women’s abilities to be introspective and the expression of emotions and feelings (Hass, 1979; Simon & Nath, 2004). The current study results might also reflect epidemiological data highlighting mood disorders and depressive symptoms as more prevalent among women (J. Evans, Heron, Francomb, Oke, & Golding, 2001).
The findings in the current study suggest the need to also support female nurses to advance their health and well-being in targeted ways. Programs focused on female nurses may be helpful in promoting mental health and work-shopping strategies for addressing the multiple and ever-increasing demands that come with combining career and domestic lives. In addition, women might especially benefit from employer provided or subsidized child care services, onsite female groups, or individualized mental health promotion programs and coaching services to guide their self-management strategies.
In lobbying for workplace gender-sensitive health promotion programs that target nurses, it is also important for future work to more fully integrate physiological sex–based analyses to apprehend cause–effect in thoughtfully considering prevention and remedies. Central to identifying and effectively targeting modifiable health risk factors is the exploration of physiological diversity and differences within and across men and women. For example, building on the evidence about how estrogen and testosterone influence women and men’s disease outcomes is critical to optimizing the potential of biological and behavioral based health promotion efforts (Samad et al., 2014).
Collectively, the current study findings offer health administrators and employers valuable insights and impetus for developing gender-sensitive workplace health promotion programs. Nursing is a profession plagued by high fatigue- and burnout-induced staff turnover (Hsu et al., 2010). Previous work has argued for increased leisure-time activity as a precursor to better nurse health (Henwood, Tuckett, & Turner, 2012), which in turn can increase workers’ health and workplace vitality and improve patient care (Tuckett & Henwood, 2014). Outcomes from the current study suggest that a gender-specific approach holds great potential for optimizing nurse health. Specifically, although some health practices and lifestyle issues might be shared, the specific content and mechanisms for engaging male and female nurses likely differs. For example, targeting men about heart and lung health might involve engaging them with activities and achievable goals along with some friendly competition and social connection as a means to self-managing their own health more fully. Female nurses might benefit from a mental health promotion focus to help them strategize the demands of career and family as well as overcome the emotional challenges inherent to providing nursing care.
Study Limitations
There are a number of limitations to be considered in the interpretation of this work. Primarily, the female cohort was generated by SPSS random sampling and might have been biased toward a better example of “healthier” nurses. However, randomized number generation is widely used and is arguably the most appropriate method in formulating a sample from such a large cohort (Rovai, Baker, & Ponton, 2012). Moreover, demonstrating validity in the randomization was that both males and females had BMI that classified them as overweight, which is an established risk factor for metabolic disease. Also worth considering is that the eCohort survey is self-reported, and therefore participants can over- or underrepresent their actual health and well-being, and that, in contrast to the total available populations of Australian and New Zealand nurses, only a small percentage are represented in this work. However, data here and those found in other eCohort publications by our group (Henwood et al., 2012; Tuckett & Henwood, 2014) speaks equally to other local and international work, whether by gender or not, that nurse health is not optimal.
Conclusion
The current study identified significant sex differences in lifestyle, functional vitality, and health status between male and female nurses. In turn, the case was made that gender provides insights about these differences. Also addressed were the possibilities and potential for men- and women-centered workplace health promotion programs. By investing in such gendered health promotion programs, administrators could meaningfully advance nurses’ health and their collective capacity to provide optimal patient care.
Footnotes
Author Note
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This is project is supported by grants from the Australian Research Council (LP0562102), (SR0566924), Australian National Health and Medical Research Council (2005002108) and New Zealand Health Research Council (456163). Industry Partners providing additional funding include Queensland Health, the South Australian Department of Health, Injury Prevention and Control Australia (Pty Ltd), Nursing Council of New Zealand and the Macquarie Bank Foundation. Industry partners providing in-kind support to the project include the Queensland Nursing Council, Nurses and Midwives Board of New South Wales, Nurses Board of Tasmania, Nurses Board of Western Australia, Nurses Board of the Australian Capital Territory and the Nursing Council of New Zealand, Corporate sponsors include Virgin Blue, Virgin Atlantic, and MessageNet.
