Abstract
Introduction
Parkinson’s disease (PD) leads to the deterioration of gait and balance abilities, 1 a negative trend of falls and injuries, 2 fear of falling, 3 a decline in physical activity,4,5 and decreased quality of life. 6 Pharmacological treatment is the first-choice therapy for PD; however, despite optimal medical management, individuals with PD still experience balance impairments. 7 Therefore, to prevent balance-related problems and to facilitate the maintenance of a physically active lifestyle, effective nonpharmaco-logical strategies such as novel exercise regimes need to be established for PD.
The pathophysiology of balance impairments in PD incorporates multiple subsystems (sensory, motor, and cognition).1,8 Sensory problems compromise equilibrium, particularly owing to impaired proprioception and problems integrating different sensory modalities into a frame of reference for the body. 8 Motor features (eg, bradykinesia, impaired coordination, and inflexible motor commands) further constrain the efficiency of postural adjustments to anticipate upcoming perturbations or to allow recovery from instability. 1 Also essential for balance control is the ability to perform a motor task while simultaneously engaging in a cognitively demanding task, that is, dual-tasking (DT). In individuals with PD, DT leads to degraded balance and gait performance, resulting in vulnerability to falls during many daily activities.9-11 Although recent studies have indicated improved gait performance after DT training in individuals with PD,12-14 hitherto no randomized controlled trial has confirmed this finding.
To be successful, all types of training, including balance exercises, need to be performed at or near the limits of one’s capacity. 15 For individuals with PD, exercise is an essential part of treatment,16,17 and recent experimental studies have shown that training, particularly when highly challenging, induces neuroplasticity in animals18,19 and in humans with PD.20,21 However, balance training compromising highly challenging exercises has been sparsely tested in clinical trials involving persons with PD. 17 Furthermore, training that involves challenging motor and cognitive demanding exercises may induce synergistic effects for brain plasticity, 18 which could lead to enhanced transfer of training effects to real-life situations. 22
Based on a translational approach that integrates knowledge from basic science, motor learning, and clinical practice, we have designed a program that emphasizes highly challenging aspects of balance control, the HiBalance program. 23 To address PD-specific balance impairments, this program was developed by linking PD symptoms to core areas of balance control and was subsequently translated into principles of training.23,24 The present study aimed to investigate the short-term effects of a 10-week balance program compared with usual care in the elderly with mild to moderate PD. We hypothesized that balance training would lead to specific improvements on balance and gait performance (single-task and DT, respectively), and that these effects also would transfer to everyday living (ie, concerns about falling, physical activity levels and activities of daily living).
Methods
Design
This study, approved by the Regional Ethical Board in Stockholm, was carried out as a randomized controlled study for elderly individuals with PD (trial registration: NCT01417598; for study protocol, see Conradsson et al 23 ). Data were collected from the spring of 2012 to the spring of 2013.
Study Population
Community-dwelling individuals with a clinical diagnosis of idiopathic PD (Queens Square Brain Bank criteria) 25 were recruited via advertisements in local newspapers, from Karolinska University Hospital and outpatient neurological clinics in Stockholm County. Based on a clinical assessment, we included individuals with impaired balance, such as instability during postural transfers and gait impairments. This approach aimed to apply clinical reasoning by recruiting individuals who would be assigned to balance training in clinical practice. In addition, inclusion criteria included a Hoehn and Yahr score of 2 or 3, 26 age ≥60 years, the ability to independently ambulate indoors without a walking aid, and ≥3weeks of stable anti-Parkinson’s medication. Exclusion criteria were a Mini-Mental State Examination score 27 of <24 and other medical conditions that would substantially influence balance performance or participation in the intervention. The assessment for eligibility covered 3 steps: First, participants reported their interest to one of the study coordinators. This was followed by a telephone interview to screen whether the volunteer met the inclusion criteria. Finally, eligible participants were called for baseline testing that evaluated their cognitive function and balance performance. All participants signed an informed consent form before entering the study.
Participants who met the criteria for inclusion were divided into 2 geographic cohorts, and after baseline testing the participants in each cohort were randomized in blocks of 4 to either the training group or the control group. The random sequence for group allocation was performed by one of the study coordinators using Web-based software. To ensure that testers and participants were unaware of the group allocation, opaque envelopes (sealed and numbered) were used. Masking of the test leaders was not possible after baseline assessments, given that some also served as trainers for the balance training. During the follow-up assessments, participants were never assessed by a test leader who had been involved in their training.
The sample-size calculation, detailed in the study protocol,
23
was based on a pilot study
24
and similar intervention studies in PD.12,28 The power calculation was performed separately for the 3 main outcome measures: (
Testing Procedure
Participants were assessed by experienced physiotherapists at baseline (pretest) and at the 10-week follow-up (posttest). All participants followed their normal scheme for PD medication and were tested during the on-phase at the same time of the day at the pre- and posttest. Data collection comprised 2 steps: first, physical tests of gait and balance performance and self-reported questionnaires in a movement laboratory; and subsequently, objectively measured physical activity levels in free-living conditions. To avoid bias, the order of the balance and gait tests was randomized and preceded by a standardized learning session. Demographic data (age, gender, body weight, and length), fall history, and the motor section of the Unified Parkinson’s Disease Rating Scale (UPDRS) were recorded at pretest. In addition, at both test occasions, participants’ daily levodopa equivalency dose was recorded. 29
Balance and Gait Outcomes
The Mini-BESTest is a 14-item clinical test that covers 4 components of balance control (anticipatory postural adjustments, postural responses, sensory orientation, and stability in gait). 30 Each item is scored from 0 (unable or requiring help) to 2 (normal), and the maximum score is 28 points. 30
Gait characteristics were assessed with a 9-meter electronic walkway system, GAITRite (CIR Systems, Inc, Havertown, PA, USA) during normal walking and while performing an additional cognitive task (DT; reciting every second letter of the Swedish alphabet). The participants were instructed to walk at a normal pace during both conditions, placing equal focus on the walking and the cognitive task. Each gait condition was performed 6 times, and an average value was used for analysis. In addition to gait velocity, step length and cadence were also analyzed for both gait conditions. To gain more insight into DT performance, we evaluated the performance of the cognitive task during walking (DT) and as a single task while seated. For the performance of the cognitive task, percentage of errors (ie, the number of errors/total number of letters recited) was used for analysis.
Balance performance was also assessed with the Modified Figure-of-Eight test (MFE). 31 The participants were instructed to walk 2 cycles on a figure-of-eight course (marked on the floor with a 40 mm wide tape, each loop having an internal diameter of 1.63 m) as fast as possible while trying to step on the tape. The test was performed twice where the average time and number of oversteps (ie, steps not touching the tape) were used for analysis. 31
Activity Outcomes
Physical activity level (steps per day) was assessed during free-living conditions, using an accelerometer worn around the waist (Actigraph GT3X+, Pensacola, FL, USA). Participants were instructed to wear the accelerometer throughout the day and to record on a log sheet the exact times the device was worn. Data were downloaded and processed with ActiLife 6 software. Participants with 4 or more valid days were included in the analysis since this has shown to be reliable in adult and elderly populations.32,33 In order for a day to be considered valid for analysis, we required data of at least 9 hours (>90 consecutive minutes of zeros was considered nonwear time). 32
Activities of daily living were assessed with the second part of the UPDRS, a 13-item questionnaire focusing on the effects of PD on various daily activities (eg, speech, handwriting, dressing, and mobility). The UPDRS-ADL is reported on a 4-point scale and is summarized into a total score (range 0-52), where a higher score indicates more limitations. 34
Concerns About Falling Outcome
Concerns about falling was assessed with FES-I, a 16-item questionnaire measuring concern about falling during different activities. Each item, graded on a 4-point scale, is calculated to a sum score (range 16-64), where higher scores indicate greater concerns about falling. 35
The HiBalance Program
The HiBalance training program has proved feasible in clinical practice, 24 and its content and progression have been detailed in a previous publication. 23 The balance training was performed in groups of 4 to 7 participants, 3 times per week, 60 minutes per session, for 10 weeks at a university hospital. Because of the highly challenging exercises, each session was supervised by 2 physiotherapists. Importantly, no fixed scheme of predetermined exercises was used in the intervention. Instead, a framework based on motor-learning principles (specificity, progressive overload, and variation) was used as a foundation for the application and adaptation of exercises to the participants’ individual abilities. Consequently, this approach not only resembles clinical practice but also requires continuous evaluation, modification, and planning of the training. Therefore, all the trainers involved in this study were physiotherapists (n = 10) educated in the framework of this training concept during two 4-hour sessions of both theory and practice. In addition, to ensure alignment to the HiBalance program, the trainers were supported in the practical aspects of the training when needed.
To target cognitive impairments, DT exercises were gradually integrated into the program by adding concurrent cognitive (eg, counting, remembering items) and/or motor tasks (eg, carrying and/or manipulating objects) to the balance exercises. These DT exercises were not the same tasks as those used during pre- and posttest. Moreover, 4 balance components specific to PD impairments were emphasized: (
Highly challenging training conditions were defined as exercises where the participants were forced, intermittently, to use reactive postural adjustments to control their balance during single-tasking. Similarly, the level of difficulty for DT exercises was aimed at a level where there was consistent interference of the participants’ motor performance. Moreover, to promote progressive overload and exercise variation, the 10-week period was divided into 3 blocks (A, B, C). In block A (weeks 1-2), participants were introduced to the single-task exercises of each balance component separately (no DT-exercises were practiced), emphasizing quality of movement and the objectives of the exercises. In block B (weeks 3-5), basic DT exercises were introduced (approximately 40% of each session), and the level of difficulty for each balance component was increased. The level of difficulty of all the exercises was further enhanced in block C (weeks 6-10) by increasing the variation through exercises that combined several balance components, as well as the level of difficulty and time spent on DT exercises (approximately 60% of each session).
The participants in the control group were encouraged to maintain their normal physical activities and were not restricted from participation in ongoing rehabilitation programs. All participants were advised to keep up their normal level of exercise throughout the intervention period.
Data Analysis
Statistical analysis was conducted using STATISTICA software (Statsoft, version 12, Tulsa, OK, USA). The Student
Results
There were no significant differences between groups regarding demographic data, PD severity, daily levodopa equivalent dose, fall history (Table 1) or for any outcome measure at pretest (
Participant Characteristics. a
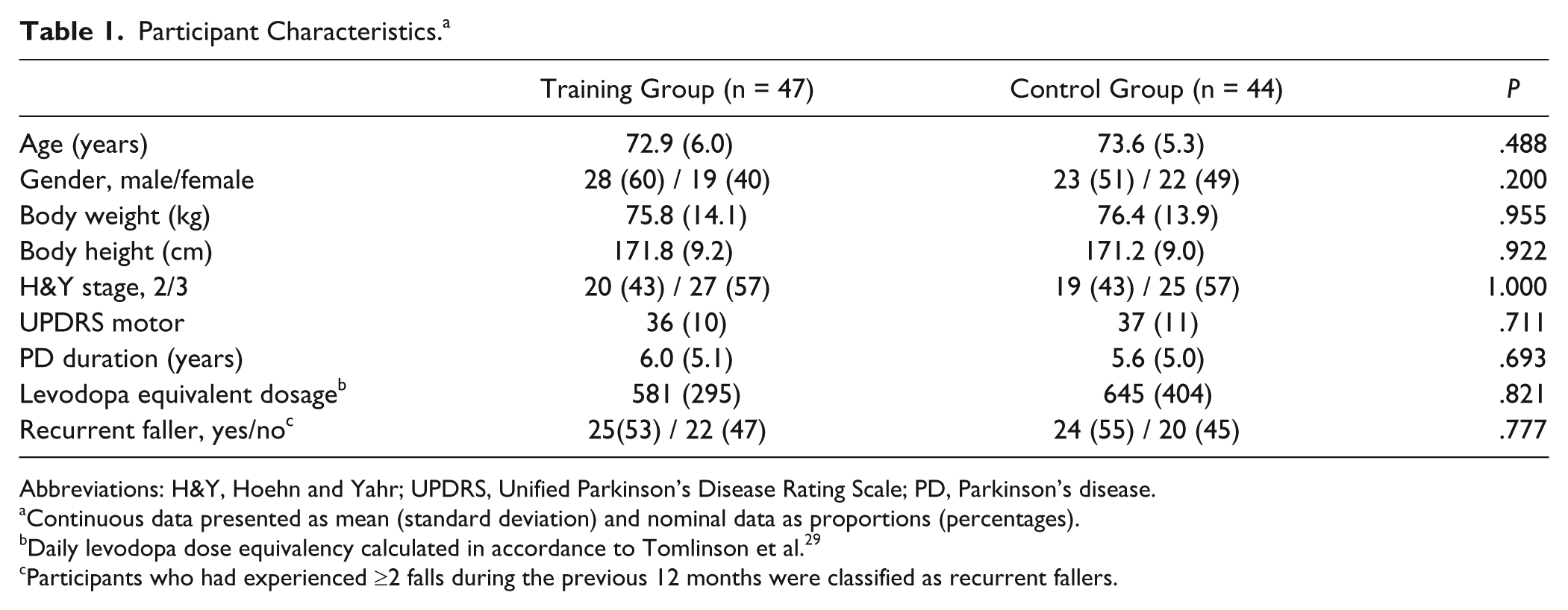
Abbreviations: H&Y, Hoehn and Yahr; UPDRS, Unified Parkinson’s Disease Rating Scale; PD, Parkinson’s disease.
Continuous data presented as mean (standard deviation) and nominal data as proportions (percentages).
Daily levodopa dose equivalency calculated in accordance to Tomlinson et al. 29
Participants who had experienced ≥2 falls during the previous 12 months were classified as recurrent fallers.
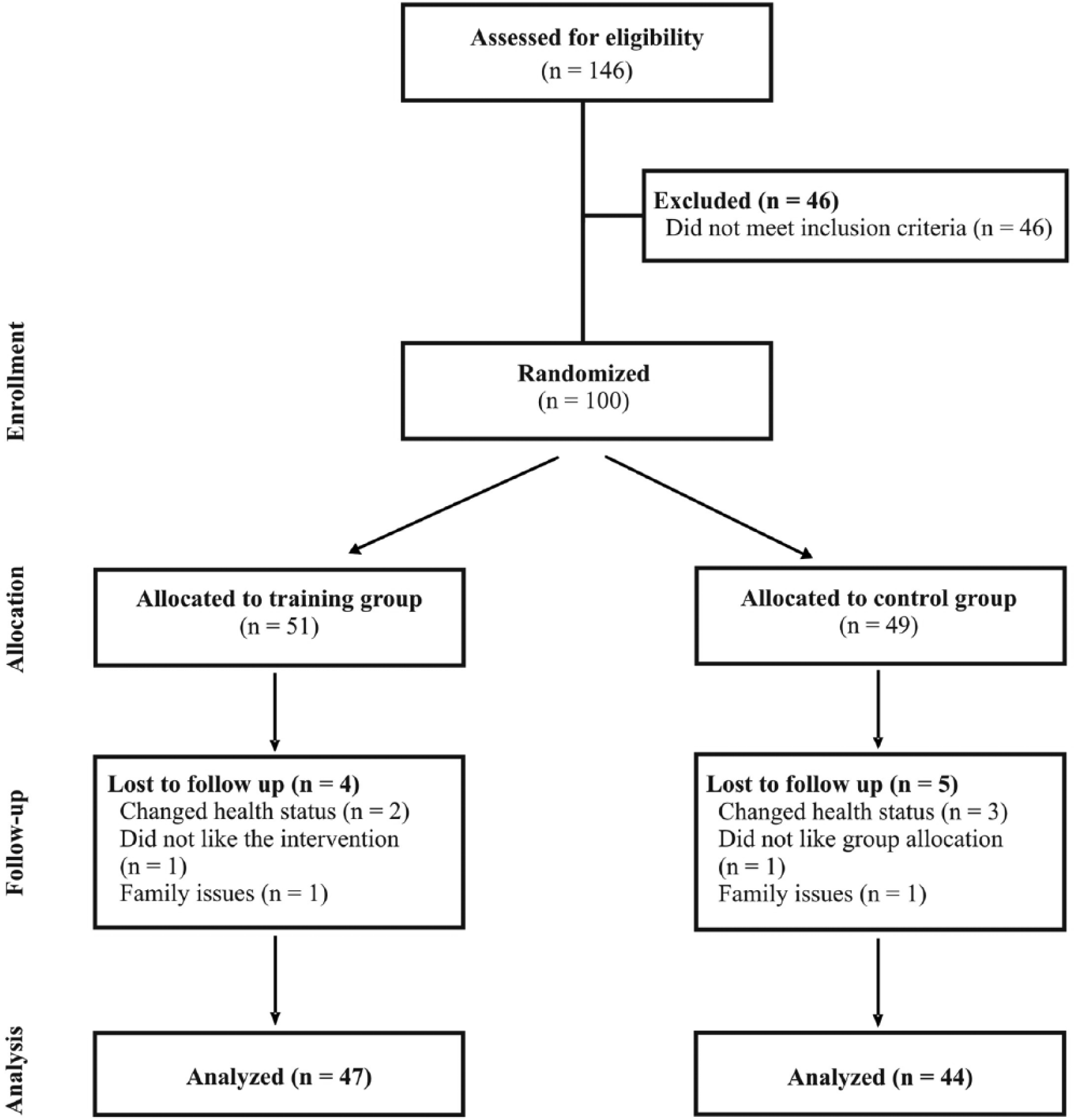
CONSORT flow diagram illustrating recruitment, randomization, and tracking of the participants over the course of the study.
Effect of Training on Balance and Gait
We found highly significant interaction effects for the Mini-BESTest,
Treatment Effects for the Training Group and Control Group at Baseline and 10-Week Follow-up.
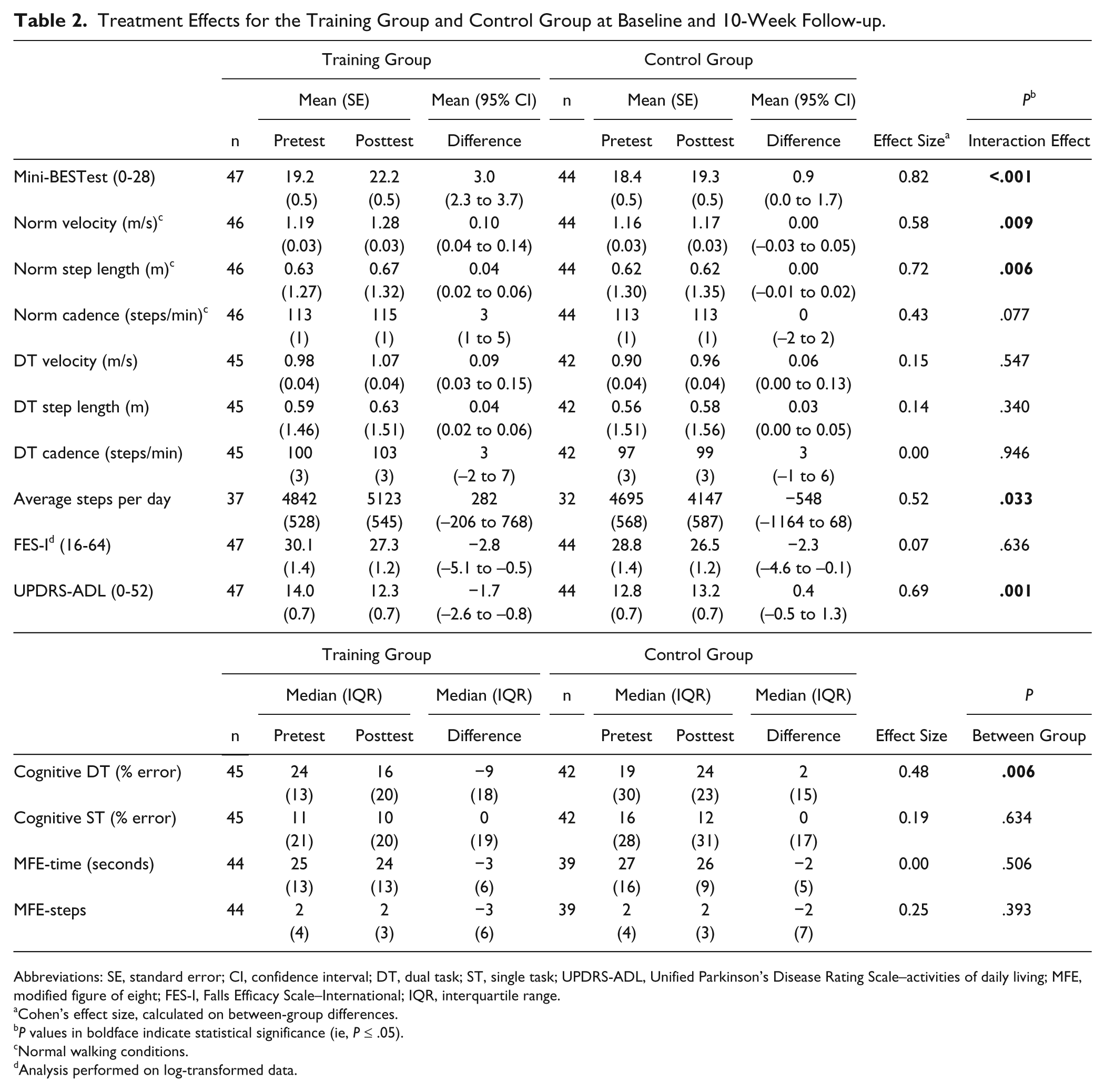
Abbreviations: SE, standard error; CI, confidence interval; DT, dual task; ST, single task; UPDRS-ADL, Unified Parkinson’s Disease Rating Scale–activities of daily living; MFE, modified figure of eight; FES-I, Falls Efficacy Scale–International; IQR, interquartile range.
Cohen’s effect size, calculated on between-group differences.
Normal walking conditions.
Analysis performed on log-transformed data.
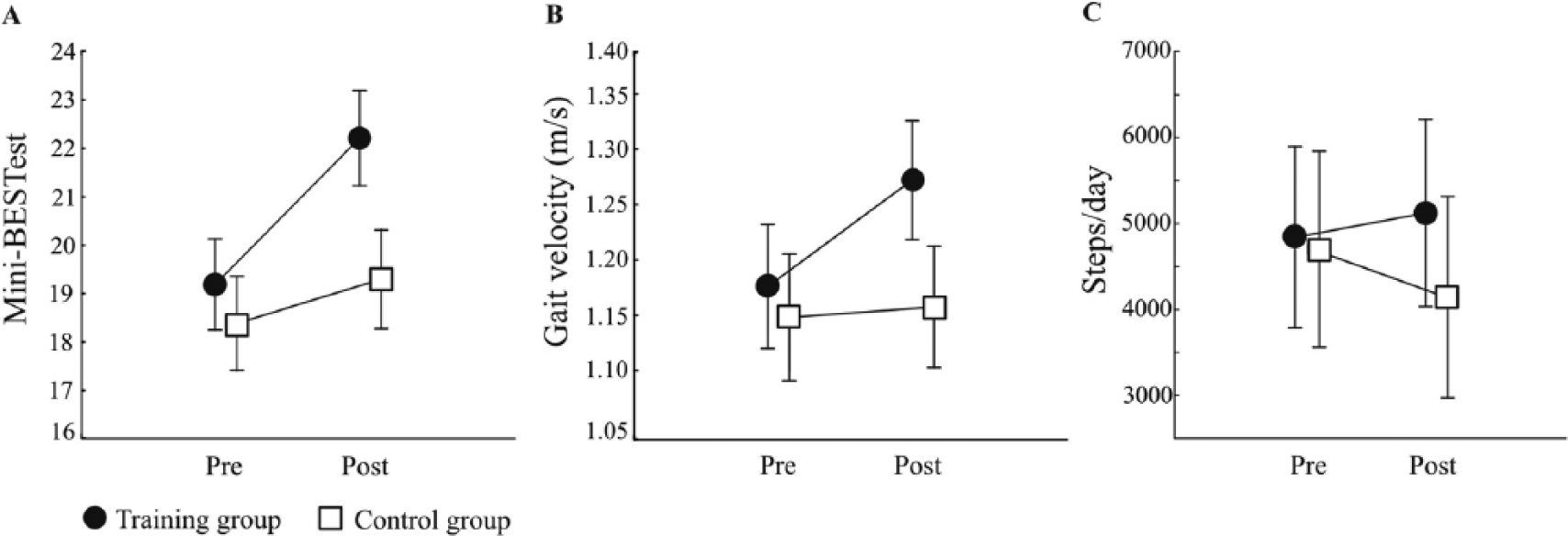
(A) Mini-BESTest score, (B) gait velocity (m/s), and (C) steps per day in the training group and control group at pre- and postintervention. Data are plotted as mean and standard error.
Effect of Training on Daily Activity
For physical activity levels, a significant interaction effect was found for the average number of steps per day,
Effect of Training on Concerns About Falling
We found no interaction effect for concerns about falling (Table 2).
Compliance and Adverse Events
The average attendance rate for the training group was 90%. In all, participants took part in 1380 training sessions, resulting in a total of 13 adverse events (all were falls during training) and an incidence rate of 0.9%. None of these events caused injury or pain that interfered with the participants’ ability to proceed with the balance training or other activities.
Discussion
In this study, we investigated the short-term effects of a 10-week program with an emphasis on motor and cognitively challenging balance exercises in elderly individuals with PD. The findings of this trial revealed that the training group that received a specific intervention targeting balance and gait performance improved significantly better in terms of balance control and gait performance when compared with the control group that received usual care.
Consistent with 2 meta-analyses reporting the beneficial short-term effects of exercise on balance performance in individuals with PD,16,17 we found a significant effect and a large effect size (0.82) for the Mini-BESTest in the training group. Our effect size on balance performance was similar to previous studies that evaluated challenging balance exercises in PD.37-39 However, the training stimuli in the balance training, that is the level of challenge on postural demands in relation to individual capacities, are inconsistently reported between studies. Therefore, from a methodology perspective, to enable comparison, there is a need for psychometrically validated tools to monitor balance training and its progression. 40
In contrast to our results of the Mini-BESTest, we found no training effects for the single-item balance test MFE. The Mini-BESTest is a multi-item test that aims to cover the complexity of balance performance, 30 hence our results indicate that in PD, it may be important to use a combination of tests in order to cover different aspects of balance impairments. 41 This 3-point improvement on the Mini-BESTest exceeds the previously found standard error of measurement (1.5 points) in elderly individuals with mild to moderate PD. 42 However, comparable trials using the Mini-BESTest are sparse and data on minimal clinically important difference (MCID) in PD is lacking. Nevertheless, our results are promising, especially since enhanced balance performance was also linked to improved gait velocity (0.10 m/s) in the training group. Gait velocity is a vital indicator of health in older adults,43,44 and our effect exceeded the pooled effect for exercise in PD (0.04-0.05 m/s), which was recently reported in 2 meta-analyses.16,17 In fact, few randomized controlled trials in PD38,45,46 have shown training effects exceeding an MCID of 0.10 m/s for gait velocity.43,44 In addition, short step length, a typical feature in individuals with PD, has rarely been improved by training interventions. 16 In our study, the increased step length (0.04 m) in the training group provides further confirmation that this intervention efficiently targets gait impairments.
To date, this is the first randomized controlled trial showing that DT training can improve certain aspects of DT performance in individuals with PD. Although we found no between group differences regarding DT gait performance, the training group improved the performance of the cognitive task while walking compared with the control group. Since the performance of the cognitive task was unchanged when performed as a single task (while seated), it provides evidence of a specific improvement regarding DT performance in the training group. These DT improvements may derive from increased automatization of single tasks, or it might be a consequence of improved efficiency in integrating both tasks.14,47 Furthermore, although no interaction effect was found for gait velocity during DT, the effect in the training group (0.09 m/s) was close to the MCID (0.10 m/s). It is noteworthy that this effect is similar to the results from previous studies regarding DT training in PD.12-14 However, none of these studies included a control group—hence, potential training effects cannot be differentiated from learning effects owing to repeated assessments. In summary, even though the field of DT training for individuals with PD is nascent, our findings indicate that DT performance might be improved in this population. However, the underlying mechanisms of DT impairments and the potential for rehabilitation need further investigation.
Despite growing evidence regarding the advantages of exercise for individuals with PD, it is unclear whether specific improvements in balance and gait can translate into “real-world” settings.16,17 In our study, the notion of short-term transfer effects is supported by physical activity levels and activities of daily living. In particular, although not significant, the training group showed an increasing trend in physical activity (6%), while the control group, in line with the progressiveness of PD, 48 showed a declining trend (12%). Even though the absolute difference between groups is rather small, we believe that these findings are important, especially since benefits in terms of general health and disease modification could be expected to result from maintaining physical activity throughout the course of PD. 49 Only 2 previous studies, the ParkFit trial 50 and the RESCUE trial, 51 have used objective measures (eg, accelerometry) to investigate the impact of rehabilitation programs on daily physical activity in individuals with PD. In line with their results, our study showed that enhanced physical activity occurred at the same time as improvement in physical functioning. Regarding activities of everyday living, the improvement of 1.7 units on the UPDRS-ADL must be cautiously interpreted since it only approached the MCID values between 2 and 3 units for the UPDRS-ADL. 52
In accordance with the current body of research in PD,16,53 we found no short-term effects of balance exercise on concerns about falling. Although this intervention was greatly appreciated by the participants, it is uncertain how the experience of threatening postural situations in highly challenging exercises may influence patients’ concerns about falling and their awareness of personal boundaries. These aspects require another approach; therefore a qualitative study of the participants’ experience of this intervention is in progress.
The main strengths of this study are the large sample size, the low dropout rate, and the comprehensive assessment of outcomes related to balance impairments (clinical tests, objective measures of gait, physical activity levels, and self-perceived disability). However, the study also had several limitations. First, a majority of the participants were recruited by advertisement, a method that can lead to a convenience sample of individuals interested in training and improving balance abilities. Second, the results can only be generalized to elderly, specifically community-dwelling individuals with mild- to moderate-stage PD without known cognitive impairments. Third, some participants were unable to maintain a constant dosage of anti-Parkinson medication throughout the trial. However, reported changes of medication were equivalent between groups and not related to pre/post difference in dyskinesia (a possible cause for medication change and balance improvements). Moreover, analyses on the subgroups that changed medication dosage revealed no difference in balance performance. Finally, the assessors were not masked to group allocation at the posttest assessment, thus bias related to the physical testing cannot be ruled out. On the other hand, we believe that the clinical approach of this study strengthens the ecological validity of this research.
In conclusion, the results of this randomized controlled trial showed that highly challenging exercises, when compared with usual care, improved balance and gait performance in elderly individuals with mild to moderate PD. This study also showed positive transfer effects to activities performed in real-world settings, indicating that appropriate training programs could promote physical activity and daily activities. Further explorations of these effects in a long-term follow-up are underway.
Footnotes
Acknowledgements
The authors would like to thank all the participants, physiotherapists, and research assistants who contributed to this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by grants from the Swedish Research Council, the Swedish Parkinson Foundation, the Karolinska Institutet, the Loo and Hans Ostermans Foundation, the Gun and Bertil Stohnes Foundation, the Swedish NEURO Foundation, the Norrbacka Eugenia Foundation, and the regional agreement on medical training and clinical research (ALF) between Stockholm County Council and Karolinska Institutet.
