Abstract
Keywords
Introduction
Muscle weakness has been widely observed following brain injury in children1-3; however, the distribution of weakness within the paretic limb and its relationship to the time of injury occurrence remains unknown. In this study, the distribution of weakness in the paretic arm is postulated to be dependent on the time of injury occurrence in immature brains because of profound changes that occur in the central nervous system during development. Childhood-onset hemiparesis (CH) is an ideal model for identifying the role of injury timing on neuromuscular output in childhood through young adulthood. Unique etiology of injury at different time points (PRE-natal, PERI-natal, and POST-natal injuries) suggested by imaging studies have been related to generalized gross motor outcomes,4-8 but the impact of injury timing on strength at multiple joints has never been quantified.
During typical neural motor system maturation, both contralaterally and ipsilaterally projecting corticospinal connections exist in fetal felines 9 and rats. 10 On a synaptic level, there is refinement of responses to neural activation 11 because of the strengthening of the most active synapses. 9 During typical development, this refinement leads to reduction in ipsilateral corticospinal projections and maintenance and strengthening of contralateral corticospinal projections, which far outnumber the ipsilateral projections in adulthood. However, the activity-dependent nature of neural development is demonstrated by a markedly changed distribution of corticospinal projections in cats and rats following unilateral brain injury, such that the undamaged cortex maintains typically transient ipsilateral corticospinal projections.9,12
In humans, connectivity between the motor cortex and muscles of both upper extremities has been demonstrated at birth, proving that both contralateral and ipsilateral projections are in place. However, the strength of the ipsilateral responses decreases rapidly in early life, 13 and predominantly contralateral motor responses to cortical stimulation are found by early childhood. Some individuals in a subgroup of the CH population—those with hemiplegic cerebral palsy—also maintain fast-conducting ipsilateral connectivity from the nonlesioned hemisphere to the paretic limb after the time when these types of responses would be typically seen. 13 Therefore, it can be hypothesized that injury to the brain early in development inhibits ipsilateral pruning of the CS system and subsequently preserves muscle activation throughout the paretic upper extremity, particularly at distal joints, because of a greater proportion of CS tract projections to distal muscle motoneurons.14-17 The corticomuscular connectivity studies of Eyre and colleagues13,18-20 suggest that there may be retained ipsilateral corticospinal connectivity in both the PRE-natal and PERI-natal injury periods of the current study. However, the impact of apoptosis 21 and myelination21,22 during the third trimester of gestation was hypothesized to decrease the flexibility of the nervous system to respond to brain injury in the PERI-natal group. In the POST-natal group, when an injury occurs after 6 to 12 months of age, the ipsilateral CS connections are less likely to be available for control of the paretic arm. With respect to remaining neural resources, this group was theorized to instead rely on alternative control systems, such as the reticulospinal (RS) tract, for movement on the paretic side of their body. Projections from the RS pathway anatomically project to diffuse segments of the spinal cord motoneuron pools, particularly innervating proximal musculature and to a lesser extent wrist and hand musculature23-25 in a diffuse fashion. 17
In this study, all CH groups are expected to be weaker than their typically developing (TD) counterparts. Furthermore, it is postulated that the POST-natal group will demonstrate greater weakness than PRE-natal or PREI-natal groups, especially at the distal joints of the paretic arm and especially in extension because of innervation patterns of the RS system. The PRE-natal group is expected to have the least relative weakness throughout the paretic limb because of preserved CS influence (as a result of abnormally retained ipsilateral undamaged contralateral projections) on the paretic limb, resulting in the innervation of motoneuron pools activating even the more distal muscles, as in the TD cohort. Finally, the PREI-natal group is expected to perform between the PRE-natal and POST-natal groups, with moderate levels of weakness and somewhat greater distal involvement. To test these hypotheses, isometric torque generation ability was quantified at the shoulder, elbow, wrist, and finger joints of both upper extremities in 3 CH groups, based on time of injury. The results confirm that timing of injury is crucial to the overall expression and distribution of weakness in the upper extremity, with different potential underlying neural mechanisms and clinical implications for timing groups.
Methods
Participants
A modified CONSORT 26 flow chart for the participants in this study can be found in Figure 1. A total of 120 possible CH candidates for the study were identified through the Cerebral Palsy Research Registry, 27 local clinics, newspaper advertisements, and parent support groups. After screening, 24 of these individuals were included in the final analysis. To be included, participants had to be at least 6 years of age and had to have sustained a brain injury in the developing central nervous system that resulted in unilateral upper-extremity motor impairment. Exclusion criteria included muscle tone abnormalities and motor/sensory impairment in the nonparetic limb, severe cognitive or affective dysfunction, significant concurrent medical conditions, and botulinum toxin injections to the upper extremity within 6 months of testing. Participants were divided into 3 groups (PRE-natal, PERI-natal, or POST-natal) based on the timing of their injury. PRE-natal was defined as timing between the late second and early third trimesters of gestation (prior to approximately 34 weeks postconceptual age 28 or 36 weeks gestational age), PERI-natal was defined as being from the late third trimester of gestation until 2 months following birth, and POST-natal was defined as being between 6 months and 10 years of age. Timing of injury was ascertained by medical record review and parent report using the decision matrix outlined in Figure 1. Those participants in whom the timing of injury could not be clearly ascertained (n = 2) because of lack of imaging and unclear etiology were excluded from the study. Age-matched, right-hand dominant, TD participants with no history of neurological injury were recruited for comparison with the CH groups.
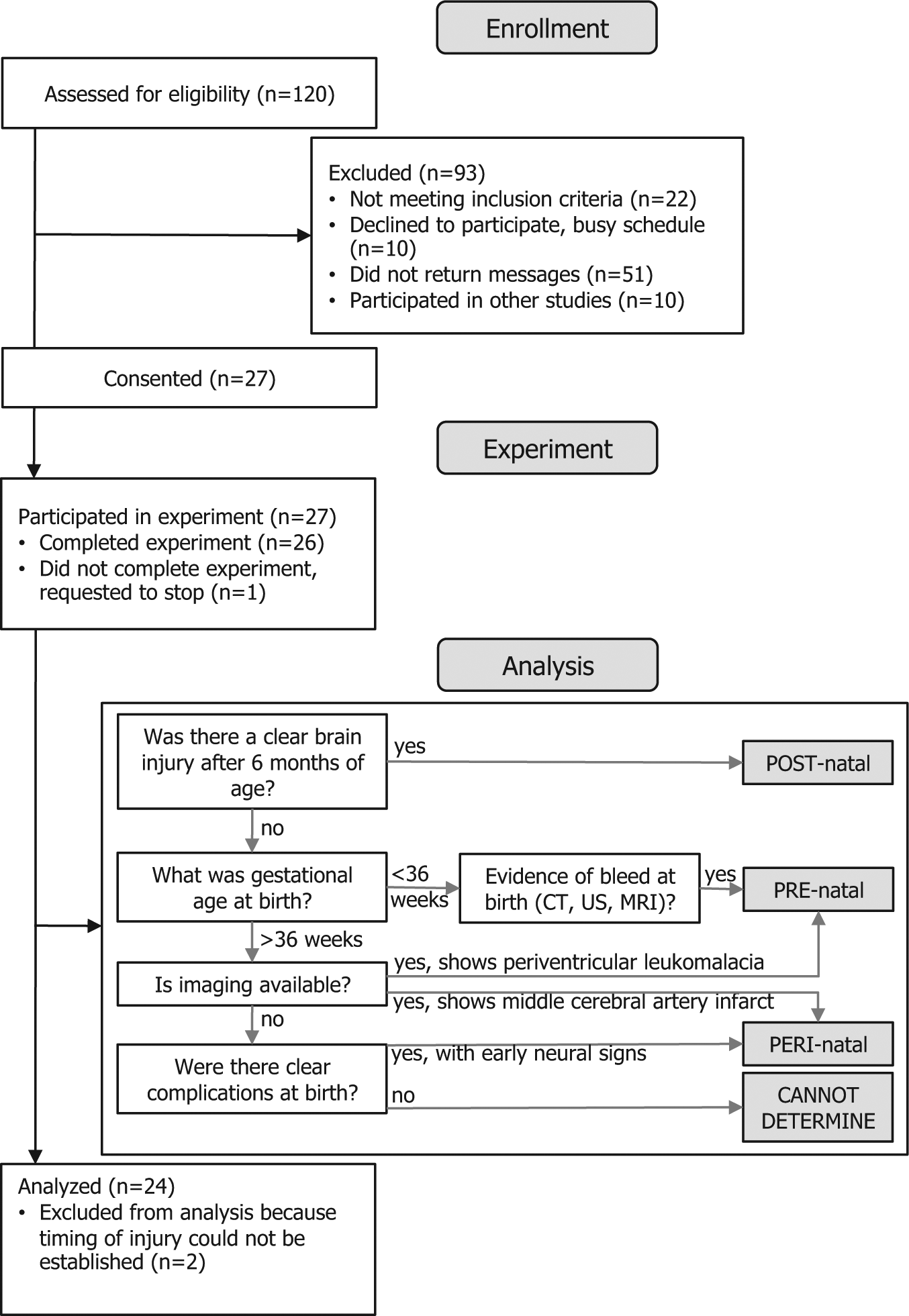
Flow chart for participant inclusion and injury timing group assignment.
In all, 24 participants with clearly defined CH injuries (8 PRE-natal, 8 PREI-natal, and 8 POST-natal) and 8 TD controls completed the study. All participants, and their guardians as applicable, provided informed consent and/or assent prior to enrolling in the study, which was approved by the institutional review board of Northwestern University. Table 1 contains demographic and clinical information for the 32 participants included in the analysis.
Participant Characteristics.
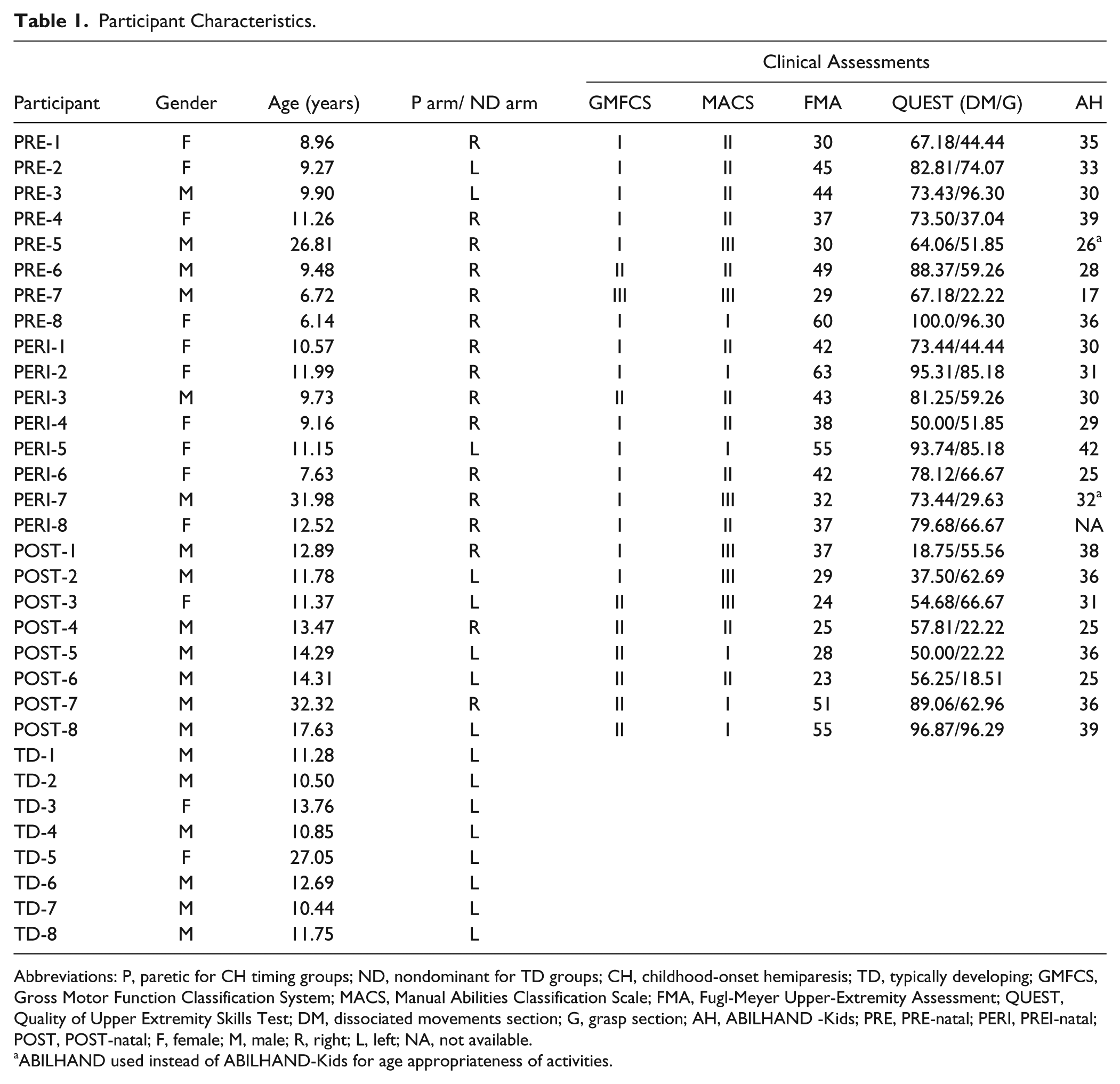
Abbreviations: P, paretic for CH timing groups; ND, nondominant for TD groups; CH, childhood-onset hemiparesis; TD, typically developing; GMFCS, Gross Motor Function Classification System; MACS, Manual Abilities Classification Scale; FMA, Fugl-Meyer Upper-Extremity Assessment; QUEST, Quality of Upper Extremity Skills Test; DM, dissociated movements section; G, grasp section; AH, ABILHAND -Kids; PRE, PRE-natal; PERI, PREI-natal; POST, POST-natal; F, female; M, male; R, right; L, left; NA, not available.
ABILHAND used instead of ABILHAND-Kids for age appropriateness of activities.
Protocol
Participants were seated comfortably in a Biodex experimental chair (Biodex, Inc, Shirley, NY), as shown in Figure 2A, with straps across the shoulders and waist to minimize trunk movement. Participants’ forearms were placed in a fiberglass cast from just distal to the elbow to just proximal to the wrist in order to be secured comfortably and rigidly to a 6-degrees-of-freedom load cell (JR3, Inc, Woodland, CA) with a shoulder abduction (SB) angle of 85°, shoulder horizontal adduction angle of 40°, and elbow flexion (EF) angle of 90° (Figure 2A). Forces and moments measured by the load cell at the radius/ulna connection were converted to torques at the elbow and shoulder using Jacobian matrices based on free-body analysis of the upper limb. 29 Participants’ hands and fingers were strapped into a custom finger and wrist force sensor 30 (Figure 2B), the casings of which were each equipped with tension-compression load cells (LC201, Omega Engineering, Stamford, CT). Wrist and finger torques were determined based on calibration curves and distance from the sensor to joint centers. 30
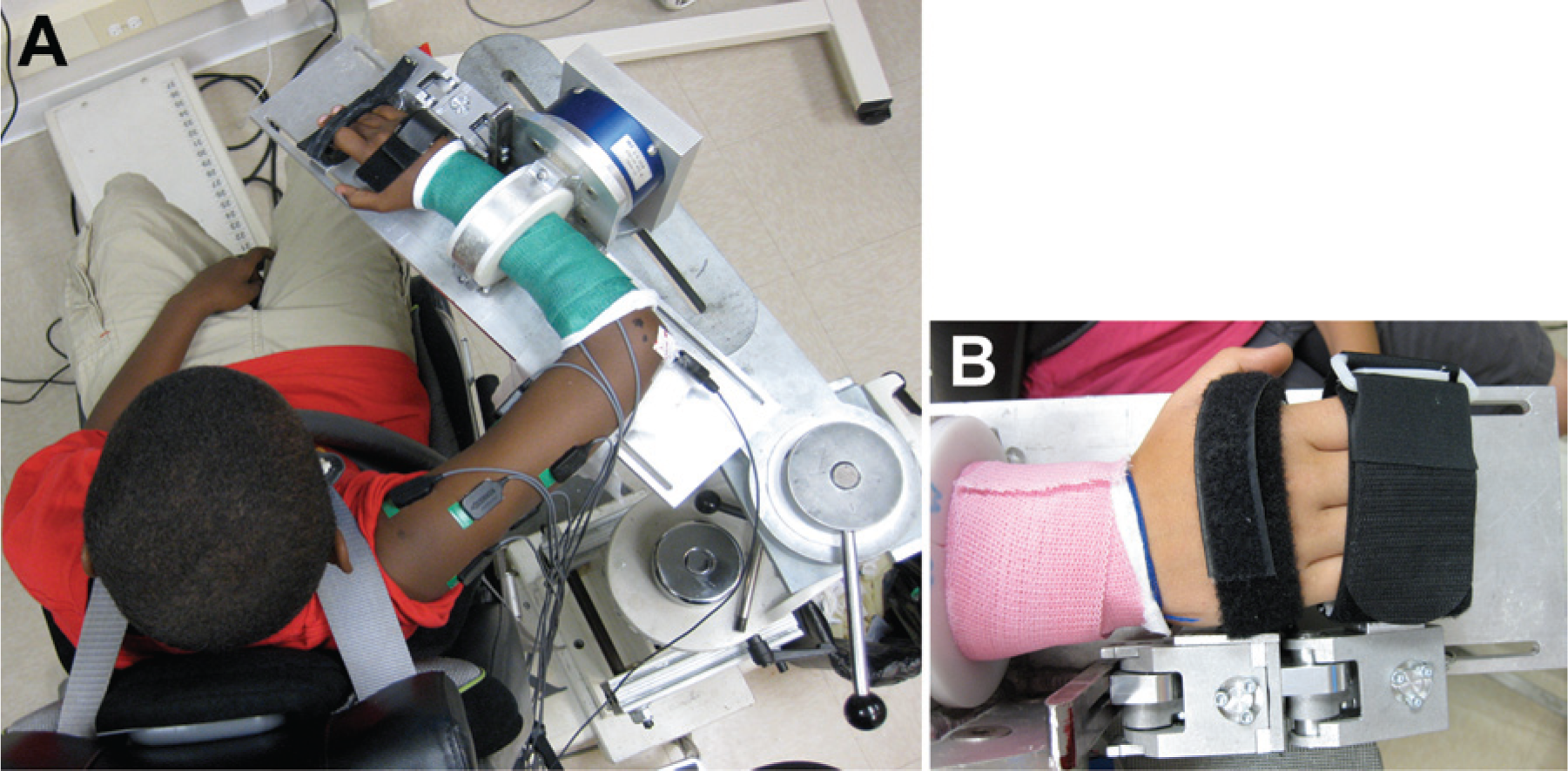
Experimental setup: The participant was seated with the arm placed in a fiberglass cast and connected rigidly to a 6-degrees-of-freedom load cell (A). The arm was positioned such that the shoulder abduction angle was 85°, the shoulder horizontal adduction angle was 40°, and the elbow flexion angle was 90°. The participant’s hands and fingers were secured to a device to measure torques generated at the wrist and fingers (B). Placement of the finger and wrist sensors were made such that the center of rotation of the wrist was in line with the wrist sensor axis and the center of rotation of the second and fourth metacarpal-phalangeal joints were in line with the axis of rotation of the finger sensor.
Each participant was asked to generate an isometric maximum voluntary torque in 1 of 10 randomly ordered primary directions during a 5-second trial. Primary directions included SB, shoulder adduction (SD), shoulder horizontal adduction termed here shoulder flexion (SF), shoulder horizontal abduction or shoulder extension (SE), EF, elbow extension (EE), wrist flexion (WF), wrist extension (WE), finger flexion (FF), and finger extension (FE). At least 3 trials within 10% of the maximum were collected in each primary direction, the last of which could not be the greatest, to remove any possible impact of a learning curve. Rest periods were provided between trials and extended on participant request to reduce the effects of fatigue. The participant started each trial in a relaxed state and received visual and verbal feedback to optimize performance.
For each trial, the joint torque data were filtered using a 250-ms moving average filter, and the maximum torque in the primary direction was identified. The maximal value across all trials of an intended primary torque direction was recorded as the maximum voluntary torque. To compare across individuals, a relative weakness ratio was computed for each primary torque direction by dividing the difference between maximum voluntary torques on the paretic side and nonparetic sides by the sum of the 2 maximum voluntary torques. A relative weakness ratio of 0 indicates equivalent strength in both arms, and a relative weakness ratio greater than 0 indicates greater strength on the nonparetic (or dominant in TD participants) side.
Several clinical assessments were used to compare upper-extremity function and strength across injury timing groups. Motor function was classified clinically using the Gross Motor Function Classification System–Expanded and Revised (GMFCS-ER)31,32 and the Manual Abilities Classification Scale (MACS). 33 Evaluation of motor function in the upper extremity was completed using the Quality of Upper Extremity Skills Test (QUEST), 34 the Fugl-Meyer (FM) Motor Assessment,35,36 and 3 maximal grip strength trials (Jamar Hydraulic Hand Dynamometer, B&L Engineering, Tustin, CA). 37 Parent-reported outcome measures of function were assessed using the ABILHAND-Kids instrument 38 or the ABILHAND instrument 39 for participants older than 18 years.
Statistics
Demographic differences between PRE-natal, PERI-natal, POST-natal, and TD groups were assessed using a 1-way ANOVA for age and Fisher’s exact tests for the binary variable of handedness. Clinical score differences were assessed using 1-way ANOVAs, with a factor of group for each of the following dependent variables: FM score, GMFCS level, MACS level, QUEST dissociated movement section, QUEST grasp section, ABILHAND score. Grip relative weakness ratio differences were also tested with a 1-way ANOVA with a 5-level factor of group, which included a group of 8 adults following a hemiparetic stroke, published elsewhere. 40
A mixed-model ANOVA was performed to ascertain the effect of independent variables of group (between-subject, 4 levels) and primary torque direction or task (within-subject, 10 levels) on the dependent variable of relative weakness ratio. Bonferroni-corrected pairwise comparisons were made on the main effects.
To further elucidate the interaction between a joint’s distance from the trunk (shoulder, elbow, wrist, and finger joints each progressively further from the trunk) and the level of relative weakness, categorical linear regression analyses were completed in the flexion synergy (SB, EF, WF, and FF) and extension synergy (SD, EE, WE, and FE) muscle groups for each participant. For each set of muscle group synergies, 4 multiple linear regressions were completed. An ordinal predictor of joint and a nominal predictor of group were used on the dependent variable of relative weakness ratio, with full entry regression. Indicator variables were used for the 4-level categorical predictor of group to compare each of the groups (PRE-natal, PERI-natal, POST-natal, and TD) with one another.
Statistical analysis was completed using SPSS software (version 19.0. SPSS, Inc, Chicago, IL). A
Results
A total of 8 PRE-natal, 8 PERI-natal, 8 POST-natal, and 8 TD participants were included in the analysis. No significant difference was detected for age between the 4 groups of participants (
The overall clinical presentation of individuals in each of the study groups was similar. No significant differences were found between groups of CH for clinical scores of GMFCS (
Group results for the 10 primary torque directions, or tasks, showed differences in relative weakness ratio between PRE-natal, PERI-natal, and POST-natal groups (Figure 3A). The mixed-model ANOVA for relative strength ratio revealed significant effects of timing group (
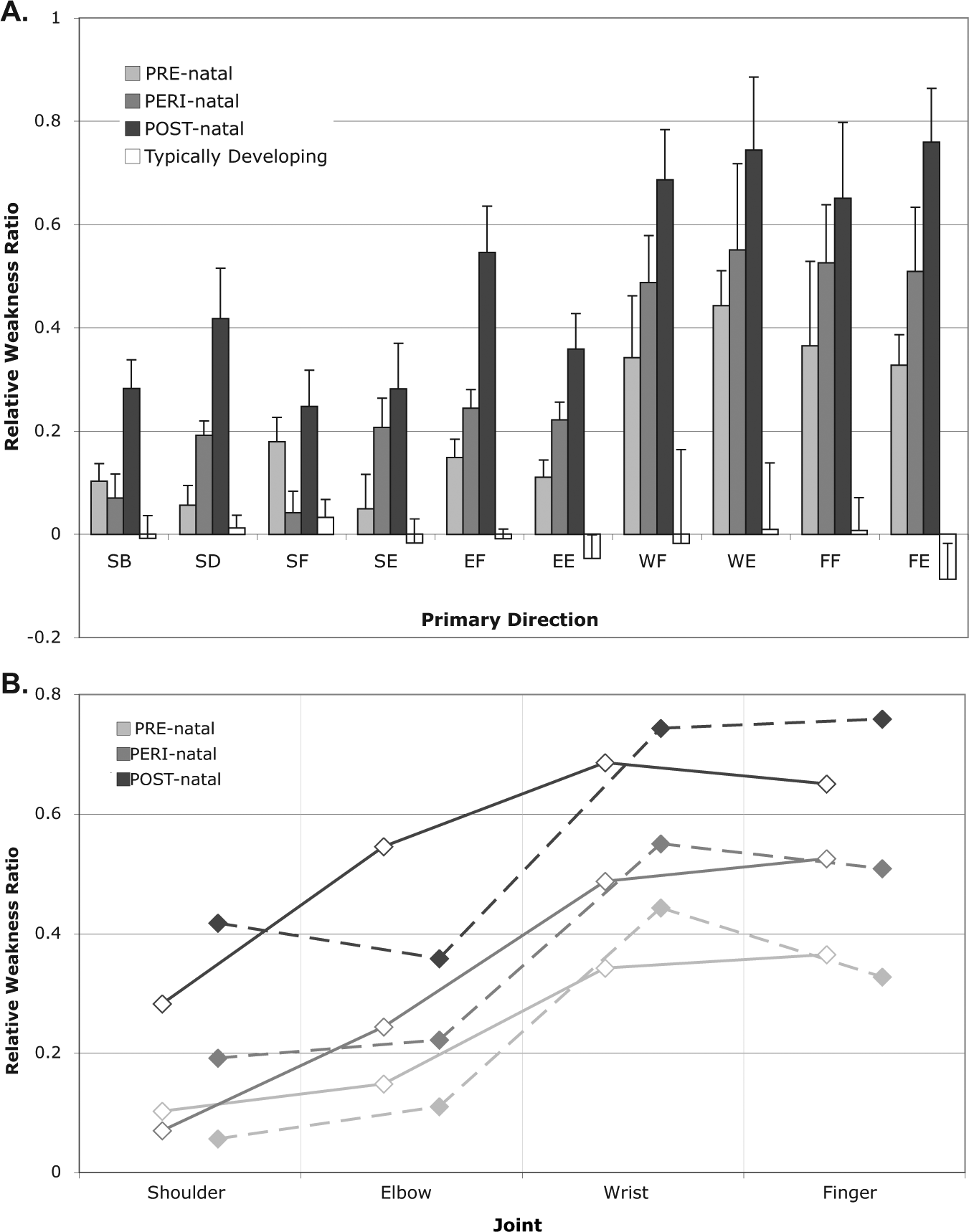
A. Relative weakness ratios in each of 10 primary task directions, including shoulder abduction (SB), shoulder adduction (SD), shoulder flexion (SF), shoulder extension (SE), elbow flexion (EF), elbow extension (EE), wrist flexion (WF), wrist extension (WE), finger flexion (FF), and finger extension (FE). The relative weakness ratio was calculated as the difference between maximal torques between arms divided by the sum. A value close to 0 indicates equivalent strength in the paretic and nonparetic, or dominant and nondominant limbs, whereas a value closer to 1 indicates a larger nonparetic torque than paretic. Standard error bars are shown. There is a significant effect of group, task, and the group-by-task interaction (
The multiple linear regression analyses further explained the nature of the interaction effect between group and primary torque direction, demonstrating significant differences in the gradient of weakness from proximal to distal joints in both regression models (flexion regression
Regression Results.
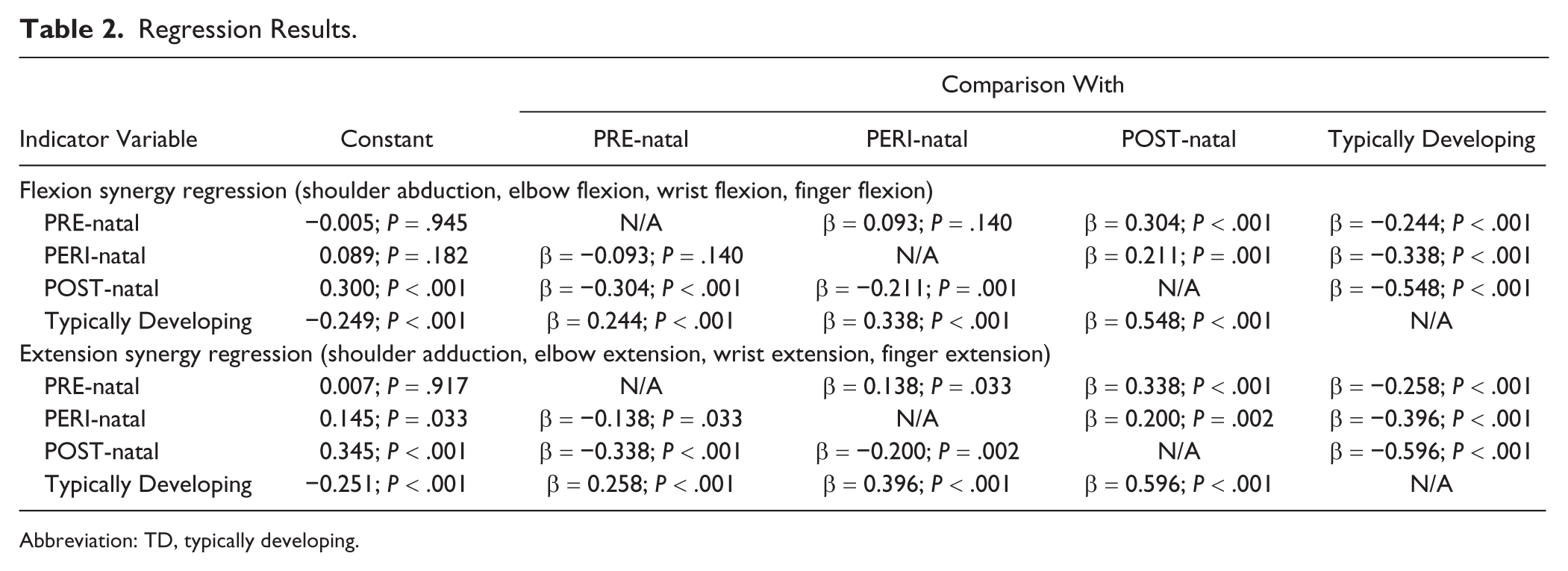
Abbreviation: TD, typically developing.
When extending the comparison to adults following a stroke, there was a main effect of group for grip strength relative weakness ratio (
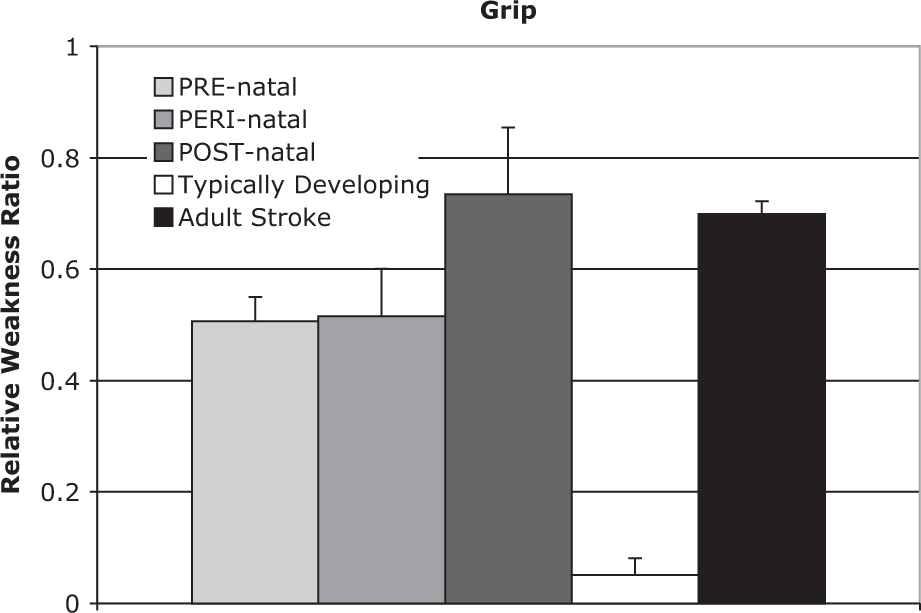
Relative weakness ratio for grip in 3 CH injury timing groups, typically developing participants, and participants with an adult-onset stroke resulting in hemiparesis. The relative weakness ratio was calculated as the difference between maximal torques between arms divided by the sum. A value close to 0 indicates equivalent strength in the paretic and nonparetic, or dominant and nondominant limbs, whereas a value closer to 1 indicates a larger nonparetic torque than paretic. Standard error bars are shown. There was a significant effect of group (
Discussion
Brain injuries early in life are likely to have a fundamental impact on subsequent neural and musculoskeletal development, but few motor studies have addressed or controlled for the timing of injury onset in CH despite the demonstrated impact on gross anatomy of motor pathways.4-7 Depending on the state of development of the nervous system when brain injuries occur, different avenues for neural reorganization are available. Maximal voluntary torque generation was measured for 10 tasks in the upper extremity, which included both proximal and distal joints. The results of this study demonstrate that the timing of brain injury in CH does have a significant impact on the distribution of weakness in the upper extremity. In all, 3 timing-of-injury groups were defined in this study based on important milestones of the motor system during typical development. Although the groups in this study were small, relative weakness of the paretic arm was found to be greater in distal joints compared with proximal joints in all groups and most especially in the POST-natal group. The explanation for the relationship between relative paretic arm weakness and timing of injury likely lies in the sequence of typical neuromotor development and the state of the nervous system at the time of injury.
Neuromotor Development and Impact on the Distribution of Upper-Extremity Weakness
In human development, the second trimester of gestation is characterized by neuronal multiplication followed by myelination of axons, starting at approximately 28 weeks, 41 with the posterior limb of the internal capsule becoming largely myelinated at 33 weeks. 42 Direct histological evidence from felines 9 and rats 10 demonstrates bilateral corticospinal projections from each of the cortical hemispheres during a comparable period of gestation. Retrograde tracing has shown ipsilateral corticospinal projections 43 at birth in the monkey, with terminations, including intrinsic distal muscles used for fine motor control in older animals. 44 Similar histological studies are not possible in TD humans, but immediately following birth, short-latency motor-evoked potentials, indicative of the corticospinal system,13,20 have been recorded from each cortical hemisphere to muscles in both arms. Over the first months of life, there is rapid differential development between increasing contralateral and reduced ipsilateral corticospinal projections to the hand.13,18,20 This is an example of activity-dependent shaping of the nervous system from an early age, 45 a process that leads to pruning of underutilized synaptic connections and eventually axons. Crossed corticospinal pathways become more dominant in their connections onto spinal motor circuits 9 concurrent with continued rapid myelination of axons. 41 Higher-level skill acquisition throughout childhood and adolescence is indirect evidence of further motor system refinement, including continued myelination, albeit at a slower rate, 46 and increasing coherence of low-frequency oscillations between the brain and distal limb muscles. 47 Coherence reaches adulthood levels of prevalence and magnitude in the 15- to 35-Hz β range by approximately 12 to 15 years of age, 47 at which time, motor development can be considered to have reached adult levels. In each group of the current study, there was 1 adult who could be considered to be at an age of mature motor development.
The interruption of typical early neural development with a unilateral brain injury has a profound impact on subsequent neural motor development. There is evidence13,20 to suggest that contralesional (ispilateral to the paretic limb) corticospinal connections from the nondamaged hemisphere are maintained well after the typical period of withdrawal when the injury occurs before approximately 6 months of age. Lower levels of relative weakness, especially in the distal joints of the PRE-natal and PERI-natal groups found in this study, are also consistent with utilization of the preserved contralesional corticospinal tracts, given corticospinal distributions and specialized innervation of the hand muscles, particularly wrist/finger extensors. Although there was no significant post hoc difference found between the PRE-natal and PREI-natal groups in the ANOVA with a conservative Bonferroni correction, regression analysis demonstrated a significant difference in the proximal to distal gradient when comparing the extensor muscles between the 2 groups, where the PERI-natal group became weaker in distal joints. This could be reflective of myelination during the third trimester strengthening more active corticospinal tract axons 48 or limited apoptosis having occurred before injury in the PRE-natal group 49 but appears to indicate less-effective innervations of the extensor muscles.
With unilateral brain injury occurring after pruning of the ipsilateral corticospinal projections, such as in the POST-natal group, neural reorganization may involve the remaining indirect contralesional pathways, similar to stroke occurring in adulthood.50,51 A possible alternative means of neural reorganization is through the RS pathway. Shoulder abductors, wrist/elbow flexors, 25 and intrinsic hand muscles 24 have been activated from the reticular formation in the macaque. Our results support this hypothesis, in that relatively higher levels of weakness are observed across all joints in POST-natal compared with PRE-natal/PERI-natal groups. In addition, regression comparisons with other timing groups showed that the muscles activated by the RS tract (flexor regression—SB, EF, WF, and FF) were less weak than those without demonstrated RS innervation (extensor regression—SD, EE, WE, and FE). This is consistent with described innervation of the RS system, specifically diffuse proximal innervation, limited distal influence, 23 and more flexor than extensor innervation. 52 Previous studies investigating upper-extremity isometric strength following stroke in adulthood did not find a difference in residual weakness between shoulder and elbow either, 53 but reported more pronounced hand and wrist weakness, 54 comparable to that in the POST-natal group in this study (Figure 4). These similarities indicate that findings in adult stroke may be relevant to the POST-natal CH population, but further study is warranted in the younger group to fully explore the potential impact of development.
Clinical Implications
Most clinical assessments of impairment were unable to differentiate between the 3 CH timing groups. This study was not intended to elucidate differences in a total population, and the chance that our cohorts were statistically similar in low-resolution clinical exams requiring submaximal efforts demonstrates the advantage of quantitative measures such as the ones used in this study. Weakness is one aspect of impairment and was not directly tested in the selected motor examinations, with the exception of the grip strength test, which did demonstrate significant differences between groups. Of note is the statistical trend found in the dissociated movements section of the QUEST, with lower scores found in the POST-natal group. The QUEST includes assessments of abnormal movement synergies, and the lower scores may indicate the presence of a loss in independent joint control in the POST-natal group. With the use of a quantitative measure with high resolution and accuracy, significant differences in the distribution of weakness were uncovered between different injury timing groups.
There are important implications for therapeutic intervention in the injury timing groups. In the context of the current study, it could be inferred that targeting remnant corticospinal tracts would be beneficial in the POST-natal group, potentially in ways that have been described in the adult stroke literature. 55 Individuals with remaining direct contralesional corticospinal projections, such as the PRE-natal group, are likely to benefit from different types of interventions because their primary deficits may include high levels of obligatory mirror movements during unilateral and bilateral tasks. 56 A greater understanding of mechanisms underlying neurological impairments and associated neural plasticity is required to guide the selection of appropriate, targeted interventions for each of the 3 CH timing groups. Lack of imaging data for every participant in this study limits our ability to draw correlations between lesion morphology and outcomes. However, it has been previously shown that lesion size is not well related to function. 57
Conclusion
In summary, studies conducted to date have shown either differences in etiology based on time of injury or grouped all children with CH together in an effort to understand complicated altered movement patterns.58-61 This study has shown, for the first time, that the distribution of weakness in the upper limb is affected by the timing of brain injury during early neural development and suggests a neuroanatomical explanation. Targeted interventions throughout the lifespan are the best opportunity for clinicians to improve motor performance in CH, and understanding the underlying neural mechanisms would facilitate development of more effective training paradigms.
Footnotes
Acknowledgements
We thank most especially the participants and their families. Donna Hurley, DPT, and Isabel Aguilar played vital roles in participant recruitment. Rachel Hawe, BS, assisted with data collection. Alexis Kuncel, PhD, Laura Miller, PhD candidate, Jacob McPherson, PhD, and Michael Ellis, DPT, provided helpful comments on the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institutes of Health (5R01NS058667-02 and T32EB009406 to JPAD) and the National Science Foundation (graduate student fellowship to TS-M).
