Abstract
One of the most critical aspects of safe operations in biosafety level 3 and 4 and animal biosafety level 3 and 4 biocontainment laboratories is the effective inactivation of biological select agents and toxins in the waste generated in these environments. Steam sterilization has been used for decades to effectively kill microbial contaminants in a variety of medical and commercial settings. In biocontainment research settings, steam sterilization is often used to inactivate biological select agents and toxins in various types of waste prior to removal from the containment laboratory. This method is especially important for types of waste for which other decontamination methods are not as effective or practical, such as chemical decontamination (quaternary ammonium, sodium hypochlorite, formalin fixation, paraformaldehyde), ultraviolet light, or incineration. Bulk trash, animal waste, and animal carcasses in particular do not easily lend themselves to decontamination via chemical or radiation methods. Decontamination of these types of waste remains most effectively achieved with steam sterilization. Here we review the method used in our institute to validate the steam sterilizers (autoclaves) and associated procedures to ensure destruction of microbial contaminants from these challenging types of waste.
Keywords
With biosafety level (BSL-3 and BSL-4) and animal biosafety level 3 and 4 (ABSL-3 and ABSL-4) containment laboratories, it is imperative that all items leaving the containment laboratory are effectively decontaminated to eliminate the presence of biological select agents and toxins. Typically, at least one of the following forms of decontamination is used: chemical decontamination (quaternary ammonium, sodium hypochlorite, alkaline digestion, formaldehyde solutions, or formaldehyde vapor), radiation (ionizing radiation, ultraviolet light), or thermal sterilization (steam, incineration).
Chemical decontamination and, to a lesser extent, radiation, are typically used for surface decontamination of impervious material and equipment. Some types of waste, however, do not lend themselves to decontamination via chemicals or radiation, and some bacterial spores have significant dry heat resistance, making incineration less desirable for this application. 1 For several decades, steam sterilization has been successfully used at multiple government and academic research institutions for the decontamination of trash, carcasses, and other biological waste prior to their removal from BSL-3 and BSL-4 and ABSL-3 and ABSL-4 containment laboratories.
Effective steam sterilization must address key principles: steam quality, chamber pressure, chamber temperature, and time. 2 Steam should be dry saturated steam (dryness fraction ≥97%). 2 Chamber pressure and temperature are usually controlled in unison, with pressures above atmospheric pressure being used to achieve temperatures above the nominal temperature of steam at atmospheric pressure. Achieving higher chamber temperatures results in more efficient (faster) killing of microorganisms. Typical temperatures used in commercial steam sterilization units 2 are 121°C and 132°C; however, other temperatures can be used, provided that the time for which the chamber is maintained at these temperatures is sufficient. In fact, some modern computer-controlled autoclaves use the concept of an F0 (F-naught) value, in which the additive effect of time at various temperatures throughout the cycle are calculated to achieve the sterilization equivalent to 121°C at 15 psi above atmospheric pressure for 15 minutes. 3 This allows for time spent at relatively lower temperatures to count toward the total sterilization effect of the cycle and can significantly reduce sterilization time requirements. Utilizing standard autoclave cycles typically results in a 10-3 to 10−6 reduction in viable organisms 4 ; however, some organisms, such as prions, may require additional time and/or temperature to achieve the desired reduction in bioburden. 5 The Centers for Disease Control and Prevention guidelines stipulate a sterility assurance level of 10−6 for microbiological and biomedical laboratories. 6
While the principles of steam sterilization used for biological waste decontamination are identical to those used for disinfection and sterilization of instruments and supplies in the health care industry, the nature of these types of waste introduces additional challenges to the sterilization process and the validation thereof. These challenges include variability in thermal mass and density, high water content, presence of trapped air pockets, and differences in autoclave design, efficiency, and sterilization cycle capabilities and configurations.
Variability in thermal mass and density is an especially challenging aspect of biohazard waste sterilization, particularly when sterilizing large amounts of animal tissue or carcasses. In standard autoclave cycles utilized in the health care industry, steam sterilization is used to sterilize instruments and supplies that are constructed of impervious materials that readily conduct heat, such as metal and plastic, or fabrics and other porous materials that can be effectively penetrated by the steam within the autoclave chamber. However, this is not the case when sterilizing animal waste, tissues, and carcasses. These materials do not readily conduct heat; in the cases of carcasses, some tissues (eg, skin, fat, and muscle) act as effective insulators and impede the conduction of heat to the deeper tissues in the carcass. Nor do these materials have sufficient porosity to allow for the effective penetration of steam. As a result, significant additional time must be programmed into the autoclave cycle to ensure that sufficient sterilization temperatures are reached at all levels of the biohazard waste within the autoclave.
Water content, particularly in carcasses and animal waste, is another challenging aspect of sterilization. High water content further slows the conduction of heat through the tissues due to the water’s large capacity to absorb heat energy. Additionally, the high water content of these materials dictates that a liquid sterilization cycle must be used to avoid vaporization of autoclave contents at the end of the cycle. Liquid sterilization cycles differ from dry cycles most significantly in the way that pressure is evacuated from the chamber at the end of the cycle. In a liquid cycle, the rate of pressure release from the chamber is controlled to minimize the flash boiling of water to steam. This allows any liquid contents that are in the chamber to cool as chamber pressure is gradually decreased to atmospheric pressure. In other types of cycles, the pressure is evacuated from the chamber abruptly, often assisted by vacuum, which results in the flash boiling/vaporization of any liquid in the chamber. This abrupt reduction in pressure is designed to flash off and remove any water in the chamber to assist in drying of the load.
Animal carcasses, tissues, and waste are packaged prior to steam sterilization to prevent personnel and environmental contamination, contain the materials, and maintain autoclave cleanliness. Packaging typically consists of 1 to 3 layers of impermeable heat-resistant plastic autoclave bags and/or a cardboard box that provides some structural rigidity to the package. While necessary, this packaging has the potential to further impede the penetration of steam and heat into the biohazard waste. Additionally, any pockets of trapped air created by this packaging will act as an insulator and further impede the conduction of heat. Therefore, care must be taken while packaging biohazard waste to ensure that none of the packaging is sealed air-tight and that some movement of air into and out of the package is maintained. 7
The final challenge for sterilizing this type of material is the significant difference in efficiency that is inherent to the physical engineering of the multiple makes and models of autoclaves that may be found in any given institute. The removal of air from the chamber and load prior to the exposure/kill phase of a cycle differs significantly among manufacturer, machine model, and cycle configuration. Some autoclaves are only capable of gravity displacement with steam pressure to push air from the chamber out through the drain. With this process, air evacuation is often incomplete and greatly impedes steam penetration and heating efficiency. In an autoclave that performs a prevacuum, the contents are subjected to ≥1 vacuum pulses prior to the exposure/kill phase to remove entrapped air from the contents. With this process, air evacuation is more efficient and complete, resulting in significantly faster steam penetration and heating efficiency. Various modifications of these processes—such as the steam flush-pressure pulsing and super-atmospheric steam-vacuum pulsing—may further alter air evacuation efficacy. 2
Methods
An appropriate validation/verification protocol for steam sterilization should include initial installation qualification (IQ), operational qualification (OQ), and performance qualification (PQ) tests. 8 A robust system of documentation must be established to accompany all 3 phases (IQ, OQ, PQ) of the validation/verification process.
IQ is completed once the autoclave has been installed; all aspects of the design requirements (established prior to acquisition of the autoclave) must be satisfactorily addressed. For autoclaves used for the sterilization of biological waste from biocontainment suites, this validation should address unique containment laboratory characteristics, such as one-way door interlock systems, chamber drain effluent routing, chamber effluent filtering, and vacuum pump discharge. In our institute, various vendors over the past 20 years have installed multiple makes and models of autoclaves, and IQ was performed and documented as part of the initial validation of the equipment jointly by both the vendor and the institute per the acceptance criteria established contractually.
OQ includes verification that the installed equipment is operating properly within predetermined limits when used by trained personnel in accordance with standard operating procedures. 8 Unlike, IQ, OQ is not a onetime event but rather should be accomplished on a recurring basis to ensure continued verifiable operation of the autoclave over time by institute staff. The formal tests to perform should include, at a minimum, a vacuum leak test, air evacuation/steam penetration test (Bowie-Dick or equivalent test), steam quality testing, temperature and pressure sensor calibration, equipment preventive maintenance, and integrator strip testing. 8 An example of an OQ program used by our institute is described in Table 1.
Recurring OQ Tests for Sterilizer Validation.
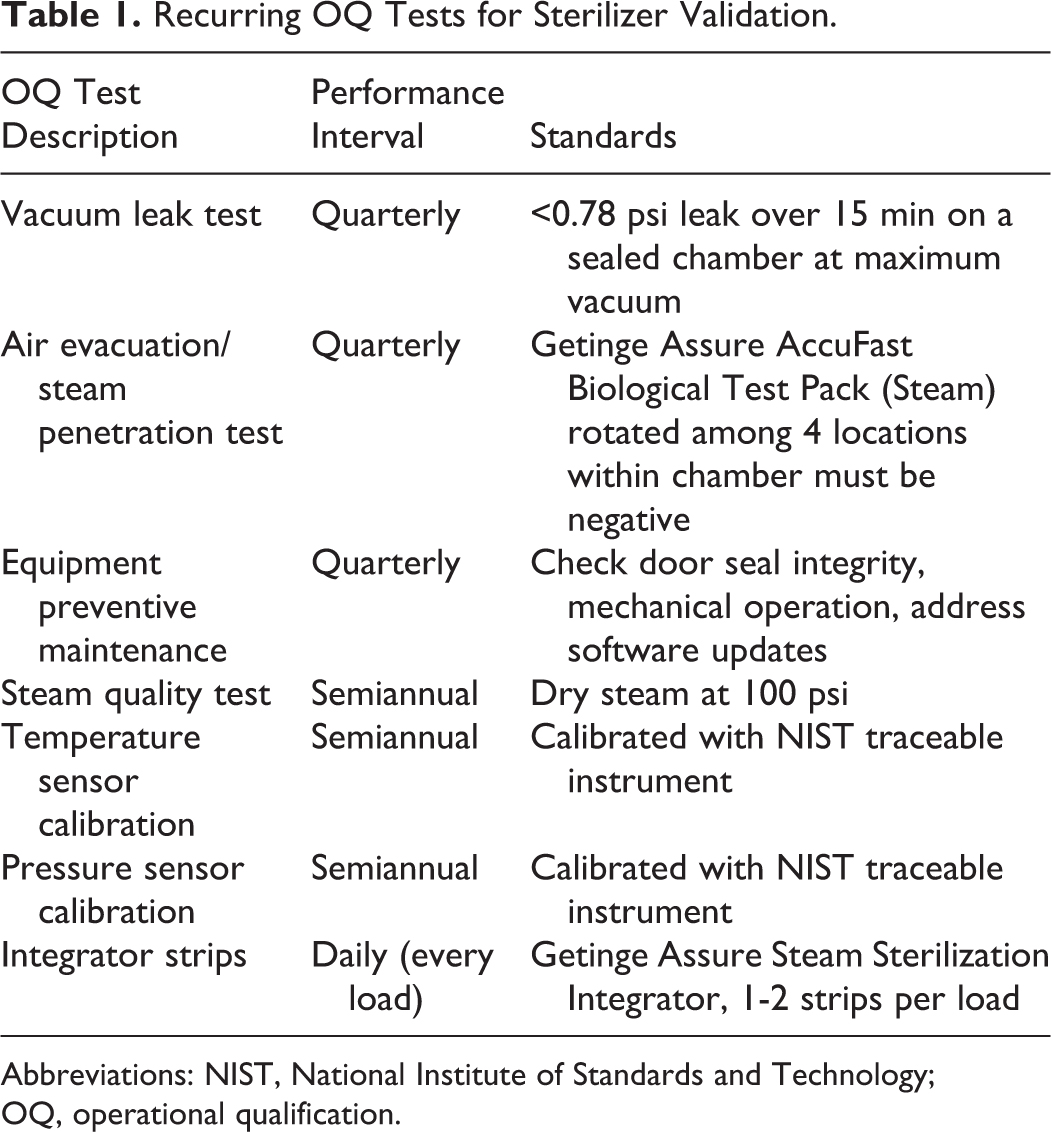
Abbreviations: NIST, National Institute of Standards and Technology; OQ, operational qualification.
The PQ phase of autoclave verification must be designed to verify that the equipment is able to deliver the desired lethality when used by qualified personnel in accordance with standard operating procedures and therefore has, as a prerequisite, a robust and successful IQ/OQ program. 8 PQ testing should include both physical and biological measurements to determine repeatable, uniform lethality in a typical autoclave load. Due to the large number of autoclaves in use at our institute and to account for differences in performance, autoclaves were subgrouped according to control system, design specification, and operational characteristics; PQ verification was performed on representative autoclaves from each subgroup.
For this validation, each autoclave subgroup was verified for both liquid (for carcasses) and dry/wrapped goods (for trash and laundry) cycles. The liquid cycle was verified with 6 nonhuman primate carcasses, each weighing no more than 10 kg, for a total maximum load of 60 kg. Nonhuman primate carcasses were used for the liquid cycle verification because, in our experience, they are the most challenging type of waste to sterilize; these carcasses were sourced from Institutional Animal Care and Use Committee–approved animal protocols that were occurring in the laboratory serviced by the autoclave being verified, thus avoiding the need for using additional animals specifically for the verification process. The dry/wrapped-goods cycle was verified via a mixed load of 3 or 4 bags (enough to fill the chamber while maintaining a minimum 2-inch clearance between the load and all interior surfaces of the autoclave chamber) of dry trash and/or laundry, also sourced from the trash/laundry being generated as part of normal laboratory operations. These load size limits were determined by the volume capacity and efficiency of the autoclaves within our facility. The temperature limits were determined by the ability of the bags, packaging materials, and fabrics to withstand high temperatures. All test runs were conducted through our facility’s standardized packaging procedures for the appropriate types of waste.
Biological indicators (BIs) were used to evaluate the efficacy of each sterilizer run. Our institute used MagnaAmp
Following the sterilization cycle, the contents of the autoclave were brought back into the containment laboratory where they originated, and the BIs and data logger were retrieved, decontaminated, and removed from the laboratory for incubation. For easier retrieval and positive identification following the sterilization cycle, both the BIs and the data logger were identified by a plastic tag with a unique identifier, which was secured to the BI or data logger with Kevlar dental floss. Following confirmation of successful autoclave verification, the remaining contents of the autoclave verification run were resterilized prior to leaving the containment laboratory.
BIs were incubated per manufacturer instructions at 57°C for 48 hours and observed for color change and/or turbidity, which indicates spore germination; 1 ampoule containing spores that was not sterilized (positive control) and 1 ampoule not containing spores that was not sterilized (nonsterilized negative control) was incubated concurrently with the BIs from each verification run. Data from the data logger were downloaded for analysis.
Results
During the validation of the numerous autoclaves at our institute, we encountered considerable differences in unit efficiency. Not surprising, the more modern autoclaves that employed prevacuum air evacuation at the beginning of the cycle were far more efficient. They were able to achieve sterilization of test loads in liquid cycles in <4 hours and in dry/wrapped-goods cycles in <2 hours. Other older autoclaves relying on gravity displacement required as much as 7 hours to achieve sterilization in liquid cycles and as much as 3 hours in dry/wrapped-goods cycles. To account for these differences in efficiency, we used the verification results of the least efficient autoclave, with an additional safety margin, to develop a single standard for all autoclaves within the facility. Our facility’s liquid cycle standard for carcass decontamination is an 8-hour exposure time at 121°C, and the dry/wrapped-goods cycle standard for trash and laundry is 4 hours at 121°C. These exposure times and temperatures are unique to our institute’s existing equipment and standard operating procedures; operating parameters for any new autoclaves will have to be validated to confirm that the standard facility procedures for autoclaving carcasses and dry waste are adequate for effective decontamination of these types of waste. No attempt should be made to extrapolate these values to equipment in other facilities without proper validation.
The need for these extended cycle times is a direct result of the list of challenges for autoclaving waste reviewed earlier. In our experience, the most challenging type of biological waste to sterilize is animal carcasses. Various barriers—including multiple layers of sealed plastic autoclave bags, cardboard boxes with tight-fitting lids, high tissue density and water content, and the insulating properties of other animal tissues (eg, fat and hair)—significantly hamper air extraction and steam penetration into the center of the carcass. One cannot overstress the importance of removing as many of these barriers as is feasible. In our experience, reducing the number of bags, maintaining a loose closure on bags, and predrilling holes in the cardboard boxes used for rigidity is critical to ensure proper sterilization. However, even with these controls in place, extended exposure times were required to achieve sterilization at the center of the carcass.
The results of the data logger used in our verification process demonstrated that successful sterilization of a carcass does not necessarily require attaining the same temperature at the center of the carcass tissue mass as is attained in the autoclave chamber. As mentioned in the discussion of the F0 sterilization concept, even relatively lower temperatures can have a lethal effect on microbes, provided they are exposed for a sufficient amount of time. Peak core carcass temperatures of 110°C to 115°C registered by the data logger were uniformly lethal for the spores in the adjacent BIs, provided the time held at these temperatures was sufficient. To predict lethality more accurately during our verification process, we developed a time/temperature lethality curve (Figure 1) for the BIs. This was accomplished in an empty autoclave with BIs placed directly in the autoclave chamber. The results of this lethality curve correlated accurately with the combined results of the BIs and data logger time/temperatures encountered in our liquid cycle and were predictive of successful validation tests in carcasses.
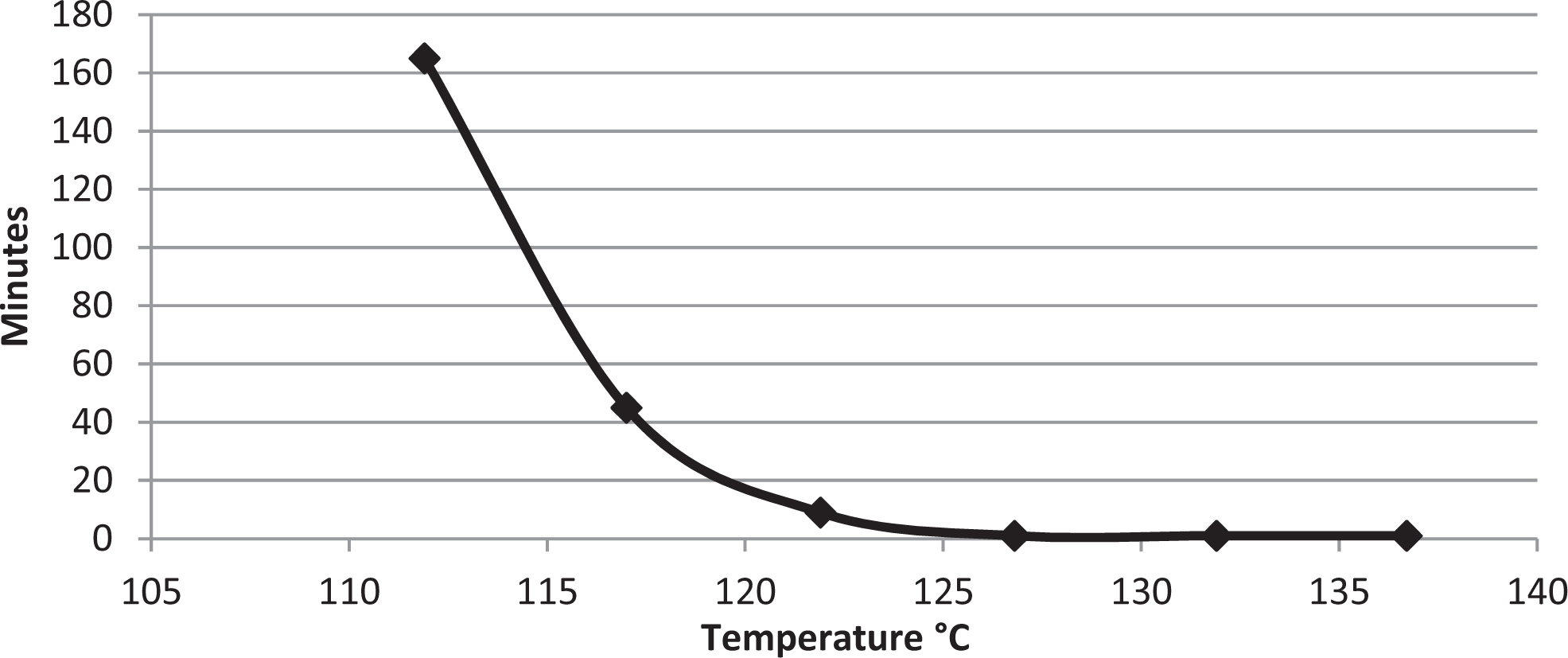
Time versus temperature curve for predicting 100% lethality for
For the purposes of uniformity and reducing potential for user error, load limits in our institute are standardized for all autoclaves, based on the capacity of the smallest units. However, during the verification of some of the larger autoclaves, the size of the loads were increased to determine the maximum potential load size for these larger units. In our experience, physical volume of the chamber was the only significant limiting factor on the maximum load volume. Data from our verification tests indicate that the more substantial steam supply and greater thermal mass of chamber and steam jacket walls were more than sufficient to offset the increased autoclave load. However, one factor that had a significant effect on sterilization efficacy was the temperature of the contents at the beginning of the cycle. Verification tests carried out on frozen carcasses required significantly more time (hours) to achieve sterilization. As a result, standard operating procedures at our institute dictate that the contents of the autoclave must be >0°C at the beginning of any cycle.
Discussion
Reliable lethality of sterilization cycles used for all types of waste (BSL-3, BSL-4, ABSL-3, and ABSL-4 biocontainment laboratories) is a critical component to safe biocontainment laboratory operation and is crucial to protect public, occupational, and environmental health. A number of challenges must be overcome when using steam sterilization to process these unique types of waste. The process described here has been used to successfully validate the numerous models and designs of autoclaves operated in our institute. As with any validation process, robust documentation of the validation plan and all results is essential. Some parts of the validation process, such as the IQ portion, will occur only at the time of installation and following any major upgrades to design or function. Other parts of the validation process, such as the OQ, must be performed on a recurring basis to ensure that operation of the sterilization units is reliable and consistent. Similar to IQ, the PQ process must be conducted following initial installation and any time there are significant changes in equipment, design, or user standard operating procedures, particularly when sterilization of waste is such a critical component of safe biocontainment laboratory operation. In performing PQ and developing standard operating procedures, physical characteristics unique to the biohazard waste generation practices of the facility that might affect sterilization efficiency should be carefully considered. While time-consuming, this steam sterilization validation process is essential to maintain the public trust in our ability to safely work with biological select agents and toxins.
Footnotes
Authors’ Note
Opinions, interpretations, conclusions, and recommendations stated within the article are those of the authors and are not necessarily endorsed by the US Army or the Department of Defense. Special thanks to Philip Haines and Jeremiah DeWolf for their extensive technical expertise in steam sterilizer theory, operation, and validation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
