Abstract
Breast cancer is the most prevalent form of cancer in women. Despite significant advances in conventional treatment, additional safer complementary treatment options are needed. Recently, ozone therapy has been considered as a type of medical adjunctive treatment that could inhibit cancer cell survival and reduce chemoresistance. However, only a few studies have been conducted on its use in breast cancer, and the optimal dosage and time of administration are unknown. Currently, preclinical studies suggest that ozone alone or in combination with chemotherapy is an effective method for inhibiting breast cancer cell growth. However, rather than investigating the effects of ozone as an antitumor therapy, current clinical trials have generally assessed its effect as an adjunctive therapy for reducing chemotherapy-induced side effects, increasing oxygen tension, normalizing blood flow, restoring blood lymphocytes more rapidly, and reducing fatigue symptoms. In this article, the use of ozone as a medical adjunctive treatment for breast cancer and its role in integrative therapy are summarized and discussed.
Introduction
Breast cancer is one of the most prevalent cancers affecting women worldwide. Despite significant advances in conventional treatment options, safer and more effective alternative therapies are needed, especially for patients with late-stage disease.
Ozone (O3), which is one of the most harmful pollutants if inhaled, can be used as an immune bioregulator in adjunctive medical treatment via parenteral, topical, or injection routes, owing to its hormetic action.1,2 Its mechanisms of action in medicine have been researched over the past 20 years. Ozone has been proposed for use in treating various pathologies. 3 In medical care, ozone therapy, which has been used for almost 60 years, 4 acts by exerting controlled levels of oxidative stress produced by ozone reactions that promote the upregulation of the antioxidant system and boost the immune system.5 -7 It involves the administration of ozone, an allotrope of oxygen, to the body. Ozone can increase the oxygen concentration in tissues and induce antimicrobial effects capable of causing chromosome breakages in human cell cultures. 8 In 1974, Wolff 9 first used ozone therapy as ozonated auto-hemotransfusion (O3-AHT). Ozone therapy has subsequently been used as an adjunctive medical treatment in various medical conditions, including cancer.10 -13
Based on the literature, ozone therapy has emerged as a potential adjunctive treatment in different types of cancer because of its immunomodulatory, anti-inflammatory, and oxidative stress-inducing properties.14,15 In this review, we summarize and discuss ozone therapy as a medical adjunctive treatment for breast cancer and its use in integrative therapy, including its mechanism of action, preclinical and clinical evidence, safety, and challenges with its use.
Literature Search Methods
We conducted a literature search to find articles in which ozone has been used to directly kill breast cancer cells in vivo, in vitro, or in human patients. We conducted a systematic review by searching in the PubMed database and Google Scholar, including different types of articles (preclinical controlled, preclinical non-controlled, and case series). 15 English language was set as search restriction criterion, and no other restrictions were applied to the year of publication, study type, or sample size. All relevant studies that focused on basic research on ozone for treating breast cancer were included. The search was conducted using a combined filter and the following medical subject headings (MeSH) terms: [“Ozone/breast cancer” (MeSH) OR “Ozone/breast carcinoma” (MeSH) OR “Ozone/mammary cancer” (MeSH)]. The PubMed search identified 41 references. After a critical reading of the title and abstract, preclinical, and clinical studies that did not focus on treating breast cancer using ozone directly were excluded. After a critical reading of the title and abstract, 14 articles fulfilled the scope of the review.
Mechanism of Ozone Therapy
Ozone is a potent oxidizing agent that induces oxidative stress in cells and tissues. Although controlled oxidative stress can play a role in angiogenesis, excessive and uncontrolled production of reactive oxygen species (ROS) may lead to cellular damage and contribute to the development of oxidative stress-related diseases.16,17 ROS act as regulators of important signaling pathways. The ozone dosage is important for determining the effects of ROS. At low levels, ROS act as a “redox messenger” in intracellular signaling and regulation and can be recruited to act as “Trojan horses” to kill cancer cells. Previous studies suggest that a mild excess of ROS can induce oxidative modification of cellular macromolecules, inhibit protein function, and promote cell death,17,18 but that at moderate levels, ROS may promote tumor progression. At high levels, ROS increase oncogene activity and stimulate growth factor-dependent pathways and oxidizing enzymes, inducing genetic instability.17,19,20 Specifically, small increases in ROS preferentially activate the PI3K/Akt pathway, whereas further increases trigger MAPK-dependent apoptosis.21,22 The cellular responses to ROS are also associated with their location—mitochondrial ROS can promote cell death; however, in contrast, NOX-generated ROS is associated with the promotion of cell proliferation and migration. 17
Ozone-dependent ROS-mediated fatty acid oxidation is involved in the formation of lipid ozonation products, and these processes are associated with the Nrf2/Keap1/ARE and AMPK/FOXO/mTOR/Sir1 pathways and Nrf2/NF-κB crosstalk. 23 Moreover, ROS damages lipids, proteins, and DNA. Thus, an increasing number of therapeutic strategies is being developed to elevate ROS levels to overwhelm the redox adaptation of the cells by inducing oxidative stress. These include the use of platinum drugs, bortezomib and procarbazine, for treating Hodgkin’s lymphoma, breast cancer, and head and neck squamous cell carcinoma.17,24,25 Ozone is primarily a strong oxidant; however, when it is used as a medical drug, it is crucial to carefully monitor the dose and exposure time to avoid harmful effects on healthy tissues and organs.26,27
Increasing attention is also being paid to the immunomodulatory properties of ozone therapy. By interacting with the immune system, ozone therapy exerts a range of effects, including the activation of immune responses, regulation of cytokine production, and modulation of inflammatory processes.3,28 The effects of ozone on macrophages, T cells, B cells, NK cells, and dendritic cells can be used in the treatment of infectious diseases, autoimmune disorders, and cancer immunotherapy. 1 In clinical use, ozone therapy not only increases leukocyte activity and the immunoglobulin G (IgG) level in patients with selective immunoglobulin A deficiency, 29 but ozone has also been shown to increase the production of both IL-8 and tumor necrosis factor alpha (TNF-α) in a human monocytic cell line (THP-1 cell) model.1,30,31 Owing to its immunomodulatory and anti-inflammatory effects, ozone affects the tumor microenvironment (TME), which plays a critical role in cancer initiation, progression, and response to therapy. Ozone affects the TME by influencing immune cells, cytokine production, angiogenesis, and extracellular matrix remodeling. Thus, understanding the immunomodulatory effects of ozone therapy could facilitate its integration into disease management, either as a standalone therapy or as an adjuvant to existing therapy.
Moreover, ozone modulates pro- and anti-angiogenic factors, influences endothelial cells, remodels the extracellular matrix, and regulates angiogenesis by modulating vascular endothelial growth factor (VEGF) expression,32 -34 which offers potential therapeutic benefits in wound healing, ischemic conditions, and tissue regeneration. Thus, careful consideration of the ozone dose and treatment duration is necessary to prevent potential complications associated with altered vascular permeability (Figure 1).
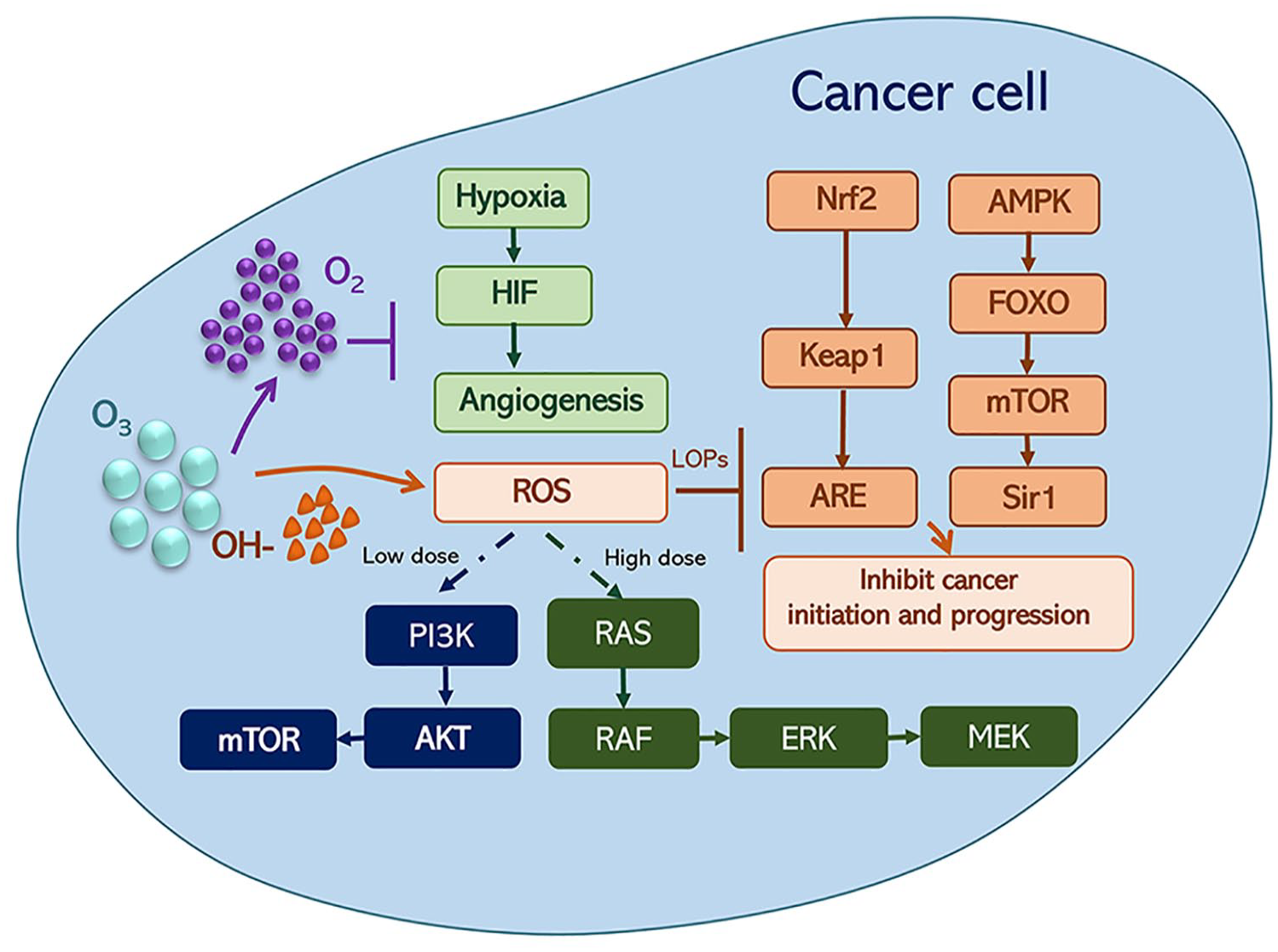
Ozone (O3) can generate hydroxyl radical (OH−) and oxygen (O2), which could have anticancer effects by inducing reactive oxygen species (ROS) anticancer effect and relieving hypoxia. Light green labels: Oxygen relieves hypoxia. Hypoxia inhibits hypoxia-inducible factor (HIF) generation and angiogenesis; Brown labels: OH−-associated high-level ROS can block the activation of the Nrf2/Keap1/ARE and AMPK/FOXO/mTOR/Sir1 pathways. Dark blue labels: Low doses of ROS activate the PI3K/Akt pathway; Dark green labels: High doses of ROS can trigger MAPK-dependent apoptosis.
Side Effects and Safe Dose of Ozone Therapy
Despite the effectiveness of ozone therapy, its potential adverse effects must be carefully considered. Ozone can be administered through various routes, such as intravenous, intramuscular, rectal insufflation, or topical application, and different modes of administration have different toxicities. Each method has unique safety considerations, and an appropriate route of administration should be chosen based on the patient’s condition and medical history. At an appropriate dose, ozone does not induce toxic effects on the cells of normal tissue because the antioxidant system of the cells can typically handle mild ozone-induced injury2,23; however, at high concentrations, it may cause serious side effects, including respiratory and vascular effects, allergic reactions, hemolysis, and transient oxidative stress.15,35
Previous studies have shown that short-term exposure to ozone may result in acute respiratory inflammation. Inhalation of ozone gas can irritate the respiratory system and cause coughing, chest discomfort, and shortness of breath.36,37 Proper ventilation and air purification are essential in ozone therapy clinics to minimize the risk of respiratory side effects. Ozone can influence vascular function and blood flow. In some contexts, it enhances blood vessel formation, leading to improved tissue oxygenation, whereas in other contexts, it causes vascular constriction. Ozone also can increase the number of white blood cells, activate red blood cell metabolism, improve the oxygen saturation of hemoglobin, and promote platelet aggregation.34,35,38,39
Thus, the optimal dose and treatment duration should be carefully considered to minimize oxidative damage. Further research is required to determine the long-term effects of increased oxidative stress. The safe dose of ozone varies according to disease type and location. 40 In animal models, concentrations of ozone ranging from 10 to 80 µg/mL are beneficial with positive effects and no toxicity; however, in humans, the safe dose varies between 15 and 50 µg/mL.41 -44
Challenges of Ozone Therapy
Although ozone therapy has shown promising results in preclinical studies and a limited number of clinical trials, several challenges and limitations must be considered before its widespread application in breast cancer treatment. The biggest challenge is the lack of standardization of the ozone dose used in previous studies, with several reports not specifying the dose that was used. This may be because of the unstable properties of ozone gas, which makes it difficult to measure. 45 However, the non-specific nature of ozone therapy may limit its ability to specifically target cancer cells. Ozone-induced oxidative stress affects not only tumor cells but can also affect healthy cells and lead to unintended side effects.
Preclinical Studies of Ozone Therapy for Breast Cancer
Preclinical studies have assessed the effects of ozone therapy on the development of malignancy and the prognosis of established cancer. Only a few basic research studies on ozone therapy for breast cancer treatment have been published. These are summarized in Table 1.
Preclinical Studies of Ozone for Treating Breast Cancer.

Abbreviations: 5-FU, 5-fluorouracil; O3_PFD@ liposome, ozone-carrying liposome perfluorodecalin nanosystem; PAM, plasma-activated medium; Ref: reference; TNBC, triple-negative breast cancer.
In 1980, Sweet et al 12 reported that ozone therapy was effective for treating breast cancer. The growth of human breast cancer cells was inhibited in a dose-dependent manner by ozone at 0.3 to 0.8 parts per million of ozone in ambient air over an 8-day period. The presence of ozone at a concentration of 0.3 to 0.5 parts per million inhibited cancer cell growth by 40% and 60%, respectively, and at a concentration of 0.8 parts per million, cancer cell growth was inhibited by more than 90% compared with 50% inhibition in normal cells.
In 1990, Zänker and Kroczek 46 found that ozone had an effect on increasing ROS levels within cultured cells, similar to that of chemotherapeutic drugs. They reported that ozone and 5-fluorouracil (5-FU) had a synergistic or additive effects on breast cancer, and that ozone could overcome 5-FU resistance.
In 2018, Mokhtari et al 47 showed that the generation of ozone by cold atmospheric pressure plasma-activated medium (PAM) was effective in suppressing SKBR3 and MCF7 breast cancer cell lines, and that increasing the PAM application time induced more ozone generation, accompanied by greater cytotoxicity. Ozone-induced ROS triggered the c-Jun NH2-terminal kinase (JNK) and p38 kinase pathways and promoted mitochondrial perturbation.
In 2022, Karagulle and Yurttas 48 detected anticancer effects of ozone after doxorubicin chemotherapy in the MCF-7 human breast cancer cell line (luminal-A type). MCF-7 cells were cultured with different concentrations of doxorubicin (1-50 μM) for 24 hours, and then half of each group were treated with 30 μg/mL ozone for 25 minutes as the combination therapy groups. The MCF-7 cells treated with doxorubicin + ozone had lower viability than the MCF-7 cells treated with doxorubicin alone, and the combined treatment enhanced the apoptotic effect of doxorubicin. The combined treatment reversed the suppression of TNF-α levels by doxorubicin and considerably reduced doxorubicin-induced suppression of matrix metalloproteinase-2 (MMP-2) and MMP-9 levels. Thus, ozone treatment potentiated the apoptotic and anticancer activities of doxorubicin in MCF-7 cells by activating the expression of TNF-α, MMP-2, and MMP-9. Moreover, in 2023, Karagülle and Yurttaş 49 detected the effect of ozone plus doxorubicin chemotherapy in the BT-474 human breast cancer cell line (luminal-B type) again; the results showed that doxorubicin’s anti-proliferative and apoptotic effects could be enhanced by ozone in BT-474 cells.
In 2022, Merve Yıldırım et al 50 described the dose-dependent effects of ozone therapy. Ozone treatment was performed in isotonic sodium chloride solution at 5, 10, or 20 μg/mL concentrations, and were applied to the MDA-MB-231 breast cancer cell line and the human umbilical vein endothelial cell (HUVEC) normal cell line. The ozone-treated MDA-MB-231 cells had an increased rate of cell death and decreased migration potential. The mRNA expression levels of pro-apoptotic genes were several-fold higher in the MDA-MB-231 cells after 10 μg/mL treatment. These experiments revealed that ozone causes death of MDA-MB-231 cancer cells, whereas the same ozone concentration has little or no cytotoxicity in normal HUVEC cells. Therefore, ozone therapy administered at an appropriate dose is effective and safe.
Furthermore, to address the challenge of ozone instability, ozone-coated nanomaterials have been developed and used as a potential treatment for triple-negative breast cancer (TNBC).10,51 In a previous study, we developed an ozone-carrying liposome perfluorodecalin (PFD) nanosystem (O3_PFD@Liposome), which promoted ozone solubility 18.4-fold compared with ozone in water solution. These particles increased ozone-induced ROS under the stimulation of X-ray irradiation. The combination of O3_PFD@Liposome and irradiation induced apoptosis and immunogenic cell death in vitro and sensitized radiotherapy in vivo without any obvious toxicity. The combination regimen enhanced the infiltration of lymphocytes into the TME by inducing immunogenic cell death, releasing neoantigens, and relieving hypoxia. 10 Moreover, in 2023, a novel Pt (IV)-prodrug self-assembled micelles of O3_PFD@PtF was created that represented high efficiency and safety. In this new nano-particle, ozone was well stabilized, and the ROS from the ozone decomposed rapidly, relying on the irradiation excitation. O3_PFD@PtF plus irradiation had a strong inhibitory effect on triple-negative breast cancer (TNBC) cell proliferation in vitro, outperforming the conventional cisplatin plus irradiation group. 52
Clinical Studies of Ozone Therapy for Breast Cancer
The integration of ozone therapy with conventional cancer treatments such as chemotherapy, radiation therapy, and immunotherapy requires careful consideration. Understanding the potential synergistic effects and adverse interactions between ozone therapy and standard treatments is crucial for the development of effective and safe combination therapies. However, few clinical trials have used ozone as an antitumor therapy for breast cancer. Ozone is generally used as an adjunctive therapy for breast cancer. Thus, extensive clinical trials are needed to further elucidate the anticancer effect of ozone. Clinical trials of ozone-related therapy for breast cancer are summarized in Table 2.
Clinical Studies of Ozone Therapy for Breast Cancer.

Abbreviations: AHT, auto-hemotransfusion; BC, breast cancer; BCRL, breast cancer-related lymphedema; Ref, reference.
In 2001, Kontorshchikova et al 53 enrolled 32 patients with breast cancer in a clinical trial. The patients received ozone therapy via intravenous infusion, rectal insufflation, and ozonated water after chemotherapy. The results confirmed that ozone therapy decreased the incidence and degree of cytostatic toxicity, improved the quality of life, and immunological parameters, and significantly increased the activity of the antioxidant defense system.
In 2011, Clavo et al 54 reported using ozone therapy to treat a patient with breast cancer with a persistent PORT-A-CATH®-related fistula and fibrosis in a previously irradiated area. After using insufflations of an O3/O2 gas mixture (100 μg/mL) through the fistulous cavity and multiple infiltrations for 8 sessions, local pain and symptoms significantly improved, and the subcutaneous induration decreased.
In 2012, Alekberov and Potanin 55 reported the use of ozone therapy in patients with breast cancer who underwent breast reconstruction. A total of 151 patients were enrolled, of whom 71 were given ozone therapy in the form of an ozone-oxygenated crystalloid solution. After ozone therapy, the oxygen tension in the tissues and blood increased, blood flow normalized, and the blood lymphocytes were more rapidly restored after breast reconstruction surgery. Furthermore, in patients who received ozone therapy, the frequency of early postoperative complications such as necrosis of the autotransplant, was 2.5 times lower than that in patients who did not receive ozone-oxygenated crystalloid solution.
In 2013, Waked et al 56 reported using ozone therapy to treat breast cancer-related lymphedema (BCRL). In this randomized clinical trial, patients received ozone therapy after complex physical therapy for lymphedema, consisting of pressure garments, remedial exercises, and skin care for 12 weeks. The treatment was more effective at reducing limb volume and thickness in patients with BCRL.
In 2018, to demonstrate the effectiveness of ozone on treating fatigue in patients with breast cancer, 15 patients with breast cancer were enrolled and treated using ozone via AHT twice a week for 1 month and then twice a month as maintenance therapy, according to the Scientific Society of Oxygen Ozone Therapy protocols. Eleven of the 15 patients (73%) achieved a significant reduction in their level of fatigue, without experiencing significant side effects. These results suggest that ozone therapy could be used as a supportive therapy to reduce fatigue in patients with breast cancer, both during cancer therapy and in a palliative setting. 6
Discussion
Breast cancer is the most prevalent form of cancer in women; thus, additional efforts directed toward finding a new, effective, and safe anticancer medication for human breast cancer, especially for late-stage breast cancer, are needed.48,57 Recently, ozone has been used as a novel method to reduce inflammation in preclinical and clinical settings. The results suggest that ozone therapy can modulate the TME, induce cancer cell death, and enhance immune response against cancer. Here, we reviewed the application of ozone for the treatment of breast cancer.
Ozone therapy has attracted clinical interest in the field of oncology because it could change the TME and inhibit the level of cytokines related to cancer cell survival and chemoresistance. 58 However, the effect of ozone is dose dependent and has different effects at different concentrations in the 1 to 50 μg/mL range.48,59,60 Several challenges and limitations remain, warranting further research and well-designed clinical trials to establish its safety, efficacy, and optimal application of ozone therapy in different cancer types and stages. Results of previous studies have shown that ozone has variable effects, and previous studies have revealed that not all tumors are equally susceptible to ozone therapy. 15 In a rat C6 glioma cells model, daily application of ozone induced an increase in cell proliferation and an increase in DNA concentration. Conversely, applying ozone every second day reduced the C6 cell concentration in vitro. 23 Cholesterol and triglyceride concentrations are associated with effects of ozone. At a high ozone dose, cholesterol and triglyceride concentrations were reduced by 40% and 25%, respectively, but at a low ozone dose, cholesterol and triglyceride concentrations increased by 50% and 30%, respectively. Thus, administering a low ozone dosage may be most effective for treating tumors via the regulation of ROS concentration.23,61
We found 9 preclinical studies published to date (2023) that indicated that ozone alone or in combination with chemotherapy is an effective method for inhibiting breast cancer growth. In 1980, Sweet et al 12 demonstrated that the growth of human breast cancer cells could be inhibited by ozone in a dose-dependent manner. Ten years later, in 1990, Zänker and Kroczek 46 found that ozone had an effect similar to that of chemotherapeutic drugs in increasing ROS levels inside cultured cells, and could enhance the anticancer properties of 5-FU. We found no further preclinical studies on ozone therapy for breast cancer published until 2018. From 2018 to 2022, studies by Mokhtari et al, 47 Karagulle and Yurttas, 48 and Merve Yıldırım et al 50 demonstrated that ozone alone or in combination with chemotherapy, such as doxorubicin, can inhibit breast cancer cell lines by inducing ROS-triggered JNK and p38 kinase pathways; potentiate apoptotic and anticancer activities by activating TNF-α, MMP-2, and MMP-9 expression; and inhibit cell growth by increasing the mRNA expression levels of pro-apoptotic genes. We have previously demonstrated that photon radiation therapy combined with ozone treatment can regulate PD-1 activation in the TME and enhance the effects of radiation by promoting OH− generation in breast cancer. 10
However, few clinical trials have used ozone as an antitumor therapy for breast cancer. Recent studies have shown that ozone therapy is potentially a valuable adjuvant regimen. From 2001 to 2018, studies by Kontorshchikova et al, 53 Clavo et al, 54 Alekberov and Potanin, 55 Waked et al, 56 and Tirelli et al 6 demonstrated that ozone therapy can reduce chemotherapy-induced side effects, improve persistent PORT-A-CATH®-related fistula and fibrosis, increase the oxygen tension in the tissues and blood, normalize blood flow, restore blood lymphocytes more rapidly in patients undergoing breast reconstruction, cure BCRL, and reduce fatigue symptoms.
Although ozone therapy has been shown to be effective in breast cancer treatment in preclinical studies, one major limitation is the lack of clinical trials evaluating the efficacy and safety of ozone therapy in breast cancer treatment as a second- or later-line treatment. Safety considerations and addressing potential challenges are paramount to successful integration of ozone therapy into cancer treatment strategies. Careful dosage and treatment protocols, a comprehensive understanding of immune responses, and personalized approaches are necessary to harness the therapeutic potential of ozone therapy by minimizing risks and optimizing patient outcomes. Further research and well-designed clinical trials are crucial for establishing the safety and efficacy of ozone therapy in breast cancer treatment.
Conclusion
Ozone therapy is a promising complementary treatment option for breast cancer. As the field of oncology advances, the integration of ozone therapy with conventional cancer treatments could potentially improve outcomes in patients with breast cancer. Collaborative efforts among researchers, clinicians, and regulatory authorities are necessary to advance evidence-based integration of ozone therapy with conventional treatments in breast cancer management.
Footnotes
Contributors
Dr. Yanchu Li contributed to the conception of the review, participated in the data collection, and drafting of the manuscript. Prof. Pu Rong supervised data collection and drafted and revised the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Natural Science Foundation of the Science and Technology Bureau of Sichuan, China (2022NSFSC0772).
Informed Consent
Not applicable as this is a review of published studies.
