Abstract
Background:
A prior phase III, multicenter (United States and China), clinical trial found true acupuncture (TA) resulted in lower xerostomia scores 12 months after radiotherapy than that of a standard care control group. This small pilot study examined brain function changes comparing TA to sham acupuncture (SA) in US and Fudan patients undergoing head and neck radiotherapy.
Methods:
To determine cerebral activity during TA versus SA acupuncture, patients underwent electroencephalogram evaluation (EEG) immediately prior, during and after both conditions. Acupuncture occurred during weeks 3 to 5 of radiotherapy, with patients receiving either TA or SA, followed 2 to 3 days later by the other treatment in a counterbalanced manner.
Results:
In the TA minus SA condition (N = 14 Fudan; N = 13 US), most changes were in the delta (0.5-3.5 Hz) and alpha (8-12 Hz) bandwidths. Delta was present in the frontal gyrus and parahippocampal gyrus. Alpha was present in the anterior and posterior cingulate, lingual gyrus, amygdala, precuneus, medial frontal gyrus, fusiform gyrus, and superior frontal gyrus. Maximal cortical differences in the Fudan cohort between TA and SA were in areas previously shown to be associated with (TA). In the US cohort, maximal differences between TA and SA were associated with areas which are usually decreased in TA conditions.
Conclusions:
There were distinct differences in brain function between those receiving TA and SA and there were clear differences between cultures, helping to explain the lack of placebo effect in the Fudan participants and strong placebo effect in the US patients.
Introduction
Radiation-induced xerostomia (RIX), or hyposalivation, affects greater than 50% of head and neck radiation patients and may result in a significant quality of life deficits associated with dental complications, dysphagia, and dysgeusia to name a few, that can last for years following radiotherapy.1,2 Acupuncture has been used successfully to both prevent and treat dry mouth that occurs as a result of radiation to the salivary glands.3-7 Our recently published multicenter clinical trial recruited, randomized, and treated 339 patients undergoing radiotherapy for head and neck cancer at MD Anderson Cancer Center, Houston, Texas, US (MDA) and Fudan University Shanghai Cancer Center, Shanghai, China (FU). True acupuncture (TA) and Sham acupuncture (SA) were given 3 times a week for the 6 to 7 weeks of radiotherapy with patients randomized to TA = 112 patients, SA = 115 patients, or Standard care controls (SCC), SCC = 112 patients (patients who completed baseline and 12-month follow-up). For the primary aim, the adjusted least square mean (SD) xerostomia score in the TA group (26.6 [17.7]) was significantly lower than in the SCC group (34.8 [18.7]) (P = .001) and marginally lower but not statistically significant different from the SA group (31.3 [18.6]) (P = .06). Incidence of clinically significant xerostomia 1 year after radiation therapy ended followed a similar pattern, with 38 patients in the TA group (34.6%), 54 patients in the SA group (47.8%), and 60 patients in the SCC group (55.1%) experiencing clinically significant xerostomia (P = .009). Post hoc comparisons revealed a significant difference between the TA and SCC groups at both institutions, but TA was significantly different from SA only at Fudan and SA was significantly different from SCC only at the MD Anderson. The inconsistent response to placebo acupuncture between centers is what stimulated interest in examining the neurological responses to TA versus SA by site.
Several RCTs of acupuncture to treat a variety of conditions determined that acupuncture improves symptoms clinically, but there is less consistency between the effectiveness of TA compared to SA.8-13 In fact, many hypotheses exist about why placebo works as well as true interventions in some trials, and yet in other trials TA seems to be superior. Factors that have been proposed to influence these mixed results include the type of condition being treated, patient expectancy, the acupuncture points chosen, the type of placebo intervention, and the heterogeneity of treatment protocols across studies.14-16 However, mechanistic studies have shown that by examining neurophysiology, it is possible to distinguish between TA and SA,17-19 albeit neuroimaging has failed to produce a consistent pattern of activation of either TA or SA. However, alpha (~8-12 Hz), has been shown to be involved in TA conditions. Specifically, in healthy humans, EEG power significantly increases in the alpha band under TA and alpha power can remain high after TA.20,21
It is known that brain function can vary across cultures, resulting from differing influences of the environment, belief systems, and allocation of attention, to name a few. Indeed, neuroimaging studies have also shown differences in the manner in which culture influences interpretation of social constructs related to brain function, and specifically between Eastern and Western cultures,22-24 as well as in biological differences in resting state activity.25,26 Therefore, 1 explanation for differences in acupuncture efficacy between trials could be that culture determines responsiveness to acupuncture.
A key aspect of acupuncture, and certainly of placebo, is the expectation of the outcome of treatment, which may also vary between cultures. For example, a study conducted in China found that patients who used traditional Chinese medicine (TCM) for conditions other than current back pain were 8 times more likely to have tried it again for their current pain than those who were not familiar with TCM, and that patients whose families used TCM were 3.5 times more likely to use TCM themselves, representing a cultural and familial belief in the efficacy of TCM and specifically of acupuncture. 27 Previous research has also demonstrated activation of different brain regions in response to social and non-social tasks when comparing East Asian and Western cultures, demonstrating mediation by distinct neural networks. 28 For example, East Asian cultures are associated with increased neural activity in the brain regions related to inference of others’ mind and emotion regulation whereas Western cultures are associated with enhanced neural activity in the brain areas related to self-relevance encoding and emotional responses during social cognitive/affective processes. 28 Others have also found that cultural background moderates activation in brain networks engaged during even simple visual and attentional tasks. 29
Although there are potentially both specific and non-specific effects of TA, until we can separate these components acupuncture will likely be dismissed from a scientific standpoint and as a standard of care treatment. Therefore, we explored potential mechanisms for the beneficial effects of acupuncture for xerostomia by using electroencephalographic (EEG) neuroimaging to examine the effects of a single session, blinded, cross-over design, trial of TA and SA with patients at Fudan Cancer Hospital in Shanghai, China and at MD Anderson Cancer Center in Houston, Texas, United States.
Methods
Participants were identified by faculty in the Department of Radiation Oncology at both institutions and referred to study personnel for assessment of eligibility. Thirteen patients from MDA and 14 patients from Fudan undergoing radiation for head and neck cancer were recruited at each site, between 3 and 5 weeks into radiotherapy. All participants signed an informed consent. This trial was approved by the Institutional Review Boards of The University of Texas MD Anderson Cancer Center (11 September 2014; #2013-0769) and Fudan University Shanghai Cancer Center.
Patients
Eligible patients were recruited from either Fudan University Cancer Center or MD Anderson Cancer Center. Patients undergoing radiotherapy for head and neck cancer are treated on an inpatient basis at Fudan and on an outpatient basis at MD Anderson.
Inclusion criteria were as follows: adult ≥18 years of age and able to give informed consent; diagnosed with oropharyngeal (MD Anderson) or nasopharyngeal head and neck squamous cell carcinoma (Fudan); planned intensity-modulated radiation therapy (IMRT), with or without concurrent chemotherapy, at a mean dose of at least 24 Gy to at least one of the parotid glands (the other gland could receive any dose level); anatomically intact parotid and submandibular glands; and Karnofsky performance status >60. Exclusion criteria were a history of xerostomia prior to head and neck radiation therapy, Sjögren’s disease, or another underlying systemic illness known to cause xerostomia; prior head and neck radiation treatment; suspected or confirmed physical closure of salivary gland ducts on either side; known bleeding disorders or taking any dose of warfarin or heparin; upper or lower extremity deformities that could interfere with accurate acupoint location or alter the energy pathway as defined by traditional acupuncture theory; local skin infections at or near the acupuncture sites or active systemic infection; history of cerebrovascular accident or spinal cord injury; mental incapacitation or significant emotional or psychiatric disorder that, in the opinion of the investigator, may prevent the patient from cooperating with the slightly invasive procedures or the data collection process; current use of any illicit drugs or evidence of alcohol abuse as defined by The American Psychiatric Association; or current use of alternative medicines, such as herbal (TCM) preparations, that could affect salivary function. Participants taking amifostine, cholinergic agonist medications (pilocarpine, cevimeline), certain beta-adrenergic antagonists, anticholinergic agents, or other medications known to affect salivary function were also excluded. Finally, patients were excluded if they were currently receiving acupuncture for any condition or if they had had any prior acupuncture treatment.
Procedures
Patients were randomized using simple randomization based on a random number table, in a counter balanced design, to either the true or sham acupuncture first then followed 2 to 7 days later by the other treatment. Patients were told that the purpose of the study was to test 2 different acupuncture approaches. This wording was used to avoid deception while maintaining naiveté as to the existence of a sham group. Each patient either randomly received 1 session of either TA or SA first, followed 2 days later by the other treatment in a counter balanced manner. EEG data was collected with eyes closed for 5 minutes before needle insertion, throughout the time the needles remained in place, and then for 5 minutes after removal of the needles. Staff recording EEG parameters were blinded to group assignment.
Acupuncture Treatment
Treatments were given by a qualified, hospital-credentialed acupuncturists with at least 10 years’ experience. Quality control was maintained by having members of the study team (including acupuncturists) from MD Anderson visit Fudan, and vice versa. Patients were treated in a comfortable supine or semi-supine position on the day of XRT, either before or after XRT. Upon insertion, needles were manipulated until deqi was elicited at the appropriate points. They were not manipulated further during the needle retention period. The specific acupuncture points and needling methods used are reported in detail elsewhere. 7 The sham procedure in this trial involved a real needle at a real point not indicated for xerostomia (GB32), real needles at sham points (helix of the ear), and sham needles at sham points. The mixture of real and sham points and needles utilized is defined as acupuncture. The Park system (a validated, non-penetrating, telescoping needle with a separate device that attaches it to the skin) was used for the sham needles.30,31
EEG Analyses
To simplify analyses, acupuncture in both the TA and SA conditions was examined. We contrasted post versus baseline for each condition then contrasted those results using a SA versus TA design. As all 14 patients had both TA and SA, we compared EEG differences between each condition across all patients and between sites.
The LORETA method of EEG analysis allows the localization of electric activity in the brain based on scalp potentials from a multiple channel EEG and is capable of determining the relative activity of regions in the brain using surface electrodes. 32 LORETA estimates the distribution of neuronal activity in three-dimensional space utilizing information acquired from a grid of electrodes placed on the scalp. While traditional EEG information is limited to activity measured on the scalp, intracranial activity can be inferred from the use of inverse solution techniques. 33 LORETA has been validated from studies that combine LORETA with other established localization methods such as fMRI, structural MRI, positron emission tomography, diffusion spectral imaging, and localization findings from invasive, implanted depth electrodes.34-40 Regions of interest (ROIs) are defined based on previous neuroimaging research separately on acupuncture, autonomic nervous system function,41-46 and our pilot data.
To determine brain activity profiles between TA and SA conditions and between Fudan and MD Anderson, we conducted 3 separate analyses by site using LORETA current source density (CSD) as the analysis tool which allowed us to infer subcortical changes from data collected cortically. First, by combining Fudan and MD Anderson TA and SA groups (MD Anderson TA + Fudan TA; MD Anderson SA + Fudan SA) we examined maximal differences in TA and SA contrasted with baseline for each bandwidth in the EEG. Second, we determined CSD within several predetermined regions of interest that are known to be active during acupuncture separately for Fudan and MD Anderson, specifically Brodmann areas 3, 6, 11, 13, and 33. Third, we contrasted the SA conditions by site (Fudan and MD Anderson) and examined whole brain power differences for both sites.
For each subject, power means within the frequency bands were summed across all electrode sites in both absolute and relative power. Within-group differences were examined using paired sample t-tests. Between-group differences were examined using univariate ANOVA with the condition as the fixed variable, and changes of EEG scores from baseline to post-treatment as the dependent variable. Our primary comparisons focused on true versus sham acupuncture and then between sites (Fudan and MD Anderson).
Results
Thirteen patients with oropharyngeal cancer undergoing radiotherapy at MD Anderson and 14 patients with nasopharyngeal cancer undergoing radiotherapy at Fudan were approached to participate. One of the patients at MD Anderson declined and all 14 at Fudan agreed to participate. Thirteen patients at MD Anderson and 14 patients at Fudan provided 2 EEGs. Both sites had a majority of men (MD Anderson—9 of 13; Fudan 10 of 14) with the participants at Fudan tending to be younger, receiving a higher cumulative dose of radiotherapy (P < .001) and had more advanced disease (P = .02) (see Table 1). There were no significant site differences in age or sex (P’s > .05). EEG data was collected from the participants after at least 3 weeks of radiotherapy and no more than 5 weeks. Each treatment (TA and SA) was delivered in a counterbalanced manner with 2 days between treatment.
Demographics and Baseline Features.

Abbreviation: gy, Gray; absorbed energy per unit of mass tissue.
Combining the Fudan and MD Anderson Sites: Overall Brain Analysis in TA Condition Relative to SA Condition According to Bandwidth
Delta: Maximal power differences between conditions were found where TA showed increased activity in the inferior frontal gyrus (Brodmann area 47), parahippocampal gyrus (BA 37), middle frontal gyrus (BA 9), superior frontal gyrus (BA 9 and 10), and middle frontal gyrus (BA 10 and 47) relative to SA. Maximal decreases in activity were found in the inferior parietal lobule (BA 40), inferior temporal gyrus (BA 37), postcentral gyrus (BA 2 and 1), precuneus (BA 7), superior parietal lobule (BA 7), and postcentral gyrus (BA 5).
Theta: Maximal increases of theta activity were found in the inferior frontal gyrus (BA 47), superior frontal gyrus (BA 10), superior temporal (BA 29), and parahippocampal gyrus (hippocampus). Maximal decreases were found in the postcentral gyrus (BA 3), superior parietal lobule (BA 7), inferior parietal lobule (BA 40), inferior frontal gyrus (BA 7), middle frontal gyrus (BA 11), and middle temporal gyrus (BA 21).
Alpha: Maximal increases in activity were found in the fusiform gyrus (BA 20); paracentral lobule (BA 5); postcentral gyrus (BA 5 and 3), paracentral lobule (BA 5), supramarginal gyrus (BA 40), superior frontal gyrus (BA 9), insula (BA 13), and precentral gyrus (BA 4). Decreases were found in the inferior frontal gyrus (BA 47), extra nuclear (BA 47), insula (BA 13), middle temporal gyrus (BA 39), and angular gyrus (BA 39).
Beta1: Maximal increases in activity were found in the middle temporal gyrus (BA 39) and inferior parietal lobule (BA 40), while decreases were found in the parahippocampal gyrus: (BA 37), anterior cingulate (BA 24), subcallosal gyrus (BA 34), and superior frontal gyrus (BA 6).
Beta2: Maximal increases in activity were found in the precuneus (BA 19), inferior parietal lobule (BA 40), and postcentral gyrus (BA 5). Decreases were found in the superior frontal gyrus (BA 11 and 10), subcallosal gyrus (BA 34), superior frontal gyrus (BA 9), and middle frontal gyrus (BA 8).
To summarize findings from our first analyses, results indicated a differential effect between real TA and SA, contrasted with baseline, where the most consistently active frequencies across locations were the delta and alpha frequency bands with group differences based on BA location.
CSD in Predetermined ROIs for Fudan and MD Anderson (Contrasting TA and SA With Baseline)
We conducted further analyses in specified regions of interest that have been shown to be active in other acupuncture studies as well as regions that may correlate with perception of saliva production. Results showed that for both Fudan and MD Anderson, CSD decreased in the TA versus the SA conditions in all of the regions analyzed with the exception of BA 11 (Figure 1), consistent with previous studies showing decreased activity in TA versus SA. 47
CSD changes in Fudan and MD Anderson.
Despite the commonalities in brain regions deactivated during TA and activated during SA, there were minimal statistically significant differences between the conditions in the MD Anderson cohort, with larger differences noted for the Fudan patients (Figure 1). The only statistically significant power difference at MD Anderson was an increase in activity in the middle frontal gyrus when TA (P = .11) was compared to SA in delta (P = .01). In contrast, at Fudan TA versus SA demonstrated a statistically significant power difference at multiple locations between the 2 conditions (P’s ≤ .05).
Comparing Sham Groups Between Fudan and MDA
In the MD Anderson relative to the Fudan cohort, maximal activity after SA was seen in the lingual gyrus (BA 18), cuneus (BA 17), and fusiform gyrus (BA 18), which are thought to be associated with the perception of phenomenon rather than the physical results of an activity. The Fudan cohort demonstrated maximal activity in response to SA in areas that we saw in our first analysis that were associated with TA such as BA 3, 4, 5, and 40, insula, coupled with a decrease in activity in areas thought to be associated with perception such as BA 20.
We further hypothesized that these differences in brain activity to SA are culturally driven. To explore potential cultural differences in brain activity, we determined CSD in Brodmann areas that have been identified as being influenced by culture.28,29 Although not conclusive, when comparing the 2 Fudan and MD Anderson in terms of overall brain activity in response to SA, the Fudan cohort had greater CSD activity than the MD Anderson cohort in BAs 3, 4, 6, 7, 9, 24, 32, and 40.
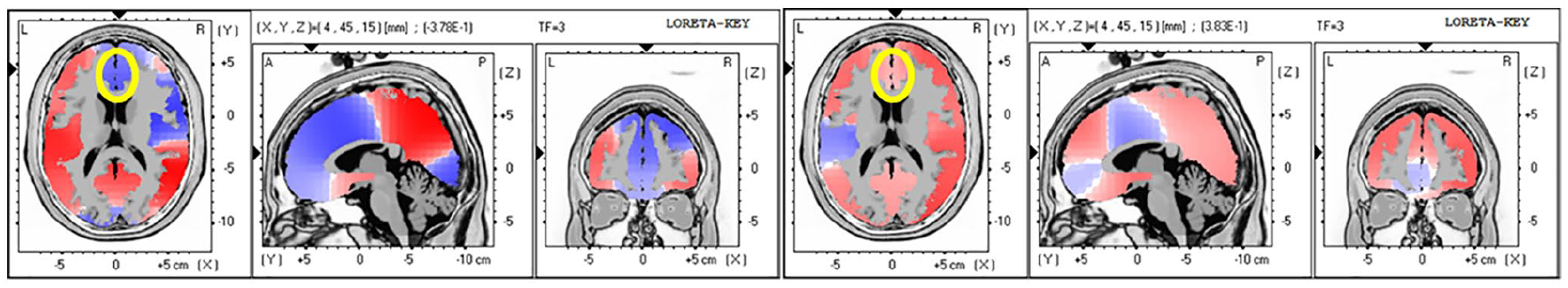
Guided by our first 3 analyses, we were aware that most differences in amplitude between TA and SA were in the frontal regions and the strongest effect was in alpha. As an unplanned analysis, we combined frontal areas (F1, F2, F3, F4, FZ) and found a statistically significant difference in alpha amplitude in the TA minus baseline versus the SA minus baseline conditions, meaning there is greater alpha amplitude in the SA condition (P = .003). Likewise, there was a statistically significant difference in frontal alpha amplitude 5 minutes after SA versus 5 minutes after TA in the frontal regions, (P = .003), where SA shows greater amplitude of alpha activity (Figure 2). Analysis of frontal alpha power showed a non-significant difference (t = .67, P = .51) between the SA and the TA conditions. We found a decrease in beta activity in the anterior cingulate in the acupuncture TA condition only.

True acupuncture indicated a decrease in alpha activity in the cingulate, controlling for baseline (left). Sham acupuncture indicated an increase in alpha activity in the cingulate (right) alpha.
Discussion
Overall, our results indicate a differential effect between TA and SA. In both institutions, for the acupuncture minus sham condition the most active bandwidths overall were the delta and alpha bandwidths. The largest magnitude of change was found in the frontal regions in delta and parietal regions in alpha. We also found an increase in CSD in regions of interest in the current study that were common to other studies 46 of acupuncture and salivary production using fMRI, specifically the inferior frontal gyrus, middle frontal gyrus, insula, and postcentral gyrus.
There were some commonalities to both sites (MD Anderson and Fudan) such that alpha activity decreased in the cingulate in the TA condition and increased in the SA condition. The most “active” frequencies, or those that demonstrated the greatest magnitude of change after TA in Fudan and MD Anderson patients were the delta (0.5-3 Hz) and alpha (8-12 Hz) bandwidths, a finding demonstrated in other research. 48 These results mimic findings from other studies of acupuncture and the brain, specifically that the alpha frequency is one of the most active frequencies and that the cingulate is activated during acupuncture.47,48 We also found a decrease in beta activity in the anterior cingulate in the TA condition only.
As with most of our analyses in this study, we did not see statistical significance between cohorts. However, our data are valuable to guide subsequent analyses and the fact that there was a reduction in activity, consistent with the notion that the degree of disorder of the brain could be brought down during TA. 49 At MD Anderson, there were minimal power differences among brain areas examined in this study, however the power differences between TA and SA at Fudan demonstrated a power difference in multiple locations. This may help explain why in the large, multi-center trial there were no group differences at MD Anderson between SA and TA in self-report salivary outcomes (xerostomia questionnaire, XQ), yet there were XQ differences between SA and TA at Fudan. 7
To better understand the findings from the large, multi-center trial where the Fudan cohort showed no XQ differences between the SA and SCC group, we sought to determine what may be different about the perception of acupuncture across cultures by comparing data from the Fudan SA condition to that of the MD Anderson SA condition. In the MD Anderson cohort relative to the Fudan cohort, maximal activity was seen in the lingual gyrus (BA 18), cuneus (BA 17), and fusiform gyrus (BA 18) which are thought to be associated with the perception of phenomenon rather than the physical results of an activity. During the SA condition, the MD Anderson brains looked as if they were under the “real acupuncture” condition with maximal activity in areas associated with acupuncture such as BA 3, 4, 5, and 40, insula, coupled with a decrease in activity in areas thought to be associated with perception such as BA 20. Further, BA 20 is a component of the default mode network, and in acupuncture conditions has been shown to decrease in activation, reiterating that Fudan participant brains were processing the SA condition as if it were TA. Although this may seem contradictory, results suggest that although the brain is processing SA as TA, the SA condition did not increase activity in areas associated with perception. We propose, therefore, that TA may have a “true” effect in salivary production when brain regions associated with perception and saliva production are congruent, irrespective of conscious beliefs. In other words, the ingrained belief system about effects of acupuncture (or any other intervention) could be culturally driven and in part, depend upon brain activity that was developed as a part of involvement in society. However, it is important to note that in the large, multi-center trial there were no differences between MD Anderson and Fudan participants in expectations at baseline or for the TA and SA conditions after 4 acupuncture sessions and at the end of treatment.
Research has shown that cultural background moderates the activation of brain networks engaged during even simple tasks. 29 In the current study, brain activity in areas that have been identified as being influenced by culture showed increased activity in the Fudan participants compared to the MD Anderson participants during SA. Results showed that in predetermined regions of interest, brain activity between SA and TA conditions was minimally different in the MD Anderson participants, with larger differences noted in the Fudan participants. 50 In all areas analyzed (BAs 3, 4, 9, 24, 32) the Fudan cohort had greater activity in these regions than the MD Anderson cohort. These findings are consistent with prior research examining cultural differences in brain region activation during different tasks where they found that for non-social tasks and for social affective tasks East Asian brains have increased activity compared to Western brains (non-social tasks: BAs 40 and 7; social affective tasks: BA6). This potentially demonstrates a much more “active” brain in the Fudan cohort, and, further, that activity in the cingulate may be indicative of the expectation that acupuncture would be effective. This may start to explain why there was little difference in XQ scores at MD Anderson between TA and SA compared to these groups at Fudan. We suggest that in Fudan patients, the brain was processing sham in part as “real acupuncture”; the sham condition did not increase activity in areas associated with perception which may be necessary to modify outcomes on a symptom report like xerostomia. We propose, therefore, that acupuncture will not have a “true” effect in perception of salivary production unless areas of perception and saliva production reach a certain magnitude of activation. However, there was also reduction in overall activity during the acupuncture condition, consistent with the notion that the degree of disorder of the brain may be decreased during acupuncture.
There are a number of limitations with the current study. The sample size was small and the stability of the findings could be improved with a larger sample size. However, a sample size of 13 to 14 per group, especially with a cross-over, between and within group comparison is typical of neuroimaging studies. Moreover, the cross-over design may have resulted with a residual effect from the prior treatment. However, after 2 days it is unlikely that residual neurological effects would still exist and the counterbalanced design would help to remove any order biases. The study also only examined the effects after 1 treatment. Based on the concept of neuroplasticity through learning, we hypothesize that more sessions of acupuncture will result in an initial increase in the effects highlighted above, although there could be a plateau effect where acupuncture reaches its maximum neuroplastic effect after an undetermined number of sessions.51,52 However, although greater and more permanent neurological changes may be apparent after more treatments, most mechanism-based acupuncture research uses a single session to explore brain changes and this allows for examination of within participant changes. In addition, the sham procedure used 3 different sham approaches (sham needle at sham point, real needles inserted at sham points, and a real needle inserted at a real point), making it difficult to interpret the findings from a pure placebo perspective. However, the sham procedures were identical at each site and finding between group and cultural differences becomes more intriguing as both the sham and real groups had real needles inserted. The study also did not report on subjective symptoms, as changes after 1 acupuncture would be negligible. Finally, there were some uncontrollable differences between the demographic and medical characteristics between the 2 sites such as dose of radiotherapy, stage, and cancer type. A future, larger trial could use a more homogenous sample and explore longer term effects of TA and SA on neurological outcomes.
Further research is needed to improve the accuracy of regions of interest that are activated during acupuncture as well as to analyze coherence and other measures that could be indicative of acupuncture’s mechanism in prevention of xerostomia. Implications of the belief system of the culture a person belongs to could be instructive as to how to discuss acupuncture treatment and efficacy. It is accepted that elaborating on an effect of an intervention will increase the efficacy of that intervention via participant expectation. In order to improve clinical outcomes, as well as emphasize differences in research between TA and SA, we suggest that future studies augment the education of participants about acupuncture in an effort to enhance the effects of acupuncture.
Footnotes
Acknowledgements
We thank Drs. Peiying Yang and Zongxing Liao for their support with language, culture, and politics and Wenying Bei and Caijun Wu for help with data collection.
Data Access
Access to the data will be provided upon request with documentation of appropriate approvals from IRB for data sharing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Support was provided in part by United States National Cancer Institute (NCI) grants CA148707 (PI: L Cohen) and the NCI Cancer Center Support Grant CA016672. Partial funding provided by the Richard E. Haynes Distinguished Professorship for Clinical Cancer Prevention at The University of Texas MD Anderson Cancer Center (L Cohen). Financial support agencies for this project had no role in the design or interpretation of the data. Partial funding was provided by the National Center for Complementary and Integrative Health (1K01AT008485-01; PI: S Prinsloo), the Rising Tide Foundation (S Prinsloo) and The American Cancer Society (S Prinsloo).
