Abstract
Keywords
Introduction
Cancer is among the leading causes of death worldwide. There are numerous therapies for cancer at present, but only surgical resection, chemotherapy, and radiotherapy have demonstrated confirmed effectiveness. Still, there are limitations to surgical excision, and the uses of chemotherapy and radiotherapy are limited for individuals with serious adverse events. Cancer chemotherapy destroys normal cells, leading to anemia, bleeding, infection, gastrointestinal symptoms, and long-term risks associated with secondary malignant lesions. Being unable to selectively eradicate all remaining tumor cells is a major disadvantage of the use of the conventional therapy. A more effective treatment strategy must be developed for cancer-specific treatment.
Cancer immunotherapy has played an important role in cancer therapy. There is an inherent defense system called the “cancer immunity cycle,” which causes apoptosis in tumor cells. 1 Specifically, the so-called “immune checkpoints” are important targets, as they suppress the body’s immune response to cancer cells. Programmed cell death-1 (PD-1, CD279), which is a surface protein of activated T cells, and PD-L1 (programmed death-ligand 1; B7-H1, CD274) and PD-L2 (B7-DC, CD273), which are ligands of PD-1, are found on the surface of antigen-presenting cells and most cancer cells. 2 PD-L1 strongly emerges on the cell surface of untransformed cells present in tumors or in the tumor microenvironment. 3 When PD-L1 binds to PD-1, the production of cytokines from T cells decreases, and the activity of T cells is inhibited. Tumor cells use this checkpoint signal transduction of immunity to escape recognition from T cells and to obtain immunological unresponsiveness. 3
MK615 is an extract from the Japanese apricot (
Thus, MK615 was shown to have strong anticancer, antiproliferative, and anti-inflammatory effects by recent in vitro investigations. Various relevant clinical experimental reports have been published,20,25 but in vivo evidence from mouse research is scarce. Herein we investigated the in vivo antitumor effects of MK615 and examined the underlying mechanism by focusing on the downregulation of PD-L1.
Materials and Methods
MK615 Preparation
MK615 was kindly provided by AdaBio Co (Takasaki, Gunma, Japan). The MK615 was derived from the pressure extraction of apricot fruit juice from which squeezed residue was removed. The juice was then heated and concentrated. Before use, the concentrate was dissolved in water, and the pH was adjusted to 7.0 with NaOH. The final step was the sterilization of the solution in an autoclave.
Cell Line and Culture
The cell line B16/BL6 (mouse melanoma) was provided by Riken BRC (Tsukuba, Japan) through the National Bio-Resource Project of the Ministry of Education, Culture, Sports, Science and Technology (MEXT), Japan. B16/BL6 melanoma cells are a murine cell line that can induce lung metastasis by injection into the tail vein.26,27 The B16/BL6 cells were cultured in RPMI-1640 medium supplemented with 10% fetal bovine serum and incubated at 37°C in a humidified 5% CO2 atmosphere. Three days after the cells were plated, tumor cells were harvested and injected into mice via the lateral tail vein.
Laboratory Animals
Male C57BL/6JJcl mice and male BALB/c-nu/nu mice were obtained from CLEA Japan (Hamamatsu, Japan) at 8 weeks after birth. Their weight was approximately 20 g. The mice were maintained for 1 week in our animal facility before the tumor cell injection. They were housed in plastic cages with sawdust bedding and were given standard pellet diet and water ad libitum. The room was kept controlled at 23°C, humidity 10%, and a 14-hour light/10-hour dark cycle. The animal research was approved by the Tokyo Women’s Medical University of Animal Care and Use Committee (Approval Nos. 14-143, 15-20, AE16-25, and AE17-114).
Experimental Procedures for the Lung Metastasis Murine Model of B16/BL6 Melanoma Xenografts
Thirty-two C57BL/6 mice (body weights = 22-24 g) were prepared: 20 C57BL/6 mice were used for the survival observation experiment, and 12 C57BL/6 mice were used for the lung observation experiment. B16/BL6 melanoma cells (2.5 × 103 cells) were injected into the lateral tail vein of each mouse after being cultured in 10-cm dishes for 3 days. The C57BL/6 mice of the MK615-treated group were orally administered MK615 at 10 µL/g (body weight) every other day after the tumor injection. The control group mice were given the same volume of saline. The oral administration was provided using a disposable oral sonde (Fuchigami, Kyoto, Japan).
Twenty-eight days after the tumor cell injection, 12 C57BL/6 mice (MK615-treated group: n = 6, control group: n = 6) were sacrificed by exposure to isoflurane in oxygen until their breathing stopped; the lungs were then harvested for the analyses described below. In the survival studies, 20 C57BL/6 mice (MK615-treated group: n = 10, control group: n = 10) were observed for 8 weeks after the tumor cell injection. For immunodeficient mice, 12 BALB/c-nu/nu mice (body weight = 27-29 g) were prepared and divided into 2 groups, in the same manner as the grouping of C57BL/6 mice.
Immunofluorescence Analysis of the Lung Tissues
The lung tissue samples from B16/BL6 melanoma-injected mice were fixed with 4% paraformaldehyde for 1 hour at room temperature and then embedded in paraffin. The paraffin-embedded samples were sectioned into 6-µm-thick slices, and the sections were mounted on slide glasses. Deparaffinized specimens were incubated with 1% bovine serum albumin in phosphate-buffered saline containing 0.1% Triton X-100.
After being washed with Tris-buffered saline (TBST, Tris-buffered saline containing 0.02% Tween 20), the specimens were incubated with a mouse anti-melanoma antibody (HMB45 + M2-7C10 + M2-9E3, Cat. No. ab732, Abcam, Cambridge, UK; 1:40 dilution) and a rabbit anti-NF-κB (p65) antibody (Abcam; Cat. No. ab7970, 1:50 dilution) or anti-PD-L1 antibody (Abcam; Cat. No. ab205921, 1:200 dilution) at 4°C overnight. After being washed with TBST, the specimens were incubated with Alexa Fluor 488-conjugated goat antirabbit IgG (rabbit Ig horseradish peroxidase-linked Whole Ab, from Donkey; Cat. No. NA934, GE Healthcare Japan, Tokyo, Japan; 1:4000 dilution) for 1 hour at room temperature. After another wash with TBST, the specimens were stained with 40,6-diamidino-2-phenylindole dihydrochloride n-hydrate (DAPI; P36935, Thermo Fisher Scientific, Yokohama, Japan) and then immediately observed for intracellular localization with a fluorescence microscope (model AX80, Olympus, Tokyo, Japan).
Western Blotting
Anti-PD-L1 antibody (#ab205921) and anti-NF-κB antibody (#ab7970) were purchased from Abcam. First, we used a scalpel blade to harvest tissue samples (2-3 mm2) from a lung metastatic colony of colored melanoma. The cells obtained from the lungs were disintegrated by an ultrasonic vibration. The cells were then lysed with 200 µL of RIPA buffer (Thermo Fisher Scientific, Waltham, MA) and concentrated at 10 000 g for 5 minutes. The supernatant was adjusted to include proteins of equal quantity using a Pierce BCA protein assay kit (#23225). Each 20-µg protein sample was run on 4% to 12% Bis-Tris Protein Gel (NuPAGE Novex, NP0321BOX, Thermo Fisher Scientific), and the separated proteins were transferred to a nitrocellulose membrane (IB301001, Thermo Fisher Scientific) using iBlot (Thermo Fisher Scientific).
The membrane was blocked with 50 g/L nonfat dry milk powder in 0.1% TBST for 1 hour at room temperature. The membrane was then incubated with a primary antibody in TBST containing 5% nonfat dry milk overnight at 4°C. After extensive washing, the membrane was then incubated with horseradish peroxidase–conjugated anti-rabbit IgG polyclonal antibody (NA934; GE Healthcare Biosciences, Piscataway, NJ; dilution 1:2000) in TBST containing 5% nonfat dry milk for 1 hour at room temperature. The membrane was washed again, and immunoreactive bands were visualized using an enhanced chemiluminescence detection system (RPN2232, Amersham ECL Prime Western Blotting, GE Healthcare Biosciences). The bands were quantitatively analyzed using ImageJ software. 28
Flow Cytometry
PE rat anti-mouse CD274, which is also known as (PD-L1, was purchased from BD Pharmingen (San Diego, CA). B16/BL6 melanoma cells (1 × 106) were cultured in 10-cm dishes. After 24-hour cultivation, MK615 was mixed with each dish at one of several concentrations (0, 1, 3, 5, 10, 15, and 20 µg/mL). Forty-eight hours later, cells were harvested and blocked with Normal Rat Serum (Jackson Immuno Research Laboratories, West Grove, PA). After being stained with control or anti-PD-L1 antibody for 1 hour, the cells were washed twice with phosphate-buffered saline and then analyzed by a Gallios flow cytometer (Beckman Coulter, Indianapolis, IN).
Statistics
The survival of each group of mice is represented as Kaplan-Meier survival curves and were analyzed by the Wilcoxon test. Differences in the weight of the mouse bodies or lungs were analyzed by Student’s
Results
Macroscopic Observation of Lungs
The greater part of the surfaces of the lungs from the control group mice showed a dark reddish-brown color due to melanoma metastasis. By contrast, the greater part of the surfaces of the lungs from the mice treated with MK615 showed small nodules (Figure 1). After they were sacrificed, the mice were dissected and observed carefully. In addition to the lungs, we examined the skin, heart, liver, kidney, intestinal tract, and so on, but metastasis to organs other than lung was not observed. The average lung weight of the MK615-treated mice (0.37 ± 0.12 g) was significantly less than that of the control mice (0.77 ± 0.19 g;

Inhibition of metastasis to lung by the interference of MK615 in B16/BL6 mice. Twenty mice were randomly divided into 2 groups. Photographs of lungs harvested from a control mouse and MK615-treated mouse.
Immunofluorescence Assay of Lung Metastatic Tumor Sites
The expression levels of NF-κB and PD-L1 in lung metastatic tumor sites were determined by an immunofluorescence assay. Tumor cells were labeled with antimelanoma antibody and DAPI (Figure 2A and B). The fluorescence of both NF-κB (Figure 2A) and PD-L1 (Figure 2B) in the tumor cells from MK615-treated C57BL/6 mice was decreased compared with that of the control mice.

Immunofluorescence analysis of lungs harvested from MK615-treated and control mice. (A) The fluorescence of NF-κB was diminished on the tumor site labeled with the antimelanoma antibody and DAPI. (B) The fluorescence of PD-L1 was diminished on the tumor site labeled with the antimelanoma antibody and DAPI (original magnification, ×400).
Western Blotting Analysis
Cell lysates from lungs of C57BL/6 mice were analyzed by Western blotting using anti-NF-κB antibody. Anti-β-actin antibody was used as a loading control. The results of the Western blotting analysis indicated that the expression of NF-κB was decreased in the lungs of the MK615-treated mice (Figure 3A) compared with that of control mice. The bands of NF-κB were quantitatively analyzed with ImageJ (Figure 3B). The expression ratio represents the change in the ratio relative to β-actin compared with the untreated control group. The data are presented as the mean ± SD of a triplet assay.
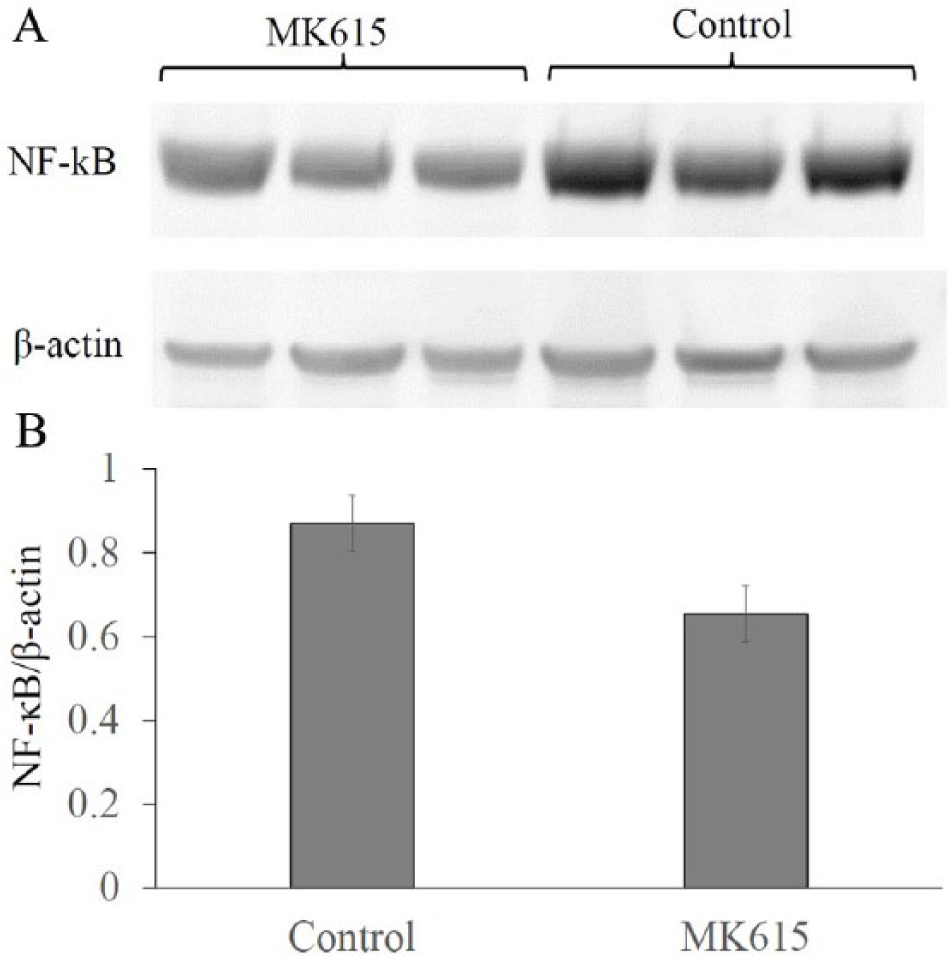
(A) Western blotting assay of NF-κB. NF-κB expression was diminished on the lungs harvested from MK615-treated C57BL/6 mice. (B) The quantitative analysis of the band of NF-κB revealed 0.65 ± 0.08 in the control group versus 0.87 ± 0.07 in the MK615 group. NF-κB/β-actin tended to be lower in the MK615 group.
Survival Observation of C57BL/6 Mice After Tumor Injection
In the survival experiment, we randomly divided 20 C57BL/6 mice into an MK615-treated group and a control group. After the injection of B16/BL6, no complications such as esophageal rupture or aspiration by vomiting, were found. The MK615-treated mice survived significantly longer (

(A) Kaplan-Meier survival curves of the mice after tumor injection. The survival of mice treated with MK615 (red line; n = 10) was significantly longer than that of the control mice (blue line; n = 10;
The Effect of MK615 in the Immunodeficient Mice
We performed a similar experiment using the BALB/c-nu/nu mice to assess the immunological effect of MK615 in vivo. The survival curves of the control group and MK615-treated group showed no significant difference (Figure 5A). There was no significant difference in the body weights of the 2 groups (Figure 5B). Lung metastases were observed in both groups (Figure 5C). The results of the Western blotting showed that MK615 inhibited the expressions of NF-κB (Figure 5D) and PD-L1 (Figure 5E). The bands of NF-κB and PD-L1 were quantitatively analyzed, revealing that the expressions of both NF-κB/β-actin and PD-L1/β-actin were suppressed compared with the control (Figure 5F and G). These results indicated that MK615 loses its effectiveness when the immune system becomes compromised.

(A) Kaplan-Meier survival curves of the mice after tumor injection. The survival of the BALB/c-nu/nu mice treated with MK615 (red line; n = 6) was not longer that of the control mice (blue line; n = 6). (B): The weights of the mice after tumor injection. There was no significant difference between the weights of the MK615-treated BALB/c-nu/nu mice and control mice. (C) A photograph of lungs harvested from an MK615-treated BAL/c mouse and a control mouse. Lung metastases were found on both lungs in each group. (D) Cell lysates were obtained from the lungs of the mice, and the expression of NF-κB was evaluated by a Western blotting assay. The NF-βB expression was diminished on the lungs harvested from MK615-treated BALB/c-nu/nu mice. (E) Cell lysates were obtained from the lungs of mice, and their PD-L1 expression was evaluated by a Western blotting assay. (F, G) The PD-L1 expression was diminished on the lung harvested from MK615-treated BALB/c-nu/nu mouse.
Flow Cytometry of PD-L1 on B16/BL6 Tumor Cells With MK615 In Vitro Culture
We investigated the effect of MK615 on the expression of PD-L1 on the cell surface of B16/BL6 melanoma cells by flow cytometry in vitro. B16/B6 cells were incubated with different concentrations of MK615 in vitro. The expression levels of PD-L1 were 96.5%, 97.0%, 97.1%, 94.6%, 75.4%, 64.9, and 60.5% at MK615 concentrations of 0, 1, 3, 5, 10, 15, and 20 µg/mL, respectively (Figure 6A and B). These results demonstrated that MK615 inhibits the expression of PD-L1 in a concentration-dependent manner.
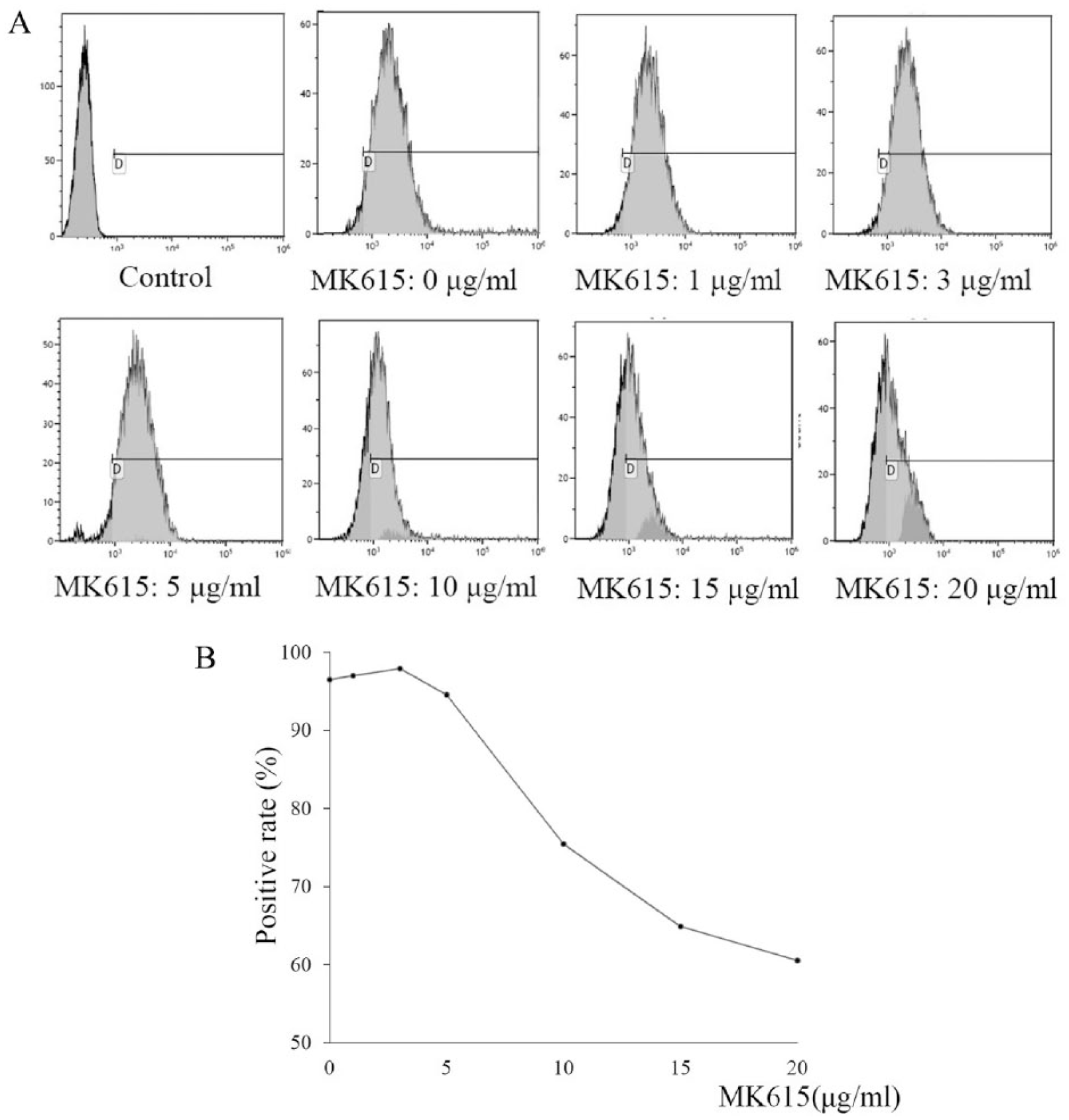
(A) Expressions of PD-L1 on B16/BL6 cells cultured with different concentrations of MK615, measured by flow cytometry. (B) The PD-L1 expression of cultured cells was decreased in an MK615-dose-dependent manner.
Discussion
The Japanese apricot is well known as a traditional healthy food in Japan. Some mechanisms of the components of Japanese apricots have been reported; in particular, triterpenoids are thought to play an important role in health. As a compound extracted from the Japanese apricot, MK615 is prevalent in Japan as a health supplement. Its anti-inflammatory effect has long been known, and some antitumor effects were recently reported.
Several mechanisms are thought to be involved in MK615’s inhibition of tumor growth. It was reported that the hydrophobic fractionation of MK615 inhibits cell proliferation, increases the G2-M period of the cell cycle, and decreases the G0-G1 phase; this suggests the induction of G2-M arrest. Another report demonstrated that the hydrophobic fraction of MK615 induced G2-M arrest, and it inhibited the activities of aurora kinase A and aurora kinase B. The induction of G2-M arrest was observed with an esophageal squamous cell carcinoma cell line, and the induction of G0-G1 arrest was observed with a non–small cell lung cancer cell line.
As noted above, MK615 has shown different effects on the cell cycle, namely, the induction of either G0/G1 arrest or G2-M arrest, but these are not opposed to each other, and the differences may be caused by patterns in cell proliferation. While it is certain that MK615 is associated with the expression of proteins associated with the cell cycle, the details require further examination. MK615 restrains cell proliferation, and it has an antitumor effect that is important to the induction of cell death.
Regarding the induction of cell death by MK615, the apoptosis of cancer cells and the induction of cell death with autophagy have been reported.29,30 The expression of Id-1, an inhibitor of DNA binding, is also reported to be inhibited by MK615. The Id family is associated with regulatory functions involved in cell proliferation and cell differentiation; strong Id-family expression occurs in conjunction with both undifferentiated cells and cancer cells. The presence of Id-1 causes an overexpression of the melanoma cell line, and an association between the Id-1 level and the cancer grade has been reported. It was also reported that a decrease in the Id-1 expression by MK615 is associated with a decrease of Bcl-2 expression.
In addition, antitumor and anti-inflammatory effects have been shown by triterpenoids including ursolic acid, which is one of the ingredients of MK615.8,9,31 It was reported that MK615 inhibits the production of tumor necrosis factor-α and interleukin-6 in a concentration-dependent fashion. MK615 was also reported to inhibit the phosphorylation of MAP kinases (ERK1/2, p38MAPK), and the phosphorylation of MAP kinase by MK615 was demonstrated. 32 Such phosphorylation would cause the inhibition of NF-κB activation. The signal from the toll-like receptor corresponding to lipopolysaccharide induces the activation of MAP kinases and NF-κB, primarily through MyD88. Cytokines are produced as a response of the transcription factor activated by shifted intranuclear-activated NF-κB and MAP kinases. The activating pathway of MAP kinase and NF-κB leads to various types of inflammatory stimulation, so MK615 is thought to have the potential to inhibit cytokine production.
In this study, we achieved the first demonstration that MK615 would decrease the PD-L1 expression on tumor cells as well as suppress NF-κB. PD-L1 is a major molecule constituting the group of immune checkpoints that develop in a cancer cell. It has speculated that PD-L1 is able to escape attack by acting on cytotoxic T lymphocytes to bind the PD-1 molecules expressed on T cells. Immunocompetent cells come to recognize cancer cells and invalidate this evasion via anti-PD-L1 antibodies, leading to an antitumor effect that enables attack. 33 We suspect that the various antitumor and anti-inflammatory effects of MK615 might be related to each other. Since MK615 did not act in the T cell–deficient nude mice, it seems that the in vivo efficacy of MK615 requires the T cell–mediated host’s immune system.
The improvement of survival by MK615 in this study suggests the possibility that MK615 could prolong the survival of cancer patients in a clinical setting, but no clinical trials to assess the effect of MK615 have been performed yet.
At this time, there is no confirmed evidence of antitumor T cell activation via MK615-induced PD-L1 downregulation in tumor sites. It is also not certain whether MK615 would actually be effective against cancer in clinical practice; further investigations are needed to assess the antitumor effect of MK615. The ability of MK615 to activate antitumor T cell immunities via PD-L1 downregulation should be tested in future studies. Clearly, MK615 exhibits the potential to be a useful addition to cancer therapies administered to enhance antitumor reactivity.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
