Abstract
Introduction
During the past 2 decades, complementary/integrative medicine (CIM) has been increasingly integrated into conventional supportive and palliative care in many leading oncology centers. In 2003, the Society for Integrative Oncology (SIO) was established in the United States, with the goal of advancing integrative medicine by providing evidence-based CIM treatments, improving quality of life (QoL) and function among patients. At its inauguration, the SIO convened a conference of international experts, assessing the most up-to-date scientific evidence supporting the integration of CIM in supportive cancer care. The SIO has since then offered practical guidelines for the implementation of CIM in the oncology setting. 1
The inclusion of CIM in cancer care uses a wide range of complementary medicine treatment modalities, which include nutritional guidance and advice on the use of medicinal herbs and dietary supplements; traditional medicine practices such as acupuncture, meditation, and body-mind approaches; music therapy, manual therapies; and more. CIM treatments are often provided to patients in conjunction with conventional treatment and are monitored by integrative physicians (IPs) who are conventional physicians with training and extensive knowledge on the disciplines and paradigms of CIM care.
Integration of CIM in the general conventional medical setting has been advancing in great strides throughout Israel. CIM services are evident in departments of oncology, psychiatry, surgery, cardiology and others throughout the country, as well as in the community care setting. Referrals by health care professionals (HCPs) to CIM have risen steadily, from 6% in 1993, to 10% in 2000 and 17% in 2007. 2 Hospital-based CIM services are often part of subsidized services provided by the country’s 4 health maintenance organizations, in addition to CIM treatments being offered to their customers throughout more than 100 clinics 3 . In 2002, the Israeli Medical Association registered the Israeli Society for Complementary Medicine (ISCM) as a recognized and official body representing the integration of CIM as part of conventional care. The ISCM currently has 250 physician members and has the stated goal of creating a body uniting physicians, CIM therapists, and researchers in the field of integrative medicine; creating a database of the findings of scientific research on the effectiveness and safety of CIM therapies; and finally, advancing research initiatives in the Israeli scientific community in order to clarify the impact of this integration on conventional medical care. 4
In Israel there are currently 10 active oncology and/or hemato-oncology CIM programs. Four of these services are located in northern Israel (Rambam Medical Center, Lin Medical Center and B’nai Zion Medical Center in Haifa; the Poriah Medical Center in Tiberias); 4 in the central coastal area (Meir Medical Center in Kfar Saba, Rabin Medical Center in Petah Tikva, Sheba Medical Center in Ramat Gan, and Sourasky Medical Center in Tel Aviv); and 2 in Jerusalem (Shaarei Zedek Medical Center, Hadassah-Ein Kerem Medical Center).
The provision of CIM therapies within the public health care system presents a number of challenges. These include addressing the need for working with the conventional oncology system; the design and implementation of a structural and organizational model of care; and the objective assessment of the impact of CIM on quality of life-related outcomes. In addition to these challenges, there is a need to train CIM practitioners so that they are able to work within the conventional oncology system. 5 It has been suggested that there are six key components required to create an integrative environment of cancer care, which can be assessed using what has been termed the “Integrative Oncology Score.” The components of this score include the physical location of the IP consultation room; the source of referral to the IP (oncologist, nurse-oncologist, psycho-oncologist, etc); the ongoing communication between the IP and the patient’s oncologist; the creation of an academic environment, at both the student and CME level; the participation of the oncology institution in remuneration of the CIM staff; and the presence of out-of-pocket costs for the services provided. Each of the 6 components is scored from 0 (not present) to 2 (fully implemented), with a maximum score of 12 points for all 6 factors. 6
The goal of the present study was to examine and compare the structural, operational, financial and academic/research-related aspects of the CIM programs currently taking place within Israeli oncology centers. The challenges and obstacles to integration are identified, with possible solutions to these obstacles discussed.
Methods
Study Design
The study was designed as a descriptive survey, with the goal of identifying the characteristics of the participating integrative oncology services that are active today in Israel. The study was conducted in 7 medical centers throughout Israel, between June 2015 and July 2016.
Inclusion Criteria
The study questionnaires were sent to medical centers in Israel that provide integrative oncology services to patients and are headed by an integrative physician. Participating centers are listed in the database of the Israeli Society for Complementary Medicine, Israeli Medical Association.
Questionnaire Design
For the design of the study tool a PubMed-Medline search was conducted, using the keywords: “complementary medicine,” “integrative medicine,” “oncology,” “supportive/palliative care,” and “Israel.” A number of articles were identified, which dealt with core issues in the establishment and operation of integrative medical centers, primarily in the oncology setting.
One of the studies included in this search used a questionnaire that was designed to compare six integrative oncology programs in the United States, Argentina, the United Kingdom, Germany, and Israel. The study examined the 6 key components of care, which included the “Integrative Oncology Score.” 6 The results of this study were used to address factors related to the integrative oncology setting, which were similar to what was being examined in the present study: the location of the CIM consultation/treatment rooms, and their proximity to the conventional oncology services provided; HCP-IP communication; CIM-related academic activity (ie, research and education); and cost-related aspects, specifically the coverage provided for the CIM activities by the oncology institution (vs out-of-pocket payment).
Next, questionnaires that had been used in an earlier study on integrative oncology settings in Israel, for both patients and HCPs, were examined for their suitability for the present study.7-9 These questionnaires were assessed for a number of elements that address communication between patients and their oncology HCPs, such as the goals of the CIM therapeutic process; models of the integrative medicine program (eg, the CIM modalities being provided; method of referral to the CIM service); and expectations regarding the interaction between the CIM staff and the conventional oncology HCPs. Before incorporating the relevant questionnaires into the present study’s protocol, a focus group of twelve physicians and integrative oncology practitioners was convened for the final design and refinement of the study tool.
The focus group’s recommendations led to the implementation of a number of small changes to the study questionnaires. These included the addition of questions which asked respondents at each of the participating medical centers to assess the extent to which the conventional oncology staff was supportive of the CIM program. This question was to be assessed by examining the HCPs’ referral to the CIM service, and their feedback regarding the impact of the integrative program on patients’ well-being.
The questionnaire was sent by e-mail to each IP heading the eligible integrative oncology services, initially for their input on the study questions and in order to identify functional core questions that did not appear in the study tool. The final version of the questionnaire (see the appendix) was sent to the IP directors (via e-mail), and included 33 questions that dealt with the structural and operational aspects of their respective services; explored the method of referral to the CIM service; addressed economic aspects of the service, with questions on the method of payment by the patient, and staff salaries; and determined academic/research aspects, including the process of training CIM practitioners. The questionnaire contained 24 multiple-choice questions, 6 yes-or-no questions, and 3 open questions.
Statistical Analysis
The findings from the data were compiled in a Microsoft Excel table (Windows 2007) and presented in percentages. Qualitative analysis of patient narratives, appearing as 2 open-ended questions and comments in the “others” option of the multiple-choice questions, were analyzed using content analysis method. 10
Ethics
HCP perspectives on the impact of the integrative oncology program on quality of life were nested within a registry study protocol, which was approved by the Ethics Review Board (Helsinki Committee) of the Carmel Medical Center in Haifa, Israel (0024-09-CMC); and registered at ClinicalTrials.gov (NCT01860365). All respondents in this study participated on a purely voluntary basis and provided informed consent following oral as well as written explanation of the research methodology and goals.
Results
A total of ten medical centers in Israel were found to be providing integrative oncology treatments (Israeli Society for Complementary Medicine Database). Of these, seven were headed by an integrative physician, thereby fulfilling the study’s inclusion criteria: in northern Israel, the Rambam Medical Center, Lin Medical Center and the B’nai Zion Medical Center, all in Haifa; in central Israel, the Sheba Medical Center (Ramat Gan), Meir Medical Center (Kfar Saba) and the Rabin Medical Center (Petah Tikva); and in Jerusalem, the Hadassah (Ein Kerem branch) Medical Center. The structural, operational, financial, and academic/research-related aspects of the seven participating IO programs are presented in Table 1. In all of the programs CIM treatments were focused on improving patients’ quality of life, within the context of supportive and/or palliative care. Patients were undergoing CIM treatments at different stages of their disease, including during active chemotherapy and radiation, as well as before and after surgery. Most of the participating centers provided treatments to patients with solid tumors, with only two treating patients with hematological malignancies. For example, the integrative oncology service in center 7 was established by the head of the hospital’s hematology department, in conjunction with the director of the integrative medical service. The goal of this service was to help reduce the symptom load of hemato-oncology patients who were undergoing chemotherapy and biological treatment regimens. The majority of integrative oncology services (n = 5, 71%) provide treatment following the completion of chemotherapy/radiation therapies, in conjunction with preventive oncological treatments, and during the convalescence phase. Only 1 of the participating services reported that they were also providing CIM to family members, with 2 services providing treatment to the oncological staff as well.
Characteristics of Integrative Oncology Centers in Israel. a
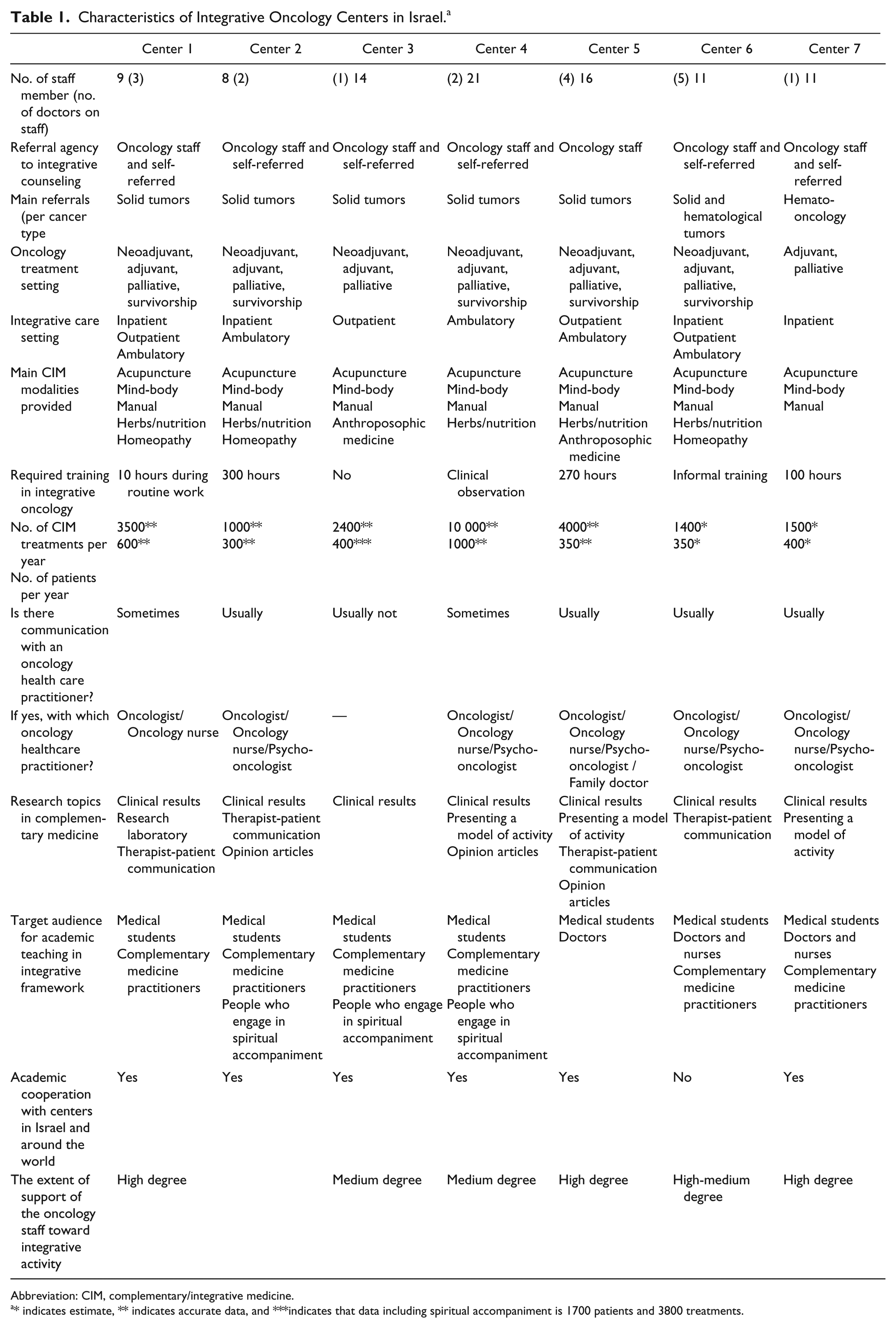
Abbreviation: CIM, complementary/integrative medicine.
* indicates estimate, ** indicates accurate data, and ***indicates that data including spiritual accompaniment is 1700 patients and 3800 treatments.
The provision of CIM was found to take place in a number of oncology settings, which included inpatient (57%, n = 4), outpatient day hospital (57%, n = 4), and ambulatory treatment services (86%, n = 6). For example, most of the integrative oncology activity in center 5 was provided to patients who were undergoing chemotherapy in an outpatient service, while other centers provide these treatments within a tertiary-care inpatient setting. The CIM modalities provided included acupuncture, manual techniques (at all 7 centers); relaxation and mind-body medicine modalities (6 centers); nutritional counseling and guidance on the effective and safe use of medicinal herbs and supplements (5 centers). In 4 of the study centers homeopathic treatment was offered as well, as were spiritual and art therapy, both provided by trained therapists. In 2 of the study centers patients were offered treatments based on anthroposophical medicine.
The number of CIM practitioners varied between the participating study centers, ranging from 5 to 18 practitioners. All centers required CIM therapists to have extensive training in complementary medicine, as well as work experience in their respective fields. In 5 of the centers (71%), CIM practitioners were required to receive on-site training prior to the commencement of work. All of the centers provided CIM treatments to patients who had been referred by an oncology HCP (health care provider), with 6 centers accepting patients who had been self-referred.
At 5 of the participating centers, the initial consultation was conducted by an integrative physician. For example, more than half of the patients in center 1 had been referred to the integrative physician consultation by their oncologist or oncology HCP, with a specific clinical indication given for the referral. The integrative physician at this center is dually trained in supportive cancer care and in a number of CIM modalities which include traditional Chinese medicine and hypnosis. During the initial IP consultation (lasting between 45 and 60 minutes), the IP assesses the patient’s expectations from the CIM treatment program; discusses any previous experience they may have had with complementary medicine; and identifies the leading concerns related to impaired quality of life and well-being. At the end of the consultation, the IP and patient co-design an integrative medicine treatment plan, which is both evidence-based and patient-tailored, with the goal of reducing oncology treatment–related toxicities and improving quality of life.
The summary and recommended treatment plan were documented in a number of ways: in the computerized patient file of the medical center (n = 5); in the integrative service computer file (n = 1); manually, in the CIM service’s internal records (n = 3); or manually, documented in the patient’s oncological medical file (n = 1). Five of the centers reported holding staff meetings, at which the progress of the treatment regimen was discussed and re-assessed. However, with the exception of 2 centers, the scheduling of such evaluations was not at regularly scheduled intervals. At 3 of the centers, the evaluation of progress was conducted using validated patient-reported study outcomes. In addition to the CIM team, communication with the oncology staff was ongoing at 6 of the centers, specifically with regard to the patient’s distress (n = 4), goals of the CIM treatments (n = 4), assessment of treatment outcomes (n = 4), and coordination of CIM treatments with those of the conventional oncologists (n = 1). Seven of the centers reported conducting research that examines the implementation of the integrative treatment; the clinical impact of the therapeutic process; and attitudes toward the integration of these practices in cancer care. Five of the centers reported collaborating on a number of research projects, which have been published in the scientific literature. All 7 of the participating centers reporting academic activities targeting medical students, physicians, nurses, and/or complementary medical therapists.
Further evidence that supports the advancement of integrative oncology can be seen in the clinical and preclinical research that is taking place at the study centers, in many cases in collaboration with conventional oncologists. In addition, the centers report providing extensive medical educational programs in which they are teaching medical students, physicians, nurses, and CIM therapists about each other’s paradigms of care, along with the evidence supporting the benefits of CIM in cancer care. In 5 of the centers, academic and research projects are being conducted in cooperation with one or more of the other study centers. At the same time, the treatment-related aspects of care differ between the 7 centers in a number of ways. These include the extent of training required for IPs and CIM practitioners in CIM-related supportive cancer care; the qualifications of the health care practitioners performing the initial evaluation (ie, physicians vs nurses); the variety of CIM treatments that are being provided at each of the centers; the tools used to identify and assess quality-of-life–related concerns and distress; and finally, the implementation of structured follow-up visits.
As complementary medicine is not included in the Israeli health ministry’s basket of services, payment for the CIM treatments varied between the participating medical centers. At some of the centers, patients were required to pay for the treatments themselves (“out-of-pocket”; n = 4). At others, the treatments were administered as part of a research project and without charge (n = 4). In others, the medical centers themselves covered the expenses of the CIM treatments (therapists, administration, rooms, equipment, etc; n = 3), in some cases with CIM practitioners who were working in a voluntary capacity (n = 3).
Communication between the CIM staff and oncology departments was manifest in a number of ways: At all of the participating centers, patients were referred by their oncology health care professional with some of the centers enabling the patients to schedule an appointment for these services on their own. At the majority of the centers, CIM practitioners report providing feedback to the oncological staff regarding the impact of the treatment on patient quality-of-life–related outcomes (n = 5). However, 6 of the centers reported a lack of cooperation between the oncological and CIM staff with regard to the design of the integrative treatment plan.
Discussion
Israel is one of a number of developed countries in which CIM is increasingly being incorporated into conventional supportive cancer care. The present study examined this integration in 7 Israeli oncology centers, all headed by integrative physicians with training in CIM-related fields. The present survey discovered a number of commonly shared characteristics among the participating centers, such as the focus of treatment goals on quality-of-life–related outcomes and reducing the symptom load related to the oncological treatment. This approach to cancer care separates integrative medicine from “alternative” medicine, which takes place outside the conventional medical setting and often makes claims regarding the impact on survival (even to the point of “cure”), and less emphasis on improving quality of life. The integrative approach typified the participating CIM centers, whose mandate is guided by both a scientific, and an ethical commitment to patient care and providing evidence-based medicine to their patients. The centers all recognize the importance of open and nonjudgmental communication with patients and oncologists. In some of the centers, the CIM approach addressed not only the patient but also the primary caregiver and family members, as well as the distress of the oncology medical staff.
The process of incorporating a CIM service within the conventional oncology setting presents a number of challenges, such as the physical location of the integrative program. At 6 of the 7 centers, CIM treatments take place within an oncology department, in some cases as part of an out-patient clinic. Still, the interaction between the oncology team and the IP and CIM staff is most often limited to the referral of patients, as opposed to taking a more active role in design and implementation of the treatment plan. In order to ensure effective and enhanced communication between integrative physicians/therapists and the oncological staff, each visit is documented in the patient’s medical file.
The 7 centers differ significantly with respect to their administrative and financial characteristics. CIM treatments are not covered by the Israeli national insurance program, and while five of the centers provide these treatments either without charge or else at subsidized rates, this coverage is dependent on the availability of research funds, donations, and additional sources. Until CIM is included in the Israeli “health basket,” it will not be possible to include these therapies as a routine part of supportive cancer care, within the conventional oncology setting.
The study centers also varied greatly with regard to the number of treatments given to each patient. This ratio ranged from 3 to 10 treatments per patient seen. It is likely that this variance reflects the setting of each center (eg, outpatient vs inpatient); the structure of the service (research vs pay for service; single consultation on herbal medicine vs series of acupuncture treatments); and the expectations of the patients and staff members.
Integrative medicine in the Israeli oncology setting is unique as in that it is largely situated within conventional oncology departments and clinics. This contrasts with the 29 integrative oncological programs surveyed by Seely et al, 11 where less than half the programs (41%) were providing CIM therapies in the same location as conventional treatment was being administered. The findings of the present study, which examined 7 integrative oncology programs in Israel, differ in a number of ways from those of a study conducted among 124 Australian hospitals, where only 11 of the oncology centers surveyed were found to provide complementary medicine services as an integral part of the conventional oncology setting. 12
Israeli centers of IO are characterized by a high rate of referral from medical staff; communication between integrative physicians/therapists and in-house oncology health care practitioners; and the documentation of CIM consultations and treatments in the patient’s medical file. Israeli IO centers are also conducting a large number of research initiatives in CIM and integrative oncology, in some cases collaborating with other centers in the country. The results of the present study are similar to those in a recently published article by Lim et al, 13 comparing 6 oncology centers providing integrative medicine in the United States and Germany. In both this and the present study, the integrative physician plays a dominant role (when compared with nonphysician CIM practitioners) at both the initial consultation phase and with regard to academic activities such as research and medical education. Both studies also described settings that required a referral from a conventional oncology HCP to the CIM consultation and treatment program, or else which preferred HCP referral to patient self-referral. A referral from a conventional health care practitioner is reflective of the integrative process and plays a key role in advancing communication between and among the conventional and nonconventional medical teams.
Integrative medicine research at the centers is conducted without the existence of national research institutions in Israel, in contrast to other countries (eg, the Office of Cancer Complementary and Alternative Medicine of the National Cancer Institute and the National Center for Complementary and Integrative Health of the National Institutes of Health in the United States).
The present study has a number of limitations, which need to be addressed in future research on this subject. First, the survey included only those centers that operate within oncology departments, and are directed by physicians with training and experience in CIM, and not similar services provided by hospitals, health maintenance organizations and private clinics. Second, the survey’s data are based on the responses of the participating centers’ medical directors to a structured questionnaire. Future research needs to examine other models of care, and to also survey the oncology staff and patients. Finally, the study examined the financial and administrative aspects of the various models but did not examine the employment status of the CIM therapists (eg, salaried vs volunteer), or additional cost-effective variables. These aspects need to be better understood in order to advance the integration of CIM in cancer care.
In summary, the present study illustrates the relatively high degree of integration of CIM in the Israeli oncology setting. There remains a wide variance among the different centers’ operating models, with each presenting different and common obstacles to the integrative progress. The role of medical education varied greatly between centers, with regard to both education initiatives in integrative medicine for conventional oncology HCPs and the requirement for specialized integrative oncology training for CIM practitioners. Yet despite these differences, the 7 oncology centers share similar objectives, which include providing CIM therapies that can improve patients’ wellbeing, within a patient-centered context of supportive and palliative care. It would therefore be extremely constructive to create a national collaborative effort, which would be shared by the integrative oncology centers in Israel. The goal of this project would be to promote a research-focused environment which would focus on both improving quality-of-life outcomes for patients with cancer and facilitating medical education to oncology HCPs.
Footnotes
Appendix
Authors’ Note
Eran Ben-Arye is not affiliated to Graduate Studies Authority, Haifa University, Haifa, Israel.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
