Abstract
Background. Complementary therapies (CTs) are increasingly utilized by cancer patients. Nonetheless, patients report insufficient support from health care practitioners (HCPs) and there is a general lack of patient-practitioner communication about CT use. Best care practices suggest that HCPs should address the needs of patients, including CT use. This study examined current practices of patients and HCPs as well as their interactions relating to CTs. Methods. A total of 481 cancer outpatients and 100 HCPs completed questionnaires. Patient questions addressed CT use and information needs; HCP questions addressed knowledge, opinions and beliefs about complementary and alternative medicine. Patient-practitioner communication around CT was also examined. Results. 47% of patients reported using CTs since diagnosis. Many commenced CT use to improve quality of life (65%) based on recommendations from family or friends. Patients acknowledged the need for trusted sources of information and would attend a hospital-based education program (72%). HCPs reported limited training about CTs but most (90%) expressed interested in receiving more training. The majority of HCPs (>80%) reported limited knowledge about the role of CTs in cancer care or evidence to support CT use. Questions about communication and interactions revealed that 80% of patients reported not having had an HCP speak to them about CTs. However, 63% of HCPs reported addressing CT use. Conclusion. Results demonstrate a need for improved CT education and training for patients and HCPs. increasing HCP knowledge and clinical skills will ensure patients’ information needs about CTs are acknowledged and attended to, thereby providing safer and comprehensive cancer care.
Introduction
Cancer is the leading cause of death in Canada, accounting for approximately 30% of all mortalities. 1 Along with increasing cancer incidence and prevalence in Canada, 2 survival rates are increasing due to enhanced screening and better treatment. 3 This has resulted in a large cohort of people termed “cancer survivors.” 4 To enhance quality of life and cope with treatment toxicities, many cancer survivors look beyond conventional medicine and are turning to complementary and alternative medicine (CAM). 5
CAM is defined by the National Center for Complementary and Integrative Health (NCCIH) as “a group of diverse medical and health care systems, practices, and products that are not generally considered part of conventional medicine.” 6 CAM is a broad umbrella term for several categories including natural health products, mind–body medicine, manipulative and body-based practices, energy therapy, and whole medical systems (eg, naturopathy). 6 It includes both complementary and alternative therapies, 2 distinct forms of treatment. Complementary therapies (CTs) are used in addition to standard treatment, whereas alternative therapies are used instead of conventional medicine. 6
A recent meta-analysis found that 45% of all cancer patients worldwide have used CAM since their diagnoses. 5 CAM is most popular with females, breast cancer patients, younger individuals, and those with a higher level of education and higher socioeconomic status.7-9
Despite the high use of CAM by cancer patients and a preference to receive CAM information from credible sources, 10 patients list support groups, friends, family, and books as their primary sources of CAM information.11,12 This presents a problem as patients may be receiving unreliable information and are often overwhelmed and confused about the credibility of CAM information available. 10 Additionally, it has been reported that up to 77% of cancer patients do not disclose their CAM use to their HCP, demonstrating a lack of patient–practitioner communication about CAM. 13 This lack of communication is concerning given the potential for CAM to exacerbate or alleviate symptoms related to conventional treatments, as well as the risk of interaction with conventional medications. 14
HCPs have a responsibility to provide optimal care for their patients and this should include addressing the risks and benefits of CAM. Indeed, many patients assume that HCPs will do so. 10 However, this is not occurring in practice, possibly because many HCPs are unaware that CAM is within their scope of practice, are uncertain of CAM evidence, lack training about CAM therapies, or are skeptical about CAM use.10,15-18
The goal of this study was to understand why communication about CAM is not occurring between patients and HCPs, and how CAM communication could be improved during HCP–patient interactions. Therefore, we examined (a) patient preferences, use, and reasons for using CT; (b) deficiencies in patients’ access to information and information-seeking behavior; (c) HCPs’ knowledge, preparedness, opinions, and beliefs about CAM; and (d) patient–HCP interactions, with a focus on communication about CAM.
Methods
Participants
Patients
People diagnosed with any type of cancer, aged 18 years and older, and who were attending outpatient clinic appointments at the Tom Baker Cancer Centre were eligible to participate. There were no restrictions on stage of disease, time since diagnosis, or treatments received.
HCPs
Health care providers of any discipline working at the Tom Baker Cancer Centre who had contact with cancer patients were eligible to participate. The research was approved by the Conjoint Health Research Ethics Board of the University of Calgary. Participation was voluntary, and it was explained that completion of questionnaires was considered implied consent.
Procedures
Patients were approached in 2 outpatient clinics in Calgary, Alberta. The researchers informed the patients of the purpose of the study, and those that agreed to participate were given the option of completing the questionnaire at the clinic, or taking a questionnaire home, and returning it using a postage-paid envelope. Patients were only asked about CTs, not alternative therapies. The focus on CTs was used to avoid suggestions that the researchers advocated the use of alternative therapies instead of conventional medicine.
HCPs were recruited from the main cancer care hospital in Calgary, Alberta. The HCP survey asking about CAM was distributed via email to all HCPs. To reach as representative a sample as possible, the survey was also distributed at various department meetings by the research team or department heads. Hard copies of the survey were distributed to oncologists’ mailboxes.
Questions: Patients
Use of CTs
Patients were asked whether they had used CTs since their cancer diagnosis, and if they had used CTs, which type(s) based on the NCCIH categories. These questions were adapted from a patient needs assessment survey designed and used within the University of British Columbia (UBC)/British Columbia Cancer Agency (BCCA) Complementary Medicine Education and Outcomes Program (CAMEO). 19 Permission for the use and modification of the CAMEO survey was obtained.
Interest in CTs
Patients were asked to rate their interest in learning more about each type of CT on a 5-point Likert-type scale. This question was created in order to determine relative interest in the various categories of CTs.
Reasons for Using CTs
Patients were asked to check all reasons for their use of CTs. The options were predefined and adapted from previous research examining CAM use in cancer patients.12,20 Patients were also asked to indicate the single, primary reason for their use of CTs.
Barriers to Using CTs
Eight items comprising established barriers to CT use reported during focus groups in the United Kingdom, 21 and other barriers the researchers hypothesized would affect patient use of CTs were presented within the questionnaire. Using a 5-point Likert-type scale patients indicated the extent to which they found each potential item a barrier to their use of CTs.
CT Information Needs
Patients were asked whether they had needed information on any of 8 listed questions about CTs since their cancer diagnosis. These questions were replicated from the UBC/BCCA CAMEO survey. 19 Furthermore, patients were asked whether they would use an in-house hospital-based CT education program if one were available.
Patient Perceptions of HCP Relationship
Patients were provided with 9 questions, again drawn from the UBC/BCCA CAMEO survey, 19 asking about patient–practitioner CT communication. First, patients were asked if any HCP had spoken to them about CTs. If patients had been spoken to about CTs, they were asked to identify the specific HCP who had spoken to them. The remaining 7 questions utilized a 3-point Likert-type scale to examine information seeking, decision making, comfort, and satisfaction in relation to CT communication with the HCP.
Questions: HCPs
Knowledge About CAM
Eight questions were used to assess knowledge of CAM and its role in cancer care. These questions came from a HCP practices and learning needs survey designed and utilized by the UBC/BCCA CAMEO program. 19 The term CAM was used in the provider questionnaires to replicate the original instrument. 19
Preparedness for CAM
Practitioners were required to rate their CAM clinical and information seeking skills preparedness on a 4-point Likert-type scale for 10 items. Six questions assessed clinical skills whereas 4 assessed preparedness to find credible information about CAM therapies. All questions were drawn from the UBC/BCCA CAMEO HCP survey. 19
Opinions and Beliefs About CAM
Opinions and beliefs about CAM were obtained through 6 questions using a 5-point Likert-type scale. The questions were adapted from a survey conducted by Visser and Peters 22 on the attitudes of Turkish general practitioners (GPs) toward alternative medicine. The questions have high internal consistency (Cronbach’s α = .86) 22 and have been previously used to assess the opinions of Canadian GPs toward alternative medicine. 23 The wording of the questions were altered from the original 22 and replaced the term “alternative medicine” with the term “CAM.”
Perceptions About Patient Relationship and CAM
The questionnaire contained 25 questions addressing HCPs’ current practice in the previous month. Six questions asked HCPs about how patients were interacting with them. The following 13 questions addressed HCP interactions with patients. Two questions asked HCP if they had directed patients to consult with another HCP to have their questions answered or information needs met. The next 2 questions asked HCPs to report if they had consulted with other HCPs in order to answer patient questions. The final 2 questions in this section asked HCPs whether they had referred patients to websites for CAM information, and to which website(s) they referred patients. All questions were derived from the UBC/BCCA CAMEO HCP survey. 19
Interest in Further Education
HCPs were asked to indicate, on a 5-point Likert-type scale, their interest in receiving more information, education, and/or training about CAM.
Data Analysis
Data were analyzed using descriptive statistics and frequencies to explain the outcomes for the 2 participant groups. Chi-squares analysis, using SPSS v21.0, examined relationships between the prevalence of various categorical variables and demographic data. Power calculations revealed a sample size of 599 patients would provide a confidence level of 99%, with a 5-point margin of error. A sample of 170 HCPs, out of a total population of 300, would achieve a 95% confidence level with a 5-point margin of error.
Results
Demographics
Patients
Approximately 800 cancer outpatients were approached to participate. A total of 481 patients completed the surveys, resulting in approximately 60% response rates. Therefore, the final sample size is marginally underpowered, resulting in a 95% confidence interval with a 5-point margin of error for patients. The complete demographics of the patients are reported in Table 1. Briefly, the mean age of the patients was 59 years, 62% were female, 78% Caucasian, diagnosed with a variety of cancer types.
Demographic Characteristics of Patients (n = 481).
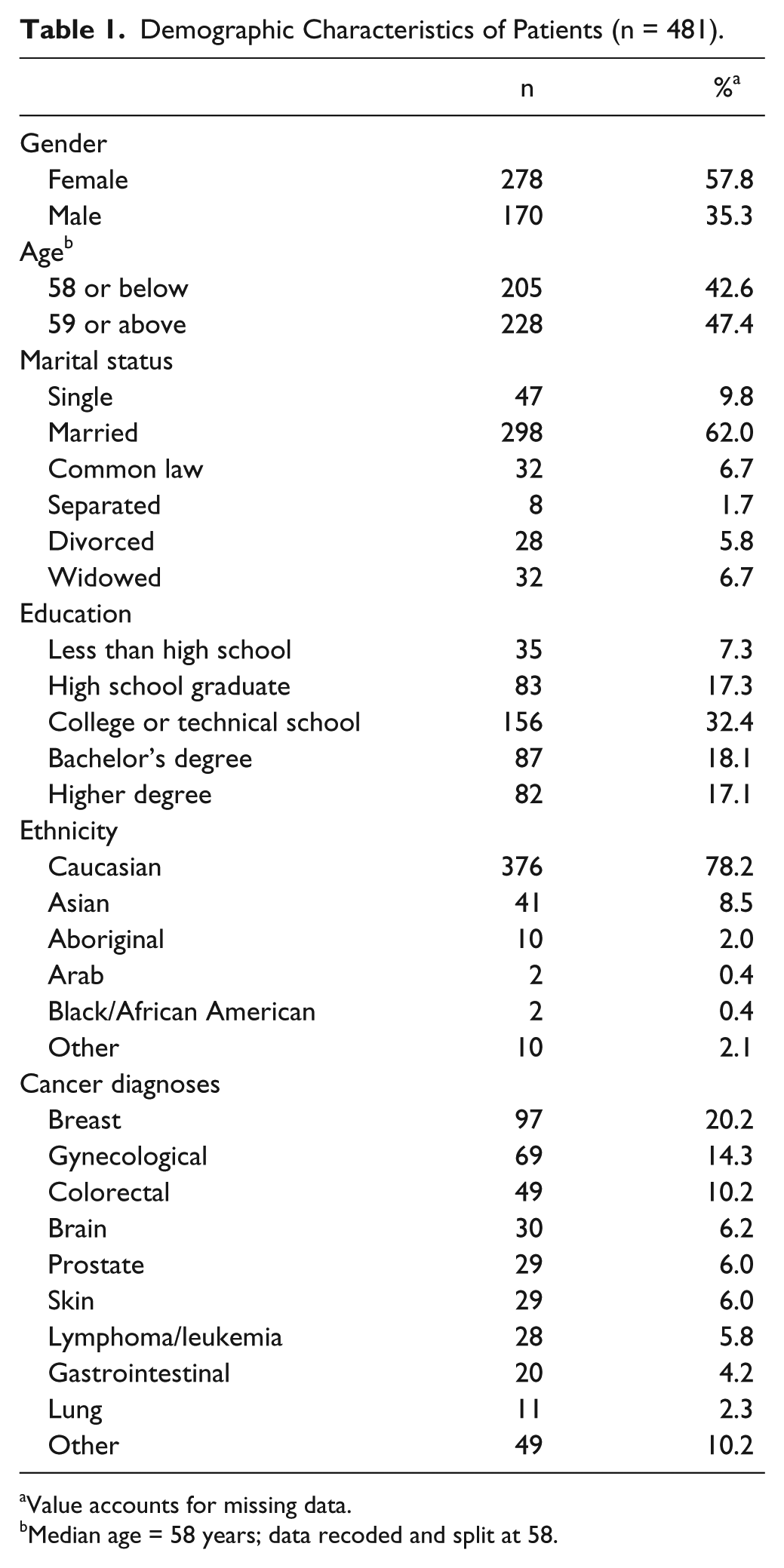

Value accounts for missing data.
Median age = 58 years; data recoded and split at 58.
HCPs
Approximately 300 HCPs were approached to participate and 100 completed the surveys, resulting in a 30% response rate. Therefore, the final sample size is marginally underpowered, resulting in a 95% confidence interval with an 8-point margin of error for HCPs. The complete demographics of the HCPs are reported in Table 2.
Demographic Characteristics of Health Care Practitioners (HCPs; n = 100).

Value accounts for missing data.
Patients’ Use, Interest, Reasons for Use, and Barriers to Use of CTs
Almost half of all patients surveyed (47.2%, n = 227) reported using CTs since being diagnosed with cancer. Biologically based therapies (74.9%, n = 170) were most commonly used. Mind–body therapies were used by 48.5% (n = 110) of CT-using patients, followed by energy-based CTs (34.4%, n = 78), manipulative and body-based CTs (31.7%, n = 72), and lastly whole medical system use (14.1%, n = 32). Fifty-three participants (23%) also reported using other forms of CT, such as cleansing programs and following special diets.
Significantly more females, χ2(1) = 7.1, P = .009, younger individuals (≤58 years old), χ2(1) = 5.9, P = .016, those with more education, χ2(6) = 21.3, P = .002, and those who were diagnosed over a year prior to the survey, χ2(2) = 15.8, P < .001, reported utilizing CTs.
Approximately 65% of patients expressed an interest in learning more about at least one CT. Interest was spread across all 5 domains, but was relatively consistent across each type (46% to 53%). When including those patients who reported being “neither interested nor uninterested,” 77.2% of patients may desire to learn more about CTs.
Among the 224 participants who indicated their reasons for using CTs, the 4 most prevalent reasons were the following: to improve quality of life (QOL; 64.7%, n = 145), to improve immune system (54.3%, n = 121), to treat/be good to myself (40.8%, n = 91), and to increase feelings of hope (35.1%, n = 78). Relieving either cancer-related or treatment-related fatigue was the most common symptom for which CT was used, reported by approximately 24% of all patients. Forty-eight patients (21.6%) also reported that they were using CT to cure their cancer.
The primary reason for commencing CT use was answered by 166 patients. Most (43.4%, n = 72) revealed that their CT use was motivated by recommendations from family and/or friends. When questioned about their barriers to CT use, the majority of patients reported being unsure about the quality of evidence supporting CTs (71%, n = 245/345) and a lack of knowledge about CTs (68.6%, n = 243/354) to be barriers to their use of CTs.
Patient CT Information Needs
The most common questions about CTs were the following: (a) What complementary therapies can be used safely in combination with medical cancer treatments? (36.4%, n = 175); (b) What complementary therapies are helpful for people with cancer? (35.6%, n = 171); (c) When is it safe to use complementary therapies after being diagnosed with cancer? (32.6%, n = 157); and (d) Where do I find trustworthy information about complementary therapies? (32.4%, n = 156). In response to whether or not they would use an in-house, hospital-based CT education program, 281 of 387 (72.6%, 58.4% of the total sample) reported that they would use such a program.
HCPs’ Current Knowledge, Preparedness, and Opinions and Beliefs About CAM
CAM knowledge of HCPs was very limited. Between 20% and 40% reported having no knowledge in 7 of the 8 measures reported in Table 3. The majority of HCPs reported being only somewhat knowledgeable or not at all knowledgeable about various aspects and roles of CAM, and almost none professed to be very knowledgeable.
Health Care Practitioners’ Complementary and Alternative Medicine (CAM) Knowledge Level.

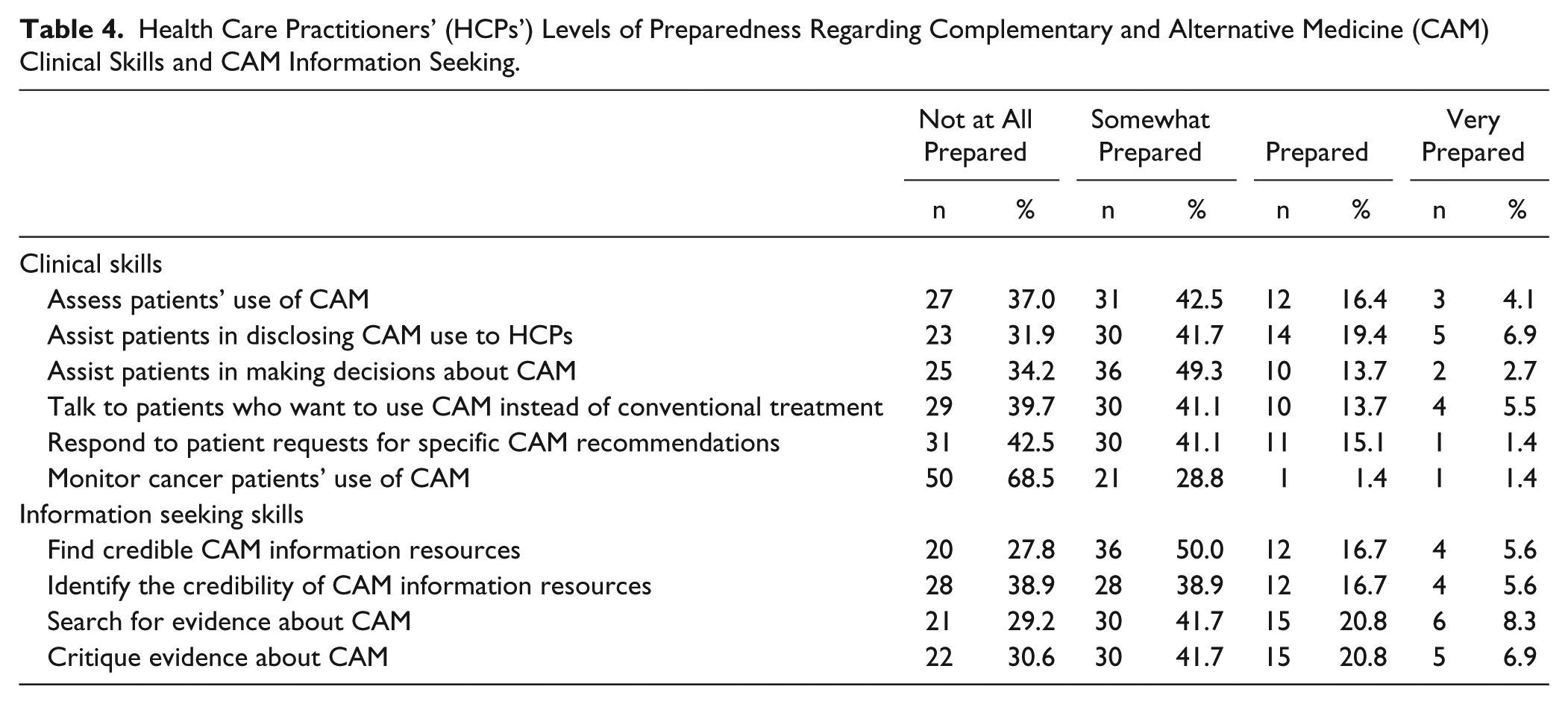
The majority of HCPs reported being only somewhat or not at all prepared when asked about CAM clinical and information seeking skills (see Table 4). Almost 70% of HCPs felt not at all prepared to monitor cancer patients’ CAM use and fewer than 9% of HCPs reported being very capable of searching for credible evidence-based information on CAM and cancer.
Health Care Practitioners’ (HCPs’) Levels of Preparedness Regarding Complementary and Alternative Medicine (CAM) Clinical Skills and CAM Information Seeking.
Mixed results were also found when examining the beliefs and opinions of HCPs toward CAM (Table 5). For example, 49.9% (n = 36) agreed that CAM is a useful supplement to regular medicine, whereas almost 21% (n = 15) disagreed. The most widely agreed view (66.6%, n = 48) was that CAM includes ideas and methods from which conventional medicine could benefit.
Health Care Practitioner Endorsement of Opinions and Beliefs About Complementary and Alternative Medicine (CAM).

Patient–Practitioner Relationship and Communication About CAM
The vast majority of patients (79.7%, n = 374) reported that no HCP had spoken to them about CTs. Of those patients who indicated they did speak to a HCP, most often this was with either medical oncologists (40.2%, n = 43) or nurses (40.2%, n = 43). In spite of so few patients engaging in CT communication, more than 70% (n = 295) reported that they were comfortable talking to their HCPs about CTs, but only 28.8% (n = 99) of patients agreed that their HCP had listened to what they had to say. Overall, only 55 (16%) patients felt that they had received enough information about CTs from cancer health care professionals (Table 6).
Patient Perceptions of Communication With Health Care Practitioners (HCPs).

A significant relationship was found between information and support-seeking and the information and support received. Significantly more patients who requested CT information from their HCPs felt that they received enough CT information, χ2(4) = 139.2, P < .01, and that they received enough support in making decisions about CTs, χ2(4) = 73.1, P < .01. Similarly, significantly more patients who requested CT decision-making support from their HCPs felt that they had received enough CT information, χ2(4) = 139.2.1, P < .01, and that they had received enough support in making decisions about using CTs, χ2(4) = 157.1, P < .01. In addition, significantly more of those patients who felt their HCP listened to them about CTs were comfortable in discussing CTs, χ2(4) = 88.2, P < .01, requested information about CTs, χ2(4) = 498, P < .01, and felt that they had received enough CT information, χ2(4) = 82.3, P < .01, and CT decision-making support, χ2(4) = 75.5, P < .01.
HCP Perceptions
To complement patient reports, HCPs were asked how patients were interacting with them about CAM. Just over 70% (n = 61) of HCPs indicated that at least one patient had told them about CAM use in the past month. On average, HCPs reported that roughly 1 in every 5 (23.3%) patients was telling them about CAM use. Moreover, 50 (58.1%) HCPs reported a similar ratio (21.1%) of patients seeking advice about a CAM therapy that they were currently using. It was less common for HCPs to be asked to monitor patient use of a CAM therapy (12.3%, n = 11), or refer patients to a CAM service or CAM practitioner (15.1%, n = 13).
HCPs were also asked about how they were interacting with patients about CAM. Close to 63% (n = 50) of HCPs reported asking patients about their use of CAM. Nearly half (45%, n = 36) of HCPs provided patients with recommendations about a CAM therapy, while only 8.8% (n = 7) of HCPs were monitoring a patient’s use of CAM and even fewer (6.3%, n = 5) were providing a CAM therapy to patients. Close to a third (32.5%, n = 26) of HCPs reviewed CAM evidence with patients and 25.0% (n = 20) provided patients with CAM educational materials. Very few HCPs (11.5%, n = 9) referred patients to websites for CAM information. A greater proportion of HCPs (49.5%, n = 39) had suggested a patient discontinue a CAM therapy than had suggested a patient use a CAM therapy (32.9%, n = 26).
Of those HCPs who had suggested a patient discontinue a CAM therapy, antioxidants (especially when on radiation therapy), herbs, and high-dose vitamins were the therapies most often advised against. The main reasons practitioners suggested CAM therapy discontinuation included theoretical concerns of interaction (92.3%, n = 36), literature evidence of interaction/harm (46.2%, n = 18), no evidence of efficacy (43.6%, n = 17), and personal clinical experience of interaction/harm (12.8%, n = 5).
HCPs who suggested patients use a CAM therapy most often suggested mind–body therapies and acupuncture. Practitioners based these suggestions mainly on positive effects seen in other patients (73.1%, n = 19), literature evidence of benefit (65.4%, n = 17), and personal clinical experience of benefit (57.7%, n = 15).
By their own admission, most HCPs believed that they required further education and/or training about CAM for cancer care. When surveyed, 90% (n = 63) reported being interested (44.3%, n = 31) or very interested (45.7%, n = 32) in receiving additional CAM training. Only 31.4% (n = 22) of HCPs reported having already received some CAM training, predominantly in the form of conference presentations, through a hospital in-service program, and from seminars/lectures in medical school.
Discussion
This study explored patients’ use, interest, and information-seeking behavior around CTs as well as HCPs’ knowledge, opinions, and beliefs and revealed some interesting discrepancies between the perceptions of patients and those of their HCPs. For example, many patients reported that HCPs did not discuss CT use with them, but a greater proportion of HCPs felt they had. Other unique findings discussed below explore communication between patients and HCPs, patient needs for information and decision support, as well as training needs of HCPs.
Patients’ Use, Interest in Use, Reasons for Use, and Barriers to Use of CTs
Similar to previous reports, 5 47.2% of patients reported using CTs since cancer diagnosis, biologically based and mind–body therapies were most popular, and CT use was higher among females, younger individuals, and those with greater education.7-9 Individuals who were at least 12 months post diagnosis were more likely to report using CTs. This finding suggests that CT use changes over the cancer trajectory, which supports previous findings that identify the influence of disease status as well as psychological social, cultural, and other factors, such as patient–provider communication on CT use.10,24,25 At the time of diagnosis, many patients are interested in taking stock of the full range of conventional and CT treatment options, requiring open, unbiased, and purposeful communication about CTs and CT decision support by HCPs. Complementary therapy decisions and use has been shown to shift over the cancer trajectory, particularly at times of transition, such as at the end of primary treatment, or when disease, social, or other contextual factors shift. 10 These transition are also key points for interaction and communication with HCPs about CTs to ensure patients’ CT information and decision support needs are met. 26
Consistent with previous research, the most common reason patients reported using CTs was to improve their quality of life.12,20,27 Research also suggests that patients use CAM for other beneficial effects and to play an active role in their treatment,9,10 which was echoed in the present study. Patients were using CTs as a form of symptom management, to reduce cancer and treatment-related fatigue and to improve their immune system. CT use was also employed as a means of improving emotional well-being with patients reporting CT use to be good to themselves or to improve feelings of hope.
Surprisingly, just over 1 in 5 patients indicated using CTs to cure their cancer. This underscores the need for greater patient education about CTs to reduce misperceptions and reinforce the necessity of using CTs as an adjunct to conventional medicine, not as an alternative.
When asked about their primary reason for initiating CT use, most patients reported that they began due to recommendations from family or friends. This finding replicates previous research, as did the finding that few patients began using CTs due to HCP recommendation.11,12 Though family and friends are well intentioned, it is concerning that they are the primary motivators for uptake of CT as the information provided may be inaccurate or not account for potential adverse effects the CT could present to the patient. This finding is surprising since the largest barriers to CT use were either being unsure about the quality of evidence supporting CTs and a lack of knowledge about CTs. The lack of HCP-initiated communication about CTs (80% of patients reported no HCP had asked them about CT use) may deter patients raising this subject further. However, it is also possible that patients choose not to tell their HCPs about their CT use, thus eliminating any role, be it positive or negative, that their HCP may have in their use of CTs. Despite concerns about the impact CTs may have on their health and wanting to be informed about safety and effectiveness of CTs, patients do not appear to be sufficiently engaged with HCPs. Therefore, the availability of evidence-based patient resources to increase patients’ knowledge of CTs would likely enable patients to be better prepared to make informed decisions about using CTs.
HCPs’ Knowledge, Preparedness, Opinions and Beliefs, and Interest in Further Education About CAM
Congruent with previous studies,15,16,28 HCPs reported little knowledge about CAM. Similarly, HCPs felt relatively unprepared to address CAM in a clinical context, or to find and evaluate information about CAM. These findings are concerning as patients either already are or should be turning to their HCPs for advice and guidance about comprehensive cancer care, including CAM. A lack of knowledge about CAM limits a HCP’s ability to provide patients with accurate and supportive advice. Moreover, if practitioners are not prepared to assess and monitor CAM use, or provide specific CAM recommendations and guidance, this is likely to negatively affect the patient–practitioner relationship and cancer-related outcomes. Previous research has demonstrated that when HCPs do not engage patients or are perceived as unwilling or unprepared to discuss CAM, this can impair the overall patient–HCP relationship.18,26 This lack of communication about CAM may place patients in a situation where they are required to independently make CAM decisions as well as self-monitor their CAM use. Lack of guidance and support for HCPs about CAM may lead to unintended patient self-harm and/or interfere with expected conventional treatment outcomes. 26
Also concerning was that many HCPs reported being unprepared to evaluate whether information was credible or suitable for their patients (Table 4). In general, HCPs have training in information seeking and evaluation, so this result may be related to the complexities and unfamiliarity of CAM literature for these professionals. Only a third of HCPs reported having received any CAM training; this lack of training may explain practitioners’ deficiencies in CAM knowledge and preparedness, highlighting the need for further education to improve competencies in these areas.
HCPs acknowledged the need to learn more about CAM. It was found that 90% of practitioners reported interest in receiving further CAM education. This interest is consistent with practitioners’ efforts to address CAM needs for patients reported by others.15,16 Furthermore, it is known that increasing CAM training leads to an increase in CAM recommendations, improves patient–practitioner communication about CAM, and creates more positive and open attitudes toward CAM. 29
Patient–Practitioner Perceptions and Communication
Patients and HCPs were asked several questions about the type and quality of communication that was occurring. The findings in this area were generally not consistent, and did not always reflect positively on the overall relationship. It is possible that HCPs and patients hold different perceptions of what “speaking to” and “being spoken to” about CTs consists of. Patients may be expecting a more in depth discussion of CTs than HCPs are offering, or the timing of the discussions initiated by HCPs may not align with when patients are most receptive to hearing or engaging in them. The discrepancy may also be explained by the large proportion of patients who were diagnosed with cancer for a year or less. As reported above, patients in this study were more likely to use CTs with increasing time since diagnosis and, therefore, the practitioners may have been more focused on conventional and curative treatment and not yet have had a chance to speak to patients in the early stages of their cancer care journey about CTs.
A notable discrepancy existed between HCPs’ reports of their current practice around CTs and patients’ reports of communication about CTs. The findings from the patients in this study suggested that HCPs are not adequately addressing their needs or providing sufficient information and support about CTs. In contrast, two thirds of practitioners reported asking patients about their use of CAM, which could provide a doorway for further discussion. The difference in results between patients and practitioners may be explained by the sample of HCPs being examined. The HCPs who responded to this questionnaire may have been more interested in CTs and thus a more involved and informed subsample of practitioners.
Nonetheless, it is apparent that the majority of patients are not discussing CTs with their HCPs, even though patients are willing to discuss their CAM use and are turning to their practitioners for advice and guidance. Patients trust their HCPs 21 and want them to play a role in determining how and when CAM therapies are used. Patients expect that HCPs will initiate discussions of CTs 10 and have cited in the past “not being asked about CTs” as a reason for nondisclosure of their use. 27 The lack of HCP-initiated CT discussions is concerning for a number of reasons, particularly the potential for negative impact on patient health.
HCP results suggested that patients are increasingly initiating discussions of CTs. Over two thirds of HCPs indicated that a patient had told them about their CAM use. This is a positive finding as patient disclosure of CAM use has been associated with patient-centered communication, which in turn has been shown to enhance satisfaction with care, reduce distress, and improve conventional treatment adherence.26,30,31 On average, a quarter of the patients seen by practitioners were reporting their CAM use to HCPs; a similar proportion has been reported in previous studies. 32 This figure reveals that three quarters of patients are not self-disclosing their use of CAM to their practitioners, once again highlighting the need for HCPs to initiate CAM discussions.
In contrast, almost half of the HCPs indicated that they provided recommendations about CAM to their patients. Practitioners suggested more often that patients discontinue, as opposed to commence CAM. Initiating CAM was only suggested on the basis of research evidence or personal clinical experience displaying beneficial effects. However, almost all practitioners reported that they would suggest discontinuing CAM based on theoretical concerns about interactions with conventional medicine. This was often supplemented with evidence of harmful interactions or lack of efficacy. In general, HCPs required a higher standard of proof to recommend CT than they needed to remove it. This practice ensures patient safety and is complimented by research demonstrating that HCPs are not willing to recommend CAM that is not backed by scientific evidence. 15
Limitations
Some limitations should be considered when interpreting the findings of this study. The response rate of 30% for HCPs limits the generalizability of these findings, and raises questions about whether the overall positive view of CAM is a true representation or if self-selection bias affected the opinions and beliefs of HCPs. This bias may have led to practitioners who hold more positive views of CAM to participate. Reasons for nonparticipation were not recorded and, therefore, it is not possible to determine whether HCPs withdrew due to a lack of interest or knowledge of CTs.
The response rate of 60% was far greater for the patients; however, the generalizability of the results is also affected by the fact that a large proportion of patients were diagnosed less than 12 months previously. Therefore, findings may not be applicable to individuals with more chronic cancers or long-term cancer survivors.
A final limitation of the study, faced by all research in this area, is the broad definition of CAM and the large number of therapies it encompasses. Both the patient and HCP questionnaires addressed this issue by using standardized definitions. The patient questionnaire further addressed the issue by using examples of CTs and asking patients about CTs in general, the 5 categories of CTs, and to list the specific CTs they utilized. The HCP questionnaire was less successful at addressing the variety of therapies and products encompassed by CAM as it only asked about CAM as a whole. Several HCPs commented that their practice, knowledge, skills, opinions, and beliefs varied based on the CAM therapy or product being discussed.
Conclusions
In summary, almost half of the cancer patients surveyed had utilized CTs since their diagnosis. Patients report that HCPs are not communicating with them about CTs and that their CT information and decision-making needs are not being met. However, when communication occurs, it appears to be effective in satisfying patient concerns. Patients are interested in learning more about CTs, specifically the impact on their health, and would utilize a hospital-based education program to obtain this knowledge. In contrast, HCPs reported a greater incidence of patient-initiated communication about CAM and also report more practitioner-initiated communication than patients did. HCPs are cautious in the recommendations they make about CAM, making more recommendations toward discontinuation of CAM. Similar to patients, HCPs were interested and willing to receive more education and training in CAM.
There is a clear need for improved education and training materials and programs for both patients and HCPs. Such materials and training will help ensure HCPs are meeting patients’ CT needs. It will also help guarantee that patients are receiving reliable and accurate information about CTs and guidance that will allow for CTs to be used to improve their health and well-being, while avoiding the potentially harmful impact of inappropriate CT use. Finally, increased education and training about CTs will move cancer care toward providing a more integrative form of oncology that will allow patients to have all of their care and information needs to be met at a single location.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr Linda Carlson is holder of the Enbridge Research Chair in Psyhosocial Oncology, cofunded by the Canadian Cancer Society Alberta/NWT Division and the Alberta Cancer Foundation.
