Abstract
Background. The use of complementary and alternative medicine (CAM) has increased and little is known on CAM use during the initial period. Therefore, the aim was to determine prevalence of CAM use among newly diagnosed breast cancer patients prior to seeking conventional treatment. Methods. This is a cross-sectional study involved interviewing newly diagnosed breast cancer patients in the University Malaya Medical Centre (UMMC) using a structured questionnaire. Eligible respondents were interviewedduring a routine clinical visit. Results. A total of 400 patients were interviewed, of whom 139 (34.8%) were CAM users. Dietary supplementation (n = 107, 77.0%) was the most frequently used type of CAM, followed by spiritual healing (n = 40, 28.8%) and traditional Chinese medicine (n = 32, 23.0%). Malay ethnic group (n = 61, 43.9%) was the largest group of CAM users, followed by Chinese (n = 57, 41.0%) and Indian (n = 20, 14.4%). Majority of these CAM users (n = 87, 73.1%) did not disclose the use of CAM to their doctors. Most of them used remedies based on the recommendation of family and friends. Malay ethnicity and patients with 3 or more comorbidities were more likely to use CAM. Conclusion. There is substantial use of CAM among breast cancer patients in UMMC prior to seeking hospital treatment, and the most popular CAM modality is dietary supplements. Since, the majority of CAM users do not disclose the use of CAM to their physicians, therefore health care providers should ensure that those patients who are likely to use CAM are appropriately counseled and advised.
Keywords
Introduction
Breast cancer is the most common cancer among women worldwide. 1 Over the past few decades, advances in diagnostic screening and adjuvant therapy have dramatically increased the number of breast cancer survivors, 2 and they are the largest group of female cancer survivors.3,4 In addition to conventional therapies, many women want to improve and maintain a healthy lifestyle by using complementary and alternative medicine (CAM) as well as making adaptive lifestyle changes that are related to behaviors such as quitting smoking, not drinking alcohol, and engaging in regular physical activity and dietary change.5,6 Complementary and alternative medicine is defined as “a group of diverse medical and healthcare systems, practices, and products that are not generally considered as a part of conventional medicine.” 6 Other terms used to describe these health care practices include natural medicine, nonconventional medicine, integrative medicine, and holistic medicine. 7
Worldwide surveys suggest that the use of CAM is becoming increasingly popular among the general population as well as among cancer patients.8,9 In Asia, 40% to 80% of breast cancer survivors use CAM,10-12 whereas in western countries, approximately 47% to 83% do so.13-16 In Malaysia, a multiracial and multicultural country, breast cancer patients are exposed to CAM from both western and eastern countries, the modalities of which range from the use of dietary supplements, herbs, and homeopathy to traditional medicines such as traditional Chinese medicine (TCM), traditional Malay medicine (Jamu), and traditional Indian medicine (Ayurveda). The National Centre of Complementary and Alternative Medicine (NCCAM) has classified CAM into 5 categories for ease of standardization: whole medical system, mind-body medicine, biologically based practices, manipulative and body-based practices, and energy medicine. 6
The use of CAM starts at different time points in the cancer journey and addresses a range of different patient concerns. 17 For instance, a previous study has shown that most breast cancer patients experience a higher level of stress after they have been diagnosed. 18 They use CAM at this time to relieve stress and to cope with the disease. However, patients who use CAM during and after conventional treatment believe that CAM use could help them remain symptom free with good quality of life (QoL) during cancer treatment. 19
Despite the lack of evidence of CAM efficacy in relation to breast cancer, many women believe that CAM could help them in “naturally” treating their disease and, thus, improve their QoL.17,20,21 Malaysians, irrespective of their ethnic group, have a strong tradition of using traditional medicine for treatment and relief of breast cancer symptoms. 22 However, there has been no proper documentation on the practice of CAM among newly diagnosed breast cancer patients in Malaysia. Few studies have reported CAM use immediately after a diagnosis of breast cancer and what motivates the patients to use CAM before commencing conventional treatment.5,23 Therefore, this article is a baseline report that aims to describe the prevalence of CAM use immediately after breast cancer diagnosis and identify patterns of CAM use and the motivations behind them. It is hoped that the information provided will help improve our understanding of CAM use among this patient group. It is also hoped that this article will help health care practitioners identify CAM practices that may affect a cancer-related prognosis and adherence to conventional breast cancer treatment.
Methodology
Design and Procedure
This is a single-center, cross-sectional study conducted at the University Malaya Medical Centre (UMMC). The UMMC is a tertiary hospital with established breast oncology services and breast cancer registry system 24 located in Kuala Lumpur, the capital city of Malaysia. Patients were recruited during the period February 2012 to December 2014. In total, 400 patients were enrolled as part of the Malaysia Breast Cancer Cohort (MyBCC) study. 25 The MyBCC study is an ongoing hospital-based prospective cohort study of Malaysian women who are newly diagnosed with primary breast cancer (within 3 months of diagnosis), >18 years old, and able to read and understand Malay, English, Mandarin, or Tamil. The exclusion criteria are the following: patients who have a prior history of any other cancer, patients who are bedridden at the time of recruitment, patients whose attending physician certifies them as unfit as a result of other prevailing medical conditions, and patients who are reluctant to join the study. This study used the NCCAM’s 5 categories of CAM: whole medical system (TCM, Indian traditional medicine, and homeopathy), mind-body medicine (spiritual/prayer, traditional Malay medicine, yoga, and cupping), biologically based practices (dietary supplements), manipulative and body-based practices (reflexology and massage), and energy medicine (Qigong and Tai Chi).
This study was approved by the Medical Ethics Committee of the UMMC (Reference Number: 866.31), and written informed consent was obtained from all participants.
Questionnaire
Participants were individually interviewed by trained enumerators by using a detailed questionnaire that consisted of 2 parts: 1 on demographic characteristics and 1 on CAM use. The patients’ clinical profile, pathological tumor characteristics, and treatment modalities were extracted from the UMMC’s cancer registry. 26 In this particular study, CAM users were defined as patients who had been using one or more of the reported types of CAM (including nutritional supplements) since the diagnosis of breast cancer (within 3 months of diagnosis). 9 Patients who reported CAM use were requested to provide additional information on their patterns of CAM use, such as the type, the reasons or motivations for CAM use, consultations with doctors, and the perceived effectiveness of CAM use. The questionnaire was adapted from a questionnaire previously used by the Shanghai Breast Cancer Survival Study. 27 Some modifications were made to suit the local context, particularly in relation to the types of CAM use being investigated in this study (ie, traditional Indian Treatment, traditional Malay medicine, and TCM) by experts (physician, breast surgeon, and nurses) who went through the content and face validity.
This study collected the following demographic data: age; ethnicity; education level; marital status; working status; monthly household income; presence of comorbidities, such as diabetes mellitus, kidney and liver disease, heart disease, and hypertension; and alcohol use and smoking. The clinical data consisted of disease stage, menopausal status, oral contraceptive (OCP) use, and hormonal replacement therapy (HRT) use, which were extracted from the medical records of the patients.
Enumerators were given a list of patients who were undergoing surgery or adjuvant therapy for breast cancer. The patients were recruited from the oncology clinic or a surgical ward. Eligible patients were asked to give written consent before participating in this study. The involvement of multiethnic enumerators was very helpful in conducting the interviews because the patients were of different ethnicities.
Data Analysis
Data were analyzed using the Statistical Package for the Social Sciences (SPSS Inc, Chicago, IL) version 17.0. Descriptive statistics (frequencies and percentages) were used to present sociodemographic information and patterns of CAM use among breast cancer patients. The χ2 test was used to compare the use of CAM between users and nonusers with respect to sociodemographic characteristics.
Univariate analysis was performed using Pearson’s χ2 test or Fisher’s exact test for categorical variables and the Mann-Whitney test for continuous variables. To determine the independent factors associated with CAM use, a multivariable logistic regression analysis was used. Factors considered in the analysis were age, ethnicity (Malay and non-Malay), education level (primary and higher education), marital status (married or single), monthly income (<RM3500 or >RM3500), employment status (employed or unemployed), number of comorbidities (none, 1-2, or >3), alcohol consumption (ever or never), smoking status (ever or never), having attained menopause (yes or no), stage of breast cancer (1 and 2 and above, or >3 [advanced cancer]), OCP used (ever or never), and HRT used (ever or never). The P values of the analysis were considered statistically significant if P <.05.
Results
Characteristics of the Participants
During the study period, a total of 574 eligible patients were invited to participate in this study during their appointment with surgical or clinical oncologists before commencing any primary cancer treatment. Among these patients, 174 did not agree to participate in this study. Therefore, a total of 400 patients agreed to participate in the study.
The demographic characteristics of the participants are presented in Table 1. They were ethnically diverse, consisting of Chinese (n = 198, 49.5%), Malay (n = 122, 30.5%), and Indian (n = 77, 19.3%) patients. The average age (median ± interquartile range) at cancer diagnosis was 57.0 ± 16 years. Almost half of the patients had at least a secondary education (49.4%). The monthly household income for most of the participants was <RM3500 (n = 218, 61.9%). Most of the participants were married (n = 276, 69.0%), and many were in employment (n = 17, 42.8%). Also, the majority of the participants were nonsmokers (96%) and had never consumed alcohol (83.8%). The majority of the participants were postmenopausal (66.5%), had never used the OCP (72.6%) or HRT (90.7%), and had been diagnosed with early-stage breast cancer (73.5%). Many of the participants (56.1%) had at least 1 comorbidity, such as diabetes, hypertension, or hypercholesterolemia.
Demographic Characteristics of the Participants Based on Their CAM Use Status.

Abbreviations: CAM, complementary and alternative medicine; IQR, interquartile range.
Nonnormally distributed data are expressed as median (IQR).
Significantly different at P <.05.
Categorical data are expressed as percentage.
Patterns of CAM Use
There were significant differences in the proportions of CAM and non–CAM users by ethnicity, education level, and employment status (Table 1). For ethnicity, the difference was significant (P < .05). CAM use was also significantly higher among the participants who were educated (P = .017) and among those in employment (P = .014).
The sociodemographic factors related to CAM use among breast cancer patients are presented in Table 2. To improve statistical calculation, we recategorized some of the variables: ethnicity was decreased from 4 categories to only 2 (Malay and non-Malay), educational level was also decreased from 3 categories to 2 (primary education and higher education), and stage of breast cancer from 3 categories to 2 (stage 1, and stage 2 and above). From the univariate logistic regression, Malays (odds ratio [OR] = 2.47; 95% CI = 1.55-3.96), patients with secondary education (OR = 1.99; 95% CI = 1.17-3.38), and working women (OR = 1.68; 95% CI = 1.11-2.55) were more likely to be users of CAM. In addition, after adjusting for potential confounding factors (age, ethnicity, education level, marital status, monthly income, employment status, comorbidities, alcohol consumption, smoking, menopausal status, and stage of breast cancer), it seems that Malays were twice as likely to use CAM compared with non-Malays (OR = 2.09; 95% CI = 1.20-3.64). Also, participants who had 3 or more comorbidities were found to be more likely to use CAM compared with those without comorbidities (OR = 2.38; 95% CI = 1.14-4.98).
Association Between CAM Use and Sociodemographic Characteristics.

Abbreviation: CAM, complementary and alternative medicine.
Multivariate logistic regression was done. Odds ratio was adjusted for age, ethnicity, education level, marital status, monthly income, employment status, comorbid condition, alcohol consumption, smoking, menopausal status, and stage of breast cancer, with a P ≤.05.
Statistically significant.
Table 3 shows the pattern and prevalence of CAM use among the participants. Dietary supplementation (n = 107, 26.8%) was the most commonly used CAM, followed by spiritual healing or prayer practice (n = 40, 10%) and TCM (n = 32, 8%). The most commonly used supplements in this study were herbs and botanicals such as Sabah snake grass (n = 16), apricot seeds (n = 14), and Lingzhi mushroom (n = 8), as shown in Table 4. Vitamins and minerals were also commonly used as supplements (eg, vitamin B [n = 7] and vitamin C [n = 6]).
Pattern and Prevalence of CAM Use Among Participants. a
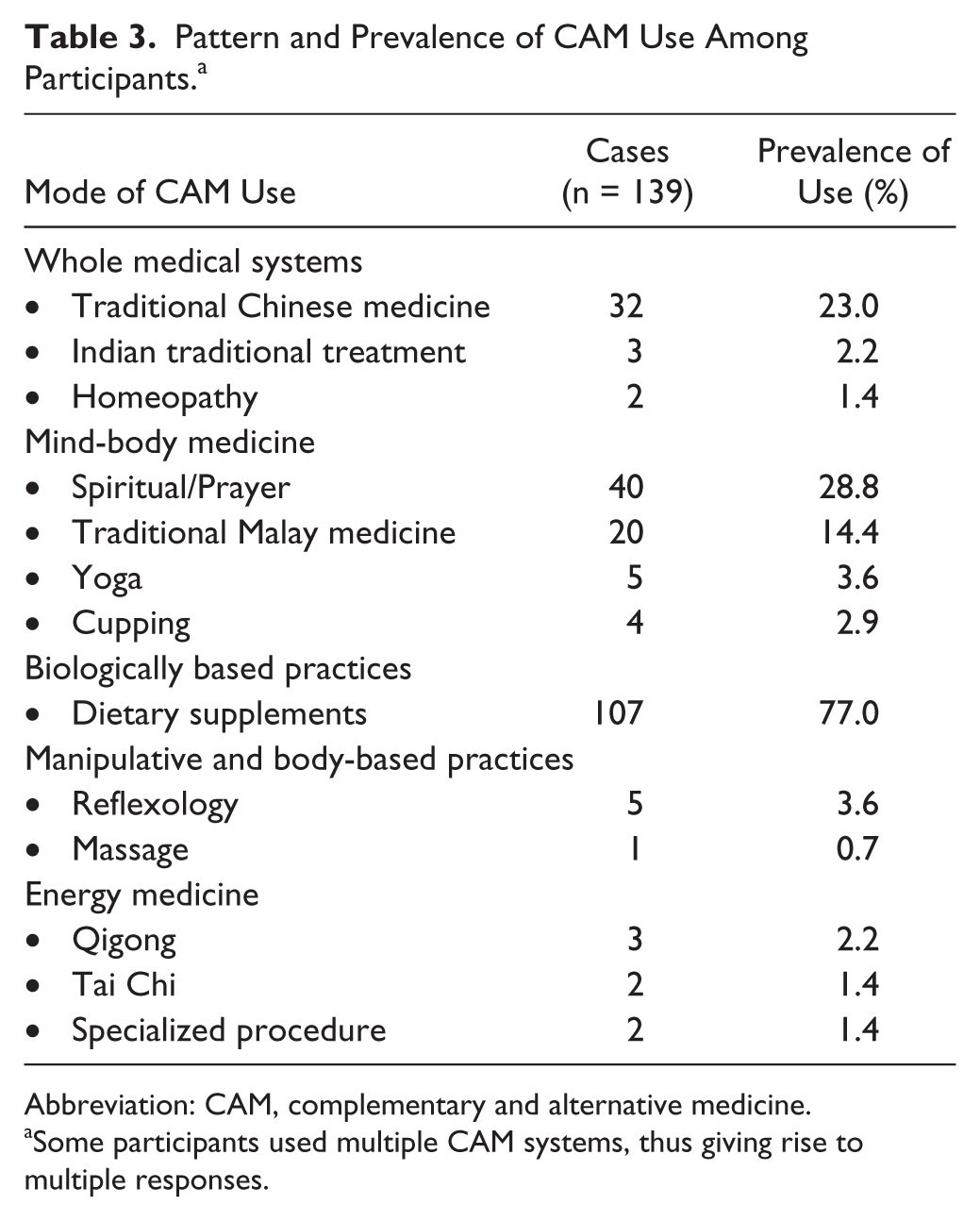
Abbreviation: CAM, complementary and alternative medicine.
Some participants used multiple CAM systems, thus giving rise to multiple responses.
Types of DSs Used by CAM Users. a

Abbreviations: DS, dietary supplement; CAM, complementary and alternative medicine.
Some participants used multiple dietary supplements, thus giving rise to multiple responses. Types of DSs were reported by the patients.
Table 5 shows the patterns of CAM use. The majority of CAM users (64.7%) used 1 type of CAM. Very few (1.4%) had tried a variety of CAM types. Most of the CAM users (73.1%) did not discuss their CAM use with their physicians, and among them only 47.1% provided a reason as to why they did not do so. The main reason for not informing their doctors about their use of CAM was that they felt that the doctor would not understand why they were using it (39%). The majority of CAM users (95.6%) claimed that they had not experienced any side effects when using CAM.
Patterns of CAM Use.

Abbreviation: CAM, complementary and alternative medicine.
Figure 1 shows the reasons for CAM use. The 2 most common reasons for CAM use were that it was recommended by family, friends, and survivors (n = 116) and that it helped them have a peaceful mind and calm (n = 20).
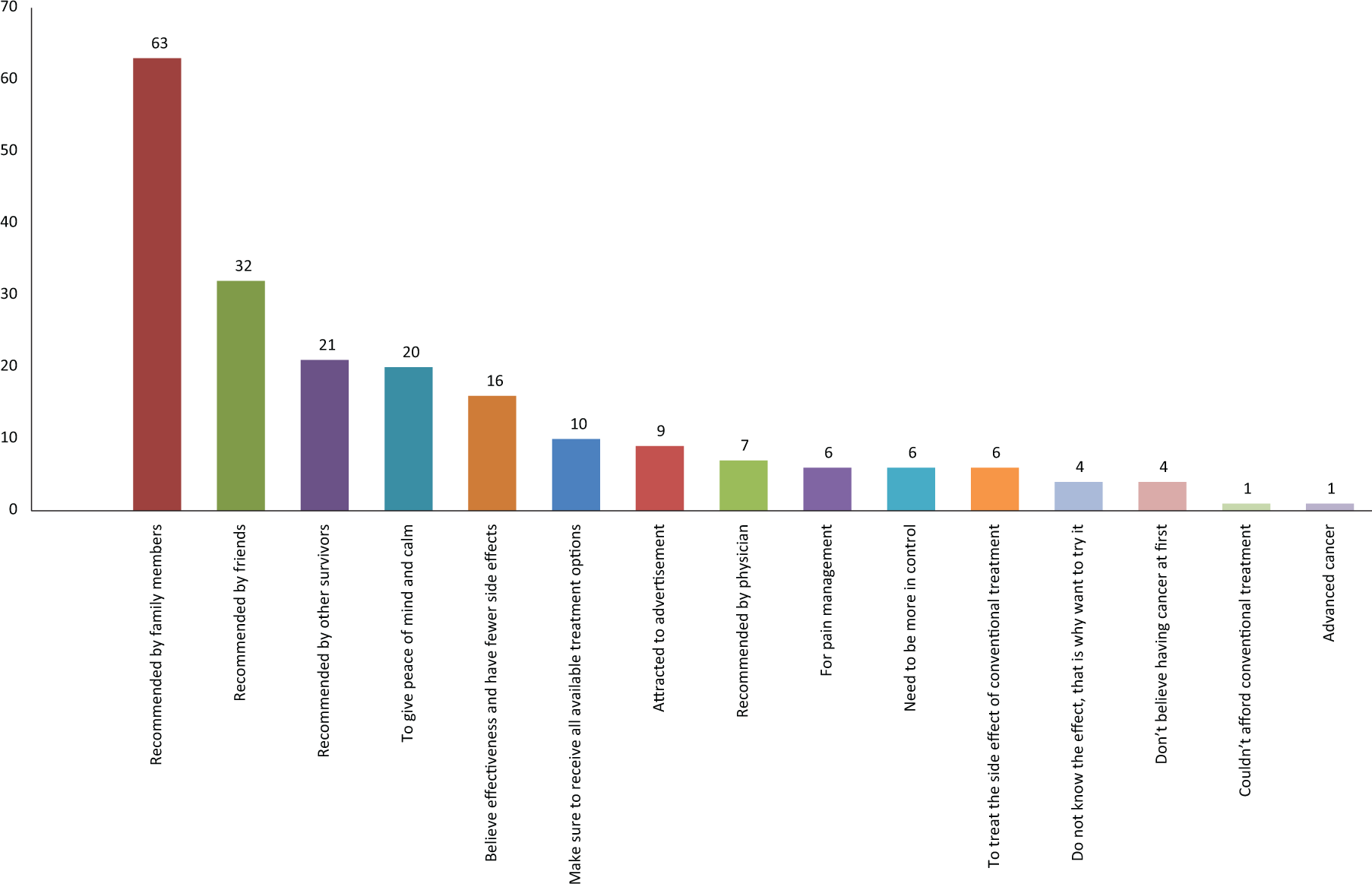
Reasons for complementary and alternative medicine (CAM) use (n = 98); multiple responses.
In this study, more than half of the CAM users (65.1%) perceived that the use of CAM was helpful, as shown in Figure 2. Figure 3 shows the perceived effectiveness of CAM use. Some of the participants believed that using CAM brought calm (n = 13), pain reduction (n = 12), and a reduction in the size of their lump (tumor) (n = 10).

Perceived effectiveness of complementary and alternative medicine (CAM).

Effectiveness of CAM use.
Discussion
The use of CAM in this study (34.8%) was lower than that seen in other CAM studies conducted in Malaysia. Most of those studies have reported a higher prevalence among patients with breast cancer.20,28,29 However, different studies from all over the world show that the percentage of CAM use ranges quite widely, from 20% to 84%.9,15,30 Unfortunately, a comparison of the observed prevalence of CAM in different studies was difficult because the period of data collection might have taken place during different trajectories of the patients’ cancer journey. Most of the studies were cross-sectional and hospital based like ours. However, data collection in previous studies involved patients who were undergoing or had completed conventional treatment,9,20,22,28,29 whereas in this study, data were collected from breast cancer patients prior to their receipt of conventional treatment. It is possible that participants may have underreported CAM use in this study, which may have contributed to the low prevalence observed. Underreporting of CAM use is common, and a previous study 31 has indicated that patients are uncomfortable in disclosing CAM use to their physicians and other health care professionals because of stigmatization and when CAM is not accepted socially. Also, a recent diagnosis (within 3 months) might be another causal factor for the low prevalence of CAM use identified in this study.
In this study, it was found that most of the participants used CAM because of they were influenced by their family members. This supports the findings of other studies conducted locally20,28,29 and in other countries.13,32,33 In fact, it seems that the decision to use CAM was mostly made by family members rather than by the patients themselves. This could be a result of the strong ties among family members in Malaysia.20,29 In this study, only 27% of the patients were willing to discuss their CAM use with their doctors. The reason for not disclosing CAM use to physicians was based on the participants’ assumption that physicians may perceive their reasons for using CAM to be irrelevant. In addition, they had never been asked about CAM use during a consultation with their physicians. This finding is similar to that reported in other studies, which have found that most patients are not willing to discuss CAM use with their physician.9,28 In one study, only 38% of the patients said that they disclosed their use of CAM to their physicians. 34 The patients’ presumption that their physician would give them a pessimistic response to the use of CAM might be hindering disclosure. Therefore, physicians and nurses should create an ambience that encourages patients to share their use of CAM. Transparent communication between the patient and health care professionals is of the utmost importance in reducing the chance of a negative impact on patients’ health occurring as a result of the toxicity caused by CAM itself or by interactions between CAM and conventional treatment. 35
Previous studies in Malaysia and in western countries have reported that dietary supplements and spiritual therapies are commonly used by breast cancer patients,20,28,29,36,37 and this finding is similar to ours. In this study, the most popular dietary supplements were vitamins and minerals as well as herbs and botanicals (Sabah snake grass products and apricot seed). Other chronic illnesses such as diabetes mellitus, hypertension, peripheral neuropathy, and dyslipidemia are associated with the use of dietary forms of CAM. 38 The high prevalence of dietary supplement use among breast cancer patients may be influenced by the beliefs of the participants that dietary supplements are a very good immunity booster and may potentially increase their QoL.15,37 Furthermore, the extensive availability of over-the-counter dietary supplements, media publicity about the benefits of supplementation, 39 and the recommendations about direct sale products given by friends or relatives may also have influenced the high use among the patients in this study. Religiosity and spiritual beliefs are important coping mechanisms for patients with breast and other cancers. Many of the CAM users in this study were Malays (43.9%) and Muslims, so this may be the reason for prayer and spiritual healing being the second most commonly used CAM method in addition to conventional treatment. This is in line with other studies that have reported that religious spiritual beliefs and practice influence the treatment of Malaysian breast cancer patients.20,40 TCM was the third most-used form of CAM and consists of herbal medicines and other forms of treatment, including acupuncture, massage (Tuina), exercise (qigong), and dietary therapy. In this study, there were 32 TCM users, among whom 26 (81%) were Chinese. Because the second highest ethnicity of CAM users in this study was Chinese, this probably explains why TCM was also a popular form of CAM among breast cancer patients in UMMC, after spiritual healing and prayer.
The results from this study also showed that patients with 3 or more comorbidities were twice as likely to use CAM compared with those who did not have comorbidities. This supports a previous study 41 that found that cancer patients with comorbidities are more likely to use CAM. This finding suggested that people who experienced many health problems were more likely to use alternative medicine for their general health because they may believe that CAM provides additional protection from the effects of treatments, the disease, or comorbidities.
When considering the above findings of this study, some limitations should be taken into account. First, despite our best efforts, there could still have been underreporting of CAM use, as seen in other studies. 31 This study showed that many were reluctant to disclose their CAM use to their physicians, and those who responded that they did not disclose CAM use to their physicians said that they felt the physicians would find it irrelevant and that the subject was never brought up in the consultation. This finding shows that CAM may not be a subject that is openly discussed by patients or physicians. Many cancer centers in the developed world have incorporated complementary practices such as integrative therapies within conventional treatment centers. 41 Innovative approaches to bring in patient values in discussions into mainstream practice are much needed in Asian countries where paternalistic medicine is still widely practiced. Second, the study sample was drawn from an urban population that contains a large number of Chinese, which may inadvertently have led to a higher proportion of TCM users among the study participants. Therefore, the findings might not reflect the overall situation in terms of the type of CAM used by breast cancer patients in Malaysia.
Although this study merely captures the prevalence of CAM use and the types of CAM used, it is the first study that has focused on CAM use during the initial period of diagnosis. This study also identified why CAM users do not disclose their use of CAM. This issue should be covered in medical education programs because it is important to enable patients to freely discuss CAM use during consultation at the diagnosis stage in order to enhance the success of the care that patients undergoing breast cancer therapies receive.
Conclusion
In this study, it was found that approximately one-third of patients in Malaysia’s ethnically diverse population used CAM before commencing any conventional treatment. This was particularly the case among Malay patients and among those who presented with 3 or more comorbidities. The most popular type of CAM among newly diagnosed breast cancer patients was dietary supplementation. Given that most CAM users did not disclose the use of CAM to their doctors, health care providers should pay special attention to their patients and discuss this matter with them. An exploratory study has revealed that alternative medicine is as accepted as conventional breast cancer treatment among patients in Malaysia and that this is a cause of advanced breast cancer presentation. 42 Furthermore, Malaysia has one of the highest breast cancer mortality rates in the region. Hence, to improve treatment effectiveness and adherence, and possibly breast cancer survival in Malaysia, it is important to determine the extent of CAM use at diagnosis in order to recommend best practice in relation to discussing CAM during the diagnosis consultation. It is, therefore, recommended that future studies should examine not only the prevalence of CAM use at different time points in the cancer journey, including during the survivorship period, but also the association between the uptake of CAM use and adherence to treatment. Most important, future research should investigate the impact of CAM on the quality of life and survival of breast cancer patients.
Footnotes
Acknowledgements
We would like to thank the doctors, nurses, technical staff, and hospital administration staff at UMMC for the daily administration of the Malaysian Breast Cancer Survivorship Cohort Study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was supported by a High Impact Research Grant (UM.C/HIR/MOHE/06) from the Ministry of Higher Education Malaysia. This study was also supported in part by the University Malaya Research Grant (RP057A-17SBS) from the University Malaya.
