Abstract
Introduction. Improved models of care are needed to meet all the support needs of people with cancer, which encompass psychological, emotional, physical, spiritual, sexual, occupational, social and existential needs. The aim of this article is to (a) evaluate short- and long-term impacts of using a whole person approach to support people with cancer on the Living Well with the Impact of Cancer Course (LWC) and (b) use these data to inform strategic decisions about future service provision at Penny Brohn UK. Methods. Longitudinal mixed-methods service evaluation (n = 135). Data collected included health-related quality of life (HRQoL) (FACIT-SpEx); Concerns (types and severity–MYCaW); lifestyle behavior (bespoke questionnaire), and participants’ experiences over 12 months postcourse. Results. Statistically and clinically significant improvements from baseline to 12 months in severity of MYCaW Concerns (n = 64; P < .000) and mean total HRQoL (n = 66; P < .000). The majority of MYCaW concerns were “psychological and emotional” and about participants’ well-being. Spiritual, emotional, and functional well-being contributed most to HRQoL improvements at 12 months. Barriers to maintaining healthy lifestyle changes included lack of support from family and friends, time constraints, and returning to work. Three to 6 months postcourse was identified as the time when more support was most likely to be needed. Conclusions. Using a whole person approach for the LWC enabled the needs of participants to be met, and statistically and clinically significant improvements in HRQoL and MYCaW Concerns were reported. Qualitative data analysis explored how experiencing whole person support enabled participants to make and sustain healthy lifestyle changes associated with improved survivorship. Barriers experienced to making health behavior change were also identified. These data then informed wider and more person-centered clinical provision to increase the maintenance of positive long-term behavior changes. Comparison of whole person approaches to cancer treatment and support and standard care are now urgently needed.
Keywords
Introduction
Globally, there is a continued increase in cancer incidence (14.9 million cases in 2013 vs 8.5 million in 1990). 1 Approximately 2 million people in the United Kingdom are living with cancer, and this number is projected to increase by approximately 1 million per decade from 2010 to 2040, resulting in an estimated 4 million people living with cancer by 2030. 2 People living with and beyond cancer have poorer well-being and health than the general population, and often feel need of further support at the end of medical treatment.2,3 The unmet needs of people with cancer have been highlighted as psychological, emotional, physical, sexual, occupational,4,5 social, 6 and existential.7,8 The increasing population of people with cancer with unmet needs, 9 the desire from patients to be more informed and involved with their own care,10,11 and the increased financial and operational challenges facing cancer services,12,13 all signal the need for these dimensions of a person with cancer to be routinely supported, facilitating self-management in order to bring about both short- and long-term improvements and economic benefits in patient care.
To expand effective models of cancer survivorship and support services requires robust evaluation data to understand how patients respond to these different models of care. Determining the most appropriate methods and tools to holistically evaluate all important aspects of these models can be challenging in a nonacademic/real-world environment, and needs to balance capturing key patient outcomes while not overly burdening patients or staff with paperwork. Furthermore, there has been a welcome shift from solely measuring clinical activity using randomized clinical trials, to using mixed-methods approaches and patient-reported outcome measures (PROMs) to capture patient experience and patient outcomes—approaches that recognize the complexity of evaluating clinical provision.14,15 It is the combination of these data that facilitates deeper understanding of how to improve service provision and patient outcomes.16-18
Internationally, there is increasing evaluation of the short-term outcomes of the models of supportive and integrative oncology.19-27 Few of these evaluations, however, extend to understand the outcomes and experiences of clients and patients over an extended period, such as 1 year or more, or the longer-term implications once they have stopped using these services. It is also of note that the design of a service evaluation is different to that of a traditional controlled study. As set out by Craig et al, 15 an evaluation can be used when there is a need to understand, for instance, more about how a service is working, who it is and is not working for and what level of outcomes are achieved with the service. In the United Kingdom, service evaluation is one of the recommended approaches to gathering essential data from a complex health intervention (eg, response rates, attrition rates, effect sizes, appropriateness of choice of outcome measures) prior to designing a study where the intervention may then be controlled against no intervention or compared against usual care. In addition, a service evaluation approach, using a mixed-methods design of obtaining both qualitative and quantitative information about experience of a service may provide a rich and rounded understanding of service user experience.
The Penny Brohn UK “Living Well with the Impact of Cancer” Course
Penny Brohn UK (PBUK), one of the leading integrative cancer support charities in the United Kingdom, developed the ‘Living Well with the Impact of Cancer’ course (LWC) using a “whole person approach” to supporting a person with cancer. The LWC is a motivational, facilitated 15-hour group intervention, which aims to promote long-term health and well-being and facilitate self-management of health for adults living with any type of cancer and their supporters. It involves a combination of physical, psychological, emotional and spiritual support using information, lifestyle advice and education, group support and activities, and self-help techniques. The LWC was designed by a team of health care professionals, including medical doctors, nutritional therapists, and psychotherapists to run alongside conventional treatment, at any stage of the cancer continuum.
As demand for PBUK services continues to grow on a national scale, this service evaluation was therefore deemed necessary in order for PBUK to be able to demonstrate to what extent the LWC can be measured and audited against set objectives, in a manner that captures clinically meaningful patient outcome necessary to represent the whole person model being used. These data are also critical for supporting the decisions of commissioning boards, and for informing effective service provision and future comparative effectiveness research design for PBUK and those currently involved in cancer survivorship.
This article therefore reports data from a longitudinal mixed-methods service evaluation. The purpose of the evaluation was to (a) evaluate the short- and long-term impact of the LWC and (b) use these data to inform strategic decisions about future service provision.
Methods
Intervention
LWCs are led by experienced, trained facilitators and are delivered as a 2-day residential or a weekly nonresidential course (2 hours over 7 weeks) at the National Centre, in Bristol, England. Clients are given scientific information and evidence, as well as a toolkit of techniques, for example, relaxation, meditation, mindfulness, and imagery, aimed at helping address physical, psychological, emotional, and spiritual health, as well as financial and relationship issues. Clients are encouraged to share their experiences with others in similar situations to reduce the sense of isolation and are also facilitated to set achievable “SMART” goals to focus their efforts to “live well” after leaving the course.
Procedure
Ethical approval was obtained from the research ethics committee at the University of Westminster and all participants provided written informed consent. All clients with a cancer diagnosis attending LWCs between August 2011 and January 2012 were invited to take part in the evaluation. Data were collected before the course, immediately after the course, 6 weeks after the course and at 3, 6, and 12 months after the course (see Figure 1) using online or paper-based questionnaire packs (according to participant preference). Measures were carefully selected to capture participant outcomes and experiences of all parts of the LWC.

The recruitment and flow of participants through the service evaluation, time points, and type of data collection.
Measures
To ensure that the whole person approach could be fully evaluated, a range of tools were selected that would capture all relevant outcomes for this holistic approach while aiming to not burden the participant. Measure Yourself Concerns and Wellbeing (MYCaW) is a brief validated PROM that quickly identifies and scores the severity of an individual’s 2 most pressing concerns, as well as scoring their overall well-being.10,11 MYCaW also collects qualitative data at follow-up detailing what other things are going on in the individual’s life that are affecting their health and what was particularly important about the center they visited. Functional Assessment of Chronic Illness Therapy Extended Spiritual questionnaire (FACIT-SpEx) is a validated psychometric PROM 28 that holistically assesses people’s management of chronic illness. A total health-related quality of life (HRQoL) score can be calculated, as well as scores for discrete aspects of quality of life, for instance, physical, emotional, functional, social, and spiritual well-being.
Customized evaluation questions assessed participant satisfaction with the course and the center by rating each item between 0 (worst) and 5 (best). Further questions captured basic data regarding diet, exercise, and stress management techniques, and assessed whether clients implemented lifestyle advice after the course. Finally, participant experience questionnaires using open-ended questions explored participants’ experiences of the LWCs and the effect of using the information and techniques provided, 6 weeks after a LWC. At 12 months post LWC, enablers and barriers to implementing and sustaining healthy lifestyle changes and the wider impact of the LWC on a person’s life were explored.
Statistical Analyses
Fully anonymized data were analyzed using IBM SPSS version 19. The analysis of each type of data is described in detail below.
Participant Characteristics
Participant characteristics were presented as percentages and any quantitative data from the customized evaluation forms were expressed as means and standard deviations. To identify any potential differences in MYCaW and FACIT-SpEx baseline scores between different groups of participants, data were stratified by the following variables and Mann-Whitney U tests were carried out—responders versus nonresponders; returners to PBUK versus nonreturners; came alone versus came with a supporter; primary versus metastatic disease. Kruskall-Wallis tests were also carried out to identify any baseline differences between age groups, cancer types, treatment stage, and additional life events affecting health. To determine the level of representativeness of the 12-month cohort, a comparison of variables between cohorts at baseline and 12 months was also carried out.
Patient-Reported Outcome Measures
FACIT-SpEx total and subscales scores, as well as MYCaW Concern, Well-being, and Profile scores (mean of concern and well-being scores combined) were calculated for each participant. Score changes relative to baseline were calculated at each relevant follow-up time point (see Figure 1). Nonparametric tests (Wilcoxon signed ranks) were used to determine statistical significance of change. Friedman tests determined if there were significant changes across all time points for MYCaW and FACIT-SpEx data. The percentage of participants with clinically relevant changes at 12-month follow-up were calculated. These were classed as at least a 1 point change for MYCaW; FACIT-SpEx scores were categorized according to Yost and Eton. 29
Qualitative Analysis
Qualitative data from MYCaW questionnaires were analyzed by MJP, EB, HS, and RJ using the qualitative analysis guidelines. 30 Qualitative data from the patient experience questionnaires administered at 6 weeks and 12 months were thematically analyzed by MJP to identify core themes around experiences of the course (6 weeks) and experiences over the subsequent year (12 months).
Results
Response Rates
Figure 1 details the flow of participants through the service evaluation; response rates gradually dropped over the 12-month follow-up period to 52% (n = 70). Fourteen percent of nonresponders had passed away at 12 months, the rest (n = 82) were sent a very brief questionnaire to understand why they did not return questionnaires. Twenty responses were received. Predominant reasons included “forgot” (23%), “too busy” (11%), “lost the questionnaire” (11%), “don’t want to be reminded of cancer experience” (6%), and “too ill” (6%).
Participant Characteristics
Table 1 shows the participant characteristics at baseline and 12 months later. Briefly, participants were primarily female (82.3%), mean age 53 years (range 27-84 years). 21 cancer types were represented, the majority comprising breast, bowel, prostate, and gynecological. The majority of participants (58%) were undergoing primary treatment for cancer. Forty percent were 3 months or less since the start of their treatment, 33% were 3 to 12 months, 24% were 1 to 5 years, and 3% were more than 5 years since the start of their treatment. Participants with metastatic disease had a significant difference in physical well-being at baseline compared with participants without metastasis (17.15 vs 21.28, P = .004). No other significant baseline differences between variables were found.
Participant Characteristics at Baseline and 12 Months Postcourse.
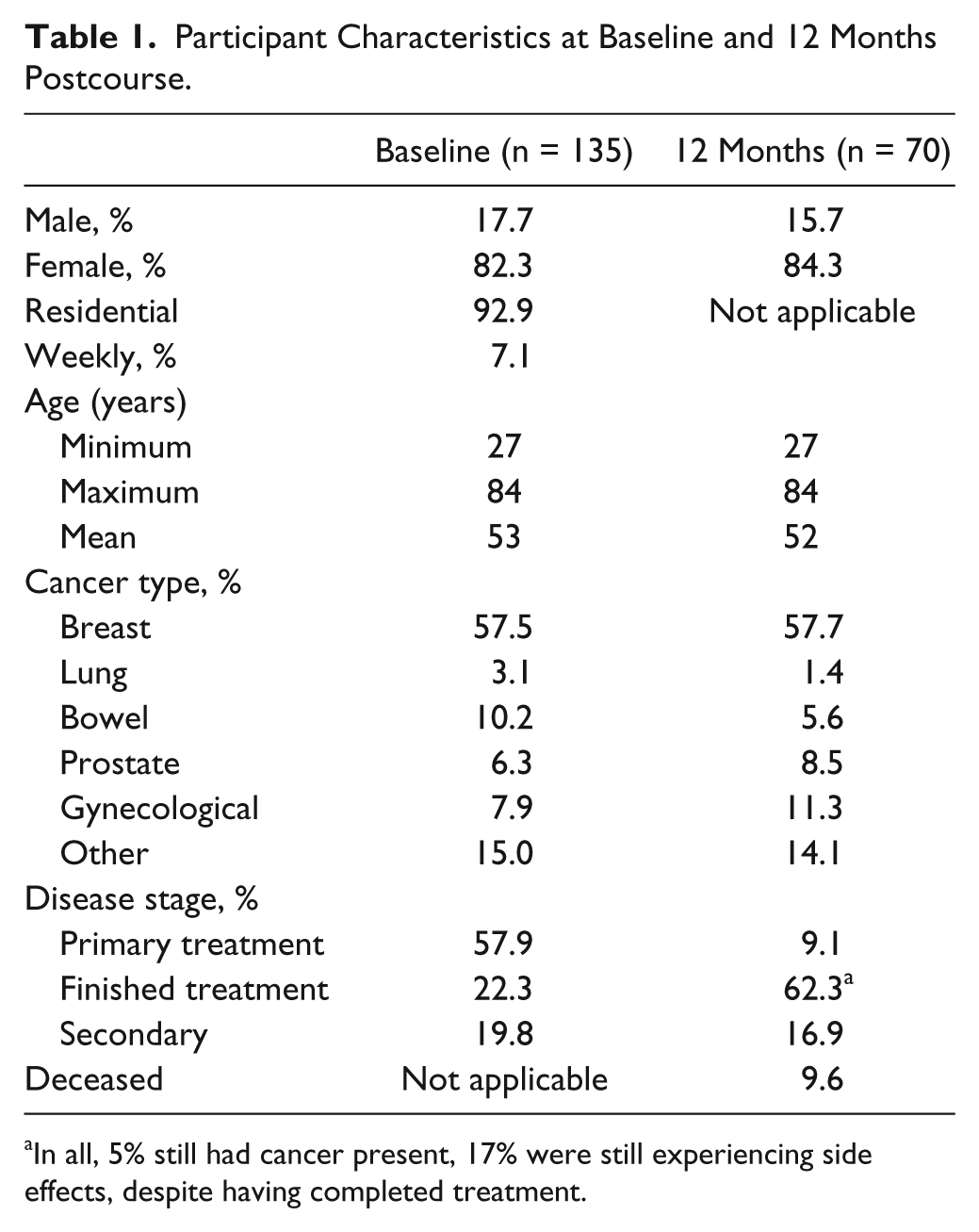
In all, 5% still had cancer present, 17% were still experiencing side effects, despite having completed treatment.
We further compared the data from participants left at 12 months to the whole group of participants at baseline (see Table 1). There was a significant reduction in the number of participants having primary treatment at 12 months compared with baseline. We could not find any other significant differences between the data from participants at 12 months and at baseline.
MYCaW Concerns
MYCaW concerns at baseline (n = 128 Concern 1, n = 123 Concern 2) were coded according to Jolliffe et al. 11 A total of 45% of concerns reported were in the S1: “psychological and emotional” category that has 13 types of concerns. The most commonly reported concerns here were family problems and relationships, emotional problems, adapting and coping, and psychological issues. 20% of concerns were in Category S4: “Concerns about Well-being,” which has 6 concern types. Here concerns focused on general well-being, nutrition, exercise, and relaxation. Sixteen percent of reported concerns were in S2: “physical concerns,” which included physical problems in general, concerns about recurrence and spread, concerns with pains and aches, and poor energy levels.
Twelve percent of concerns were in Category S5: “practical concerns” relating to work and finances, and 7% of pressing concerns were in Category S3: “hospital cancer treatment concerns” and related almost exclusively to aspects of cancer treatment in general.
MYCaW Scores
Mean scores at baseline are shown in Table 2. For both Concerns 1 and 2, statistically significant mean improvements were reported directly after the LWC (P < .000, in each case), which continued to improve throughout the 12-month follow-up. Mean well-being scores were statistically significantly improved at all time points relative to baseline. The biggest mean wellbeing score change was observed immediately after the course (0.86, P < .000), mean change at 12 months was 0.63 (P = .005). Significant improvement across all time points (P < .000) for Concern 1, Concern 2, Well-being and Profile scores were detected (Friedman test). Clinically relevant improvements after 12 months are detailed in Table 2.
Changes in MYCaW and FACIT-SpEx Scores Over 12 Months Postcourse. a
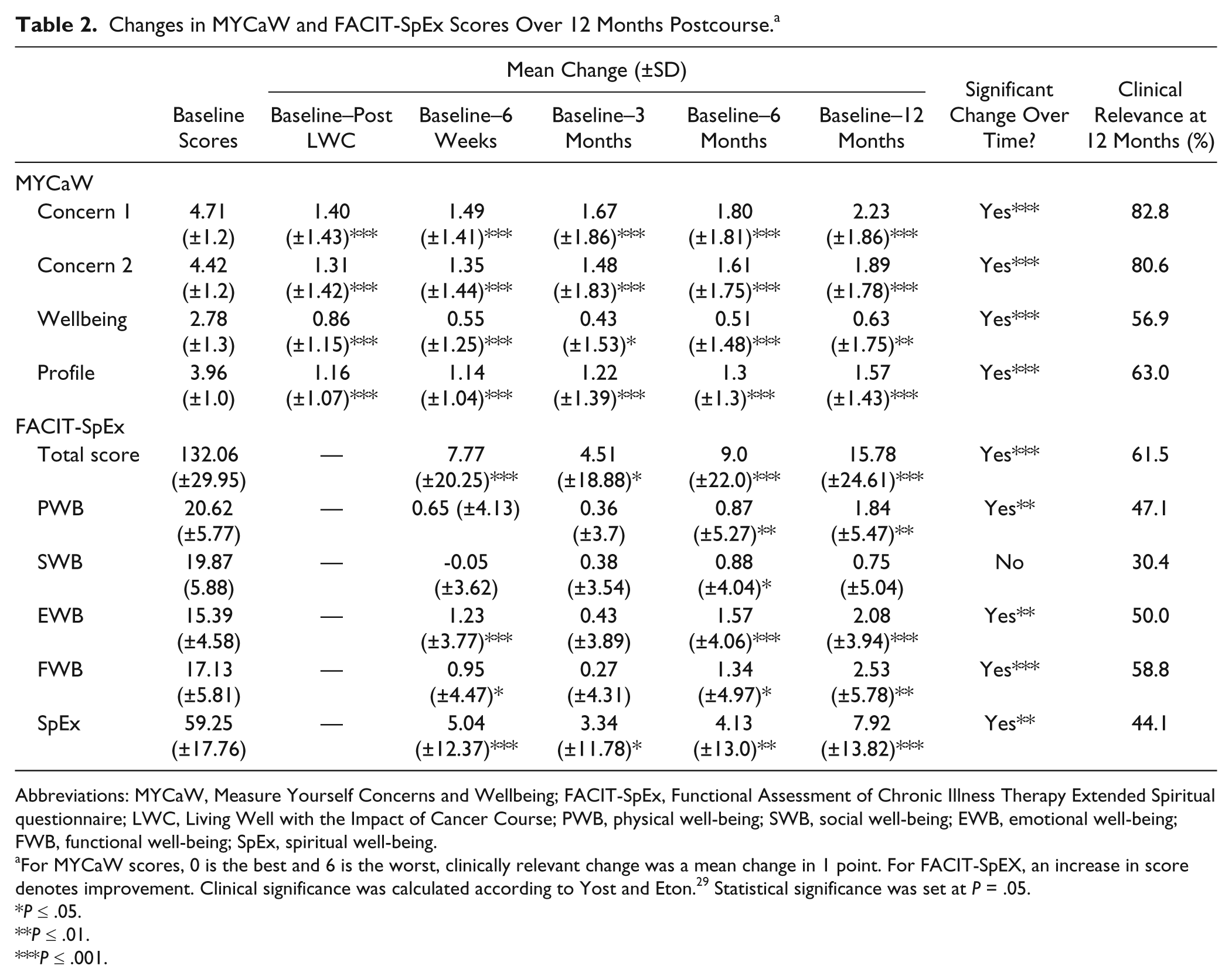
Abbreviations: MYCaW, Measure Yourself Concerns and Wellbeing; FACIT-SpEx, Functional Assessment of Chronic Illness Therapy Extended Spiritual questionnaire; LWC, Living Well with the Impact of Cancer Course; PWB, physical well-being; SWB, social well-being; EWB, emotional well-being; FWB, functional well-being; SpEx, spiritual well-being.
For MYCaW scores, 0 is the best and 6 is the worst, clinically relevant change was a mean change in 1 point. For FACIT-SpEX, an increase in score denotes improvement. Clinical significance was calculated according to Yost and Eton. 29 Statistical significance was set at P = .05.
P ≤ .05.
P ≤ .01.
P ≤ .001.
FACIT-SpEx Scores
The mean baseline FACIT-SpEx scores and change in mean scores over the 12-month period are detailed in Table 2. Briefly, statistically significant improvements in mean total HRQoL scores were reported at all time points compared with baseline although less so at 3-month follow-up (P < .000 6 weeks, 6 and 12 months; P = .037 at 3 months). Spiritual well-being was significantly improved at every follow-up, emotional and functional well-being scores were statistically significantly improved at all time points except at 3 months. Together these 3 domains contributed most to the improvements in HRQoL (see Table 2). Physical well-being did not significantly improve until 6 months after the course (P = .009), then remained significantly improved at 12 months (P = .002). Significant improvements in social well-being scores were only observed at the 6-month time point (P = .029). Friedman tests for the overall effect of time were significant for total HRQoL and all subdomains except social well-being (Table 2).
Clinically Relevant Changes
The large percentage of participants with clinically relevant improvements in MYCaW and FACIT-SpEx scores are detailed in Table 2.
Only 7.8% and 6.5% of participants had clinically relevant decreases in MYCaW Concern 1 and 2 scores (respectively) at 12 months—indicating the concern had got worse. A total of 23% (n = 14) of participants experienced a clinically relevant decrease in MYCaW Well-being scores. Of these 14 participants, 5 also reported a clinically relevant decrease in their total FACIT-SpEx scores (which were most likely to occur in the physical and social well-being subdomains) and 5 reported no change in their HRQoL.
Participant Satisfaction
Participants (n = 126) rated items relating to the center and the LWC using customized evaluation forms. Participants were highly satisfied with how the course met their needs and expectations (4.5/5). All items relating to the course and center had a mean rating of over 4/5 except the session on financial welfare, which had a mean rating of 3.7/5.
Impact of LWC
Qualitative data were collected at 6 weeks follow-up, on what participants had found particularly helpful or unhelpful on the course. Thematic analysis of 111 responses (65%), revealed 5 themes: “sharing with others,” “the course in general,” “nutrition and food,” “the doctors’ talk,” “relaxation, meditation, and self-help.”
. . . thank you to the Penny Brohn centre for getting me through the cancer and the treatment, and come out the other side a better informed person about the condition, what to expect, the support from others going through the treatment and survived, and to change my life attitudes and take time to enjoy life and recognise what is important and what’s not important. (LWC participant)
Further data showed that 6 weeks after attending the LWC, 84% of participants reported improving their diet, 57% were using self-help techniques for relaxation and stress reduction, 56% of participants had improved their physical activity, and 49% felt that their close relationships were improved.
Understanding Why Some Participants Needed More Support
To further understand why some participants needed more support than others to address their long-term needs, an in-depth review of the data for these participants was carried out (n = 75, 58%). On average those participants who did come back for more support returned 4 times in the 12 months (SD ±5, range 1-23) to attend other courses or receive individual complementary therapy sessions, for example, counselling. Baseline scores for MYCaW and FACIT were more likely to be worse than the nonreturners, but this was not significantly so. There was, however, a greater degree of improvement in their MYCaW Concern 1 scores (n = 39, P = .011), Concern 2 scores (n = 38, P = .002) and in their HRQoL scores (n = 40, P = .007) compared with nonreturners. Qualitative data at 12 months post LWC revealed that participants predominantly wanted a refresher to motivate them to keep up the changes implemented, to get more practical advice and resources, and to clarify information they first received on the LWC.
I seem to fall back into old habits and require a return to PB to keep me on track (every 6 months) . . . (LWC participant)
Barriers to Making Changes
All participants at 12 months post LWC were asked what challenges were experienced in making and sustaining changes (n = 69; 92% response rate).
Two-thirds of respondents reported challenges specifically around sustaining the dietary changes. A common barrier was the lack of social support from family and friends, who did not understand why the participants wanted to make changes.
I feel it is very difficult trying to get family and friends to try to understand how important it is for me to eat and live as healthy as it is possible. They don’t believe in special healthy eating, sometimes I feel as though they feel I am over the top in my wanting to eat healthy and sometimes scoff at my decisions. They don’t believe in it making any difference to my having had cancer or trying to prevent it coming back. Yes it is very hard making changes from living on everyday foods for years . . . (LWC participant)
Key themes also emerged relating to the time needed to self-care, returning to work and shouldering family responsibilities, highlighting a key stage in cancer survivorship where participants need targeted support.
I do sometimes find it difficult to fit time for meditation and relaxation into my daily routine especially when the kids are at home with me all day. (LWC participant)
Being unable to remember all the information from the course (often due to side-effects of treatment affecting memory) was also a barrier, as was associating some of the less healthy eating habits, such as excessive alcohol, cakes, and caffeine, with reward or comfort that they did not want to give up.
. . . I find it hard not to have a glass or 2 [of wine] most evenings and it is a real challenge to me to monitor and reduce this, it is such a pleasure and a comfort and a reward! (LWC participant)
Participants also described strategies that they had implemented to help them achieve long-term changes. Practical suggestions included: schedule meditation in diary once back to work, introduce changes slowly, do short meditation sessions not long ones, cook in bulk, and freeze food. Other suggestions involved having more support, for example, having regular contact with PBUK via phone appointments or returning for a refresher course, using a personal trainer as a motivator, keeping in contact with others from the LWC. Finally, having more realistic expectations of self were reported as helpful.
Combining Quantitative and Qualitative Data to Inform Future Service Provision
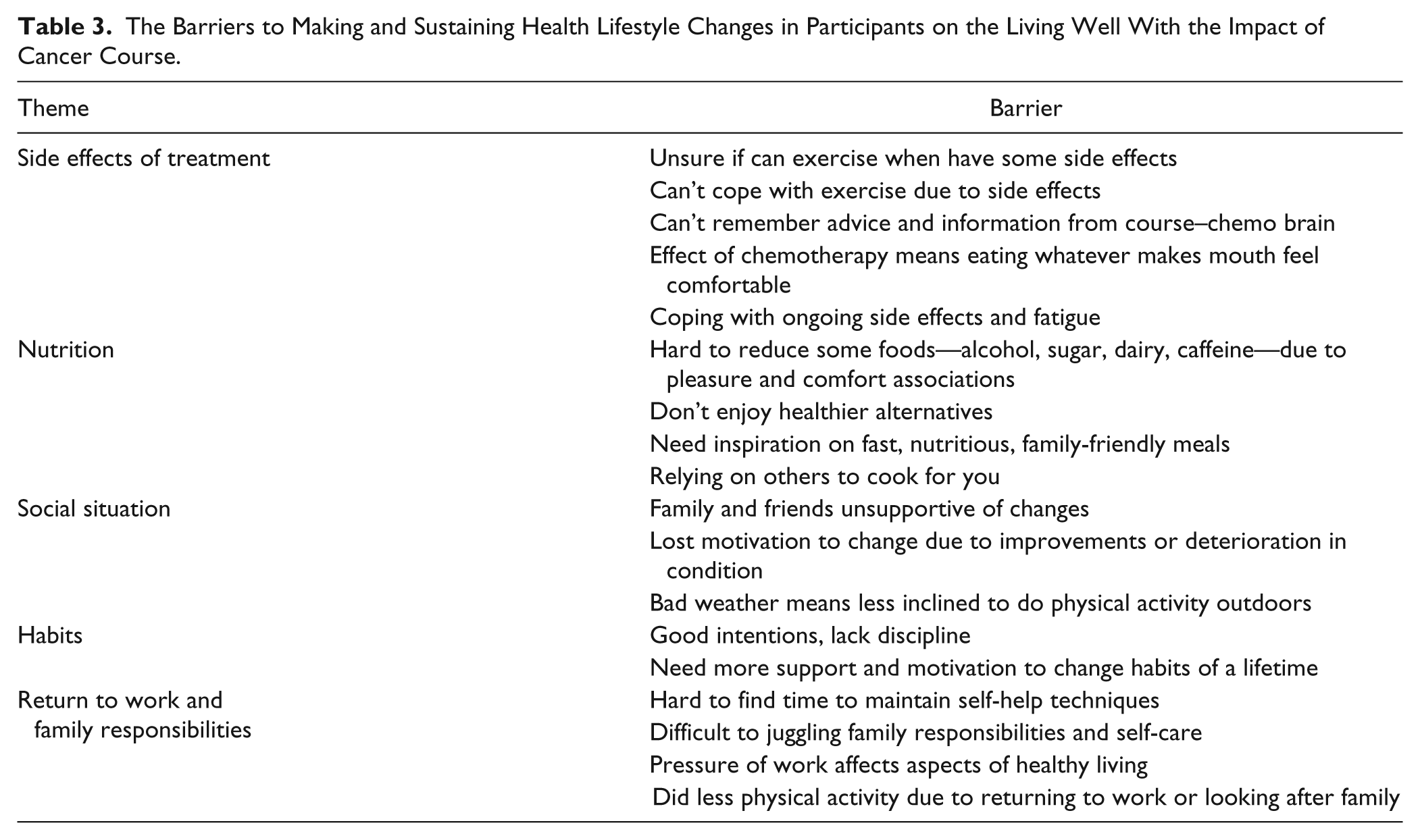
Because all quantitative data at 3 months post LWC had a noticeable dip in the level of improvement, the themes from the qualitative data were mapped chronologically over the course of the 12 months. Different stages in the participants’ journeys emerged. The first 6 weeks after the LWC were generally used to “experiment with and implement” information and techniques from the course. A small group of patients experienced transformations that left them empowered, doing activities they always “meant” to do, with better personal relationships and navigating the medical system with more confidence—they appeared to be thriving. From 6 weeks to 3 months onward, the majority of participants reported barriers to sustaining initial changes (Table 3), which led to 2 broad trajectories. Some participants could not consistently maintain a positive change, but reported knowing what they needed to do. When these participants realized that they were not maintaining their lifestyle changes as well as they wanted to, they were able to renew their efforts to make changes without further support from PBUK. For a smaller group of clients, however, the barriers they experienced felt insurmountable without further support and they often reported resorting to “old habits.”
The Barriers to Making and Sustaining Health Lifestyle Changes in Participants on the Living Well With the Impact of Cancer Course.
Discussion
The first aim of the evaluation was to scientifically document how well the LWC meets and supports participants’ needs, and participants gave an average rating of 4.5/5 for this. A combination of tools and questions were required to ensure that all aspects of the whole person approach were evaluated, while minimizing the burden on participants. MYCaW was used to map participants’ most pressing concerns, the most common being psychological and emotional. Many participants were also concerned about self-management and wellbeing, for example, nutrition and physical activity. After 6 weeks, participants reflected on what was helpful about the course, which led to identifying 5 key themes (eg, nutrition and food, information from medical doctor, sharing with others, meditation and relaxation, the course in general), which correspond to some of the themes previously identified as helpful in other supportive and integrative oncology settings.8,31 Together these data confirmed the value of using a whole person approach as a model for the LWC course content, to enable the range of concerns and needs of participants to be fully met. The many effects of providing a combination of physical, psychological, emotional, and spiritual support using information, lifestyle advice and education, group support and activities, and self-help techniques on cancer survivorship are reviewed here. 32 Furthermore, participants were given a voice in this evaluation by using MYCaW to let them freely nominate and rate their “concerns,” which provided data that would not normally be captured using standard outcome measures of HRQoL used in cancer research. This is important as research suggests that identifying and meeting patients’ needs can influence outcomes associated with HRQoL (eg, Hussan et al 33 ). We have discussed the wider implications of the need for careful selection of outcome measures when working in a holistic setting previously. 11 Internationally, holistic models of care are being used by many service providers. 19 In the United Kingdom specifically, supportive care alongside the NHS (Naitonal Health Service) care pathway is increasingly understood to be valued by patients, as exemplified by the growth of such provision in the charity and statutory sector. 34
Both MYCaW and FACIT-SpEx showed statistically and clinically significant improvements in mean scores, which remained for at least 1 year after attending the course (see Table 2). The baseline scores and changes in Concern and Well-being Scores for MYCaW were similar to other reported scores internationally.10,22,23
It is important to highlight that this evaluation showed psychological and emotional concerns to be at the forefront of participants’ minds at the start of the course, and this is correlated with improvements in emotional well-being (FACIT-SpEx) and psychological and emotional concerns (MYCaW) at 12-month follow-up. Other studies by ourselves and other UK- and US-based cancer centers have also shown psychological and emotional concerns and concerns with own well-being to be the most predominantly reported concerns.10,22,23 A large proportion of participants in this evaluation were undergoing physical treatment, hence it may be anticipated that physical concerns would be more frequently reported. The physical side effects, however, are most likely to be addressed within the hospital while the participant is undergoing treatment, yet there still exists a lot of variance in the amount and quality of self-management information and advice that is given to patients while undergoing treatment. There is also a lack of consistent high-quality psychological and emotional support within the current biomedical system. It is likely that when a patient is given the opportunity to express their most pressing concerns, that these data reflect the wider impact of cancer on the whole person, not just the physical symptoms and side-effects.
Functional well-being showed statistically significant improvements over time, 59% of participants’ improvements being clinically significant. These data relate to a person’s ability to work, enjoy life and activities, accept their illness, sleep well and feel content with their quality of life. LWC participants often mention that they want to return to “normal” and these functional well-being data match the qualitative reports from participants on how they benefited from the course. Similarly in the emotional well-being domain there was significant improvement over time, and 50% of participants’ improvements were clinically relevant. These data relate to the level of sadness, worry about the disease and dying, a person’s ability to cope with the illness and their level of hope. Again we noticed that there were clear associations in the qualitative data and the improvements reported on the emotional well-being domain.
Interestingly, spiritual well-being on FACIT-SpEx was the only domain to significantly improve at every time point and made a noticeable contribution to the overall HRQoL improvement for participants (see Table 2). Improved spiritual well-being further confirms how important whole person approaches to care are in addressing issues such as meaning, purpose, connectedness, and sources of joy in life. Yet these outcomes, unlike other well-being domains we measured, are not routinely monitored, despite increasing research showing spiritual well-being to be a key component in total HRQoL and in managing the negative impact of cancer treatment.8,35,36 Social well-being was the only domain that did not show statistically significant improvement over time, although there were a group of participants (30%) who has clinically relevant improvements at 12 months. This domain related to a person’s communication with their family, the level of support from family and the level of acceptance of the disease by family and friends. In the qualitative data, the lack of support from family and friends was found to be one of the biggest barriers to making and sustaining lifestyle changes. The LWC is open to supporters and carers as well, and it may that the 27% of participants who brought a supporter with them and had a shared experience, were more likely to score improvements in social wellbeing. These data and data from others37-39 highlight the importance of including the main supporter or carer in the process of supporting a person with cancer.
Although there were significant improvements between pre- and postcourse scores that are difficult to attribute to other causes, these quantitative data do not prove that the LWC directly caused the sustained improved quality of life, as a control group was not part of the service evaluation design. It is noted that a larger proportion of participants had completed their treatment at 12-month follow-up (compared with baseline) and some participants had passed away, thus one would anticipate a natural improvement in physical well-being over the course of time. While this may account for some of the improvement in HRQoL scores, we suggest that it may not account for it all. Of the 67% participants who completed primary treatment at 12-month follow-up, 22% still had side effects or were living with treatment-resistant cancer. A further 16.9% of participants had metastatic cancer (Table 1) and finishing treatment is unlikely to explain the degree of improvement in spiritual well-being. Furthermore, physical well-being had the highest proportion of clinically relevant deterioration at 12 months. When interpreting the quantitative scores with the qualitative experiences of participants, it becomes more apparent that participants largely attribute the improvements in HRQoL and MYCaW scores to attending the LWC. The LWC improved the participants’ abilities to make positive informed choices on self-management and behavior changes once they returned home and was reported to have facilitated transformational change in some cases (where quality of life improves beyond what it was before the diagnosis of cancer)—similar to reports by Skeath et al. 40 Supporting participants with the knowledge, tools, and techniques to make appropriate lifestyle decisions were also key to sustaining the initial benefit experienced on the LWC. At the time of this evaluation, there was no clear service provision to continue to support clients unless they returned to the National Centre, which for many participants was not feasible. The combined data, however, had highlighted a critical time-point for supporting clients to sustain positive long-term changes and the potential negative impact on their HRQoL if this support was not accessible.
The second aim of the evaluation was to provide data to inform strategic decision making for expanding service provision. Capturing a fuller picture of the experiences of LWC participants, the range of impacts of the LWC and which barriers could be addressed, was essential to evolve future service provision. After thorough discussion of the service evaluation data with all key stakeholders in PBUK, and armed with the greater depth of understanding of the client experience that this evaluation provided, in 2014, PBUK designed a package of follow-up support to more effectively meet the differing support needs of their clients. Follow-up consists of a supportive phone call at 6 weeks, and light touch support (eg, information reminders on email), which provides new recipes, videos of relaxation techniques taught on the course, signposting and reviews of books and other helpful resources. This particularly caters for PBUK clients who find that they cannot recall all the information while on the LWC or just need a bit motivation to maintain their lifestyle changes. Clients who feel that they need a greater level of follow-up support to overcome barriers, are offered one-to-one telephone or face-to-face appointments with an Integrative Doctor or Nutritional Therapist, and can attend a Follow Up day or join a PBUK Community Group (currently running at the National Centre and in the north of England). The evaluation data also informed PBUK as to what types of additional support to provide at the National Centre to meet clients’ needs. Support available includes a Treatment Support Clinic for people preparing for, undergoing or recovering from cancer treatment, Wellbeing Days, counseling (telephone or face-to-face), individual complementary therapies (eg, massage, reflexology), healthy cookery demonstrations and group physical activity sessions (eg, Qigong, Yoga, Nordic Walking).
As analysis of the data for this service evaluation was carried out, it became clear that collection of key data about comorbidities, types of biomedical treatment and social and economic data needed to be collected routinely and be easily accessible implemented for analysis alongside PROMs data. This evaluation therefore led to the implementation, in 2014, of an improved core outcomes set to monitor the performance of LWCs. To ensure the quality of LWCs as they are implemented in locations around England, Wales, and Scotland, these evaluation data are used as “benchmark” standards that are routinely achievable. Being able to audit course performance is essential for further commissioning of LWCs and also for reporting benefits to insurance providers. From a wider research and evaluation perspective these data have also established the degree of changes in outcomes that are possible, the proportion of clinically relevant data that is achievable, and the breadth of outcomes to capture when evaluating a holistic, whole person approach.
The data we report here are limited in their generalizability to other cancer support organizations due to not having a control group to determine what level of change in concerns, well-being, and HRQoL occur without the LWC. However, there exist much data that can be useful to other organizations. We aimed to understand how participants experienced the whole person approach to supporting people with cancer. We have determined the core elements that make the LWC a success in the eyes of the participants and what serves to hinder positive changes to health behavior. These core elements can be translated into existing service provision in different cancer support organizations. Furthermore, we have shown the importance of collecting both quantitative data and qualitative data to provide contextual insight into the changes in outcomes that participant’s score. This is especially important when capturing data from a complex intervention when it is likely that there is no single element of the intervention that is “causal” in nature. We therefore hope that this evaluation provides valuable insights and data that can be translated into well designed, accurately powered, patient-centered, comparative effectiveness studies of complex health interventions in integrative oncology.
Conclusions
Using a whole person approach on the LWC has immediate and long-term beneficial impacts for participants in their HRQoL, particularly with spiritual, emotional, and functional well-being. Qualitative data has identified important information about the positive transformative experiences that some patients had following attendance at a LWC, as well as a number of barriers to sustaining change and ways of addressing these. Using carefully selected outcome measures and a mixed-methods approach was critical in determining key stages in the cancer continuum when participants needed more support to sustain positive lifestyle changes. All these data were translated into a package of follow-up support to efficiently support the ongoing needs of clients at PBUK. These data provide the necessary information to accurately design a comparative effectiveness study to further understand the level of clinical benefit when using the whole person approach for supporting people with cancer.
Footnotes
Acknowledgements
Participants of the evaluation attending Penny Brohn UK, Wendy Freeman for data administration, data input volunteers and services staff at Penny Brohn UK.
Authors’ Note
This article is in memory of Lisa Joseph.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was partly funded by the James Tudor Foundation.
