Abstract
Ganoderma lucidum spore (GLS), an over-the-counter herbal supplement, is widely used by cancer patients in China. Although preclinical studies have shown it to be safe, complete safety data on GLS is still lacking. In this article, we report 5 cases of gastrointestinal cancer that were treated with GLS plus multiple strategies between 2010 and 2011. These patients presented with increased levels of the serum tumor marker CA72-4, one of the most valuable markers for monitoring therapeutic response in patients receiving gastrointestinal cancer treatment, after oral ingestion of GLS twice a day for 1 or 2 months. Interestingly, CA72-4 rapidly returned to normal levels when the patients discontinued the supplement and no change in clinical symptoms accompanied the CA72-4 surge. Taking into consideration that the underlying mechanism of this reaction is obscure, we suggest that additional studies are urgently needed and GLS be used with caution in cancer patients.
Introduction
Due to the limitations of conventional cancer treatment, large numbers of cancer patients turn to complementary and alternative medicine,1,2 most commonly traditional Chinese medicine (TCM). 3 Ganoderma lucidum (Figure 1A), also known as Lingzhi or Reishi, is a species of basidiomycete. It was recorded in the oldest Chinese materia medica, Classical Pharmacopeia of the Heavenly Husbandman (206 BC-8 AD) and has been used in China for more than 2000 years. 4 It is well known as the “mushroom of immortality,” widely used in China and many Asian countries to promote longevity, maintain vitality, and treat multiple diseases, including gastrointestinal cancer.5-8 Since the 1980s, its anticancer properties, such as cytotoxicity, immunomodulation, and the ability to suppress angiogenesis and induce apoptosis, have been investigated.7-10

Fruiting body of Ganoderma lucidum (A) and Ganoderma lucidum spore (B).
As an over-the-counter supplement, this fungus has been commercially processed into many products,11,12 one of which, Ganoderma lucidum spore (GLS; Figure 1B), is becoming increasingly popular among cancer patients in Asian countries.13,14 Clinical observations of GLS have shown that it may be effective in treating gastrointestinal cancer with few adverse effects 15 : animal studies demonstrate that long-term toxicity in rats only occurs at dosages higher than 5.40 g/kg, which corresponds to 60 times of the clinical human dosage. 16 However, the clinical safety evaluation of this remedy is far from sufficient.
In the current report, we describe 5 cases of gastrointestinal cancer. Each of these patients presented with a surge of the serum tumor marker CA72-4 after taking GLS; however, no disease progression was observed. Although the underlying mechanism of this reaction is obscure, our cases indicate that additional studies are urgently needed since a consistent rise of CA72-4 is generally thought to be indicative of disease progression17,18 and physicians would conventionally shift the treatment for these patients.
All GLS administered to these patients was processed using standard quality controls with a composition ratio of 1:4 of Ganoderma lucidum sporophore and broken GLS. The high performance liquid chromatograms (HPLC) of the samples are shown in Figure 2.
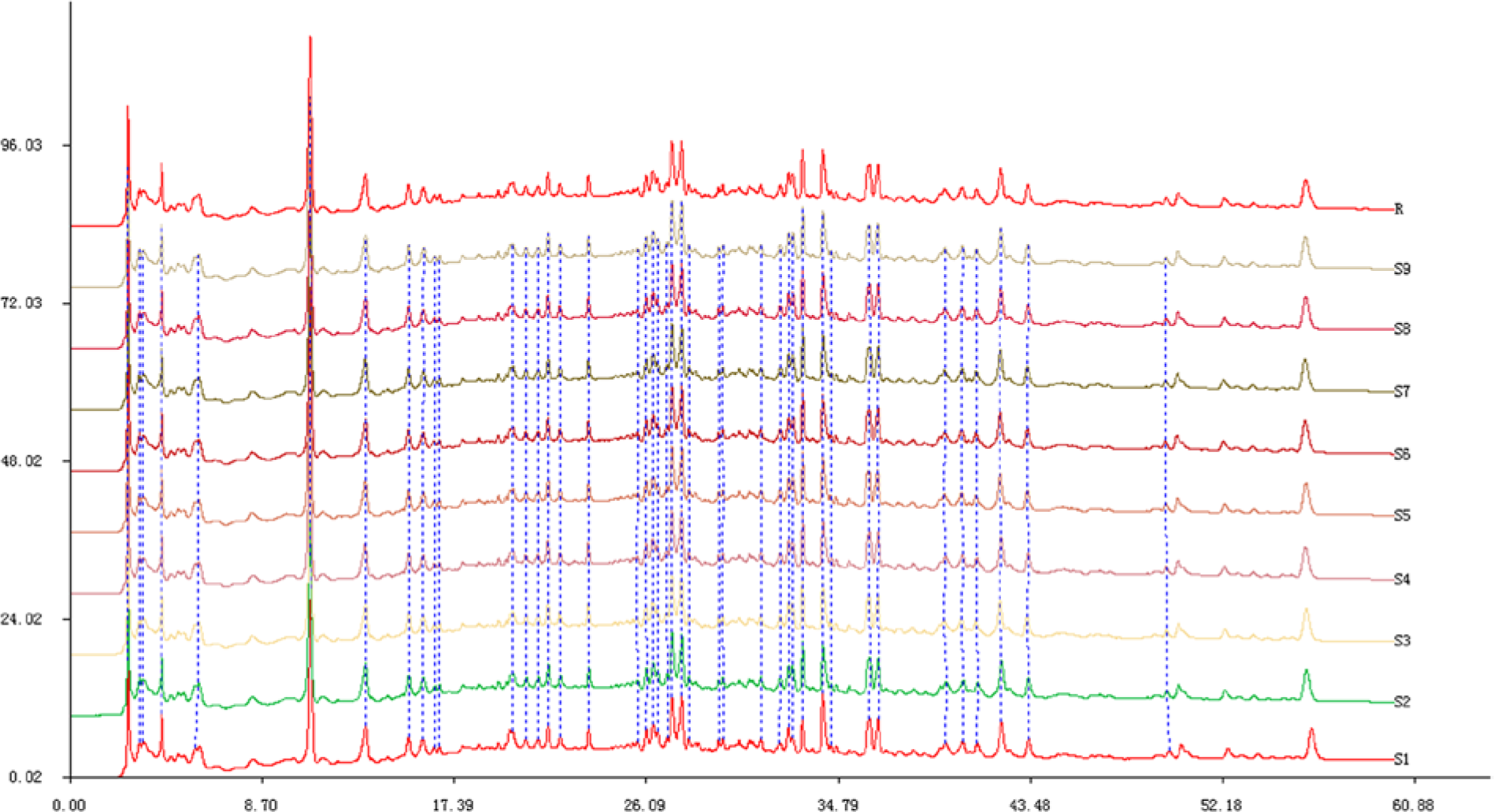
HPLC-DAD of the sample. Samples were randomly tested 10 times, and the absorbance was at 280 nm.
Case Reports
Case 1
A 64-year-old man was diagnosed in 2010 with gastric adenocarcinoma (Table 1). After a distal subtotal gastrectomy, he underwent 5 one-month cycles of chemotherapy. He responded to treatment for only 4 months before carcinoembryonic antigen (CEA) and CA72-4 levels began to rise (reference values = 0-5 µg/mL and 0-8.2 U/mL, respectively). Along with a new chemotherapy regimen, he began taking 6 capsules (1.8 g) of GLS a day as a dietary supplement. One month later, when the CA72-4 had surged to 126.30 U/mL and the CEA was still rising, we suggested that he stop the GLS and try an alternative herbal medicine, Hua Chansu, a Chinese medicine that comes from dried toad venom from the skin glands of Bufo gargarizans or Bufo melanostictus, which was commonly used to treat gastrointestinal cancer. 19 After 2 cycles of treatment, the CA72-4 values fell into the normal range. He began taking GLS again; a month later, the CA72-4 had sharply risen to 435.78 U/mL, so the supplement was stopped. When he came to our department for follow-up 1 month later, CA72-4 levels had returned to normal and the CEA level had decreased (Figure 3A). An enhanced computed tomography scan of the abdomen 6 months after the last CA72-4 surge showed no progression of the disease. During the treatment, his liver function indexes all remained within the normal range.
Clinical Pathology of the 5 Patients.

Abbreviations: GLS, Ganoderma lucidum spore; GA: gastric adenocarcinoma; CA: colorectal cancer; AJCC, American Joint Committee on Cancer.
The stages follow AJCC gastric cancer guidelines (2010, 7th version).
The last CA72-4 value detected before the first use of GLS.
Peak value of CA72-4 during GLS treatment.
The CA72-4 value of Patient 4 was obtained 2 months after GLS was discontinued; the other patients’ values were taken 1 month after discontinuation of the supplement.
Anastomotic gastric adenocarcinoma, not applicable to the AJCC staging system.

Multiples of the measured values of CA72-4 and CEA compared to their respective reference values at various treatment stages.
Case 2
A 77-year-old man was diagnosed in 2010 with gastric adenocarcinoma (Table 1). After a total gastrectomy and splenectomy, he underwent 5 cycles of chemotherapy. The response was good; only his CEA value was greater than the reference level, and it trended toward the normal range. He then presented in our department to obtain the alternative treatment β-elemene,20,21 which was a naturally occurring compound isolated from the TCM herb Curcumae Radix 22 and began using 1.8 g of GLS a day as a dietary supplement (β-elemene was not stopped in the subsequent treatment). His CA72-4 level immediately surged to 99.23 U/mL; it fell back into the normal range a month after the GLS was stopped (Figure 3B). He visited our department for 8 more months, during which we detected no progression of the disease. During the treatment, his liver function indexes remained normal.
Case 3
A 61-year-old woman was diagnosed in 2009 with gastric adenocarcinoma (Table 1). After a radical proximal gastrectomy and gallbladder resection, she responded to chemotherapy for only 4 months before her CEA and CA72-4 levels began to rise. We recommended an alternative herbal medicine, Xiao Aiping, a Chinese medicine that comes from Glaucescent Fissistigma Root, which was frequently used for gastrointestinal cancer in China. 23 After 3 cycles of treatment, the CEA value had increased to 54.51 µg/L, but the CA72-4 had declined to normal. She then took GLS as dietary supplement along with the Xiao Aiping, which was continuously applied in the subsequent treatment. A month later, the CA72-4 had surged to 99.92 U/mL and the CEA to 60.83 µg/L. Dramatically, both the CA72-4 and CEA dropped sharply by the next month without any change in treatment. The GLS was then withdrawn, and the CEA and CA72-4 both rapidly fell into the normal range (Figure 3C). Ten months later, when she visited our department for follow-up, we detected no progression in her disease. During the treatment, her liver function indexes remained within the normal range.
Case 4
A 56-year-old man was diagnosed in 2008 with anastomotic gastric adenocarcinoma (Table 1). Initially, he used Hua Chansu 19 as a treatment. Serum tumor markers were monitored every month; after 24 one-month cycles of treatment, CEA and CA72-4 were normal, as was liver function. He then took GLS as a dietary supplement accompanied with Hua Chansu. The CA72-4 titer increased sharply to 562.30 U/mL by the 1-month follow up; it decreased rapidly to 27.65 U/mL 2 months after withdrawal of the GLS. Throughout this period, the CEA only showed small changes (Figure 3D). The patient was followed by our department for 8t more months, during which we detected no progression of his disease. During treatment, his liver function remained normal.
Case 5
A 59-year-old woman was diagnosed in 2010 with colorectal cancer (Table 1). After radical surgery, she responded to chemotherapy for 6 months before her CEA levels began to rise. She stopped chemotherapy and began Xiao Aiping 23 plus 1.8 g of GLS a day (Xiao Aiping was not ceased in the subsequent treatment). Her CA72-4 had surged to 287.10 U/mL 1 month later, and her CEA had risen slightly. She stopped the GLS. Her CA72-4 immediately returned to normal, and her CEA also became normal after 2 months (Figure 3E). Our department followed her for 9 months, during which an enhanced abdominal computed tomography scan detected no progression of the disease. During treatment, her liver function remained normal.
Discussion
With herbal therapies becoming increasingly popular among cancer patients, it is important for physicians to recognize the effects of such therapy in their patients since the majority of these agents are commonly not subjected to premarket toxicity examination to test their safety or efficacy.24,25 As shown in Figure 2, all 5 gastrointestinal cancer patients experienced a surge of the serum tumor marker CA72-4 after taking GLS. Except in Case 3, the supplement was withdrawn immediately when their CA72-4 levels surged, after which their levels decreased sharply to reference levels. Interestingly, in Case 3, the only patient who kept using GLS after her CA72-4 level peaked, CA72-4 also sharply decreased after an initial month of increase. Additionally, although 1 patient experienced a surge in CEA along with the rise in CA72-4, the patients showed no significant change in clinical symptoms, and in follow-up we found no progression in disease. These data demonstrate that GLS, alone or combined with other agents, may induce the elevation of CA72-4. However, this elevation may not correlate with disease progression.
Our cases do highlight concerns regarding the safety of GLS. GLS is an herbal remedy containing multiple constituents, not all of which have been identified. However, the preparation is known to contain major bioactive components such as ergosterol, triterpenoids, unsaturated fatty acids, and polysaccharides,12,26-28 all of which are generally believed to be safe. Furthermore, in animal studies the LD50 of GLS has been shown to be more than 10.0 g/kg with no mutagenic or teratogenic action, which suggests that GLS is probably safe. 29
CA72-4 is one of the most valuable markers for monitoring response to treatment in gastric cancer patients30-34 and that an increase in level of this tumor marker may invariably heralds disease progression; however, the phenomenon of tumor marker surge during treatment is registered in some special conditions, which should catch our attention. Previous studies report that cytotoxic drugs can induce a surge in serum tumor markers. For example, Sørbye and Dahl report a transient CEA increase at the start of oxaliplatin combination therapy for metastatic colorectal cancer; the CEA levels peaked between 13 and 56 days, and the median rise from baseline was 263%. 35 Loprinzi et al found a CEA surge in 14 of 29 responding metastatic breast cancer patients treated with dibromodulcitol, doxorubicin, vincristine, tamoxifen, and fluoxymesterone (DAVTH) or DAVTH alternating with cyclophosphamide, methotrexate, 5-fluorouracil, and prednisone (CMFP); the mean rise was 243% of pretreatment CEA levels. 36 This phenomenon was commonly interpreted as the result of more powerful chemotherapy agents inducing greater tumor cell lysis. In our Case 3, the only patient who continued GLS for a long period, CA72-4 surged rapidly when GLS was initiated and then sharply decreased, as did CEA, without any change in treatment, thus mirroring the aforementioned studies. Taking into consideration that studies demonstrate that the GLS extract possesses direct cytotoxic effects on cancer cells through multiple mechanisms such as apoptosis, cell cycle arrest, and enhanced cell-mediated immune response,37-40 there is a possibility that the surge of CA72-4 might be due to GLS-produced tumor cell lysis. However, evidence to support this hypothesis is lacking as no other clinical symptom improvements accompanied the CA72-4 surge.
To date, the production mechanism of CA72-4 in cancer cells is not well illustrated. An additional possibility for the surge of CA72-4 in our cases is that GLS may directly or indirectly modulate CA72-4 production without a corresponding promotion of either tumor progression or antitumor effects. In such a scenario, tumor cells may not be growing while GLS is effectively promoting CA72-4 production. However, we cannot draw clear conclusions based on the current data.
The history of mushroom use for medicinal purposes began with TCM more than 5000 years ago, and on most occasions, these agents are categorized as “generally regarded as safe,” 8 but a long history of use, traditions, faith, popularity, and anecdotes cannot always be taken as evidence for the safety of these agents. 41 Although our cases may indicate that the usage of GLS in gastrointestinal cancer patients be harmless, it cannot be taken as an evidence for its free application in patients. Rigorous evidence for its safety or efficacy can only be obtained from randomized controlled trials in the future.
Conclusion
Our cases suggest that the safety of GLS in cancer patients should be further studied. GLS should be used with caution, and patients should be carefully monitored and followed-up.
Footnotes
Acknowledgements
We thank Dr Lyn Lowry of the Center for Integrative Medicine, University of Maryland School of Medicine, for her editorial support.
Authors’ Note
Bing Yan and Xianze Meng contributed equally. Other authors contributed to language translation, editing, and scientific advice.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors(s) received no financial support for the research, authorship, and/or publication of this article.
