Abstract
This scoping review examines the impact of inappropriate sexual behaviors (ISBs) in people with dementia on their family caregivers. Through synthesizing 15 studies from 8 countries, 6 themes were identified: complex emotional responses, psychological distress, increased caregiver burden, practical caregiving challenges, impaired marital relationships, and social isolation. Findings reveal caregivers frequently experience helplessness, embarrassment, anger, anxiety, depression, and social withdrawal, exacerbated by societal taboos surrounding sexuality and limited professional support. Spousal caregivers are particularly affected, reporting increased emotional strain and marital distress. Practical caregiving difficulties, including safety and privacy concerns, limited access to care services, and challenging institutionalization decisions, further intensify caregiver burden. The review highlights significant research gaps, including the need for specialized assessment tools, broader and culturally diverse studies, and exploration of ISBs as distinct phenomena. Addressing these gaps is crucial for developing targeted interventions and adequately supporting caregivers, particularly within home-based and culturally sensitive dementia care services.
Keywords
Introduction
According to the WHO, 57 million people worldwide are living with dementia, 1 and most of their care is provided by family members. 2 Family members serve as a critical resource3,4 and play a key role in ensuring positive outcomes for people with dementia. 5 Given their essential role, ensuring the well-being of family caregivers is crucial. 6 However, caregiving can be highly stressful, affecting both physical and mental health and, in turn, influencing the quality of care provided.7-9 A major source of stress is managing the behavioral symptoms of dementia,10,11 which include inappropriate sexual behaviors (ISBs), physical aggression, agitation, screaming, restlessness, hoarding, cursing, shadowing, wandering, and culturally inappropriate behaviours. 12 While ISBs are among the less common behavioral symptoms, they can cause significant distress to both family and professional caregivers and may lead to emotional and even physical harm.13-16
According to the International Psychogeriatric Association, ISBs, also referred to as sexual disinhibition or hypersexuality, encompass a range of uninhibited sexual behaviors directed toward oneself or others. 12 Examples of such behaviors include lewd or suggestive language, inappropriate sexual requests (e.g., requesting unnecessary genital care), unwanted touching or grabbing, disrobing of self or others, viewing pornography in public, and public masturbation. 16 However, there is no consensus in the literature on how ISBs in dementia should be defined. 17 Some studies define ISBs strictly as sexually motivated behaviors, excluding those stemming from cognitive impairment rather than sexual intent (e.g., undressing in the wrong room). 18 Others consider ISBs within the framework of social and cultural appropriateness17,19,20 or include emotional responses when sexual advances are refused. 21 Moreover, some researchers define ISBs in relation to deviations from an individual’s prior sexual behaviours.17,20,21 These definitional variations contribute to inconsistencies in the identification, assessment, and reporting of ISBs, leading to wide-ranging prevalence estimates across studies. 17
Reported prevalence rates of ISBs in people with dementia vary substantially, ranging from 1.8% to 25.9% with higher rates in institutional settings compared to community settings.19,22,23 Research examining the prevalence of ISBs among community-dwelling people with dementia is limited. During the study selection process for this scoping review, five studies were identified that reported prevalence data on ISBs in this population. Across these studies, reported prevalence varied widely, ranging from 2.9% to 25.9%.17-21
Although ISBs are relatively uncommon, those who directly experience these behaviors may find the distress overwhelming. 24 Among the various behavioral symptoms, ISBs are particularly distressing and embarrassing for caregivers. 25 Family caregivers, in particular, may experience heightened social isolation due to the stigma surrounding ISBs. 25 Some caregivers fear that ISBs may be directed toward healthcare providers, leading them to limit access to in-home support. 25 Others may restrict visits from family members, such as grandchildren, to shield them from exposure to such behaviours. 24 These responses, though protective, further contribute to caregiver isolation and reduce opportunities for respite and external support.24,25
While the existing literature contains numerous studies focusing on the behavioral symptoms of dementia, research on ISBs remains limited. 26 Furthermore, in the study of ISBs in dementia, most research has focused on nursing facilities and hospitals, often overlooking the experiences of family caregivers providing care at home.26,27 Hayward et al 27 found that healthcare staff encountering ISBs in inpatient settings often experienced shock, embarrassment, and distress, prompting calls for specialized training and support systems. However, family caregivers often lack access to such resources, making it more difficult for them to manage these behaviours. 28 As healthcare policies increasingly emphasize supporting people with dementia to remain in their homes, understanding the impact of ISBs on family caregivers is essential to ensuring that dementia care services adequately address their needs.27,29
Despite the increasing awareness of the need to support family caregivers, the specific impact of ISBs on them remains underexplored. 27 This scoping review aims to address this gap by examining the impact of ISBs on family caregivers. By synthesizing existing literature, this review seeks to identify key themes, highlight research gaps, and provide insights to inform future studies and the development of home-based dementia care services. To guide this review, the following question was posed: What is the impact of inappropriate sexual behaviors (ISBs) in people with dementia on their family caregivers?
Methods
The review followed the Joanna Briggs Institute (JBI) methodology for scoping reviews
30
and reported the evidence in accordance with the
Inclusion Criteria
Studies involving any aspect of ISBs’ impact on family caregivers were included. Studies focusing solely on professional caregivers were excluded.
Peer-reviewed empirical research studies or systematic reviews/meta-analyses were included. Non-empirical studies such as book reviews, editorials, opinion pieces, book chapters, and letters to the editor were excluded. Studies without full-text availability, such as conference abstracts or registry entries, were excluded.
No language restrictions were applied. One French-language 17 and one German-language 32 article were included and were translated with the assistance of translators to ensure accurate interpretation and data extraction. There were no restrictions on the publication year to ensure a comprehensive review of the literature.
Search Strategy
Search Terms Used in the Search Strategy

Source of Evidence Selection
Following the final search re-run (2 October 2025), retrieved records were imported into Covidence for duplicate removal. Additional duplicates were then manually identified and removed. The search identified 698 articles, leaving 491 after duplicate removal. Two reviewers (HL and LM) worked independently throughout the selection process. Any disagreements between the two reviewers at any stage were resolved through discussion with a third reviewer (CC). The two reviewers initially screened titles and abstracts to assess eligibility. The initial screening excluded 414 articles that were clearly irrelevant to the review question. A full-text assessment of the remaining 77 articles was then conducted in accordance with the established inclusion criteria. Following full-text assessment, 15 articles were deemed eligible for inclusion in the review. Compared with the initial search (6 October 2024), the final re-run identified two additional eligible articles published in 2025. No additional articles were identified after analyzing the references of the included studies. The selection process is documented in a PRISMA flow diagram (see Figure 1). PRISMA flow diagram of study selection process
33
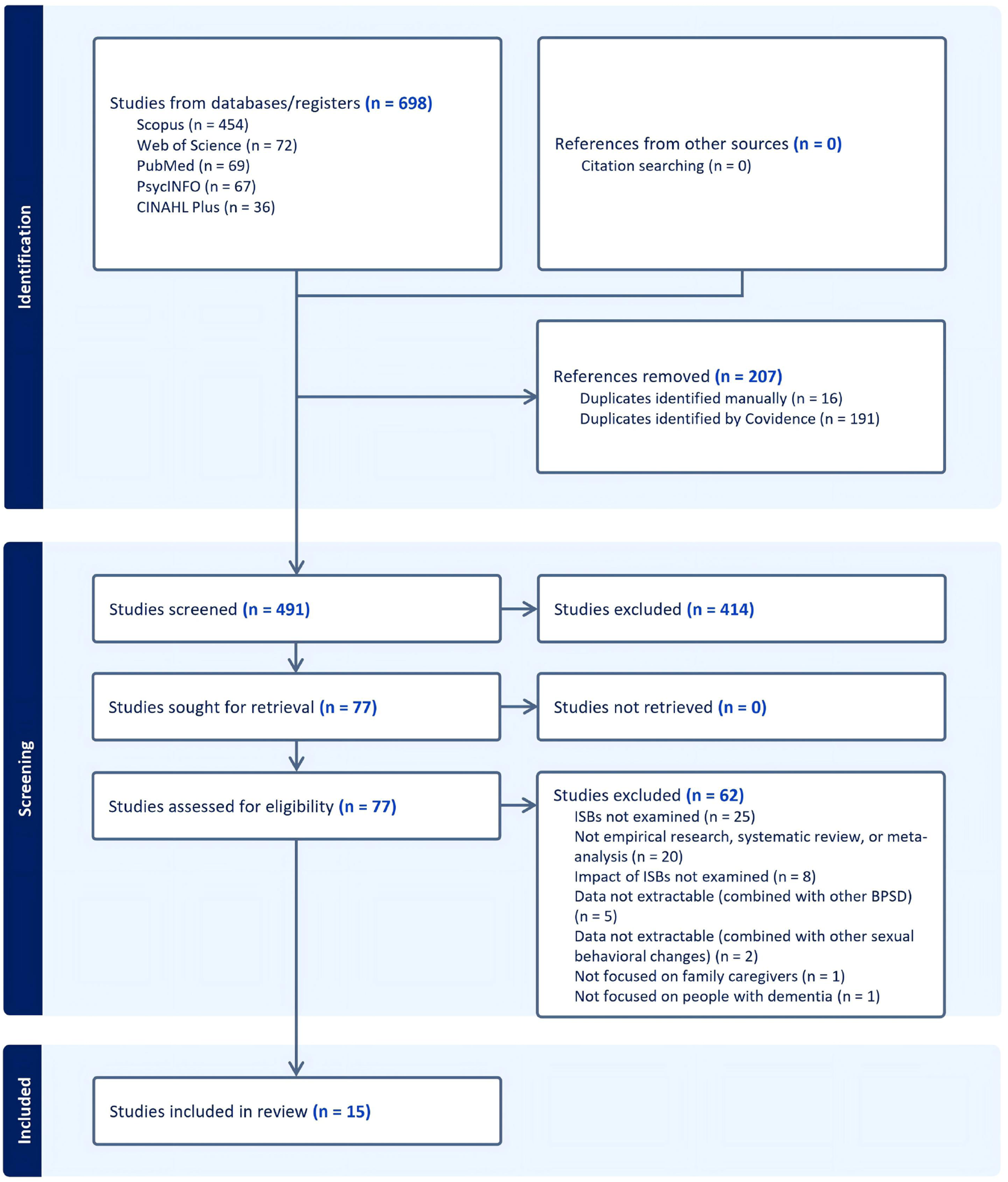
Data Extraction
Data from the included sources of evidence were extracted using a structured spreadsheet that was developed and tested by the research team prior to use. Two reviewers (HL and LM) independently extracted data. Any discrepancies between the two reviewers during data extraction were resolved through discussion with a third reviewer (CC). Since not all included studies focused solely on ISBs, only key findings specifically related to ISBs and their impact on family caregivers were extracted. The extracted data included study characteristics (author(s), publication year, country, study design, sample size, and participants), study aim, study focus (whether ISBs were the primary or secondary topic), type of ISBs reported (specific forms of ISBs observed in people with dementia), and key findings related to their impact on family caregivers.
Data Analysis and Presentation
Characteristics of Selected Studies
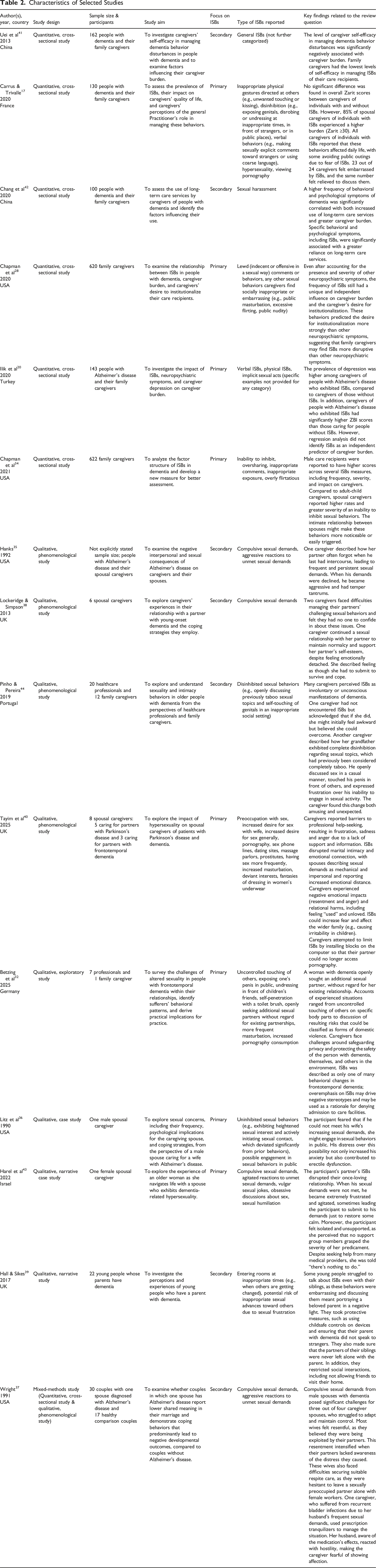
Results
The 15 studies included in this review were conducted in 8 countries. The studies were distributed as follows: five from the USA,28,34-37 three from the UK,38-40 two from China,41,42 and one each from Germany, 32 France, 17 Israel, 43 Portugal, 44 and Turkey. 20 The majority of the studies are from Western countries (12 out of 15), with a significant portion from the USA (n = 5). In this review, Turkey is categorized as a non-Western country and Israel as a Western one, based on their cultural patterns and societal characteristics rather than strict geographical definitions.45,46
Six studies used quantitative methods, all of which were cross-sectional.17,20,28,34,41,42 Another 8 studies used qualitative methods, including phenomenological, narrative, exploratory, and case studies.32,35,36,38-40,43,44 One study used a mixed-methods approach, combining cross-sectional and phenomenological designs. 37 The studies varied in terms of their focus on ISBs: 8 treated ISBs as the primary topic,17,20,28,32,34,36,40,43 while seven others examined them as a secondary topic, focusing on broader caregiving issues.35,37-39,41,42,44
Six themes were identified during the review: Complex emotional responses; psychological distress; increased caregiver burden; practical challenges in caregiving; impaired marital relationships; social isolation.
Complex Emotional Responses
Caregivers often experience a complex range of emotions in response to ISBs, including helplessness, embarrassment, and anger. A predominant feeling among caregivers is helplessness, as they struggle to manage ISBs without adequate support. One significant barrier to support is the difficulty in discussing ISBs, both within families and in medical settings. Hall and Sikes 39 found that adult children caring for parents with dementia often hesitated to discuss ISBs, even with siblings, fearing it would portray their parent in a negative light. Similarly, Carrus and Trivalle 17 found that most caregivers in their study had never discussed ISBs with healthcare providers. However, when given the opportunity to share their experiences, most caregivers expressed relief, highlighting the silence surrounding the issue. The taboo surrounding sexuality contributes to this silence, particularly in French culture, where both doctors and patients feel uncomfortable discussing ISBs due to concerns about modesty or upbringing. 17
Recent research has reinforced that seeking professional help for ISBs faces a range of issues, including communication difficulties, gaps in understanding and education, neglect by health professionals, stigma, and a general discomfort in discussing sex. 40 Tayim et al 40 reported that all caregivers in their study experienced difficulty accessing adequate assistance or information, expressing sadness, frustration, and anger over the unavailability of help.
However, not all caregivers remain silent. Some actively seek support but often feel dismissed or unheard. Harel et al 43 illustrated this through a case study of a female caregiver who repeatedly sought assistance from peer support groups and healthcare providers. She was dismissed by her support group and told by multiple doctors that “there’s nothing to do,” exacerbating her sense of helplessness. Similarly, Lockeridge and Simpson 38 reported that two caregivers felt they had no one to confide in about their partner’s ISBs, leaving them to cope with these challenges alone.
Another dominant emotional response is embarrassment. Carrus and Trivalle 17 reported that 23 out of 24 caregivers expressed significant embarrassment about their care recipient’s behaviors. Moreover, anger may permeate the entire family. Tayim et al 40 reported that one caregiver described intense anger in response to her partner’s behaviors, alongside a reluctance to be touched by him. The study also documented how a father’s behaviors were associated with his children becoming “irritable,” as they were unable to reconcile his conduct with his upbringing and the way he brought them up.
Psychological Distress
Caring for a family member with dementia who exhibits ISBs can have profound psychological consequences for caregivers. Research indicates that ISBs are associated with diminished self-efficacy, 41 heightened anxiety, 36 and an increased prevalence of depression among caregivers. 20
One of the most significant psychological effects is a decline in self-efficacy, referring to the caregiver’s reduced confidence in managing ISBs. Uei et al 41 found that family caregivers reported the lowest self-efficacy when dealing with ISBs compared to other behavioral symptoms of dementia. Two other studies further supported this, reporting that many caregivers struggled to manage ISBs, finding it difficult to adapt and maintain control.37,38
However, not all caregivers experience ISBs in the same way. While some find these behaviors distressing, others adopt a more accepting perspective. Pinho and Pereira 44 found that many caregivers viewed ISBs as involuntary or unconscious manifestations of dementia rather than deliberate actions. One caregiver in their study had not encountered ISBs but acknowledged that if she did, she might initially feel awkward but believed she could adapt over time. These contrasting perspectives suggest that personal experiences and perceptions of ISBs influence caregivers’ confidence in managing ISBs. Nevertheless, for those who do struggle with these behaviors, the sense of inadequacy and lack of control can significantly impact their psychological well-being.
Anxiety levels among caregivers can be heightened by ISBs. The unpredictable nature of these behaviors can serve as a persistent source of stress, as caregivers may be concerned about these behaviors occurring in public. Litz et al 36 illustrated this in a case study where a caregiver expressed deep concern that if he could not meet his wife’s increasing sexual demands, she might engage in ISBs in public. His distress over this possibility not only increased his anxiety but also contributed to erectile dysfunction, demonstrating how ISBs can affect both the caregiver’s psychological and sexual well-being.
Moreover, the presence of ISBs can lead to increased rates of depression among caregivers. Ilik et al 20 found that caregivers who managed ISBs reported significantly higher rates of depression compared to those caring for individuals without such behaviors.
Increased Caregiver Burden
Research indicates that ISBs contribute to an increased burden on family caregivers. Most studies assessing caregiver burden used generic scales, with four employing the Zarit Burden Interview (ZBI)17,20,28,41 and one utilizing the Chinese Caregiver Burden Inventory (CCBI). 42
Two studies found a direct association between ISBs and increased caregiver burden.20,28 However, the findings regarding ISBs’ independent contribution to caregiver burden are mixed. While Chapman et al 28 found that ISBs independently contributed to higher caregiver burden, even when accounting for the presence and severity of other neuropsychiatric symptoms, Ilik et al 20 found no such independent effect. Ilik et al 20 suggested that the small number of individuals with ISBs (13 out of 143) may have limited the statistical power to detect an independent effect.
Other studies by Uei et al 41 and Chang et al 42 found that as the frequency of behavioral symptoms, such as aggressive behavior and ISBs, increased, caregivers reported higher levels of burden. Although neither study separately analyzed the impact of ISBs on caregiver burden, Uei et al 41 reported that caregivers exhibited the lowest self-efficacy in managing ISBs. Moreover, lower self-efficacy in managing the behavioral symptoms was significantly associated with a higher caregiver burden. This suggests that ISBs may contribute significantly to caregiver burden due to their difficulty in managing these behaviors.
While most studies indicate an association between ISBs and increased caregiver burden, Carrus and Trivalle 17 found no statistically significant difference in the overall burden between caregivers of individuals with and without ISBs. However, their subgroup analysis revealed that spousal caregivers of individuals with ISBs experienced a higher burden, with 85% scoring 30 or higher on the ZBI. This lack of a significant difference in the overall burden may have stemmed from limitations in measurement tools. While the ZBI has been widely used to assess general caregiver burden, it may not fully capture the unique stressors associated with ISBs, potentially underestimating their impact. 17 Another possible explanation is that the inclusion of non-spousal caregivers (e.g., children, relatives) in the ISBs group may have diluted the results, as they might experience less strain than spouses. Their lower ZBI scores could have masked the more intense burden reported by spousal caregivers of individuals with ISBs.
Practical Challenges in Caregiving
The presence of ISBs poses significant practical difficulties in daily caregiving tasks. Ensuring safety is a primary concern. Betzing et al 32 pointed out that caregivers often face major challenges in ensuring the safety of the person with dementia, themselves, and others in the environment. In some cases, ISBs may escalate into situations that could be classified as forms of domestic violence. The study further reported extreme manifestations that raised safeguarding concerns for others (e.g., undressing in front of a child’s peer group) and serious risks to the person with dementia (e.g., self-penetration with a toilet brush). Maintaining the care recipient’s privacy presents another distinct challenge. Betzing et al 32 identified this as a key difficulty when ISBs occur, reporting cases that resulted in severe losses of bodily privacy, such as a man exposing his genitals in public.
In response, caregivers employ various protective measures. Tayim et al 40 reported that some caregivers attempted to curb ISBs by implementing technological controls, such as placing blocks on the computer to prevent access to pornography. Hall and Sikes 39 also described caregivers enabling Childsafe settings across devices to reduce the risk of the care recipient doing something that could get him into trouble. Moreover, these caregivers had adopted collective strategies to prevent potential incidents, such as ensuring that their friends and the partners of their siblings are never left alone with the care recipient. These protective measures reflect the ongoing vigilance required to manage ISBs in a home setting.
Caregivers also struggle with accessing appropriate care services. A study showed that ISBs significantly influenced caregivers’ decisions to use long-term care services, including home-based care, community-based respite care, and institution-based services. 42 Statistical evidence from this study indicated a strong correlation between ISBs and the use of such services. However, spouses, particularly wives caring for partners with dementia, struggled to find suitable respite care due to concerns about ISBs. 37 The predominance of female respite workers further complicated this issue, as caregivers feared leaving a care recipient who may exhibit ISBs alone with a female respite worker.
The challenge of accessing care services may be further compounded by stereotypes surrounding ISBs in frontotemporal dementia. Betzing et al 32 noted that ISBs are only one of several possible behavioral changes in frontotemporal dementia, but they are often overemphasized in public discourse. Interviewees in their study cautioned that such emphasis may reinforce stereotypes that frame people with frontotemporal dementia as sexually inappropriate. They further warned that some facilities may invoke this stereotype to justify denying admission to residential care. Consequently, when caregivers seek institutional services in response to ISBs, they may encounter barriers linked to this stereotype, making it more difficult to access care services.
Another significant challenge is the difficult decision of whether to institutionalize the care recipient. Chapman et al 28 found that ISBs, even when accounting for other neuropsychiatric symptoms, independently contributed to caregivers’ decisions to seek institutional care. Their findings suggest that ISBs are particularly disruptive, outweighing other neuropsychiatric symptoms in driving institutionalization. However, for caregivers in societies that emphasize filial piety, this decision is emotionally complex. In such societies, caregivers may experience additional moral and social pressure to provide care at home. In a study conducted in China, Chang et al 42 reported that when asked about the best way to care for people with dementia, most caregivers preferred home-based care by family members or others. Chang et al 42 suggested that this preference might stem from concerns about being criticized for failing to honor their parents. As a result, caregivers of individuals with ISBs may face a profound dilemma: while institutionalization might be necessary due to the disruptive nature of ISBs, it conflicts with deeply ingrained societal expectations and personal beliefs about filial responsibility.
Impaired Marital Relationship
Intimate and loving partnerships are significantly eroded by ISBs, transforming them into relationships marked by distress, role strain, resentment, and fear. While several studies have primarily documented female spousal caregivers navigating these challenges in the context of male care recipients,35,37,38,40,43 emerging evidence indicates that male spousal caregivers may also face these challenges when caring for female partners with dementia. 32 Betzing et al 32 described a case in which a woman with dementia sought an additional sexual partner and proposed that her husband consider the three of them living together, illustrating a lack of empathy, limited self-reflection, and an inability to adopt the partner’s perspective regarding the emotional impact of such actions.
Chapman et al 34 found that spousal caregivers reported more frequent and severe symptoms of an inability to inhibit sexual behaviors in their care recipients compared to adult-child caregivers. The intimate nature of spousal relationships may make these behaviors more noticeable or easily triggered. 34 Moreover, research consistently indicated that ISBs were more prevalent and severe in male care recipients,17,34,37 which correlates with a greater impact of ISBs on female caregivers. 34 Wright 37 found that most female spousal caregivers reported that compulsive sexual demands from their partners with dementia caused significant distress.
The distress caused by compulsive sexual demands often leads to emotional detachment from their partner with dementia. Both Lockeridge and Simpson, 38 Harel et al, 43 and Tayim et al 40 reported cases where female caregivers no longer felt the same emotional connection, affection, or intimacy with their partner as before. Instead, they reported feeling compelled to comply with their partners’ sexual demands out of a sense of duty to preserve normalcy and protect their partner’s self-esteem, or out of compassion, rather than out of genuine emotional closeness or desire. These caregivers struggled with the loss of the partners they once knew and had to adjust to a new dynamic that starkly contrasted with their past relationships.
Tayim et al 40 found that half of the caregivers in their study felt “used” for sexual gratification and unloved by their husbands, as the sexual relationship had become mechanical and non-affectionate. Furthermore, this mechanical and impersonal nature of the sexual relationship generated resentment. 40 This aligns with another study in which most caregivers reported resentment because they felt exploited by their partners’ compulsive sexual demands. 37 This resentment intensified when their partners lacked awareness of the distress they caused. 37
Hanks, 35 Wright, 37 and Harel et al 43 documented cases where male care recipients became agitated, emotionally distressed, or even physically aggressive when their sexual demands were unmet. For instance, one individual exhibited excessive drinking, crying, and fears of divorce, 43 while others displayed tantrums or physical aggression.35,37 In severe cases, caregivers were forced to take extreme measures to manage their partner’s behaviors. Wright 37 reported a case in which a caregiver, suffering from recurrent bladder infections due to her husband’s frequent sexual demands, attempted to manage the situation with prescription tranquillizers. However, when her husband became aware of the medication’s effects, he reacted with hostility, leaving the caregiver fearful of expressing even basic forms of affection, like a hug. Tayim et al 40 also described a case in which a caregiver experienced intense fear. After discovering her partner’s pornography use, which the caregiver reported involved boys, and learning that he needed to imagine himself wearing women’s clothes to engage sexually with her, she was so overwhelmed that she made him move out of their bedroom and locked the bedroom door.
Social Isolation
A prominent theme emerging from the reviewed studies is the experience of social isolation among caregivers. ISBs significantly impact caregivers’ social lives and relationships, often leading them to withdraw from social interactions. Carrus and Trivalle 17 found that all caregivers in their study reported an impact of ISBs on their daily lives. Some caregivers stopped leaving their homes altogether, fearing that their care recipient might exhibit ISBs in public.
In addition to avoiding public outings, caregivers also limit social interactions within their own homes to prevent potential incidents. Hall and Sikes 39 described how caregivers, concerned about ISBs, restricted visits from their friends to maintain a controlled environment. While this precaution may be necessary, it reduces opportunities for social engagement. Over time, the inability to host friends and maintain relationships can deepen feelings of isolation.
Moreover, caregivers may feel abandoned within formal support networks. Harel et al 43 reported that a caregiver felt frustrated by the lack of understanding from her peer support group, as her distress over ISBs was not taken seriously. When even support groups, which are designed to provide comfort and understanding, fail to recognize the severity of their experiences, caregivers may feel even more isolated.
Whether social isolation results from personal choice or external circumstances, ISBs can gradually distance caregivers from their pre-existing social support networks, limiting their access to emotional and practical support.
Discussion
Main Findings
This scoping review highlights the profound and wide-ranging consequences of ISBs in people with dementia for family caregivers. The synthesis indicates that difficulties in dealing with ISBs span emotional, psychological, relational, and practical domains, affecting everyday caregiving, intimate relationships, and social participation.
Family caregivers commonly report helplessness, embarrassment, and anger in response to ISBs. Barriers to discussing ISBs with others and seeking professional help can contribute to feelings of helplessness.17,39,40 However, even when caregivers reach out for help, they may feel dismissed or unheard.38,43 Embarrassment was particularly prominent and often intense. 17 Anger may extend beyond the primary caregiver to other family members. 40
ISBs are associated with diminished self-efficacy for managing these behaviors, 41 heightened anxiety over potential public incidents, 36 and higher rates of depression. 20 Moreover, caregiver burden increases in the context of ISBs, with some evidence indicating that these behaviors independently contribute to greater burden beyond the other behavioral symptoms. 28 Spousal caregivers, in particular, experience a heightened burden due to ISBs. 17
ISBs also pose practical caregiving challenges. Caregivers often remain vigilant and adopt strategies to manage safeguarding risks and protect privacy.32,39,40 Accessing care services can be difficult, particularly due to concerns about ISBs toward (often female) respite workers 37 and the stereotype that people with frontotemporal dementia are sexually inappropriate, which may create barriers to residential care. 32 Decisions regarding institutionalization are complex, as ISBs independently drive this consideration, 28 but may conflict with cultural expectations such as filial piety.
A notable finding was the deterioration of marital relationships. ISBs disrupted intimacy and partnership roles, shifting relationships from reciprocal and affectionate to distressing, duty-based, resentful, and fearful. This pattern was most commonly reported by female spouses caring for male partners.35,37,38,40,43 They described repeated advances or compulsive sexual demands that eroded emotional intimacy, leaving them feeling “used,” unloved, and emotionally detached. Caregivers often complied out of duty or compassion, while unmet demands could trigger agitation or aggression, sometimes forcing caregivers to take extreme protective measures and even fear ordinary affection.35,37,38,40,43
Finally, ISBs contribute to social isolation. Caregivers may withdraw from public outings and restrict home visitors to avoid incidents,17,39 and may feel dismissed within formal or peer support networks, further deepening isolation. 43
Gaps in Research Evidence
Insufficient Exploration of Specialized Assessment Scales for ISBs
Much of the current quantitative research relies on the ZBI scale to study the impact of ISBs on caregiver burden.17,20,28,41 However, the ZBI scale may not fully encompass the specific stressors associated with ISBs. 17 In response to the need for a more specialized assessment scale, Chapman et al 34 designed a scale to assess the level of impact caused by the care recipient’s ISBs. However, no studies have yet been conducted using this scale. Chapman et al 34 highlighted the need for validating this scale in more diverse populations and through alternative recruitment methods, such as clinic and residential samples, to ensure its suitability for various groups.
Limited Breadth of ISBs-Focused Qualitative Evidence
Across the 8 qualitative studies, ISBs are treated as the primary topic in four, two of which are single-case study designs.36,43 Harel et al 43 noted that, although a single-case study can offer rich insight into complexity and intersectionality, it may not capture the diverse forms of ISBs, thereby constraining the breadth of understanding of this phenomenon.
Insufficient Isolation of ISBs as a Distinct Focus Across the Evidence Base
A large proportion of the current evidence base (7 out of 15 studies) explores caregiving situations broadly without isolating ISBs as a distinct focus.35,37-39,41,42,44 Studies that do not isolate ISBs from broader caregiving situations may fail to fully capture the unique impact that ISBs have on caregivers.
Insufficient Exploration of Non-Western Cultural Contexts
Research indicates that cultural background, ethnicity, and race may influence how ISBs are recognized, reported, and experienced by caregivers.17,20,27,34 However, current research lacks sufficient data to develop a strong theoretical understanding of these cultural variations. The majority of studies in this review (12 out of 15) are from Western societies,17,28,32,34-40,43,44 with limited evidence from non-Western contexts. For instance, neither of the two quantitative Chinese studies separately analyzed the impact of ISBs on caregiver burden.41,42
Conclusion
This scoping review highlights the significant impact of ISBs in people with dementia on family caregivers. ISBs contribute to complex emotions, psychological distress, increased caregiver burden, practical caregiving challenges, and social isolation, with particularly severe effects on spousal relationships. While these findings underscore the challenges faced by caregivers, research on ISBs remains limited, leaving gaps in understanding their unique difficulties. Addressing these gaps is essential to developing effective interventions tailored to caregivers’ needs, particularly within non-Western cultures.
This review did not impose a time limit on publication years, which introduced certain limitations. Over time, awareness and understanding of the behavioral symptoms of dementia, including ISBs, have evolved, potentially affecting the comparability of studies conducted in different periods. However, given the scarcity of research on ISBs and their impact on family caregivers, including studies without a time restriction was essential for capturing a comprehensive body of evidence. Imposing a date restriction could have further reduced the available literature, excluding valuable insights. Some older studies remain highly relevant, as the challenges caregivers face in managing ISBs persist despite advancements in dementia care. Given the limited research available, reviewing these older studies was necessary. The review of older studies also revealed gaps in the literature, highlighting the need for more recent research that reflects contemporary caregiving contexts.
Future research should focus on developing and validating specialized assessment tools for ISBs to enable more precise measurement of their impact on caregivers. To improve generalizability, studies should move beyond single-case qualitative designs and include a larger and more diverse group of participants. Moreover, ISBs should be studied as a distinct phenomenon rather than being grouped with broader neuropsychiatric symptoms, allowing for a clearer understanding of their specific effects on caregivers. Given the increasing prevalence of dementia globally, exploring ISBs across diverse cultural contexts, particularly in non-Western societies, is also necessary to ensure a broader understanding of these behaviors.
By recognizing the unique challenges posed by ISBs, targeted interventions can be more effectively developed to support family caregivers. Training healthcare professionals to recognize and discuss ISBs in a sensitive and supportive manner is crucial to ensuring that caregivers feel heard and receive adequate guidance. Furthermore, breaking societal taboos around sexuality in dementia care is essential for fostering an environment where caregivers can seek help without fear of stigma. Expanding alternative care options, such as gender-specific respite services or trained respite workers equipped to manage ISBs, can also provide necessary relief to caregivers facing these challenges.
Supplemental Material
Supplemental Material - The Impact of Inappropriate Sexual Behaviors in People With Dementia on Family Caregivers: A Scoping Review
Supplemental Material for The Impact of Inappropriate Sexual Behaviors in People With Dementia on Family Caregivers: A Scoping Review by Huiping Lin, Leah Macaden, Colin Chandler in American Journal of Alzheimer’s Disease & Other Dementias®
Footnotes
Acknowledgements
We thank David Beckett for translating the German-language article and Le Song for translating the French-language article.
Ethical Considerations
This study did not require ethical approval as it involved no human or animal participants and did not include the collection of primary data.
Author Contributions
HL and LM conceived the study design. HL conducted the literature search. HL, LM, and CC performed the literature screening, review, and analysis. HL drafted the initial manuscript. LM and CC critically reviewed and revised the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
