Abstract
This was a descriptive study of elderly persons with dementia who were found dead after becoming lost in the community. Nineteen forensic autopsy cases were performed at Kochi Medical School, Japan. The mean age of the patients (9 males and 10 females) was 82.1 ± 6.6 years. Causes of death were drowning (n = 8), trauma (n = 5), hypothermia (n = 2), and debilitation possibly due to fatigue (n = 1) or were unknown (n = 3). Thirteen (68%) individuals had been reported missing, most at least 6 hours after they had left. They moved on foot (n = 14), by car (n = 3), or by bicycle (n = 2). Distances from residences to spots of death ranged from 20 to 5800 m for 11 patients on foot. In 8 cases, it was less than 500 m. The study has potential implications for enabling their early discovery and protection.
Introduction
In 2010, 35.6 million people worldwide were estimated to have dementia, and this number is expected to double every 20 years, likely reaching 65.7 million in 2030. 1 The G8 Dementia Summit, recently held in London in December 2013, confirmed that the rise in aging-related dementia was not just an issue in certain countries or regions but a common one globally. Japan and other G8 member countries have agreed that there is an urgent need to jointly address this growing health concern. 2
Japan is currently facing the unprecedented challenge of a rapidly aging society that has yet to be encountered by any other country. In 2012, people aged 65 years or older in Japan accounted for almost a quarter (24.1%) of its total population 3 ; the number of patients with dementia is anticipated to reach 3.45 million by 2015 and a further 4.7 million by 2025. 4 Recognizing the necessity for a systematic, effective response to the increasing prevalence of dementia in its aging population, the Japanese government formulated the “Orange Plan” in 2012, which outlined the national strategic measures against dementia. 5 At present, 1.49 million individuals representing about half of Japan’s patients with dementia are living at home, 4 and a major social issue that has arisen in caring for these patients is their tendency to wander.
The term “wandering” has been used to broadly encompass a variety of behaviors. These include aimless locomotion with a repetitive pattern, such as lapping or pacing, as well as excessive walking or leaving a safe environment and becoming lost alone in the community. 6 Several studies have recently demonstrated notable differences between missing incidents and wandering behaviors 7 –13 ; some have reported no established correlations between them. 7 , 14 The Alzheimer’s Foundation of America has defined a “missing incident” as an instance in which the whereabouts of a person with dementia are unknown to the caregiver and the person is not in the expected location. 15
All persons with dementia who can walk as well as those who continue to drive are at risk of going missing or becoming lost. 15 The majority of persons with dementia who become lost are found and returned home safely. 16 Thus, little research has focused on the specific circumstances of those found dead. Rowe et al reported that 87% of 93 cases of persons with dementia dying as a result of becoming lost in the community were found dead in natural, secluded, unpopulated area, such as woods, fields, ditches, and bodies of water. 17 In another report by Rowe et al, 87% of those found alive were found within a 5-mile radius of the place last seen, and 73% of those found dead were found within a half mile of the place last seen. 18 In Japan, according to a national survey conducted by the National Police Agency, 23668 people had been reported as dementia-related missing incidents. 19 Of these, 548 (2.3%) had died, 357 (1.5%) had yet to be found, 17842 (75.4%) had been found alive, and 4921 (20.8%) had returned home by themselves; approximately 900 people had either died or had not been found. Clearly, a great number of families were involved in maintaining the safety of these persons with dementia. In the worst-case scenario, missing incidents may lead to death; thus, the mental and physical burdens borne by families and caregivers are substantial. Despite this, hardly any research investigations have been performed on the autopsy cases of older adults with dementia to prevent accidental deaths because of missing incidents. Ordinary Japanese people have a poor understanding of the fact that at a certain stage of missing incidents, independent living is impossible, with missing incidents being one of the greatest risks for death. Therefore, we analyzed the cases of outdoor deaths among older adults with dementia who had been found dead after becoming lost, in order to identify preventive measures or protective factors against such deaths.
Methods
This study employed a retrospective descriptive design. Data were gathered from police investigative reports and our autopsy records of 19 elderly persons with dementia who had died outdoors because of becoming lost in the community. The autopsies were requested by the police and performed by the Department of Legal Medicine of Kochi Medical School between January 2003 and December 2013. The police collected the information on the victims from their relatives, neighbors, and homes and obtained medical record information from medical institutions where the patients were visiting. The police sent a forensic pathologist at the department with the investigative reports, which included data on patients’ age and gender; the time they went out and means of mobility while they were out; whether they were residing with family or alone, had a prior history of missing incidents, and had been reported missing to the police; and the circumstances surrounding the sites of their discovery. We also used autopsy records on causes of death, pathological findings, data on estimated times of death, and the results of drug and alcohol analysis in our examination of (1) the time interval between when they had left and the discovery of their body and (2) the direct distance from their home or residence to their place of death. The present study included dementia-suspected cases corresponding to Level 1 of degrees of independent living prescribed by the Ministry of Health, Labour, and Welfare according to information regarding mild memory loss and cognitive impairment provided by patients’ proxies (relatives of patients), although patients had not been diagnosed with dementia by medical professionals.
Results
Table 1 gives an overview of 19 older adults with dementia who died while missing, 9 of whom were male (aged 80.9 ± 5.4 years) and 10 were female (aged 83.2 ± 7.7 years). Table 2 details the characteristics of all 19 autopsy cases. Of the 19 patients, 11 had dementia, 5 were suspected of having dementia, 2 had Alzheimer’s disease, and 1 had Pick disease. Of the 15 patients for whom information on antemortem missing incidents was available, 7 (47%) had wandered out of their homes every day or almost every day.
Overview of 19 Cases of Death Due to Dementia-Related Missing Incidents.
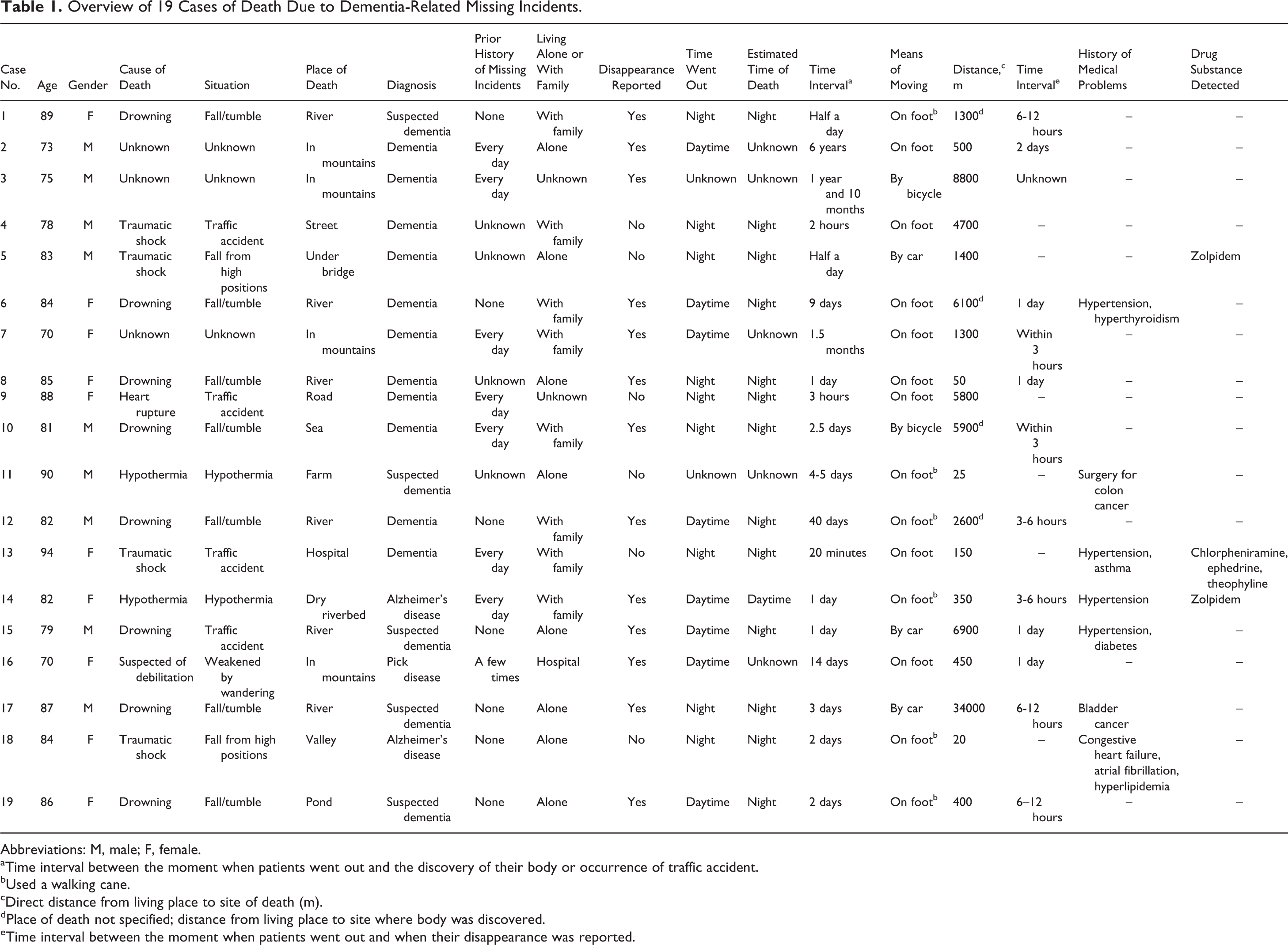
Abbreviations: M, male; F, female.
aTime interval between the moment when patients went out and the discovery of their body or occurrence of traffic accident.
bUsed a walking cane.
cDirect distance from living place to site of death (m).
dPlace of death not specified; distance from living place to site where body was discovered.
eTime interval between the moment when patients went out and when their disappearance was reported.
Characteristics of 19 Cases of Death Due to Dementia-Related Missing Incidents, by Frequency.
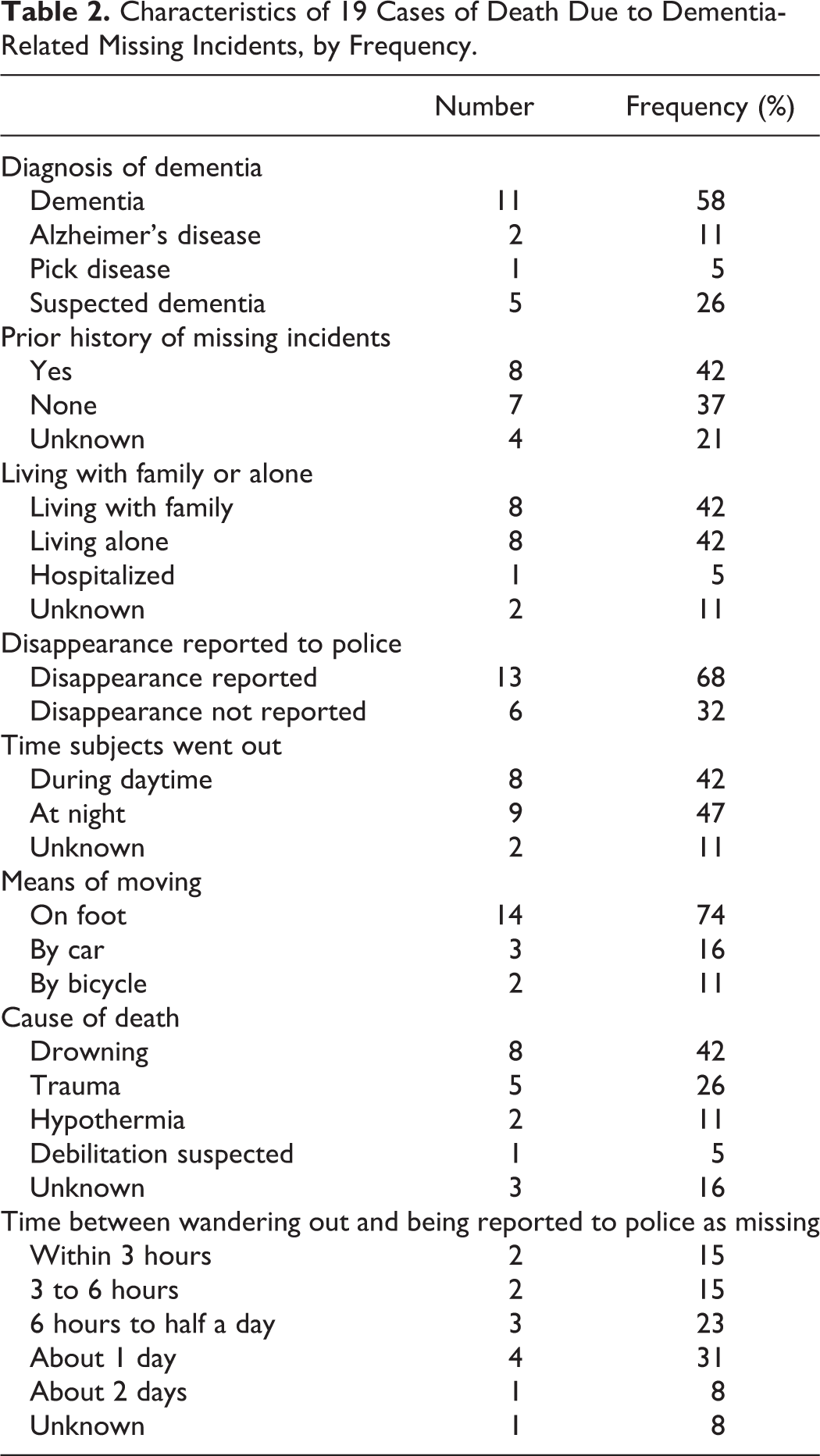
The causes of death were drowning (n = 8), trauma (n = 5), hypothermia (n = 2), debilitation possibly due to wandering fatigue (n = 1), or were unknown (n = 3). Drowning sites included the river (n = 6), sea (n = 1), and pond (n = 1), and the probable cause of death in every instance was falling into the water while walking or driving. Deaths from trauma (n = 5) were caused by being hit by a vehicle (n = 3) and falling from high positions (n = 2) while walking at night. Two hypothermia cases occurred due to walking outdoors in low temperatures, while 1 debilitation-related death was suspected of having been caused by fatigue from walking in the mountains. The cause of death in 3 cases where individuals had been found as skeletal remains in the mountains remained unknown.
Patients generally resided at home (n = 18), although one had been admitted to the hospital. Among those who resided at home, 8 were residing with family, 8 resided alone, and 2 were unknown. Of the 19 patients, 13 (68%) were reported missing to police after disappearing (6 of whom resided with family, 5 resided alone, 1 in the hospital, and 1 was unknown). However, no significant differences were found between patients who resided with family and those who resided alone. Further, 2 cases had been reported to the police within 3 hours after patients had gone outside; 2 between 3 and 6 hours; 3 between 6 and 12 hours; 4 after a day; 1 after 2 days; and 1 whose time interval was unknown. Of the 6 unreported cases of disappearance, 4 had involved a search by the family or neighbors of missing individuals, while 2 had ended in death. None of the patients had GPS, mobile phones, or other electronic devices that could deliver location information.
Nine patients went out at night, 8 during the daytime, and 2 were unknown. The estimated times of death were nighttime in 13 incidences, daytime in 1, and unknown in 5. Further, 8 (42%) of 19 individuals were found dead within 1 day after they went out.
In all, 14 patients went out on foot, 3 by car, and 2 by bicycle. Of 14 patients, 6 moving around on foot had been using a cane before death. Excluding the 3 patients whose specific situations surrounding their deaths could not be identified, the direct distances from patients’ living places to their sites of death (or traffic accidents) ranged extensively from 20 to 5800 m for 11 patients on foot. In 8 (73%) cases, it was within 500 m. Of 11 patients, 4 on foot used a cane or similar walking aid, and the direct distance from their living places to their sites of death averaged 199 m, with a range of 20 to 400 m. This distance was considerably shorter compared with that of 1850 m (range: 50-5800 m) for 7 patients on foot who had no walking problems before death. Of the 3 patients who had gone out by car, 2 had become lost before reaching their destinations and caused minor accidents. Of the 2 patients, 1 going out by bicycle accidentally fell into the river while riding and drowned, while the other stopped riding and walked into the mountains nearby before being found dead.
Drugs were detected in 3 (16%) patients. Zolpidem, a prescription sleep aid, was detected in 2 patients. Its side effects have been reported to include sleepwalking and sleep driving. The alcohol test results for 16 patients were all negative.
Discussion
The mean age of men and women in our study was relatively close to the mean Japanese lifespan of 79.9 and 86.4 years for men and women, respectively. 20 In general, patients with dementia who stay in a hospital or nursing home are less likely to become lost in the community. Our results showed that 95% of the 19 deaths examined in our study occurred among the patients who were living at home. Probable reasons for the higher risk of such deaths among older adults with dementia living at home, compared with those staying in hospitals, include the increase in those living alone and the reduced capacity to care for these individuals in their homes due to the current trend toward nuclear families in Japan. According to the Ministry of Health, Labour, and Welfare statistics for the year 2012, 4 about half of 3.05 million older adults with dementia were residing at home (1.49 million), and this number can be expected to grow in the future. Accordingly, the prevalence of missing incidents will likely become a more serious concern.
According to a 1996 questionnaire sent to families caring for older adults with dementia, 79% (696) of these adults exhibited wandering outdoors, of whom 78% (543) had gotten lost or had gone missing. 21 Meanwhile, it was not known how many of those who died due to dementia-related missing incidents had a prior history of missing incidents. According to autopsy reports by Yamazaki et al, 22 10 (25.6%) of the 39 older adults they examined, who had died after becoming lost, had gone missing on previous occasions due to similar behaviors. Although the patients of Yamazaki’s report were also aged 65 years or older, they were not restricted to individuals with dementia. Our survey of such deaths, on the other hand, focused on those who had dementia or had been suspected of dementia. The results indicated that 47% of 15 patients occurred in individuals with a prior history of missing incidents—becoming lost every day or almost every day. In other words, about half of these older adults with dementia died in specific accidents after having suddenly begun to wander outdoors on a particular day. The incidences of such deaths among older adults with dementia are difficult to predict, as they could possibly involve a relatively large number of individuals without everyday wandering habits.
Ours is the first study to focus on causes of death or accidents in cases of deaths due to dementia-related missing incidents in Japan. According to Yamazaki et al, 22 20 (51%) of 39 deaths examined among older adults (of whom, 25 had dementia) were caused by drowning. One possible explanation for the higher proportion of deaths from drowning when compared to deaths from trauma (eg, in traffic accidents) lies in the regional characteristics of Kochi Prefecture. The region is known for its low population density, rivers, and extensive mountainous areas. In our study, falls/tumbles were the most frequent causes of death, influenced by factors such as impaired cognitive functioning associated with dementia, in addition to the deterioration in physical functioning that frequently affects individuals of this age. The causes of death and accidents among older adults with dementia who become lost may differ somewhat between cities and rural areas, as individuals’ living environments would differ substantially. In order to plan and develop preventive measures against deaths due to dementia-related missing incidents, the actual cases of such deaths should be carefully analyzed by considering the characteristics of specific regions in which they occur.
Little research has been done on drug analyses of people with dementia who died because of missing incidents. Among the cases we looked at, patient No. 5 was likely to have been sleep driving, due to the side effects of Zolpidem, and caused a minor traffic accident. This person then moved on foot at night, and probably fell from a bridge.
Missing incidents should be identified as quickly as possible and reported to the police and other emergency response organizations. This would then enable a search by many individuals to locate and ensure the safety of the missing person. According to a previous questionnaire survey of families caring for older adults with dementia, 21 62.4% of 543 caregivers had reported missing people to the police. Another report 22 noted that 71.8% of those who had gone missing had been reported to the police. In our survey, police reports had been made with a similar degree of frequency as previously observed. Furthermore, only 2 of these reports had been filed within 3 hours after the individual had gone missing. None had GPS, mobile phones, or other electronic devices that could provide them with information as to their whereabouts. These results revealed that measures and actions to discover and secure these missing people early were insufficient. In a systematic review by Robinson et al, there is no adequate, robust evidence to recommend the use of any nonpharmacological intervention to reduce wandering in dementia. 23
According to a previous report, 21 in most cases, missing people with dementia are traveling by foot. Traveling by foot also occurred most often among the patients of our study. Prior investigations of the direct distance from individuals’ homes to the sites where they were found dead have indicated that it was frequently less than 1 km as in 21 (54%) of the 39 cases examined by Yamazaki et al, 22 which included individuals who had rode on bicycles and motorbikes as well as on foot. The present study investigated this distance according to the different means of moving and found that 73% of individuals who had moved on foot were found within 500 m of their homes. Distances to sites of death tended to be shorter among those using canes or other walking aids. Our results may serve as useful evidence regarding the area on which an intensive search might focus on for individuals who go missing, which could lead to their early discovery and survival. An individual aged 75 years or older walking on a flat, straight road without any obstacles at a speed of 1.03 m/s (the mean walking speed of persons of this age) 24 will be able to cover a distance of 500 m in a mere 8 minutes. The results of this simple calculation suggest that missing adults with dementia traveling by foot poses potential emergency situations that would need to be addressed in a timely, effective manner.
Japan has become the world’s fastest aging society; its current population of older adults with dementia is expected to swell as a result. In 2010, the Japanese Society of Neurology published treatment guidelines for dementia, in collaboration with the Japanese Society of Psychiatry and Neurology, Japanese Psychogeriatric Society, Japanese Society of Neurological Therapeutics, Japan Society for Dementia Research, and Japan Geriatrics Society. 25 However, there is presently insufficient evidence to produce a consensus protocol for the care of patients with dementia who can no longer safely care for themselves. Incidences of deaths due to dementia-related missing incidents are likely to rise, against a backdrop of increasing numbers of older adults residing alone and decreasing capacities to care for those who are sick, associated with the trend toward smaller nuclear families in Japan. First, society as a whole, in addition to families and caregivers of older adults with dementia, should be well aware of the fact that missing incidents for such individuals is a matter of life and death involving potential emergency situations. In order to build communities and a society in which patients with dementia and their families can lead safe and secure lives, the actual state of deaths due to dementia-related missing incidents among this population warrants further study.
Limitations
Our study of older adults with dementia, who died as a result of becoming lost in the community, had a few limitations. As it was conducted in a single institution with a small sample of forensic autopsy cases, the results from our descriptive study may not be applicable to missing incidents that do not result in death in Japan. Because this was a retrospective study, there were minimal or no data from patients’ medical records on dementia, including severity and pharmacological treatments, and on patients’ caregivers, preventive measures employed to decrease the risk of missing incidents, and interventions for missing incidents. Further collaborative studies with geriatricians, psychiatrists, and nurses who treat or care for people with dementia may help address these limitations and produce an “Elopement Search Template” which could aid rescuers in focusing their search for missing people and thus reduce the time between elopement and rescue.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
