Abstract
Keywords
Introduction
Hepatocellular carcinoma (HCC), a prominent malignant neoplasm, globally ranks highly in both incidence and mortality rates among malignant tumors. Characterized by its insidious onset, the disease often remains asymptomatic during the early stages, making it a considerable challenge for timely diagnosis and intervention. Transhepatic arterial chemoembolization (TACE) currently stands as the preferred clinical approach for the management of intermediate to advanced HCC. 1 As an effective interventional technique, TACE inhibits tumor cell proliferation and extends patients’ survival time by administering a blend of chemotherapeutic agents and iodinated oil via chemoembolic injection.2,3 Nevertheless, employing TACE as a standalone treatment for intermediate and advanced HCC bears significant drawbacks, including a high propensity for recurrence and stimulation of tumorous neovascularization. Such drawbacks can substantially compromise long-term therapeutic effectiveness, proving detrimental to the patient's prognosis. 4 Consequently, the development of effective therapeutic strategies for intermediate to late-stage HCC to improve patient prognosis is an area of significant research interest.
Lenvatinib, a multitarget receptor tyrosine kinase inhibitor, inhibits tumor cell growth by blocking various signaling pathways, including FGFR1-4, and has shown promising applications in the clinical treatment of intermediate and advanced HCC.5,6 Over recent years, blockade of programmed death factor 1 (PD-1) has gained widespread recognition in the clinical treatment of a variety of malignancies, positioning itself as a pivotal immunotherapeutic strategy in managing malignancy. 7 PD-1 and its ligands have demonstrated relative safety and efficacy in treating various malignancies, and are known to effectively impede the immune response evasion in hepatic tumor cells, suggesting promising therapeutic prospects. 8 Despite these advancements, clinical literature remains sparse on the combined approach of lenvatinib, PD-1 monoclonal antibody, and TACE for managing intermediate to advanced HCC. In light of this, our study aims to investigate the therapeutic efficacy of lenvatinib, PD-1 monoclonal antibody, and interventional treatment for intermediate to advanced HCC, particularly examining its impact on serum vascular endothelial growth factor (VEGF) and matrix metalloproteinase-9 (MMP-9) levels. Our findings are intended to provide a reference point for the clinical development of treatment protocols for patients diagnosed with intermediate to advanced HCC. The results of this study are detailed in the following sections.
Materials and Methods
Patient Selection and Data Collection
This study conducted a retrospective analysis of the clinical data of 93 patients with intermediate to advanced hepatocellular carcinoma, treated at our hospital from May 2018 to April 2020. The cohort comprised 52 males and 41 females, ranging in age from 44 to 78 years with a mean age of 58.85 ± 6.84 years. According to the Child-Pugh classification, 60 patients were categorized as grade A and 33 as grade B. In terms of the tumor node metastasis (TNM) stage, 58 patients were stage III and 35 were stage IV, with disease durations ranging from 2 to 10 years, averaging 6.33 ± 2.48 years. Based on the implemented treatment regimens, patients were classified into 2 groups: the control group (n = 43) and the study group (n = 50). Our study was approved by the Ethics Committee of Chinese PLA General Hospital (approval no. YJEJ2205349). The reporting of this study conforms to STROBE guidelines. 9 Due to the retrospective nature of the study, the informed consent was waived by the Ethics Committee of Chinese PLA General Hospital. All patient details were de-identified.
Inclusion and Exclusion Criteria
Inclusion criteria comprised patients who adhered to the diagnostic criteria of primary liver cancer as per established guidelines, 10 confirmed through imaging or pathological examination such as computed tomography. Eligible participants had complete clinical data, aged between 40 and 80 years, with a minimum expected survival time of 6 months, categorized as TNM stage III-IV, and Child-Pugh grade B or C, and had not previously undergone radiotherapy, chemotherapy, or other antitumor drug treatments presented and were subsequently diagnosed with advanced-stage liver cancer after they admitted to hospital due to physical discomfort. Exclusion criteria encompassed allergy to the investigational drugs, comorbid malignancies, severe cardiac, cerebral, renal or other organ failure, pregnancy and lactation, concurrent hematological diseases, psychiatric conditions, coagulation disorders, infectious diseases, history of hepatic or upper abdominal surgery, inability to tolerate the trial treatment, or patients with massive ascites and active bleeding.
Treatment Regimens
The study group underwent treatment with lenvatinib in combination with a PD-1 monoclonal antibody and TACE. Lenvatinib (Chengdu BITE Pharmaceutical Co., Ltd, State Drug Approval H20213811) was orally administered, with the initial dosage set at 8 mg/day for patients weighing <60 kg and 12 mg/day for those weighing 60 kg or more. After 1 to 2 weeks of lenvatinib treatment, TACE was introduced, with lenvatinib discontinued 3 days prior to the procedure.
The specific protocol for TACE involved the patient in the supine position under local anesthesia. The right femoral artery was punctured using the modified Seldinger technique, and a 4F RH catheter was guided into the celiac trunk artery and superior mesenteric artery. Imaging was utilized to ascertain the size and location of the lesion, following which a microcatheter was navigated to the lesion's feeding artery. A mixture of 3 to 6 mL of recombinant human vascular endothelial inhibitor injection (Shandong Xiangsheng Biopharmaceutical Co., Ltd, State Drug Approval S20050088), 50 to 100 mg of oxaliplatin (Yuanda Pharmaceutical Huangshi Feiyun Pharmaceutical Co. Ltd, State Drug Approval H20045982), and an iodized oil suspension was then administered under fluoroscopic guidance until the lesion staining shadow disappeared. The catheter, guidewire, and other devices were subsequently removed, and a routine pressure bandage was applied. Camrelizumab (Suzhou Shengdian Biopharmaceutical Co., Ltd, State Drug Administration S20190027) monotherapy was initiated within 1 to 2 days post-TACE, at a dosage of 200 mg per intravenous infusion, administered every 3 weeks for a total of 6 cycles. The control group received lenvatinib in combination with TACE, where the protocols for administering lenvatinib and TACE mirrored those in the study group. The flow diagram of this study is shown in Figure 1.
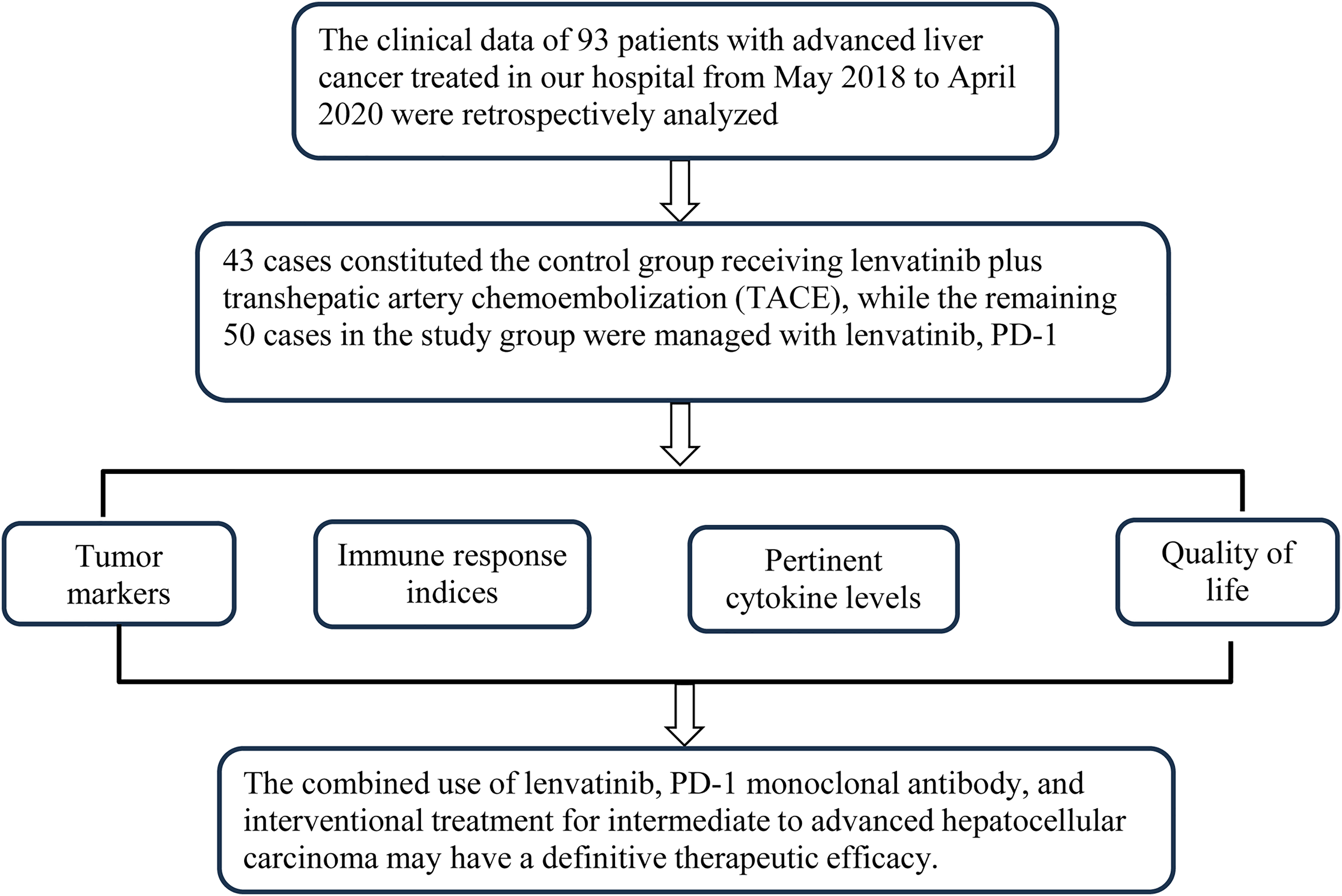
Flow diagram of study design.
Outcome Measures
Clinical efficacy: Efficacy was evaluated using the Criteria for the Evaluation of Therapeutic Efficacy in Solid Tumors. 11 Complete remission (CR) was defined as the total disappearance of target lesions for more than 4 weeks. Partial remission (PR) was defined as a reduction in the sum of all measurable target lesion diameters by ≥30%. Stable disease (SD) was characterized by a < 30% reduction or <20% increase in the sum of all measurable target lesion diameters. Progressive disease (PD) was defined as an increase of ≥20% in the sum of all measurable target lesion diameters or the emergence of a new lesion. The overall response rate was calculated as the sum of the CR and PR rates.
Tumor marker analysis: Fasting venous blood samples were obtained from both groups pretreatment and post-treatment. Serum was isolated following centrifugation at 3500 rpm for 10 min. The levels of carcinoembryonic antigen (CEA), alpha-fetoprotein (AFP), α-L-fucosidase (AFU), and carbohydrate antigen 199 (CA199) were quantified using enzyme-linked immunosorbent assay (ELISA) kits supplied by Nanjing Wanmuchun Biotechnology Co.
Immune function assessment: T-lymphocyte subsets (CD3+, CD4+, CD8+) were analyzed via flow cytometry before and after treatment in both groups, and the CD4+/CD8+ ratio was calculated.
Cytokine analysis: The serum concentrations of VEGF, MMP-9, and both acidic and basic fibroblast growth factors (aFGF and bFGF) were measured using ELISA kits from Beijing Kangrena Biotechnology Co. before and after treatment in both groups.
Quality of life assessment: The Quality of Life Assessment Scale for Cancer Patients (QOL-LC) 12 was used to evaluate patients’ quality of life before and after treatment. This scale evaluates symptoms/side effects (5 items), physical function (6 items), social function (5 items), and psychological function (6 items), with each item scored out of 10. Higher scores indicate a higher quality of life.
Adverse event reporting: The incidences of fatigue, rash, diarrhea, nausea, vomiting, and fever were compared between the 2 groups.
Survival analysis: Patients were followed up until April 2023. Survival rates were compared between the 2 groups at 1, 2, and 3 years after a 3-year follow-up period.
Statistical Analysis
Data analysis was conducted using SPSS version 24.0. The results of tumor markers, immune function, relevant cytokines, and quality of life were presented as mean ± standard deviation (SD). An independent sample t-test was used to compare these variables between groups, while a paired sample t-test was employed for within-group comparisons. The results of clinical efficacy, survival rates, and adverse events were expressed as percentages, with differences between groups assessed using the χ2 test. A P-value <.05 was considered statistically significant.
Results
General Patient Information Comparison
No statistically significant differences were found between the 2 groups when analyzing demographic characteristics such as gender, age, Child-Pugh classification, TNM stage, and disease duration (P > .05). Refer to Table 1 for more details.
Comparison of Clinical Data n (%)/(`χ ± s).

Abbreviations: HBV, hepatitis B virus; HCV, hepatitis C virus; TNM, tumor node metastasis.
Clinical Efficacy Comparison
The study group demonstrated a superior total response rate (74.00%) compared to the control group (53.49%). This difference was statistically significant (P < .05), indicating that the combination of lenvatinib, PD-1 monoclonal antibody, and interventional treatment shows enhanced efficacy for intermediate to advanced hepatocellular carcinoma compared to lenvatinib plus interventional treatment alone. Refer to Table 2 for further details.
Comparison of Clinical Efficacy n (%).
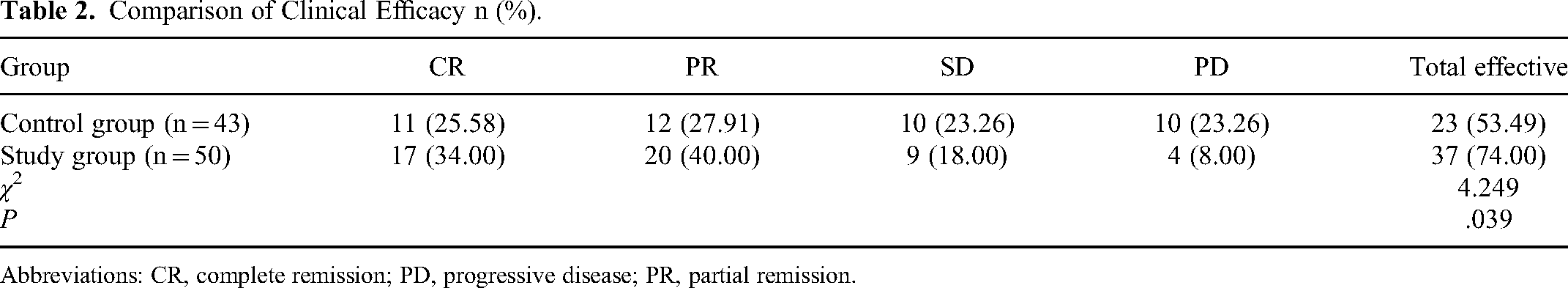

Abbreviations: CR, complete remission; PD, progressive disease; PR, partial remission.
Tumor Marker Comparison
Prior to treatment, no significant differences were observed in the levels of CEA, AFP, AFU, and CA199 between the 2 groups (P > .05). However, following treatment, a significant decrease was observed in both groups for all markers. This decrease was more pronounced in the study group (P < .05). Refer to Figure 2 for a graphical representation.

Effect of lenvatinib + PD-1 monoclonal antibody + interventional therapy on the levels of tumor markers in patients with intermediate to advanced hepatocellular carcinoma. Figure illustrates a significant decrease in levels of (A) CEA, (B) AFP, (C) AFU, and (D) CA199 following the administration of the combination therapy of lenvatinib, PD-1 monoclonal antibody, and interventional treatment, compared to levels pretreatment and post-treatment in the control group. Note: Compared with those before treatment, ***P < .001; compared with the control group, ###P < .001. Abbreviations: AFP, alpha-fetoprotein; AFU, α-L-fucosidase; CEA, carcinoembryonic antigen; CA199, carbohydrate antigen 199; PD-1, programmed cell death protein-1.
Immune Function Comparison
No significant differences were identified in the baseline immune function indicators between the 2 groups (P > .05). After treatment, CD3+, CD4+, and CD4+/CD8+ ratios significantly increased in both groups, but these increases were more substantial in the study group. CD8+ significantly decreased in both groups, but the decrease was more marked in the study group (P < .05). Please see Figure 3 for further details.

Effect of lenvatinib + PD-1 monoclonal antibody + interventional therapy on the level of immune function in patients with intermediate to advanced hepatocellular carcinoma. Figure delineates the augmentation in levels of (A) CD3+, (B) CD4+, and (D) CD4+/CD8+ following the lenvatinib, PD-1 monoclonal antibody, and interventional therapy, contrasted with the levels prior to treatment and those in the control group post-treatment. In contrast, (C) CD8+ levels were significantly attenuated compared to before treatment and post-treatment in the control group. Note: Compared with those before treatment, ***P < .001; compared with the control group, ###P < .001. Abbreviation: PD-1, programmed cell death protein-1.
Cytokine Comparison
No significant differences were detected in the baseline levels of VEGF, MMP-9, aFGF, and bFGF between the 2 groups (P > .05). Following treatment, levels of these cytokines significantly decreased in both groups, but this decrease was more pronounced in the study group (P < .05). Please see Figure 4 for a visual representation.

Effect of lenvatinib + PD-1 monoclonal antibody + interventional therapy on the levels of cytokines VEGF, MMP-9, aFGF, and bFGF in patients with intermediate to advanced hepatocellular carcinoma. Figure depicts a notable reduction in the levels of (A) VEGF, (B) MMP-9, (C) aFGF, and (D) bFGF after the combination treatment of lenvatinib, PD-1 monoclonal antibody, and interventional therapy, in comparison to levels before treatment and those in the control group post-treatment. Note: Compared with those before treatment, ***P < .001; compared with the control group, ###P < .001. Abbreviations: aFGF, acidic fibroblast growth factor; bFGF, basic fibroblast growth factor; MMP-9, matrix metalloproteinase-9; PD-1, programmed cell death protein-1; VEGF: vascular endothelial growth factor.
Quality of Life Comparison
No significant difference was noted in the baseline scores of the QOL-LC scale between the 2 groups (P > .05). However, after treatment, the QOL-LC scale scores were significantly elevated in both groups, with a more pronounced increase observed in the study group (P < .05). Refer to Table 3 for further information.
Comparison of QOL-LC Scale Index Scores Between the 2 Groups`(χ ± S, Points).

Note: Compared with those before treatment, ***P < .05; compared with the control group, ###P < .05.
Adverse Reactions Comparison
The incidence of adverse reactions was comparable between the 2 groups (23.26% vs 26.00%), with no significant difference observed (P > .05). This indicates that the combination of lenvatinib, PD-1 monoclonal antibody, and interventional treatment did not exacerbate adverse reactions, demonstrating satisfactory patient tolerability. See Table 4 for more details.
Comparison of Adverse Reactions n (%).

Survival Comparison
The 1-, 2-, and 3-year survival rates were significantly higher in the study group compared to the control group (P < .05). See Table 5 for additional details.
Comparison of Survival n (%).

Discussion
HCC, a frequently encountered malignancy, presents a complex etiology encompassing environmental factors, chemical substance exposure, cirrhosis, and viral hepatitis. 13 Recent trends indicate an escalating incidence of primary liver cancer, a consequence of the deteriorating global environment, posing a substantial threat to human health. 14 Surgical intervention remains one of the most effective treatments for HCC. However, due to the often asymptomatic nature of early-stage disease, many patients present with advanced or metastatic HCC at diagnosis, having missed the optimal window for surgical intervention. Hence, treatments like interventional therapy, ablative therapy, immunotherapy, and targeted molecular therapy are typically employed to prolong survival.15,16
Our investigation employed a combination therapy of lenvatinib, PD-1 monoclonal antibody, and interventional treatment for patients with intermediate to advanced HCC. The data revealed a superior total response rate in the study group compared to the control (74.00% vs 53.49%). Moreover, post-treatment levels of tumor markers (CEA, AFP, AFU, and CA199) and quality of life, as assessed by the QOL-LC scale, were significantly better in the study group (P < .05). The incidence of adverse reactions was comparable between the 2 groups (P > .05), implying the combination therapy effectively reduces tumor marker levels and enhances patients’ quality of life without compromising safety.
The efficacy of this regimen may be attributed to several factors. Transarterial chemoembolization (TACE) is a preferred interventional treatment for patients with intermediate and advanced HCC as it may effectively occlude tumor-feeding vessels. However, TACE cannot completely eradicate tumor cells, leading to possible recurrence. 17 Lenvatinib, a multitarget receptor tyrosine kinase inhibitor, was initially used in thyroid cancer and has gradually replaced sorafenib as a first-line treatment for intermediate and advanced HCC due to its precise efficacy and survival benefits. 18 Lenvatinib inhibits tumor cell growth by hindering the proliferation of platelet-derived growth factor receptors, fibroblast growth factor receptors, and other oncogenic factors. 19 Simultaneously, lenvatinib promotes apoptosis of tumor cells by inhibiting VEGF receptors kinase insert domain receptor and FMS-like tyrosine kinase 1. 20 Furthermore, lenvatinib enhances the antitumor immune response of PD-inhibitors. 21 Immunotherapy, a relatively novel approach in oncology, employs agents like camrelizumab, an immunosuppressive molecule, to improve T-cell function and destroy tumor cells by interrupting the interaction between T-cell PD-1 protein and tumor cell PD-L1 protein, thereby alleviating T-cell inhibition by tumor cells. 22 Research has indicated that the combined treatment of camrelizumab and famitinib in 38 patients with advanced liver cancer demonstrated effective and enduring antitumor activity. 23 However, reports on the therapeutic application of camrelizumab combined with lenvatinib are limited. This study observed the efficacy of camrelizumab combined with lenvatinib in the treatment of intermediate to advanced hepatocellular carcinoma patients. The results indicated that lenvatinib plus PD-1 monoclonal antibody combined with interventional therapy demonstrated definite effect for intermediate to advanced hepatocellular carcinoma, significantly reducing tumor marker levels, improving survival rates, and yielding favorable prognosis. This suggests that PD-1 monoclonal antibody in combination with other drugs may be a more effective approach for patients with intermediate to advanced hepatocellular carcinoma, worthy of clinical recommendation.
Research has shown that immune function is intimately linked with the progression of malignancies, as patients with intermediate and advanced HCC often exhibit an immune dysregulation that fosters immunosuppression. This enables tumor cells to evade immunological recognition and clearance, thereby promoting malignancy. 24 Our study demonstrated significantly improved CD3+, CD4+, and CD4+/CD8+ ratios, and decreased CD8+ levels in the study group after treatment (P < .05). These results suggest that our combination therapy may enhance immune function and aid recovery in patients with intermediate to advanced HCC.
Tumor proliferation, infiltration, and metastasis primarily determine malignancy and rely on neovascularization and extracellular matrix degradation. 25 VEGF, an essential regulator of neovascularization, fosters tumor genesis, invasion, and metastasis by inducing neovascularization, which in turn accelerates tumor progression. VEGF also increases MMP-9 activity, promoting tumor cell invasion and metastasis through activation of multiple protein kinase pathways. MMP-9, an extracellular matrix protease, can degrade various collagen types in the extracellular matrix and basement membrane, facilitating tumor cell invasion and metastasis. Moreover, MMP-9 promotes tumor neovascularization and enhances tumor cell survival. A study by Zhu et al 26 found that levels of VEGF and MMP-9 in patients with malignancies were significantly higher than those in healthy individuals. Additionally, aFGF and bFGF can induce liver tumor neovascularization and tumor cell proliferation and metastasis. Our study revealed significantly lower post-treatment levels of VEGF, MMP-9, aFGF, and bFGF in the study group (P < .05), suggesting that our combination therapy may inhibit tumor neovascularization and promote tumor cell apoptosis in patients with intermediate to advanced HCC by modulating levels of VEGF, MMP-9, and other related cytokines.
Notably, our study also showed higher 1-, 2-, and 3-year survival rates in the study group compared to the control group (P < .05), highlighting that our combination therapy can effectively enhance survival rates and improve prognosis in patients with intermediate and advanced HCC.
Conclusions
In summary, the lenvatinib, PD-1 monoclonal antibody, and interventional treatment combination for intermediate-advanced stage HCC effectively reduced tumor marker levels, improved immune function, regulated levels of VEGF, MMP-9, and other related cytokines, without increasing adverse effects. This approach led to an improved quality of life and survival rates, yielding a favorable prognosis. However, this study does have limitations. There is a lack of nonrandomization in data review. Additionally, due to the small number of patients using lenvatinib, it is not possible to estimate the sample size, resulting in small sample size and singular data source, which may lead to biased results. In the next step, a large-scale prospective randomized controlled study in multiple clinical centers with an expanded sample size will be conducted, so as to validate the findings of this study.
Footnotes
Abbreviations
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statement
Our study was approved by the Ethics Committee of Chinese PLA General Hospital (approval no. YJEJ2205349). All patients provided written informed consent prior to enrollment in the study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
