Abstract
Canada's legalization of Medical Assistance in Dying (MAiD) in 2016 has had important implications for nursing regulators. Evidence indicates that registered nurses perform key roles in ensuring high-quality care for patients receiving MAiD. Further, Canada is the first country to recognize nurse practitioners as MAiD assessors and providers. The purpose of this article is to analyze the documents created by Canadian nursing regulatory bodies to support registered nurse and nurse practitioner practice in the political context of MAiD. A search of Canadian provincial and territorial websites retrieved 17 documents that provided regulatory guidance for registered nurses and nurse practitioners related to MAiD. Responsibilities of registered nurses varied across all documents reviewed but included assisting in assessment of patient competency, providing information about MAiD to patients and families, coordinating the MAiD process, preparing equipment and intravenous access for medication delivery, coordinating and informing health care personnel related to the MAiD procedure, documenting nursing care provided, supporting patients and significant others, and providing post death care. Responsibilities of nurse practitioners were identified in relation to existing legislation. Safety concerns cited in these documents related to ensuring that nurses understood their boundaries in relation to counseling versus informing, administering versus aiding, ensuring safeguards were met, obtaining informed consent, and documenting. Guidance related to conscientious objection figured prominently across documents. These findings have important implications for system level support for the nursing role in MAiD including ongoing education and support for nurses' moral decision making.
Keywords
On June 17, 2016, the Criminal Code of Canada was changed to permit Medical Assistance in Dying (MAiD) (Bill C-14, 2016). Historically, registered nurses have played an important, albeit largely undocumented, role in assisted death. For example, evidence from countries where assisted death is legal has revealed that nurses play key roles in negotiating requests, participating in decision making, and supporting clients and families throughout the process (De Bal, Dierckx de Casterle, De Beer, & Gastmans, 2006; De Beer, Gastmans, & Dierckx de Casterle, 2004; Denier, Gastmans, De Bal, & Dierckx de Casterle, 2010; Dierckx de Casterle, Denier, De Bal, & Gastmans, 2010; Dierckx de Casterle, Verpoort, De Bal, & Gastmans, 2006; van de Scheur & van der Arend, 1998). Beyond the important role that registered nurses perform in assisted death, Canada became the first country to permit nurse practitioners to act as MAiD assessors and providers. As such, the legalization of MAiD in Canada has important implications for nursing practice.
Nursing Regulation in Canada
Canada has 10 provinces and 3 territories. The Canadian Nurses Association (CNA) is the national voice of Canadian nursing. The regulation of nursing occurs at the provincial and territorial levels. Regulated nurses include licensed practical nurses, registered psychiatric nurses, registered nurses, and nurse practitioners. The groups of regulated nurses relevant to this discussion are registered nurses and nurse practitioners. Nurse practitioners are the only group of regulated nurses whose full scope of practice includes diagnosing medical conditions and prescribing medications to treat them. In this article, when we refer to registered nurses we are specifically referring to nurses who hold the regulatory title of registered nurse (RN) and do not hold the nurse practitioner (NP) credential. Further, when we use the general designation nurses, we are referring to both registered nurses and nurse practitioners.
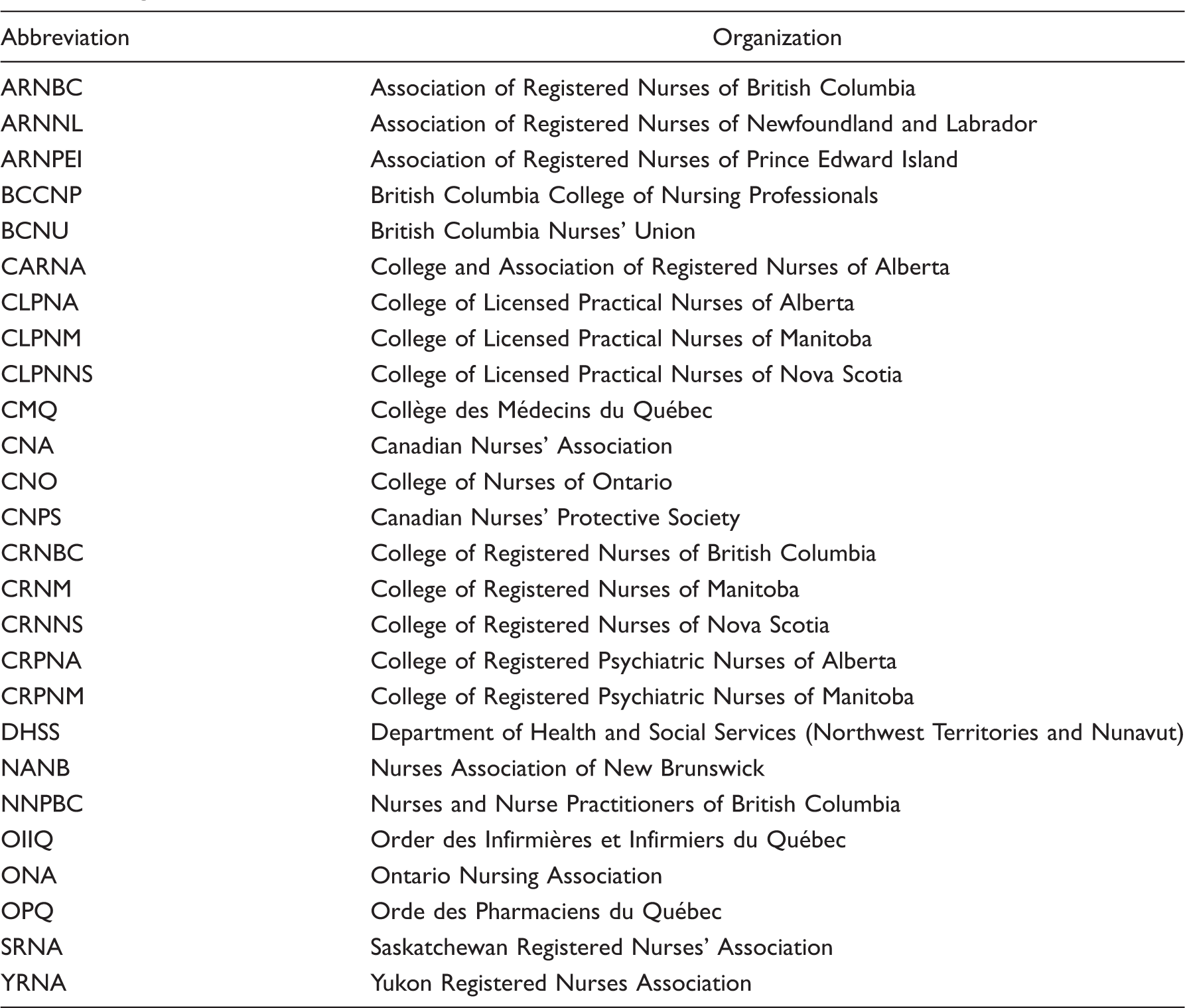
Organizational Abbreviations.
Political and Historical Background of MAiD in Canada
In Canada, until June 2016, all forms of assisted suicide were punishable by law under section 241 of Canada's Criminal Code (Dalhousie University Health Law Institute, 2018). However, in February 2015, the Supreme Court of Canada released its landmark decision which struck down the Criminal Code's prohibition on assisted suicide on the basis that it violated section 7 of the Canadian Charter of Rights and Freedoms, an individual's constitutional right to life, liberty, and security of the person (Carter v. Canada, 2015). Under the Supreme Court's 2015 ruling, the federal government was given 12 months to craft legislation that would regulate MAiD in Canada. At this point, the federal government could have declined to craft legislation and MAiD would have been regulated provincially, similar to other health care services (Downie & Chandler, 2018). However, in June 2016, after considerable public and parliamentary debate, Bill C-14: An Act to amend the Criminal Code and to make related amendments to other Acts (medical assistance in dying) received Royal Assent, thereby introducing assisted suicide into Canadian legislation. Under Bill C-14, MAiD is defined as: (a) the administration by a medical practitioner or nurse practitioner of a substance to a person, at their request, that causes their death; or (b) the prescribing or providing by a medical practitioner or nurse practitioner of a substance to a person, at their request, so that they may self-administer the substance and in doing so cause their own death. (Bill C-14, 2016) (a) they are eligible – or, but for any applicable minimum period of residence or waiting period, would be eligible – for health services funded by a government in Canada; (b) they are at least 18 years of age and capable of making decisions with respect to their health; (c) they have a grievous and irremediable medical condition; (d) they have made a voluntary request for medical assistance in dying that, in particular, was not made as a result of external pressure; and (e) they give informed consent to receive medical assistance in dying after having been informed of the means that are available to relieve their suffering, including palliative care. (Bill C-14, 2016)
Throughout the time that parliament was debating the bill, the CNA performed an advocacy role by monitoring the political process and speaking on behalf of nurses. After the Supreme Court ruling in 2015, the CNA released the following statement: CNA respects the Supreme Court of Canada's decision and welcomes the opportunity to work with physicians, federal, provincial and territorial governments as policies and practices are developed. Our first priority, as always, is supporting RNs in delivering the best care to Canadians. (CNA, February 9, 2015)
The Canadian legislation has been significant for nursing in two major ways. First, nurse practitioners can now act as MAiD assessors and providers, a role that carries significant legal and ethical responsibilities. Second, how Canadian lawmakers enacted MAiD has impacted practice. Of all the ways that assistance in dying can be permitted in a country, legislation carries the highest degree of obligation (Luzon, 2018). This obligation means that “people are legally bound by a rule, so that their behavior is subject to examination under the general rules, procedures, and discourse of the law” (Luzon, 2018, p. 7). The rules and procedures that govern MAiD in Canada place a high degree of obligation on nurses to ensure that eligible patients are granted their right to MAiD and that it is conducted in compliance with the law.
Under the legislation, part of this compliance includes ensuring that individuals requesting MAiD have access to palliative care. However, the limited availability of palliative care in many parts of Canada makes this obligation a significant source of moral tension for health care providers (Collins & Leier, 2017; Schiller, 2017). Nurses who receive requests for MAiD may have difficulty fulfilling this obligation as there may be limited or no available palliative care resources in their community. For this, and other reasons, the introduction of MAiD has been particularly difficult for some health care providers working within palliative care (Bernard, 2018; Canadian Hospice Palliative Care Association, 2013).
Given these important obligations, and the implications that they have for professional nursing practice, our research team conducted a systematic review to gather the available evidence on the practice, policy, and ethical implications of MAiD for nursing (Pesut et al., 2019; Pesut et al., 2019). Having this evidentiary base is critical for ensuring that nurses can practice safely, ethically, and confidently within this new treatment option. This is particularly important in light of the legal and ethical considerations that are part of MAiD practice, and the impact that participating in a MAiD death can have on nurses (Denier, Dierckx de Casterle, De Bal, & Gastmans, 2010).
The purpose of this article is to provide an overview and analysis of the Canadian nursing regulatory documents that were identified as part of our research team's systematic review. We begin by describing the methods of the review, followed by a summary of the review's results and key findings. Next, we explain the relevant safety concerns identified within these documents and the issue of conscientious objection. We conclude by discussing the findings in relation to the existing empirical literature by delineating implications for practice, policy, and research.
Methods
To gather the regulatory literature that is the focus of this article, we conducted a web-based search in May of 2018 to collect MAiD-related regulatory documents from each province and territory in Canada. In addition to documents identified through nursing regulatory websites, we searched other relevant nursing websites such as unions, associations (specifically those that do not have a regulatory role), and the CNA. Additional documents from the following four nonregulatory associations were identified but not included in the analysis because these organizations had no regulatory responsibilities: CNA (2017b), British Columbia Nurses Union (2017), Association of Registered Nurses of British Columbia (now NNPBC; 2016), and Ontario Nurses' Association (2016).
The regulatory documents were downloaded into NVivo11 for analysis. Analytic questions were derived inductively based upon the content of the documents and included the following: (a) What is the length of the document and what other sources are considered relevant or important? (b) How are various roles and responsibilities described? (c) What are the safety considerations? (d) What is common content across documents and what is unique? We used a qualitative descriptive approach to the coding which was further informed by interpretive description (Sandelowski, 2010; Thorne, 2016). A qualitative descriptive approach seeks to produce thematic surveys that stay close to the original data (Sandelowski, 2010). We first read the documents to identify common conceptual content that then became codes which we used to code all of the documents. We then compared and contrasted these conceptual categories to determine similarities and differences. Finally, we constructed a thematic summary that represented similarities and differences across documents. The initial analysis was conducted by the lead investigator (B. P.). Themes were discussed and negotiated by the research team which, alongside academic members, included representatives who were embedded in regulatory practice in national and provincial contexts. These representatives were chosen by the team based upon their participation in the development of MAiD-related nursing regulatory policies. Negotiation was conducted via teleconference and email and only concluded when all members of the team were satisfied with the account provided.
Results
Overview of Regulatory Documents.
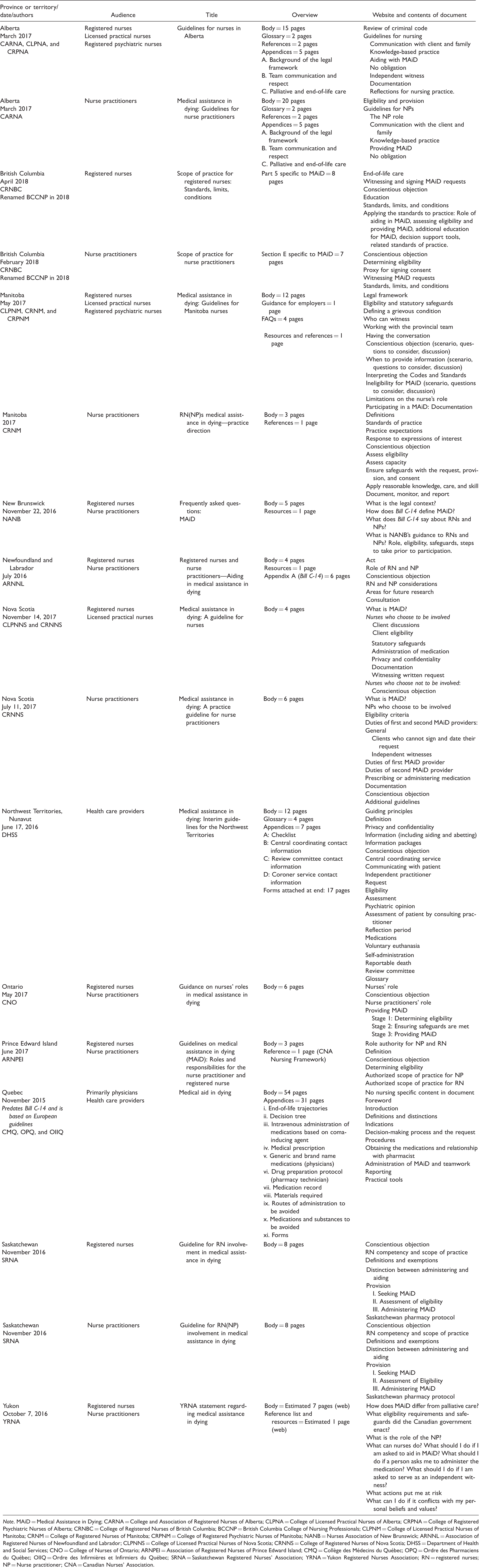
Note. MAiD = Medical Assistance in Dying; CARNA = College and Association of Registered Nurses of Alberta; CLPNA = College of Licensed Practical Nurses of Alberta; CRPNA = College of Registered Psychiatric Nurses of Alberta; CRNBC = College of Registered Nurses of British Columbia; BCCNP = British Columbia College of Nursing Professionals; CLPNM = College of Licensed Practical Nurses of Manitoba; CRNM = College of Registered Nurses of Manitoba; CRPNM = College of Registered Psychiatric Nurses of Manitoba; NANB = Nurses Association of New Brunswick; ARNNL = Association of Registered Nurses of Newfoundland and Labrador; CLPNNS = College of Licensed Practical Nurses of Nova Scotia; CRNNS = College of Registered Nurses of Nova Scotia; DHSS = Department of Health and Social Services; CNO = College of Nurses of Ontario; ARNPEI = Association of Registered Nurses of Prince Edward Island; CMQ = Collège des Médecins du Québec; OPQ = Ordre des Pharmaciens du Québec; OIIQ = Ordre des Infirmières et Infirmiers du Québec; SRNA = Saskatchewan Registered Nurses' Association; YRNA = Yukon Registered Nurses Association; RN = registered nurses; NP = Nurse practitioner; CNA = Canadian Nurses' Association.
Document Overview
The length of a document may be a proxy for the perceived importance and potential risks of MAiD for nursing. The main bodies of these documents varied between 3 and 15 pages. Notably, there was little difference between the length of the documents created for registered nurses and the length of the documents created for nurse practitioners, despite the significant differences in their scopes of practice in relation to MAiD. In some provinces the MAiD-related practice information was located within currently existing regulatory documents (e.g., Standards, Limits and Conditions in BC), whereas, in other provinces (CARNA, 2017; CARNA et al., 2017; CRNM, 2017; CRNM et al., 2017; SRNA, 2016a, 2016b), resources had been dedicated specifically to MAiD. The two documents that provided guidance to nurses in a multidisciplinary document were more extensive at 18 and 54 pages. These documents from Quebec (CMQ et al., 2015) and the Northwest Territories (DHSS, 2016) included information relevant to all team members and hence provided more information for nurses. For example, the inclusion of information related to appropriate medication use, interdisciplinary expectations, and provincial guidelines and checklists gave nurses a more comprehensive overview of the MAiD process. Reference lists varied from a single reference to two pages, suggesting that the degree to which documents drew upon external or peer-reviewed sources varied widely.
The regulatory documents created for registered nurses and nurse practitioners contained common content, derived from the legislation, across provinces and territories. However, the depth to which that content was discussed, how MAiD was positioned in relation to nursing, and the supplementary resources included were varied. For example, Nova Scotia provided a concise four-page overview (CRNNS & CLPNNS, 2017), while Alberta, Manitoba, and Saskatchewan provided more extensive coverage that included supplementary materials to support practice (CARNA, 2017; CARNA et al., 2017; CRNM, 2017; CRNM et al., 2017; SRNA, 2016a, 2016b). Typical supplementary materials included the Criminal Code, relevant guidelines, flow charts, case studies, frequently asked questions, and self-reflective practices.
The purposes of the regulatory documents reviewed were to raise nurses' awareness; to guide nurses' ethical reflection; to provide practical guidance for nurses; and to inform nurses of their roles, responsibilities, and accountabilities. Many of the documents referred to a number of other policies to which registered nurses and nurse practitioners were accountable in their MAiD-related practice. For example, nurses needed to know all applicable MAiD-related information from the following: employer standards, guidelines, and policies; provincial MAiD team guidelines, standards, and policies; nursing codes of ethics; guidelines from other regulatory bodies (e.g., physicians and surgeons, pharmacists); MAiD and other affiliated legislation; and guidelines from the Canadian Nurses Protective Society, a not-for-profit society that offers professional liability protection and legal advice to nurses. So, although the regulatory documents espoused a variety of purposes in relation to nursing practice, nurses also needed to be aware of many more standards, policies, and procedures that governed their practice in relation to MAiD.
We identified the following themes from these regulatory documents: roles and responsibilities of registered nurses, safety concerns, conscientious objection, and the relationship of MAiD to palliative care. When reviewing these findings, it is important to remember that a particular finding may not be common across all documents and that the examples provided are not exhaustive. There was a great deal of overlap between the information provided to registered nurses and nurse practitioners, hence, we integrate the information here.
Roles and responsibilities of registered nurses
Responsibilities of Regulated Nurses.
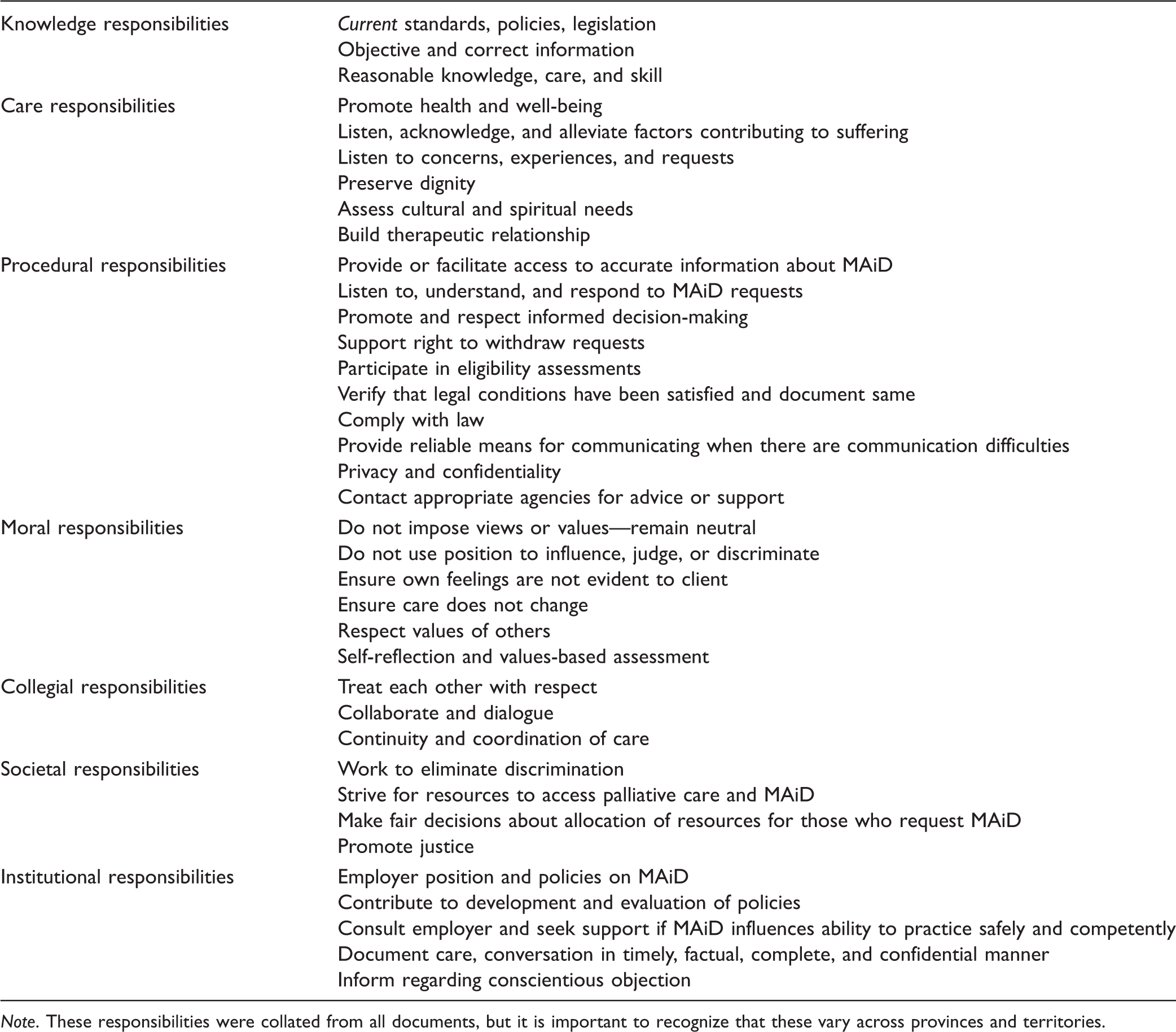

Note. These responsibilities were collated from all documents, but it is important to recognize that these vary across provinces and territories.
The British Columbia document also specified that registered nurses would require further education pertaining to MAiD (BCCNP, 2018b). A PowerPoint presentation with follow-up discussion was provided as an example of suitable education (p. 53). The documents from both Alberta and Manitoba provided important questions for registered nurses to consider when evaluating their role and competency to participate in MAiD (CARNA et al., 2017; CRNM et al., 2017). For example, in the Manitoba document, nurses were encouraged to ask themselves how they might respond if they were asked about MAiD (p. 16), and in the Alberta document, they were asked if they were aware of their own responses to suffering and death (p. 16).
Differing emphases on the role of registered nursing in MAiD were further illustrated by differences in the language used to describe nursing practice. For example, some documents emphasized that nurses participate in the MAiD process only in the capacity of aiding the physician or nurse practitioner who is the legal MAiD provider. However, language was also used to emphasize the unique and intense relational nature of nursing practice (e.g., knowing patients' best, one-on-one relationships, and acting as a vital link with the team). In other words, while registered nurses only aid in the MAiD procedure, they play an important relational role in the MAiD process.
Safety concerns
The documents identified five issues as possible safety concerns, which are discussed here, for nurses that could potentially lead to indictable offenses. Often these sections of the document were highlighted or bolded, thereby emphasizing their importance.
Counseling versus informing
The documents instructed nurses and nurse practitioners to inform clients about the option of MAiD, while refraining from anything that could be construed as counseling to commit suicide. The language was emphatic in some documents. For example, the document from the Northwest Territories instructed nurses to exercise “extreme caution to ensure they do not recommend, incite, or encourage medical assistance in dying” (DHSS, 2016, p. 4). This particular passage was underlined and written in red font. The document produced by Newfoundland (ARNNL, 2016) delineated the difference between therapeutic counseling and counseling, as defined in the Criminal Code. It encouraged nurses to explore meaning and to offer information about the availability of MAiD while refraining from encouraging, suggesting, recommending, advising, or inciting uptake.
The documents further instructed nurses about their responsibility to inform patients about MAiD. Clients must request information in such a way that it is clear that they are requesting information about MAiD and not simply expressing a desire to die. Once it is clear that a client is referring to MAiD (usually by using the terminology), there were differences among the provincial and territorial documents with respect to how the requirement to provide information about MAiD was emphasized. For example, the document from Alberta emphasized the constitutional right of individuals to have accurate information about MAiD (CARNA et al., 2017). Nurses who felt unable to give that information had to refer the client to someone who could. In the Nova Scotia document, that right to know was somewhat softened (CRNNS, 2017). Nurses “may” engage in the conversation or they “may” refer to other health care providers who are in a “better position to respond” (pp. 1–2). However, it required nurses to report the request to the primary care provider and to document the conversation.
Administering versus aiding
The safety issue of administering versus aiding was discussed in the context of the procedure of giving the medication that caused death. Nurse practitioners are MAiD providers, so this particular safety issue was not evident in those documents that were created specifically for their practice. However, the registered nurse's role in MAiD includes all aspects of procedural support except for administering medications or managing the unintended consequences of medications. Some regulatory documents emphasized that registered nurses do not pick up medications from the pharmacy or dispose of them and that there must be careful boundaries around patient self-administration of medication. Registered nurses must not aid in any way except to pass a medication to a patient when it has been requested by the patient. Nothing can be done to ease self-administration of the medication, such as mixing the medication with food or liquid (e.g., ARNPEI, 2017; CARNA et al., 2017).
Ensuring safeguards are met
The third safety issue pertained to the responsibility of nurses to ensure that appropriate safeguards were met prior to providing or participating in MAiD. Nurse practitioners are accountable to ensure safeguards are met; however, the role of the registered nurse related to safeguards was a bit more tenuous. For example, in the document from Saskatchewan, assessment of whether a patient was eligible for MAiD was clearly the role of the physician or nurse practitioner. Registered nurses were “not responsible to ensure safeguards are met” (SRNA, 2016a, p. 6). However, this was qualified by stating that “nurses should not assist if there is reason to believe that these safeguards are not met and should inform the team of the concerns” (p. 6). The document from Alberta stated that prior to aiding a physician or nurse practitioner in the provision of medical assistance in dying, nurses ensure that they are aware of the eligibility parameters, safeguards and requirements for medical assistance in dying and have a reasonable objective basis to support that the physician or nurse practitioner providing medical assistance in dying has met all requirements as set out in legislation. This needs to be done through reliable sources of information. (CARNA et al., 2017, p. 11)
Obtaining informed consent
According to the legislation, registered nurses and nurse practitioners may act as witnesses in the informed consent process if they are not directly involved in providing health care services or direct care to that patient. What constitutes direct health care services or care was not always clear. Alberta provided clarification of who is a direct care provider by indicating that any nurse who has provided care to the client or who may anticipate providing care to the client would be ineligible to act as a witness (CARNA et al., 2017, p. 13). However, most documents did not define direct involvement as clearly as Alberta leaving it to the clinician to decide whether what they were doing constituted health care or direct services.
Documenting
Lastly, documentation was often highlighted as a safety concern. The documents cautioned registered nurses and nurse practitioners to only document the care they provided. They also emphasized the criminal nature of inappropriately altering documents. This emphasis on documentation was an interesting safety concern in light of the fact that such documentation guidelines are already accepted nursing practice. However, from a regulatory perspective, complete and accurate documentation in all aspects of nursing practice is an area of ongoing concern. The impact and legal implications of MAiD make this clarity regarding documentation particularly important.
To assist registered nurses and nurse practitioners in mitigating the above safety concerns, documents commonly instructed nurses to contact their regulatory body, their protective society, and in some cases, their employer for guidance and advice should they choose to participate in MAiD.
Conscientious objection
Conscientious objection figured prominently in all documents. Most documents took the position that nurses must opt out of MAiD if they do not wish to participate in it. In other words, participation is assumed unless nurses informed their employer that they have a conscientious objection. However, other documents assumed an opt-in position through the use of language such as “if they choose to participate” (SRNA, 2016a, 2016b, p. 2) or “once a nurse has decided to participate” (CRNM et al., 2017, p. 15) or “nurses who choose to be involved” (CRNNS, 2017, p.1). The difference was subtle but important in that one perspective assumes that nurses participate unless they conscientiously object, while the other assumes that nurses do not participate unless they choose to do so.
Those nurses who do conscientiously object must do so on the basis of informed and reflective choice. According to the document from Manitoba, this choice should be based upon a “longstanding and deeply held belief” (CRPNM, 2017, p. 8). Further, nurses must not convey this conscientious objection to clients and client families. Instead, nurses are required to inform their employer in a timely manner so that the employer can make other arrangements for the patient's care. Employers are responsible for establishing procedures to manage a conscientious objection. Nurses' degree of involvement in MAiD may vary. For example, the Manitoba document listed tasks that nurses should reflect on to determine their comfort levels with MAiD (CRPNM, 2017). This same document indicated that even those who conscientiously object “are required to continue providing any routine care that is not related to medical assistance in dying” (p. 7) and that failure to do so could result in a claim of client abandonment. This is in keeping with the CNA Code of Ethics statement that requires nurses to provide “safe, compassionate, competent and ethical care until alternative care arrangements are in place to meet the person's needs or desires” (2017a, p. 17).
The documents we reviewed encouraged nurses to reflect on what it means to be both a person and a professional in a situation of MAiD. As people, nurses are required to reflect on their own values and beliefs. As professionals, they are required to respect the values and beliefs of others. This is an interesting obligation and raises the question of whether one can respect competing values or whether one actually respects the person holding those values—this may be a subtle but important distinction. Although respecting diverse values and beliefs is common to the nursing role, it does imply a type of moral relativism that can be avoided if nurses instead choose to respect the person who may happen to hold different values than the nurse. In the situation of different values, nurses have a number of professional responsibilities that include not disclosing their own values to clients or compromising care (see Table 3). Several documents provided supplementary material to assist nurses in reflecting on their values. For example, Manitoba provided a case study, reflective questions, and outlined possibilities for participation while Alberta provided an appendix on team communication and respect (CARNA et al., 2017; CRNM et al., 2017).
Relationship of MAiD to palliative care
The issue of whether MAiD should be considered just one more end-of-life option within palliative care or whether it is antithetical to the palliative philosophy of neither hastening nor postponing death has characterized some of the debate about the relationship of MAiD to palliative care in Canada. Several regulatory documents situated MAiD by emphasizing close alignment between nursing's role in palliative care and nursing's role in MAiD. For example, the Manitoba document suggested that in the context of palliative care, expressed wishes to die are not new, therefore “end of life conversations do not have to change” (CRNM et al., 2017, p. 16). Similarly, the Nova Scotia document emphasized the important role that nurses play in end-of-life care and stated that MAiD “does not change nurses' accountabilities as they relate to clients who are seeking advice or requiring palliative care” (CRNNS, 2017, p. 4). In contrast, the BC document made an “important and notable distinction between the intended outcomes of MAiD and palliative care,” distinguishing and outlining the nursing roles in these two contexts (BCCNP, 2018b, p. 48).
Under Canada's MAiD legislation, patients considering MAiD must be offered palliative care. Importantly, advocacy for equitable access to health care services, such as palliative care, is an important responsibility for professional nursing practice (CNA, 2017b). As such, the documents from Alberta indicated that the role of the nurse in the context of MAiD includes advocating for better palliative care (CARNA et al., 2017; CARNA, 2017). The documents from Saskatchewan acknowledged the federal commitment to improving access to palliative care without necessarily situating this within a nursing responsibility (SRNA, 2016a, 2016b).
Discussion
The purpose of this article was to provide an overview and analysis of the Canadian nursing regulatory documents that were developed in response to the legalization of MAiD in Canada. Although there was a common and congruent message about registered nurses' and nurse practitioners' obligations in relation to the MAiD legislation, how nursing regulatory organizations chose to present and augment that message was diverse.
A number of countries are in the process of decriminalizing or legalizing assisted death and we can anticipate that, similar to what has happened in Canada, nurses will play an important role. Findings from this review illustrate the many factors that Canadian nursing regulatory agencies felt to be significant, and hence, needed to be addressed in regulatory documents. Although the substance of the legislation will be different across contexts, the breadth and substance of the information provided by Canadian nursing regulatory agencies to guide nursing practice may be useful for persons responsible for creating nursing regulation and policy in relation to assisted death. Further, for those nursing regulatory bodies in a position to influence evolving legislation, these documents highlight important issues for consideration such as the involvement of nurse practitioners as assessors and providers, the roles and responsibilities of registered nurses, important safety considerations, and how to negotiate conscientious objection. In the remaining discussion, we present the implications of these findings for practice, policy, and research.
Implications for Practice
Assisted dying, when implemented as part of the health care system as has been done in Canada, has important implications for nursing practice. When MAiD is enacted through legislation with its accompanying obligations, it is essential that nurses receive (a) education to perform their responsibilities competently and (b) support to assist their moral decision-making. Information contained in these regulatory documents indicated the substantial amount of knowledge that nurses require to feel confident to participate in MAiD. This includes knowledge of the regulatory environment, the actual procedure relative to their context, and the practice knowledge required to give good care within such unique circumstances. Nurses also need to feel confident in their abilities to use that knowledge. The legislative approach to assisted death, with its attendant obligations, rules, and procedures means that nurses are participating in a care context that can be perceived as high risk and high impact. Nurses risk criminal conviction, civil liability, and professional discipline if their care does not align with legislated roles and safeguards. The procedure itself is high impact in that the expected outcome is irreversible. This may explain why studies of nurses' experiences with hastened death in other jurisdictions have suggested that nurses carry a heightened sense of responsibility (Elmore, Wright, & Paradis, 2018). Nurses need to receive education and support commensurate with those responsibilities.
Further, nurses require support to assist them with their moral decision-making when choosing to participate in such a potentially contentious procedure. Evidence from other countries has indicated that it takes time for nurses to develop in their role in relation to MAiD and that this development often impacts who they are as people. “Nurses reported that being involved in caring for patients requesting euthanasia has had an impact on their own identities, on who they are and how they view life” (Denier, Dierckx de Casterle, De Bal, & Gastmans, 2009, p. 270). Although all of the documents reviewed recognized the right of nurses to conscientiously object to participating in MAiD, there was a lack of acknowledgement of how nurses grow into these decisions over time, and the moral work required for that growth. The enactment of MAiD, or any form of assisted death, has important educational and moral implications for nurses in practice. Nurses must feel capable of engaging in their role with the full confidence that they are acting within the law. Without this knowledge and confidence, nurses may decline to participate, even if they are not conscientious objectors, leaving patients with insufficient support during times of difficult decision-making. A systems approach is required to support nurses as they become involved in MAiD, and just as importantly, this support needs to continue in the days, months, and years following implementation.
Implications for Policy
Two policy concerns become particularly important for nursing when assisted dying is introduced in a geographic context. The first relates to the roles and proximities nurses will have as a result of the method chosen for assisted dying. The second relates to the types of ambiguities that might arise for nursing as a result of the legalities that govern the practice of assisted dying.
Under the Canadian legislation, nurse practitioners have a clearly defined role as MAiD assessors and providers and the importance of the role is clear. However, it has been less clear for registered nurses who find themselves in an aiding rather than a providing role. The differing emphasis placed on the nursing role among these regulatory documents illustrates this lack of clarity for nurses. The nursing ethics literature widely acknowledges the importance of the nurse patient relationship in the context of assisted dying (Pesut et al., 2019). It describes this relationship as one in which nurses and patients co-construct meaning in a relationship of trust, caring, respect, and altruistic beneficence (Davis, 1994; Ferrell & Rivera, 1995; Hawkey, 1997). When the nursing role in MAiD is de-emphasized, nurses are placed in the paradoxical position of being in a close interpersonal relationship with a patient while potentially being peripheral to a procedure that will bring a finality to that relationship. How nurses experience the conclusion of the relationship will most likely depend upon the degree to which they are involved in the process of MAiD.
Further, studies from other countries where assisted dying is permitted have revealed the important roles nurses perform in discerning the intent of the initial requests, seeking to identify and remediate suffering, and providing supportive care for clients and family (De Bal et al., 2006; De Beer et al., 2004; Denier, Dierckx de Casterle, et al., 2010; Dierckx de Casterle et al., 2010; Dierckx de Casterle et al., 2006). If the nursing role is de-emphasized, there is a significant risk that these important roles will not be performed, potentially causing both moral distress for nurses and poor quality of care for clients. When assisted dying is integrated into health care, and hence placed into close proximity with nursing practice, policies should clearly recognize and support nursing contributions to care, even if nurses perform an aiding as opposed to an administering role.
The second policy implication relates to the potential legal ambiguities inherent in the process of assisted dying. In the Canadian context, ambiguities surrounding the language describing MAiD eligibility have been endemic (Downie & Chandler, 2018). Terms such as “reasonably foreseeable natural death,” “serious and incurable condition,” “intolerable suffering,” and “irreversible decline in capability” are all concepts that must be interpreted using clinician judgement (A.B. v. Canada, 2017). Anecdotal evidence from across Canada has indicated that there is substantial clinician variability in interpreting these terms. Therefore, one of the most important policy implications is to assist nurses in navigating this complex and ambiguous landscape.
Implications for Research
The regulatory documents reviewed in this article were developed immediately after the legislation was passed and without knowledge of how MAiD would be implemented within the day to day realities of nursing practice. Gathering primary evidence about nurses' and nurse practitioners' experiences with MAiD in the Canadian context is an important focus for research (e.g., Beuthin, 2018; Beuthin, Bruce, & Scaia, 2018). Our team is currently conducting a qualitative study of Canadian nurses' experiences with MAiD with the view of informing the development of policy and practice. Gathering data about the other regulations impacting nursing practice, such as those created by health regions, is another important focus for further research.
An important limitation of this article is that it is a textual analysis that does not incorporate the context of document development. Authors of the article who were embedded within regulatory practice suggested that attention to language is paramount. Further, documents were developed with sensitivity to each provincial and territorial context. Such nuances cannot be adequately captured in a document analysis. Despite these contextual differences, there were common findings that have implications for system level development of nursing practice in the context of MAiD. Further, this review was conducted in 2018, and as this is a rapidly changing area of practice, documents may have been revised since that time.
Conclusion
Since the legalization of MAiD in Canada in 2016, there has been increased uptake by patients, particularly in urban areas of British Columbia and Ontario. A report covering January to December 2017 indicated that there were 1,961 MAiD deaths, bringing the total since legislation enactment to 3,714. Only one death in 2017 was self-administered and nurse practitioners were providers in 5% of the clinician-administered deaths (Health Canada, 2018). Preliminary qualitative evidence collected from interviewing Canadian nurses has indicated that some nurses are becoming increasingly comfortable with MAiD and see it as an essential part of patient-centered care; others remain more reluctant. Health regions have effectively mobilized teams, policies, and procedures to ensure that patients have accessibility to MAiD, an important consideration under the Canadian Charter of Rights and Freedoms. Anecdotally, access remains a problem in some geographic areas. Despite these differences, there is wide agreement that MAiD is an impactful development in Canada. Nursing regulators across Canada have done an admirable job of providing guidance to nurses about MAiD through the documents reviewed in this article. But, much remains to be done in addressing system wide issues to promote good nursing practice in the public interest while supporting the needs of nurses amidst this complex moral and legal landscape.
Footnotes
Author Contributions
Study design: B. P., S. T., C. S., and J. R.; Data collection: B. P., M. G., and M. L. S.; Data analysis: B. P., S. T., and M. L. S.; Study supervision: B. P.; Manuscript writing: B. P., M. G., and M. S. L.; Critical revisions for important intellectual content: S. T., C. S., C. P., C. H., and J. R.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: C. P. is employed by a Canadian Nursing Regulatory Agency. J. R. is employed by the Canadian Nurses’ Association.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project is supported by a Canadian Institutes for Health Research Project Grant PJT-376065. Barbara Pesut is supported, in part, through the Canada Research Chairs program.
