Abstract
Background:
Inflammation plays a pivotal role in the pathogenesis of diabetes and its complications. Arachidonic acid lipoxygenases have been intensively studied in their role in inflammation in metabolic pathways. Thus, we aimed to explore variants of lipoxygenase genes (arachidonate lipoxygenase genes) in a diabetes adult population using a case-control study design.
Methods:
Study population consisted of 1285 elderly participants, 716 of whom had type 2 diabetes mellitus. The control group consisted of non-diabetes individuals with no history of diabetes history and with a glycated haemoglobin <6.5% (<48 mmol/mol)] and fasting plasma glucose levels <126 mg/dL. Blood samples were genotyped on Illumina Infinium PsychArray. Variants of ALOX5, ALOX5AP, ALOX12, ALOX15 were selected. All statistical analyses were undertaken within PLINK and SPSS packages utilising permutation analysis tests.
Results:
Our findings showed an association of rs9669952 (odds ratio = 0.738, p = 0.013) and rs1132340 (odds ratio = 0.652, p = 0.008) in ALOX5AP and rs11239524 in ALOX5 gene with disease (odds ratio = 0.808, p = 0.038). Rs9315029 which is located near arachidonate ALOX5AP also associated with type 2 diabetes mellitus (p = 0.025). No variant of ALOX12 and ALOX15 genes associated with disease.
Conclusion:
These results indicate a potential protective role of ALOX5AP and 5-arachidonate lipoxygenase gene in diabetes pathogenesis, indicating further the importance of the relationship between diabetes and inflammation. Larger population studies are required to replicate our findings.
Introduction
Almost a century after the discovery of insulin, diabetes mellitus remains a worldwide health problem. Currently, there are 415 million adults diagnosed with diabetes, a number estimated to increase to 642 million by 2040, according to the International Diabetes Federation. Although modern medicine has made great progress in diabetes treatment, the pathophysiology of the disease is yet to be fully unveiled. Lipoxygenases (LOXs) represent a class of enzymes that catalyse the dioxygenation of poly-unsaturated fatty acids (PUFAs), such as arachidonic acid. It is converted into leukotrienes by the enzyme 5-lipoxygenase, when activated by arachidonate 5-lipoxygenase-activating protein. Human LOXs have been implicated in the pathogenesis of cardiovascular and inflammatory diseases as well as in diabetes but the detailed mechanistic basis for their pathophysiological roles remains unclear. However, it has been suggested that 12-LOX plays a role in inflammation and metabolic-stress-induced β-cell islet functional abnormalities. 1 Ma et al. 2 showed that a byproduct of 12-lipoxygenase biological action inhibits insulin secretion and promotes cell-death in human islets in vivo. It has also been demonstrated that 15-hydroxyeicosatetraenoic acid (15-HETE), a product of 15-LOX, is expressed in the epithelial membranes of patients with diabetic retinopathy, whereas the 5-LOX pathway likely plays a significant role in progression of diabetic retinal disease. 3 Moreover, variants of ALOX12 (12-arachidonate lipoxygenase gene) gene have previously been associated with albuminuria in patients with type 2 diabetes mellitus (T2DM). 4 Polymorphisms within ALOX12, ALOX5 (5-arachidonate lipoxygenase gene) and ALOX5AP (arachidonate 5-lipoxygenase activating protein gene) also associated with markers of subclinical atherosclerosis in families with T2DM, thus enhancing the hypothesis that atherosclerosis and T2DM are linked through inflammation. 5 Thus, we aim to explore genetic variants of ALOX (arachidonate lipoxygenase gene) in the presence of T2DM.
Methods
The study population consisted of 1285 individuals, of whom 716 were patients with T2DM. Diagnosis of T2DM was based on the 2010 American Diabetes Association Criteria. Community-dwelling individuals, in whom normal glycaemia was documented by fasting plasma glucose (FPG) and glycated haemoglobin (HbA1c), were recruited as a control group (CG). The CG criteria were (a) age > 65 years, (b) HbA1c < 6.5% (48 mmol/mol), (c) FPG < 126 mg/dL, (d) no past history of a T2DM diagnosis as previously described and (e) no prior or current administration of anti-diabetic drugs. Clinical information and anthropometric measurements as well as written informed consent were obtained from all study subjects. Blood chemistry was examined during a fasting state. All study procedures conformed to the declaration of Helsinki and were approved by the Ethics Committee of the Aristotle University of Thessaloniki.
Selection of polymorphisms and genotyping
Genomic DNA was extracted from peripheral blood. Samples were genotyped on Illumina Infinium PsychArray (603132 SNPs, 559921 of those are submitted to dbSNP as rs). After individual and single nucleotide polymorphism (SNP) quality control, polymorphisms of ALOX were selected using a window of 20-kb upstream and downstream of every gene. EIGENSOFT and PLINK software suite were used.
Statistical analysis
Differences in the clinical characteristics of case and CGs were examined using Student’s t-test on SPSS, Inc. for Windows, Version 21.0. The allele-specific odds ratios (ORs) for T2DM were calculated using logistic regression analysis with and without adjustments for age, sex and body mass index (BMI) by implementing PLINK v.19. The results were further evaluated for their significance by correction for multiple testing. We employed two methods to assess the significance of our results. The first, considered the gold standard in association studies, is a permutation test that shuffles the sample phenotypes and reports the empirical p values (pperm) as performed by PLINK. 6 The second calculates the number of effective SNPs that capture most variance through principal component analysis. 7 Values of p < 0.05 determined the level of significance.
Results
The clinical and biochemical characteristics of all participants in the study are presented in Table 1. After individual quality control analysis was conducted, the total population was reduced to 1141 subjects. When Bonferroni correction was implemented in our study, no variant reached the level of significance. Correcting p value by calculating effective SNPs slightly raised the p value cut-off to 0.001 but no significant association could be revealed. Multivariable logistic regression analysis using permutation test analysis showed that the presence of G allele in rs1132340_A/G and allele C for rs9669952_T/C exhibited both a negative association with T2DM [odds ratio (OR) = 0.65 (95% confidence interval (CI), 0.47–0.89), passoc = 0.007, pperm = 0.008 and OR = 0.74 (95% CI, 0.58-0.94), passoc = 0.012, pperm = 0.013, respectively]. Moreover, allele G in rs11239524_T/G of ALOX5 gene was associated with T2DM when permutation analysis was applied [OR = 0.08 (95% CI, 0.64-1.00), passoc = 0.057, pperm = 0.038.]. Interestingly, rs9315029_T/G located 14809b upstream ALOX5AP gene was also associated with T2DM [OR = 0.81 (95% CI, 0.66–0.97), passoc = 0.023, pperm = 0.025]. No polymorphisms of ALOX12 and ALOX15 (15-arachidonate lipoxygenase gene) genes were associated with disease. No variant adjusted for age, sex and BMI showed significance. The datasets generated during and/or analysed during this study are available in the Github repository (https://github.com/ftsetsos/aloxdiabetes).
Study population clinical and biochemical characteristics.
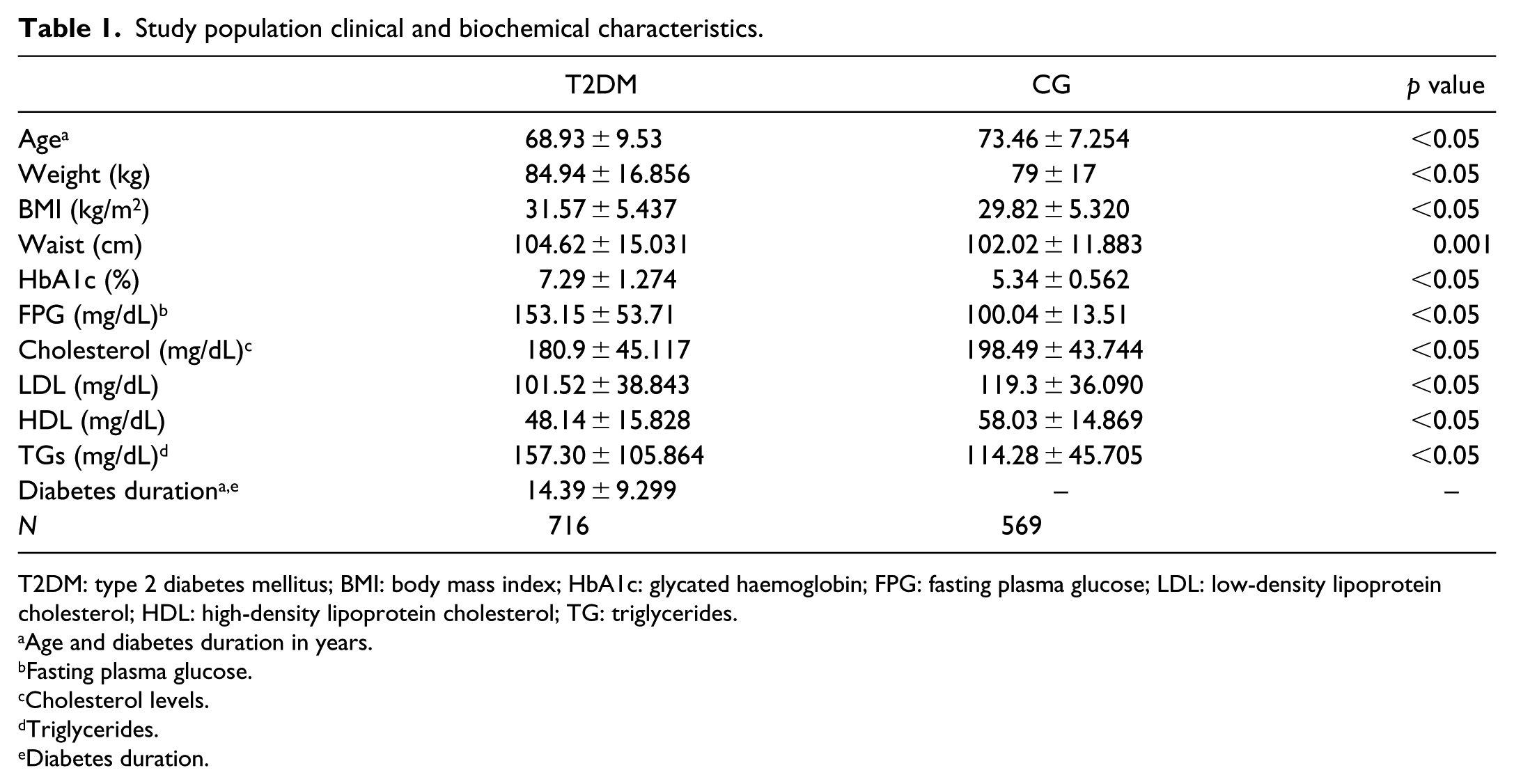
T2DM: type 2 diabetes mellitus; BMI: body mass index; HbA1c: glycated haemoglobin; FPG: fasting plasma glucose; LDL: low-density lipoprotein cholesterol; HDL: high-density lipoprotein cholesterol; TG: triglycerides.
Age and diabetes duration in years.
Fasting plasma glucose.
Cholesterol levels.
Triglycerides.
Diabetes duration.
Discussion
In this study, we assessed whether SNPs in ALOX genes are associated with T2DM. By implementing permutation analysis, we were able to compute the permuted p values that unravelled the association between ALOX and T2DM. Carriers of allele G for rs1132340 are 34.8% less likely to be associated with T2DM, whereas carriers of C allele in another variant of ALOX5AP, rs9669952 exhibited a protective role as well. To our knowledge, these two variants of ALOX5AP gene have not previously been associated with T2DM. Rs1132340 is located in the 3-UTR (3-prime untranslated region), whereas rs9669952 is located in an intron region, both in chromosome 13. No underlying mechanisms of action have been described in the literature regarding these two polymorphisms and T2DM. Our results also report another novel, protective variant, located upstream of ALOX5AP. Carriers of allele G of rs9315029 are 19.5% less likely to develop T2DM. ALOX5AP has been previously associated with subclinical measures of atherosclerosis, whereas its haplotypes have been associated with myocardial infarction and stroke in diabetic population, enhancing further the well-established linkage between T2DM and cardiovascular disease.5,8 Moreover, ALOX5AP has been associated with obesity and insulin resistance, as it was shown that the higher Homeostasis Model Assessment – Insulin Resistance (HOMA-IR) levels, the more increased ALOX5AP messenger RNA (mRNA) levels were in adipose tissue, suggesting a possible implication of ALOX5AP products in glucose metabolism. 9 A recent study by Elias et al. 10 demonstrated that transgenic mice overexpressing ALOX5AP in adipose tissue had higher lipoxin A4 levels, were leaner, and showed increased energy expenditure, in part due to browning of white adipose tissue, suggesting a potent mechanism of action to be therapeutically targeted. In addition, our results showed that carriers of mutant G allele of rs11239524_T/G of ALOX5 are 19.2% less likely to present with T2DM. This protective role of rs11239524 is also novel. Burdon et al. 5 failed to associate rs11239524 and other variants of ALOX5 gene with markers of subclinical atherosclerosis. In a recent study by Heemskerk et al. 11 , ALOX5 and ALOX5AP were expressed significantly higher in subcutaneous white adipose tissue of diabetic women compared to control.
Although our results show no association between variants of ALOX12 and ALOX15 and T2DM, these genes do seem to be implicated in diabetes pathogenesis as ALOX12 is expressed in human islets in vitro and may play a role in autoimmune diabetes development by compromising β-cell viability. This is also supported by Grzesik et al, who showed up-regulation of 12-LOX under inflammatory conditions in the diabetic pancreas. 12
Strengths and limitations
Our study is subjected to limitations, such as the small sample. In our study, the age of the CG was restricted to elderly people, in an attempt to exclude diabetic cases that have yet to emerge. This limitation, though, may have enabled the unravelling of protective variants. The implementation of HbA1c value of 6.5% (48 mmol/mol) as a cut-off for non-diabetes, instead of a lower value, may enable the appearance of prediabetes cases in our CG. The absence of an oral glucose tolerance test for T2DM diagnosis is noted. We report the absence of a replication sample and failure to adjust for co-factors in permutation analysis.
In conclusion, in this case-control study, we distinguish variants of ALOX5 and ALOX5AP that are suggestive of protection against T2DM. No associations were detected for ALOX12 and ALOX15 genes. However, further studies with greater sample size and perhaps tighter stratification are needed to replicate our findings and contribute to unravelling the pathogenesis of T2DM.
Footnotes
Acknowledgements
M.A.G. is a recipient of an ΙΚΥ fellowship of excellence for post-graduate studies in Greece-Siemens programme.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This research was supported by the European Social Fund and Greek funds through the Operational Programme ‘Education and Lifelong Learning’ of the National Strategic Reference Framework–Research Funding Programme: THALES. Investing in knowledge society through the European Social Fund (MIS 380273). It was also supported by Hellenic Association for the Study and Education of Diabetes Mellitus.
