Abstract
The Scottish Photobiology Service (SPS), hosted in the Photobiology Unit at Ninewells Hospital, Dundee, celebrated its 50th anniversary in 2023. Dedicated to providing diagnostic and therapeutic services for individuals with cutaneous photosensitivity disorders, the SPS has consistently sought to improve patient care. In 2015, the Chief Medical Officer for Scotland, published a national report entitled ‘Realistic Medicine’, which challenged medical practitioners to improve patient care through the development of personalised approaches, with patients placed at the centre of their care. In 2019, the SPS initiated a patient engagement programme aimed at better understanding the needs of patients with photosensitivity conditions, underpinning the objectives of the Realistic Medicine concept. This article outlines the development, implementation and outcomes of this initiative, which has become a core function of the service. Through ongoing collaboration with patients and staff, the programme has informed service improvements, addressed key issues such as referral delays, peer support and educational resources, and fostered an inclusive approach to care.
Introduction
The Scottish Photobiology Service (SPS) provides a tertiary referral service for patients with photosensitivity disorders and has been dedicated to enhancing the care and support of its patients for over 50 years. It is funded by National Services Scotland and offers specialised diagnostic services and clinical management to ~250 patients/year with a wide range of suspected and confirmed photosensitivity conditions. Photodermatoses are a broad group of skin conditions, which are caused or worsened by exposure to light, typically sunlight. The prevalence of these conditions varies considerably. For example, polymorphic light eruption is relatively common, with a reported prevalence of 21.4% in the Irish population, 1 whereas solar urticaria is considerably rarer, with a point prevalence of 3.1/100,000 individuals in the Tayside region of Scotland. 2 These conditions pose a unique set of challenges for affected individuals. Behavioural modification is often necessary to avoid triggering or exacerbating the condition, such as altering activities to minimise time outdoors, seeking shade and wearing protective clothing, hats and sunscreen. A recent systematic review by Rutter et al. highlighted the substantial impacts of these conditions on quality of life (QOL) and psychological welfare of affected patients, with between 31% and 39% of photosensitive patients reporting a very large adverse impact on QOL (Dermatology Life Quality Index >10). 3
In 2015, the Chief Medical Officer for Scotland, Catherine Calderwood published a national report entitled ‘Realistic Medicine’, which challenged medical practitioners to improve patient care through the development of a more personalised approach, one in which patients are placed at the centre of their care. 4 With the concept of Realistic Medicine in mind and given the unique impact of these conditions, in 2019, the SPS embarked on an initiative to enhance its understanding of what truly matters to patients. 5 While the service had collected feedback through patient questionnaires on several aspects of service delivery over many years, the evolving needs of patients prompted the development of a more structured and patient-centred engagement approach. This programme aimed to bridge the gap between service provision and patient expectations, ensuring that care is responsive, personalised and informed by the lived experiences of those affected by photosensitivity.
Methods/results
The Double Diamond design concept is a design-thinking framework that structures innovation into four phases: Discover, Define, Develop and Deliver. It emphasises divergent thinking to explore problems and solutions, followed by convergent thinking to refine and implement them. 6 This concept was employed to inform the SPS patient engagement programme, which was launched in 2019 with the goal of fostering direct communication between patients and healthcare professionals. A collaborative approach was adopted, involving both patients and staff, in workshops designed to identify patient needs and areas for service improvement.
In-person event (April 2019)
The first step in this initiative was an in-person event held at the, then newly opened, V&A Museum in Dundee to provide a neutral, non-hospital environment. All patients of the SPS service and all staff members involved in the SPS were invited to attend. A total of twenty-eight patients and ten staff members attended this event. Patients were invited to share their journeys with photosensitivity, while staff listened empathetically and facilitated discussion. For many individuals, this event marked their first opportunity to connect with others who shared a similar experience of photosensitivity, fostering a sense of understanding and validation through a common, lived condition. Key themes that emerged from the event included:
Lengthy delays in referral from primary care (up to 12 years).
The lack of peer support post-diagnosis.
The need for additional disease-specific information for patients, families, friends and employers.
These insights highlighted several critical gaps in the service and set the stage for targeted improvements.
Follow-up workshop (October 2019)
In response to the issues identified during the first event, the SPS invited a subgroup of four patients to participate in a follow-up workshop. In this session, patients and staff discussed emerging themes in greater detail and collaborated to define actionable goals. SMART (Specific, Measurable, Achievable, Relevant, Time-bound) objectives were established, leading to the creation of work packages that focused on:
Raising awareness of photosensitivity among the general public, patients, families, friends and employers.
Increasing educational outreach through a dedicated ‘Light Sensitivity Awareness Day’.
Improving recognition of photosensitivity in primary care, including the identification of ‘red flag’ features.
Expanding the provision of disease-specific information for patients and their support networks.
Facilitating continuity of care by establishing patient support groups.
The patient engagement programme was further refined and expanded over time. Key outcomes from the initial workshops informed subsequent service improvements, which are now embedded in the day-to-day operations of the SPS.
Virtual patient engagement (post-2020)
Following the onset of the COVID-19 pandemic, the patient engagement programme successfully transitioned to a virtual format. As well as a biennial in person events, the SPS organises twice-yearly virtual half-day events via Zoom online platform, providing patients with a convenient and accessible platform to discuss issues that matter most to them. The outline of these sessions is generally an overall introduction and then a discussion of a particular theme, such as sun protection or coping strategies or an area of our recent research development, then followed with smaller break-out discussion groups held within the main virtual meeting format and finishing up with an overall discussion of emerging themes, concepts and potential actions and solutions. These online sessions are well-received, with positive feedback regarding their content, utility and the convenience of remote participation. During these events, patients have voiced concerns about the isolation, anxiety and embarrassment associated with their condition, as well as the challenges of explaining their condition to family and friends who may not fully understand its impact.
Newsletters and continued support
To ensure ongoing communication, the SPS began distributing newsletters twice a year, starting in 2020 during the COVID pandemic. These newsletters keep patients informed about service developments, research advancements and upcoming events. The newsletters are well-received, reinforcing the message that SPS is committed to supporting patients.
Addressing referral delays
One of the major concerns identified by patients was the significant delay in referrals from primary care to specialised photobiology services. Feedback indicated that many patients felt their symptoms were not taken seriously, potentially due to a lack of awareness of photosensitivity among general practitioners. In response, the SPS in collaboration with designers from the DesignCrowd website, developed a ‘Photosensitivity Red Flag’ poster for distribution throughout primary care settings in Scotland. This poster aims to increase awareness of the key symptoms of photosensitivity and facilitate earlier referrals for patients. It has been distributed to all primary care practices in Scotland in newsletter format through the Scottish Practice Management Development Network with a plan to add this poster to the national pathway guidance soon (Figure 1).

Red flag poster for General Practitioners.
Educational resources and awareness
The SPS has also taken steps to raise awareness of photosensitivity through the development of ‘The Light Sensitivity Podcast’ educational podcasts. Available on all major platforms, these podcasts have been downloaded over 200 times both in the United Kingdom and wider afield in Europe, the United States, Canada, Japan and Australia. The podcasts feature informal discussions between patients and consultants in the presence of a moderator, with the aim of highlighting the everyday impact of photodermatoses on individuals’ lives. All the major photosensitivity disorders are featured in these seven podcasts, and there is scope for us to develop other areas of photodermatology interest for patients through this format. By sharing these real-life stories, SPS hopes to promote greater understanding of photosensitivity amongst healthcare professionals, patients and the public (Figure 2). The SPS also ensures patients have access to reliable and accessible information by publishing on the NHS Inform website, having in conjunction with the NHS24 Digital Programme team and patients, developed two new NHS Inform webpages relating to the photosensitivity diseases and their management.7,8 We have also expanded and developed activities locally in Ninewells hospital aimed at creating awareness of photosensitivity during Sun Awareness week each year.
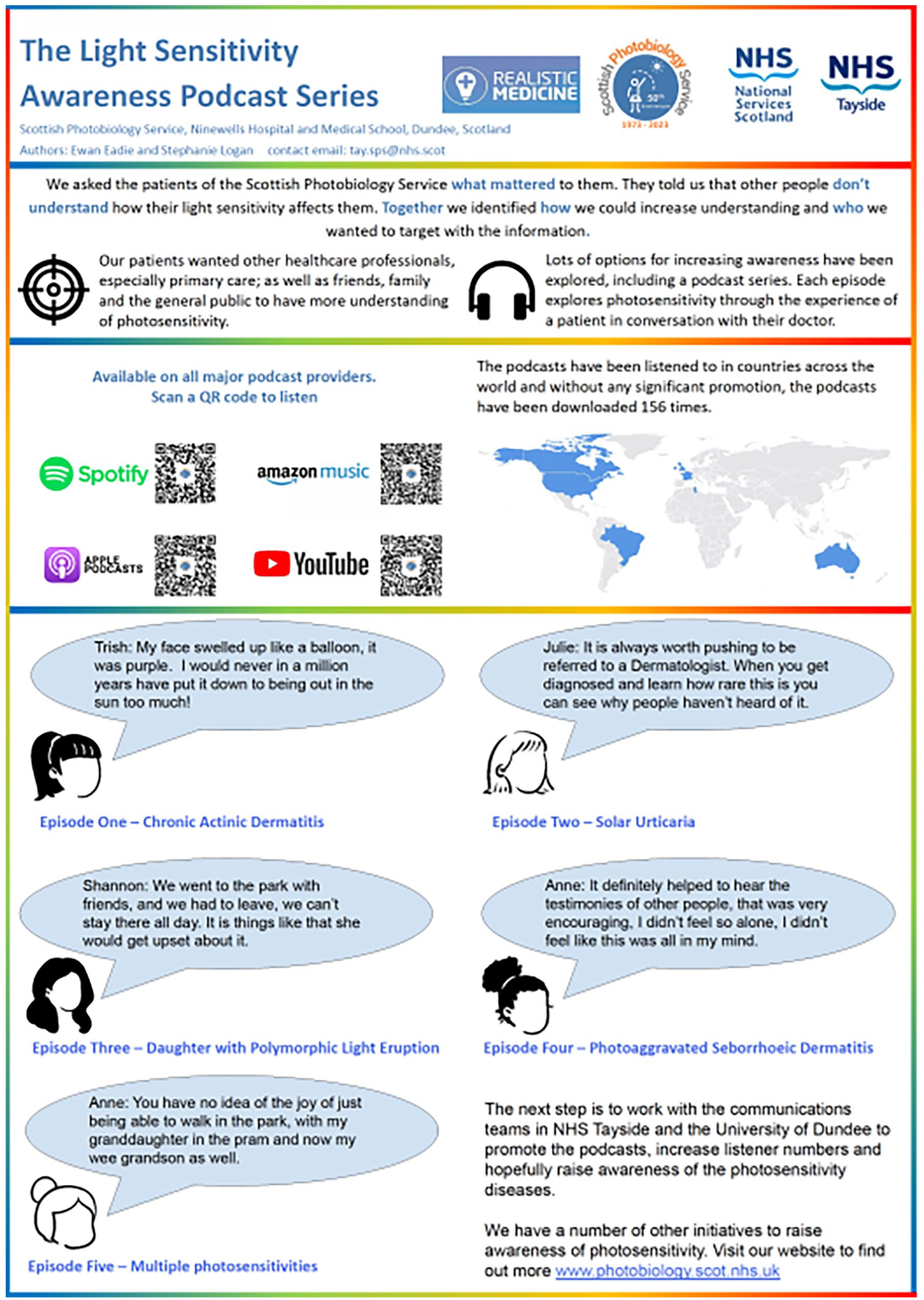
The Light Sensitivity Awareness Programme.
Information for employers/teachers
In response to patient involvement, we created information cards for teachers (Figure 3) and employers (Figure 4) outlining reasonable adjustments they could make for individuals with photosensitivity conditions to make their learning or working environments better suited to their individual needs dependent on their photosensitivity requirements. In addition, we are also developing a similar information card for families and friends given that it has been brought to our attention that even those closest to the photosensitive patient, may still not fully understand or appreciate the demands imposed by their photosensitivity condition.
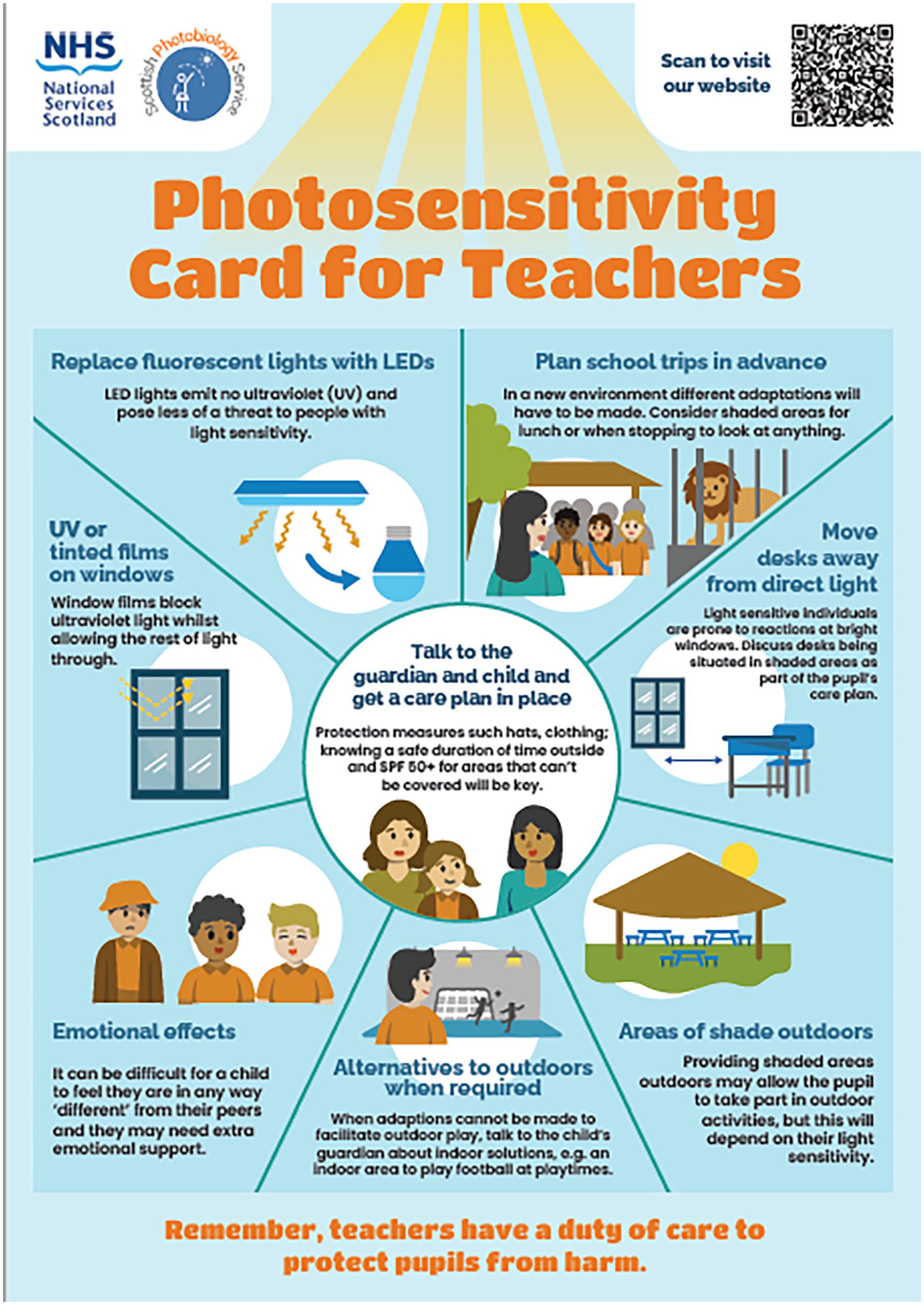
Card for teachers.
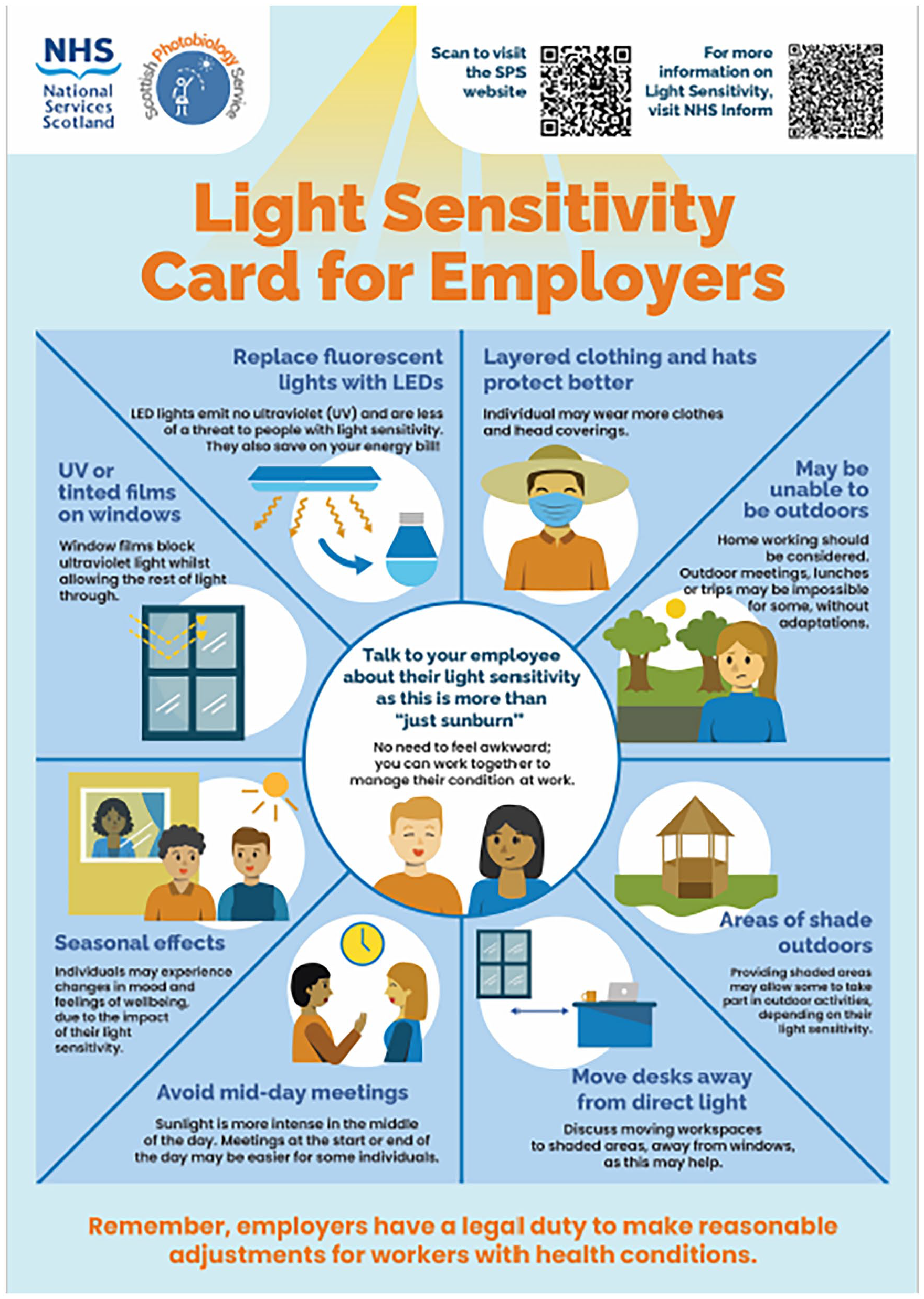
Card for employers.
Peer support group
The patient engagement programme facilitated the establishment of the peer support group, Photosensitive and Living with Sunshine (PALS), founded by two individuals diagnosed with photosensitivity conditions. These patients met through the engagement programme and collaborated to create an informal support network for others facing similar challenges. PALS provides monthly virtual meetings for individuals diagnosed with photosensitivity, offering a platform for peer support. Information about the group is made available to all patients diagnosed with photosensitivity attending the photobiology unit, ensuring that newly diagnosed patients have access to this valuable resource. Support groups, such as PALS, fulfil multiple essential functions. They provide education for patients and their families, allow for the sharing of personal illness experiences, offer emotional support, raise public awareness about the condition and often engage in fundraising initiatives. Given these diverse roles, PALS has become an important resource for patients with photosensitivity conditions, enhancing both their knowledge of photosensitivity and their sense of community. Furthermore, this group and the wider engagement group now provide essential patient input for the SPS team in terms of offering advice and opinions on service delivery development and research activities and priorities.
Results
By actively listening to the voices of patients, SPS has successfully identified critical gaps in care and developed targeted interventions that address the real-world challenges faced by individuals with photosensitivity. This patient-centered approach has not only enhanced satisfaction but has also informed the ongoing evolution of the service.
Feedback on the SPS service has consistently been excellent, with 94% of patients reporting they were extremely satisfied with their experience at the photobiology unit over the past three years. The positive impact of this patient engagement programme is further reflected in comments gathered from patients following patient engagement events:
Living experience sharing is wonderful.
I really like the updates from the department and chatting to other people with sensitivity to light.
My favourite bit is hearing experiences or solutions to photosensitivity issues from others.
It is really interesting to hear about all the research that is going on and how patient-focussed it is.
It helps you realise that it is not just you affected.
These remarks highlight the value patients place on shared experiences, peer support and transparent communication. The programme’s success was formally recognised with the Chair and Chief Executive STAR Award at the 2025 NHS Tayside Awards Ceremony. This recognition underscores the vital importance of collaboration between patients and healthcare providers in driving meaningful improvements in clinical services.
Limitations
The main unavoidable limitation of this patient engagement programme is that only the service users who are most interested and able participate. However, all service users of the SPS were invited to attend and we offered to reimburse travel expenses. It is now part of our routine practice to provide the details of this programme to all patients attending the photobiology unit for assessment. Furthermore, we have transitioned the majority of the meetings to a virtual format to increase accessibility.
Conclusion
The SPS patient engagement programme represents a model of patient-centred care that actively involves patients in the co-design of services. By fostering a deeper understanding of patient needs, the SPS has created a more responsive and supportive service that is better equipped to meet the unique challenges of patients with photosensitivity disorders. Objectively assessing the impact of these activities on patients’ QOL represents a key area for future research and development within the department. Current initiatives aim to explore this impact in greater depth to capture the multidimensional effects of these conditions and guide more personalised patient care strategies. Building on this patient engagement programme and a recent review on the photodiagnostic services in the United Kingdom and Republic of Ireland, 9 another key research priority is to assess the availability, quality and access to photodiagnostic services for patients with photosensitivity diseases worldwide in the Global Assessment of Photodiagnostic Services (GAPS) study. The GAPS study will provide critical insights into the current state of photodiagnostic services for photosensitivity disorders, enabling the development of targeted interventions to improve access, quality and outcomes for patients worldwide.
The SPS’s patient engagement programme provides a powerful example of how patient involvement can be used to shape the future of healthcare delivery. Through empathy, collaboration and a commitment to ongoing improvement, the SPS has been able to address key issues affecting patients with photosensitivity and enhance the overall quality of care. The SPS patient engagement programme exemplifies the concept of Realistic Medicine by building more informed patient-staff partnerships to improve the lives of patients. This model of patient engagement is flexible and adaptable, making it a valuable tool for other healthcare services seeking to improve patient-centred care in a variety of clinical contexts.
Footnotes
Acknowledgements
We would like to express our sincere thanks to all the SPS patients, their families and our dedicated staff for their invaluable contributions to the patient engagement programme. Without their input, this initiative would not have been possible.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
