Abstract
Background
Young sudden cardiac death (YSCD), often occurring in previously healthy individuals, is a tragic event with devastating impact on affected families, who are at heightened risk of posttraumatic stress and prolonged grief and may themselves be at risk of YSCD. Previous research suggests that surviving family members’ psychosocial support needs are often unmet.
Purpose
This study sought to identify how YSCD-affected families experience dedicated community and peer support in light of their psychosocial support needs.
Methods
The study used a qualitative design, employing a thematic analysis of focus group and interview data. Three focus groups and five individual interviews were conducted with affected family members (
Results
Three super-ordinate themes were identified: 1. YSCD community support as offering a place of safety, 2. YSCD community support as fostering sense-making, 3. YSCD community support as facilitating finding new meaning.
Conclusions
YSCD-affected families can benefit from access to dedicated community and peer support that offers a safe environment, provides affiliation, understanding and normalisation and enables sense-making and the rebuilding of a sense of self. Dedicated community support can facilitate meaningful re-engagement with life through helping prevent YSCD and through memorialisation and legacy-building to maintain a continuing bond with the deceased. Clinicians need to be aware of the need to incorporate available community and peer support into patient pathways.
Keywords
Introduction
Young sudden cardiac death (YSCD) is a devastating event for affected families, often occurring in healthy and active young people without prior symptoms. 1 The cause of the death is frequently uncertain or associated with genetic heart diseases, suggesting possible future risks for other relatives and thus imposing additional stresses on the surviving family. 2 YSCD-bereaved family members are at increased risk of anxiety and depression; 3 half experience post-traumatic stress and prolonged grief symptoms, with particularly high rates reported for mothers and those who witnessed the death. 4 Prolonged grief is furthermore associated with other health complications such as cancer and heart disease and carries an elevated risk for death by suicide.5,6 Bereavement through sudden death has been linked with greater feelings of isolation, 7 and parents’ heightened support needs following the sudden loss of a child from any cause have been noted. 8 Although the significant psychosocial burden and unique challenges for YSCD-bereaved families have been observed, 2 support provision for YSCD-affected families has been found wanting. 9 A cross-sectional survey investigating the support needs of Australian YSCD-bereaved families found that psychosocial needs – particularly the need to understand the cause of death – were most likely to be left unmet in comparison with medical, spiritual and financial needs. 10 While the authors identified broad categories of need, more detailed understanding of those needs and of what would be most helpful to families is required. Families may, for example, seek support from dedicated community organisations that offer medical and social (peer) support outside or alongside statutory service provisions. It would be of interest to ascertain how families engaging with such organisations experience this support and how it might meet or not meet their needs. The current study therefore aimed to identify YSCD-bereaved families’ specific psychosocial needs and the impacts of targeted community and peer support provision.
Methods
Design and sampling
The methodological approach was qualitative and exploratory. Participants were drawn from YSCD-affected families that had lost a member under the age of 35 and had accessed community (e.g. fundraising events, newsletters and social media groups) and peer support from a dedicated charity, Cardiac Risk in the Young (CRY), one of the largest European charities for families affected by YSCD. 11 It offers clinical support through expert pathology, cardiology and screening services to identify young people at risk. It funds research, engages in awareness-raising and has a dedicated peer-to-peer bereavement support programme. It also offers general community support through fundraising and other events, publications and social media networking. Other charities such as Compassionate Friends 12 and the Sudden Arrhythmia Death Syndromes (SADS) Foundation 13 also offer some relevant support. However, Compassionate Friends offers broader support to families bereaved due to any cause, and SADS is not aimed at young SCD specifically. Families accessing CRY as dedicated specialist support for YSCD bereavement thus constituted the target population. Recruitment aimed to secure a broad sample with members from each of the different stakeholder groups: 1. peer supporters who had provided telephone support for at least a year, 2. peer support users who had received telephone support, 3. bereaved families who had accessed the organisation’s general community support but had not opted into the peer support. Those bereaved for less than 18 months were excluded.
Patient and public involvement
Prior to designing the study, the first author attended events run by the charity and conducted interviews with supporters and support users to gain an initial understanding of the field and the ethical requirements of the study. Information gathered from stakeholders informed decisions on the study design, interview and focus group schedule development, and geographical locations and settings for data collection. A report of the findings was made available to the charity.
Data collection
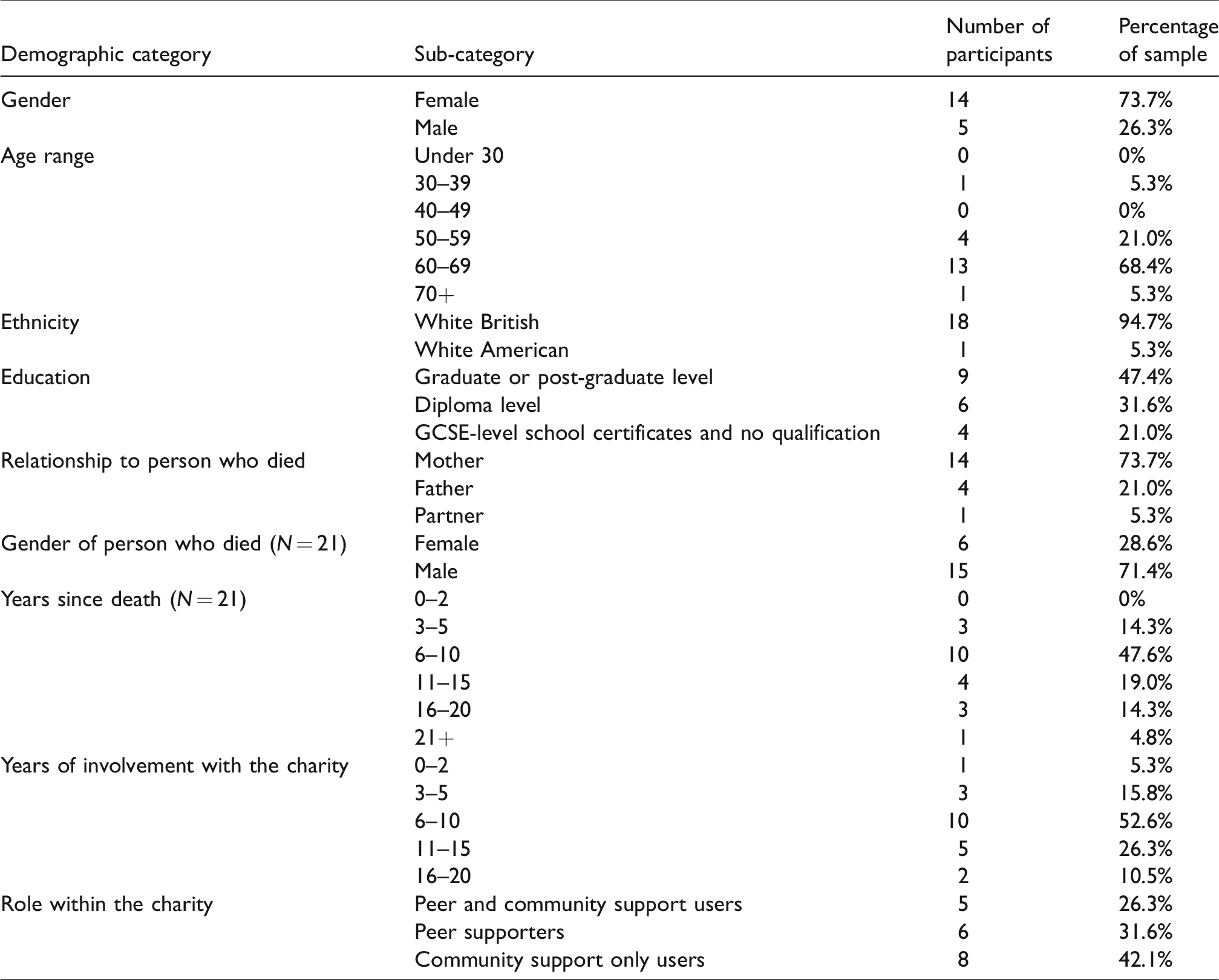
The investigation was approved by the University of Surrey’s Research Ethics Committee (EC/2013/132/FAHS) and conforms with the principles outlined in the Declaration of Helsinki14 (see Supplementary Material Appendix A online for data collection procedure). Nineteen people made up the final sample (see Table 1). The majority of participants were female (73.7%), White British (94.7%) and had diploma, graduate or postgraduate level qualifications (79%). Participants’ age ranged from 30 to 71, with a mean age of 61.23 (SD = 8.29) years; 18 (94.7%) stated their ethnicity as White British. In terms of their relationship with the deceased, there were 14 (73.7%) mothers, four (21%) fathers and one (5.3%) partner. In 15 cases (71.4%), the person who died was male and in six cases (28.6%) female (some had lost more than one person to YSCD). In three cases (14.3%) the loss had occurred 3–5 years previously. In 10 cases (47.6%) the loss had occurred 6–10 years previously, in eight cases (38.1%) 11 or more years had elapsed since the death.
Sample characteristics.
Data collection consisted of three focus groups (one for each stakeholder group) and five individual interviews. The focus group participants were trained and experienced peer supporters (Focus Group 1;
Data analysis
Interviews and focus groups were audio-recorded, transcribed and analysed using an inductive and semantic version of thematic analysis so as to stay as close to the participants’ meanings as possible15,16 (See Supplementary Material Appendix C online for data analysis procedure). Data analysis was conducted by three researchers working closely together to ensure that themes were grounded in the data and that criteria for high-quality qualitative research were met. 17 None of the researchers had experienced YSCD personally, although all of them had experienced bereavement previously. This facilitated an empathic stance but also some distance from the specific phenomenon. Standards for Reporting Qualitative Research 18 were used in the preparation of this report.
Results
The thematic analysis of the data produced three themes, each consisting of two sub-themes (see Table 2). In what follows, key findings are described, illustrated by data excerpts. The following abbreviations have been used to indicate which focus group or individual interview the data stem from:
Themes and sub-themes.

YSCD: young sudden cardiac death; FG: Focus Group; II: individual interview
FG1 = Focus Group 1 (peer supporters);
FG2 = Focus Group 2 (peer and community support users);
FG3 = Focus Group 3 (community support users);
II1 = Individual Interview 1 (community support user);
II2 = Individual Interview 2 (community support user);
II3 = Individual Interview 3 (community support user);
II4 = Individual Interview 4 (peer and community support user);
II5 = Individual Interview 5 (peer supporter).
Theme 1: YSCD community support as offering a place of safety
This theme describes YSCD-bereaved family members’ need for support that provides a sense of safety and comfort, particularly in the early days following the death. Participants often described feeling desperate or afraid of going mad, and they referred to community support as helpful if it conferred safety.
Sub-theme 1.1: A safe haven in the aftermath of YSCD
This sub-theme is mostly connected with the perception of YSCD community support as rescuing the bereaved at the time of greatest distress in their life: It was like an anchor in the storm. I was going to capsize, I was going to drown, and it was that profound, that I knew she was there. (FG2) It was certainly quite a saviour, I think, to be able to speak to somebody who had had the same thing happened and yeah…could empathise. (II4) And the fact that there’s an organisation there that you could turn to, should you so wish to, for support, is a great comfort. (FG3) …where no one asks the wrong questions, where no one says ‘How many children [do you have]?’ The first question people ask is ‘Who did you lose? Tell me about your story.’ (FG2) Just being with people who you know you don’t have to explain anything to. (II1)
Participants emphasised the devastating change to their sense of self following this traumatic loss and the importance of this being understood: It’s like being stripped and being put into a place where you’re totally…you don’t speak the language any more. And that person on the phone knows who you are and you can speak to them. (FG2)
Sub-theme 1.2: Shared experience of YSCD
The sub-theme of ‘safe haven’ or ‘home’ closely aligns with a sense of belonging based on shared experience. Having experienced the uniqueness of YSCD bereavement, participants across the data set expressed the importance of a sense of affiliation and community: It’s the sort of realisation that you’re not…you know, you’re not alone in it, that, you know, there are other people out there. (FG3) It’s such…an isolating trauma that you go through, because, you know it’s the connection with somebody that’s had exactly that happen to them. (FG1) ‘It’s actually very important to have somebody who’s been through a semi-identical experience because then they understand you and you understand them’. (II1) Once they know that – it’s almost like then, it’s like… ‘Oh, it is the same’, and then they feel safe. (FG1) In a word, the first word that comes to mind is ‘family’ because it’s the one place…it’s the one group of people you can go with and can feel safe. (II2)
Theme 2: YSCD community support as fostering sense-making
The second theme centres on the psychosocial need for making sense of unexpected YSCD and developing understanding of the unique impacts of YSCD loss on the surviving family. The complex sense-making processes that such a loss entails require YSCD-sensitive support provisions.
Sub-theme 2.1: Making sense of YSCD
The difficulty of making sense of a death as unexpected as YSCD and how services and agencies can be helpful in finding an explanation were apparent across the data set. In one focus group, when being asked what YSCD-affected families wanted from services, a participant said: Answers really I think – a few answers we wanted, didn’t we really? (FG3) I think clear medical explanations are very important. I don’t know whether the bereavement counsellors can give those clear medical explanations because, actually, they need to come from…probably from cardiologists, who may not have the time or the…possibly always the empathy to do it. (II1) For me, as in personally, I…I have…if I can see a reason for something, it’s easier, but I could see no reason whatsoever for [daughter’s name] dying. (II2)
Sub-theme 2.2: Understanding YSCD-related grief
Sense-making in the aftermath of YSCD loss also includes developing an understanding of how such a sudden and untimely death impacts those affected by it. Learning about and understanding the nature of one’s grief may be part of the journey through it. Having access to a YSCD-dedicated organisation meant that the affected families’ grief can be met with expert understanding: People couldn’t understand except [organisation] could. [Organisation] understood the depth of the grief and the sorrow that people who’d lost a child so suddenly, and it’s just dismissed as Sudden Adult Death Syndrome – doesn’t tell you why, what sort of medical condition there was, and so you’re just left. But [organisation] understood. (FG3) And they tell you they had the same, you can then say, ‘Oh okay, it’s because of the experience, it’s not that I’m having these thoughts or whatever, it’s not me, that I’m having a psychotic breakdown.’ (FG2) Seeing the supporters who have been through it, they take up life again, you know. You don’t want to get over the loss of a child – that’s the last thing you want to do. But obviously, you do want to be able to function in life again. (II5) It’s not that you’re telling them what to do but they need to know something about you so that they can…clutch at something and… ‘OK, so I can…can I get through this?’ ‘Yes, you can, but you’ll do it your way.’ (FG1)
Theme 3: YSCD community support as facilitating finding new meaning
The third theme captures how participants saw YSCD-related community support as opening up ways of engagement that could be meaningful in connection with their loved ones’ death and providing them with an ongoing connection with the deceased.
Sub-theme 3.1: Finding a new ‘cause’ through helping to prevent YSCD
Some participants described how engaging in YSCD-related fundraising activities provided them with a different kind of support: I think it’s the fact that you feel so helpless and you’ve got to do something, and fundraising was the big thing with us. (FG3) He [husband] finds the fundraising is his therapy. (FG3) I’ve had this hideous disaster but actually I’ve got to make something of it. I mean, just something has got to change now and it’s that real drive to make some change happen. (II1)
Sub-theme 3.2: Finding meaning after YSCD through honouring the deceased
Participants talked about their engagement in fundraising not only as providing them with a new purpose but also as meaningful in connection with their deceased loved one. One participant described a fundraising walk as ‘a sort of memorial to the person that you’ve lost’ (II5). The importance of the personal connection to the loved one was also emphasised in the following data extract: I couldn’t see the point in the fundraising at first because I just thought ‘I’m not bothered. It won’t bring back [son’s name] so why should I bother?’ But then I just thought ‘[Son’s name] would have hated me to say that because he was such a caring person.’ So you go to that other level where you think, ‘No, this is for him, because he would have wanted us to do that.’ (FG3) You want to keep in touch with [organisation] because that is part of your life which is going to go on, in a way, because you can’t just put it behind you. (FG2)
Discussion
The present study constitutes the first interview-based study of the psychosocial support needs of YSCD-affected families and the role that dedicated community and peer support can play in meeting those needs.
First, our results are broadly in line with general observations about the devastating impact of the sudden loss of a child and resulting support needs. 8 As regards the specific challenges of YSCD, our results concur with the recent needs analysis by McDonald et al., 10 which identified needs for instrumental support in the form of a safe place to turn to and emotional support through affiliation and informational input. This is reflected in Theme 1 (YSCD community support as offering a place of safety). Our study extends previous findings by drawing on the actual voices of affected families. Participants spoke about ‘drowning’ or ‘capsizing’, conveying the enormity of their ordeal, thus highlighting the significance of highly empathic and sensitive support (‘an anchor in the storm’; ‘safe haven’), particularly in the acute phases following YSCD. Psychological reactions have been found to be more intense in early grief 19 and interventions for those with very severe early distress are called for, particularly as this is a vulnerable group with a potentially complicated or prolonged grief trajectory if left unsupported. 20 Participants’ use of analogies such as ‘drowning’ and then finding a ‘safe haven’ could be seen as pointing to their need for a ‘holding environment’ in early grief, something that seems especially important after a sudden or violent death. 21
Second, our study draws attention to the significance of meaning-making as an overarching psychosocial need in the aftermath of YSCD. This is reflected in Theme 2 (YSCD community support as fostering sense-making). McDonald et al.
10
observed that the need for medical information and for understanding the cause of the death constituted the most significant need in families and was mostly unmet. Our study showed that making sense of the death was not only about medical explanations but about meaning-making at a broader level, reflecting definitions of sense-making and meaning-making in the literature on trauma and bereavement.
22
An expansive understanding of what sense-making entails links with research on the significance of meaning as a mediator for complicated or prolonged grief.
23
This may partially answer concerns expressed by Christiaans,
24
who drew attention to the lack of
Third, our study highlights the need for peer support following YSCD. This is reflected across Themes 1 and 2. The value of peer support has been reported for bereavement in general. 25 A recent investigation into the utility of bereaved people’s social networks found peer support to be particularly helpful. 26 This was linked with a number of benefits for the bereaved including the provision of emotional and informational support as well as instilling a sense of communality and belonging. 27 The latter quality is particularly critical in unique or rare bereavement circumstances 28 such as YSCD bereavement. Our study adds to these findings by giving nuanced insight into the actual experience of receiving support from trained supporters and how this may function as a psychosocial conduit for processing grief and ‘relearning the world’. 29
Fourth, our analysis highlights that effective community support for YSCD-affected families is more than ‘support
Specific recommendations for practice are given in Table 3. These include providing families with a safe and understanding environment in the immediate aftermath of the death. Medical explanations should be provided sensitively, including, if possible, relevant resources developed by patient representative organisations. It should be noted that clinical pathways often focus on the immediate needs of the patient within the context of determining risk due to a diagnosis of a condition. In the case of YSCD, an additional step should be integrated into the patient pathway whereby, at the conclusion of the clinical appointment, families are made aware of patient representative groups that can offer additional and ongoing support. This should involve informational and emotional support and would ideally include access to families with prior experience of YSCD. It should be ensured that patients are aware of any such available resources when they leave the clinical appointment.
Recommendations for practice.
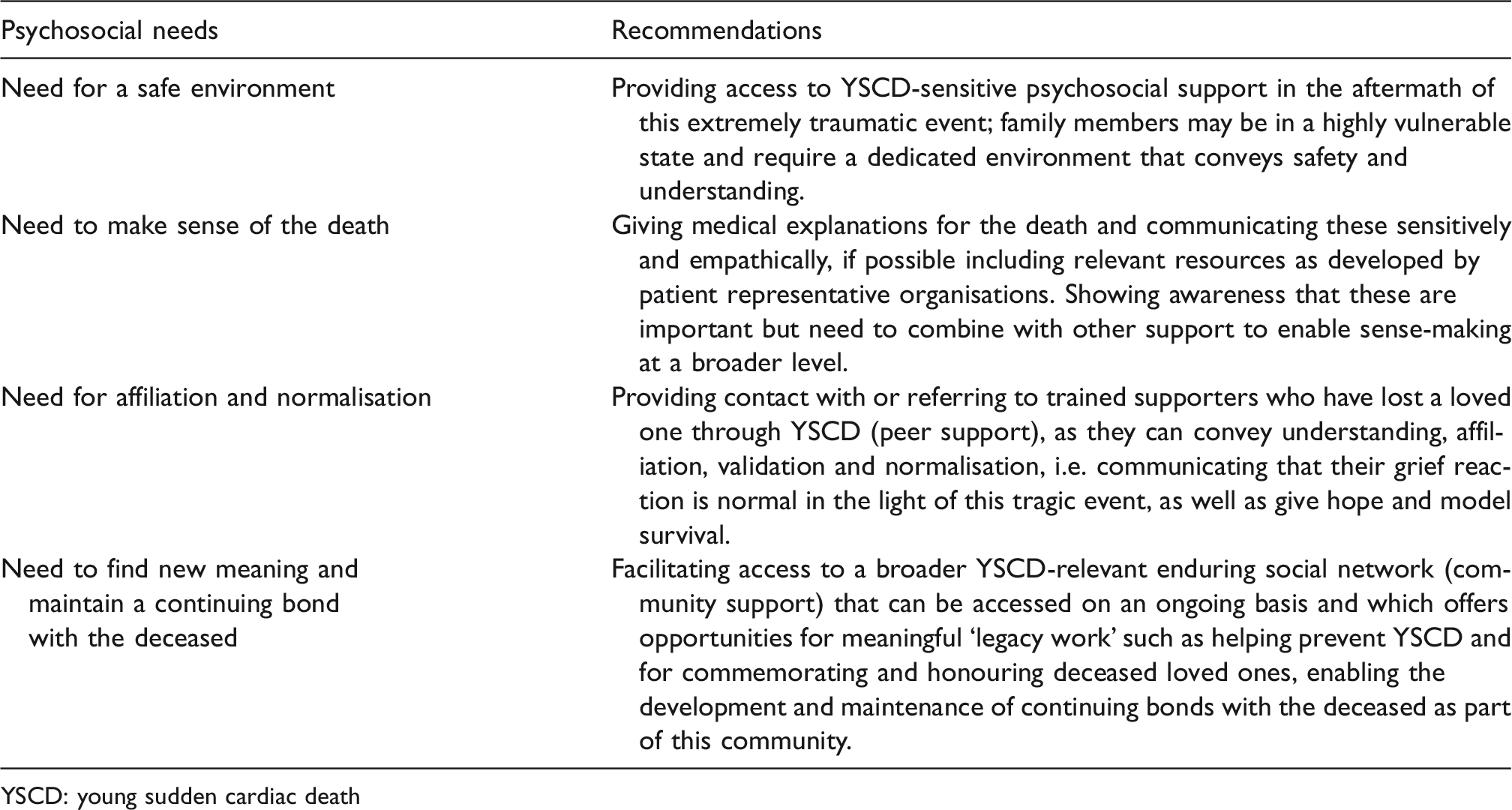
YSCD: young sudden cardiac death
Limitations
The present study is based on a sample drawn from an YSCD-specific UK charity, Cardiac Risk in the Young (CRY). Participants were already engaged with the organisation and may have been motivated to emphasise the benefits of this involvement. However, previous research with non-involved samples stressed people’s expressed need for community support, and our study provides evidence for what YSCD-affected families perceive as effective support. Psychosocial support needs and impacts relating to provision outside YSCD-dedicated settings were not our focus. Future qualitative research could explore YSCD-affected families’ psychosocial support needs and experiences relating to informal support networks, or other formal provisions such as workplace assistance or religious community support. Another limitation of the research is that while the entire database of the support organisation had been contacted, only some chose to contact the researchers, and out of those who wanted to participate, not all were able to. However, the recruitment of a broad sample across the three stakeholder groups means that the themes are likely to be common in this population.
Conclusions
YSCD-affected families can benefit from having access to YSCD-sensitive peer and community support. Whilst YSCD trauma and the associated experiences of loss are often characterised by their uniqueness and isolating consequences, the concept of recovery seems to be anchored in social relationships. What is particularly important is the rebuilding of a sense of belonging through a community that can provide an anchor and a home to affected families, enabling meaning-making and the maintenance of continuing bonds with the loved ones who are no longer physically present. This paper highlights the need to incorporate patient representative groups and peer-to-peer support into patient pathways. Clinicians need to be aware that this is an essential part of patient care.
Implications for practice
Provide safety through young sudden cardiac death-sensitive support; Communicate medical explanations sensitively; Allow for sense-making of death through ongoing support; Refer to peer supporters for normalisation of grief; Facilitate involvement in an enduring young sudden cardiac death-specific network.
Supplemental Material
sj-pdf-1-cnu-10.1177_1474515120922347 - Supplemental material for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support
Supplemental material, sj-pdf-1-cnu-10.1177_1474515120922347 for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support by Edith Maria Steffen, Lada Timotijevic and Adrian Coyle in European Journal of Cardiovascular Nursing
Supplemental Material
sj-pdf-2-cnu-10.1177_1474515120922347 - Supplemental material for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support
Supplemental material, sj-pdf-2-cnu-10.1177_1474515120922347 for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support by Edith Maria Steffen, Lada Timotijevic and Adrian Coyle in European Journal of Cardiovascular Nursing
Supplemental Material
sj-pdf-3-cnu-10.1177_1474515120922347 - Supplemental material for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support
Supplemental material, sj-pdf-3-cnu-10.1177_1474515120922347 for A qualitative analysis of psychosocial needs and support impacts in families affected by young sudden cardiac death: The role of community and peer support by Edith Maria Steffen, Lada Timotijevic and Adrian Coyle in European Journal of Cardiovascular Nursing
Footnotes
Acknowledgments
Author contribution: LT, AC and EMS designed the study. EMS organised the data collection and set up the study. EMS and AC collected the data. EMS, LT and AC analysed the data. EMS wrote the first draft. All authors commented on and amended the draft. We would like to thank Cardiac Risk in the Young (CRY) for enabling access to their supporters and users. Special thanks go to Mrs Alison Cox, MBE, the Founder of CRY, and Ms Lily Burke, Support Programme Manager, CRY, for their effort in helping recruit the participants into the study. We wish to thank especially the YSCD-bereaved participants who volunteered and generously gave of their time to take part in focus groups or individual interviews. We would also like to thank Dr Andrea Malden for her contribution in the early stages of the project.
Declaration of conflicting interests
The authors have no conflicts of interest to declare.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the UK-based charity, Cardiac Risk in the Young (CRY), grant number 115504.
Supplementary material
Supplementary material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
