Abstract
Summary
The COVID-19 pandemic has had a negative impact on older adults in geriatric residential care facilities worldwide. In Canada, the mortality rate in these care settings was particularly high. To curb the spread of the virus, social distancing and other restrictions were introduced with inadvertent negative impacts on psychosocial well-being of residents in facilities. The goal of this Living Systematic Review (LSR) was to synthesize emerging evidence on social care strategies in Canadian residential care facilities during the COVID-19 pandemic.
Findings
Results from the 35 studies show that the inclusion of older adults from residential care in research samples has been rare. Also, most of the identified social care interventions were on micro-, meso-, and exolevels, whereas macrolevel focus was limited.
Applications
For the profound systemic impact of macropolicies, future studies should evaluate macrolevel interventions to ensure high quality of geriatric residential care in Canada. Also, future research should amplify the voices of older adults living in these care settings. Finally, greater attention to social care is required in Canadian geriatric residential care facilities.
Background
The COVID-19 pandemic had a profoundly negative impact on older adult populations worldwide, marked by particularly high death rates among the residents of congregate care facilities such as long-term care and assisted or supportive living settings (Hsu et al., 2020; Iaboni et al., 2020; Miller, 2020). Advanced age and decreased immune system due to multiple chronic health conditions as well as the communal living situation elevated the risk of infections and mortality in residents of these care settings (Iaboni et al., 2020). In the first six months of the pandemic, over 80% of all reported COVID-19 deaths in Canada were in geriatric residential care facilities, compared to an average of 38% in similar care settings in other developed countries, members of the Organization of Economic Co-operation and Development (CIHI, 2020; Sepulveda et al., 2020). By July 2022, the COVID-19-related deaths in Canadian geriatric residential care fell to 43% of all pandemic-related deaths in the nation (NIA, 2022). However, facility residents were still disproportionately affected as they represented 6.8% of all older adults in Canada (Employment and Social Development Canada, 2019).
To curb the mortality rate, strict public measures were introduced in Canadian residential care facilities, including social distancing, family visitation restrictions, etc. (CIHI, 2020). However, these restrictive measures resulted in unintentional adverse psychosocial and environmental effects, such as social isolation, loneliness, and decreased social support (El Haj et al., 2020; Figueroa & Aguilera, 2020; Hsu et al., 2022; Iyamu et al., 2023; Miller, 2020; Nwachukwu et al., 2020; Reid et al., 2023; Thombs et al., 2020). Social isolation had already been a long-standing unaddressed issue in residential care facilities before the onset of the pandemic (Nicholson, 2012). Enforcing physical and social distancing to prevent the spread of the COVID-19 rendered older adults in these care settings more vulnerable to the harms arising from social isolation and loneliness (Chu et al., 2020, 2023; Power & Carson, 2022).
Research evidence suggested that unaddressed social care needs during the COVID-19 pandemic such as loneliness, social isolation, social exclusion, decreased safety net, and other social determinants of health (Raphael et al., 2020) were associated with adverse health outcomes, including increased mortality and healthcare costs (Office et al., 2020). In healthcare settings, such as residential care facilities, social care refers to services and interventions that cater to health-related social needs (National Academies of Sciences, Engineering, and Medicine, 2019). In Canada, social care in geriatric residential care facilities has been long underprioritized in favor of physical care (Azulai & Hall, 2020). However, human life is not only about physical health; social care is essential and requires equal attention (Azulai & Hall, 2020).
Considering the COVID-19 pandemic and its devastating impact on the social environment, there has been a rapid growth of studies on various social care strategies in geriatric residential care facilities to alleviate social isolation, social exclusion and other concerns (Bilal et al., 2020; Figueroa & Aguilera, 2020; Jecker, 2021; Khowaja et al., 2023; Office et al., 2020; Sepúlveda-Loyola et al., 2020). Sun et al. (2023) found that “social isolation” was the 14th most found keyword in their bibliometrics study on COVID-19 in long-term care facilities. Some scholars reported the emerging use of technology as a strategy to mitigate psychosocial impacts of the pandemic, referring to telehealth and various digital social connection tools, including emails, social media, and other forms of digital technology or electronic communication (Bilal et al., 2020; Clayton & Astell, 2022; Figueroa & Aguilera, 2020; Khowaja et al., 2023). Sepúlveda-Loyola et al. (2020) recommended a multifaceted program of services to include physical exercise and technology, such as software applications, online videos, and telehealth. Other studies on social care interventions for older adults during the pandemic suggested medical student telephone contact with older adults to reduce social isolation (Office et al., 2020), sociable robots for older people (Jecker, 2021), and iPads to allow for communication outside the facilities (Khowaja et al., 2023).
Evidence on the usability of these strategies is inconclusive. In a systematic review of the barriers to utilizing telehealth with older adults to improve access to wellness services in the lockdown, Kruse et al. (2020) suggested that, although telehealth improves access and proximity to services for populations with chronic health and mental health and mobility restrictions, the utilization can be hindered by technical literacy level of older adults, costs involved, and a lack of desire to engage through technology on the part of some residents. Sacco et al. (2020) reported that older adults in residential care facilities express satisfaction with video calls and phone calls when they are helped to ensure access and connection, meaning that technological solutions should be applied while considering the level of physical, cognitive, and mental health ability of residents to utilize technology, as well as environmental infrastructure conditions. However, Khowaja et al. (2023) commented that access to funding for digital technology has been limited in these care settings.
In an investigation into long-term care policies, Irwin et al. (2023) found that basic care often took precedence over quality of life within long-term care policies. Colenda et al. (2020) attributed a lack of attention to quality of life of older adults in residential care facilities to the growing ageist bias that implied a devaluation of individuals as they age as not valuable members of society and, therefore, leading to the social exclusion of older adults from services that other population groups would have access to. Further investigation of social care strategies in geriatric residential care is necessary to respond to the devastating impact of the pandemic on the social environment of older adults in these care settings (Bilal et al., 2020; Figueroa & Aguilera, 2020; Thombs et al., 2020).
Thus far, no knowledge synthesis of social care strategies during the COVID-19 pandemic in Canadian geriatric residential care facilities has been conducted. Therefore, the goal of this study was to synthesize the emerging knowledge on social care strategies used in Canadian geriatric facilities during the pandemic and to identify gaps in addressing social determinants of health (Raphael et al., 2020) in these care settings. This article presents findings on social care strategies, while findings on social determinants of health are published elsewhere.
Methods
Research Question
This knowledge synthesis study sets out to answer the following research question: What social care strategies have been used in geriatric residential care facilities in Canada during the COVID-19 pandemic?
Design
The research team conducted a Living Systematic Review (LSR) (Brooker et al., 2019) to synthesize all emerging evidence from the start of the pandemic in Canada in 2020 until July 2023. Brooker et al. (2019) define LSR as a type of systematic literature review that is updated on an ongoing basis to include pertinent emerging evidence as it becomes available (p. 6). As an emerging approach to knowledge synthesis, LSR has been growing in popularity owing to its ability to collect and integrate current and reliable data. The main premise of the LSR method is that evidence in conventional systematic reviews is often collected in retrospect, after which point continually maintaining the currency of systematic reviews is not feasible; this means that there is a risk of missing important new evidence on the topic (Brooker et al., 2019).
The core principles of the LSR method are like other Cochrane Reviews (Brooker et al., 2019) but diverge in disclosing decisions on the frequency of periodic screens for new evidence (e.g., monthly, weekly, etc.) as well as at which points and how new evidence is incorporated into the review. This ongoing knowledge synthesis can benefit policy and practice decision-makers, researchers, and educators to integrate research and practice (Brooker et al., 2019; Thombs et al., 2020).
Thombs and colleagues (2020) provided a recent example of LSR when curating and synthesizing emerging evidence on mental health during the COVID-19 pandemic. Other researchers who also conducted LSR studies reflected on their experiences and challenges, providing guidance and recommendations as well as highlighting that LSR requires considerable resources but are important, especially in healthcare, in continually presenting new evidence in a topic area and informing policy and practice (Butler et al., 2024; Heron et al., 2023; Iannizzi et al., 2022; Millard et al., 2019; Wagner et al., 2024). Owing to these benefits, LSR presented as a suitable method for the current study to allow for the ongoing review and synthesis of the rapidly emerging research evidence during the COVID-19 pandemic. The study followed the Cochrane protocol and guidance for LSR (Brooker et al., 2019). It was registered in PROSPERO as a systematic literature review.
Data Collection
Timeline
The research team conducted three sets of literature searches at different points in time: first search (January 2020 to October 2021), second search (October 2021–September 2022), and third search (September 2022 to July 2023). The decision to end the data collection in July 2023 and transition the LSR out of the living phase (Brooker et al., 2019, p. 38) was informed by the report of the World Health Organization (WHO) in May 2023, who declared that although COVID-19 has been “an ongoing health issue, … [it] no longer constitutes a public health emergency of international concern” (WHO, 2023, para. 3).
Eligibility Criteria
The eligibility criteria included original research studies that used any research methodology, published in peer-reviewed journals in English language, conducted during the defined time period of the COVID-19 pandemic (January 2020 to June 2023) in Canadian geriatric congregate residential care facilities (i.e., long-term care facilities or nursing homes, and assisted or supportive living settings), included older adults in the sample, and focused on social care and social determinants of health.
Search Strategy
The searches were conducted in English-language databases (Canadian Business and Current Affairs (ProQuest), CINAHL Plus with Full Text, MEDLINE (EBSCO), Nursing and Allied Health (ProQuest), ProQuest Public Health, PubMed, SAGE Journals Online, Social Science Citation Index, Social Services Abstracts (ProQuest), Social Work Abstracts (EBSCO), SocINDEX with Full Text (EBSCO), Sociological Abstracts (ProQuest), SpringerLink, Taylor and Francis Social Sciences and Humanities Journal Collection, and Wiley Online Library). Limiters were utilized in each database if applicable (i.e., date, language, location, peer-reviewed, article/journal type).
The search strategy employed Boolean string to include terms such as residential care, long-term care, assisted living, supported living, nursing home, skilled nursing, continuing care, institutional care, lodge, covid, covid-19, coronavirus, 2019-ncov, sars-cov-2, cov-19, pandemic, and COVID-19 (Supplementary Material). The first search generated a lot of articles that were not Canadian. Therefore, the Boolean string was updated (Campbell, 2022) for use in the following two searches (Supplementary Material).
Data Management
The research team used Zotero citation software (Zotero, Inc, n.d.) for the management of the research citations as well as for the initial screening of titles. Rayyan data management software (Rayyan, Inc., 2021) was utilized for the screening of abstracts against the inclusion criteria, and Google Sheets application software was used for the management of the included articles. These software tools were selected for their robustness in conjunction with their free open access to the public.
Article Selection
Articles emerging from the initial search in the selected databases were first imported into the Zotero data management system, where the groups of at least two research members reviewed the titles of the identified articles, removing duplicates and articles irrelevant to the study domain. The initial three data search rounds in this systematic review identified 95,706 studies, of which only 4,339 were found relevant for the abstract screening phase. The remaining articles were transferred to Rayyan for abstract screening, where each article was screened blindly by at least two research members against the study eligibility criteria. Blind setting was turned off in Rayyan to review, discuss, and collectively resolve any decision conflicts among the research team members. At times, full articles had to be retrieved to resolve the conflicts.
The resultant 35 studies, fully meeting the eligibility criteria, have been included in this systematic review for the data analysis. Figure 1 presents the PRISMA flow chart that summarizes the search strategy, screening process, and the search outcomes.
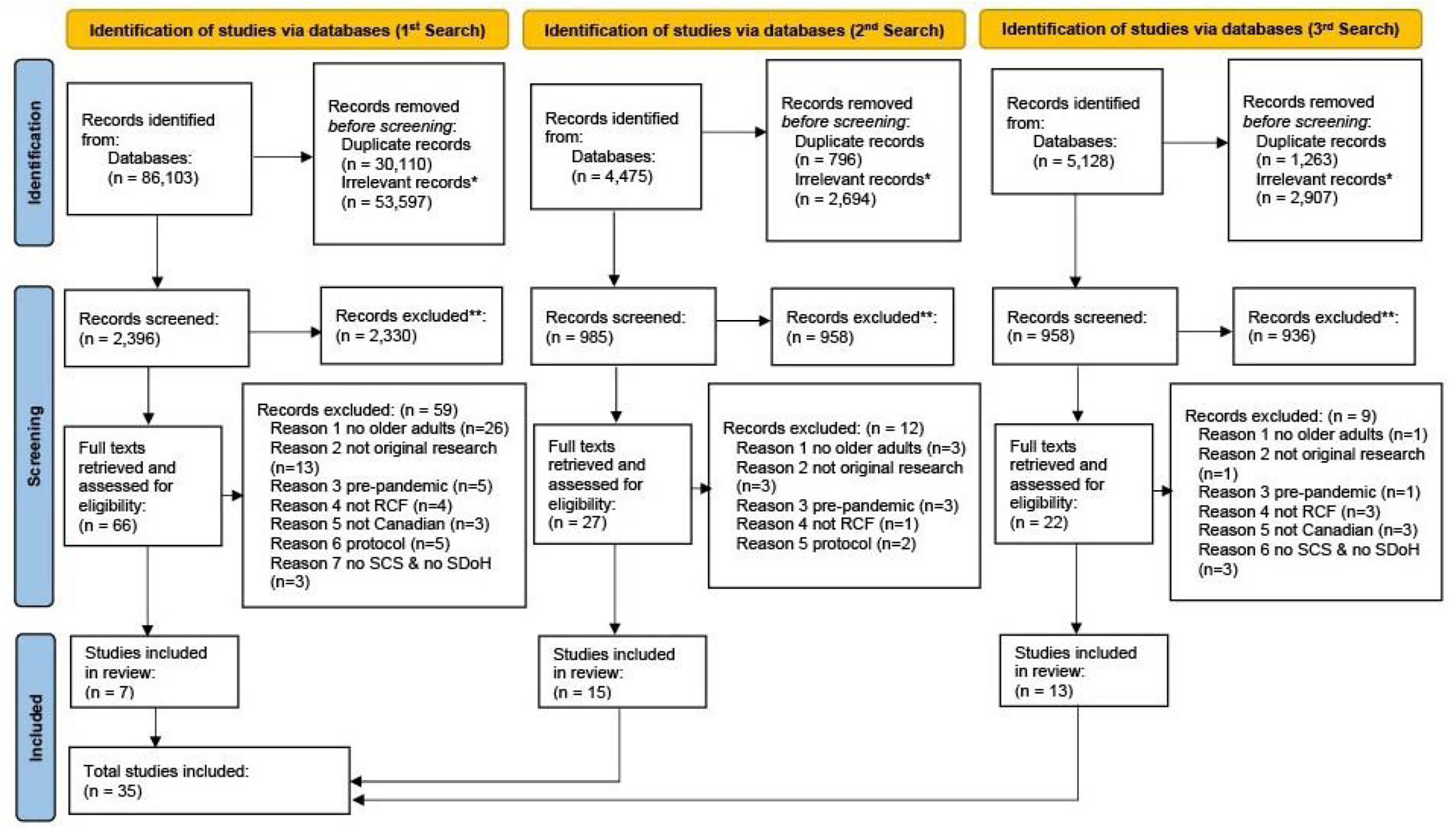
PRISMA Flow Chart of the Study Design.
Data Analysis
Theoretical Framework
This study was informed by the Ecological Systems theory by Uri Bronfenbrenner (Crawford, 2020). Ecological Systems theory describes human social experience as a function of five interconnecting systems: the microsystem (the person's immediate interpersonal interactions), mesosystem (interactions between microsystems), exosystem (interactions on the institutional or community level that affect a person), macrosystem (socio-cultural values and structure), and chronosystem (the impacts of time and historical events on the person's life) (Crawford, 2020).
Confirmatory Document Analysis Method
The data in the included articles were analyzed manually, using confirmatory document analysis (Bowen, 2009), which refers to “defining … categories (often themes) prior to reviewing the data, and then systematically searching the data for instances or expressions of these categories” (Guest et al., 2013, p. 254). This type of qualitative analysis is deductive and directional in how a researcher “draws from existing theory to set up the categories/themes that guide the research” (Kibiswa, 2019, p. 2059). Within the predefined themes, confirmatory document analysis focused on developing codes, grouped into the predefined categories. In this study, social care strategies in the selected articles were identified and coded inductively and then organized deductively into micro, meso, exo, and macrosystems categories as per the definitions in the Ecological Systems Theory (Crawford, 2020). The chronosystem for the population of older adults in residential care facilities in this study was predetermined as the COVID-19 pandemic.
At least two research team members analyzed each eligible article to identify social care strategies. Any conflicts were resolved through discussion with the entire team. The results were then synthesized and presented narratively.
As part of the LSR process, the team disseminated preliminary findings from the first search through presentations, conferences, and media interviews. In this article, the final results from all three searchers are integrated and reported.
Quality Appraisal
The research team conducted a quality appraisal of each included article. A variety of research methodologies, designs, samples, data collection strategies, data analyses, and reporting styles proved difficult in selecting a suitable quality appraisal approach. Mertz (2019) states that such a challenge is a recognized conundrum in systematic literature reviews, which currently does not have a perfect resolution even by the most robust methods. From the feasibility perspective, the quality appraisal in this study was based on the clarity of information that the studies provided on methodological choices, using the following four questions: Q1. Are the study goal and research question/s clearly stated? Q2. Is the study design appropriate for answering research questions? Q3. Are methods and procedures described clearly in sufficient detail? Q4. Have the research questions been answered?
Each of the four questions was ranked on a scale from 0 to 2 (0 = not at all; 1 = partially done; 2 = fully done), so that each study received a total quality score from 0 (poor) to a maximum of 8 (excellent) quality. Out of the 35 assessed studies, 23 (about 65%) scored an 8, demonstrating excellent quality. However, 13 studies lost quality points for either not reporting the sample size, not reporting a clear research question or goal, or for methodological lack of clarity (Table 1).
Quality Appraisal of Selected Articles from the First, Second, and Third Searchers (N = 35 Articles; 613,508 Older Adults).
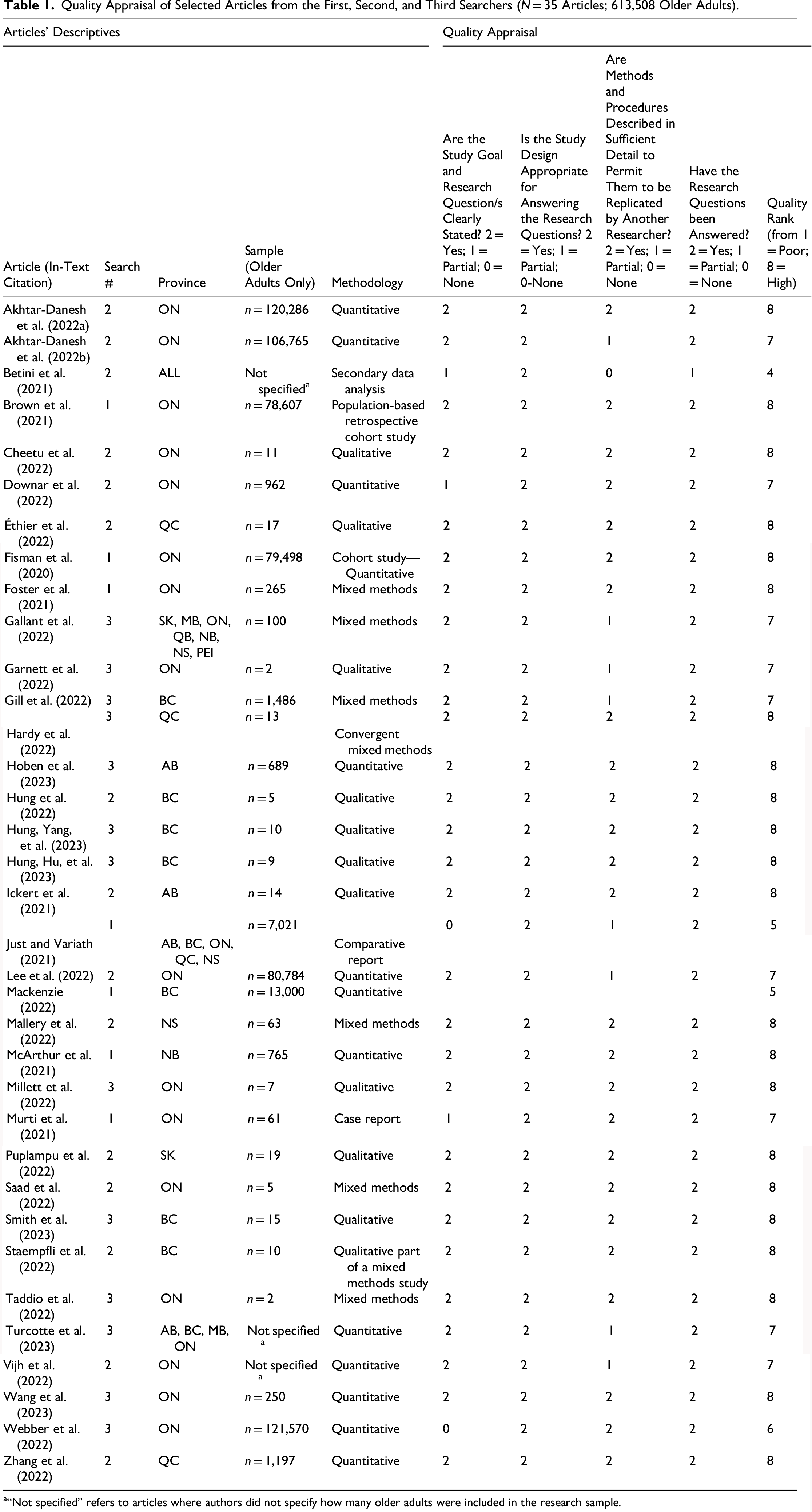
“Not specified” refers to articles where authors did not specify how many older adults were included in the research sample.
Results
Included Studies
Thirty-five (N = 35) included studies had a cumulative sample of 613,508 older adults, except for three studies that did not clearly report numbers of older adults involved but rather reported numbers of facilities and other residents’ data. Most studies were conducted in specific Canadian provinces, including Ontario (19 studies), British Columbia (9), Quebec (5), Alberta (4), Nova Scotia (3), New Brunswick (2), Manitoba (2), Saskatchewan (2), and Prince Edward Island (1). One study was pan-Canadian (Table 1).
Social Care Strategies in Residential Care Facilities During the Pandemic
Out of 35 included studies, only 21 mentioned social care strategies of some sort for older adults in facilities during the time of the COVID-19 pandemic: three articles from the first search, and nine articles in each of the second and third searches. These social care strategies are organized in Table 2, as they pertain to the four main systems of Bronfenbrenner's Ecological Systems Theory: micro, meso, exo, and macrosystems (Crawford, 2020). Almost all articles provided examples of social care strategies on the microsystem level (n = 20), followed by exosystem strategies (n = 18) and mesosystem strategies (n = 16). Only five articles suggested macrolevel strategies.
Social Care Strategies in Residential Care Facilities at Different System Levels (N = 21).
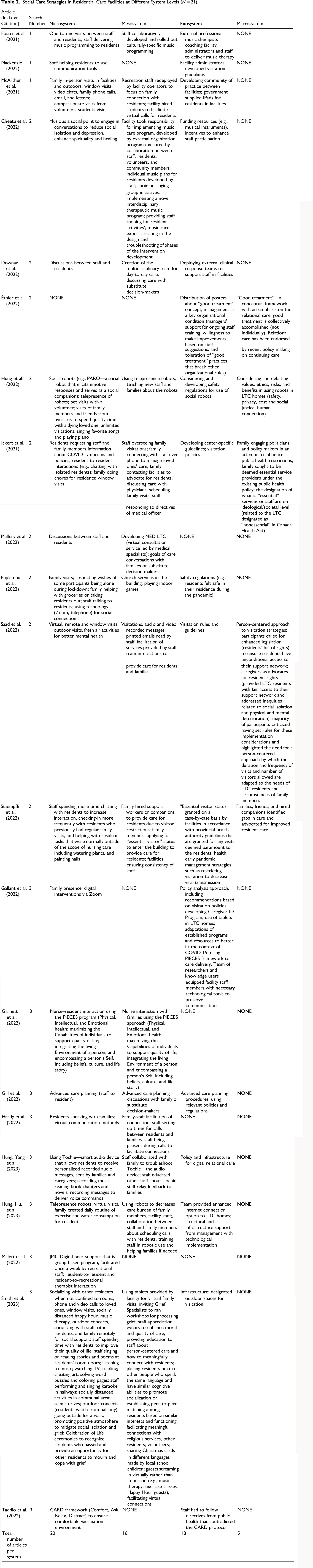
Examples of the microsystem social care strategies, offered on the level of residents interacting with their microsystems included direct interpersonal or remote staff–resident interactions (e.g., care provision, music activities provision, helping residents to use technology or communication tools, robots, discussing advanced care planning with residents, helping residents to write letters to families, etc.), family–resident interactions (in-person visits, window visits, phone conversations, direct care provision), resident–volunteer interactions (compassionate visits), resident-to-resident interactions (socializing with other residents or attending peer-support groups) (Table 2).
Mesolevel strategies entailed interactions between various microsystems. For example, collaboration between staff, families, volunteers, clergy, and community members to develop and roll out various programming for residents (music and other recreational programs, robotic programs, medical specialist virtual consultation programs, programs to cope with grief and loss), staff supporting families, staff providing feedback to families, facilitating connections with families, overseeing family visitations, staff discussing advanced care planning of residents with their families as proxies, creating interprofessional care plans for residents, families hiring support workers to provide care for their loved once in their absence due to visitation restrictions, etc. (Table 2).
Exosystem level includes interactions between mesosystems, which indirectly impact residents’ lives. As Table 2 shows, examples of exolevel interventions are facility infrastructure, such as availability of outdoor spaces for residents, facilities providing technology infrastructure (Internet connection, tablets for residents), funding and resource allocations by facilities and provincial governments, including allocation and education of staff, facility policies and regulations, policy analysis, application of PIECES framework to care planning (physical, intellectual, emotional, capabilities, environmental, social aspects of care), collaboration between facilities and external organizations (government, researchers, community organizations, etc.) to benefit residents’ social care provision, designating “essential visitor” status to families to support residents’ care, visitation rules and guidelines, safety regulations and staff employment procedures, developing posters for information sharing with staff, families, and residents, developing communities of practice for staff across facilities, etc.
Finally, macrolevel strategies manifested in developing and endorsing conceptual frameworks for care, grounded in professional and societal values on social care (e.g., person-centered approach to care), family advocacy to engage politicians and facility administrators to improve social care for residents, bringing value-laden terminology that defines care for deliberation and reconsideration (e.g., a conviction that families must be designated as essential care visitors because they support staff in providing essential care services to residents in facilities), and identifying and publicizing gaps in geriatric residential care to promote social change (Table 2).
Discussion and Implications
This systematic narrative review synthesizes all emerging evidence on social care strategies used in Canadian geriatric residential care facilities during the COVID-19 pandemic between 2020–2023. Findings indicate a lack of inclusion of older adults in research and limited focus on macrolevel interventions to enhance social care as discussed below.
Underrepresentation of Older Adults in Research
One of the main findings of the study was the limited amount of research that includes older adults as research participants. Many relevant studies were excluded from this review because they relied on collateral sources to learn about older adults. Underrepresentation of older adults in research has been well acknowledged (Petrovsky et al., 2022). Some reasons for this phenomenon include a combination of ageist bias, financial constraints of researchers and communication difficulties with older adults with chronic health conditions (e.g., hearing challenges, impaired vision, physical immobility, cognitive impairment, etc.) (Azulai, 2014; Barrett et al., 2021; Bernstein et al., 2022; Colenda et al., 2020; Swift & Chasteen, 2021). Future studies should aspire to include older adults in research about their experiences.
Social Care Strategies in Geriatric Residential Care in Canada
Findings in this study show that the most frequently used social care strategies were on the micro, meso, and exosystems’ levels, while macrosystem strategies were rarely utilized. Microlevel social care strategies (e.g., interpersonal or remote interactions between residents and their staff, residents and their family members, volunteers, or other residents) were effective when implemented. However, microlevel interventions rely on direct interaction between a client and their environment, whether it is in-person or at a distance. These direct interactions were not always available during COVID-19 due to the pandemic restrictions and systemic challenges, prompting decreased social support for residents, social isolation, and loneliness. Supporting this finding, previous studies document how decreased social support due to social distancing and restrictions on family visitation presents risks to safety and wellbeing of residents in residential care facilities (El Haj et al., 2020; Figueroa & Aguilera, 2020; Miller, 2020; Nwachukwu et al., 2020; Thombs et al., 2020).
Social care strategies on the mesolevel in this review include interprofessional and multidisciplinary collaboration between staff members and various healthcare providers or community services, as well as staff facilitating virtual visits between residents and families. Developing and rolling out various programming for residents was another mesostrategy (e.g., music program, virtual dance program, employing telerobots for residents, virtual consultation service with physicians and other care providers, etc.). These findings are congruent with previous research, testifying to the beneficial use of programmatic enhancements and technology to enhance healthcare provision in residential care (Ashcroft et al., 2022; Office et al., 2020). For example, Jecker (2021) describes utilizing sociable robots for older people to mitigate psychosocial impacts of the pandemic. Other scholars document using telehealth, digital social connection tools, emails, social media platforms, and other forms of digital technology or electronic communication to facilitate connection and social health between residents and their social environment (Bilal et al., 2020; Clayton & Astell, 2022; Figueroa & Aguilera, 2020; Khowaja et al., 2023; Sepúlveda-Loyola et al., 2020). Still others comment on the importance of increasing access to computer hardware like iPads and laptops to improve channels of communication, social connection, and social stimulation (Khowaja et al., 2023).
Social care strategies on the exolevel in this systematic review include developing technology infrastructure by facility operators, ensuring funding and resources allocation by facilities and provincial governments, including education of staff. These strategies also include facility policies and regulations such as visitation rules and guidelines, safety regulations, staff employment procedures, developing communities of practice for staff across facilities, fostering collaboration between facilities and external organizations to benefit residents’ social care provision, and developing information posters to share with staff, families, and residents. One of such collaborative strategies is implementation of PIECES model, which refers to the following aspects of care provision: Physical, Intellectual, and Emotional health; maximizing the Capabilities of an individual to support quality of life; integrating the living Environment of a person; and encompassing a person's Self, including beliefs, culture, and life story (Garnett et al., 2022). Supporting the finding on PIECES in this review, Garnett et al. (2022) state that PIECES model has been implemented across Canada by interprofessional teams in a variety of medical settings, including residential care facilities. Implementation of PIECES requires an interactive effort on the micro–meso and exolevels of care, including adequate facility infrastructure to address living environment.
The importance of adequate facility infrastructure for social care has been mentioned in previous research (Ashcroft et al., 2022). For example, to successfully provide family virtual visits, telehealth, and virtual social and recreational care, facilities must ensure effective Internet connection and equip all clients with digital devices (Bilal et al., 2020; Clayton & Astell, 2022).
Organizational factors, such as built environment, institutional policies and facility culture are also important exofactors that influence social care in residential facilities (Hunter et al., 2024).
Some scholars document the crucial role of the built environment as enabling or hindering direct care delivery, demonstrating how facility infrastructure, layout and physical conditions on the exolevel interconnect with the mesolevel of care organization and the microlevel of care provision (Gurung & Chaudhury, 2023). For instance, Young and colleagues (2024) argue that traditional long-term care facilities, built as institutions, had higher mortality rates during the pandemic than more home-like residential environments such as the Green Houses model. Also, geographical location has been a factor in differing infrastructure, organizational culture conditions, and care organization in the facilities (Egbujie et al. (2024). For example, Ontario and Quebec facilities struggled more to meet the needs of their residents during the pandemic than facilities in other Canadian provinces (Liu et al., 2020).
Aside from the built environment, institutional policies and organizational culture play a critical role in care delivery. For example, deprioritizing compensation for difficult labor of personal care in residential care facilities has created a deterring environment for trained and qualified labor force, who are forced to look for employment elsewhere for higher earnings and better working conditions. Developed nations, like Canada, the U.K., and the U.S., are increasingly relying on an underpaid and undertrained immigrant women as a major workforce in geriatric residential care (Chamberlain et al., 2019; Estabrooks et al., 2015). Recent Canadian studies document worsening mental health, burnout, and decreased professional efficacy of underpaid, understaffed, and overworked Personal Support Care Workers (aka Healthcare Aides in Canada) in geriatric residential care during the pandemic (Boamah et al., 2023; Song et al., 2024). As Lowndes and colleagues (2021) argue in another Canadian study, “conditions of work are the conditions of care.” These conditions include setting's location, physical layout of facilities, staffing levels, work organization, and governing regulations, which impact the social care of residents as well as their overall health and wellbeing (Lowndes et al., 2021).
Another example of institutional policy is visitation rules and guidelines in facilities during the pandemic, which disrupted the roles of family members as care partners due to their mis-conceptualization as nonessential personnel (Lecours et al., 2023). Being designated as nonessential is particularly unsettling in the context of Canadian facilities historically relying on family members to supplement personal care due to inadequate funding, vague care standards, and the resultant few hours of professional direct care for the residents (Lecours et al., 2023). This reminds how social workers in Canada, who had provided direct social care in facilities prior to the pandemic, were designated as nonessential workers during the pandemic and denied opportunities for in-person communication with facility residents and staff (Ashcroft et al., 2022).
For the resultant inability to provide adequate necessary in-person care to older adults in some facilities, the Government of Canada had to deploy Canadian Armed Forces to ensure basic care to struggling and ill residents (Government of Canada, 2023). This illustrates how physical restrictions policies in medical settings without psychosocial considerations can harm the biopsychosocial care of patients (Ashcroft et al., 2022).
Macrosystem social care strategies in this systematic review included macro policies and social values on care for vulnerable older adults in Canada, such as person-centered care on the policy level, family policy advocacy to improve social care for older adults in Canadian residential care facilities and identifying and publicizing gaps in geriatric residential care to promote social change. It is important to reconsider value-laden terminology that defines aging care. For instance, in the context of the earlier mentioned exclusion of families as nonessential in care of their loved ones, there is a need in health and social policy change to formally redefine families as essential care personnel owing to their necessary and valuable contributions to client care provision.
Restricting access of family members as nonessential visitors during the pandemic has been grounded in the historical macro policies on medical care provision in Canada, some of which are outdated in prioritizing physical care over patients’ psychosocial and other needs. Keefe et al. (2022) studied 21 policies that regulate long-term care in four Canadian provinces to understand how the Canadian system facilitates or inhibits family involvement in the context of historical underfunding of the long-term care sector. The authors confirm the long-standing gap in the provincial and territorial government policies on supporting familial contribution in geriatric residential care facilities. Keefe et al. (2022) as well as Irwin et al. (2023) in their more recent study of Canadian long-term care policies conclude that some existing policies are mainly focused on security and safety, deemphasizing quality of life and relational aspects of care in the geriatric residential care facilities.
In Canada, the long-term care sector is outside of the scope of the Canada Health Act 1985 (Legislative Services Branch, 2017), where long-term care services are declared nonessential and funded modestly as opposed to the essential hospital care services (Government of Canada, 2023). This part of the legislation does not reflect the contemporary reality of the Canadian older adult population in residential care facilities with complex health, mental health, and social care needs. Meeting social care needs necessitates organizational and government policies that acknowledge the importance of social care and focus on enhancing social safety net and overall well-being (Cederbaum et al., 2022).
Thankfully, there has been a promising cultural shift towards resident-focused quality of life and greater person-centeredness of care (Irwin et al., 2023). The Government of Canada (2023) has acknowledged that the COVID-19 pandemic illuminated the long-standing systemic challenges in long-term care facilities across Canada, including infection prevention, quality of care, staffing, and infrastructure. This has prompted the Minister of Health and the Minister of Seniors to begin developing a Safe Long-Term Care Act (Government of Canada, 2023), which is yet to be scheduled for review at the time of writing of this paper. Also, the COVID-19 pandemic has renewed public interest in improving the quality of care in geriatric residential acre facilities, leading to the development or revision of national best-practice guidelines on care standards in Canada (Kirkham et al., 2024). Specifically, Kirkham et al. (2024) mention National Long-Term Care Services Standards 2023 by the Health Standards Organization (2023), Long-Term Care Home Operations and Infection Prevention and Control by Canadian Standards Association (CSA Group, 2023), and Mental Health and Well-Being in Long-Term Care and Assisted Living Settings Guidelines by the CSA Group that have been in development.
In addition to federal policies, Keefe et al. (2022) document developing provincial post-pandemic policies to enable increased meaningful family engagement and focus on the quality of life of residents in the facilities in British Columbia, Alberta, Ontario, and Nova Scotia. For instance, a new legislation in Alberta, Continuing Care Act 2022, was developed and passed to repeal the earlier Nursing Homes Act, Supportive Living Accommodation Licensing Act, Long-Term Care Information Act, and Resident and Family Councils Act. This new policy covers the revised content of the repealed acts under one legislation piece (Government of Alberta, 2024).
These new policies and their complex impact across all systems levels on care organization, care delivery, and health outcomes of older adults in residential care facilities in Canada will need to be studied and evaluated in future research. It is important to leverage this macro policy shift to enhance advocacy, increase organizational capacity and further develop policies that promote quality of life and person-centeredness in Canadian geriatric residential care.
Limitations of the Study
We recognize that this study has limitations. First, there is a potential selection bias. Although the research team screened a vast variety of databases, it was not feasible to include all available databases. Likewise, our inclusion criterion of only original peer-reviewed publications has resulted in omitting gray literature reports, preprints, scoping and systematic reviews, thereby potentially missing some relevant sources. Also, the selected articles were all published in English. It is possible that relevant Canadian studies published in French were missed. Furthermore, we excluded articles that did not use older adults in samples; thus we could have missed a segment of relevant evidence collected from collateral and proxy sources. However, discovering the profound lack of studies that include older adults as research participants is an important finding. Next, using the formally defined COVID-19 pandemic timeframe as the search boundaries means that studies published after July 2023 were not included in this systematic review. However, the team is confident that with the considerable time and effort in screening an impressive amount of information, the results of this study are sufficiently robust.
Second, using the Ecological Systems theory as theoretical lenses has offered valuable insights and helped organize the findings. However, it is plausible that another perspective, potentially, could have provided different insights.
Third, our decision to use a deductive method of qualitative data analysis could have limited the emergence of novel insights. An inductive method might have helped to offset this limitation. Unfortunately, this was not feasible in this study due to the time constraints.
Fourth, the LSR method implies ongoing data collection and analysis after the study is finished. In the case of this systematic review, however, the team was focused on the COVID-19 acute pandemic phase, which was formally declared as concluded in 2023. This effectively determined the boundaries for our data collection. The team recognized this methodological conflict with the LSR method only close to the completion of the study. The suitability and feasibility of the LSR method, therefore, needs to be explored in future.
Finally, the research team agrees with Thombs et al. (2020) on the importance of robust quality evaluation of the rapidly proliferating research during the COVID-19 pandemic. It can be argued that the simplified quality appraisal in this study may not have been robust enough. However, according to Mertz (2019), there is no one currently available quality appraisal tool that perfectly accounts for the methodological and content diversity of the studies in systematic reviews. The simplified approach used in this review was successful in identifying 35% of the included studies that lost quality points, meaning that the findings of this review should be interpreted with caution.
Significance and Conclusion
This study is the first systematic review of social care strategies in Canadian geriatric residential care facilities during the COVID-19 pandemic. There is a growing recognition among human service and medical professionals about the impact of social environment and social needs on human well-being, quality of life, health outcomes, and healthcare costs (Irwin et al., 2023; Keefe et al., 2022). Understanding which social care strategies can be implemented is beneficial for social workers, nurse professionals, physical and occupational therapists, health care aides, recreational specialists, facility operators and others who work with older adults in geriatric residential care facilities. Also, knowledge of social care strategies in these care settings can be transferable to other types of institutional care for older adults (e.g., hospital settings, correctional services, addiction care facilities, etc.).
Contemporary Canadian geriatric residential care facilities offer challenging physical, social, cultural, and political environments to our most vulnerable older adults at the end of their lives. Social care is one of the keys to changing these medical institutions to offer more holistic, dignified, and respectful care. After all, we are not only our bodies: physical existence without meeting social, cultural, and spiritual needs is not fulfilling or sufficient for any human being across lifespan. Old age should not be an exception. We hope this study will contribute to the public discourse on social care in the era of aging population in Canada and globally as well as to the growing body of research that prioritizes social care as pivotal to healthy aging.
Supplemental Material
sj-docx-1-jsw-10.1177_14680173251369661 - Supplemental material for It is Not Only About Staying Alive: A Living Systematic Review of Social Care Strategies for Older Adults in Residential Care Facilities During the COVID-19 Pandemic
Supplemental material, sj-docx-1-jsw-10.1177_14680173251369661 for It is Not Only About Staying Alive: A Living Systematic Review of Social Care Strategies for Older Adults in Residential Care Facilities During the COVID-19 Pandemic by Anna Azulai, Beverly Michel Baluyot, Alison Pitcher and Sejla Catovic in Journal of Social Work
Footnotes
Acknowledgements
We would like to thank Dr. Hongmei Tong from MacEwan University for the contribution during the conceptual and initial screening stages of the study. Also, we are grateful to Megan Kause and Elaine Tran, research assistants, for the initial screening of the articles at different circles of the data collection process. Finally, our gratitude goes to the Social Sciences and Humanities Research Council in Canada for funding the study (file number: 430-2021-00592).
Ethical Approval
This study did not involve human subjects. Ethical approval for this project was granted by the Research Ethics Board at MacEwan University, Edmonton, Canada (file reference number: 101931).
Authors’ Contributions
All authors participated in developing the systematic review and contributed meaningfully to the preparation of the manuscript. AP guided the search and screening phase of the study, wrote the manuscript background and results sections in collaboration with BB and SC. BB led data storing and management of the study, coded data in collaboration with AA and SC, developed methods section for the manuscript in collaboration with AA, and developed PRISMA chart. All authors reviewed coding for major themes. SC developed tables for the manuscript and contributed to editing in collaboration with AP. AA led the overall study and manuscript development, guided the data analysis phase, wrote discussion section of the manuscript, and conducted revisions of the manuscript with input by AP, BB, and SC.
Funding
The authors disclosed receipt of the financial support for this research from the Social Sciences and Humanities Research Council of Canada (reference number: 430-2021-00592).
Declaration of Conflicting Interests
The authors confirm that they have no conflict of interest in respect of the material submitted in this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
