Abstract
Providing evidence-based information at the point of care for time-poor nurses may lead to better clinical care and patient outcomes. Smartphone applications (apps) have the advantage of providing immediate access to information potentially increasing time spent with patients. This small-scale pre-post survey study explored the impact a smartphone app had on the distance nurses walked and their perceived clinical decision-making ability. A total of 20 nurses working in a rural hospital medical/surgical unit participated. The findings suggest that the use of the smartphone app did not decrease nurses’ walking distance. Nor did using the app enhances nurses’ perception of their clinical decision-making ability. However, there was a statistically significant increase in confidence in the app over time (F(1,16) = 5.416, p = 0.033, partial η2 = 0.253), suggesting that providing training opportunities including time to learn how to use smartphone applications has the potential to enhance nurses work.
Introduction
Nurses typically walk about 6.6–8.0 km in a 12-h shift. 1 While unit design or layout and patient assignment may impact distance walked, 2 concern has been raised that the amount of time nurses spend on indirect patient care activities which includes walking might negatively impact the amount of time spent on patient care. 3 Consequently, some researchers believe that less walking time would contribute to more patient care activities and better patient outcomes.4,5 Exploring ways to reduce the amount of time nurses walk so that they have more time for patient care activities has never been more urgent given the increased acuity of hospitalized patients.
Using mobile technologies that offer convenient, quick, and easy access to relevant, evidence-based information at the point of care may decrease the amount of time nurses use to walk to nursing stations where practice resources that guide clinical decisions are typically found. 6 These technologies may in fact provide “just in time” information needed for important practice issues. 7 Given the rapid and wide adoption of mobile technologies by healthcare professionals,8 –11 how these technologies impact nurses’ work make this study timely, practical, and deeply relevant.
Literature review
The impetus for examining nurses’ walking patterns and behavior seems to revolve around three major themes: (1) a graying, nursing workforce and associated occupational stressors in older nurses that can lead to potential joint pain and injuries;12,13 (2) the effect of hospital layout on walking patterns;1,2 and (3) nurse work efficiencies. 3 Some authors 14 have also suggested that increasing patient acuity requires adjustment in resource requirements and allocation. In particular, they suggest minimizing the distance between nurses and patients in an era of increasing patient acuity is essential for the provision of safe, quality patient care.
In a scoping review of the effectiveness of handheld computers in clinical practice, positive outcomes were reported in patient documentation, patient care, information seeking, and professional work patterns. 15 It would seem that handheld computers improved patient documentation by supporting more complete documentation that also contained fewer errors, provided easy access to clinical decision support systems which improved decision making for patient care, saved time and provided earlier access to new information, and enhanced work patterns and efficiency. Studies that have examined the impact of handheld devices on nursing practice have also found that nurses perceive handheld or mobile devices as useful tools in terms of information retrieval and improved access to relevant information, patient safety, quality of care, confidence in the work place, and time savings.7,16,17 Mobile devices also seem to enhance nurses’ use of research in nursing practice which has led to improved patient care and job satisfaction. 18 However, according to McBride, 19 while mobile technologies may appear to be advantageous in the provision of patient care, they may also cause distraction for nurses given the time needed to learn how to use the technology and implement it on busy, understaffed units.
Be that as it may, the use of information and communication technologies in healthcare settings has become widespread—some might even say ubiquitous. Consequently, some researchers have investigated the relationship between clinical role, clinical task, and selection of computer hardware devices in hospital units. Using a mixed-method approach with a total of 80 h of observation, Anderson et al. 20 found that nurses’ work requires highly mobile computer devices. These participants preferred generic computers on wheels over tablet personal computers because of their availability, mobility, and design. Since medication-related tasks require high levels of mobility, having a computer device like generic computers on wheels that allow medication and chart storage supports completion of this task with ease. Other researchers 5 have examined the impact a hands-free wireless voice communication device has on distance walked by nursing personnel. They found that in a typical 7.5-h shift, using the communication device could save an average of 20.5 percent of nurses’ working time. They concluded that the average distance traveled by nurses can be reduced using such a device.
While the value of mobile technologies appears significant for practice, rapid rates of change in the technology outpace rates of research production. Hence, there remains a significant need for research and evaluation of these devices.15,21 Studies exploring the impact of using mobile technologies that provide professional information (e.g. medications, diagnostics, pathologies, and patient teaching) on distance walked and nurses’ perceived clinical decision-making ability could not be located. Consequently, the intent of this small-scale study was to explore the impact a smartphone app had on the distance nurses walked and their perceived clinical decision-making ability.
Method
A pre-test post-test survey design was used. It was hypothesized that having access to mobile technologies would reduce the distance nurses walked during a typical shift. A second hypothesis was that using an information app at the point of care would enhance nurses’ perception of clinical decision-making ability. Ethical approval was received (protocol # Pro00054491). All data were managed using Tri-Council Policy Statement II guidelines. Study participants provided written consent at the start of the study and prior to data collection. Participants were assigned code numbers for tracking purposes.
Data were collected over a 2-month period. In phase one, the participants completed the Clinical Decision Making In Nursing Scale 22 questionnaire. Demographic data were also collected at that time. Upon completion of the questionnaire, each participant was given a foot pedometer and were instructed to wear the pedometer every shift they worked for the following 31 days. At the end of each shift, they were to record on a tracking sheet, the number of steps taken and distance walked. At the end of the first phase and prior to start of the second phase, the participants completed the Clinical Decision Making In Nursing Scale 22 questionnaire.
At the beginning of the second phase of the study, the PEPID Professional Nursing Suite app was downloaded unto each participants’ personal smartphone. Using the criterion of comprehensiveness and accessibility, this particular app offered the most comprehensive suite of resources the authors believed the participants might use. The suite includes clinical/medical information for over 2300 health conditions, nursing diagnoses, medication and intravenous compatibility, recently published research, laboratory and diagnostic information, and patient teaching information. Moreover, since the app is a native app, access to the Internet during use is not required. Prior to the start of data collection, the participants received instructions from a member of the research team on how to use the app and were given 2 weeks to become familiar with the app. They were then asked to use the app while at work and to continue to record the number of steps and the distance they walked during their shifts. A member of the research team was available in person and via telephone throughout the study to address any questions about the app and/or pedometer. At the end of the second phase (31 days), the participants completed the Clinical Decision Making In Nursing Scale 22 questionnaire.
Questionnaire
Proficiency in critical and creative thinking are essential cognitive qualities nurses must possess if they are to make knowledgeable, confident, and effective decisions in regard to the delivery of high-quality patient care. Developed in 1983, the Clinical Decision Making in Nursing Scale questionnaire assesses and evaluates clinical decision making in nursing. Tested for reliability and validity on 111 participants, the questionnaire is reported to have an overall Cronbach’s alpha of 0.83. 22 The instrument consists of 40 items with a 5-point Likert-type response scale. The scale assesses four categories of decision making: (1) search for alternatives or options, (2) canvassing of objectives and values, (3) evaluation and re-evaluation of consequences, and (4) search for information and unbiased assimilation of new information. Lending credence to its value as a reliable research instrument, this questionnaire has appeared in at least 90 published studies. 23
Participants
Regulated nurses involved in making decisions about patient care were eligible to participate in the study. This included registered nurses, licensed practical nurses, and unit managers. A total of 20 nurses participated in this study: 14 were registered nurses and 6 were licensed practical nurses. Five participants were between 20 and 25 years, five were between 26 and 40 years, and ten participants were over 40 years of age. In total, 17 participants worked part-time, 2 worked full-time, and 1 worked casual hours. The participants worked day/evening or day/night rotations on a medical/surgical unit with patients experiencing varying degrees of acuity. At the outset of the study, 16 (80%) participants rated their level of comfort using mobile technologies as comfortable to very comfortable. In all, 12 (60%) participants indicated that they regularly accessed professional materials from their mobile device.
Study setting
The setting for this study was carefully considered since there are variables that can potentially impact the findings of this type of research. For example, the architectural design of a nursing unit and the distance to or between patients and nursing desk needs to be factored into research in this area. As well, the distance to other areas of the hospital nurses access in order to coordinate patient care need to be critically considered. To address this concern, we concluded that using one group of nurses who work on one unit and are familiar with the layout of the nursing unit and hospital would help reduce the impact of these extraneous variables. We selected a nursing unit in a rural hospital as the ideal study setting since there was only one nursing unit and all staff would most likely be very familiar with the architectural design of the hospital.
Data analysis
A general linear model repeated-measures analysis of variance (ANOVA) statistical method was adopted in this study. Our aim was to find out if there were differences between pre-post intervention walking steps/distance in miles, number of steps walked in work shift (day, evening, and night), and to check if distance walked per shift in miles differed. Whenever there was evidence of statistical significance in the test of homogeneity of variance (Levene), we report the Robust Test of Equality of Means (Brown-Forsythe). Games-Howell (post hoc) test was used for the follow-up test.
Results
The first hypothesis that nurses would walk less when having access to the PEPID Professional Nurse Suite app was not supported by the data. There was no statistically significant difference in the number of walking steps and distance walked pre-app access and post-app access (Table 1).
Descriptive for pre- and post-test tracking collections (N = 20).
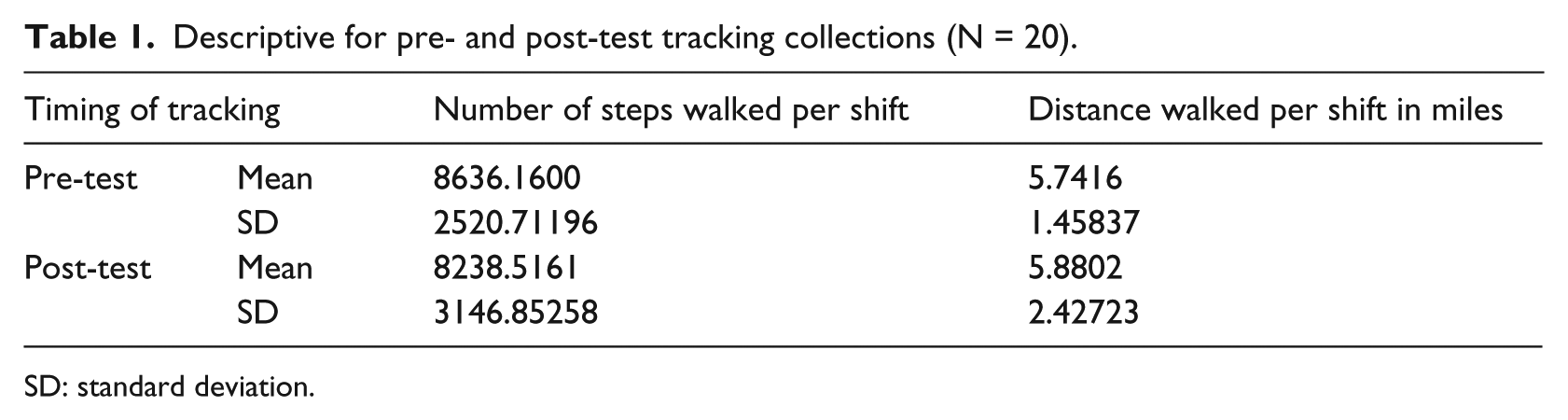
SD: standard deviation.
The second hypothesis that stated use of the app would enhance perception of clinical decision-making ability was also not supported by the data. There was, however, a significant positive correlation between hours per day of using mobile devices and level of comfort using mobile technologies (r = 0.461, p = 0.018). There was also a statistically significant increase in confidence in the app over time (F (1,16) = 5.416, p = 0.033, partial η2 = 0.253). This result represents a large effect size for the question “I solve a problem or make a decision without consulting anyone, using information available to me at the time.”
Discussion
The use of mobile technologies in healthcare settings is here to stay. Although there is an abundance of evidence regarding the benefits of using mobile technologies, nurses tend to prefer to discuss patient care with colleagues and use established protocols/policies and guidelines rather than access online evidence or published research.24,25 In the rural hospital setting, efficacious decision making relies heavily on nurses’ ability to engage patients in discussion about his or her needs as well as the ability to engage other nurses and team members. 26 Indeed, clinical knowledge is understood to be socially embedded. 27 It is possible that the differences in the findings of this study compared to other studies5,16,17 are in part due to contextual differences including the social context and architectural design of the unit. Moreover, the majority of the participants in this study worked part-time or casual hours. Working part-time or casual hours might have influenced the participants’ perceived need to communicate more frequently with their colleagues through canvassing treatment options, and checking patient progress and management. Further research is needed to explore the influence of working part-time and casual hours on walking distance, use of a mobile app, and perceived clinical decision-making ability.
To enhance knowledge transfer and make the most of the potential benefits of healthcare apps, it is important for nurses to feel confident in their ability to use the apps. Findings of this study suggest that over time and exposure to the app, nurses’ confidence in the app improved. Organizations considering the adoption of smartphone applications should consider providing an orientation to the app and its features, having on-site assistance to answer questions about the app and troubleshoot, and providing nurses with time to learn how to use the app. Such strategies would increase their confidence in their ability to use these technologies. Nurses also need to feel confident about the quality and suitability of whatever app they wish to use as part of their clinical practice. To that it end, they need to be aware of the variation in quality of information within healthcare apps and how to perform a risk assessment. Moreover, appropriate apps should be officially endorsed by employing organizations.25,28
Limitations and future research
While the findings contribute toward narrowing the gap between the perception and reality of mobile device usage in hospitals, mobile device studies usually have a small number of participants due to high costs for hardware and software. 29 Furthermore, to control for the potential effect of architectural design, recruitment involved regulated nurses working in one specific rural hospital. Rural hospitals have a smaller contingency of nurses compared to large urban hospitals. The small sample size limited our ability to identify statistically significant results, thereby reducing generalizability of the findings. Caution must be used when considering the findings of this study. Consequently, the effectiveness of using mobile technologies on walking distance and clinical decision making needs to be explored with a larger sample as well as across nursing units and organizations. To add further depth to what is known about healthcare professionals’ use of mobile technologies, in particular apps, studies from the perspectives of healthcare organizations and patients should also be conducted.
Conclusion
The unprecedented adoption of mobile technologies within healthcare settings has had and will continue to have a significant impact on nurses’ work. The findings of this study suggest that with time, nurses develop more confidence in using healthcare apps. As healthcare organizations look to adopt various healthcare apps, further research is needed to determine the effectiveness of using mobile technologies on walking distance, clinical decision-making ability, and patient outcomes.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
