Abstract
This article focuses on a conceptual framework that can be applied to the use of mobile technology in the waiting room with the goal of empowering women recently diagnosed with abnormal Pap test results. It further describes trends which indicate a need for improved and timely information dissemination. Genecology practice outpatients report a predominant feeling of worry on receipt of abnormal medical test results, along with a clearly expressed wish for additional information. This research suggests that there is room for improvement in existing processes through use of mobile technology with carefully vetted materials which indicate a doctor is interested in the patient’s well-being.
Introduction
Patient education is important in treatment outcomes. This education may be done formally at doctors’ offices by healthcare professionals or through alternative methods which include computer-based learning, video, and media.1–3 Unfortunately, most alternate methods can be classified as a one way communication. Good information and communication increase patients’ capability to contribute to decision-making processes, leading to higher levels of satisfaction and favorable treatment outcomes.4,5 While it is important to have a patient fully informed and engaged in the decision-making process, it is inevitable that patient comprehension of explanations often is lacking due to the complexity or for other reasons. Evidence suggests that patients often do not understand what is being said when information is given during a medical encounter due to educational gaps between clinicians and patients. 6
The most important attribute of patient-centered care is the active engagement of patients when fateful healthcare decisions must be made. 7 In other words, the point when an individual patient arrives at a crossroads of medical options and the diverging paths have different and important consequences with lasting implications. Examples include decisions about major surgery, medications that must be taken for the rest of one’s life, and screening and diagnostic tests that can trigger cascades of serious and stressful interventions.
For some decisions, one clearly superior path exists, and patient preferences play little or no role. Examples include when a fractured hip needs repair, acute appendicitis necessitates surgery, or bacterial meningitis requires antibiotics. For many medical decisions, however, more than one reasonable path forward exists (including the option of doing nothing, when appropriate). Different paths entail different combinations of possible therapeutic effects and side effects. Decisions about therapy for early-stage breast cancer or prostate cancer, lipid-lowering medication for the primary prevention of coronary heart disease, and genetic and cancer screening tests all are good examples. In such cases, patient involvement in decision-making adds substantial value.
Recently, there has been a shift in the process of receiving medical care. This shift, often referred to as health empowerment, relates to the role patients play when receiving medical care. Health empowerment is frequently defined as a combination of “knowledge, skills, and a heightened self-awareness regarding values and needs” to help patients reach their personal health goals (p. 140). 8 Empowerment within the health context has frequently been operationalized in terms of how much patients participate in the medical decision-making process. 8 Dupuits 9 claims that the Internet and other such information media have had significant influence on patients’ empowerment and their participation in the decision-making process. However, other research asks whether high amounts of information are always beneficial to patients. Broom 10 says that for some patients with prostate cancer, Internet health information has served as a source of empowerment, while for others, it has served as a source of confusion. 11 Patients who seek health information in addition to that provided by physicians challenge the physician–patient relationship, and this can lead physicians to further limit collaboration in the treatment decision-making process. 10
Therefore, further review of the effects of health information on patient empowerment and participation is warranted. This study offers a conceptual framework to examine the benefits of presenting information to women in waiting rooms prior to a genecology professional encounter to discuss initial results regarding positive Pap test indication.
Background
Empowerment
Gibson 12 defines empowerment as the process by which individuals or groups enhance their ability to meet their needs and gain a sense of control over their lives. Research indicates that empowerment can occur at various levels including the individual, organizational, and societal levels.12–14 At the individual level, empowerment is described as a family of variables that “includes participatory behavior, motivations to exert control, and feelings of efficacy and control.” 13 This form of empowerment includes both individual perceptions (psychological aspects) and behavior. In regard to health care, Webb et al. 15 refer to empowerment as the process in which patients and providers equally contribute to the health decision-making process. Webb et al. 15 measure empowerment by asking participants generic questions about their perceived degree of involvement in and satisfaction with their treatment decisions. Thus, Webb et al. 15 allude to the notion that empowerment is a reconceptualization of participatory decision-making. Thus, there appears to be overlap and confusion among the constructs that relate to empowerment. Roberts 16 clarifies that previous research has defined empowerment as the relationship between health and power, an informed and active patient, an equal physician–patient relationship, and a type of health education. According to Roberts, 16 the various conceptualizations suggest psychological aspects of empowerment and empowered behaviors are likely to be intertwined.
Health information, including information provided by a physician as well as information sought by a patient, may have varying effects on patients’ senses of empowerment. It appears as though the information provided by a physician may allow patients to feel more empowered and efficacious; however, such information may also confuse patients and ultimately hinder the decision-making process. A great deal of literature suggests that information is a useful tool in increasing a patient’s empowerment, while other literature suggests that extreme amounts of information lead patients to information overload and confusion.17,18
Information overload
According to Chen and Chang, 19 humans have limited information processing capacity. As amounts of information increase, humans tend to increase their processing efforts accordingly. When individuals are confronted with more information to process than they are able or willing to process, they may perceive themselves as experiencing information overload. Perceptions of overload are the result of the interaction between high amounts of information and limited processing capacity. 19 When processing limits are surpassed, overload occurs and an individual may be left confused and more likely to make poor decisions as a result. 17
Women’s health clinics
A good example to represent the influence of information overload in health sensitive and complex situations can be illustrated by cervical cancer diagnosis cases. Extensive information on this topic currently is available. The effectiveness of this information in reducing anxiety in women receiving abnormal Pap tests is not clear since so much information exists and because information available at home is not always accessible. 20
Cervical cancer is the second most common cancer in women, affecting nearly 530,000 females worldwide and resulting in 275,000 deaths each year, including 31,000 cases and 13,000 deaths in Europe. 21 Human papillomavirus (HPV) infection can lead to the development of pre-cancerous lesions and cervical cancer. 22 Routine screening and HPV vaccination programs have increased the visibility of cervical cancer in the wider community, and may contribute to increased concerns about developing this cancer, particularly in younger women. 23
Cervical cancer can be detected using a Pap test. A Pap test uses a sample of cells taken from a woman’s cervix or vagina. The test looks for changes in the collected cells that show cancer or conditions that may develop into cancer. The Pap test currently is the best tool to detect pre-cancerous conditions and hidden, small tumors that may lead to cervical cancer. If detected early, cervical cancer can be cured.
A Pap test is not comfortable and its negative perception can be increased by receiving news via phone that one’s test result is abnormal. Frequently, women are given little information about what the result means. This leaves them unsure about the next steps to take. In fact, studies report women commonly feel stressed and anxious after being informed of an abnormal Pap smear test result24–26 irrespective of the severity of the result. 27 These emotions often are long lasting. 28
Other research confirms that lack of accurate and understandable medical information about the causes, prevention, treatment, and consequences of an abnormal Pap smear result and cervical cancer leads to anxiety. 29 When a doctor reports that a Pap test is abnormal, this means the test has identified abnormal cells on her cervix. But, having an abnormal test result does not mean the woman has cancer. In fact, the chances are very small. However, the patient is requested to schedule a follow-up with a professional genecology clinic and during the intervening time period, anxiety and worry may build. In response, a woman may access information on the web.
When the patient arrives at the medical encounter, she will be experiencing anxiety about the future. In this situation, it is unlikely that she will be involved in any decision-making, and this can add to confusion surrounding the forthcoming medical encounter.
She may have learned there are several options of treatment and all are considered effective to various degrees, but her information may be incomplete. For instance, she may not know the best treatment will depend on the type and extent of her problem. Some doctors will prefer one treatment method over another, and again she may not have access to this information. In this regard, it is important that a patient understand why a doctor recommends one approach or treatment over another. Therefore, it is important to empower, enable, and support women with the ability to ask questions without fear or reservation. 30 This research seeks to examine, if women’s waiting times for gynecological consultations can be leveraged to inform them in a better way, thus empowering her to be an active participant in the medical encounter decision-making, therefore increasing her patient satisfaction.
Furthermore, we look at the waiting room time as an opportunity to trigger a woman’s education regarding such sensitive issues. We hypothesize that the use of mobile technology, which includes carefully controlled health-related information, can help a woman be better informed, empowered, and enable her to communicate better in the forthcoming medical encounter. She ultimately might perceive higher patient satisfaction related to communication with the doctor.
Being well informed is, indeed, critical for lowering anxiety over abnormal results. It may be the case that many women do not understand the meaning of an abnormal Pap result and wish for more information. An Australian study has shown that women wish to participate in decisions about their care but find it hard to ask questions. 31 Physicians should bear in mind that patients may not spontaneously request further information, despite (or perhaps because of) high levels of anxiety. 29 We therefore suggest the use of mobile technologies, such as tablets, in the waiting room to provide easy access to information that was carefully vetted and communicated by the doctor regarding treatment, procedures, and long-term effects, 32 and to help reduce anxiety and improve general situational knowledge. 33
Mobile use in the waiting room
The widespread adoption and use of mobile technologies is opening new and innovative ways to improve health and healthcare delivery.34,35 These applications are being assimilated quickly into health care. 36 The use of mobile applications prior to physician encounters regarding birth control information can help foster a better understanding of how a particular method works and the long-term implications of continued use. The mobile application used in the Sridhar et al. 36 study increased patient satisfaction with counseling and showed that mobile applications are best used in addition to physician consulting. A major limitation in the Sridhar et al. 36 study was the lack of a follow-up. The study did not report whether visit times changed when the application was used after the consultation. Due to time constraints that limit a physician’s ability to deliver detailed information during a medical encounter, applications for mobile technology can be designed to educate patients and simplify communication between patients and providers. 37 Therefore, there is the potential to examine mobile applications in the waiting room.
Little formal research has been conducted to evaluate time spent in waiting areas. The limited studies conducted have attempted to improve waiting area experiences for patients and their supporters regarding design of the space and reduction in waiting times. 38 This often is specific to a local office, and is focused on patient comfort issues such as temperature, seating, coffee, television programming, or wait times.39,40 Although many opportunities for redesigning waiting room space for comfort, safety, and even entertainment exist, there also are opportunities to redesign the space to encourage learning. Traditional educational material in waiting areas is often ineffective and unacknowledged. Often, patients are provided with pamphlets and posters to learn about diseases and disorders. General practitioners agreed that patient curiosity regarding health-related information is growing and that the physician should consider the waiting room as a place for patient education. 41
A previous study assessed the value of various techniques designed to reduce patient anxiety in waiting room. 42 This study and others suggest provision of waiting room information may reduce anxiety when it concerns a care procedure the patient will subsequently experience. 43 Waiting room time can become useful with formal patient education. 44 This is particularly true in light of what is known about creating innovative, empowerment-based, educational materials. 45
Conceptual framework
Our research used a general model reflecting factors that might influence a better way to improve communication during a medical encounter (Figure 1). We specifically focused on empowerment related to waiting room times and later as an outcome obtained through use of mobile platforms to enable learning through access to physician-controlled education materials.
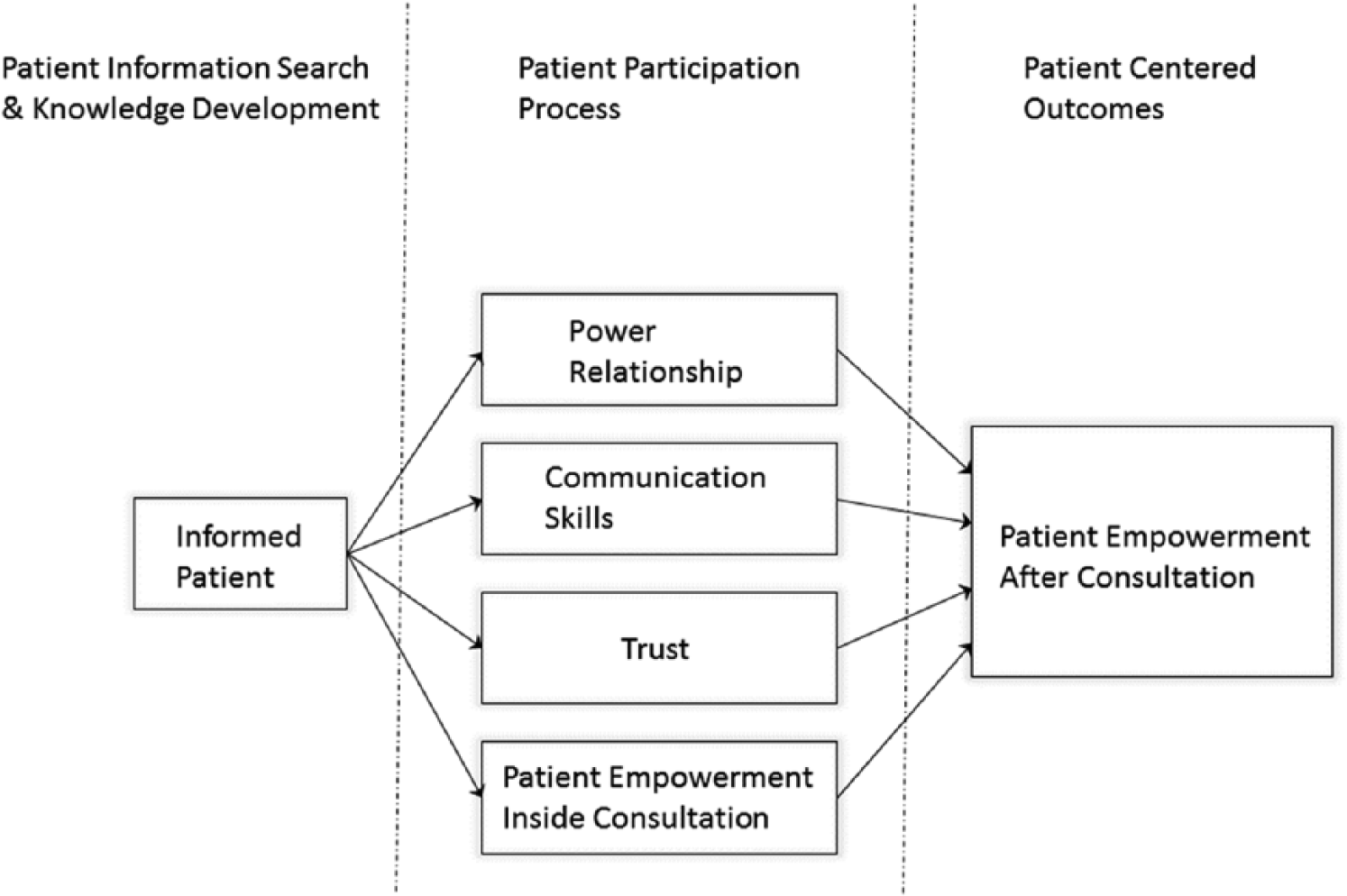
Conceptual framework for mobile use in waiting room.
Patient–physician encounter
Patient–physician interaction is an important aspect of the patient’s level of involvement, 46 and is focused on empowering patients. 47 Patient–physician interaction usually seeks to help patients become more active during consultations, and is linked to positive health outcomes such as enhancing self-efficacy, providing better ability to adopt the correct treatment plan, and achieving patient goals. In order for the encounter to empower the patients, a collaborative relation between patient and physician is necessary, as well as development of a patient’s ability to engage in self-care, and cooperation. 47
According to Feldman-Stewart et al., 48 patient–physician interaction is based on four components: (1) patients’ and physicians’ communication goals; (2) needs, skills, values, and emotions that affect communication; (3) how messages are verbally and nonverbally conveyed and received; and (4) the communication environment, including external factors such as prior education and experience. All four factors influence the outcomes gained from the encounter.
To return to the sensitive Pap test situation described earlier, a woman and her physician might have different goals during the medical encounter. For instance, the physician may focus on relevant treatment while the woman seeks to allay confusion, anxiety, and fears. A woman may enter the consultation with very low knowledge, with needs based more on support aspects and less on an interest to be involved in the decision-making process. The way a physician decides to convey the treatment options might influence overall understanding. Furthermore, this might vary from doctor to doctor—for instance, one may decide to explain, while another makes the explanation shorter in order not to inject more stress into the situation. Education and prior experience of the patient regarding the medical situation may also factor into the interaction.
In considering all four characteristics of interaction in the medical encounter, we suggest four constructs that lead to enhancement of empowerment based on self-determination theory (SDT) which proposes how specific needs of individuals drive their self-intended (self-determined) behaviors. 49
SDT states that human beings have basic psychological needs, such as the need for autonomy, which is the desire to experience satisfaction with exercising and extending one’s capabilities and mastering challenging tasks. Individuals strive to satisfy these needs to increase their well-being, and thus engage in certain behaviors they perceive as self-determined 50 such as an information search or participation in decision-making. These self-determined behaviors trigger subsequent actions, during which individuals try to keep consistent with their previous actions and underlying needs. 51 This includes activities such as complying with recommendations.
More specifically, information search is the degree to which a patient systematically and actively collects disease and treatment-related information from various information sources (e.g. personal meetings in self-help groups, books, Internet, brochures). 52 Knowledge is developed as a by-product of an information search. Knowledge development is the degree to which patients actively organize and understand the information acquired about their disease, with the goal of achieving disease-related expertise to keep up with the physician. 53 Decision participation is the degree to which patients actively work with the physician to develop a treatment strategy and make treatment decisions.54,55
The information search following knowledge development is represented by the concept of the informed patient. Our conceptual research focuses on the intensive efforts of the information search and its contribution to developing an informed patient. Active participation in SDT theory is discussed during our examination of the empowerment process, which emerges as a patient becomes informed. Being informed provides leverage that increases power of the patient in encounters and relationship development with her physician. Additionally, it increases trust and enhances patient communication skills. The results of these processes empower patients more strongly, and yield greater satisfaction.
The informed patient
In order for patients to express their preferences and feel more confident in making decisions about their health care, they must become informed by receiving appropriate information regarding their condition, including potential outcomes and treatments. This information helps patients why a treatment option might be chosen and become more likely to comply with recommended courses of action. Ultimately, the informed patient will accept the prognosis, become an active participant in managing their disease, and feel more satisfied with their treatment.56,57
However, there is heterogeneity in the knowledge and information that patients need. Not all patients require the same information and this places considerable demands on healthcare professionals because they must personalize the information to best suit a particular individual. 57
Research has shown that informed patients make better use of a health professional’s time (both quality and quantity), and show improvements in knowledge, self-efficacy, and in self-management behaviors. 58 On the down side, physicians only have limited time for counseling, and often this time is insufficient to develop an informed patient and explain the condition and treatment choices available. Thus, patients may seek information elsewhere. 57
Power relationship
In order to develop an informed patient, the distribution of power between patient and physician must change. It is important that a patient feels they have more control over their health treatment and are an active part of the decision-making process.10,16,59
Using online information challenges previous hierarchical models insofar as it encourages patients to stop being simply passive recipients of information. Instead the Internet’s search capability empowers them to actively seek relevant information.10,59–62
Henderson, 56 who studied the power imbalance between nurses and patients, found most nurses did not provide patients with information beyond what was necessary. Nurses tended to give information about a procedure, but did not provide the patient with different treatment options and expected outcomes of each. More specifically, nurses often wished to make the decision for patients, instead of assisting them to make their own decisions. We know from empowerment studies, it is important that women feel a sense of control over their situation, and must be involved in decision-making elements during a medical encounter related to a proffered treatment. In these sensitive cases, using online information, which is not controlled, may cause harm to the patient by increasing her anxiety and worry, and by preventing her from taking an active part in the medical encounter. Therefore, we believe having access to controlled information provided through the medium of mobile technology in the waiting room may have the potential to change the power relationship.
Communication skills
When patients meet a physician as part of their clinical care, their wish is to achieve the best medical outcome and get the best possible care. For that to happen, good communication is necessary between the physician and patient. 63 Engel et al. 64 found that patients regard communication with their physician as a key factor in their satisfaction. 65 Good physician–patient communication helps patients work toward their goals. 48 Good communication should be based on information exchange that leads to making treatment-related decisions together, while keeping core conditions such as honesty, empathy, and respect intact. All of these are crucial to the efficacy of the treatment and strongly influence patients’ well-being and satisfaction with the healthcare experience.66–68
In order to establish good communication, the patient must participate and cooperate during the entire treatment process, while the physician enables her to participate effectively and without worry.66–71 The information exchange between physician and patient consists of alternating between information provision and seeking. The physician needs information in order to establish the right diagnosis and treatment plan for the patient. At the same time, the patient, who desires to be understood and to understand, needs to provide relevant information including condition symptoms and concerns to the physician. The patient expects to receive all needed information from the physician.66,67,71 After the physician determines the diagnosis and treatment plan, he or she needs to efficiently impart that information to the patient in a way that enables knowledge acquisition. The informed patient will make decisions together with the physician regarding the next treatment steps.57,66–70
In order to occur in a genecology clinic, especially regarding sensitive personal issues, there is a crucial need for earlier, controlled preparation, during which waiting room time can play a role.38,72 The physician’s levels of providing/seeking information and communication skills are directly related to patient satisfaction. Lack of communication skills on either side may cause problems in diagnosis and affect patient involvement in the counseling sessions.66,70,73 Studies have shown that physicians tend to interrupt patients 50 percent of the time and 45 percent of patient concerns are not disclosed. Half of the time, physicians and patients do not agree on the problem, and patients are dissatisfied with information provided by the physician. Thus, they may try to look for information elsewhere. 68 This may include seeking physician-vetted information provided in the clinic while patients are waiting. Ultimately, this information can change the relationship and enhance active patient participation, as well as their satisfaction with the medical encounter. 38
Research has shown good communication can influence how much the patient understands provided medical information, their adherence to recommended treatment, and other health outcomes in addition to enhanced satisfaction and empowerment.16,66,67,69,70
Trust
Physician communication skills have an effect on a patient’s level of trust. When the physician communicates effectively and keeps the patient informed with all desired information, he or she helps the patient develop a higher level of physician trust. 47 A key component of establishing trust relates to development of a physician relationship that meets patient expectations. The patient expects a physician to be supportive and to actively engage them in healthcare decision-making. 47 Patients given information about their disease prior to counseling were more confident and this encouraged them to ask more questions. They also talked more during counseling and were better able to elicit relevant information from their physicians. 10
Patient empowerment
In a general sense, empowerment may be defined as a “process by which people gain mastery over their lives.” 74 Studies of empowerment in different disciplines are based on the proposition that to improve the quality of lives both in the workplace and at home, people should be able and motivated to bring about changes. This applies to personal behavior, social situations, and within organizations that influence someone’s life. As such, empowerment is a relational construct (e.g. in the doctor–patient consultation) associated with the concepts of power, equity, and situational control. This implies a capacity to solve problems and get a fair share of resources.75,76 This concept further refers to both the state of being empowered and the process of becoming so. Empowerment is prominent in the management literature, where it has two meanings, both of which are influential in conceptualizing patient empowerment. 77 One meaning often is denoted as “psychological empowerment” and refers to employees’ subjective feeling of empowerment—specifically, feelings of perceived competence to perform tasks well, feeling influential in a work role, feeling their work is important, and feeling free to choose how to execute tasks.78–80 A second meaning, often called “role empowerment” or “situational empowerment,” 81 refers to objective practice involving delegation of responsibility to employees, in order to give them decision-making authority.
Empowerment discussed in relation to health behavior generally refers to patients.74,82,83 Patient empowerment is conceived as the patient’s participation as an autonomous actor taking increased responsibility for a more active role in decision-making regarding his or her health. 84 The empowered patient emerges as a person who does not passively receive information before trying to comprehend and invariably accept the outcomes. Instead, she is someone who extracts meaning relevant to herself from proffered information and advice, then chooses and enacts behaviors she concludes as appropriate to the present health situation.85–87 Empirical research on patient empowerment antecedents and consequences is limited. 80
Patient empowerment, referring to the set of self-determined behaviors based on patients’ individual needs for developing autonomy and competence with their disease, increasingly has become a key component of a patient-centered approach to health care (i.e. information search, knowledge development, and decision participation). Patient empowerment assumes a prominent place in visions of optimal health following the Ottawa Charter of 1986, which states that health promotion is the process of enabling people to increase control over, and to improve their health. This vision takes on a relational (e.g. doctor–patient) dimension, emphasizing the need for more egalitarian structures and an equitable distribution of power between practitioners and patients.88,89
The sensitive situation of a women dealing with an abnormal Pap result that brings her to a genecology clinic can be refocused within this discussion. The need to develop autonomy associated with a person’s self-determination, and the procedural empowerment process of giving and taking power. This is consistent with our working empowerment definition and tends to minimize uncontrollability, which is inherent in living with severe health conditions. In such contexts, the autonomy of a patient may be alternatively regarded as feeling secure in caring relationships, and having “ownership” for one’s decisions as a patient. This situation can trigger one’s participation in shared decision-making and ultimately contribute to empowerment.
Moreover, patient empowerment needs to be seen as a dynamic and creative process shaped by the patient’s own activity in searching information presented on mobile technology during waiting room time. Using mobile technology to present controlled information to the patient can contribute to a sense of choice and control, and supports the need to feel secure and connected, and supports the need to develop a sense of meaning and coherence. 35 Patient needs for competence and control generally are addressed in self-management support interventions where mobile technology is used while waiting for the consultation. This promotes cognitive and enhanced communication during the medical encounter, and results in higher active participation due to greater patient empowerment.
Preserving and enhancing patient empowerment
Within a healthcare organization, empowerment implies providing necessary tools to resolve most problems or questions faced by customers on the spot.8,10,56,90,91 In most instances, these customers are patients. Empowerment is not a static trait, but rather a dynamic process that changes over time and over different contexts. When a person becomes empowered in a specific moment in a particular environment, this does not make her empowered in other environments and other contexts.92,93 People can be differentiated in various ways regarding required perceptions as well as skills or actions needed for increasing their empowerment. Different people in the same situation will need to learn different skills in order to become empowered. Likewise, different situations require different skills. While some people have these skills, others may not, and they will have to learn these skills in order to become empowered. 94
The importance of continuing to preserve and enhance patient empowerment suggests that healthcare decision-makers should consider providing controlled access to information while women wait in the genecology clinic. Furthermore, access to carefully vetted information after the consultation would provide additional benefits leading to deeper learning and understanding as the patient becomes more empowered. This process can also be leveraged by opening a discussion between a patient and her doctor regarding specific aspects of a disease and treatment options that introduce stress and uncertainties. Mobile technology can be used as a tool that the women can use in support of such a sensitive situation. 95
Another example is participation in an online support group. Patients felt it helped them become more informed as well as to feel more in control, confident, and prepared for their encounter with a physician. An improved physician relationship resulted. 96 Although most of the participants in the Van Uden-Kraan et al. 96 study had positive feelings about online support groups, the possibility of a disempowering process also was mentioned. Some participants were concerned and unsure about the quality of the information provided in these groups, felt that certain questions and topics were constantly repeated, and sometimes had to deal with either information overload or lack of needed information. 96
Outcomes
The concept of empowerment remains ambiguous. Researchers often assert that empowerment is both a means and an end result.12–14,97 Gibson 12 adds that empowerment can also be viewed as the result of participatory decision-making, negotiation, collaboration, and/or education. When an employee is empowered, his decision-making authority increases, as well as his responsibility, and he becomes more adaptive and receptive to his environment, and could continue feeling empowered through his work.16,98,99 An empowered employee feels he has more impact, better self-determination, competence, and meaningfulness. 98 When patients are empowered, they become more experienced and independent in decision-making. 56 Ultimately, this leads to better health care with a team-like partnership between doctor and patient.
Summary
When patients go to a physician, they tend to have little power over their treatment plan. One way to help them gain power is by actively empowering them. People can become empowered in a variety of ways: by being better informed; 100 by having more power and authority in decision-making processes;98,100 by having a mentor; through participating in support groups; and by achieving one’s own goals. 93 However, not everyone can become empowered by the same things. Therefore, using the mobile technology in the waiting room can provide an excellent opportunity to enhance a women’s empowerment before they enter physician consultation. This approach to sharing information enables them to become more active in decision-making during the consultation. Additionally, this information will enable the patient to feel supported and, with the continued use of mobile technology to provide controlled access to relevant information, open a communication channel with the physician. Ultimately, this helps resolve anxiety and uncertainty in complex situations. The idea of providing empowering information supports efforts to be more patient-centered. 35
Limitations
This study provides conceptual information drawn from healthcare, business, and information systems literature. It is not an empirical study and is only meant to provide guidelines for implementing mobile technology–based information in patient waiting rooms. Further empirical research should be conducted to determine if the cited studies provide the benefits described in this article. Likewise, the recommendations provided in this study might be impacted by the emotional state of patients, their prior experience with information systems, and security-related concerns 101 regarding browser history or collection of personal information. Another limitation relates to the population studied. Although this article focuses on women that receive abnormal Pap smear test results, we believe our model of empowerment can be generalized to men and women experiencing other sensitive health issues. However, our emphasis on women is important, particularly in this sensitive situation. In spite of these limitations, we believe this research offers value to healthcare providers, particularly since mobile devices are becoming ubiquitous.
Future research
More research needs to be conducted to mitigate disparities related to heterogeneity in knowledge and the information patients possess and need. Not all patients require the same information, which places considerable demands on healthcare professionals. They must work to individualize information in a way that each patient will receive what is required to enhance their empowerment. 57 We believe mobile technology can be used to provide a customer-based information model customized to each patient based on her needs.
Controlled access to mobile platform–based information prior to patient–physician interaction needs more attention. Research has shown that informed patients make more effective and efficient use of a health professional’s time, show improvements in knowledge acquisition, and are more likely to be successful in self-management behaviors. 58 A physician has limited time and often this time is insufficient for helping a patient become informed during a counseling session. Therefore, patients may seek information elsewhere. 57 The use of carefully vetted, specific information provided on mobile technology is important because the Internet is filled with contradictory, confusing, and even incorrect information. Furthermore, information found online often is perceived to contain more reliable information than information found offline and enables a convenient way for accessing a massive volume of information.10,63,102,103 Printed/written material, however, is considered time-consuming and often requires a higher reading level than possessed by most people, and cannot be updated fast enough to reflect the current best treatment options available.10,63,103
Conclusion
Access to carefully controlled information following an urgent request to meet a professional gynecologist can shape the way a doctor provides treatment. This is particularly true when communication is enhanced and a patient feels empowered. The net result is for women to become more active and cooperative in the decision-making process. This patient-centered focus contributes to higher satisfaction of a patient healthcare experience. In this situation, women express their preferences and feel more confident to participate in decisions about their health. Patients become more cooperative and satisfied with their treatment plan, and manage and accept their disease better.56,57
Coulter et al. 104 and Lesnovska et al. 57 found that in order for information to help patients make more informed decisions and enhance fluency, 105 it must contain scientifically reliable material about the course of the disease, common symptoms, objective drug-related facts, as well as disease causes and consequences. The information also must contain ways to prevent and control the disease, the full range of treatment possibilities, and an honest assessment of whether recommended treatments are effective.57,100,103,104
In conclusion, it is important for health providers to better inform patients and determine what information is needed for their empowerment. Our research suggests carefully deployed mobile technology in a waiting room can mitigate fear and uncertainty. Furthermore, implementing patient empowerment research enabled us to reduce patient stress and enhance patient satisfaction with their health care. These findings highlight the need for more accurate, updated, and easily understood information specifically tailored for use in a clinical setting related to patient visits. This information should be developed in cooperation with healthcare providers, and should be available on mobile devices provided by clinics to help patients become more empowered, thereby more actively involved in their health care.63,98,103
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
