Abstract
Lack of time or economic difficulties prevent chronic obstructive pulmonary disease patients from communicating regularly with their physicians, thus inducing exacerbation of their chronic condition and possible hospitalization. Enhancing Chronic patients’ Health Online proposes a new, sustainable and innovative business model that provides at low cost and at significant savings to the national health system, a preventive health service for chronic obstructive pulmonary disease patients, by combining human medical expertise with state-of-the-art online service delivery based on cloud computing, service-oriented architecture, data analytics, and mobile applications. In this article, we implement the frontend applications of the Enhancing Chronic patients’ Health Online system and describe their functionality and the interfaces available to the users.
Keywords
Introduction
Chronic obstructive pulmonary disease (COPD) is a preventable and treatable respiratory disease that causes limitations in lung airflow. The most common symptoms of patients suffering from COPD are frequent respiratory infections, a chronic cough, excessive sputum production, shortness of breath, and progressively worsening dyspnea. 1
According to the World Health Organization, 450 million people suffer from COPD on the planet. It is estimated that COPD accounts for >3 million deaths per year, while globally is responsible for >29 million years of life in conditions of disability. COPD will be the fourth leading cause of death worldwide by the end of 2030. 2
Epidemiological studies conducted in the United States, Denmark, Norway, Italy, Spain, Japan, and Greece reported an overall COPD prevalence of 4–10 percent in the population.3–9 In Greece, COPD’s prevalence is also high. Adult smokers from 9 to 100 suffer from the disease (8.4%), that is, 600,000 Greeks, while 56 percent of them, that is, 300,000, are not aware that they suffer from the disease. Even half of the patients continue to smoke ignoring the risks of the disease. Men suffer 2.5 times more than women (11.6% vs 4.8%). 9
Usually, COPD is recognized late, either during an acute exacerbation of the disease or because the symptoms have increased too much obliging the patient to go to the doctor. The disease lasts several decades, while progressively impairs the quality of life of patients and immobilize them at home in continuous supply of oxygen due to respiratory failure. In the final stages, the patient often needs hospitalization, even in the intensive care unit greatly increasing the health costs. Although COPD is a disease of the lungs, this can cause significant systemic effects in a percentage of patients (affects other vital organs such as the heart and muscles). It is also associated with many comorbidities (such as heart failure, metabolic disorders, sleep apnea syndrome, and depression) posing patients’ management particularly difficult.
COPD treatments include smoking cessation, vaccinations, rehabilitation, bronchodilators, steroids, and long-term oxygen therapy. 10 The total cost of the medicines, emergency visits, or hospitalizations is enormous. Various studies have estimated the cost associated with the treatment of COPD patients: £0.8 billion in the United Kingdom in 2003, 11 US$18 billion in the United States in 2005, 12 and US$2.1 trillion worldwide in 2010. 13 In a prospective 1-year follow-up study conducted in 268 general practices in Spain, 14 the hospitalization costs for the treatment of acute COPD exacerbations represented about 45 percent of the direct costs, the medication costs represented about 40 percent of the direct costs, and the costs for the in-clinic visits and the diagnostic procedures represented about 15 percent of the direct costs.
Lack of time or economic difficulties prevent patients from communicating regularly with their physicians, thus inducing exacerbation of their chronic condition and possible hospitalization. Therefore, the prevention of exacerbations of COPD patients in order to improve quality of life for chronic patients and reduce costs is the primary concern of the medical community.
In this article, we implement the frontend applications of the Enhancing Chronic patients’ Health Online (ECHO) system. 15 The ECHO system uses a combination of cloud and service-oriented computing, online services, data analysis, and eHealth applications to connect COPD patients to their physicians. The ECHO system is expected to monitor patients, verify the diagnosis with online alerts in order to avoid medical emergencies and unnecessary hospitalizations at low cost and at significant savings to the national health system. Part of this work was carried out in project ECHO. 16
State of the art
Several studies investigate the use of eHealth services in order to improve patients’ quality of life and reduce COPD exacerbations. A literature review was conducted to examine various eHealth practices such as telemetry or telephone calls or home visits by nurse specialists and their impact on the management of chronic diseases. 17 Most studies in the review have been relatively short term (<6 months); thus, no evidence for the value of telehealthcare is verified. A meta-analysis published by Cochrane Library in 2011 included 10 randomized controlled trials, which investigated the hospitalizations, the exacerbations, the quality of life measures, the hospital visits, and the mortality in COPD patients using telehealthcare. 18 According to the review, telehealthcare increased significantly the quality of life in two trials with wide confidence interval (CI; mean difference: −6.57, 95% CI: −13.62 to 0.48) and reduced the number of the patients who visited a hospital (odds ratio: 0.27, 95% CI: 0.11–0.66) and the number of admissions per year in six trials (odds ratio: 0.46, 95% CI: 0.33–0.65). The difference in mortality rates was not clinically significant.
A systematic literature review demonstrated that hospital at home schemes resulted in substantial cost savings with equal effectiveness and patient safety compared with inpatient care for acute exacerbations of COPD. 19
A currently published systematic review and meta-analysis found a significant effect of telehealthcare (telephone calls, web, or mobile services) on physical activity level and no effect on physical capacity and dyspnea. 20
Studies have used mobile application technologies to monitor patients and facilitate health in a cost-effective way for both patients and physicians. But no study has used the technologies and the architecture similar to our approach. The study by Sanchez-Morillo et al. 21 evaluated an electronic questionnaire for the detection of COPD exacerbations with a 6-month follow-up of 16 patients, using a k-means clustering algorithm. The authors found the questionnaire and the above-mentioned methodology helpful for the detection of COPD exacerbations.
A mobile-assisted home care model uses a mobile application that enables patients report their COPD symptoms. 22 A Web portal is developed for clinicians to manage and analyze patients’ data and send feedback when necessary. A method for computer-aided assistance including event detection, alerting, monitoring, and treatment advice at a distance from the hospital is developed. COPD symptoms are collected and interpreted by a probabilistic model to access automatically the risk of worsening of symptoms due to an exacerbation. 23
A basic difference in the architecture of the ECHO system and the above-mentioned studies is that our system enables the communication of patients and physicians through predefined messages based on mobile applications for both the patients and the physicians. Thus, physicians can use a push notification service for immediate alerting of emergent situations. Another capability of the ECHO system is that the patients’ mobile application gathers data automatically from mobile devices (e.g. global positioning system (GPS) location) which are used in data analysis. The backend of the ECHO system supports data processing by means of cloud computing technologies that allow fast analysis of complex or large sets of patient data in order to help physicians dynamically adjust treatment plans in a cost-effective way.
Medical problem
It is very common for chronic disease patients to not have regular and frequent communication with their physicians, as they should. Some of the reasons that lead to it are lack of time, economic difficulties, or negligence. Unfortunately, this situation may lead to exacerbation of their chronic condition and to medical emergencies. The ECHO system enables closer connectivity of humans and systems, through the use of the latest technologies of smartphones, cloud computing, and intelligent data mining, in order to ensure uninterrupted care and chronic ailment crisis avoidance. Specifically, the goals achieved by the ECHO system are the following:
Collect and manage data about the health status, medical history, current treatment, and action plan in case of worsening of symptoms, thus improving the monitoring of patients.
Reduce or eliminate symptoms and improve health status, enabling the management and treatment of COPD exacerbations.
The methodology applied for COPD is described as follows: The patient provides (on a daily basis) the following mobile data to the database supported by the backend of the ECHO system:
Measurements of predefined vital signs (biomarkers) Oxygen saturation Heart rate Temperature Peak expiratory flow rate (PEFR) Walking distance
Answers the following questions: Did your shortness of breath increased? Did your cough increased? Did your sputum changed? Did you have chest pain or discomfort? Did you change your medications?
These data are transmitted to the system and are made available to the physician who creates and regularly (e.g. at regular follow-ups or during unexpected events such as exacerbations and emergency visits to the doctor or hospital) updates a medical record of the patient. The condition of the patient is evaluated, and recommendations or treatments are sent by the physician. The detailed actions performed by the users of the system are described below.
From a health-care provider’s point of view:
The health-care provider creates and then regularly updates a detailed medical record of the patient as part of the diagnosis in compliance with appropriate health-care regulations and standards (e.g. HL7). 24 This would include the demographics, symptom and sign comorbidities, exacerbations or relapses and the appropriate tests (pulmonary function test, O2 Sat, blood gases, etc.), and quality-of-life questionnaires such as Clinical COPD Questionnaire (CCQ) 25 or others.
Based on the above, the system will verify the diagnosis using predetermined criteria (as described above).
In addition, based on the medical record and with the appropriate severity scales, the system will evaluate severity of the patients.
Furthermore, the system would evaluate whether the patient is treated with the appropriate medications in accordance with the international guidelines 26 and advice the health-care provider social interaction feedback loop.
The above data of the medical record and in particular those of the severity will be reviewed frequently at regular follow-ups or during unexpected events such as exacerbations and emergency visits to the doctor or hospital. For the regular scheduled visits, reminders will be developed to increase compliance to the follow-up. These data are also fed into the model building feedback loop which, at longer time intervals, reevaluates diagnosis and severity algorithms and risk models.
Alarms and warning flags are part of the early warning feedback loop. From a patient’s point of view:
Every day, the patients have to answer five simple questions concerning their disease, and five biomarkers (as given above) will be collected by the smartphone all predetermined and part by the patient–client interface.
These data are transmitted to the system and automatically and continuously compared with the severity indexes of the file of the patient.
The early warning and severity feedback loop evaluates daily the condition of the patient and can identify mild-moderate or severe exacerbations of the disease.
Following this analysis, early warning flags are with simple instruction to the patients such as “Increase your medication,” “Call your Doctor,” and “Go to the Hospital.” The levels of warning and the advices (flags) will be developed for each disease severity level and in accordance with the current guidelines.
Overall architecture
The ECHO system 15 consists of a frontend and a backend as shown in Figure 1.
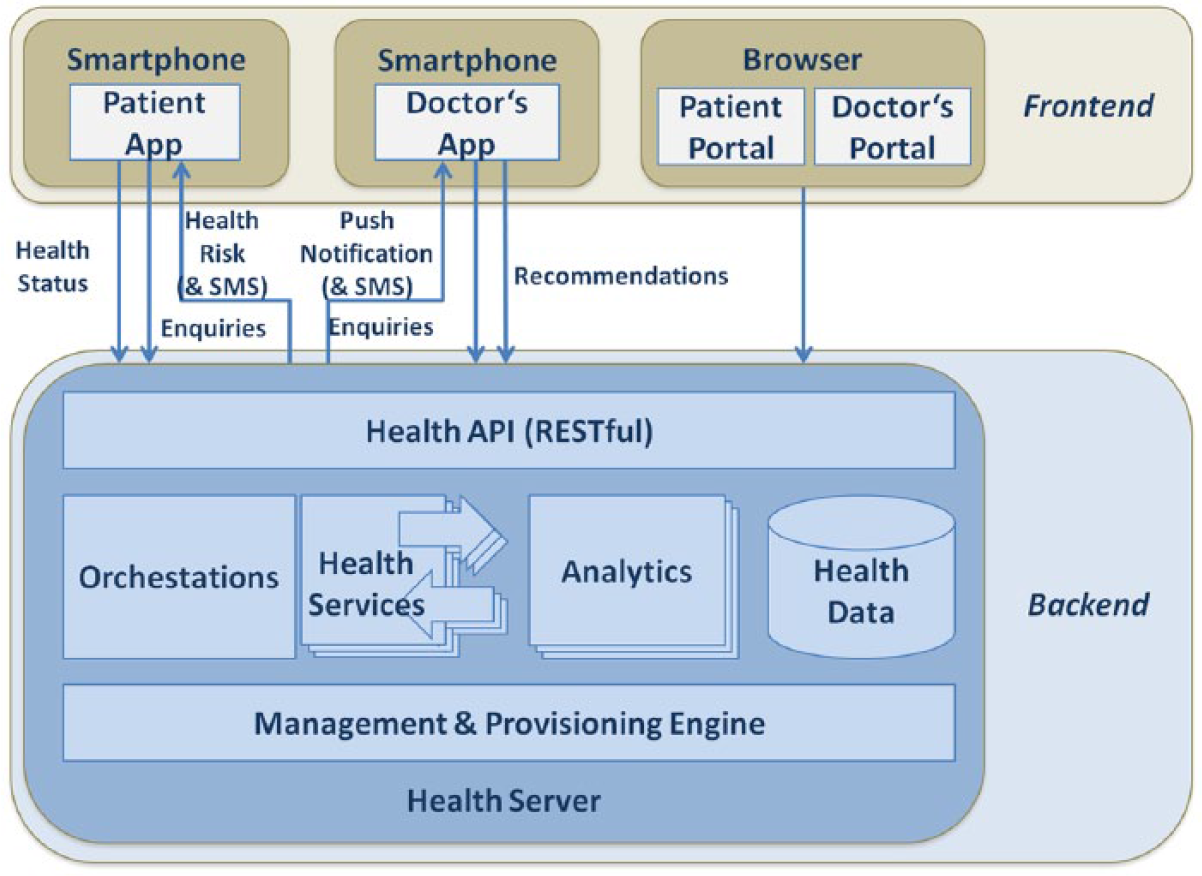
ECHO overall architecture.
The frontend is either delivered as application on iOS and Android smartphones or as a web application made available via browsers. The implementation of the backend was developed by University of Stuttgart, and the implementation of the frontend in web browsers and mobile applications was developed by OpenIT. The backend was integrated through JSON APIs to the frontends, which consisted of Android mobile application, iOS mobile application, and PHP-based web user interface (UI).
There are two types of user roles either on mobile devices or in browsers: the frontend for patients and the frontend for doctors. The application for patients allows patients to provide information about their actual health status and to be advised about actions to be taken based on their health record, all stored in the cloud infrastructure. The application for doctors allows physicians to pass recommendations to patients based on their actual health status and their health records stored in the cloud infrastructure. The application will receive notifications about urgent health situations of a patient that require immediate reactions.
The backend consists of the “Health Server” and is delivered as a cloud service, packaged in a portable manner based on the Topology and Orchestration Specification for Cloud Applications (TOSCA) standard. 27 “Health Data” stores and manages two different sources of data: patients’ health data entered from smartphones on a daily basis and physicians’ consultations (patient data, examination results, and prescriptions). Both health risks and situations requiring immediate reactions are determined by corresponding analytics functions maintained by the component “Analytics” in the backend. “Health Services” manage patients’ data and are composed into higher level services with advanced functionality by means of “Orchestrations” offered by the Health Server. The Health Server functionality with all its services is made available via a unified “Health API” following the representational state transfer (REST) architectural style, 28 ensuring the seamless integration between the backend and the frontend. All the components of the Health Server are managed by the “Management and Provisioning Engine.”
The frontend user application is described in detail in the next section. The data management and the health server implementation are described by Steimle et al. 29
Frontend implementation
We implement the application “ChronicOnline” that serves as the entry point of information by the patients, the frontend for the health data database of the backend, and a notification center serving the doctors. The application is available on the Google play store. 30 The functionality of the application for both roles, the patient and the doctor, is described in detail below.
User requirements
The ChronicOnline application reached by the role “patient” provides the following functionality:
Patient’s authentication using existing standard secure and authentication protocols of identification management (e.g. OAuth 2.0).
Linkage of the patient’s smartphone application to the health record keeping, cloud-based database.
A stream of data about the patient’s chronic disease condition (e.g. COPD), their location, and data entered manually by humans.
Push notification for the patients depending on their chronic disease situation.
The ChronicOnline application reached by the role “doctor” provides the following functionality:
Physician’s authentication using existing standard secure and authentication protocols of identification management (e.g. OAuth 2.0).
Push notifications about health status updates of their patients.
Access to all health data related to their patients.
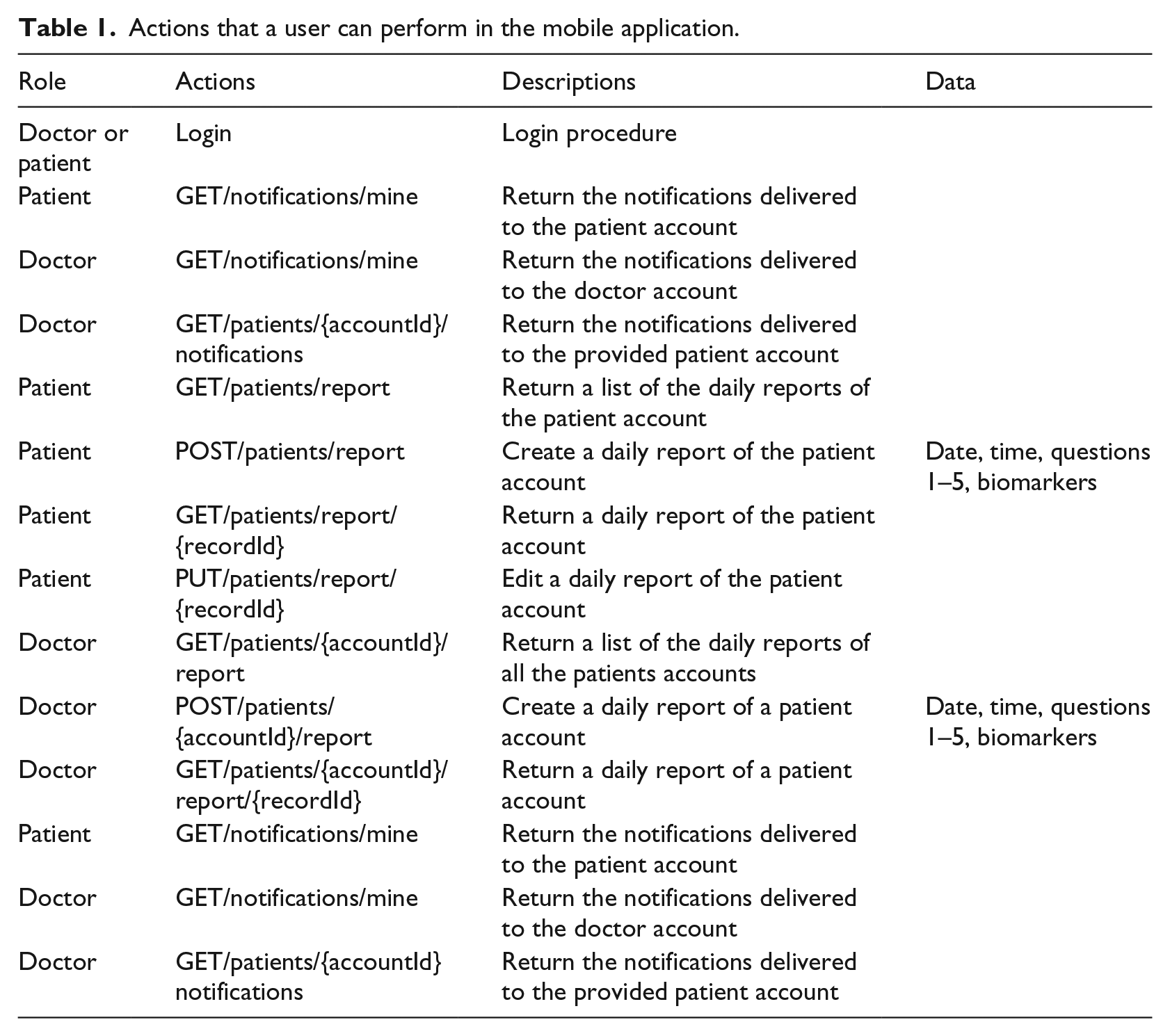
In Table 1, we present the actions that a user of the mobile application is able to perform according to his role (doctor or patient). More specific, Table 1 consists of four columns. The first column displays the role of the user (doctor or patient). The second column displays the action that the user can perform based on his role: login and get or post request methods supported by the http protocol. In the third column, there is a short description of each action. In the last column, the parameters for each action are presented.
Actions that a user can perform in the mobile application.
Design of graphical user interface
This section describes the graphical user interface (GUI) for the application that is provided by the ECHO system. The GUI for this application satisfies certain requirements so as to maximize the possibility to be attractive both to doctors and to patients. These requirements are the following:
Easy to use;
Well organized;
Complete (so that it provides all the necessary features);
Responsive (for the browser application);
Attractive.
The proposed application aligns to these requirements. Below we present thoroughly the different screens that are produced when using the GUI for the application.
ChronicOnline for patient
In case of a patient (Figure 2), the application has five different screens, apart from the login screen, which is common for all users. The first screen is the “daily report” screen. In this screen, the patient answers daily the questions that are stored in the application (see The Medical Problem section), in order to specify his health condition.
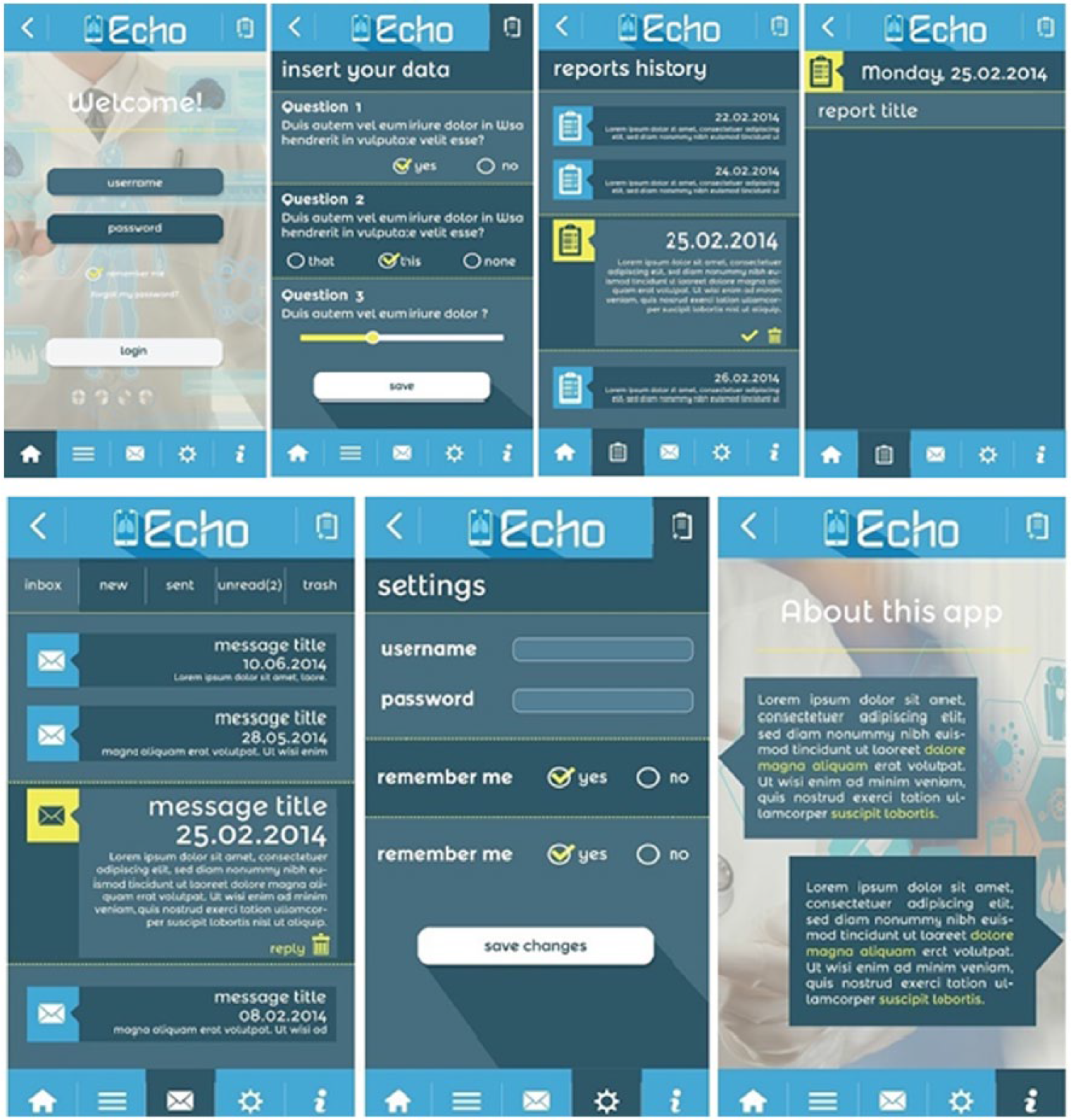
Different screens of the mobile application for the patients.
The second screen is the “reports history,” where a patient can find all his previous reports based on the date. From this screen, the patient can choose a specific date and view his report in that date. The third screen is the “message” screen. In this screen, there is a submenu with tabs for the main categories of messages that is new, sent, unread, and trash. In every screen of these categories, the user has the option to view the details of any message through the “message body” screen. The fourth screen is the “settings” screen, where the user can change his credentials. Finally, the last screen is the “about this app” screen, which gives information about the application and the ECHO project.
ChronicOnline for the doctor
In case of a doctor (Figure 3), the application has five different screens, apart from the login screen, which is common for all users. The first screen is the “list of patients,” where the doctor can choose a specific patient’s reports to view. The second screen is the “reports history” screen, which displays all the daily reports of the specific patient sorted by date. The “message,” “settings,” and “about this app” screens have the same functionality, as in the application for the patient.
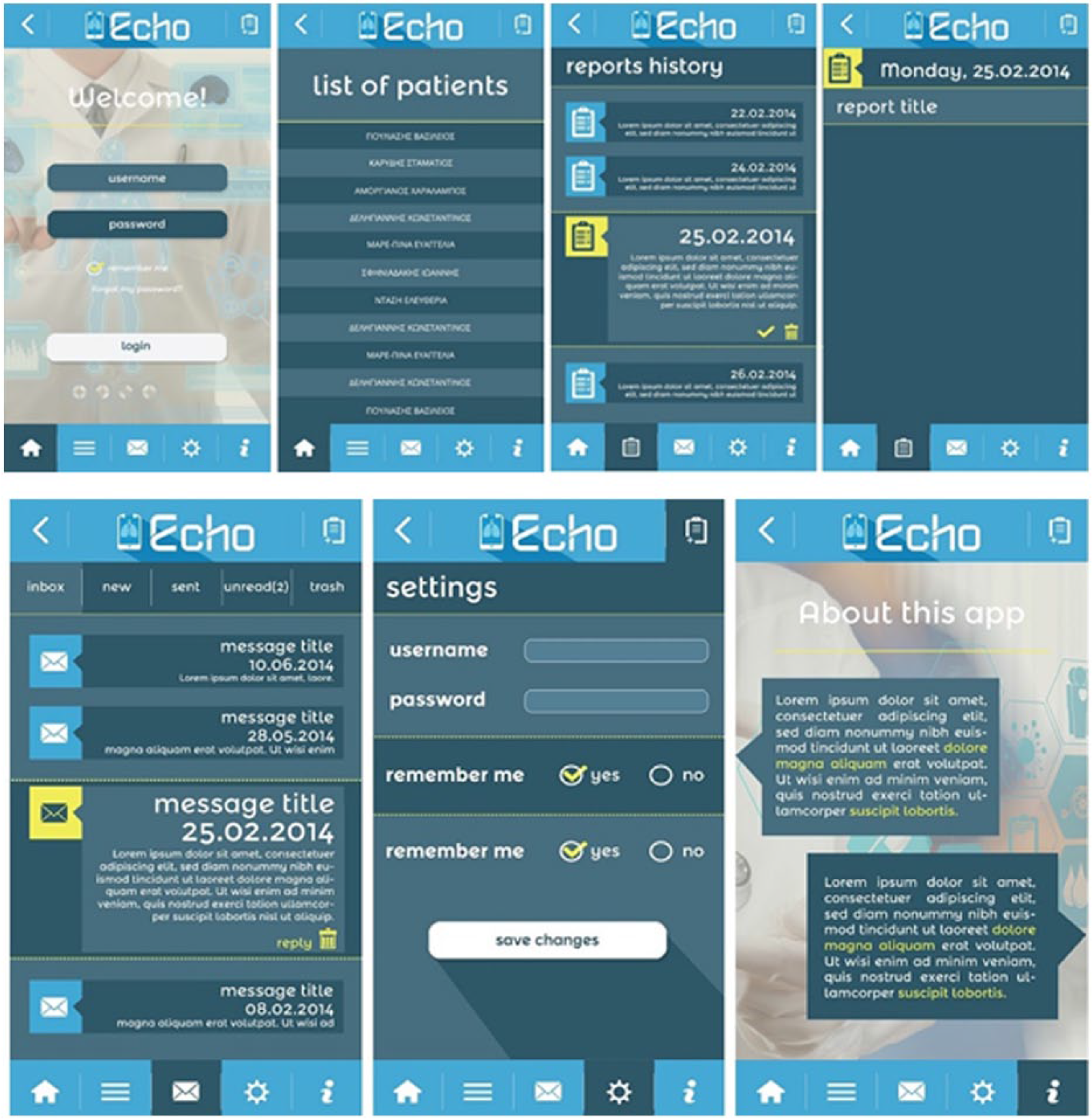
Different screens of the mobile application for the doctors.
Conclusion
The ECHO system suggests an integrated solution that connects chronic patients to their physicians through cloud infrastructure and online services, served by mobile and web applications, thereby enabling regular monitoring of patients and avoidance of medical emergencies. In this article, we implement the frontend applications of the ECHO system and describe their functionality and the interfaces available to the users. As a future work, we aim to test and validate the proposed system using a group of patients provided by the Respiratory Ailments Clinic of University of Crete.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the General Secretariat for Research and Technology of the Ministry of Education and Religious Affairs, Culture and Sports of the Hellenic Republic project ECHO (GSRT GER_1926) and by the German government-funded BMBF project ECHO (01XZ13023G).
