Abstract
We developed two virtual communities of practice (Endobloc and Pneumobloc) to increase the interaction between general practitioners and nurses in primary care and hospital endocrinologists and pulmonologists. They were designed and developed using an existing web 2.0-based virtual network belonging to the local National Health System, and we quantitatively assessed the usefulness through the participation and use during the first 24 months after the launch in 2010. A total of 26,372 visits (47% Endobloc’s visits) and 2351 contributions (Endobloc’s contribution 38.9%) to both virtual communities of practice were registered during the first 24 months. The most popular sections were the e-Blog and the e-Consultations section in both virtual communities of practice, but some differences in the pattern of use in other sections were observed. Activity on the virtual communities of practice occurred throughout the day including weekends and holiday periods. We showed that virtual communities of practice are feasible under real-life clinical practice.
Introduction
Most healthcare professionals in developed countries use the Internet in their daily professional activities. Physicians, nurses, and other healthcare providers are connected and share databases, medical records, and scientific information.1,2 A transformation from analogical procedures to digital ones has taken place in the last two decades related to these new skills for publishing and information research on new findings, clinical trials or drugs.3,4
At the beginning of the 21st century, social networks on the Internet went through a second revolution on new technologies called web 2.0 because users became active participants creating new contents that can be shared immediately. 5 This new concept of real-time collaboration between peers has been designated networking. Within networking, the concept called “virtual community” (VC) arises. A VC is defined as “an aggregation of individuals that as business partners interact around a shared interest, where the interaction is at least partially supported and/or mediated by technology and guided by some protocols or rules.” 6 VCs mainly allow participants to exchange information and provide social support to a business, a marketing project or health institution. 7 It is important to point out that a VC also allows to optimize personal resources and to spread knowledge.8,9 With regard to online health-related knowledge transfer, strategies include the use of wikis, discussion forums, blogs, social media to data/knowledge management tools, conferencing technology, and virtual communities of practice (VCoP). 10 Most VCoPs are patient-oriented supporting groups with or without healthcare professionals as moderators or participants with the goal of promoting health, but there are also VCoPs that promote learning, exchange of information and knowledge, and also share and foster evidence-based practice between healthcare professionals. 11
Examples of large VCoPs at the international level restricted to physicians include the community called Sermo (http://sermo.com), which has about 343,000 registered professionals mainly from the United States and the United Kingdom with 68 different medical specialties and subspecialties, 12 and Esanum (http://esanum.com), restricted to physicians mainly from Europe with members from different specialties who share data about clinical reports and collaborate in writing papers. The main conclusion after revising this initiative is that the benefit perceived by users is the satisfaction of sharing knowledge within a community of colleagues. The measurement of the impact, benefits, and effectiveness of these kinds of approaches is not easy to calculate, 10 but it seems that new possibilities of improvement are offered.13,14
Few data are available on the interaction between general practitioners (GPs) and hospital-specialist physicians via an online interface and their implications on daily clinical practice, 15 but online interaction has proven to improve medical care and reduce hospital referrals in several specialties.16–19 In Catalonia, for instance, the ECOPIH project (Online Communication Tool between Primary and Hospital Care; http://ecopih.webnode.es) involves a wide selection of medical specialties and includes healthcare professionals from primary care centers (PCCs) and specialists from two important cities in the metropolitan area of Barcelona.20,21 The qualitative evaluation of the performance of this VCoP found that communication between primary and hospital care led to improved primary care and fewer hospital referrals and that the closer the healthcare professionals were to their patients the more they used the platform, thus also indirectly contributing to improved healthcare. 21 Encouraged by the success of this regional VCoP, the aim of the current project was to implement a new tool for the management of medical knowledge focused on endocrine and metabolic disorders and respiratory diseases. This new tool is a web 2.0-based VC implemented by healthcare professionals from the primary care area of Lleida and specialized physicians from the departments of endocrinology and pulmonology of the reference hospital. In this article, we describe the development and implementation of these two VCoPs and the assessment of participation and use for the first 24 months after its launch.
Methods
Objectives and VCoP design
Based on an initiative from the Endocrinology and Pneumology departments at the Hospital Arnau de Vilanova, two VCoPs, one on endocrinology (Endobloc) and one on pneumology (Pneumobloc), were designed to allow online interaction of a population of GPs and nurses working on the clinical management of diabetic and obese patients and chronic respiratory patients attended at PCCs in the area of Lleida with the endocrinologists and pulmonologists of the Hospital Universitari Arnau de Vilanova (Lleida), all of them pertaining to the National Public Health System in Catalonia (Spain). This hospital is the one attending patients who are referred from the area, which is distributed in 22 basic healthcare districts including 220 primary care working teams (a nurse and a GP in each one), representing a total population of 440 healthcare professionals.
For the development of the VCoPs, we chose a web-based electronic public service meant to be flexible, safe, intuitive, cheap, and easily implemented in the context of the public institutions that were going to use it. The use of other alternatives, such as a specific program like SharePoint (Microsoft®), would have been of limited use to the participants because it would have not only required specific learning on its use, but would have been only accessible from the intranet at workplaces (i.e. hospital or PCCs) for security reasons. Conversely, the use of web-based community allows accessibility outside working hours and workplaces, thus breaking the space-time barrier to facilitate sharing knowledge between professionals. Moreover, we chose a platform belonging to the local Government, which also guarantees security in communications and ensures the privacy of the information and personal data. Both VCoPs were web 2.0-based and used the Content Management System of the platform e-Catalunya (http://ecatalunya.gencat.cat), which belongs to the Catalonian local government (Generalitat of Catalonia). This platform promotes collaborative work groups and offers a virtual space that can be easily adapted to the particular requirements of the working group or VCoP (e.g. forums, wikis, folders, mail lists, and automatic alerts) and is designed to run on desktop/laptop computers.
The process of development of both VCoPs is shown in Figure 1. Briefly, the project was developed through different consecutive stages: (1) initial design and structure of the web-site structure by a community manager; (2) definition of the initial contents to be shared by the VCoP participants by a working group consisting of a virtual manager, two specialists (one endocrinologist and one pulmonologist), and two GPs; (3) dissemination meetings by the management team at the PCCs participating in the pilot phase (6 months duration) to introduce the characteristics of the project, advantages of the collaborative work in a VCoP, procedures to allow participation, and practical training on the use of the platform and its contents; (4) evaluation of the functioning and participation after the pilot phase to adapt the structure and/or contents of the VCoP based on the users’ feedback and needs; (5) launch of the final VCoPs, with invitations through corporative e-mailing, dissemination meetings at all PCCs of the Hospital reference area, and training for healthcare professionals (physicians or nurses) willing to participate; and (6) follow-up and analyses on participation and use of each VCoP after 2 years of full functioning in real-life clinical practice.
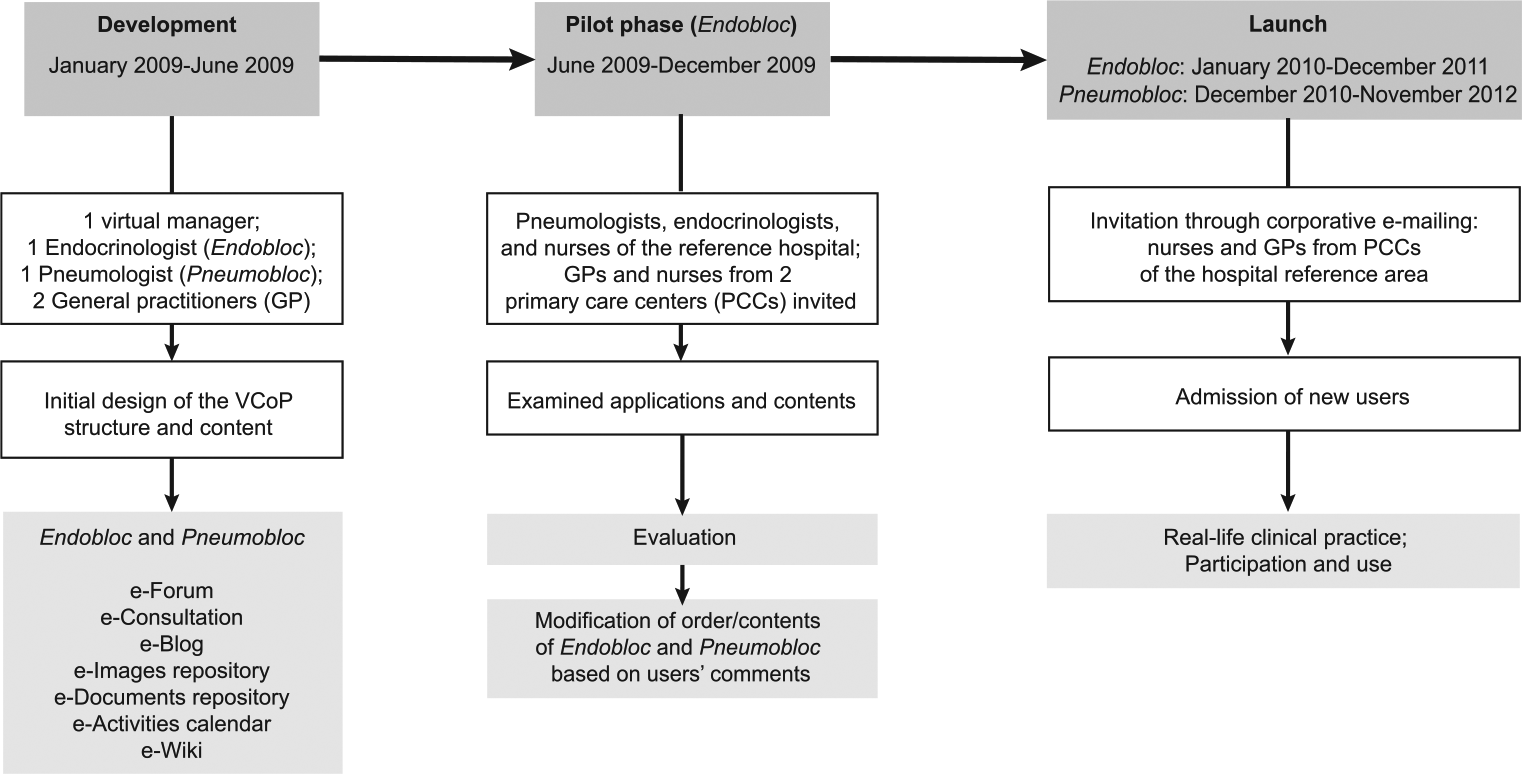
Development and launch of the two VCoPs.
Ethics and security
The research protocol was approved by the Ethics Committee and Clinical Research of the Primary Care Research Institute IDIAP Jordi Gol (Barcelona, Spain).
The e-Catalunya platform guaranteed confidentiality of personal data for the users and the content of the VCoP in accordance with the Law of Protection of Personal Data (15/1999 of 13 December). Moreover, all participants signed a letter of commitment in which they agreed to use the VCoP in accordance to the current Law, to maintain as confidential all private communications received, and to not introduce specially protected data or data that may allow identifying people (e.g. a patient’s personal data).
Variables assessed
Evaluation of the functioning and participation after the 6 months pilot phase was quantitatively assessed using the data automatically recorded by the technology platform that supported Endobloc. Variables included total number of visits/connections to the network, visits per month, and day and time of the week; total number of contributions (e.g. active participation in any section, such as making a case consultation and uploading documents or images) and their author, contributions per month, day and time of the week; and visits and contributions per section. Moreover, we qualitatively evaluated the perception, usefulness, and level of satisfaction through a specific survey consisting of 30 questions distributed among users. The participation and use of Endobloc and Pneumobloc at the end of the first 24 months after launch was quantitatively assessed through the same variables described above for the pilot phase, and we also quantified the number of lurkers, defined as subjects who initially registered as users but never visited the VCoP. Values of quantitative variables are expressed as mean and standard deviation or range, and qualitative variables are expressed as number and percentages.
Results
Development of the two VCoPs: Endobloc and Pneumobloc
The process of development of both VCoPs is shown in Figure 1. For a period of 6 months (January to June 2009), a working group designed and drafted the initial contents of each VCoP. Each team consisted of a VC manager, an endocrinologist (for Endobloc), a pulmonologist (for Pneumobloc), and two GPs. The virtual system offered three main Internet-based functions: communication and interaction with peers, access to information, and joint work. Both VCoPs (Endobloc and Pneumobloc) were identical in structure and included seven different sections, namely, an e-Forum (with common interest topics and virtual clinical sessions), an e-Consultation section (with short clinical real case reports, together with questions and comments), an e-Blog (with breaking news related to health topics and the VCoP network), an e-Images repository (for complementary data to clinical reports, e.g., X-ray images and computerized thoracic-scan images), an e-Documents repository (for common document storage), an e-Activities calendar (holding common agendas, e.g., scientific events and workshops), and an e-Wiki (with a multi-user documents creator and a sharing tool).
The site was password protected and was made available only to the participants involved and those working directly on the study. The staff working on each of the VCoPs were one community manager, aimed not only at giving methodological and technical support to participants but also at involving and committing visitors to participate, and two facilitators/moderators who reviewed content, supported participants, encouraged participants to contribute and contributed themselves, guaranteed the authenticity of contents, and ensured a respectful behavior within the group.
After the design of the structure and contents of both VCoPs, a six-month run-up feasibility period (June to December 2009) or pilot phase was performed with the Endobloc only, as both virtual communities were identical and assumed to perform in a similar way. For this pilot phase pneumologists, endocrinologists, and nurses of the reference hospital, and nurses and GPs from two PCCs were invited to participate: one PCC from an urban area of the city of Lleida where the reference hospital is located and a second one from a semi-urban and its rural reference area (between 30 and 90 min drive from the hospital).
Sixty-six healthcare professionals from the two PCCs accepted to participate. Users had access to the Endobloc and were able to examine the applications and contents, contribute in every section and, for medical consultations they could expect a reply within the following 48 h. The quantitative assessment on the participation and use showed that 59.1 percent subjects participated actively, 71.2 percent of them visited the VCoP, and 13.6 percent of them contributed with content. Nurses participated less (33% of the total participants) and were less active than GPs, with nurses accounting for 8.4 percent of total contributions, and 25 percent of total visits. Finally, a survey to assess perception and usefulness of the VCoP, answered by 63 percent of participants, showed that, on a 1–10 scale, the mean satisfaction score for all sections was above 7 and that the highest scoring services were the e-Consultation and the e-Document repository, while the e-Wiki was the least valued section. Moreover, 92 percent of participants thought that it was a good model to be used on other PCCs, and 97 percent thought that it would be useful to implement in other specialties.
The structure of Endobloc was modified based on the users’ comments, which were mainly related to the ordering or labeling of the sections’ contents, and Pneumobloc was adapted accordingly.
Implementation and use of Endobloc and Pneumobloc
After the acceptable levels of participation and the high degree of users’ satisfaction during the pilot experience with Endobloc, this VCoP was launched and fully implemented into real-life clinical practice in January 2010, and the Pneumobloc was launched in December 2010. Primary care professionals (GPs and nurses) from the 22 districts of the reference hospital area were invited to attend scheduled meetings and were contacted through corporative e-mailing to join in both VCoPs. Their participation as professionals was a personal decision and not mandatory for clinical practice. Admission to the VCoPs was open on a continuous basis for all potential candidates from the beginning of the project, and after the initial invitation, new users were admitted as requested. To ensure that new users willing to participate were staff working at PCs or at the hospital, they were advised to send an e-mail to the community moderator who in turn resent the request to the community manager, who registered them as new users and granted permission. Finally, the e-Catalunya platform sent an e-mail to the new participant with the assigned username and password.
During the first 24 months of activity, 181 primary care healthcare professionals out of the 440 invited decided to register and join each of the VCoPs (Endobloc and Pneumobloc) and contributed to or visited its content. At the end of the first 24 months of use, we registered a total of 26,372 visits, with a similar total number of connections to each of the VCoPs and also a similar mean number of visits per month (Table 1). The total number of contributions was 2352 and was higher among users of the Pneumobloc (1436; 61%). Although the mean number of contributions per month was higher among Pneumobloc users (60 vs 38), the mean number of contributors was similar (11.3 vs 10.8), which indicates that those participating in the Endobloc were equally pro-active but contributed with less content. The activity registered in both VCoPs during the first 24 months is shown in Figure 2(a) and (b); Pneumobloc had a remarkable higher number of both visits and contributions during the first 8 months after its launch than Endobloc, but afterward activity decreased to the same level, and then both VCoPs stabilized and registered a similar rate of visits and contributions until the end of the assessment period.
Summary of activity for Endobloc and Pneumobloc VCoP 24 months after the launch.
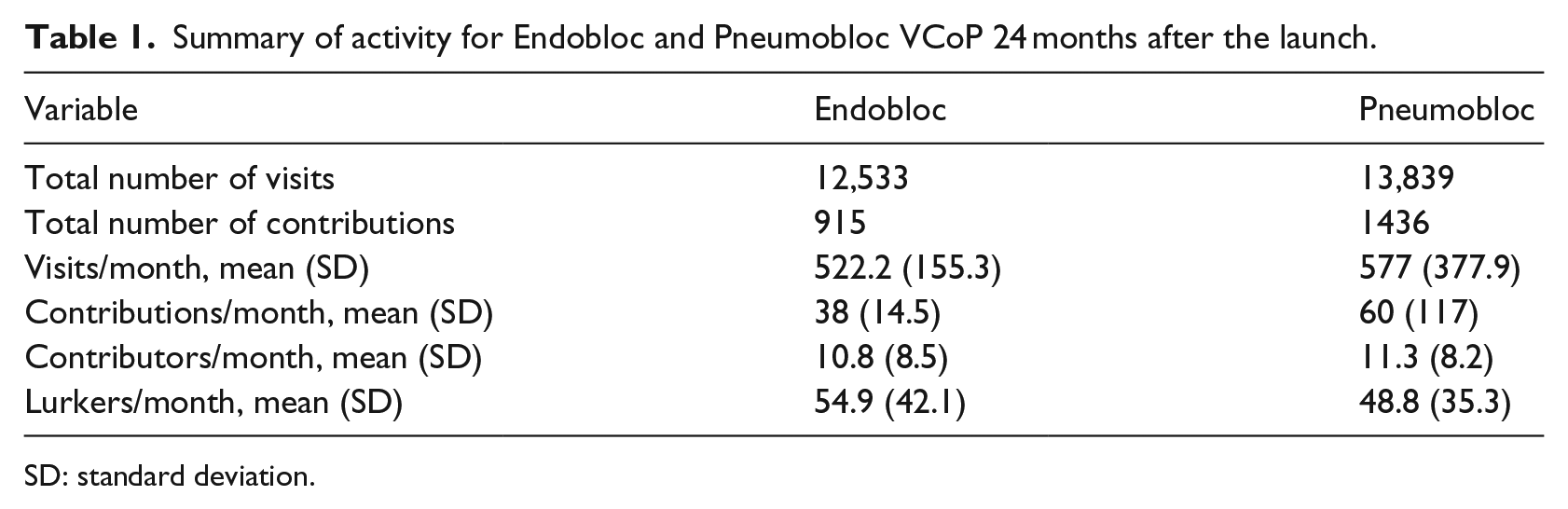
SD: standard deviation.
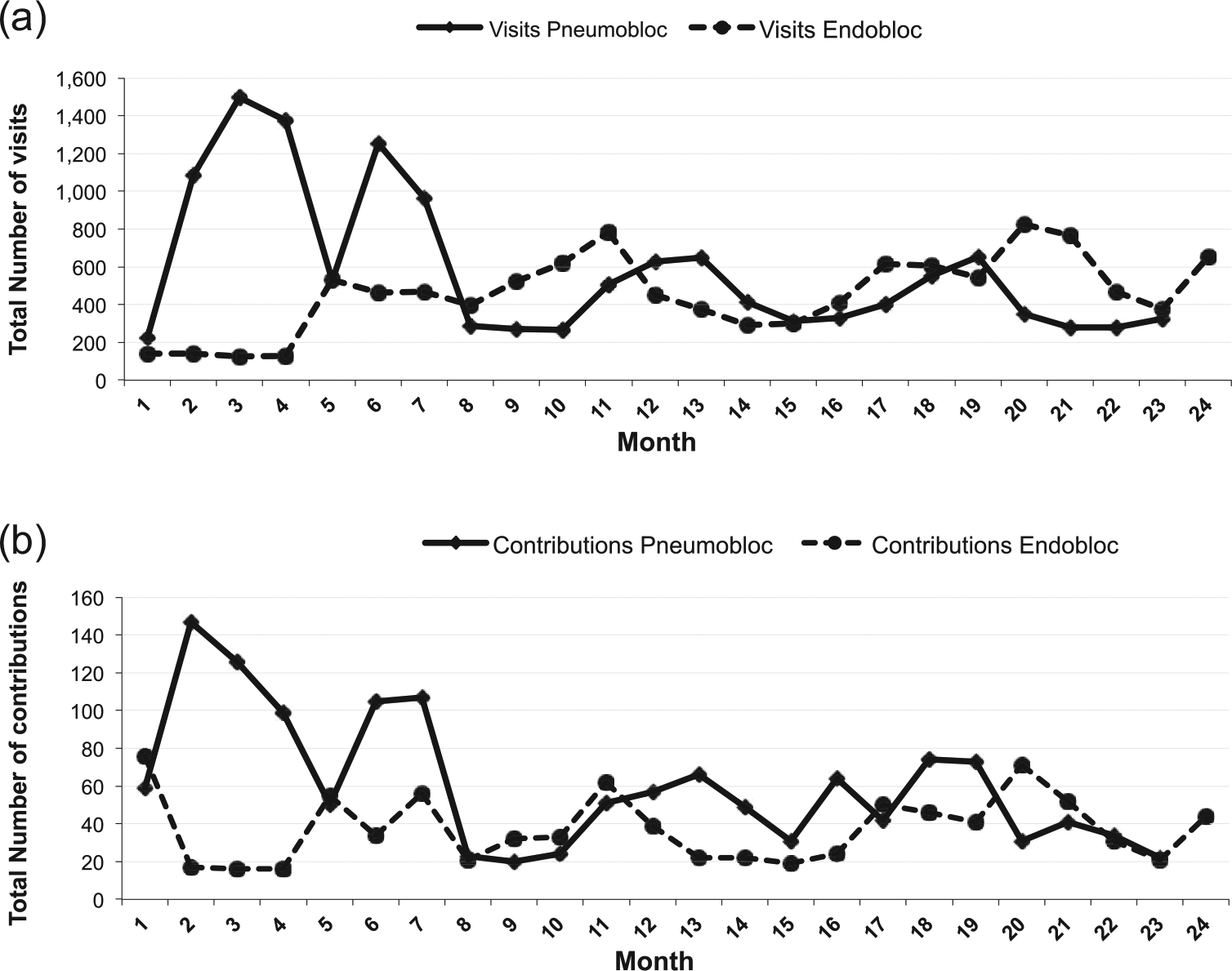
Pattern of activity (a, visits; b, contributions) of the two VCoPs during the first 24 months after the launch.
The pattern of connections to the different sections of the VCoPs is shown in Figure 3(a). While for both VCoPs the most visited section was the e-Consultation, with 64 percent of all visits by Endobloc users, and 38 percent for Pneumobloc users, Endobloc users rarely visited the e-blog; both the e-Images repository and e-Forum sections were much less visited than the e-Consultation section and more visited among Pneumobloc users. Finally, the least accessed content were the e-Documents repository and e-Wiki sections, with the e-Wiki accessed more frequently by Endobloc participants. The pattern of contributions to each VCoP (Figure 3(b)) also shows that Pneumobloc users contributed more than Endobloc users to all sections of the VCoP and were practically the only ones actively participating in the e-Blog section.
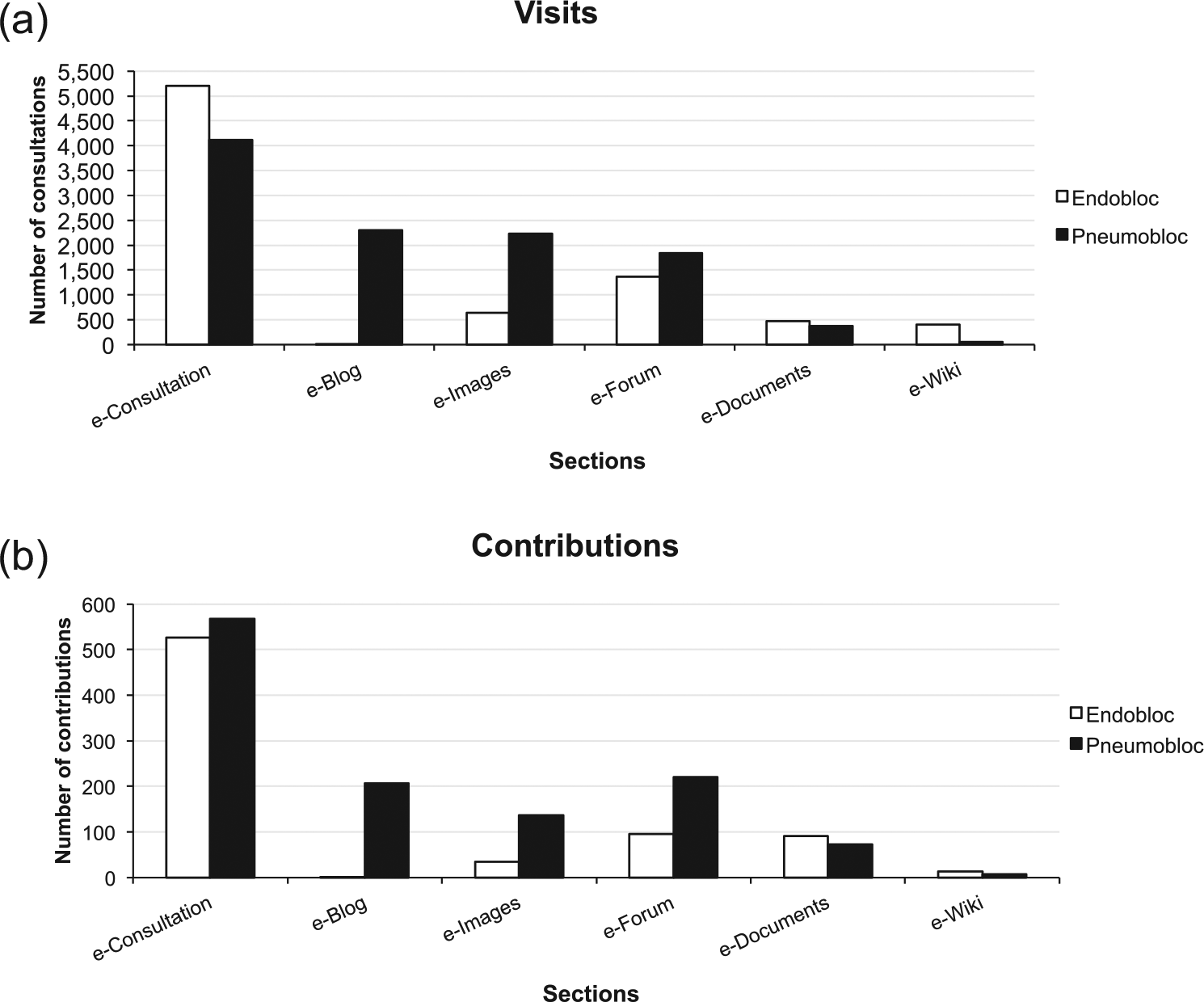
(a) Pattern of visits and (b) contributions to each section of the VCoPs.
As for the level of activity during the days of the week and time of the day, both the mean number of visits and contributions to either VCoP occurred throughout the day including the weekend and holiday periods. However, activity was steady during working days but decreased considerably during the weekend, and there were two peaks of activity during the day: one between 7:00 and 12:00 a.m. and thereafter between 3:00 and 8:00 p.m.
Regarding the composition of participants, we observed the same trend as during the pilot phase, with nurses participating less actively than other healthcare professionals. For instance, they never contributed content to the e-Blog, while specialists contributed in 12.5 percent of cases and GPs in 8 percent of cases (the remaining contributions corresponded to the moderator, the VCoP manager, and the director of the project). Moreover, nurses contributed with content to the virtual clinical sessions (e-Forum sections) in 11 percent of cases, while specialists contributed in 23 percent of cases, and GPs in 17 percent of cases.
Discussion
In this article, we assessed from a pragmatic approach the development, implementation, and access to and use of two VCoPs linked to the National Health System to increase the interaction between GPs and nurses in primary care and hospital endocrinologists and pulmonologists. We demonstrated here that these VCoPs can be implemented in real-life clinical practice, which is innovative, and also that a relevant proportion of healthcare professionals became participants, which allowed sharing of content and development of new knowledge based on non conventional social networks.22–24
GPs play an increasingly relevant role in the management of prevalent diseases such as diabetes mellitus or chronic obstructive pulmonary disease. Although a fluent communication between GPs and specialists is a requirement for a proper management, 25 primary care professionals often experience professional isolation and need to communicate with specialists at hospitals in order to seek advice and improve their clinical practices. 11 New tools such as VCoPs have been shown to be effective in minimizing professional isolation, and interactive collaboration has also been associated with better population health, reduced costs, and fewer health-disparities.16,26–28 This is mainly because of the interaction among members without limitation of work-time or location, and because participants share his or her contents openly with other members so all of them benefit from it, and this flow of information generates new knowledge. 23
Similar, although not comparable, health VCoPs include the Sermo and Esanum communities, 12 but they are restricted to physicians and do not follow the model of the experience reported here (hospital reference area with common patients for two medical specialties). Previous experiences of VCoPs to foster the collaboration between GPs and specialists in our environment include the ECOPIH community, which has a wide selection of medical specialties, although available published data do not allow a direct comparison with the VCoP described here.20,21
The behavior of the participants in our VCoP in terms of the use of the different sections is the same as the one observed in a similar VCoP set up for family physicians to facilitate knowledge sharing and reduce professional isolation in Australia. 29 As for the levels of participation in a VCoP, there are three defined categories: high contributors (or core group), active members, and peripheral members who rarely participate (or lurkers), which represent the 10–15, 15–20, and 65–75 percent of the participation, respectively.30,31 In both of our VCoPs, the patterns of participation among VCoP members was higher than expected, with an average 48 percent of active members, which may be due to the simplicity, an added value that could help other similar communities that may arise following this model. 32
We observed differences in the pattern of utilization between the two VCoPs. First, Pneumobloc users visited and/or contributed much more than Endobloc users during the first 8 months after the launch and then both VCoPs stabilized and registered similar activity rates. This is because Pneumobloc was launched 1 year after Endobloc, and users at primary healthcare centers were already familiar with the environment and positively disposed toward the use of a new VCoP. Second, despite having the same structure, the utilization of the different sections was also different between Endobloc and Pneumobloc. A higher use of the e-Image repository section on Pneumobloc and a higher use of the e-Wiki section on Endobloc were observed. Radiological tests are essential to diagnose and to manage respiratory diseases, and it is reasonable to think that this is the cause of the different pattern of use. However, the agreement during the process of decision-making between hospital and primary care staff regarding follow-up procedures is crucial for patients’ management. On the other hand, the e-Wiki section was probably more visited among Endobloc users because it was used to write the unified diets for the area.
The main advantage is that Endobloc and Pneumobloc were specifically designed for their members’ requirements (dispersed healthcare staff on a wide territory), an individualized approach that warrants its use but could also limit its reproducibility in other health-related environments. A first limitation of the study is its descriptive approach, focused on the feasibility of a VCoP on real-life clinical practice conditions, which may preclude the comparison with other existing initiatives. Moreover, it is a pragmatic project without a control group, and relevant patient outcomes and efficacy parameters have not been evaluated. Additionally, there is a potential bias in our study population, since participation was voluntary and there is a clear possibility that those professionals who participated were more interested in endocrinology and respiratory disease management than non-participants. Besides, participants familiar with the usage of new technologies could have been more readily predisposed to collaborate, although previous non-virtual activities in the same environment (e.g. clinical sessions, courses, or conferences) also had a non-homogeneous participation. Moreover, the fact that nurses participated less actively than other healthcare professionals (i.e. GPs and specialists) raises the question of whether the VCoPs were too focused on resolving physician’s doubts and problems and whether nurses would need a specific environment and/or sections to address their actual clinical needs. Finally, the VCoPs were designed to only run on desktop computers, but the design of a platform that also supports the use of mobile technologies could have resulted in a higher communication between the members of the communities, and it would be useful to work toward mobile support in the future to provide improved healthcare even in remote disconnected areas.
Further research is needed in this area regarding the feasibility of VCoPs in other environments with different healthcare systems, and satisfaction of users and healthcare outcomes impact compared with non-virtual procedures should also be explored.
Conclusion
Our data show that VCoPs are useful and feasible tools in a real-life clinical practice context. The benefits of participating in VCoPs include the possibility to access the platform despite the geographical location or connecting time to assist primary care professionals to solve clinical doubts with the support of specialist colleagues, which may eventually help to avoid unnecessary referrals to reference hospitals.
Footnotes
Acknowledgements
The authors thank all participants of the Endobloc and Pneumobloc communities. CIBER of Diabetes and Associated Metabolic Diseases (CIBERDEM) and CIBER of Respiratory Diseases (CIBERES) are initiatives from Instituto de Salud Carlos III. They also acknowledge Mònica Gratacòs and Amanda Prowse for providing support in the manuscript preparation and editing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported by a grant from Fondo de Investigación Sanitaria, Instituto de Salud Carlos III, Spanish Government (No. PI08/90458), and Pneubloc was partially funded by an unrestricted grant from AstraZeneca. The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; or preparation, review, or approval of the manuscript.
