Abstract
Methodology: Using an online, mixed methods retrospective survey capturing descriptive and narrative data.
Keywords
Background
The recognition and uptake of video consulting (VC) has accelerated through health and social care delivery since the COVID-19 pandemic.1–3 During 2020, VC use has increased across the United Kingdom (UK) and throughout the National Health Service (NHS). Despite the use of other types of digital healthcare, for example, telehealth and telecare, the utilisation of VC specifically, is a new and innovative method of healthcare practice in the UK, in that its use and acceptance presents a very different picture today than it did pre-COVID.3–4 There is accumulating evidence that VC can deliver care equivalent to face-to-face consultations in many settings and offer many benefits to patients, families, professionals and society.5,6 The majority of VC literature is based upon pilot studies, with small and often highly selected samples, ultimately casting speculation on its use, benefits and challenges across varied care sectors, specialities and circumstances. 7 Therefore, the clear gaps existing in the current evidence-base require urgent attention. 8 It is suggested that there is a need to continuously evaluate and re-evaluate on a national level to allow for sustainable VC platforms to be embedded for the long-term into health and social care systems. 9 The history of technological and digital healthcare implementations in the UK has been challenging and the subject of several reports.10–13 Recommendations to improve such implementations have been adopted in Wales by Technology Enabled Care (TEC) Cymru 14 and local Health Boards and Trusts, with an adoption in ‘agile’ principles.15–16 Working in partnership with the Welsh Government and NHS Wales Informatics Service employing this collaborative method to implementation, using a clinically driven and data informed approach has enabled a large-scale system-wide implementation at a pace not previously achieved.17–20
Technology Enabled Care Cymru are an NHS Wales multidisciplinary team, with clinical, research, programme and technical expertise. Technology Enabled Care Cymru are an All-Wales digital service, that enable the sustainable use, scale up and spread of value added technology. 13 The NHS Wales VC Service is one of TEC Cymru’s programmes that was rolled-out nationally prior to the COVID-19 pandemic, 14 and made available to all Health Boards and Trusts in Wales. Since March 2020, TEC Cymru have rolled-out and evaluated on a large-scale basis across a wide range of NHS healthcare sectors across all Health Boards in Wales. This current study is one part of the larger evaluation, with more than 50,000 research participants. For more information, please visit the TEC Cymru Web site.14,21
Aims
The aim of this study was to explore the use, value, benefits and challenges of VC from the perspective of healthcare professionals only, by using a retrospective mixed methods survey. This approach differs to other datasets captured by TEC Cymru which are typically patient and healthcare professional centred. However, this study was purposely designed to capture healthcare professional-only data in order to compare and contrast data with other datasets. Please see our Web site for other datasets.21,22
Methods
Design, setting, participants
Technology Enabled Care Cymru follow a phased approach to their evaluation and research. This involves a discovery phase, exploring gaps in the literature prior to any evaluation being conducted – please see our Web site for more information.14,21
This paper presents the All-Wales data captured across all seven Health Boards and 1 Trust, across a range of healthcare settings within primary, secondary and community healthcare. (See Appendixes 1–2 for the breakdown of these categories). This is a mixed methods retrospective survey study, which presents findings from one dataset held by NHS Wales VC Service 13,14 captured for 1-month during August and September 2020. Participant eligibility included NHS healthcare professionals with experience of using VC in NHS Wales, ranging between administrative staff, clinicians and management (see Appendix 3 for the breakdown of professional types).
Sampling and recruitment
The sampling approach used was opportunity sampling, due to access of the VC intervention and ability to attach a survey link, and access to VC user emails to contact. There is risk of some bias of those willingly completing the surveys or taking part in interviews as potentially more ‘positive’ or more ‘negative’ towards the VC intervention, potentially missing out the ‘neutral’ responses. Therefore additional efforts were taken to reduce this bias, for example, snowballing sampling was explored via adverts on social media platforms (@teccymru) and through other personal or professional networks for additional interviews. The surveys were sent as a URL link. A copy of the survey can be found as a supplementary. Whilst the survey was limited to NHS Wales healthcare professionals only, it was open to all VC platform users (not just Attend Anywhere users).
Recruitment and approvals
Full consent was obtained from all participants. At the end of each survey, a statement of consent and compulsory tick box was required. TEC Cymru obtained full service evaluation approval and risk assessments for all evaluation conducted in associated to the use of the NHS Wales VC Service. This was initially obtained from their host Health Board Aneurin Bevan University Health Board Research & Development Department (Reference Number: SA/1114/20), and then national approval was obtained from all other Health Boards in Wales.
Measures
This paper presents the All-Wales overview data from the survey including 6 out of the 10 questions (three of these questions have additional sub-questions, for example, matrix rating scales of 16-statements, 13-benefits and 8-challenges) with open-ended text boxes. For more in-depth and inclusive datasets please see the TEC Cymru Web site. 14
Statistical methods
The survey data was analysed in terms of distributions of responses, as well as differences that exist between specific groups of respondents (patients and clinicians). Statistical tests of differences were conducted to compare groups on the quality ratings of VC. The quality rating was measured ordinally, as set responses were given for respondents to select. Mann–Whitney U tests were carried out to test the statistical differences between two groups of respondents. The free-text narrative was manually extracted and thematically analysed to explore emerging themes. All data was analysed by three members of the research team [GJ, JW and BW] to ensure quality and rigour, with an additional 20% validation check on all data [AA].
Results
Respondent demographics.
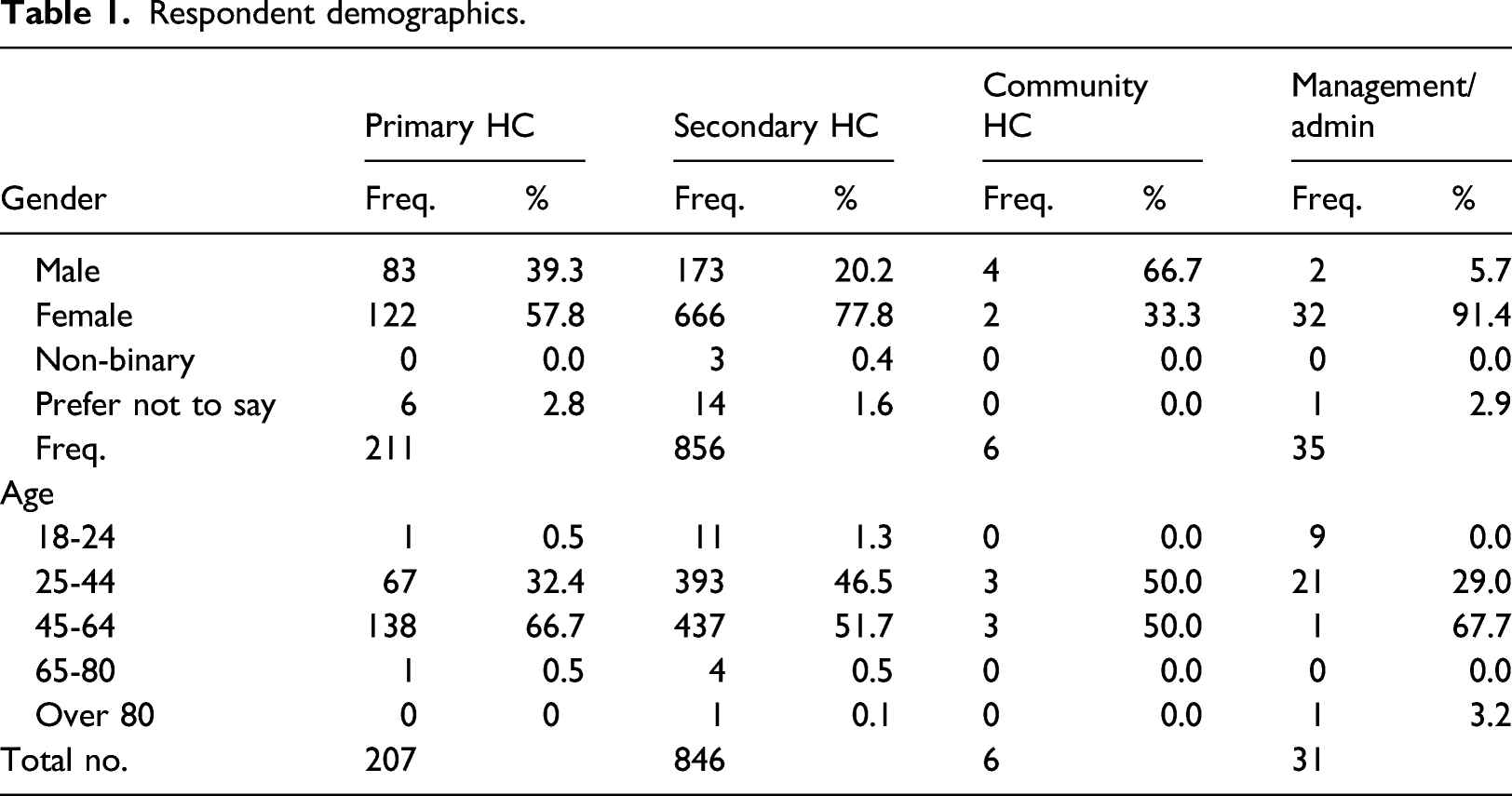
The use and value of VC
All NHS Wales healthcare professionals were asked ‘Do you think that VC should be used for health and social care appointments? (If it is clinically appropriate)’. In total, 79% responded ‘yes’, 20% responded ‘maybe’ and 1% responded ‘no’. This distribution is shown in Figure 1. The distributions of responses to ‘Should VC be used in each care sector’.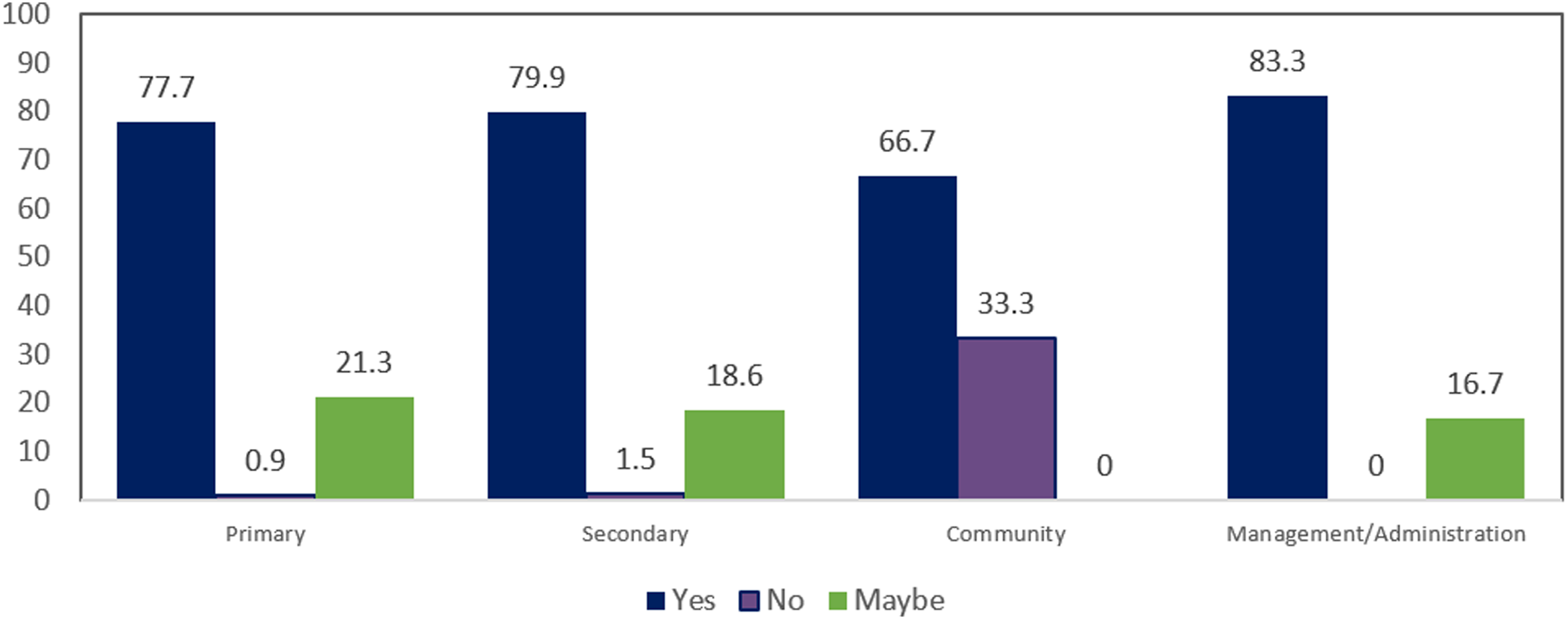
Generally, the healthcare professionals across Health Boards/Trust and care sectors had a positive regard towards the use of VC to deliver health and social care. There were a wide range of reasons to support their preferences. These are divided into five sub-categories and displayed as narrative quotes.
Flexibility
Improved flexibility was observed as a factor as to why many healthcare professionals perceived VC to be better use and value for managing patient care, compared to face-to-face. “Working professionals not having to leave work to attend appointments” (GP Doctor). “Appointment times can be more flexible to suit the patient’s needs” (Psychiatry Nurse) “Offers the patient and health system flexibility” (Respiratory medicine Nurse).
Clinical suitability
Some healthcare professionals reported that not all clinical conditions are suitable for VC; however, many state that VC is clinically suitable to reduce patient stress and anxiety levels, which in turn produces positive patient feedback. “Feedback I have had so far has been positive with patients who have reported feeling anxious to start with, but the overall experience was positive, and they chose to use it again…” (Rehabilitation Psychologist). “Patients have reported they often feel stressed when coming into hospital… and since we have been using digital platforms, they feel much more able to attend and engage…” (Pain Management Nurse).
Observing patients in their own home
The healthcare professionals’ capability to be able to observe patients within their own homes was considered to deliver better care, particularly for younger patients. “Patients are more relaxed in their home environment” (Speech and Language Therapist). “Enables patients to stay home and feel comfortable…” (Dietician). “Young persons are very familiar with using video calls anyway. They can be more open in this environment if familiar” (Psychologist).
Independent care of younger patients
Healthcare professionals report other advantages for younger patients, such as improved accessibility and independent care. “Being able to provide VC means that young people can easily access the service” (Psychologist). “Lots of young people have been more able to attend appointments independently which they perceive as being a positive outcome” (Psychiatric Nurse).
Clinical reservations and uncertainty
The survey demonstrates that 20% of healthcare professionals believe that VC should ‘maybe’ be used where possible. Healthcare professionals here state that; “VC should be used in conjunction with face-to-face” (Psychiatric Nurse) “… A one-off appointment or quarterly face-to-face if care is ongoing would be ideal too” (Psychologist). “[VC] should continue to be used forever, however… it shouldn’t replace face-to-face. We should use VC as an option…” (Support Worker).
True and false statements
The percentage of true & false statements on the use of VC.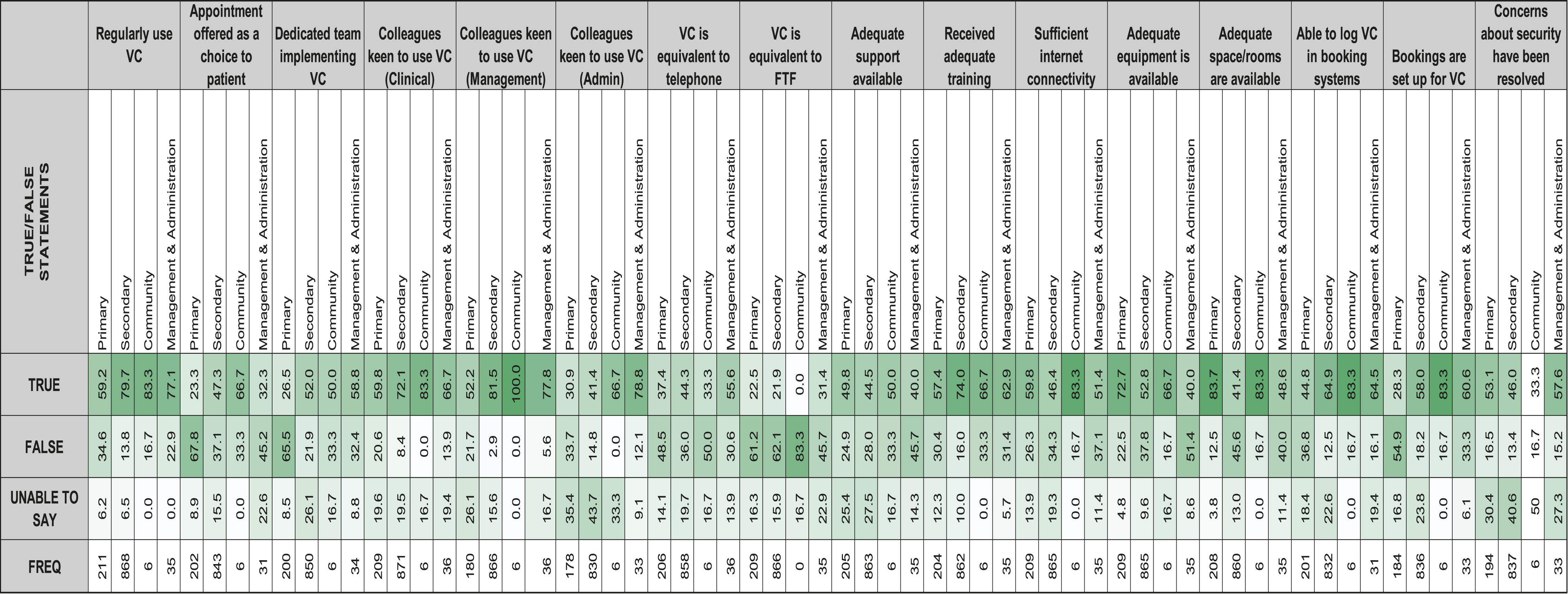
The benefits of VC
The percentage reported benefits of VC in each care sector.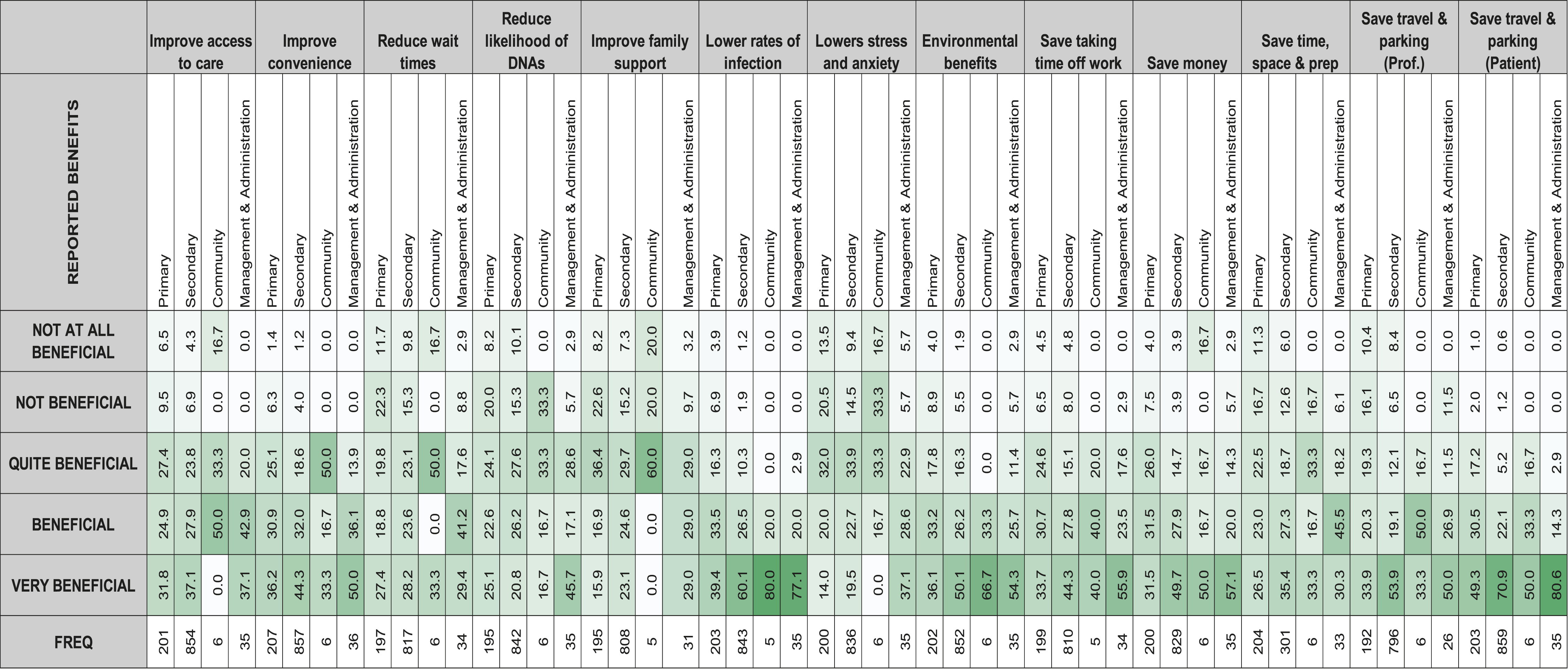
Generally, healthcare professionals across Health Boards and care sectors had a positive regard towards the benefits of VC to deliver health and social care. There was a wide range of reasons to support their preferences. These are divided into five sub-categories and displayed as narrative quotes.
Time and travel savings
A large proportion of healthcare professionals reported that there had been significant savings in time and travel for both healthcare professionals and their patients, nevertheless, more emphasis was placed on the benefits this had for their patients. “Saves travel time, especially for families with other children, saves professionals travel time” (Occupational Therapist). “Reduces the need for patients to travel long distances to appointments” (Management Primary Care)
Travel and time savings were also noted as an additional benefit for patients with mobility, psychological and neurological difficulties. “Those with social anxiety, mobility problems able to access our service for the first time” (Psychiatry Administrator). “Allows for patients with mobility issues and/or limited access to transportation to attend with ease” (Psychologist). “I have clients who prefer virtual appointments and like the convenience of this” (Psychiatry Nurse).
Environmental benefits
There were also benefits expressed regarding the environment in a move away from face-to-face consultations. “I advocate for environmental issues and agree that for various reasons (paper waste, petrol, etc.) that video calls are more environmentally friendly than face-to-face…big thumbs up!” (Trainee Psychologist). “There is less impact on the environment, with less travel” (Palliative Medicine Doctor).
Work–life balance and joined up working
Healthcare professionals identified a range of benefits that they considered specific to themselves when using VC, including an improved work/life balance, enhanced multidisciplinary team meetings (MDTs) and increased performance and flexibility of consultations. “Improved work-life balance- able to work from home more as a result…can better time appointments” (Paediatrics Pharmacist) “More efficient and direct referrals within the MDT virtual clinic” (Genitourinary Medicine Doctor) “Enables teams from across the Health Board to communicate better, more frequently, with more of the team present (virtually)” (Dietician)
In addition, joined up working also highlighted the possibility of improved interactions for both healthcare professionals and their patients with wider family involvement; “Does provide the opportunity for a second parent who may be working to be present and improve communication with both” (Physiotherapist) “Beneficial if it can involve family who would not normally be available in person” (Speech and Language Therapist)
Lowered DNAs and increasing accessibility to services
There were also other benefits mentioned, such as that of improved access to services, lowered rates of ‘Did Not Attend’ (DNAs) and the freeing up telephone lines. “Allows more free telephone lines when booking appointments” (GP Doctor) “I have observed lower rates of DNAs when conducting video calls vs. face-to-face appointments” (Trainee Psychologist) “They [patients] love the ease of it and I have had no DNAs since this has been used” (Mental Health Psychotherapist)
Infection control
The most prominent benefit reported within the data was the impact of the COVID-19 pandemic on the delivery of care, healthcare professionals expressed their gratitude for VC during this time. “Prevent[s] footfall into the surgery during the pandemic” (GP Doctor) “With the current restrictions, there is definitely a place for VC in certain circumstances” (Rheumatology Doctor) “As a staff member who has had to shield and work from home, VC has enabled me to continue to support and provide intervention to my patients” (OT Cardiology) “Also allows for review of patients receiving palliative care without increasing the risk of COVID…” (GP Doctor)
Challenges of VC
The percentage of reported challenges of VC in each care sector (healthcare professional-related challenges.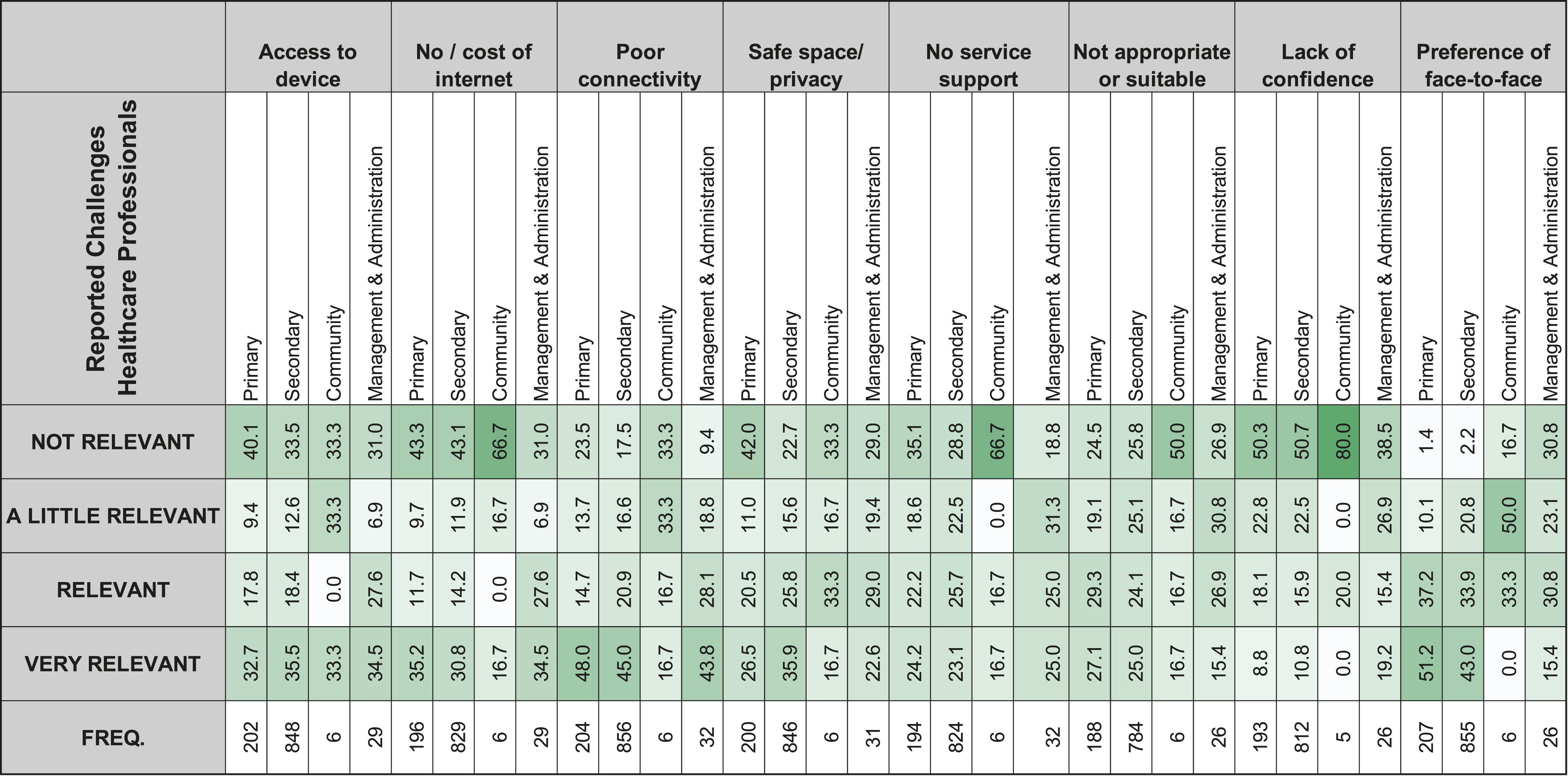
The percentage reported challenges of VC in each care sector (patient challenges from perspective of professional).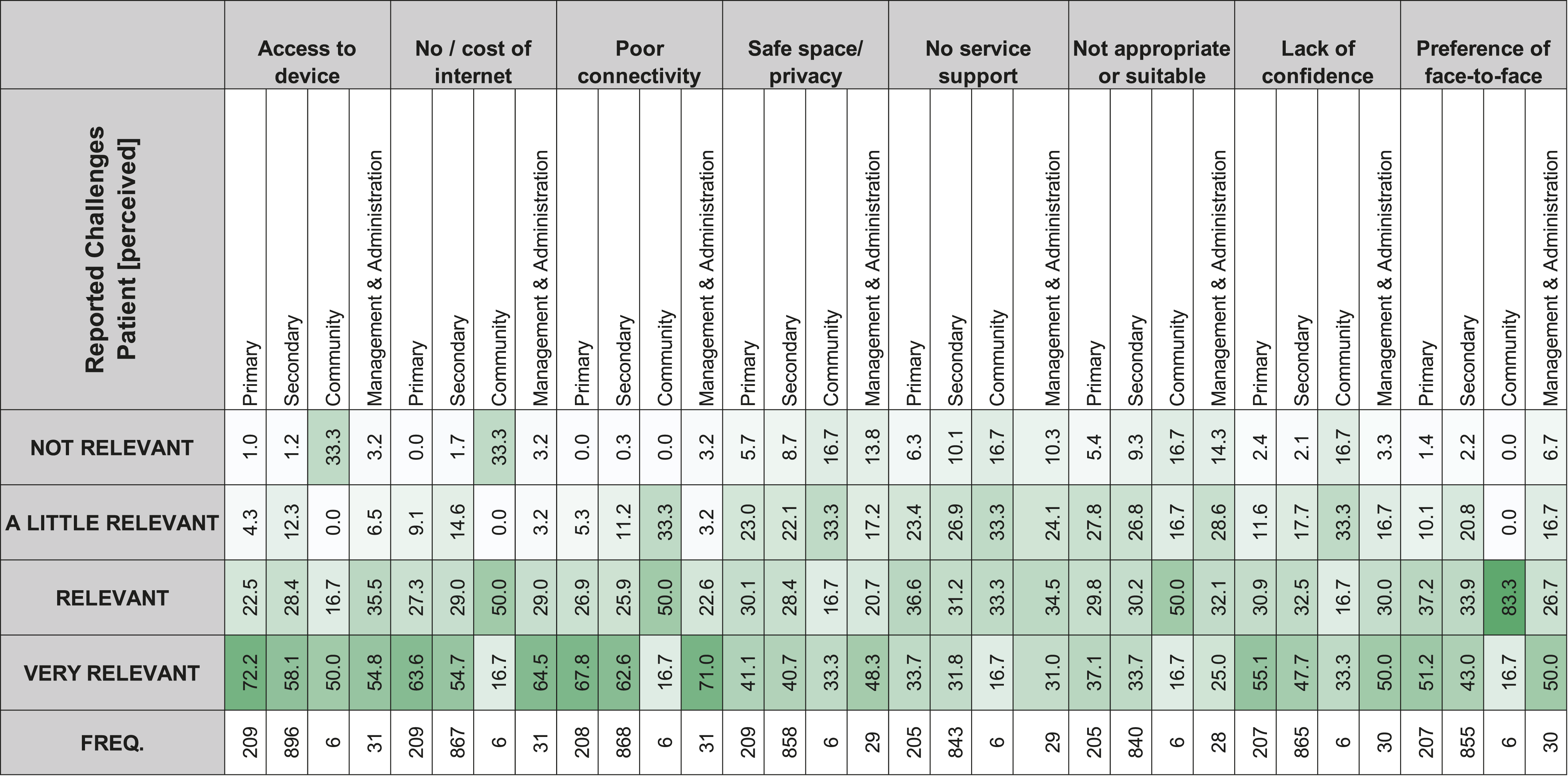
Generally, Primary and Secondary Care are similar in their ratings of potential challenges for healthcare professionals and patients using VC. One challenge that demonstrated a large difference was patients’ ‘access to a device’, with Primary Care rating this as ‘very relevant’, compared to Secondary Care. Both care sectors demonstrated these challenges to be more relevant for their patients’, than their own, which included ‘access to a device’, ‘access to internet’, and ‘having a lack of confidence to use VC’. The challenge regarding a preference for face-to-face was rated similarly for both Primary and Secondary Care for themselves and their patients, but again, large differences exist between what they consider more challenging for their patients, compared to their own challenges. For Community Care, all challenges were rated as ‘not very relevant’, and the least relevant was having ‘a lack of confidence’. In terms of challenges for patients, ‘access to a device’ was also considered most relevant. Healthcare professionals in Community Care found their own preference for face-to-face or telephone as not relevant as they felt it was for their patients, where 83.3% of healthcare professionals stated this to be ‘relevant’. In Management and Administration, it was rated that patient difficulties were more relevant than healthcare professionals’, which included ‘poor internet connectivity’ as the largest difference. On the other hand, the relevancy of having ‘adequate support’ and the ‘suitability of VC’ were similar between the patients’ view and healthcare professionals.
Healthcare professionals across Health Boards and care sectors reported a range of challenges of VC when delivering health and social care. There was a wide range of reasons to support their preferences. These are divided into three sub-categories and displayed as narrative quotes.
Healthcare delivery difficulties
Some healthcare professionals report VC to be challenging for some services to carry out their typical work in specialties that required more ‘hands-on’ healthcare delivery, such as Physiotherapy. “It can be difficult with my profession as a physiotherapy, as assessments require handling” (Paediatrics Physiotherapist) “A lot of physiotherapy input requires physical presence” (Physiotherapist)
Furthermore, healthcare professionals experienced eventualities where VC did not work as intended and were required to revert back to other forms of consultation. “We used it initially, but found that picture quality (over and above a good photograph) meant that it added little if anything to a telephone consult” (GP Doctor)
Patient difficulties [professionally perceived]
Overall, healthcare professionals retrospectively reported more perceived difficulties for their patients than they did for themselves. However, they noted that difficulties for patients were generally situation specific (e.g. where in Wales they live, that is, rural/urban) and depended on each patient’s own abilities and experience (for example, using technology). “Some of my patients live in rural areas with poor internet signal, or they simply do not have a computer or phone to access virtual meetings” (Psychiatry Nurse) “For most patients it is excellent, older adults and those without English as a first language find it harder” (Doctor) “Working with a very elderly demographic, many do not know how to use tablets, smartphones or PC, [they] prefer telephone” (Domiciliary Optometrist)
Despite some of these reported difficulties, many healthcare professionals noted that their patients had started to overcome the initial problems by equipping themselves with required resources and improved skills, thus embracing the change to digital care. “Patients are getting used to them. Surprising how even older people’s IT skills have up-scaled during the pandemic” (GP Doctor). “[Despite] unpredictable internet speeds…patients have managed to follow the instructions and engagement with the process has been positive” (Physiotherapist).
Improvements needed
Many healthcare professionals across all Health Boards reported much-needed improvements with access to better and more up-to-date technology, improved connectivity and greater levels of accessibility to produce better VC uptake, outcomes and benefits. “Lack of equipment and internet provided can cause great stress…there is no WIFI and limited internet ports so not everyone can have a PC at the same time” (Psychologist) “Often depends upon the IT set up of the patient and family. If they have good IT equipment and connection it can work well”. (Dietician)
Discussion
Prior to the pandemic, VC was rarely used in health or social care in the UK, particularly in Wales.1–3,21 Similarly to previous literature,5–6 this study suggests that VC can contribute to delivering healthcare equivalent to face-to-face consultations across a wide range of care sectors. This is also supported by other datasets captured by TEC Cymru. 22 Furthermore, the majority of VC literature is based upon pilot studies, with small and often highly selected samples, ultimately casting speculation on its use, benefits and challenges across varied care sectors, specialities and circumstances. 7 The data captured by TEC Cymru 22 contributes to this gap, providing a national understanding, and the findings in this study are a valuable contribution to this.
Overall, the responses in this study were positive, and healthcare professionals expressed optimistic views regarding the use, value and benefit of VC, even when faced with challenges on occasions.
Use of VC
Healthcare professionals reported, for the majority, that VC should be used where it is deemed clinically appropriate. In support of this, the narrative data reveals that VC should be implemented in addition to face-to-face consultations. For professionals that deemed VC more negatively, this was generally associated with holding perceptions of VC, in that it provides little more benefit than telephone calls can provide; or as a result of not having sufficient access to technology. In Primary and Secondary Care, they were very similar in their responses, where the majority would consider using VC where clinically appropriate, and a very small proportion of healthcare professionals stating that VC should not be used. Although healthcare professionals in Community Care, Management and Administration reported more negatively on this aspect, the majority still responded that VC should be used.
The majority of healthcare professionals stated that they are regularly using VC, that their colleagues are keen to use it and that they had received adequate VC training. However, there were fairly large numbers of negative comments with respect to equipment, appropriate room availability and sufficient internet connectivity, thus suggesting that healthcare professionals require more support in this area to allow them to make the most of VC in a safe and secure manner. Furthermore, healthcare professionals gave lower ratings for VC being the equivalent to telephone, and even more evident for VC being the equivalent to face-to-face. Therefore, even though VC is implemented across many services and healthcare sectors in Wales, VC is not perceived to be the same as face-to-face or even telephone for some healthcare professionals. However, this may be reflective of them seeing VC as a temporary measure. Nevertheless, it is recommended that VC should not be considered a replacement to face-to-face or telephone, but rather a tool in the clinicians’ toolbox which can be used if clinically appropriate and the patient is able to access it. This needs to be explored further, as it provides a whole service transformation in line with Welsh Policy (e.g. Healthier Wales).
Interestingly, there were notable differences between Primary and Secondary Care on the responses given to the ‘true and false’ statements. Secondary Care had a higher proportion of positive responses, including using VC more regularly than Primary Care, having colleagues more eager to use VC, and their systems set up for the use of VC. On the contrary, Primary Care were more positive in having adequate support, equipment and sufficient internet connectivity. This implies that Secondary Care perceive the need for VC more, yet lack the resources to do so, compared to colleagues in Primary Care who tend to have the resources, yet are less inclined use it. In Community Care, the healthcare professionals stated that the majority of the time VC was positive, except for perceiving VC as being equivalent to telephone and that their cyber security concerns were resolved. This was similar to the responses for Management and Administration. Interestingly, when comparing this data with more recent datasets captured by TEC Cymru, both Secondary Care and Community Care have continued using VC post lockdowns, compared to Primary Care, who now rarely use VC, and report to prefer the telephone. 22
Benefits of VC
Generally, VC was perceived as beneficial across all aspects, except for being slightly lower for aspects such as reducing stress and anxiety for their patients and reducing the likelihood of ‘DNAs’. However, these were still perceived to be beneficial by healthcare professionals, overall (approximately half of the respondents). This is supported in the qualitative data, which reveals a large proportion of healthcare professionals reporting a reduction of DNAs, with some stating they have had no DNAs since the implementation of VC. However, in view of the COVID restrictions this needs to be interpreted cautiously. Similarly, the reduction of stress and anxiety levels in patients was supported in the narrative data, with many healthcare professionals reporting VC as an improved method of care for some patients. The most positively rated benefit was saving time, travel and parking, mainly for the patient (but the professionals too). In support of this, the narrative revealed that saving travel time for the patient and professionals was useful, especially for those who exhibit difficulties with leaving their homes due to psychological, neurological and physical disorders. In addition, the lack of travel introduces environmental benefits, suggesting that VC is more environmentally friendly than face-to-face consultations. Furthermore, this data also suggests that VC makes appointments more accessible for many patients, specifically those with disorders such as autism-spectrum disorders, and for younger patients by allowing them to take a more independent role in their care. However, further research is required to explore this finding. A further benefit of VC, evidenced by the qualitative data, is the ability for healthcare professionals to observe patients in their own homes. The use of VC also had benefits for healthcare professionals, improving work–life balance, increasing flexibility and improving communication between different teams. Overall, Secondary Care clinicians were, on average, more positive in their responses for all possible benefits, except for reducing the likelihood of DNAs. The largest difference between the two care sectors was for lowering the rates of infection, in that Primary Care viewed this much lower compared to Secondary Care, although it could be suggested that this is due to Primary Care not having in-patient settings, thus less of a concern.
Challenges of VC
In general, the challenges across care sectors were considered more relevant for patients than for the healthcare professionals. There were large differences between clinicians’ challenges and their perceptions of patients’ for having access to a device, internet accessibility and connection, and having a lack of confidence. On the contrary, the preference for face-to-face was a relevant challenge for both patients and healthcare professionals, although this was rated more for patients. This challenge needs to be addressed further, supporting the previously mentioned suggestion that face-to-face and VC are enabled side by side, so that healthcare professionals and patients can make the choice of when face-to-face is appropriate based on clinical judgement and patients’ situation and experiences.
Considering the qualitative data, difficulties with technology emerged, supporting the idea that healthcare professionals and their patients encounter restraints that impact on their experience with VC. One factor that was seen to impact upon subjective difficulties was the demographics of patients, particularly older or elderly individuals, who may not be as “tech savvy” as the younger generation. However, the difficulties with technology were very specific and were not exhibited across all healthcare professionals, with most expressing positive experiences with their platforms and VC in general. Nevertheless, the benefits of VC seem to outweigh the difficulties, and further support is needed to help with adjustment to digital healthcare and long-term implementation of VC. In favour of this, healthcare professionals report that despite these issues with technology being present, patients have been able to engage and follow instructions adequately.
Overall, Primary and Secondary Care were similar in the relevancy ratings given for the possible challenges faced with VC. The largest difference, however, between the care sectors was for patients’ access to a device, being more relevant within Primary Care, although this was still highly relevant for Secondary Care. Both care sectors observed patient challenges as more relevant than their own. Thus, these findings suggest that Primary and Secondary Care are similar in their views of the relevant challenges associated with VC. For Community Care, however, the healthcare professionals’ challenges were reported as being less of a problem than they perceived for their patients.
When comparing this data with more recent datasets captured by TEC Cymru, it is clear to see that many of the challenges have been resolved, which suggests that many of the reported challenges are minor, or potential teething problems. 22
Conclusions and recommendations
In response to the emergency pandemic, TEC Cymru implemented an NHS Wales VC Service to all Health Boards in Wales using one-single VC platform ‘Attend Anywhere’. This Welsh implementation has approached VC as a venture requiring coordination and collaboration rather than direction, target-driven and traditional methodologies reflecting an emerging trend in improved systems management.20,21 The success of the NHS Wales VC service is believed to be associated to the way Wales implemented it. For example, TEC Cymru had already established a network through the technical (Assistant Directors of Informatics) and clinical leads (Chief Clinical Information Officers) in Wales enabling Health Boards to be ‘ready to receive’ the VC implementation. Building on their existing relationships, an agreed approach to implementation was adopted, involving local organisations making their own decisions about suitable services to engage, and to use their local knowledge and networks to determine a process and agreeing standards. ‘Attend Anywhere’ was the single VC platform procured in Wales, and there was encouragement across Health Boards to adopt it if it provided the required capability, but there was no formal mandate as the only solution ‘Once for Wales’. Rather, it was presented as a product that would cover the most common use cases, and it was accepted that other VC platforms may also be adopted if needed with the support from TEC Cymru to help coordinate how best to use and coordinate this collaborative learning and evaluation.
This study provides evidence of the success of this ongoing and national approach. The centralised coordination via TEC Cymru responsible for providing a framework for planning, resourcing, guidance, training, technical readiness and implementation allied to devolved local clinical and programme teams has been successful in maintaining interest and continued use of VC uptake, knowledge and expansion of use cases, for example, group VC. This highlights that there is no single model that fits all, even in a small country like Wales. The evaluation of the NHS Wales VC Service (all TEC Cymru data) demonstrates consistency of satisfaction and acceptability across all Health Boards and care sectors, and therefore, a lesson learnt in Wales is that difference is not necessarily negative, but rather a more ideal and suited approach to take when implementing new innovations into the NHS, such as VC to encourage its long-term sustainability.
Strengths and limitations
There are many strengths to this study, including its mixed methodology approach, and its relatively representative sample for VC users in Wales. However, the study did have some limitations. For example, the small sample of community care professionals recruited, which impacts on the representative nature of community care professionals using VC in Wales. Unfortunately, due to the opportunity sampling methods taken to recruit, it is unknown to the authors the reasons for why the participation is low. There were also limits on available participant demographic data, which provides limited context within the results; however, this is something TEC Cymru observed early in its evaluation phase, and has been adding more demographic questions to new dataset captures. Despite the purpose of this study being to recruit ‘healthcare professionals only’, this dataset may be considered invalid to some readers, as it is only the perception of healthcare professionals on patient satisfaction. However, the findings within this study are similar to other datasets captured by TEC Cymru that do include patient voices – see other datasets here.21,22
Footnotes
Author contributions
GJ contributed to the main design of the study and development of the research questions, the main structure and write-up of the paper, and final amendments to the manuscript. JW and BW analysed the survey data, with GJ, AA supervision. GJ, AA, SK, JW, BW discussed the data once analysed, and interpreted the data. SK, MO, KP, MH, AW helped structure the manuscript, and contributed to the Programme and clinical understanding of the findings and shaped the conclusions and recommendations. AA was responsible for overseeing the entire development of the study and paper from a clinical and programme perspective, helped structure the manuscript, and shape final conclusions and recommendations. All authors contributed to proof-reading and amendments of the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: TEC Cymru and the National Video Consulting (VC) Service is a funded programme by the Welsh Government (no award number provided).
Ethical approvals
TEC Cymru obtained full service evaluation approval and risk assessments for all evaluation conducted in associated to the use of the NHS Wales VC Service. This was initially obtained from their host Health Board Aneurin Bevan University Health Board Research & Development Department (Reference Number: SA/1114/20), and then national approval was obtained from all other Health Boards in Wales.
Statement of data sharing
Appendix
Please note: The care sector definitions are based on how the national VC service define them in the Attend Anywhere ‘tagging’ system.
Appendix 1
Primary, secondary and community care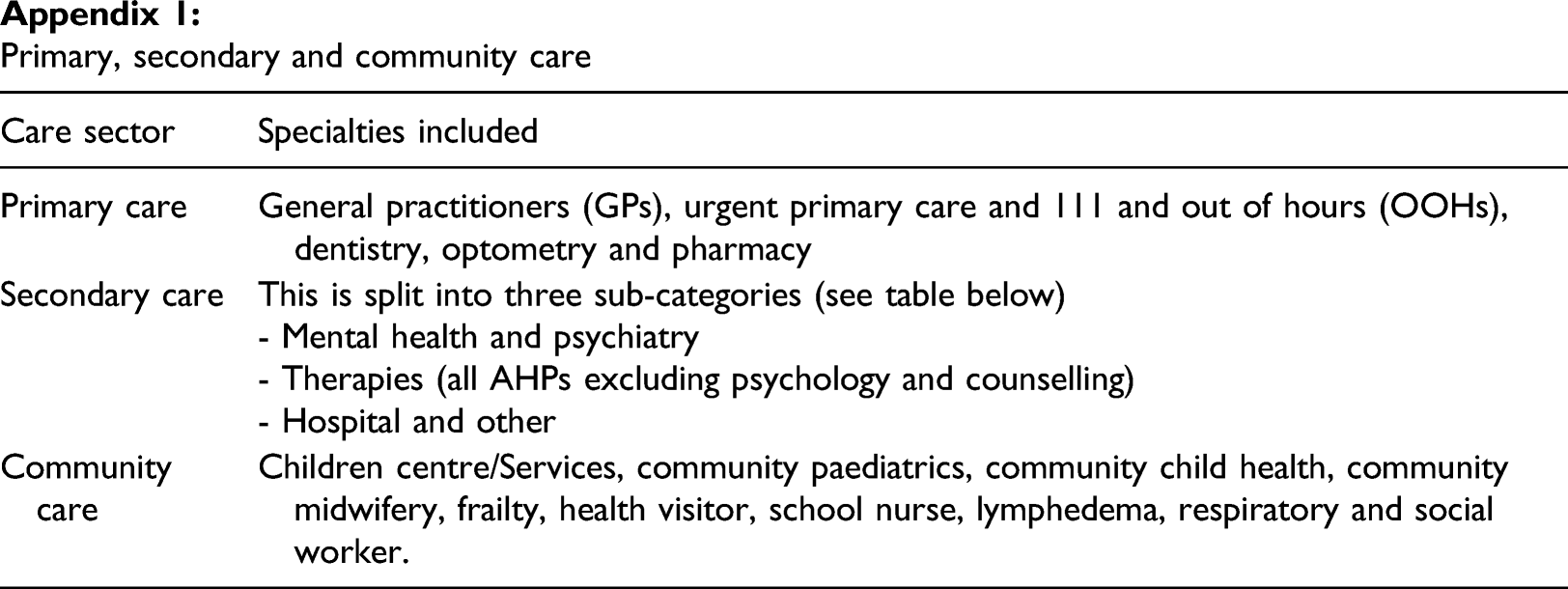
Care sector
Specialties included
Primary care
General practitioners (GPs), urgent primary care and 111 and out of hours (OOHs), dentistry, optometry and pharmacy
Secondary care
This is split into three sub-categories (see table below)
- Mental health and psychiatry
- Therapies (all AHPs excluding psychology and counselling)
- Hospital and other
Community care
Children centre/Services, community paediatrics, community child health, community midwifery, frailty, health visitor, school nurse, lymphedema, respiratory and social worker.
Appendix 2
Secondary care sub-categories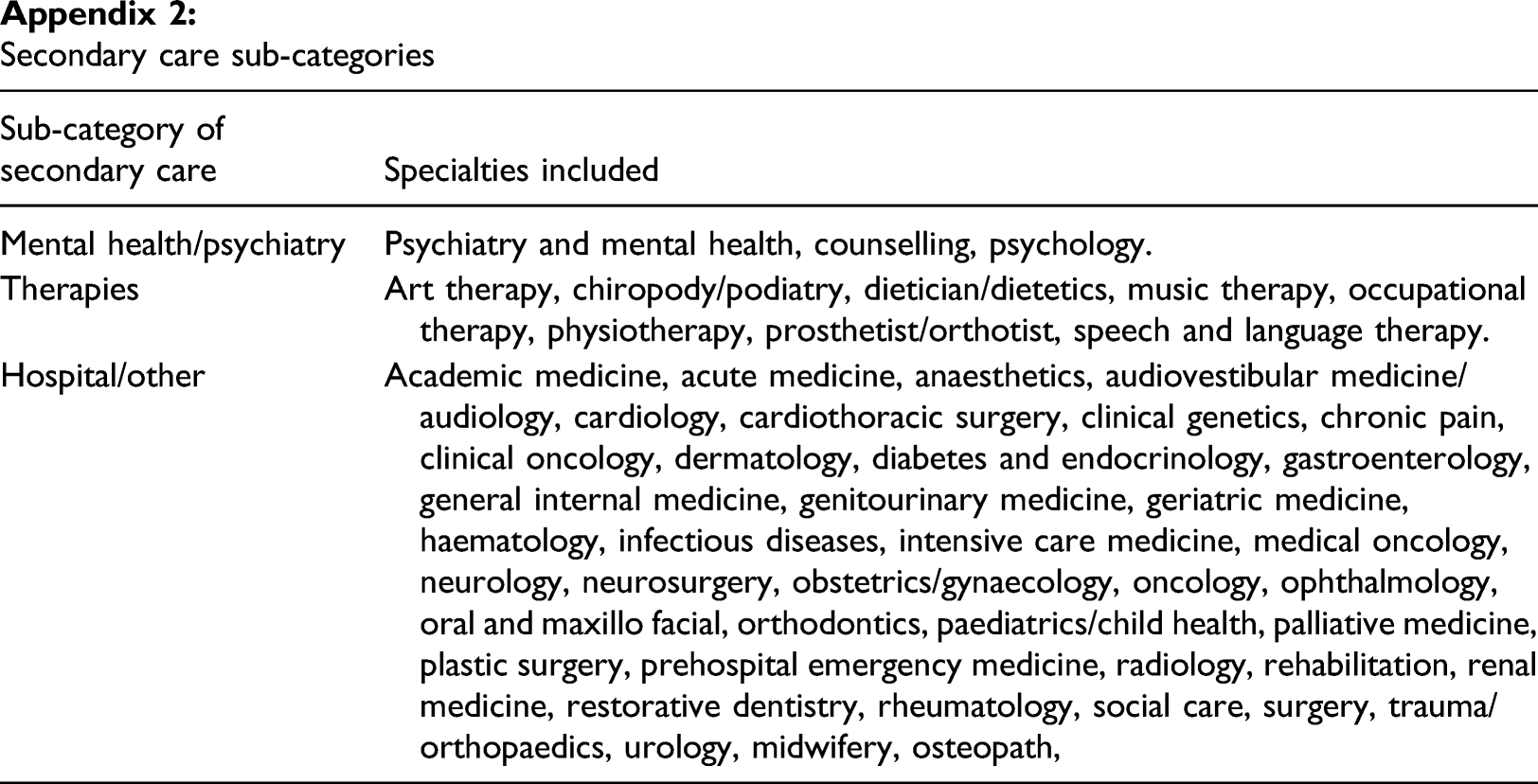
Sub-category of secondary care
Specialties included
Mental health/psychiatry
Psychiatry and mental health, counselling, psychology.
Therapies
Art therapy, chiropody/podiatry, dietician/dietetics, music therapy, occupational therapy, physiotherapy, prosthetist/orthotist, speech and language therapy.
Hospital/other
Academic medicine, acute medicine, anaesthetics, audiovestibular medicine/audiology, cardiology, cardiothoracic surgery, clinical genetics, chronic pain, clinical oncology, dermatology, diabetes and endocrinology, gastroenterology, general internal medicine, genitourinary medicine, geriatric medicine, haematology, infectious diseases, intensive care medicine, medical oncology, neurology, neurosurgery, obstetrics/gynaecology, oncology, ophthalmology, oral and maxillo facial, orthodontics, paediatrics/child health, palliative medicine, plastic surgery, prehospital emergency medicine, radiology, rehabilitation, renal medicine, restorative dentistry, rheumatology, social care, surgery, trauma/orthopaedics, urology, midwifery, osteopath,
Appendix 3
Healthcare professionals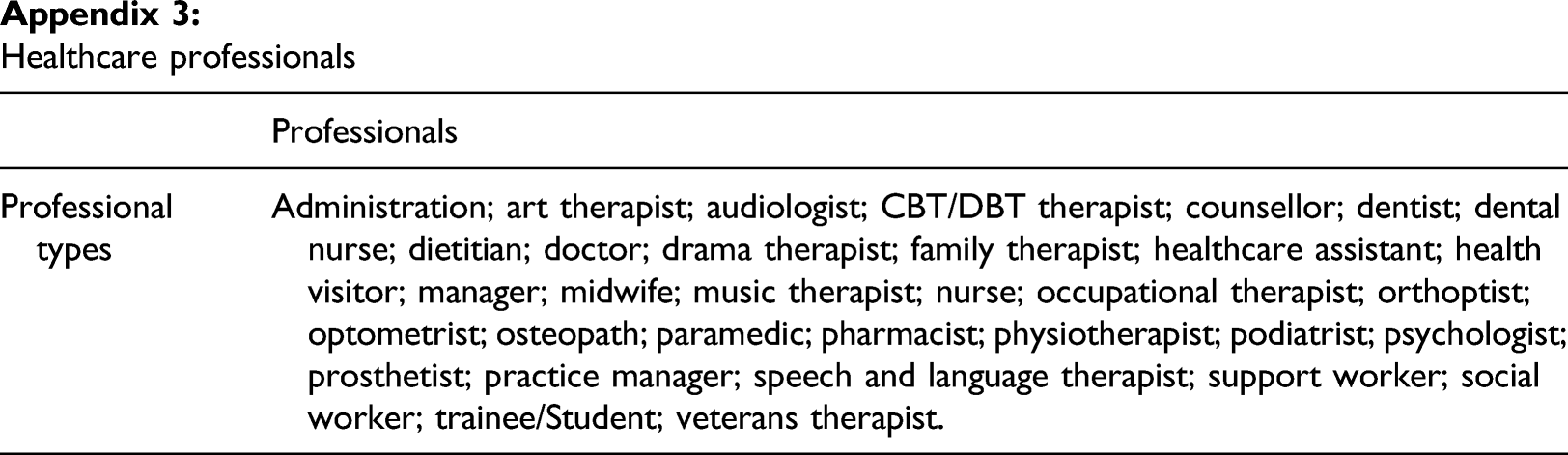
Professionals
Professional types
Administration; art therapist; audiologist; CBT/DBT therapist; counsellor; dentist; dental nurse; dietitian; doctor; drama therapist; family therapist; healthcare assistant; health visitor; manager; midwife; music therapist; nurse; occupational therapist; orthoptist; optometrist; osteopath; paramedic; pharmacist; physiotherapist; podiatrist; psychologist; prosthetist; practice manager; speech and language therapist; support worker; social worker; trainee/Student; veterans therapist.
