Abstract
Background:
The SARS-CoV-2 pandemic has had a significant impact on healthcare delivery. As resources are reallocated, surgery for benign conditions such as gallstone disease is often given low priority. We do not know how this has affected the risk of patients with uncomplicated gallstone disease to develop acute cholecystitis, biliary pancreatitis, or obstructive jaundice.
Methods:
The study was based on the population-based Swedish Register of Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography. The period prior to the first cases of COVID-19 in Sweden, that is, April 2015–March 2020, was compared to the period April 2020–March 2021 during the pandemic. Stratification was made for factors potentially related to priority decisions.
Results:
Altogether, 78,211 procedures were performed during the period of the study. The ratio of procedures performed during April 2020–March 2021 in the previous 5 years was 0.960 (p = 0.113). The ratio of procedures on patients aged <65 years was 0.945 (p = 0.008), on patients aged 65–80 years was 0.964 (p = 0.423), on patients aged >80 years was 1.336 (p = 0.025), on men was 1.001 (p = 0.841), on women was 0.934 (p = 0.006), on procedures completed laparoscopically was 0.964 (p = 0.190), on procedures completed with open approach was 0.659 (p = 0.044), on acute procedures was 1.218 (p = 0.016), on planned procedures was 0.791 (p < 0.001), on procedures performed for biliary colic was 0.808 (p < 0.001), on procedures performed for acute cholecystitis was 1.274 (p = 0.012), for biliary pancreatitis was 1.192 (p = 0.037), and for obstructive jaundice was 1.366 (p = 0.008).
Conclusions:
The COVID-19 has had a great impact on how gallstone surgery has been organized over the last 2 years. The decreased number of planned procedures probably reflects the reallocation of resources during the pandemic. However, whether the increasing number of acute procedures is the result of postponed planned surgery or a continuation of a long-term trend toward more acute surgery remains unanswered. Further studies are needed to assess and evaluate how this has affected public health and health economics.
Background
The SARS-CoV-19 (COVID-19) pandemic has had an enormous impact on public health worldwide. 1 There are detailed reports on the mortality and morbidity of patients diagnosed with COVID-19, including immediate and long-term outcomes of the disease. The secondary effects of the pandemic, in particular the consequences of the reorganization to meet the immense demand for resources required to manage a large number of patients in need of intensive care, have only partly been described. To cope with the great influx of COVID-19 patients, elective surgical procedures for benign conditions such as uncomplicated gallstone disease and hernia have often been suspended or limited during the pandemic,2,3 whereas great efforts are made to care for patients with potentially life-threatening conditions such as malignancy, cardiovascular disease, and severe trauma.
In most cases, surgery for gallstone disease is performed with the intention to relieve symptoms related to biliary colic in patients with uncomplicated gallstone disease. However, the natural course of gallstone disease is not fully known. Although gallstone disease, in general, is a benign condition, there is a low but not negligible risk of developing serious sequelae, including acute cholecystitis, biliary pancreatitis, acute cholangitis, and obstructive jaundice.4 –6 The prevalence of gallstone disease has been explored in several screening studies,7,8 but there are few studies on the risk of progress from biliary colic to conditions associated with potential morbidity and mortality. It is thus difficult to assess whether a high surgery rate prevents the development of complicated gallstone disease. 9 Indeed, there are indications that a more restrictive strategy toward stepwise selection for cholecystectomy may be beneficial. 10 On the other hand, it is possible that patients who are withheld surgery for gallstone disease develop chronic cholecystitis.
The aims of the present study were to describe how COVID-19 has affected the rate of gallstone surgery and to see whether this has led to a rebound increase in complications secondary to gallstone disease.
Material and methods
The study was based on the Swedish Register of Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography (ERCP), GallRiks. Since 2015 this register has covered more than 90% of all gallstone surgery performed, including cholecystectomy and ERCP. Patient- and procedure-related data, including intraoperative and postoperative complications within 30 days, are prospectively registered. Consent from the patient to participate in register-based research is required for registration in GallRiks. Patients have the right to withdraw their personal data from the register at any time, although that is very rarely the case. 11
The first wave of COVID-19 (April–July 2020) in Sweden was followed by a second wave (October 2020–February 2021) and a third wave (February–May 2021). 12
The period preceding the first cases of COVID-19 in Sweden, that is, April 2015–March 2020, was compared with the pandemic period and presented as bar diagrams. The ratio of procedures performed during April 2020–March 2021was compared with the mean number of procedures performed the previous five years, stratifying for sex, age, acute and elective surgery, indication for surgery, surgical approach, finding of chronic cholecystitis, and postoperative complications and mortality.
Data on waiting time to surgery were obtained from the Swedish Association of Local Authorities and Regions. 13
The study was approved by the Swedish Ethics Review Authority (2021-02843).
Results
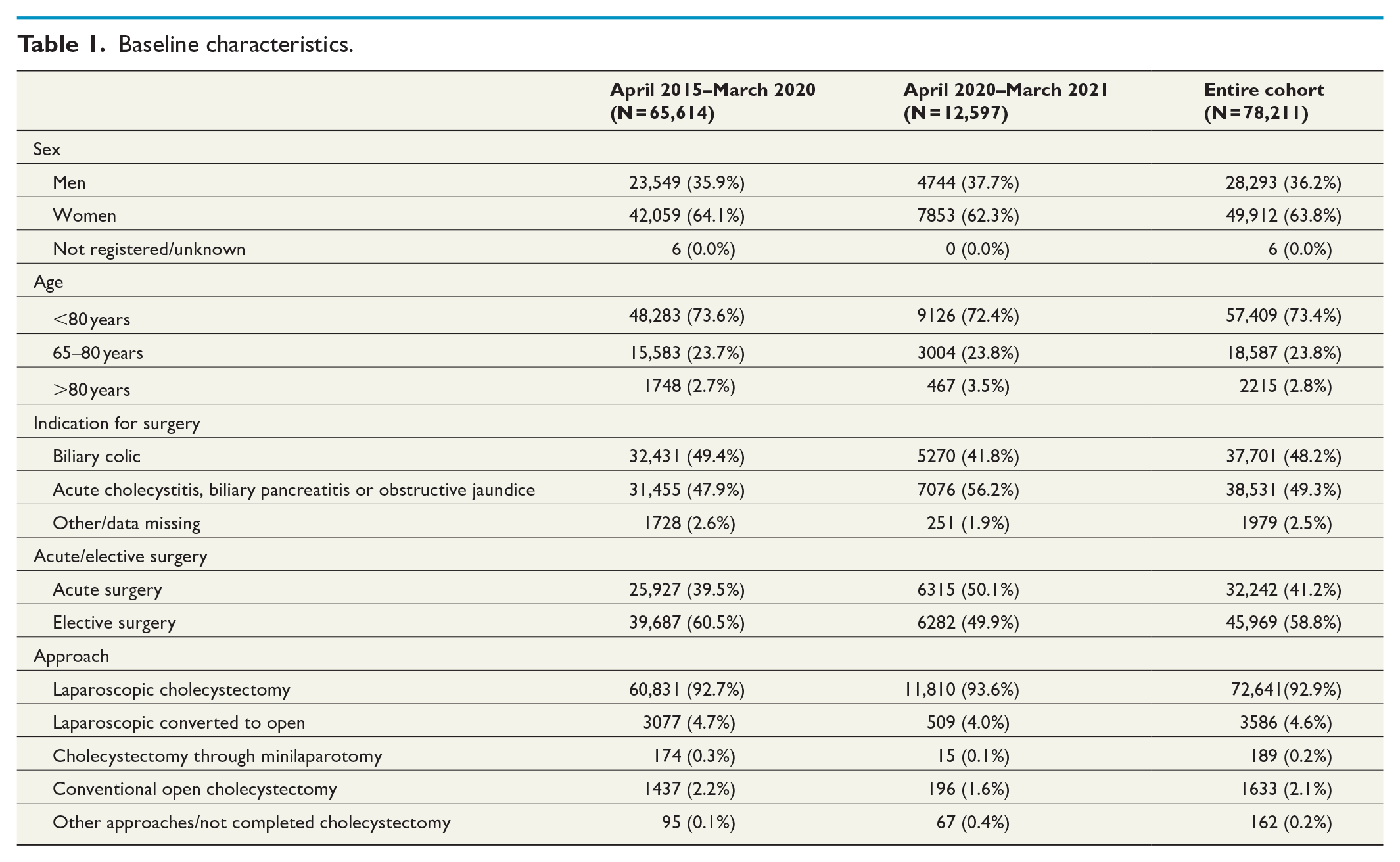
Baseline characteristics are presented in Table 1. The ratios of the number of procedures performed during April 2020–March 2021 to the mean annual number of procedures performed during April 2015–March 2020 are presented in Table 2. The total number of cholecystectomies carried out during the period of the pandemic versus the mean number of procedures performed before the pandemic are presented in Figs 1 and 2. During the pandemic, the surgery rate in patients aged ⩾80 years and the rate of acute cholecystectomies increased significantly, whereas the surgery rate for patients below 65 years, women, converted laparoscopic cholecystectomy, elective procedures, and procedures performed for biliary colic as sole indication decreased significantly. The trend toward an increasing number of acute procedures was, however, seen already before the onset of the pandemic (Fig. 2). When stratifying for indication for surgery, the differences between men and women were very small (Table 2).
Baseline characteristics.
Ratio of procedures performed during the pandemic (April 2020–March 2021) to mean annual number of procedures performed before the pandemic (April 2015–March 2020).
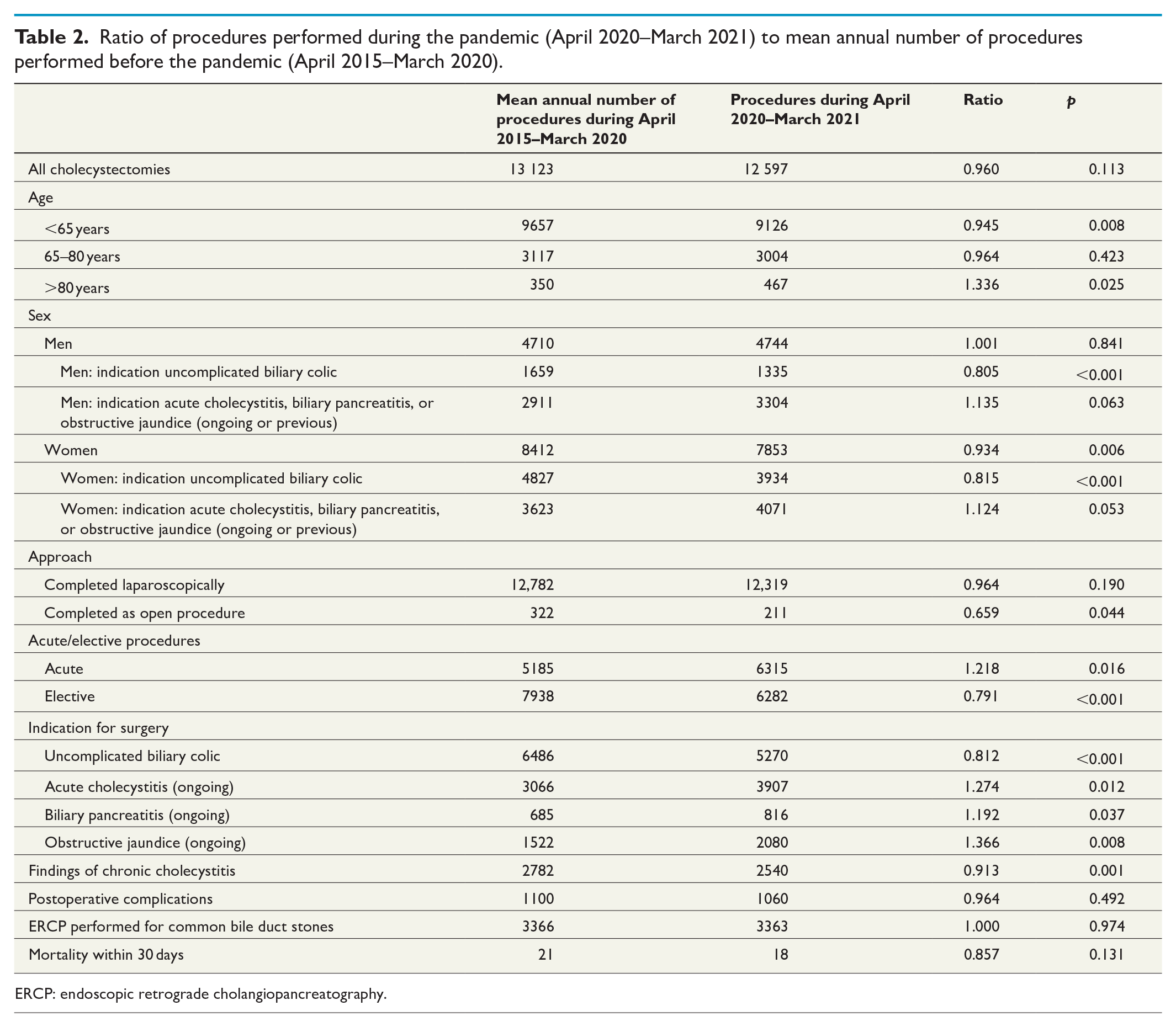
ERCP: endoscopic retrograde cholangiopancreatography.
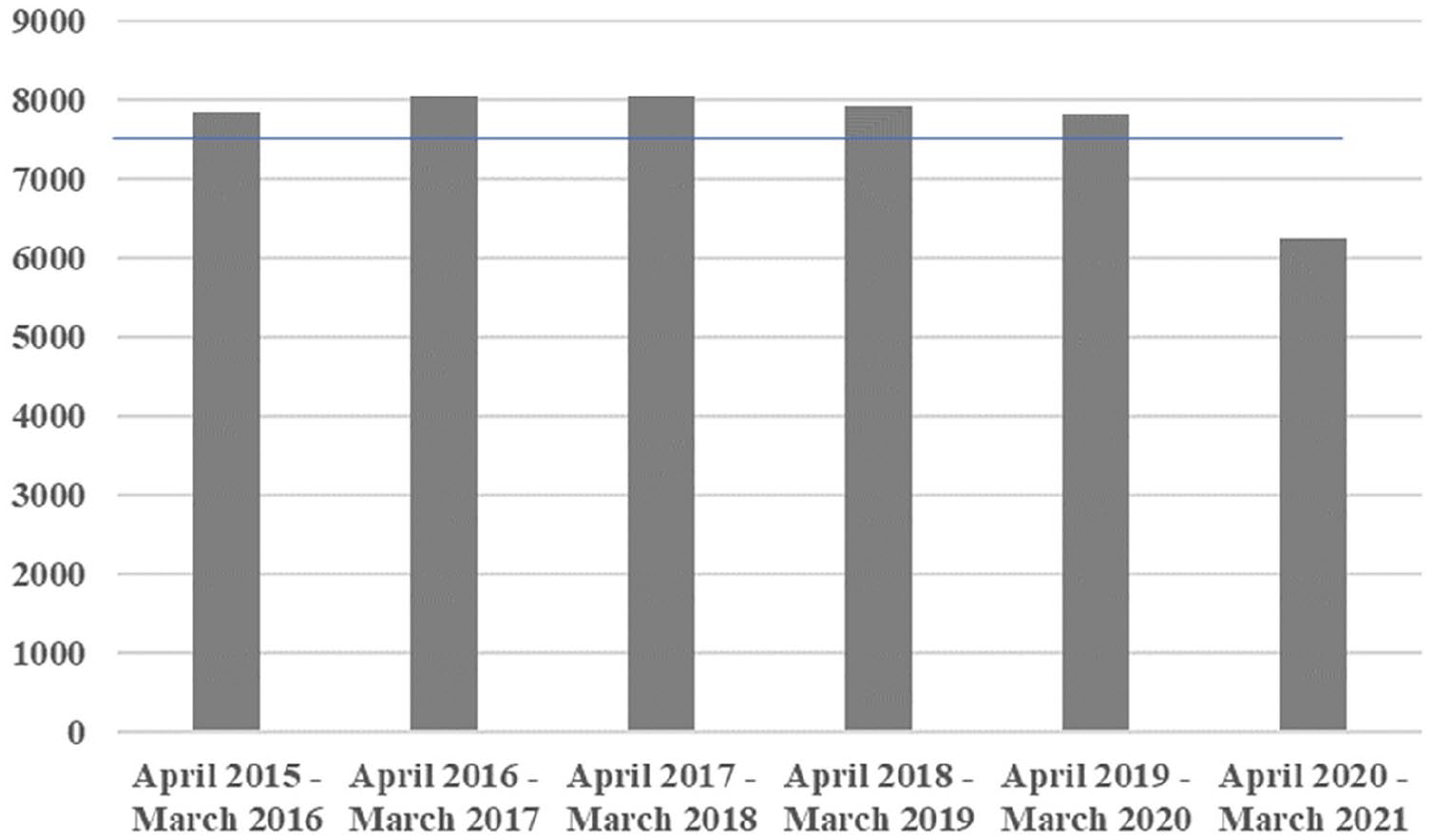
Planned procedures carried out at 2015–2020. The blue line indicates the mean annual number of procedures performed.
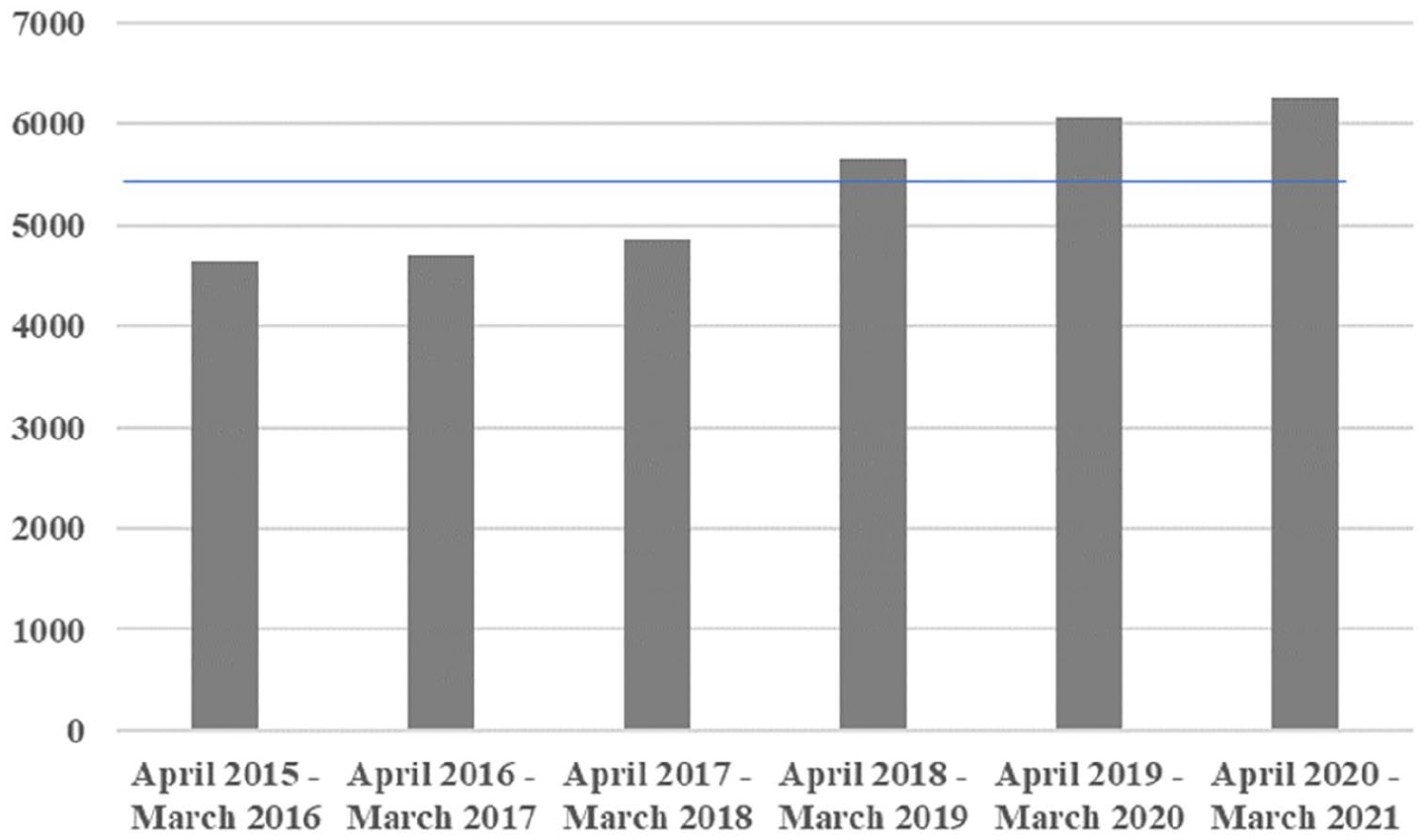
Emergency procedures carried out at 2015–2020. The blue line indicates the mean annual number of procedures performed.
According to the Swedish Association of Local Authorities and Regions, there were 567 (79%) of 714 patients undergoing planned cholecystectomy within 90 days after decision on surgery in January 2020. In July 2020, January 2021, and July 2021, the percentages undergoing surgery within 90 days were 279/316 (88%), 251/333 (75%), and 194/203 (96%).
Discussion
A rapid decrease in the number of procedures performed for uncomplicated gallstone disease was seen during the first wave of the COVID-19 pandemic. The number of patients undergoing cholecystectomy decreased by more than one-third during April 2020. During the months following the decrease, a very moderate increase in the number of procedures performed for acute cholecystitis, biliary pancreatitis, and obstructive jaundice were seen. This increase may partly be explained by a rebound mechanism caused by an increase in gallstone-related complications in patients who have had to wait too long for surgery. It could also reflect a long-term trend toward an increased tendency to perform surgery on these indications. There was a moderate increase in cholecystectomies performed as acute procedures during the pandemic. The lack of change in surgery rate in men and the decreased rate in women is explained by the fact that surgery for uncomplicated gallstone disease is more common in women compared to men. 14
Over the last decade, surgery for gallstone disease has been more common in octogenarians. 15 This is probably due to an increased life expectancy in the population as well as a lower threshold for surgery in the elderly and frail. 16 This trend persisted without interruption during the pandemic, even though lockdown and limitation of contacts are considered more imperative for the elderly (Fig. 2). There is a relative preponderance of complicated gallstone disease in patients aged over 80 years, which could explain why urgent surgery is prioritized in this group. The number of procedures carried out for obstructive jaundice increased during the pandemic, which may be explained by an accumulated group of patients with stones migrating from the gallbladder to the common bile duct or by an increasing percentage of common bile duct stones being detected intraoperatively. There was, however, no increase in the number of ERCPs performed for common bile duct stones.
At the start of the COVID-19 pandemic, a large number of operations were expected to be canceled due to a change in priorities. 17 However, although a large number of procedures were postponed during the first 2 months, there was only a minor subsequent increase in the rate of emergency procedures. Nevertheless, the accumulated number of patients in need of elective surgery may be expected to increase due to the reduced number of planned procedures during the first 2 months of the epidemic. Efforts have been made to catch up with the need for gallstone surgery during 2021, but there are no data on the number of patients suffering from symptomatic gallstone disease who are still waiting for surgery.
According to the Swedish Association of Local Authorities and Regions, the number of patients on the waiting list did not increase substantially during the pandemic. The data from 2021 are, however, incomplete. It is thus difficult to assess whether the pandemic has affected the number of patients waiting for planned gallstone surgery.
During the first year of the pandemic, concerns were raised about the possible mechanism of SARS-CoV-2 transmission through aerosols created in the operation room during laparoscopic procedures. 18 Later studies, however, showed that this concern to be exaggerated. Laparoscopic cholecystectomy was therefore recommended as the treatment of choice for acute cholecystitis by several European surgical societies, even during the ongoing pandemic. 19 A decrease in the number of cholecystectomies completed with open technique was seen during the pandemic, but this could have been the end of a long-term trend of abandoning open methods.
The data presented here could be extrapolated to most Western countries, although the external validity to some extent is limited by conditions specific for Sweden. The lockdown has not been as extensive in Sweden as in most other European countries. This may have affected the burden on the healthcare system as well as the readiness to reallocate resources. Furthermore, the majority of units where gallstone surgery is performed are part of the public healthcare system, which may also have affected the resilience of the healthcare system.
There may have been patients suffering from gallstone-related complications during the pandemic, which were not treated surgically. Since only surgical and endoscopic procedures are reported to GallRiks, we have no data on patients with acute cholecystitis treated with cholecystostomy or patients with biliary pancreatitis or obstructive jaundice that are managed conservatively. The present study may thus have underestimated the impact of the pandemic on the management of patients with complicated gallstone disease. 20 There was, however, no increase in the complication rate or postoperative mortality (Table 2).
During the beginning of the pandemic, there was a great fear of an increase in the incidence of secondary complications to the gallstone disease when planned procedures were postponed. The increase in the number of acute procedures may to some extent reflect this backlash effect. There was, however, a trend toward more acute procedures already before the onset of the pandemic (Fig. 2). The increase during the pandemic may thus be a continuation of the same trend.
In summary, the COVID-19 pandemic has had a significant impact on how gallstone surgery has been organized over the last 2 years in Sweden. There was only a minor rebound effect resulting in an increase in operations for complicated gallstone disease. Nevertheless, the COVID pandemic has caused a heavy burden on the public healthcare system as patients in need of elective surgery have been withheld treatment. Further studies are needed to assess and to evaluate how this has affected public health and health economics in the long run.
Footnotes
Acknowledgements
The authors thank Dr Peter Cox for language editing.
Author contributions
GS organized the study and made the analyses. JÖ participated in designing the study and drafting of the manuscript. PR participated in drafting the manuscript and made the figures. LE has the senior responsibility of GallRiks and participated in designing the study and drafting the manuscript. All other co-authors are members of the GallRiks board. They have participated in organizing the GallRiks data and drafting the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
