Abstract
Background and Aims:
The Finnish Hospital Discharge Register data are frequently used for research purposes. The Finnish Hospital Discharge Register has shown excellent validity in single injuries or disease groups, but no studies have assessed patients with multiple trauma diagnoses. We aimed to evaluate the accuracy and coverage of the Finnish Hospital Discharge Register but at the same time validate the data of the trauma registry of the Helsinki University Hospital’s Trauma Unit.
Materials and Methods:
We assessed the accuracy and coverage of the Finnish Hospital Discharge Register data by comparing them to the original patient files and trauma registry files from the trauma registry of the Helsinki University Hospital’s Trauma Unit. We identified a baseline cohort of patients with severe thorax injury from the trauma registry of the Helsinki University Hospital’s Trauma Unit of 2013 (sample of 107 patients). We hypothesized that the Finnish Hospital Discharge Register would lack valuable information about these patients.
Results:
Using patient files, we identified 965 trauma diagnoses in these 107 patients. From the Finnish Hospital Discharge Register, we identified 632 (65.5%) diagnoses and from the trauma registry of the Helsinki University Hospital’s Trauma Unit, 924 (95.8%) diagnoses. A total of 170 (17.6%) trauma diagnoses were missing from the Finnish Hospital Discharge Register data and 41 (4.2%) from the trauma registry of the Helsinki University Hospital’s Trauma Unit data. The coverage and accuracy of diagnoses in the Finnish Hospital Discharge Register were 65.5% (95% confidence interval: 62.5%–68.5%) and 73.8% (95% confidence interval: 70.4%–77.2%), respectively, and for the trauma registry of the Helsinki University Hospital’s Trauma Unit, 95.8% (95% confidence interval: 94.5%–97.0%) and 97.6% (95% confidence interval: 96.7%–98.6%), respectively. According to patient records, these patients were subjects in 249 operations. We identified 40 (16.1%) missing operation codes from the Finnish Hospital Discharge Register and 19 (7.6%) from the trauma registry of the Helsinki University Hospital’s Trauma Unit.
Conclusion:
The validity of the Finnish Hospital Discharge Register data is unsatisfactory in terms of the accuracy and coverage of diagnoses in patients with multiple trauma diagnoses. Procedural codes provide greater accuracy. We found the coverage and accuracy of the trauma registry of the Helsinki University Hospital’s Trauma Unit to be excellent. Therefore, a special trauma registry, such as the trauma registry of the Helsinki University Hospital’s Trauma Unit, provides much more accurate data and should be the preferred registry when extracting data for research or for administrative use, such as resource prioritizing.
Keywords
Introduction
In Finland, all hospitals and healthcare providers are required to collect and send patient information to the government-regulated national registry (Finnish Hospital Discharge Register (FHDR)) for research and statistics (1).
The FHDR, established in 1967, is among the world’s oldest individual hospital discharge registers covering an entire country (2–4). Data in the FHDR include, for example, a patient’s personal identification code (PIC; which, among other things, includes the patient’s date of birth and information about sex), area of residence, hospital identification number, admission and discharge days, diagnoses, surgical procedures, and discharge destination. Data for FHDR are automatically generated from the information that is put into the patient e-files by a secretary at the unit where the patient is discharged from. There is no need for any specific coding at that point. Once a year, hospitals send the data to the central register, where the data undergo a systematic internal quality check. More than 30 publications have previously validated the FHDR as a source of accurate data with sufficient coverage of patient diagnoses, procedural coding, hospital length of stay (LOS), and external cause of injuries (5–8). Validations have focused mostly on single injuries or disease groups (e.g. coronary heart disease, schizophrenia, bipolar disorder, stroke, hip fracture, pelvic fracture, spontaneous abortion, and glaucoma, among others) but not on severely injured patients with multiple trauma diagnoses (7). Similar validations of national registries focusing on a single injury or disease group have also been published in other Nordic countries (9, 10).
A specific trauma registry is an important tool for evaluating and improving the quality of treatment of trauma patients (11–13). Trauma registry data can serve to monitor and evaluate a hospital’s internal quality; the data derived from a trauma registry can be used to assess the effectiveness of new clinical interventions and modifications of protocols in the treatment of severely injured patients. Trauma registries can also serve to compare the quality/effectiveness of trauma care between hospitals, individual institutions, healthcare regions, or even countries (14, 15).
The trauma registry of the Helsinki University Hospital’s Trauma Unit (TR-THEL), established in 2006, includes all New Injury Severity Score (NISS) >15 trauma patients admitted to the resuscitation bay. The TR-THEL uses NISS rather than Injury Severity Score (ISS) as inclusion criteria because NISS is superior to ISS in predicting mortality after blunt trauma (16). The Helsinki University Hospital is a tertiary trauma center with a catchment area of about 1.8 million. A total of five trained trauma coordinators review and code the data using specialized software within 3 months of admission.
The collected data include parameters for predictive models (patient and injury severity variables, including Abbreviated Injury Scale (AIS; version 2005 update 2008) and WHO’s International Statistical Classification of Diseases and Related Health Problems, 10th revision (ICD-10), process mapping (variables describing care provided), and resource utilization (variables describing the hospital resources needed). All trauma coordinators collecting and feeding in the data have taken the official Association for the Advancement of Automotive Medicine (AAAM)–certified AIS-coding course successfully.
It is essential that a registry has good data coverage and that the data are sufficiently accurate to provide correct information for statistics and research. Thus, we aimed to examine the coverage and accuracy of the FHDR data on severely injured patients. We hypothesized that the FHDR would lack valuable information and that the trauma registry (TR-THEL) would be more accurate. We also aimed to validate the data in our trauma registry (TR-THEL).
Materials and Methods
For this validation study, we included all TR-THEL patients from 2013 with severe thoracic injury (THX; AIS = 3 or higher) (17). We chose this group because we wanted to evaluate a group of patients with multiple injuries in many body regions and often also on both left and right sides of the body (18). Moreover, these patients often receive treatment in the intensive care unit (ICU) and often require several procedures and rehabilitation after primary treatment.
We collected WHO’s ICD-10 (19) diagnostic codes, Nordic Medico-Statistical Committee (NOMESCO) procedural codes (20), ICU LOS, total hospital LOS, survival status (death or alive on discharge), and discharge destination (another hospital, rehabilitation, home, and other) from the TR-THEL, FHDR data, and original patient e-files (the latter served as the gold standard).
One research nurse checked the data first by carefully examining patient e-files. Individual social security numbers (=PIC) served to compare each patient’s FHDR data to the original patient e-files and TR-THEL Excel data.
We initially color coded each difference or missing bit of information. M.H. and T.S. working independently and in consensus then checked every color-coded diagnosis (i.e. difference between the two registries and/or patient e-files) against the original patient e-files and interpreted the reason for any difference/absence. Use of this method also served to identify the correct number of diagnoses, the incorrectly coded diagnoses, and the missing diagnoses as well as their ICD-10 codes for each patient and the entire patient group. We repeated the process with NOMESCO procedural codes, ICU LOS, hospital LOS, survival status, and discharge destination.
We determined the coverage of diagnoses by comparing the total number of diagnoses found in the FHDR or the TR-THEL to the number of trauma diagnoses identified in the patient e-files and radiographic reports. We determined the accuracy of the data by comparing the correct diagnostic codes to all diagnoses found. Similarly, we also counted the accuracy and coverage for procedural codes, LOS, survival status, and discharge destination, if appropriate. We report the coverage and accuracy of the FHDR and TR-THEL data as percentages with 95% confidence intervals (CIs). We determined the severity of missing diagnoses by calculating the AIS score for each missing diagnosis (17).
In Finland, the relevant legislation does not require register-based studies to obtain the approval of an ethics committee. However, all register-based studies that utilize confidential medical information, such as patient charts and radiographs, require the approval of the corresponding institution or hospital. The review board of the Helsinki University Hospital approved this study.
Results
We identified 107 patients in the TR-THEL with thoracic AIS ⩾3 (only 4 patients had isolated thoracic injury). The majority of patients were men (77.6%) with a mean age of 49 years (interquartile range (IQR): 30–64 years); nine (8.4%) patients died within the first 30 days. The most common mechanisms of injury were fall from height and motor vehicle accident; 66.4% of the patients were also polytrauma patients (AIS > 2 in two different body regions) (21, 22). Table 1 shows the patient demographics.
Patient demographics and mechanism of injury.
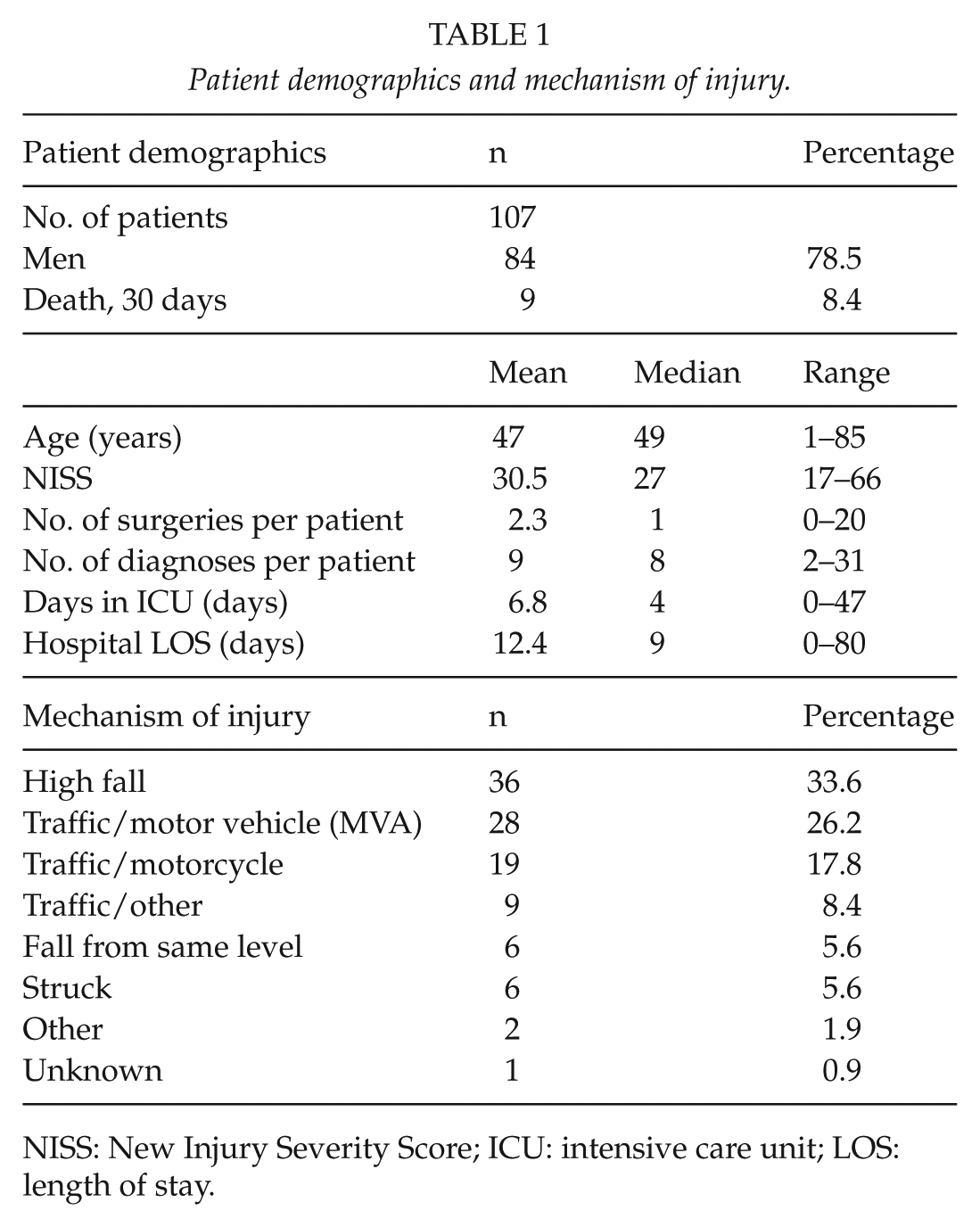
NISS: New Injury Severity Score; ICU: intensive care unit; LOS: length of stay.
Diagnoses
These 107 patients had 965 trauma diagnoses based on a review of the medical records. Interpretations of the different diagnoses and their consensus coding appear in Fig. 1. The number of diagnoses per patient appears in Fig. 2. From the FHDR data, we could identify 632 of these diagnoses and from TR-THEL, 924 of these diagnoses. The FHDR data contained 10 (1.0%) diagnoses that did not exist; the TR-THEL contained 5 (0.5%). Moreover, 170 (17.6%) diagnoses were completely absent from the FHDR but only 41 (4.2%) from the TR-THEL. Out of these 170 missing diagnoses 3 were coded critical (AIS = 5), 7 severe (AIS = 4), 39 serious (AIS = 3), and 121 moderate (AIS = 2) or minor (AIS = 1). Another 163 diagnoses were missing from the FHDR either because the diagnosis was coded only as one sided, even though the injury was bilateral, or the diagnosis was coded not separately, but together under certain injury codes that include several different injuries. For example, ICD-10 S32.7 (multiple fractures of the spine and pelvis) can have several fractures coded under that same code. In the TR-THEL, every fracture is coded separately due to the requirements of AIS coding. Out of these 163 diagnoses, only 1 was coded critical, 3 were serious, 23 severe, and 136 moderate or minor.
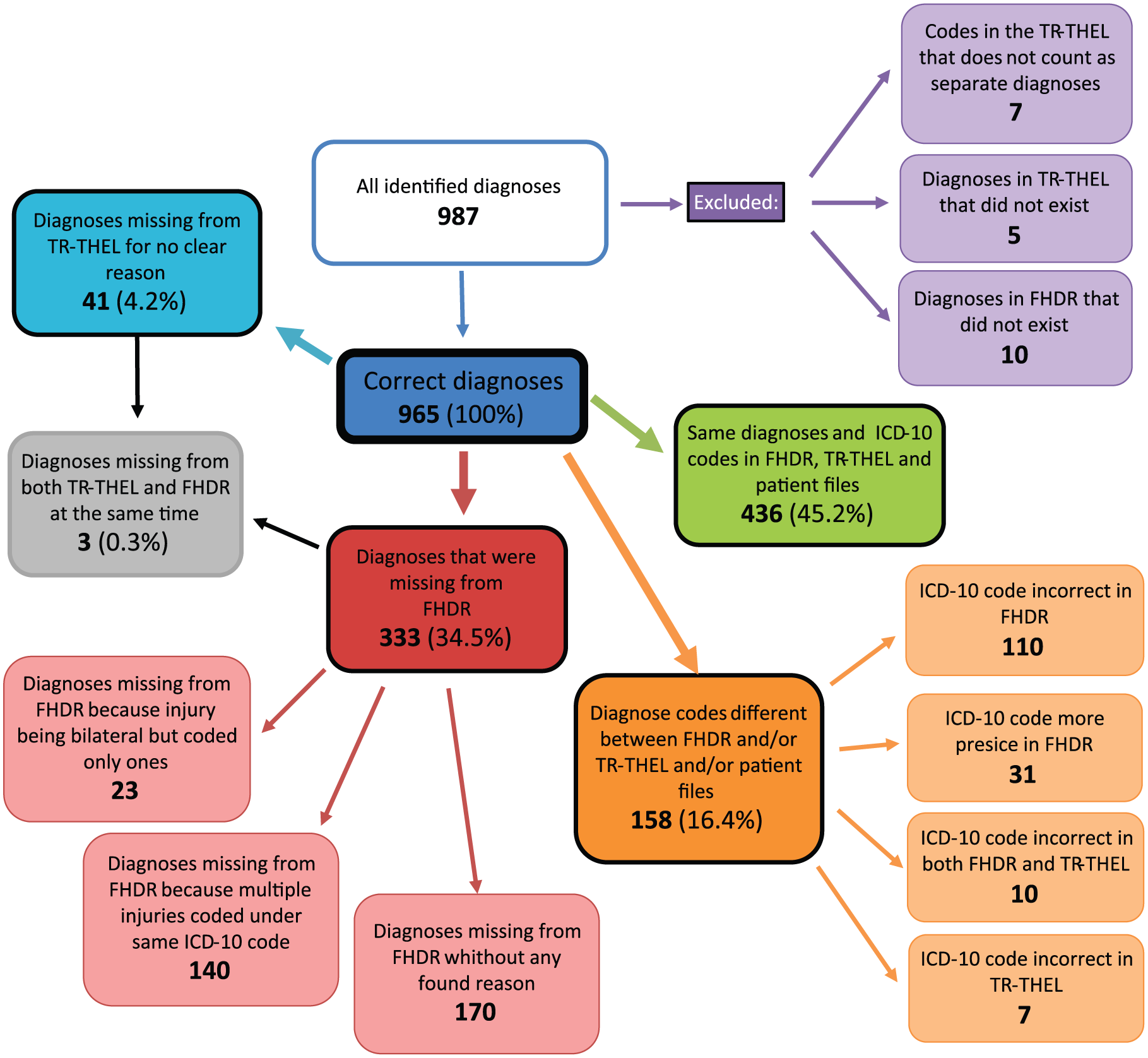
All diagnoses of all patients.
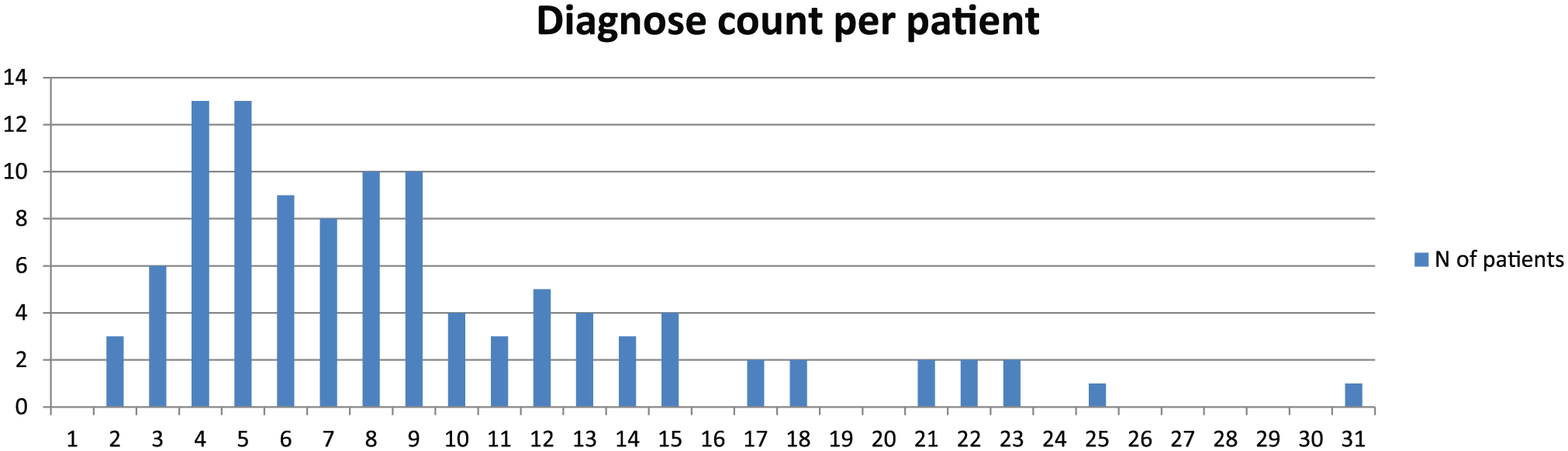
Number of diagnoses per patient.
Comparison of the FHDR and the TR-THEL showed that 436 (45.2%) of the diagnoses were exactly the same, but only 7 (6.5%) patients shared exactly the same coding. Injury classification according to ICD-10 appears in Table 2 among the distribution of missing injuries in different body regions. Table 3 shows the severity of missing diagnoses according to the AIS classification of injuries. In addition, 158 diagnoses found in both registries had the same written diagnosis but a different ICD-10 coding. Comparison to the original patient files revealed that the ICD-10 code was incorrect in 120 (18.7%) diagnoses identified in the FHDR and 17 (1.8%) in the TR-THEL. For 31 codes, the FHDR ICD-10 code was more accurate than the ICD-10 code in the TR-THEL, although both codes could be considered correct (e.g. S02.2 (nasal bone fracture) and S02.20 (nasal bone fracture; closed) are both correct, but the latter is more detailed).
The number of different diagnoses and the count/number and reason for missing diagnoses.
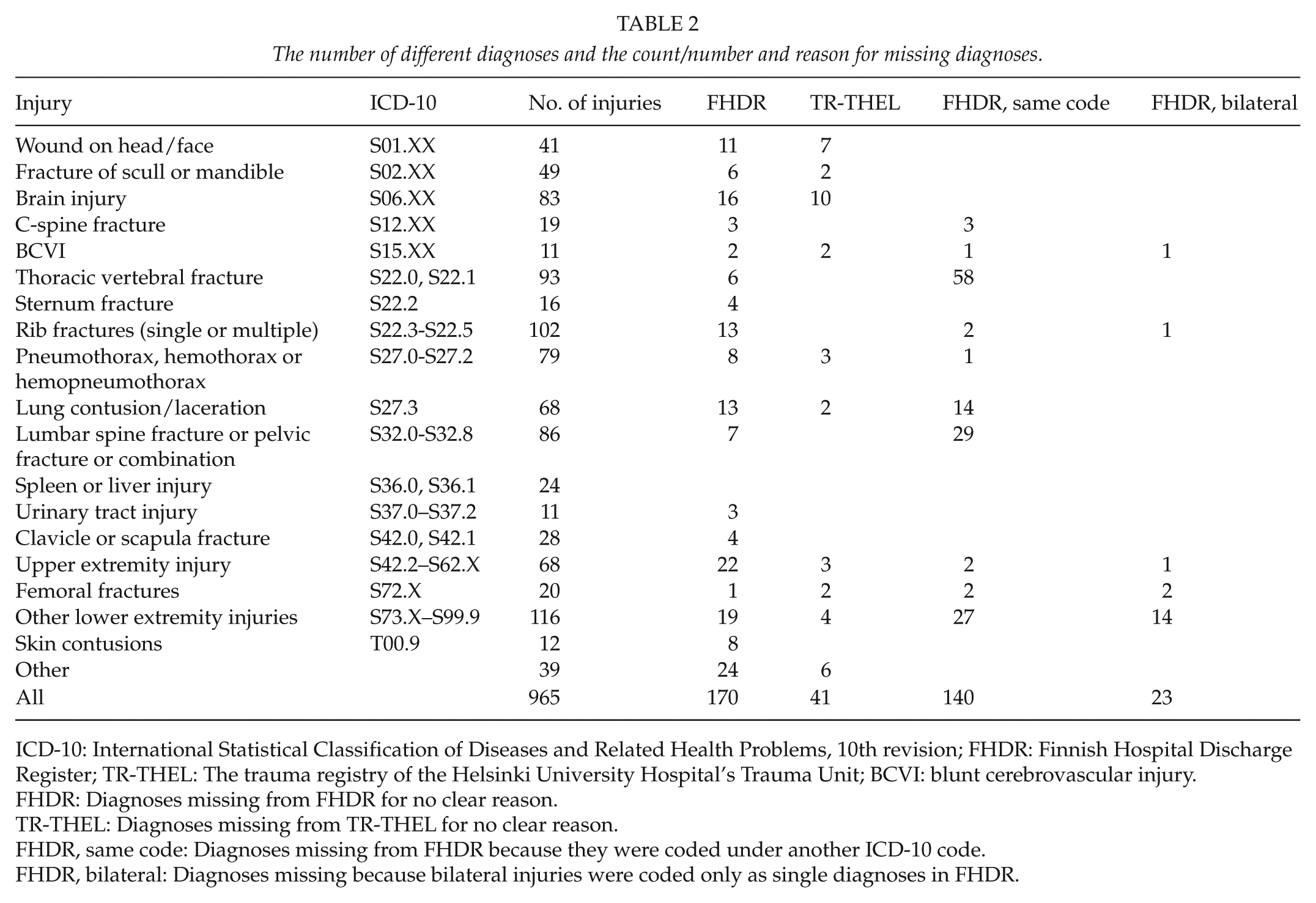
ICD-10: International Statistical Classification of Diseases and Related Health Problems, 10th revision; FHDR: Finnish Hospital Discharge Register; TR-THEL: The trauma registry of the Helsinki University Hospital’s Trauma Unit; BCVI: blunt cerebrovascular injury.
FHDR: Diagnoses missing from FHDR for no clear reason.
TR-THEL: Diagnoses missing from TR-THEL for no clear reason.
FHDR, same code: Diagnoses missing from FHDR because they were coded under another ICD-10 code.
FHDR, bilateral: Diagnoses missing because bilateral injuries were coded only as single diagnoses in FHDR.
Severity of missing diagnoses according to the AIS classification.
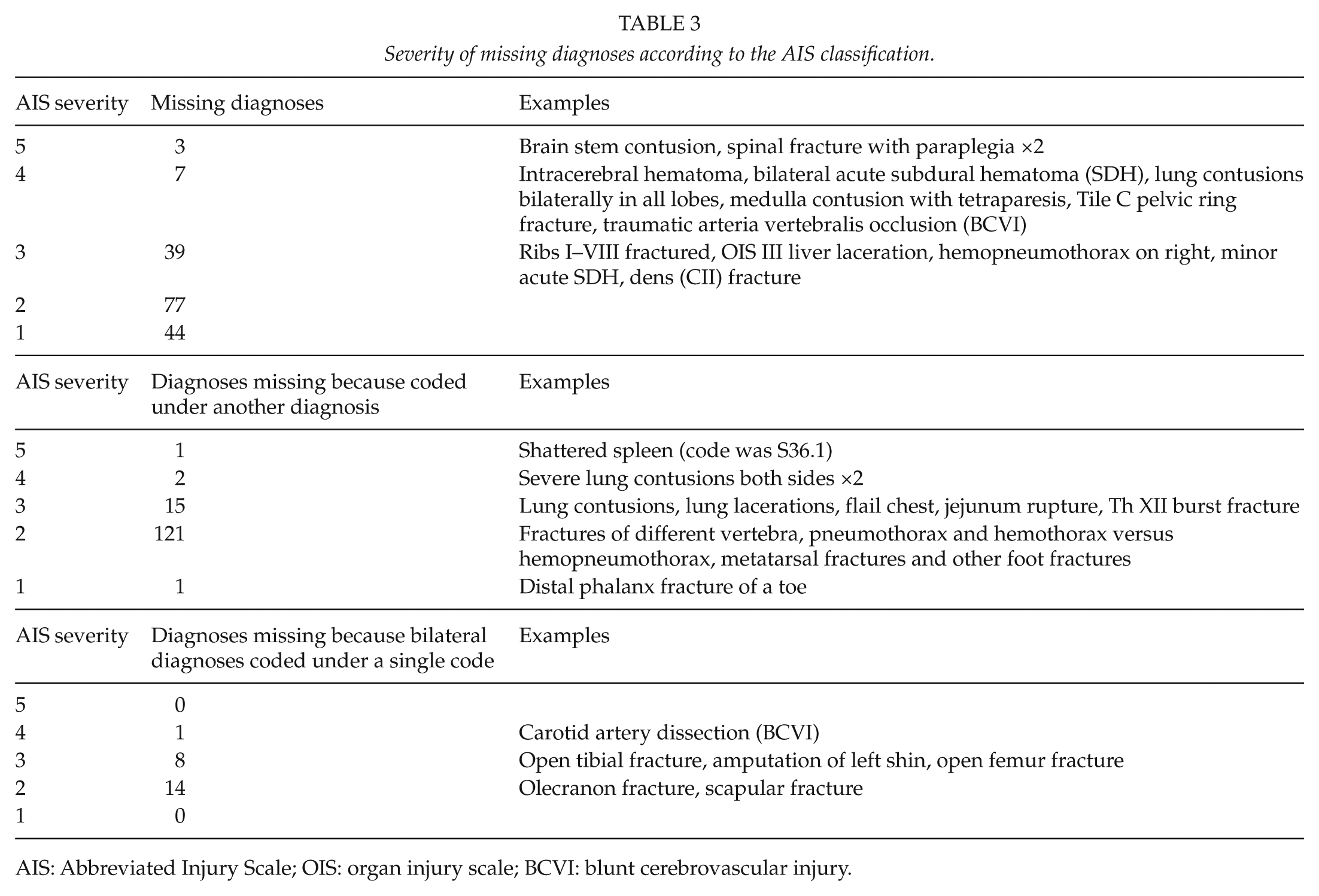
AIS: Abbreviated Injury Scale; OIS: organ injury scale; BCVI: blunt cerebrovascular injury.
A total of 333 (34.5%) diagnoses were missing from the FHDR and 41 (4.2%) from the TR-THEL. Of these diagnoses, three were missing from both registries at the same time. The coverage of the FHDR and TR-THEL for diagnoses in severely injured patients is 65.5% (95% CI: 62.5%–68.5%) and 95.8% (95% CI: 94.5%–97.0%), respectively. The accuracy of the FHDR was 73.8% (95% CI: 70.4%–77.2%) and of the TR-THEL 97.6% (95% CI: 96.7%–98.6%).
Procedural Codes
Based on the patient records, we identified 249 surgical procedures performed on these 107 patients. We did not include minor procedures, such as wound suturing in the emergency room (ER) or any procedure performed bedside in the ER, ICU, or ward, but did include operations performed in an angiography suite or operating room (OR). Of these 249 operations, 191 were coded exactly the same in both registries. In addition, 40 (16.1%, 95% CI: 11.5%–20.6%) operations were missing from the FHDR and 19 (7.6%, 95% CI: 4.3%–10.9%) from the TR-THEL; 11 operations were missing from both registries, all on the same patient. One operation listed in the FHDR never occurred (was never performed on that particular patient); the TR-THEL contained no such error. A total of eight operations were incorrectly coded in the FHDR and two in the TR-THEL. However, these 10 errors were considered insignificant because the magnitude and importance of the operation remained unchanged (Fig. 3).
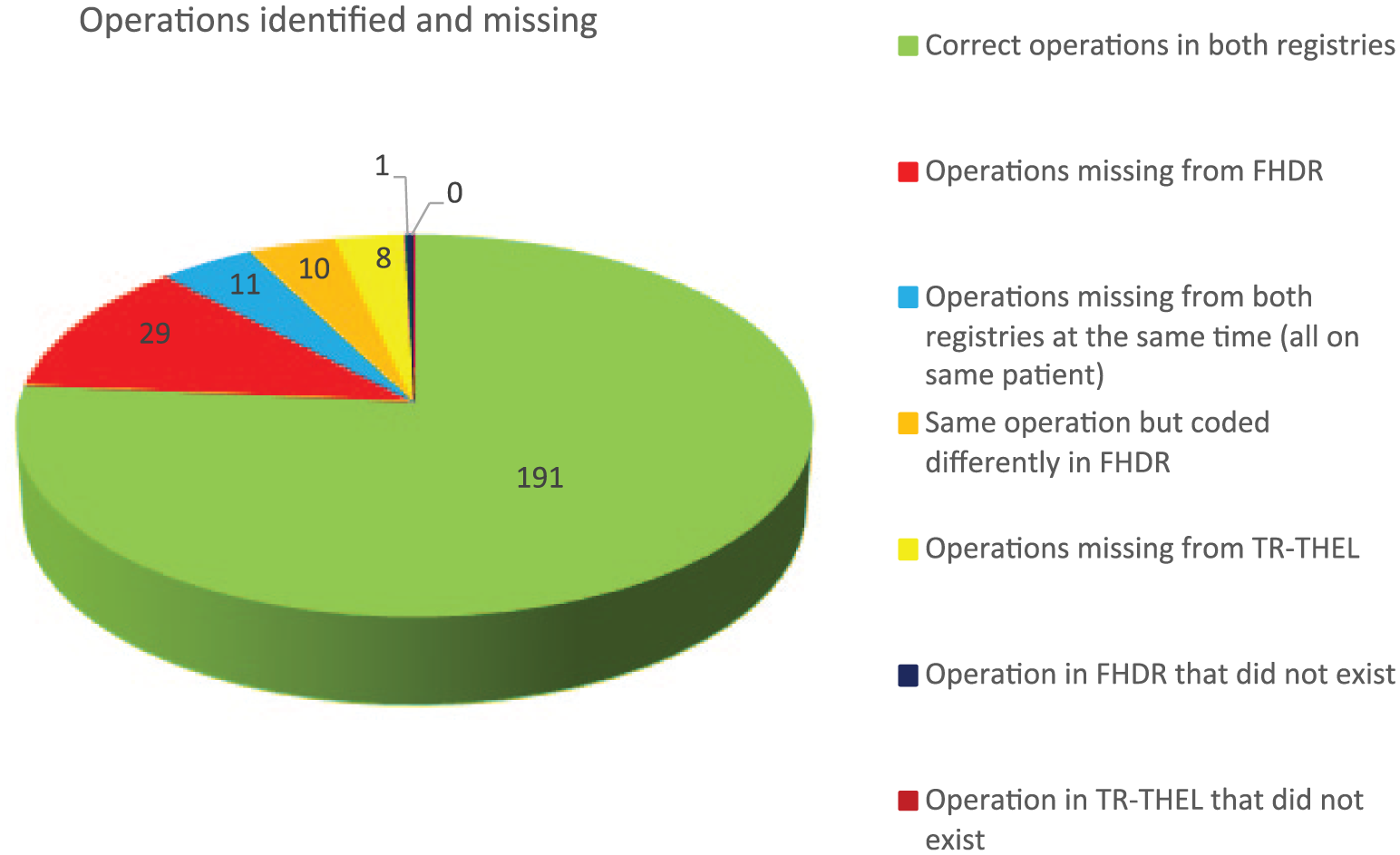
The number of operations.
The coverage of the FHDR and the TR-THEL for operations (procedural coding) was 83.9% (95% CI: 79.4%–88.5%) and 92.4% (95% CI: 89.1%–95.7%), respectively. The accuracy for operations in the FHDR and the TR-THEL was 95.5% (92.7%–98.4%) and 99.1% (97.9%–100.3%), respectively.
Icu Los and Hospital Los
The data for every patient in both registries contained all the information needed for LOS calculation, so the coverage was 100%. Even so, the FHDR contained five false discharge dates; all these patients were transferred to another hospital within the same hospital district. The TR-THEL contained two inaccurate discharge dates, and both were misinterpretations by the trauma coordinators. ICU days were correct in both registries. Because electronic patient files automatically calculate LOS, these data were correct except on those patients with incorrect discharge dates. The accuracy of hospital LOS in the FHDR was 95.3% (95% CI: 91.3%–99.3%) and in the TR-THEL 98.1% (95% CI: 95.6%–100.7%). The accuracy of ICU days listed in both registries was 100%.
Discharge Destination and Survival Status
The FHDR contained incorrect discharge destinations for 13 patients and the TR-THEL for 3 patients. Thus, the accuracy of the discharge destinations in the FHDR and TR-THEL was 87.9% (95% CI: 81.7%–94.0%) and 97.2% (95% CI: 94.1%–100%), respectively. The survival status of every patient was correct in both registries.
Discussion
As far as we know, no studies have previously evaluated the accuracy and coverage of FHDR data on severely injured patients with multiple trauma diagnoses. Nor have any studies in the international literature assessed the accuracy and coverage of the data in other national discharge registers. The FHDR as well as other discharge registers are widely used for epidemiological research, thanks to the important information for trauma and disease (7, 9, 10).
The accuracy of the FHDR has been studied extensively and proved to be good or excellent in cases involving a single injury or disease (7). In this study, we aimed to evaluate the accuracy and coverage of the FHDR in severely injured patients with multiple trauma diagnoses. At the same time, we assessed whether a specific trauma registry can provide more accurate data for research and administrative purposes than the FHDR can. Several previous studies have confirmed the value of trauma registries (11–13, 23), so comparing these two different registries seems reasonable in order to validate the FHDR with severely injured patients.
We found that the accuracy of diagnoses of severely injured patients in the FHDR is quite poor (73.8%), as is the coverage (65.5%), though part of this inaccuracy is due to limitations in the ICD-10 coding (bilateral injuries, diagnoses covering several injuries). A special trauma registry such as the TR-THEL can provide much more accurate (97.6%) diagnostic data, and the coverage (95.8%) of diagnoses is also far more complete. Moreover, the FHDR has no coding or identification method for severely injured patients, so identifying them from the FHDR database alone is impossible. However, the coverage and accuracy of surgical procedures performed on severely injured patients were good in the FHDR (83.9% and 95.5%) but excellent in the TR-THEL (92.4% and 99.1%); thus, when describing surgical trends, these registries can prove useful.
It should be remembered that the purpose of the two registries is somewhat different. The FHDR is mostly for administrative interest and less for scientific use. The purpose of a special trauma registry, such as TR-THEL, is to gather information also for administrative use but mostly for improving care protocols, getting information about patient outcomes, comparing results between centers, and for accurate scientific evaluations of specific patient groups. A recent systematic review by Sund (7) reported that most studies examined the validity of the FHDR in cases involving vascular disease (12 studies), mental disorders (10 studies), or various isolated injuries (6 studies). Most of these studies concluded that the quality of the FHDR was good or satisfactory, yet none of the studies found the quality of the FHDR to be poor.
Our results of the FHDR’s fairly poor accuracy and coverage of diagnoses among severely injured patients can partly be explained by the limitations of coding in the ICD-10. Several ICD-10 codes include multiple trauma diagnoses under a single code (S22.1 = multiple fractures of the thoracic spine and S32.7 = multiple fractures of the lumbar spine and pelvis), whereas the TR-THEL (like several other specific trauma registries) also uses AIS coding of injuries and, therefore, codes every fracture separately (i.e. more accurately). In addition, some ICD-10 codes are very similar, so coding physicians can merge them (S27.0, S27.1, and S27.2 = traumatic pneumothorax, traumatic hemothorax, and traumatic hemopneumothorax). Furthermore, some codes are similar and include multiple fractures (S92.2 = fracture of other tarsal bones and S92.7 = multiple fractures of the foot). A separate extra/supplementary ICD-10 code covers bilateral injuries (ZB0.2), but it is so little known that it is seldom used; thus, even severe bilateral injuries may be impossible to find from the FHDR unless the injury is coded twice with the same ICD-10 trauma code. In TR-THEL, every diagnose, also when bilateral, is coded separately, so, for example, bilateral femoral midshaft fracture will have two identical diagnose codes (S72.3 and S72.3), but in FHDR data, this bilateral injury might be coded only ones.
When evaluating the importance of missing diagnoses, one must consider their severity and consequences to the patient. In our study, according to AIS-coding system, only 76 (22.8%) of 333 missing diagnoses were considered serious, severe, or critical, and only 4 diagnoses were critical; 212 (63.7%) of the missing diagnoses were considered moderate and 45 (13.5%) minor.
One important aspect is the role of the person coding the information to the registry. There is no specific trained coder for FHDR information: physicians are responsible for setting the diagnoses and procedural codes, and secretaries fill in the codes to the system according to the information provided by the physicians. When treating severely injured patients, it is possible that some of the many diagnoses are coded wrong or some of the diagnoses are missed in the beginning because of more urgent priorities in treating patients in the ER. For TR-THEL, however, there are five trained trauma coordinators reviewing patient e-files, feeding in the data, doing the AIS coding, and also searching the patient e-files for all possible injuries that might not have had the ICD-10 diagnose code in the e-files before. This might be one reason why the accuracy and coverage of the diagnose codes are far better in this specific trauma registry.
In this study, the FHDR’s coverage and accuracy in procedural coding (surgical procedures) were good. This finding is in line with those of previous studies from the 21st century (6, 24). One study from 1991 rated FHDR’s accuracy regarding surgical procedures as only 74% (25). We used the TR-THEL data not only to select the patients for our study but also to validate the registry itself. We found the TR-THEL data to be more accurate than the FHDR data, especially not only for diagnoses but also for the other parameters evaluated here. However, both registries are suitable for evaluating hospital and ICU LOS, survival status, and discharge destination.
Our study has several strengths. First, we were able to include over 100 severely injured patients with nearly 1000 diagnoses and 250 procedural codes. Second, we had access to all patient medical records (e-files) and could confirm correct diagnoses against radiographic images and radiology reports, when necessary. Third, two experienced traumatologists (M.H. and T.S.) verified the data independently and then compared their results; if their interpretations varied, they reached consensus by reviewing the patient e-files together.
Our study also has some weaknesses. Our study population came from a single trauma center, which can, therefore, affect the results, even though the Helsinki University Hospital in Töölö, Helsinki, is the largest trauma center in Finland, and other hospitals in Finland have no corresponding trauma registries that include severely injured or polytrauma patients for comparison. We noted that identifying severely injured patients or polytrauma patients from the FHDR alone is impossible. Our study population was also limited to severely injured patients with severe thorax injury. Other patient groups might have shown a different distribution of diagnoses and procedures. However, our patient group is most likely typical of polytrauma patients treated in a university hospital and represents about one-third of all patients in the TR-THEL. Because other university hospitals in Finland are also introducing trauma registries, it would be important to conduct a similar study to determine whether our results are reproducible in other similar institutions.
Conclusion
Although previous studies have shown the accuracy and coverage of the FHDR to be excellent, it does not provide accurate information on severely injured patients with multiple trauma diagnoses and operations. A special trauma registry, such as the TR-THEL, provides much more accurate data and should be the preferred registry when extracting data for research or for administrative use, such as resource prioritizing.
Footnotes
Acknowledgements
We thank Satu Tirkkonen, Pirkko Tonder, and Markku Kytönen for their great work in accurately recording the data for the Helsinki Trauma Registry; Iiu Laitinen for helping with the data handling; and Kirsi Willa for managing the TR-THEL data bank. We thank Stephen Stalter for language revision of this article.
Declaration of Conflict Of Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
