Abstract
Vaccination scholarship focuses on how privilege, individualized choice and ‘intensive’ and ‘natural’ parenthood – often motherhood – lead people to delay or not vaccinate their children. Recently, examining parents’ vaccination responsibilities – and the inequalities in paid employment and unpaid care work underpinning them – has become important to understand COVID-19. This article asks who makes vaccination decisions for their children under the age of five, what COVID-19 vaccine decisions are made and how these decisions are gendered. We draw on interviews with 18 Western Australian heterosexual parents. Tracking the responsibilization of mothers and fathers, we contribute a gendered analysis of vaccine ‘decision work.’ We note that norms of intensive parenting led parents to accept or reject vaccines. Like women, men can engage in and support intensive parenting – especially where vaccines are new or widely discussed, or men are available for care work. Overall, we find some potential for children's COVID-19 vaccination to produce more responsibilized fathers and mothers.
Introduction
The intensification of heterosexual parenting responsibilities and care work during the COVID-19 pandemic has been widely discussed, with scholarship highlighting the burdens of work-from-home arrangements and disruptions to schooling and childcare (Craig & Churchill, 2021; Fuller & Qian, 2021; Otonkorpi-Lehtoranta et al., 2021; Sarker, 2021). This intensification occurred unevenly, anchored in gendered inequalities in relationships, work and lives. While past research focusing on childhood vaccinations has tended to talk about parents’ decision-making, such scholarship generally acknowledges that most parental care work is done by mothers, often without exploring the gendered inequalities that produce mothers as primary decision-makers doing ‘intensive’ parenting, or considering parents’ negotiations of their own and their children's vaccinations (Bianco et al., 2019; Greyson & Bettinger, 2022; Reuben et al., 2020).
In the context of the COVID-19 pandemic in Western Australia (WA), we ask who makes vaccination decisions for children under the age of five, what decisions are made and how such decision-making is gendered. We frame our findings in terms of what we label vaccine ‘decision work,’ that is, (gendered) care work that relates to seeking information on, making decisions about, negotiating and enacting vaccine-related medical decisions. Focusing on neoliberal responsibilization through the lenses of gender, care and inequalities in paid and unpaid work, we base our discussion on 18 in-depth, semi-structured interviews with heterosexual mothers and fathers. We note that ideals and practices of intensive parenting can lead to different vaccine decisions: expert-guided intensive parents happily accept vaccines for their children, while intensive parents concerned with ‘natural’ practices reject them. Here men, as well as women, can engage in and support vaccine decisions based on intensive parenting. This is especially true where vaccines are new, politicized and widely discussed, or men are more available for care work, such as during the COVID-19 pandemic.
Background
Much scholarship on COVID-19 and other vaccinations focuses on mothers’ attitudes, responsibilities and decision-making behaviours, either by design or as a consequence of recruitment, as mothers tend to lead vaccination decisions for their children (Bianco et al., 2019; Greyson & Bettinger, 2022; Reuben et al., 2020). However, fathers can play a significant role in decisions to vaccinate their children (Gilchrist et al., 2021; Rammohan et al., 2012; Torun & Bakırcı, 2006). As noted by McKenzie (2022), fathers’ invisibility in discussions of parenting highlights assumptions underpinning categories such as ‘mother,’ ‘father,’ and ‘parent.’ Studies on vaccination and parenthood mostly employ ‘inclusive’ language or consider parents as cohesive units, and thus often ignore or assume differences between mothers and fathers, without interrogating these differences.
Australian studies comparing mothers and fathers’ attitudes towards vaccinating children have varying results. One quantitative study found no difference between mothers and fathers’ levels of childhood vaccination hesitancy (Chow et al., 2017). Another survey of six countries found that Australian mothers were more hesitant than fathers when considering a future COVID-19 vaccine for their children (Goldman & Ceballo, 2022). It is possible, therefore, that mothers and fathers differ in relation to COVID-19 vaccine decision-making.
In considering parents’ decision-making and potential hesitancy towards vaccinating their children, it is important to acknowledge how individualized responsibility has led to a rise in delay and refusal of childhood vaccines across the Global North. Reich explains that neoliberal ideologies lead people to view economies and governmentalities in terms of ‘competitiveness, self-interest, and decentralization’ (Reich, 2014, p. 682), resulting in the prioritization of the private sector over the public, and justifying cuts to state-funded programmes for children and families (including health) (Steiner & Bronstein, 2017). The neoliberal frame holds that individuals should ‘actively manage the self’ and ‘avoid calculable risk through informed decision making’ (Reich, 2014, p. 682). In this context, parents (re)produce themselves as rational consumers, utilizing available evidence to take responsibility for their children's childcare, education, health and welfare (Sanders & Burnett, 2019; Steiner & Bronstein, 2017). Where divisions of paid and unpaid work are highly gendered, decision-making work falls largely on mothers.
The pressure to be competent, caring and responsible for children's wellbeing is also linked to what Hays (1996, p. 8) terms ‘intensive parenting,’ which is ‘child-centered, expert-guided, emotionally absorbing, labor intensive, and financially expensive,’ and influential in driving vaccination decisions (Damnjanović et al., 2018). Relatedly, the ‘natural, holistic and authentic’ ‘good mother’ who possesses ‘maternal instinct’ is often invoked by vaccine-resistant people, with such identities fostered through breastfeeding, feeding children organic foods and refusing vaccination (Baker & Walsh, 2022; McCabe, 2016; Reich, 2016; Sobo, 2015). While fathers can and do engage in and support these parenting practices (Ward et al., 2017), mothers tend to engage more with such social identities and behaviours (Duggan et al., 2015; Reich, 2020; Smith & Graham, 2019). Responsibilization can thus shape parents’ decisions to vaccinate their children (or not), yet mothers engage most with natural parenting discourses that advocate for non-vaccination (Nguyen et al., 2022; Olusanya et al., 2021; Santibanez et al., 2020).
Past scholarship on vaccination, focusing largely on mothers, has emphasized the relationship between vaccine refusal, responsibilization and intensive and natural parenthood – conflating these two forms of parenting. One exception lies in the work of Dutch scholars who have considered how vaccine refusal employs either nature-centred or science-centred health views, with both containing extensive reasoning. Inspired by this distinction – and uncovering the labour involved in following as well as rejecting expert advice – we consider how intensive parenting can lead to different kinds of vaccine decisions, not just refusal (Ten Kate et al., 2022). We discuss the gendered inequalities reflected in parents’ processes of decision-making, and how unequal responsibilities, in the context of paid and unpaid work, produce mothers as active decision-makers performing the bulk of vaccine ‘decision work,’ regardless of its outcome. At the same time, shifts in care work and more widespread discussions about vaccination (such as occurred during the COVID-19 pandemic) can affect these gender roles: fathers can also be responsibilized for vaccine decision work (Kreyenfeld & Zinn, 2021; Mangiavacchi et al., 2021; Margaria, 2021).
Gendered vaccine decision-making intersects with broader patterns of gender inequality in parenting. Research across the Global North has found that women were unequally burdened with parenting and household responsibilities during the COVID-19 pandemic (Clark et al., 2021; Mangiavacchi et al., 2021; Otonkorpi-Lehtoranta et al., 2021). In the United Kingdom, Andrew et al. (2020) found that mothers experienced more job losses than fathers, likely because female-dominated industries were worst hit during lockdowns. Mothers spent more time on unpaid domestic work, including housework and childcare, while fathers engaged in more hours of paid work (see also Sevilla & Smith, 2020). In Canada, Fuller and Qian (2021) note that paid and care work remained highly gendered, partly because women's lower-paying jobs and high childcare costs made paid employment impracticable for mothers. Thus, lockdowns sometimes exacerbated gender inequalities. Some studies have produced more varying accounts of parents’ paid and unpaid work during lockdowns (Steinmetz et al., 2022). Mangiavacchi et al. (2021) found that childcare in Italy was less unequal during COVID-19 lockdowns, potentially because fathers lacked the capacity to work intensively and remotely. In contrast, Manzo and Manillo (2020) found that, in 2020, lockdowns in Italy exacerbated gender inequality.
Here, we focus on gendered planning and decision-making about young children's vaccinations, viewed through the lens of care work and intensive parenting. Intensive parenting necessitates a substantial amount of largely unpaid or underpaid care work, which we understand to include ‘raising the young, caring for the elderly, maintaining homes, building and sustaining communities and the vast work of ecological care’ (Klein, 2021, p. 1476). Although ‘all economic activity is dependent on care work’ (Smith, 2022, p. 354), it is often devalued and hidden (Bahn et al., 2020) and disproportionately falls on women. Care work includes vaccine-related medical ‘decision work,’ which encompasses information-seeking, negotiations with partners and families, as well as decisions themselves and the work to carry them out (including emotional labour). Contributing to gender studies and vaccination social science, we explore the gendered complexities and responsibilities of decision-making, what decisions were made and how.
Materials and methods
Our analysis draws on 18 in-depth, semi-structured interviews with heterosexual WA parents of children under five years old, conducted in anticipation of general accessibility for vaccines in this age group. The first Author collected these data between May and November 2021, when large numbers of Australian adults were first being vaccinated for COVID-19, but vaccination was not available to those aged 11 and under. Vaccinations were made available to children aged five to 11 as of 10 January 2022. Vaccination was approved for children aged six months to five years at the time of writing, but only available to those who were severely immunocompromized, with disabilities, or those with complex or multiple health conditions (Attwell et al., 2023).
Our interviews formed part of a larger project, Coronavax. Project ethics approval was provided through Western Australia’s Child and Adolescent Health Services (CAHS) Human Research Ethics Committee (RGS0000004457) (Attwell et al., 2021). Research examined people's views and experiences of the COVID-19 pandemic and vaccination, exploring national and WA policies and vaccination practices. Research methods included over 200 interviews with participant groups, among them the parents of young children. It also involved two sets of functional dialogues – one with the national health department and another with the WA health department, to communicate findings to aid the rollout and increase understanding of networks within governments. Finally, the project involved a social media study, in which popular COVID-19 topics and attitudes were tracked (Harper & Attwell, 2022; Harper et al., 2022).
We recruited interviewees using brochures, posters, social media, word-of-mouth, radio and newspapers. Potential interviewees filled out online pre-screening surveys, which collected demographic information, used to ensure a more representative sample. Ultimately, 58 parents of children under five years of age completed surveys during the data collection period, and 18 were chosen for interviews based on factors including location, gender and occupation. We planned to speak to 20 parents but ceased data collection after reaching saturation. Interviews were undertaken via phone, video call, or face-to-face, and lasted one to two hours. Interviewees received an information sheet and consent form, and were provided 20 AUD gift cards.
Questions explored people's experiences of the COVID-19 pandemic regarding work and care; encounters with and understandings of policies; histories of their and their children's vaccinations; views on and access to COVID-19 vaccination for themselves and their children; and how they talked about and accessed interpretations of vaccination and the COVID-19 pandemic. We recorded interviews and transcribed them using the online service Otter, after which they were edited by a professional transcriber. The second Author led and the first Author assisted with the thematic analysis of our transcribed interviews using NVivo 20, building deductive codes based on research questions and uncovering inductive themes. Interviewees were allocated pseudonyms, and distinguishing or sensitive information was removed for analysis.
Interviewees were aged between 29 and 50 years old. Typical of research on parental vaccination decisions (Bianco et al., 2019; Dubé et al., 2018; Santibanez et al., 2020), despite numerous attempts to reach fathers via parenting groups, childcare centres and word-of-mouth, we were unable to reach a comparable number of men and women; 13 interviewees were women, and five were men (see Tables 1 and 2). It is well known that women volunteer to participate in research more than men. Moreover, we did not seek to interview more than one parent from the same family, as we sought a broad range of parents. We uncovered some differences in mothers’ and fathers’ approaches and engagement in vaccine decision-making, which both male and female interviewees commented on, confirming previous work.
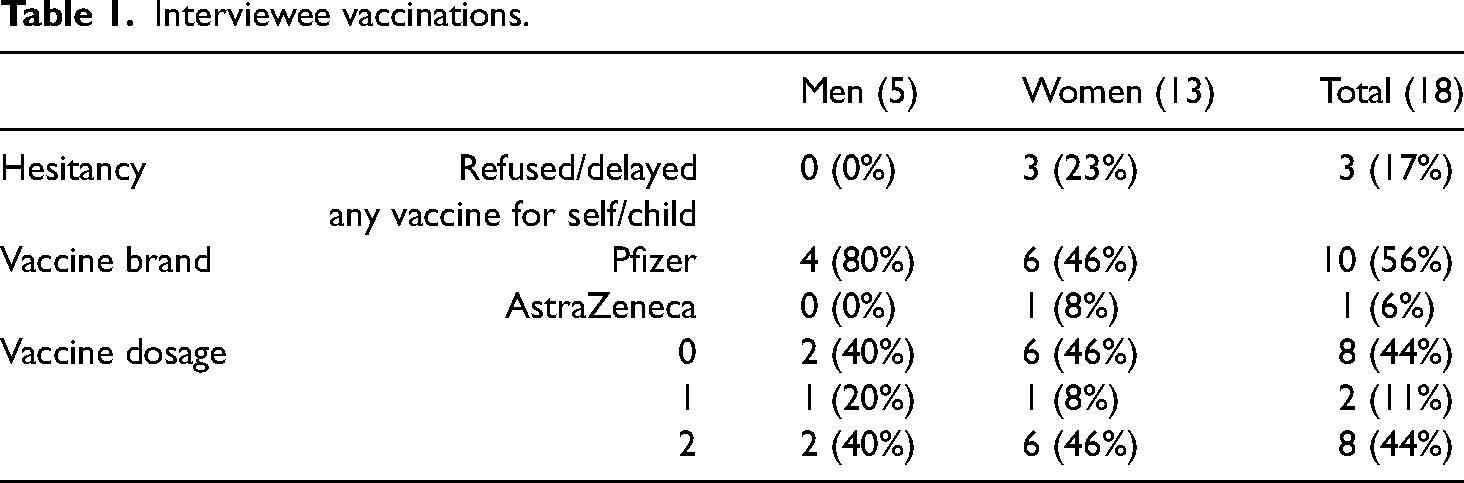
Interviewee vaccinations.
Interviewee data.
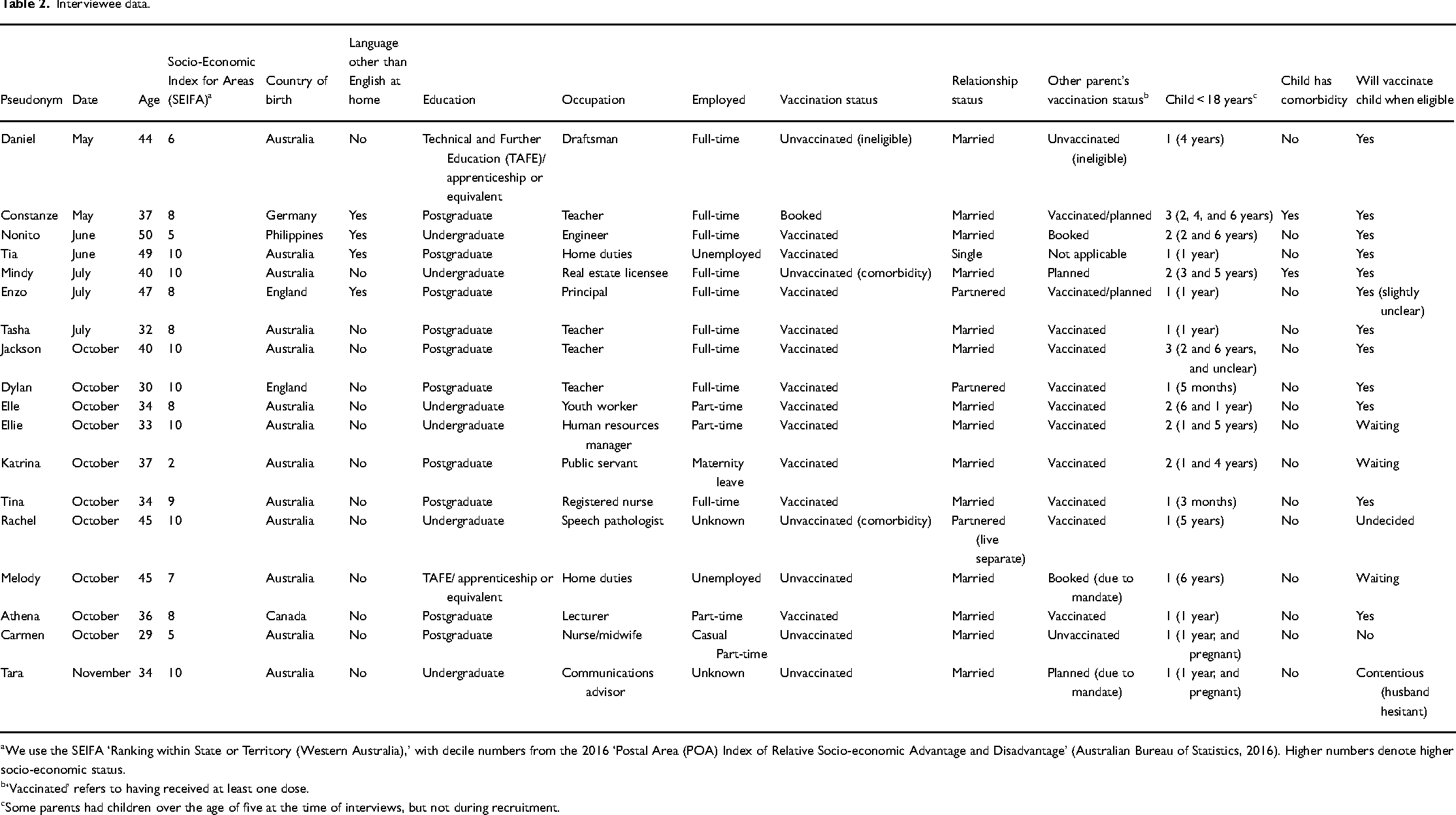
We use the SEIFA ‘Ranking within State or Territory (Western Australia),’ with decile numbers from the 2016 ‘Postal Area (POA) Index of Relative Socio-economic Advantage and Disadvantage’ (Australian Bureau of Statistics, 2016). Higher numbers denote higher socio-economic status.
‘Vaccinated’ refers to having received at least one dose.
Some parents had children over the age of five at the time of interviews, but not during recruitment.
All but one of our interviewees were married or partnered in heterosexual relationships, although in some cases their children were by previous partners (see Table 2). This provided an ideal sample to explore heterosexual parents’ decision-making. In the relationships discussed here, mothers (13 of 18 interviewees) were overwhelmingly the primary carers. Ten worked in paid part-time or full-time employment, and three were on parental leave or were stay-at-home parents. All five fathers were in full-time paid employment. In many of the relationships, mothers had shifted toward more care-focused roles or away from paid employment during the COVID-19 pandemic, either due to their refusal to vaccinate or because they had recently given birth. Interviewees came from a variety of cultural and ethnic backgrounds, worked in a range of occupations and lived in geographically dispersed suburbs across the Perth metropolitan area. Although they were not representative of the broad Australian population, they provided insights into shared understandings of COVID-19 vaccination for young children.
The parents we interviewed generally only had access to the Pfizer-BioNtech (Comirnaty) COVID-19 vaccine (henceforth Pfizer) for themselves, or no vaccine at all at the time of our conversations, and eight of our 18 interviewees had been ‘fully’ vaccinated (defined at the time as receiving two injections), while three had received only one injection. Australia's vaccine rollout initially centred on two vaccines: Pfizer; and the Oxford-AstraZeneca vaccine (now ‘Vaxrevia’). Following the emergence of thrombosis with thrombocytopenia syndrome among AstraZeneca recipients, the Australian Technical Advisory Group on Immunisation recommended that those under the age of 60 (and later 50) be preferred to receive the Pfizer vaccine. This led to national shortages of Pfizer and delays in the rollout, meaning that the unvaccinated parents discussed here were not necessarily unwilling to vaccinate.
Western Australia was also subject to numerous lockdowns and restrictions throughout 2020 and 2021, involving various rules regarding intrastate travel, work outside of home and the opening/running of facilities. Following a longer stretch of restrictions in 2020, the 2021 outbreaks were dealt with via short ‘circuit-breaker’ lockdowns, ranging from three to five days. As interviews took place between May and November 2021, many parents needed to work from home while managing children who would usually be in school or childcare. Childcare is notoriously expensive in Australia, and the Federal government provided support to parents in the form of childcare gap fee waivers, extra absences and special circumstances grants. In October 2021, WA announced Australia's most sweeping COVID-19 vaccine mandates affecting 75% of the workforce. Thus, some parents were subject to vaccine mandates to retain their employment.
While most parents were vaccinated or intended to be, intersectional factors such as race and class can impact medical and vaccine decision-making, particularly considering unequal state surveillance, access to support services and notions of medical freedom (Thornton & Reich, 2022). Considering racial disparities in the uptake of influenza vaccine among adults in the United States, Jamison et al. (2019) found that African Americans were less trusting of government and more doubtful of its motives compared to White adults. A review of studies of European migrant populations found access barriers to routine and COVID-19 vaccination but also acceptance barriers (Crawshaw et al., 2022), while our study of culturally and linguistically diverse people found that a dearth of appropriate and accessible government messaging about COVID-19 vaccines enabled misinformation to circulate, generating hesitancy and fear (Carlson et al., 2022). Among our interviewees, five were not born in Australia and four spoke languages other than English at home (see Table 2). However, all these people were vaccinated (or booked to be) and reported that they would vaccinate their child when possible.
Likely due to the self-selection of participant sign-up in our recruitment design, participants in all Coronavax studies tended to reside in largely medium to high socio-economic status (SES) areas (Attwell et al., 2021). We measured SES using the Australian Bureau of Statistics’ (2016) Socio-Economic Index for Areas (SEIFA) system – which ranks postcodes in Australia from one (low SES) to 10 (high SES), ‘according to relative socio-economic advantage and disadvantage.’ In this study, just one of our participants was from a SEIFA Index of Relative Socio-economic Advantage and Disadvantage of 1 to 4 (see Table 2). Four participants were from SEIFA Indexes 5 to 7, and 13 participants lived in places with SEIFA Indexes of 8 to 10. Although higher SES participants appeared slightly more likely to vaccinate themselves and (tentatively) their children for COVID-19, given our small sample size, this requires further investigation.
Results and discussion
COVID-19 vaccination decisions as intensive parenting work
Part of the unpaid care work that parents performed for their young children during the COVID-19 pandemic involved medical decision-making, including regarding vaccination. What decisions were made (or postponed) and how they were made forms our central focus. Family work studies often conceptualize household labour through various categories that acknowledge the work involved in decision-making for the family, including emotion work, responsibility, negotiation, management (finance, planning, organization, prioritization and scheduling) and mental labour (Robertson et al., 2019). Indeed, ‘decision work’ relating to the COVID-19 vaccine weighed heavily on parents, who had spent much time considering the benefits and risks to themselves and their children – illustrating a sense of individualized responsibility and intensive parenting. This intensive decision work was relatively uniform, regardless of whether parents ultimately planned to accept or reject a vaccine for their children. Parents’ (hypothetical) COVID-19 vaccination decisions for their children often connected to their decisions regarding their own vaccinations, and their past experiences vaccinating their children for other diseases (see Table 2).
Most interviewees expressed confidence in vaccination generally, stating that they were ‘very pro vaccination’ (Tina); have ‘always been fully vaccinated’ (Ellie); or have ‘never been opposed’ to vaccines (Dylan). For these interviewees, vaccination was guided by experts, and the COVID-19 vaccine was a matter of collective responsibility as well as individual choice. Numerous interviewees were comfortable taking government advice, declaring they would vaccinate their children ‘when it was recommended.’ Yet they also engaged in large amounts of ‘research’ – particularly around medical bodies’ recommendations – when preparing for such decisions. Thirty-two-year-old high school teacher Tasha had a child aged one, and a husband who was a pharmacist. Both parents were vaccinated for COVID-19. She suggested that taking expert advice was part of her parental responsibility: I feel like I’m much better equipped to make decisions about my driving […] and my cooking than I am to make like medical decisions […] If my doctor said this is available and yes it's safe […] I would see that as, you know, exercising my parental responsibility.
Regardless of the decision itself, it was common for parents such as Tasha to frame their vaccine decisions for their children in terms of responsibility. These decisions often entailed intensive parenthood practices.
For some interviewees, however, intensive parenting ideologies and practices led to reluctance to be led by experts, commonly where other family members had concerns. Forty-five-year-old Melody, who had a husband and three children – two of whom were grown and by a previous husband – described how her 30-year-old son engaged with ‘anti-vax’ material. Melody was unvaccinated and ‘staying at home’ while her husband ran a company in the mining sector. He planned to be vaccinated, largely because mining companies had introduced vaccine mandates. Melody discussed her anxieties about the COVID-19 vaccine, describing how a ‘little seed of doubt’ had been planted, even though she knew ‘that it's okay.’ This had resulted in her waking up one morning in ‘a panic.’ Melody repeated terms such as ‘nervous,’ ‘anxious’ and ‘uneasy’ when discussing her decisions regarding her and her youngest daughter's vaccination. Her concerns included the novelty of messenger RNA technology, perceptions of a lack of long-term medical testing and the possibility of blood clots and heart issues. These factors weighed on her (suspended) decision-making for herself and her daughter, making it an emotional and stressful process. Melody's response reflects the anxieties that can be produced by parental responsibility for medical decision-making.
Other interviewees’ concerns were not necessarily specific to the COVID-19 vaccine or scientific rigour, but pertained to the body's potential reaction to vaccines. Rachel, aged 45, had one child who was under five years of age. Rachel was a speech pathologist, lived separately from her (asthmatic, vaccinated) partner, and was unvaccinated for COVID-19. Rachel's concerns about her own vaccination centred on her previous negative experiences with tetanus vaccinations – where she had lost consciousness – and her chronic fatigue syndrome. She described herself as ‘fearful’ and ‘worried.’ Rachel's concerns for her daughter pertained to the possible effects of the vaccine on children: I’m really undecided […] it's a new vaccination and there's not that long-term information about it yet, particularly for the really young children […] And what sort of reactions there might be and long-term issues, so that's scary having to make that decision for her.
Rachel and Melody both expressed anxieties about their own and their children's COVID-19 vaccinations, although their male partners were vaccinated or planned to be. The women's current and potential decisions were framed in emotional terms, and highlighted the many considerations underpinning their choices, including their health, understandings of expert recommendations and testing and concerns and ‘information’ they had gleaned from others. Again, this reflects the anxieties produced by individual responsibility, revealing the weight of decision-making felt by these mothers.
The accounts above fulfil Hays (1996) description of intensive parenting, allocating responsibility for decision-making and the associated work to parents (leading to expert-led decisions, or not). As rational consumers, they were responsible for making decisions about vaccination based on available evidence (Sanders & Burnett, 2019), minimizing risk and maximizing benefit (Trnka & Trundle, 2014). Like other interviewees, Rachel and Melody had spent time gathering information, ostensibly because they were more concerned than their partners about COVID-19 vaccination. Yet mothers also took on these responsibilities where their partners had expressed concerns. Carmen told us ‘because I knew that my husband was more cautious’ about vaccines, she had ‘done the research on pretty much all of them’ – taking on responsibility and labour even when the concerns were not her own. This decision work, as we label it, encompassed information-seeking, negotiations, decisions and the work to carry them out.
In discussing their preliminary decisions, hesitant parents voiced their anxieties in terms of natural parenting discourse and risk. Carmen, who was 29 years old, and worked as a nurse and midwife, spoke of her decision-making for herself and her child in terms of balancing the risk of vaccination with that of getting COVID-19. She and her husband had not been vaccinated and did not plan to vaccinate their child. Explaining this decision using a natural parenting discourse, Carmen believed that her child's immune system would be sufficient to combat COVID-19: My son is almost two and I think based on his age and no comorbidities […] that there's very limited benefit in vaccinating him because if he were to catch COVID his symptoms are most likely going to be mild and he can recover at home like we do with many other, any other illnesses and let his immune system do what it's meant to do […] so I don’t feel that I would want to risk [it].
Carmen identified as ‘pro-vaccine’ and believed that ‘[for] the majority of children vaccines are safe’;’ her husband was ‘vaccine neutral’ yet anti-COVID-19 vaccination. Like the vast majority of the parents discussed here and in previous studies (even those wishing to vaccinate their children), Carmen discussed the risks that vaccination posed to her children but not the risk their non-vaccination posed to others (Baker & Walsh, 2022; Reich, 2016; Sobo, 2015). Carmen saw herself as managing the individualized responsibility of caring for her child's health without vaccinating (via natural parenting); she also undertook the vaccine decision work involved in investigating her and her husband's concerns (in keeping with intensive parenting practices).
While mothers alluded to natural parenting and the intensive work it entailed more often than fathers (in keeping with past research), some men also supported such practices. Forty-seven-year-old primary school principal Enzo, who had an 18-month-old child and had been vaccinated, stated: Having a healthy home and having healthy food, I think, is really important. I’m not saying that that's going to be the cure for everything, just as much as possible, I want it to be as natural as possible. If [vaccination in general] needs to be done, then so be it.
Enzo lived and worked in an area of Perth notorious for its ‘natural’ culture and low childhood vaccination rates (Attwell, 2019), which was central to the local movement protesting COVID-19 vaccines and mandates. Enzo's use of this discourse thus confirms previous observations that such views, and the accompanying reticence to vaccinate, tend to be geographically clustered (Baker & Walsh, 2022; Reich, 2016; Sobo, 2015). It also illustrates that fathers can take on natural parenting attitudes – something that has not been previously explored in depth.
While Tasha and many of our other interviewees enacted their parental responsibility through deferring to experts, parents such as Rachel, Melody and Carmen described their responsible parenting as informing themselves, and then using this to balance ‘risk,’ a key component of the neoliberal mindset. Both groups, including men such as Enzo, demonstrated the labour-intensity of parents’ decision-making work. Parents’ different perspectives on their children's vaccinations were not noticeably linked to gender, education, occupation, or adherence to intensive parenting, but they were strongly connected to parents’ own COVID-19 vaccination decisions and their invocations of natural parenting. How parents negotiated, interrogated and enacted decisions about their children's vaccinations were, however, highly gendered.
Gendered differences in vaccine decision-making work
By far the lengthiest discussions in our interviews about childhood vaccination came from female participants. Here we saw mothers taking on increased childcare work, aligning with others’ findings during the COVID-19 pandemic (Aslam & Adams, 2022; Craig & Churchill, 2021; Vandecasteele et al., 2022) and research finding that women take on more ‘decision work’ than men (Robertson et al., 2019). Generally, interviewees stated that their partners agreed with them regarding their children's vaccination, but both female and male interviewees said that mothers did most decision-making. As seen in Table 2 and the examples of Rachel and Melody, where mothers and fathers had different vaccine intentions, tentative decisions for children always aligned more with mothers’ decisions for themselves. Unvaccinated mothers partnered with vaccinated fathers, for instance, tended to say they were ‘waiting’ or ‘undecided’ about their children's vaccinations. Mothers who wanted to vaccinate more than fathers also took on the labour of backing up their decision with research.
Male and female partners were often highly conscious of inequalities in their parenting and vaccine decision-making, while for the most part noting their broad agreement on the decision. Thirty-seven-year-old public servant Katrina, who was on maternity leave, had two children aged one and four. She and her husband were double vaccinated. Of her children's hypothetical COVID-19 vaccination, she said of her husband: I would say, like, he's on board. He would probably do whatever I suggested. I think he works an absolutely truckload, so he would probably defer to me if I said: this is what we’re doing.
Speaking about vaccinations generally, thirty-three-year-old Ellie, a part-time human resources manager with two children aged one and five years, made similar comments about her husband. Both partners had received COVID-19 vaccines, and Ellie said: It's probably me and then going ‘do you agree or not?’ and then we’ll talk about it [laughs]. So I’m the one that usually does like the medical appointments with the kids, stuff like that […] I presume he knows I take the kids to their vaccinations. I don’t think I’ve ever told him that, like, they got the extra meningococcal vaccination.
Fathers made similar comments regarding inequalities in decision work. Enzo, discussed above, said, ‘I’d like to think we decide together, but probably it's just [my wife]. She knows I’m cool with it, she runs with it. We have the same view.’ The gendered nature of couples’ decisions was particularly evident in the language they used: women frequently used ‘I’ when discussing vaccine decisions, while men tended to use ‘we’ but indicated that their female partner was largely responsible for decisions.
Other fathers also acknowledged possessing less decision-making power than their female partners. Thirty-year-old high school teacher Dylan, who had a five-month-old baby, had received a single COVID-19 vaccination. He said of his partner: I leave most of the decisions up to her, she's definitely been more proactive in terms of the baby and things like that. I’m obviously focusing on work as well as the baby, and she's able to put her whole mind towards it.
Such claims align with the literature, which consistently finds that mothers take on more healthcare responsibility for their children than fathers, as well as taking on the substantial care work of intensive parenting (Bianco et al., 2019; Greyson & Bettinger, 2022; Reuben et al., 2020). While these comments do not noticeably reflect ‘natural parenting’ – in that they are highly pro-vaccination – mothers’ child-centred, expert-guided and labour-intensive approach places them within the realm of intensive parenting. Dylan's claim above reflects how employment arrangements facilitate such a division of labour.
Other interviewees noted how gendered decision-making within their partnership was unspoken and implicit. Elle, a 34-year-old youth mental health worker and psychology student with two children aged 19 months and six years, reported that she and her husband were both vaccinated. Discussing their (future) decision regarding their children's COVID-19 vaccinations, as well as past vaccinations, she reflected: We’ve never actually talked about it, I think it's just an assumption […] It's a mutual agreement […] It's just a natural […] we have the same ideas, I guess.
Elle's description highlighted how the couple's decisions were both mutual and gendered, with her telling her husband when their son had recently been vaccinated, with no expectation of disagreement. Another interviewee, 36-year-old Athena, who worked as a part-time lecturer, similarly stated that, because she had a medical background, her husband left ‘that kind of stuff to me, in that he just trusts that I’ll make the best decision.’ Most interviewees agreed with their partners regarding COVID-19 vaccination, yet how they negotiated decision-making work resonated with research on the gendered nature of emotional labour and intensive parenting (Baumann et al., 2019). This work included time spent researching vaccinations and recommendations from medical bodies, discussing decisions with fathers (although this did not always occur) and enacting vaccinations.
Male interviewees took on more decision-making responsibility for COVID-19 vaccines for themselves than for their families. Their responses to questions about their vaccinations were often short and matter-of-fact, suggesting that they spent less time arriving at such decisions. Unlike their female counterparts, they rarely discussed data and reporting on vaccine safety, nor their negotiations of the ‘risks’ of COVID-19 vaccination versus COVID-19 itself. Vaccinated 30-year-old full-time teacher Dylan stated ‘I don’t think I know that much about [vaccines], or I didn’t go out and do extensive research [into different brands].’ Another full-time teacher, 40-year-old Jackson, tersely explained that his motivation ‘to get vaccinated was always to protect everyone.’ Fathers took responsibility for their own vaccination decisions, however, even if they were less authoritative regarding their children.
Yet, despite these inequalities, both women and men commented that fathers were discussing their children's COVID-19 vaccinations with mothers more than their routine vaccinations, in large part due to the novelty of the vaccine and because (often politically charged) discussions were then commonplace in the media and public. Thirty-four-year-old communications adviser Tara, who had an 18-month-old son and was pregnant, remained unvaccinated for COVID-19, yet had received other vaccines recommended during pregnancy with little comment from her husband. They had not yet discussed her toddler's COVID-19 vaccination, largely because her husband remained unvaccinated and was extremely concerned about Tara receiving the COVID-19 vaccine (as recommended) during pregnancy. Tara wanted the vaccine and to vaccinate her son when he became eligible. She said: I’ve taken my husband along to two doctors’ appointments [and asked him to…] have a conversation with them about [children's COVID-19 vaccinations]. They have said some really reassuring things to him […] He seemed like he was agreeing that, ‘okay, I’ll let you do [the COVID-19 vaccine] now’, but he asked me to just wait until I was at least into my third trimester […] It’ll turn into an argument, that's the tricky thing.
Tara's experience illustrates how fathers can influence vaccination decisions (Gilchrist et al., 2021; Rammohan et al., 2012; Torun & Bakırcı, 2006). It also demonstrates that, like Carmen above, Tara was responsible for the ‘work’ of convincing her husband: seeking out medical professionals who might convince him of the vaccine's safety. Thus, decisions about COVID-19 vaccination were in some cases significantly influenced by fathers, even though in general fathers took on less decision work and intensive parenting practices than mothers, such as researching and organizing vaccinations. When men engaged with and supported intensive parenthood practices, including for vaccine decision-making, this often meant more work for women and men: both mothers and fathers were thus being increasingly responsibilized for vaccine decision work.
In/equalities in un/paid work and vaccine decision-making
Couples often struggled with the pressures of paid work and childcare during lockdowns, and these pressures intertwined with gendered processes and outcomes of vaccine decision-making. As found in other Australian studies (Craig & Churchill, 2021), most male partners worked full-time while most female partners were part-time, casual, or engaged with home duties, meaning they were more involved in caretaking of children. As research suggests that stay-at-home mothers tend to believe that ‘women are inherently better at parenting than men’ (Liss et al., 2013), and intensive parenting is time-consuming, there are links between the two. Scholars have likewise reflected that ‘work and gender norms constrain men's ability to be involved parents’ (Scheibling & Milkie, 2023). Research has found that the COVID-19 pandemic has had a disproportionate impact on women's employment and unpaid work, resulting in a decline in mothers’ autonomy and spatial and temporal boundaries (Aslam & Adams, 2022; Otonkorpi-Lehtoranta et al., 2021). Our female interviewees also indicated that their parenting burdens intensified during lockdowns. Part-time worker Ellie, discussed above, ‘felt a lot of pressure to keep the kids quiet’ and away from her husband while he was working.
Even when both parents were working, women tended to take responsibility for medical decisions and for childcare during lockdowns. Athena indicated that, despite working herself, as her baby wanted her attention, the ‘childcare work’ fell on her. In one extreme case, Elle's husband began drinking heavily and became disengaged from his family; she ‘needed to look after everybody’ and did so by ‘not requiring anything from him.’ Mindy said that it was her partner's boss’ gendered beliefs that impacted their childcare situation, rather than her husband himself; reflecting the structured nature of many gendered inequalities (Andrew et al., 2020; Sevilla & Smith, 2020). Aligning with others’ research (Andrew et al., 2020; Manzo & Minello, 2020; Otonkorpi-Lehtoranta et al., 2021; Sevilla & Smith, 2020), these experiences highlighted the tensions in childcare responsibilities that characterized lockdowns, resulting in women taking on more intensive care work and decision-making responsibilities.
The difficulties of mothers’ increasingly intensive parenting during lockdowns could act as an incentive to vaccinate their children for COVID-19. Tina, a 34-year-old full-time registered nurse, was looking forward to her children being vaccinated so that they could attend daycare: she would ‘love my son to get immunized.’ Interviewees also discussed the challenges that they faced while their children were still unable to get vaccinated. Katrina, who we discussed above, had her daycare plans disrupted when her friend and babysitter became an ‘anti-vaxxer.’ She said: That's going to affect me going back to work because if [my unvaccinated babysitter…] can’t have our youngest, then […] what do we do in terms of childcare?
Katrina viewed the babysitter's unvaccinated status as her problem, rather than a family problem. Previous Australian studies suggest that parents vaccinate their children to protect them from disease and to conform with societal expectations (Enkel et al., 2018), as well as to contribute to herd immunity (Danchin et al., 2018). The COVID-19 pandemic, however, significantly disrupted the lives of families; now that potential illness is more likely, concerns about childcare availability and inequalities in care work may have become more significant motivators for women considering vaccinating their children. Thus, women had powerful incentives to take on gendered responsibility for vaccinations and engage in vaccine decision work.
COVID-19 vaccinations also impacted parents’ practices in ways that sometimes-prompted greater involvement and responsibility on the part of fathers. Some interviewees mentioned negotiating their COVID-19 vaccination dates with their partners, to avoid them both experiencing side-effects at the same time, making paid work and care work challenging. For instance, 50-year-old full-time engineer Nonito stated: When we do the vaccine, what will be our strategy? Like, I’ll get it first and then after a couple of weeks my wife will get it, something like that, just in case like she got some side effects. It's like, we don’t have to be [sick] at the same time.
Nonito indicated the need to cooperate with his partner to ensure the household ran smoothly, taking turns to take care of the two-year-old and homeschool the six-year-old. His wife was a stay-at-home mother at the time but was looking for work. Notably, his workplace was quite flexible regarding working from home. Both found homeschooling to be a ‘struggle,’ and he stated that he was ‘not really productive’ in his work during lockdowns. Nonito became more involved in care work during these periods, demonstrating how men could sometimes take on more intensive care work.
Mothers and fathers reflected on the impact of policy adjustments during COVID-19 lockdowns, which potentially played a role in both mitigating and sustaining gendered divisions of work at home. Jackson, a 40-year-old full-time teacher, praised Federal Government-supported free childcare during the initial COVID-19 outbreak for protecting his ability to perform paid work (a short-lived reversal of the neoliberal tendency to place responsibility for childcare costs on parents). Yet numerous female interviewees lamented that the COVID-19 lockdown period in WA meant more care work fell to them, including vaccine decision-making work. Our male interviewees were very aware of these inequalities – both in vaccination decision work and in care work during lockdowns – but this did not necessarily lead to shifts in parenting practices. It is possible that, as Mangiavacchi et al. (2021) found in Italy, with appropriate policy support to reverse the responsibilization of mothers for intensive parenting, greater capacity for equality could emerge, both in terms of parenting and vaccine decision-making.
Conclusion
Although WA fared relatively well during the initial COVID-19 pandemic, particularly compared to eastern Australia, COVID-19 and related government responses impacted people in myriad ways. One significant disruption was to parenting, as parents contended with the demands of paid and unpaid work, as parents and employees working from home. Schools and childcare centres remained closed or undesirable due to the risk of viral transmission, and, in heterosexual partnerships, this often placed an increased burden on mothers, who typically already took on most home and care duties. The COVID-19 pandemic also complicated what we call parents’ gendered ‘decision work’ and responsibility regarding children's vaccinations. While some parents exhibited intensive ‘natural parenting’ attitudes and questioned the need to vaccinate their children, others took an ‘expert-led’ intensive parenting approach whereby they researched medical recommendations, including in response to more hesitant family members. Fathers, while generally less involved in their children's vaccination decisions, did this along with mothers.
This article asked who made (tentative) vaccination decisions for their children under five years of age during the COVID-19 pandemic, what decisions were made and how these decisions were gendered. It focused on how structural inequalities produced heterosexual mothers who made vaccination decisions for their young children largely without partners’ time, emotional labour, or input (but often with their implicit support and agreement). Yet we found evidence that some fathers were involved in decisions about COVID-19 vaccination for their young children (albeit sometimes in ways that increased mothers’ work). This points to the complex realities and practices of parents’ decision work, highlighting how parents’ (largely aligned) ideas about vaccination intersect with their (largely divergent) practices.
Mothers have undeniably been unequally impacted during the COVID-19 pandemic. This has incentivized mothers to engage in vaccine decision work and vaccinate their children, attempting to (partially) free them from intensified mothering practices. In contrast to prior scholarship, we find that the politicization and broad public discussion about the COVID-19 pandemic and (still novel) vaccinations have exposed the gendered workings of parenting, sometimes challenging them in unexpected ways. While previous scholarship tends to conflate intensive parenting with vaccine-resistant mothers, we find that intensive parenting can lead to different kinds of vaccine decision-making: expert-led ones or natural parenting-led ones, just as earlier work has found both ‘natural’ and ‘scientific’ discourses among vaccine refusers. We also find that fathers can engage in and support intensive, responsibilized parenting among themselves and mothers, particularly in a context where vaccines are politicized and widely discussed, and fathers are sometimes more available for care work (like during the COVID-19 pandemic).
Footnotes
Acknowledgements
We thank the participants in this project for their time and insights, as well as the broader team for the project Coronavax: Preparing Community and Government for COVID-19 Vaccination.
Ethics approval
Ethics approval was granted by the Child and Adolescent Health Services Human Research Ethics Committee (RGS0000004457).
Funding
Coronavax is funded by research grants from the Government of Western Australia's Department of Health (DOH2020-6075), a Future Health Research & Innovation Fund COVID-19 Focus Grant (FHRIFGCOVID19), as well as a Wesfarmers Centre of Vaccines and Infectious Diseases (WCVID) Catalyst Grant.
