Abstract
The concept of viewing a patient as an organization within the context of digital healthcare is an innovative and evolving concept. Traditionally, the patient-doctor relationship has been centered around the individual patient and their interactions with healthcare providers. However, with the advent of technology and digital healthcare solutions, the dynamics of this relationship are changing. Digital healthcare platforms and technologies enable patients to have more control and active participation in managing their health and healthcare processes. This shift empowers patients to take on a more proactive role, similar to how an organization functions with various stakeholders, goals, and strategies. The prevalence of mobile phones and wearables is regarded as an important factor in the acceptance of digital health.
Objective:
This study aimed to identify the factors affecting adoption intention using the TAM (Technology Acceptance Model), HB (Health Belief model), and the UTAUT (Unified Theory of Acceptance and Use of Technology). The argument is made that the adoption of the technology enables patients to create resources (ie, data), transforming patients from mere consumers to producers as well.
Results:
PLS analysis showed that health beliefs and perceived ease of use had positive effects on the perceived usefulness of digital healthcare, and system capabilities positively impacted perceived ease of use. Furthermore, perceived service, the customer’s willingness to change and reference group influence significantly impacted adoption intention (b > 0.1, t > 1.96, P < .05). However, privacy protection and data security, online healthcare resources, and user guidance were not positively associated with perceived usefulness.
Conclusions:
Perceived usefulness, the customer’s willingness to change, and the influence of the reference group are decisive variables affecting adoption intention among the general population, whereas privacy protection and data security are indecisive variables. Online resources and user guides do not support adoption intentions.
Keywords
Introduction
As a result of the rapid advancements in digital technologies, several individuals now have unprecedented access to a vast array of health information through online platforms. They also can monitor their well-being using wearable technology, telemedicine, and other digital avenues to engage with healthcare professionals. 1
This shift has ushered in a new era where some people actively manage their health, marking a significant departure from traditional patient care models. The emergence of digital patient care has revolutionized the landscape by amalgamating data from diverse digital sources such as wearable devices, electronic health records, and social media platforms. 2
Thanks to advancements in digital patient care, healthcare professionals are empowered to monitor patients in real time, identify potential issues proactively, and intervene promptly to prevent complications. 3
This paradigm shift affords medical professionals a holistic understanding of a patient’s health, encompassing their medical history, behaviors, and lifestyle choices. Thus, it facilitates the development of tailored and efficient treatment plans. 2
The new Zeitgeist movement prioritizes the active involvement of citizens, public participation, and those with firsthand knowledge in the development and improvement of the health system. This movement encompasses the principles of collaborative decision-making, enhancing the standard of care, and reconfiguring service delivery. 2 It fosters cooperation, autonomy, and inclusiveness, with the goal of providing more efficient, adaptable healthcare services that are customized to meet individual requirements and preferences.
The collaborative utilization of digital technologies by patients and healthcare providers has given rise to a data-rich environment, paving the way for a transition from an event-driven to a patient-centric healthcare paradigm, supported by robust data analysis, management, and privacy mechanisms. 4
With access to a wealth of data and information, individuals are now better equipped to embrace preventive healthcare measures, and their comprehensive digital profiles, comprising medical and non-medical data, can be leveraged for academic, professional, and commercial purposes. 5
However, this shift toward a digitally driven healthcare landscape also exposes individuals to heightened vulnerabilities stemming from the potential misuse of their data, underscoring the critical need for robust data privacy and protection measures. 6
Consequently, a paradigm shift is imperative in how we conceptualize, care for, and manage individuals within the healthcare ecosystem, necessitating concurrent changes in healthcare delivery and conceptualization. 3
This redefined the notion of individuals as active participants in their health management endeavors to foster a more equitable, secure, and efficient data-driven healthcare environment, promising to reshape the patient experience during and after treatment. In this evolving landscape, healthcare service providers are urged to contemplate the multifaceted aspects of individual conceptualization to tailor their services effectively, thereby enhancing the quality of care delivery across the healthcare continuum.
The present conceptualizations of the patient, their benefits, and limitations:
In the medical field, a wide range of patient conceptualizations exist. Common approaches of patient categorization include the following:
Patients as passive recipients of healthcare services
Patients are seen as passive recipients of healthcare services who put all decision-making authority in the hands of healthcare professionals. Doctors and nurses are seen as the go-to sources of knowledge and care in this framework. 4
The main advantages of this conceptualization were that the doctor and the caregivers, the people with the best understanding of the situation and its remedy, made professional decisions without any emotional biases, reducing the patient’s anxiety and stress. However, it made patients less engaged and did not take ownership of their conditions. It could be harmful in case of misunderstandings or other communication gaps between patients and healthcare professionals. Overall, simplifying decision-making and reducing patient stress could also lead to reduced patient autonomy and suboptimal care, and patients may feel ignored, disrespected, or unimportant.
Patients as active customers
According to Dhawan, 5 patients are regarded as proactive customers who can exercise control over their healthcare choices and influence the service provision standard by expressing their preferences. This concept centers on patient autonomy and self-determination, which confers the benefits of patients assuming an engaged role in preserving their well-being and exercising discretion regarding their medical care through the utilization of pertinent healthcare providers and interventions. 6
The aforementioned conceptualization promotes the development of “patient-centered care,” which stimulates competition among healthcare providers to provide superior treatment and enhance patient contentment, by catering to individual patient requirements and inclinations. 7
The perception of patients as customers may potentially foster greater transparency and efficacy in the communication practices of healthcare professionals. Nonetheless, this viewpoint has the potential to cultivate a customerist approach to healthcare, 8 leading to the commodification of healthcare and the preference for financial gains over the well-being of patients.
This phenomenon may also result in the stigmatization of patients for their illnesses or unfavorable health outcomes, leading them to perceive themselves as being responsible for circumstances outside of their purview, thereby eliciting emotions of regret or shame. 9
Likewise, it has the potential to result in unequal healthcare accessibility predicated on financial capacity rather than medical necessity. 10
This conceptualization could potentially facilitate marketing endeavors that are incongruous with the medical field. For instance, the incongruity between demand and supply could be leveraged to augment healthcare expenses, and advertising may disseminate erroneous information to vulnerable patients, leading them to make suboptimal decisions. 11 In general, the prevalent perception of medical professionals as vendors rather than advocates for their patient’s health may deteriorate patient-provider trust.
Patient as an individual
According to Roberti di Sarsina and Tassinari, 12 the individualistic approach regards patients as unique individuals with distinct medical needs and personal preferences. As per this framework, it is imperative to customize medical interventions to suit the unique needs of every patient. The benefits of this conceptualization lie in its emphasis on patient-centered care, which entails the consideration of individual patient attributes, including their values, preferences, and goals. The approach entails considering the entirety of the person rather than solely their ailment, surroundings, and standard of living. The conceptualization proposed by Godfrey et al 13 is conducive to a healthcare experience that is characterized by greater personalization and empathy.
The ability of physicians to perceive patients as distinct individuals enables the implementation of treatment approaches tailored to their specific needs. Individuals’ responses to treatments, drugs, and therapy may differ based on many factors, such as genetics, lifestyle, and life circumstances. By findings, medical practitioners can tailor patients’ treatment plans to achieve the best possible outcomes while minimizing any negative consequences. 14 Providing adequate time and attention to individuals as unique entities positively increases patient satisfaction. Under this conceptual framework, there is an increased likelihood of collaboration between medical practitioners and patients in developing treatment plans. According to Balarajan et al 15 incorporating patients’ individualized needs and concerns is positively associated with their engagement and adherence to treatment protocols.
An individualistic approach to patients may overlook the impact of social and environmental factors on their health, leading to insufficient understanding and ineffective care. 16 This may marginalize individuals with specific medical conditions, such as mental health and substance use disorders. Inadequate communication, misunderstandings, and suboptimal care may result from this perspective, leading to over-reliance on medications or interventions. 17 Patients perceived as deviating from the norm may experience discriminatory practices or denial of care within the healthcare system, potentially resulting in legal action against healthcare providers or organizations. 18 Considering a range of factors, including, but not limited to, social, environmental, cultural, and individual differences, is imperative to ensure the provision of effective and equitable healthcare. 19
Moreover, the patient’s individualistic perspective may intensify the insufficiency of privacy safeguards, leading to a higher probability of unauthorized disclosure of protected personal health information. Violating patient confidentiality may lead to legal consequences for healthcare providers and institutions.
Extending the conceptualization of patient in the digital health context
Many new ideas about patient and patient care exist in the extant literature. They include empowering the patients by embedding them in the larger digital healthcare ecosystem as an informed and active participant. The following are a few notable new approaches:
Norman and Conner 30 studied the use of digital health technologies by patients with chronic diseases, actively participating in their treatment due to access to their health data and the opportunity to speak with healthcare practitioners in real time. According to this model, people would be seen as members of the e-healthcare team. Mønsted 20 by using digital health technologies, people may monitor their health condition, keep track of their symptoms, and interact more effectively with their healthcare providers. Tang et al 32 contend that patients are increasingly becoming “citizen scientists” due to their use of digital technologies to gather, discuss, and engage in research about their health. Studies investigated how digital health technology might contribute to patients’ empowerment by helping them gain more knowledge about their ailments, connect with other patients, and interact with healthcare practitioners in novel ways. 21
According to these studies, the widespread implementation of digital health technology can give patients more autonomy and the tools necessary to manage their health more proactively. 22 The concept of patients increasingly incorporates the notion of an active team member who is empowered as a partner, co-creating the healthcare experiences and outcomes of their medical treatment. 23 On the other side, patients are now more vulnerable to digital eavesdropping without their knowledge or consent, misuse of the data by unauthorized use, and inappropriate sharing with different interested parties like researchers, AI technology repositories. 24
Therefore, the current understanding of the patient falls short of comprehensively incorporating these advancements into their knowledge within the digital healthcare realm. To address this, we propose an extended conceptualization of the “patient as an organization,” which better accommodates patients’ evolving roles and behaviors in the digital healthcare ecosystem. This approach facilitates a more integrated and holistic adoption of digital health.
Exploring adoption intention of digital health: A quantitative methodological approach
The healthcare sector is transforming toward digital health solutions in an era marked by rapid technological advancements. Understanding the factors that drive the intention to adopt digital health technologies is crucial for stakeholders, including policymakers, healthcare providers, and technology developers. This study employs a quantitative methodology to systematically investigate these factors, providing empirical evidence to guide effective strategies for promoting digital health adoption.
Through a structured and data-driven approach, this research aims to identify key determinants influencing individuals’ intentions to adopt digital health solutions. By leveraging statistical tools and techniques, we will analyze variables such as perceived usefulness, ease of use, technological capability, and socio-demographic factors. The insights gained from this study will enhance our understanding of user behavior in the digital health context and contribute to developing more user-centric digital health interventions.
The quantitative methodology adopted in this research involves collecting and analyzing numerical data through surveys and questionnaires. This approach enables us to quantify relationships between variables, test hypotheses, and draw generalizable conclusions. By employing robust statistical analyses, we aim to ensure the reliability and validity of our findings, thereby providing a solid foundation for future research and practical applications in digital health.
Methods
Study design
The data for this research were obtained using a cross-sectional survey. In order to collect data and verify the hypotheses presented in the theoretical framework, a randomized online survey was carried out via Google Docs. The survey was sent to mobile device users, and the questions were formulated based on prior study results. The participants were instructed to evaluate their comments using a 7-point Likert scale, with 1 indicating “strongly disagree” and 7 indicating “strongly agree” (modified from Raju and Harinarayana 25 ). This scale facilitated nuanced replies, reflecting diverse levels of agreement or disagreement with the survey items.
Target sample
The total number of collected questionnaires was 164. Data from 164 respondents were included for analysis. Forty-nine percent of the respondents were male, 51% were female, and the respondents were almost equally distributed across the age groups. Many respondents had received an education equivalent to a bachelor’s degree. The most commonly reported income in our study population was $500 to $1500. Only 8 (5%) participants had used digital health during the past year. Some respondents had major chronic diseases, such as hypertension (n = 32, 20%), diabetes (n = 48, 30%), and heart disease (n = 16, 10%), and most of the participants reported that they had visited the hospital 1 to 2 times a year.
Research model-adoption intention of digital health
According to the technology acceptance model (TAM), perceived usefulness and perceived ease of use are the two major factors involved in user adoption of a technology. 26 The TAM has been widely used to evaluate user acceptance of general technologies such as online banking, mobile commerce, healthcare, and digital healthcare technology, to name a few but few scholars pointed out that the TAM has several disadvantages. 27 :
(1) providing inadequate insight into individuals’ perspectives of novel systems,
(2) neglecting its indicators and directly investigating the external variables of perceived ease of use and perceived usefulness and
(3) ignoring the relationship between usage attitude and usage intention. Therefore, we extended the TAM with the HBM to evaluate the acceptance of digital health.
The HBM was developed by social psychologists Century and Cassata 28 to predict individuals’ habitual responses with acute or chronic diseases to the treatments received and has since been applied to guide general health habits.
The Health Belief Model (HBM) is a theoretical framework that contends that people’s health-related beliefs, such as their vulnerability to sickness and the advantages of acting healthily, may affect their health behaviors. Conversely, the TAM focuses on people’s technology adoption and usage, looking at elements like perceived utility and simplicity.
The researchers combined these two models to understand better how people’s health attitudes affect their desire to employ information technology for health improvement.
Although the TAM and HBM both have their advantages, taken alone, they are unable to explain the cognitive and associated process by which people utilize digital intervention better for health. 29
Norman and Conner 30 claim that people who believe their health is in jeopardy are more motivated to use information technology to improve it. A useful tool for predicting people’s attitudes toward health-related technology is this integration of HBM and TAM. People’s motivation to use technology to enhance their well-being appears to be significantly influenced by the notion that their health is in danger. This finding emphasizes how crucial it is to consider how people perceive their health when developing and promoting health-related technologies. 29 Healthcare professionals and designers can develop more effective interventions that are suited to each individual’s specific needs by understanding the factors that affect people’s attitudes toward technology. This strategy may ultimately result in better health outcomes and a higher standard of living for those who use these technologies.
In the context of digital healthcare technology, individuals who realize that their deviant health habits cause harm to their health are motivated to adopt digital healthcare technology to develop their health management activities. 31
Those who perceive their health as poor or need improvement may be more inclined to adopt and use technology for health maintenance. The study’s design, technique, and variables will provide additional context and information on the connections between HBM, TAM, and the adoption of health-related technologies. 29
Development of hypotheses
The Technology Acceptance paradigm (TAM) is a condensed version that emphasizes people’s attitudes and intentions toward accepting technology. It emphasizes elements like perceived usefulness and perceived ease of use as major predictors of people’s intentions to accept and utilize technology. 32
However, many more elements outside human attitudes impact how technology is accepted and used. As noted, many other components might affect technology adoption, including social influence, perceived risk, compatibility with current systems, organizational regulations, and assistance. 33
Researchers often combine the TAM with other models and frameworks to provide a more complete view of technology adoption. This method enables a more thorough investigation of the different aspects that affect people’s adoption and utilization of technology. 34
By introducing new models or frameworks, researchers may investigate the intricate interaction of human, societal, organizational, and environmental variables that affect technology adoption. This enables academics to create more successful methods for encouraging the adoption and use of technology in various situations by giving researchers a more nuanced and comprehensive knowledge of the adoption process. 26
The HBM(Health Belief Model) has been widely applied to understand and predict various health-related habits, such as preventive screenings, vaccination uptake, medication adherence, and healthy lifestyle habits. By considering individuals’ perceptions of susceptibility, severity, benefits, and barriers, health interventions can be designed to address these factors and promote positive health habits. 35
The UTAUT model offers a holistic framework for analyzing and forecasting how people interact with technology in various settings. It has been used in many fields, including medicine, e-commerce, education, and the workplace, to analyze how people adapt to new technologies and guide the development of future innovations. 36 The modified research model has been illustrated in Figure 1.

Research model.
Measures
Perceived Usefulness (PU)
The perceived usefulness of digital healthcare innovations, such as medical service applications, smartwatches, and sports-related technology products, is connected to patients’ expectations regarding its effectiveness. 37 The relationship between perceived usefulness and patients’ acceptance goals for digital healthcare innovations can be explained as improved health outcomes, convenience and accessibility, personalized features, empowerment and self-management, and increased engagement in their healthcare. 38 When patients recognize the potential benefits of these innovations, experience convenience and accessibility, engage in personalized experiences, and feel empowered in their self-management, they are more likely to embrace and adopt digital healthcare innovations. 39
H1: Perceived Usefulness has a positive impact on adoption intention.
Customer innovativeness (CWI)
Customer innovativeness refers to the willingness of customers to try out new information technology products and is linked to their general beliefs about information technology. 40 Factual literature has confirmed that customer innovativeness has a noteworthy positive impact on customers’ intention to accept information technology products. In digital healthcare technology, factual studies also postulate that customers with high innovativeness and innovation can manage uncertainty and are more keen on adoption intention. Therefore, our second hypothesis is that customer innovativeness positively impacts customers’ adoption intention of digital healthcare technology. 41
H2: Customer innovativeness has a positive impact on the adoption intention of digital health.
Health Belief (HB)
Positive habits toward health are crucial for developing and maintaining a healthy body. Digital health technologies and applications have gained popularity, offering support in individuals’ journey toward better health. 42 Engaging in positive habits triggers changes in living habits, leading to the perception of digital health tools as more useful. This increased perception can be attributed to factors like tracking progress, personalized features, accessibility, and social support. 43 When individuals make positive changes to their living habits and experience the benefits of healthier habits, they are more likely to perceive digital health tools as valuable and beneficial. Combining healthy habits and digital health technologies can create a synergistic effect, supporting individuals in their pursuit of improved well-being. 44
H3: Health belief has a positive impact on Perceived Usefulness:
Perceived ease of use (PEU)
It is defined as the degree to which individuals perceive how it is to use the technology, and PU refers to the extent to which individuals believe how useful the technology would be. 26
In this model, PEU is an antecedent of PU, a modification of the original model. TAM postulates that PEU and PU influence the user to adopt technology favorably. Here, PEU is expected to positively impact individual perceptions regarding the usefulness of digital health technology. 45
H4: Perceived ease of use has a positive impact on perceived usefulness.
Influence of the Reference Group (RG)
The term “reference group impact” refers to the extent to which the perspective of a reference group influences customers’ (or patients’) attitudes. This refers to any influential persons who form customers’ (or patients’) perceptions of the focal product, such as parents, friends, or assessment leaders. 46 In the context of data innovation products, customers often rely on their reference groups for feedback and ideas, particularly when the goods or products are novel to them. Reference groups provide a sense of social proof, which can alleviate concerns and build trust, and information sharing, which can serve as a valuable source of information. 47 Social proof is created when customers observe others within their reference group adopting and using data innovation products, creating a perception that these products are accepted and valued. 48 Information sharing is also beneficial, as customers may seek opinions, experiences, and insights from individuals within their reference group who have already used or are knowledgeable about the data innovation products. 47 This leads to the fifth hypothesis, which states that a patient’s peer group’s influence substantially affects their propensity to accept new forms of electronic medical care.
H5: The influence of the reference group has a positive impact on the adoption intention of digital health.
Privacy Protection & Data Security (PD)
Digital healthcare technology adoption relies on users’ trust in data security, which involves storing and analyzing health data in databases. Users may worry about the integrity of their information and the consequences of unauthorized access or breaches. 49 To address these concerns, digital healthcare stakeholders must prioritize privacy and data security. Encryption, access limits, and secure storage can protect health data. Transparency in data management, privacy rules, and user permission can build confidence and reduce security issues. 50
Organizations should follow data protection laws and standards to demonstrate their commitment to user data. Organizations can boost adoption and build confidence in digital healthcare technology by addressing privacy and data security concerns. Trust-based framework for virtualized networks and software-defined networking. The study specifically argued for adopting cloud computing to deploy various trustworthy security services over virtualized networks. 51
H6: Privacy Protection and data Security have a negative impact on perceived usefulness.
Online Healthcare Resources (OR)
Healthcare Institutions are spending a huge amount of money creating and maintaining websites. However, it has been found that these websites fail to achieve the objective of attracting people (patients) to online resources. This failure can be attributed to the psychology of the people.52-54 Still, people are apprehensive regarding the reliability of the health-related information provided by Internet resources.
H7: Online healthcare resources have a negative impact on perceived ease of use:
System Capability (SFC)
It plays a vital role in perceived ease of use. One of the main factors leading to PEU is a quick and robust framework for all clients. 55 Furthermore, the similarity and adaptability of the system have also been considered factors to ensure PEU.
H8: System Capability has a positive impact on perceived ease of use.
User Guidance (UG)
User guidance where a man-machine interface takes place is an important indicator of perceived ease of use. Here, self-efficacy comes into play as humans need to play their part with the help of machines. Several studies have found that self-efficacy is an important factor for perceived ease of use 55 ; however, in the case of health-related matters, people are still skeptical regarding user guidance similar to online healthcare resources. In the study “The Role of Internet Self-Efficacy in the Acceptance of Web-Based Electronic Medical Records 56 only 48% of the variation was affected by Internet self-efficacy on PEU.
H9: User guidance has a negative impact on perceived ease of use.
Aligning hypotheses to questionnaire development in studying digital health adoption
In this study, the development of our questionnaire is intricately linked to our hypotheses, ensuring that each question directly addresses the variables and relationships we aim to investigate. This systematic approach allows us to effectively gather precise data to test our hypotheses.
By aligning our questionnaire with our hypotheses, we aim to obtain clear, actionable insights into the factors influencing the adoption of digital health technologies. This structured approach ensures that our research is both comprehensive and focused, enabling us to draw meaningful conclusions and contribute valuable knowledge to the field of digital health.
Questionnaire development
To establish the credibility of the metrics, all measurement components for every variable in the model were altered or derived from pre-existing validated scales employed in pertinent research. As mentioned earlier, the measures have undergone modifications to evaluate individuals’ perceptions and attitudes toward digital health.
The questionnaire consisted of three parts.
(1) The first part pertained to perceived ease of use, including the TAM variables.
(2) The second part included questions on perceived usefulness using TAM and HB variables. 56
(3) The last part included questions on adoption intention that respondents belonged to the socio-techno-demographic class (eg, gender, age group, education level), users of digital gadgets, social media users, and experiential. 57
Variables related to health belief were taken from the Health belief model developed in 1950 by social psychologists Hochbaum and Rosenstock and others working in US Public Health Service. 30
Online resource variables are measured using the questionnaire from “Are Online Sources for Identifying Evidence-Based Practices Trustworthy? 58
Privacy protection and data security variables are measured using the question, “How significant are the accompanying security factors regarding utilizing clinical assistive gadgets?.” 59
Other variables, such as system capability, user guidance, reference group influence, and customer willingness to change, are measured using “Technical attributes, health attributes, customer attributes and their roles in adoption intention of healthcare wearable technology.” 60
The TAM variables of perceived usefulness, perceived ease of use, and intention to use digital health were developed from measurement items published by Venkatesh and Davis and Zhang et al.61,62
Perceived ease of use was measured with 3 # measurement items, and all 3 #items were used as the antecedent of perceived usefulness. Four #items were used for perceived usefulness, and all 4 #items gave good reliability and cross-loading results.
Measurement items
As mentioned in Table 1, the development of our questionnaire is meticulously aligned with our hypotheses to facilitate a comprehensive analysis using Smart Partial Least Squares (Smart PLS). Smart PLS, a robust statistical tool for structural equation modeling (SEM), will enable us to evaluate the relationships between our observed variables and latent constructs.
Measurement items of constructs.

By integrating our questionnaire development with Smart PLS analysis, we ensure a rigorous methodological approach that enhances the reliability and validity of our findings. This connection allows us to draw meaningful conclusions about the adoption intention of digital health solutions, providing valuable insights for stakeholders in the healthcare industry.
Results by using smart partial least squares
Smart PLS- In this review, we utilized Partial Least Squares-Structural Equation Modeling (SmartPLS et al.)) as the method for data analysis. Specifically, employed SmartPLS 3.0 software with the 5000-bootstrap methodology. 63
PLS-SEM was used to assess both the
(1) external (estimation) model and the
(2) internal (underlying) model.
I considered PLS-SEM due to its unique benefits in hypothesis testing and confirmation, which align with the review’s objectives.
Furthermore, PLS-SEM was deemed suitable for this study as it allows for the further development of theoretical model arguments. This means I can refine and enhance the theoretical model based on the PLS-SEM analysis. 64
Additionally, PLS-SEM is advantageous when working with smaller sample sizes, as in this review. It can handle data analysis effectively even with a limited number of observations.
Overall, the researchers chose PLS-SEM as the preferred method for data analysis. 64 This review includes it due to its suitability for hypothesis testing, capacity to refine theoretical models, and ability to accommodate smaller sample sizes.
Primary equation model
The primary equation model is separated into measurement and structural models. The measurement model helps to assess the “reliability and validity” of the construct referred to as the outer model. The structural model will help to determine the relationship between variables. 65 First, we must go to the “Measurement model” and then to “the Structural model.”
Measurement model
Reliability and validity
First, assessed the “Reliability and validity” of the model. Evaluating the factors.
The maximum iteration is 300. The factor is checked.
Measures are good enough to assess the “reliability and validity” of the constructs. I have tried to estimate things’ dependability by looking at their “variable loadings, Cronbach’s alpha, and composite Reliability (CR)” in the estimation model. 63
As detailed in Table 2, the loadings of all things were more noteworthy than 0.782 (except for HB—Health Habit) and critical (ie, the component loadings of things were gone between 0.782 and 0.936).
Construct reliability and validity.

At the same time, Cronbach’s alpha (except HB) and the CR of all of the builds were more prominent than .784, which is beyond the suggested .70 limits, affirming the unwavering quality of the estimation things and builds as revealed in Table 2.
Two sorts of legitimacy: (1) convergent validity and (2) discriminant legitimacy. I have tried the concurrent legitimacy of the model utilizing the normal difference removed “(AVE),” as all of the “AVE” estimates were bigger than the suggested worth of 0.5, affirming the united legitimacy of the builds.
Finally, the “discriminant legitimacy” (separation of the builds) was tried by utilizing the Fornell and Larcker (Table 3) standard, cross stacking, and the HTMT (Table 4).
Fornell-Larcker criterion.

Heterotrait-Monotrait Ratio (HTMT).

Fornell and Larcker Table: “The AVE square roots” were bigger than the comparing relationships, exhibiting “discriminant Legitimacy.”
The HTMT ratio (Table 4) should be less than 0.85 in some cases and 0.90 (Henslley); however, some problems were noticed in the constructs; hence, the constructs are validated through the factor loadings/cross loadings (Table 5).
Cross loadings (factor loadings).

The factors are loaded better with their parent constructs or not. The respective items, such as (F1, F2, and F3), are well-fitted with their parent construct SFC.
Similarly, the construct in question UG comprising items UG1, UG2, and UG3 shows better loading with the parent construct UG than any other constructs, which confirms the discriminant validity (Table 5).
After rigorously testing the validity and reliability of our model, we will proceed with hypotheses testing to evaluate the relationships between identified variables and their impact on digital health adoption intentions. This statistical analysis will reveal significant factors influencing user decisions, confirming our theoretical framework. This study aims to provide the design and implementation of effective digital health strategies. By understanding the factors that drive or hinder adoption, we can better support integrating digital health solutions into everyday healthcare practices, ultimately improving health outcomes and enhancing the overall healthcare experience.
Hypothesis testing
Structural modeling
Bootstrapping: It amplifies existing data to samples.
Path significant
I have used SmartPLS 3 with the 5000-bootstrap procedure to test the hypotheses in the theoretical model. Figure 2 presents the results of the structural model.

Represents good correlations between latent variables with significant T and P-values.
The hypotheses were tested by examining the t-values, P-values, standardized coefficients beta values, and the coefficient of determination (R2 value). A hypothesis was accepted when the t-value was larger than the critical value (ie, t > 1.96, P < .05), being marginally accepted when the t-value was larger than the critical value (ie, t > 1.67, P < .10), using a two-tailed test.
As Figure 2 reported, the results support 7 of the 9 hypotheses. Regarding the antecedents of perceived usefulness (PU), the impact of perceived ease of use(PEU) on perceived usefulness (PU) was the strongest (Beta = .704, t = 12.812, P < .001), followed by health belief (HB) (Beta = .176, t = 3.827 P < .05), supporting H3 and H4 as shown in Table 6.
Mean, standard deviation, t-values, P-values-total effects.

However, the impact of privacy protection (PD) on perceived usefulness (PU) was weak and non-significant (Beta = .017, t = 1.339, P > .05), rejecting H6.
Regarding the antecedents of adoption intention (AI), the impact of Reference group influence (RG) on adoption intention (AI) was strongest and significant (Beta = .529, t = 4.949, P < .001), followed by perceived usefulness (PU) (beta = .208, t = 4.084 P < .001) and customer innovativeness (CWI) (beta = .212, t = 2.123 P < .05). Therefore, H1, H5, and H2 are supported.
(Beta value calculated − Standard Deviation × T statistics).
Furthermore, the results also presented the indirect effects of the exogenous variables, including health belief, perceived ease of use, user guidance, system capability, and privacy protection, on adoption intention.
In particular, the indirect effects of health belief-HB (beta = .036, t = 2.831 P < .05), perceived ease of use-PEU (beta = .037, t = 3.884, P < .001), and system capabilities-SFC (beta = .131, t = 3.859, P < .001) on adoption intention were significant.
In contrast, the indirect effects of user guidance (UG), online resources (OR), and privacy and data protection (PD) on adoption intention (AI) were non-significant.
Table 7 exhibits the results of the indirect effects on Adoption Intention by the exogenous variables of this study.
Mean, standard deviation, T-statistics, P-values, indirect effects.

The significance of the “exogenous factors” is tested in the hypothetical model by utilizing “Cohen’s f2 investigations,” and the impact size of the exogenous factors is tested as enumerated in Table 8.
f-Square (f2).

As indicated by Cohen, the “f2 values” were evaluated as f-square 0.02 (ie, f2 ⩽ 0.02), 0.15 (ie, f2 ⩽ 0.15), and 0.35 (ie, f2 ⩽ 0.35), addressing little, medium, and enormous impacts of the exogenous inactive factors, respectively.
The outcomes show that the impact size of online resources (f2 = 0.022), Health belief (f2 = 0.082), HB, perceived usefulness (f2 = 0.073), PU, and customer innovation (f2 = 0.046), CWI were small to medium.
In contrast, the impact size of the reference group (f2 = 0.434) RG was medium to enormous. The outcomes reveal that the “exogenous factors” impact the hypothetical model.
Critically assess the logical force of the examination model by surveying the “R2 estimates” (see Table 9). The “R2 estimates” for the perceived ease of use (PEU), perceived usefulness (PU), and adoption intention (AI) were 0.791, 0.649, and 0.0684, respectively.
Quality criteria-R square.
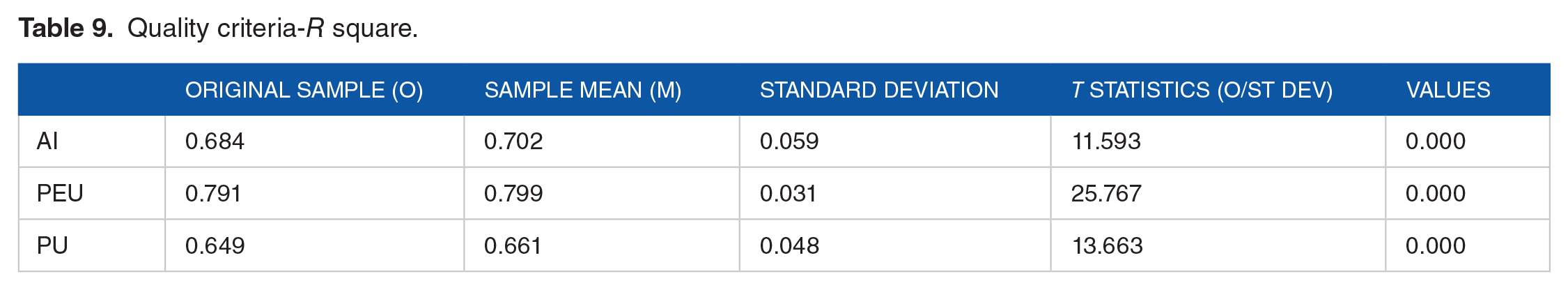
Therefore, features of these exogenous developments clarify 79.1% of perceived ease of use (PEU), 64.9% of perceived usefulness (PU), and 68.4% of adoption intention (AI), respectively.
To put it, as the R2 estimates surpass the suggested benchmark of measure (ie, >0.10), the outcomes recommend that the exploration model clarify a significant measure of variety in the “endogenous factors,” which has been exhibited in Figure 2.
Validating the research model for digital health adoption
Our study confirms that perceived usefulness, ease of use, system capability, health belief, customer willingness to change/innovate, and social influence significantly impact the intention to adopt digital health solutions. These findings highlight the need for user-friendly design, innovative solutions, robust approaches toward data privacy, and strategies that increase health awareness and leverage social networks to promote digital health adoption.
Hypothesis result
H1: Perceived usefulness has a positive effect on Adoption Intention.
H2: Customer innovation positively affects adoption intention support.
H5: Reference Group Influence has a positive effect on Adoption Intention-Supported.
H3: Health belief has a positive effect on Perceived Usefulness.
H4: Perceived ease of use has a positive effect on perceived usefulness-supported.
H6: Privacy protection and data security have a negative effect on perceived usefulness.
H7: Online healthcare resources have a negative effect on perceived ease of use-supported.
H8: System Capability has a positive effect on Perceived Ease of Use Support.
H9: User Guidance has a negative effect on Perceived Ease of Use-Supported.
Theoretical implications
This review recognizes and observes the collaborative impacts of health beliefs (wellbeing-related properties), customer innovation or innovation, reference group influence (social effects), system capabilities, user guidance, perceived ease of use, and perceived usefulness. It provides some hypothetical ramifications and supplements the current knowledge base in digital healthcare adoption. 66 This review expands on the current study by analyzing the effects of wellness conviction, system capabilities, usability, user direction, and the influence of reference groups on perceived value as direct and indirect outcomes of digital healthcare adoption, all of which contribute to better healthcare delivery. 67 The findings show that patients’ sense of well-being, convictions or health beliefs, the influence of their peer group, the system’s capabilities, and the convenience of use profoundly indirectly affect their reception objectives. 68
Security assurance is most likely not a crucial aspect of digital health adoption, notwithstanding the surprising finding that data security and privacy have a negligible impact on seen value. 69 Before the advent of perceived ease of use online, resources for medical treatment and user instructions did not matter much. 32 Conversely, system capabilities (with similarity and flexibility) emerged as a robust key antecedent of “perceived ease of use.” 70
There was a clear relation between perceived ease of use and perceived usefulness. 71 Second, the findings reveal that patients’ adoption intention of digital healthcare is significantly preceded by perceived usefulness, customer in innovation, and reference group influence. 72
The findings of this study confirm the findings of previous research that utilized reference group influence and perceived usefulness to clarify reception goals regarding data innovation items and the effects of social media, demonstrating that patients’ intention goals necessitate obvious convenience in addition to factors like accessibility, medical relevance, and novelty. 73 This quantitative research presents the patients’ path to such recognition using the modified form of TAM to examine the desired aim of digital health adoption.
This research confirms that community impacts and innovation utilization strengthen patients’ adoption intentions, such as belief in the benefits of healthy habits, perceived ease of use, and the system’s capability.
Summary of Empirical Findings: Conceptualization With the Adoption of Digital Technology in Healthcare
The concept of the patient as an organization with digital technology intrusion is based on several preceding ideas and developments. The following important precursors influenced the emergence of this concept:
Patient-centered care is an approach that prioritizes patients’ active participation in their healthcare decisions and treatment plans. 74 It acknowledges the significance of patient perspectives, preferences, and values in determining the shape of healthcare delivery. The concept of the patient as an organization strengthens the patient’s involvement in actively administering and organizing their healthcare using digital technologies. 75
The rise of digital technologies has facilitated greater patient empowerment and participation. Patients now have access to abundant health information, online communities, and resources that empower them to play a more active role in their healthcare. 76 Using digital platforms, Patients can educate themselves, access their health records, participate in collaborative decision-making, and contribute to healthcare discussions. 77
The introduction and development of digital health technologies have revolutionized healthcare delivery. Digital health includes electronic health records, telemedicine, wearable devices, mobile applications, and health monitoring instruments. 78 These technologies have facilitated the accumulation, storage, and exchange of health data, allowing patients to manage their own care actively.
Health Information Sharing and Access: The digitization of health records, test results, and health knowledge has increased accessibility. Patients can access and exchange their health information electronically with healthcare providers, facilitating care coordination and communication. 79 This access to health information is the foundation for the patient as an organization, as patients can use it to organize and manage their healthcare.
The e-patient movement is a developing community of empowered patients who use digital technologies to manage their health and advocate for their well-being. 80 E-patients search out health information online, participate in online communities, and share their experiences and knowledge. This movement emphasizes patient autonomy, informed decision-making, and patient-provider partnerships. 81
These precursor concepts and technological advancements have paved the way for the emergence of the patient as an organizational concept. It envisions patients as active participants and organizers of their healthcare, utilizing digital tools and resources to make informed decisions, administer their health information, and collaborate with providers.2,82 The concept acknowledges the potential for digital technology to revolutionize healthcare by empowering patients and encouraging a more patient-centered approach to care.
In summary, the “patient as an organization” concept puts patients in charge of their health and healthcare decisions. Patients may choose, set goals, and self-manage using this strategy. This method emphasizes patient-provider collaboration, shared decision-making, and open communication. It improves patient happiness, health outcomes, healthcare costs, and efficiency. Health records, collaborative decision-making, health education, and digital health technology may empower, engage, and collaborate with patients.
This concept emphasizes patient empowerment and involvement and a patient-centered healthcare system that satisfies social expectations. 83 It guarantees that the adoption of digital health is linked with the values and requirements of patients as active participants in their care and also producers of resources, that is, DATA scripting a unique patient entity.
Discussion
Organizational perspectives related to patients
Patient bodies that are digitized and thus able to become engaged and activated, to take control of their health and to create their data on themselves and share these data with others also to access the info produced by medical testing. 84
This section of the article presents the notion of the body’s multiplicity. Therefore, the human body can be examined through three distinct structural levels that align with the three primary categories of cultural elements: artifacts, norms, and meanings. 85 The aforementioned levels may be regarded as facets or constituents of an entity.
While scrutinizing the human body from an anthropological standpoint, it is advisable to consider it as a cultural object molded and impacted by diverse extrinsic elements such as body modifications, medical intervention, and biomedical innovation. 86 As mentioned earlier, the phenomenon can be interpreted as an organizational facet, given that the aforementioned extrinsic factors play a role in molding the physical form into a cultural construct.
Furthermore, it suggests analyzing the human body about societal norms and customs. Norms are informal regulations that dictate conduct within a specific cultural milieu. They are organizational components that direct and organize how individuals engage with and understand their physical selves. 87
Additionally, the authors underscore the significance of comprehending the body about its connotations within a given cultural milieu. Attributing importance to the human body can be considered a structuring principle that influences an individual’s self-concept, sense of self, and interpersonal relationships. 88
Within cultural anthropology, the impact of artifacts, norms, and meanings on the human body can be regarded as organizational elements, even though the body itself is not an organization. 89
Gareth Morgan’s “Images of Organization” is a classic in organizational theory and management. He employs various metaphors about machines, organisms, the brain, and even cultures to depict the inner workings of organizations. Such metaphors are not flawless and may be susceptible to prejudice and limits, but they assist in obtaining a greater understanding of the complicated and multidimensional nature of organizations. 90
This analogy compares businesses to living organisms, highlighting the necessity of specific conditions and resources for survival and prosperity. Just as patients require ongoing adaptation and adjustment to changing conditions and environments to maintain their health, businesses must also engage in continuous adaptation and adjustment to remain viable.
Like the essential resources a patient needs to sustain life, businesses also require a range of resources, including capital, employees, technology, and market demand, to ensure their survival and expansion. The absence of these fundamental resources would impede the optimal functioning of both patients and businesses. 91
Moreover, both patients and businesses must consistently adapt to novel circumstances. To sustain their overall health, individuals must acclimatize to alterations in their physical condition, daily routine, and surroundings. 92 Businesses must respond to changes in market conditions, industry trends, technological developments, and customer preferences to maintain competitiveness and succeed. 93
Similar to patients, businesses necessitate effective management and decision-making. Healthcare providers are crucial in making informed decisions about their patient’s health and treatment options. 94 Likewise, enterprises depend on their management teams and leaders to formulate strategic judgments that impact their functioning, expansion, and comprehensive triumph. 95
The analogy above drawn between businesses and patients underscores the fluidity inherent in the former and the imperative of ongoing adjustment and administration to ensure their viability and achievement. 96
Patients, like organisms, may be considered organizations; the two concepts are analogous. Comparing the structure, function, and dynamics of organizations to those of biological creatures is common in organizational theory and management studies. 97
Like a corporation, an organism comprises many pieces that must work together to complete a task. A patient might be thought of similarly as an organism with interconnected parts that must all be healthy and functioning to stay that way. 98
When we adopt the organism metaphor, patients are seen as more than simply treatment recipients. They become seen as active participants with their own unique set of systems and processes. They are like organisms in that each has specific requirements, skills, and ways of dealing with the environment. 96 From this vantage point, the patient’s ability to take charge of their care and adjust to shifting health conditions is emphasized. 99
The organism metaphor also emphasizes the interdependence of many parts of a patient’s healthcare experience. Patients depend on their healthcare professionals, technology, and support systems in the same way as organs in a body rely on each other for optimal functioning. 100
The intricacies and dynamics of patient care may be better understood if healthcare workers and stakeholders consider patients as organizations or organisms. It advocates for healthcare that takes into account not just the person receiving treatment but also their social and environmental setting and the interconnections between them. 101
The metaphor of an organism as an organization may be helpful, but it’s vital to remember that it’s not meant to be taken too literally. 102 Patients are individuals with their own set of priorities and perspectives who may not perfectly fit the mold of a conventional group or organism. However, a patient-centered approach that recognizes and values variation and uniqueness is necessary to fully realize the metaphor’s potential for illuminating the patient’s position and dynamics within the healthcare system. 103
Inside or beyond hospital boundaries, patients are to be treated akin to the organization as a means of producing and customer of real-time data, which will further ensure better coordination of clinical and non-clinical pathways to deliver high-quality care. 96 As illustrated in Figure 3, access to relevant information in real-time will help overcome potential bottlenecks. For example, if the flow of patients through the care journey is delayed, services such as other appointments, cleaning, transportation, meal ordering, and others are also pushed back. Real-time data will also enable health intervention before problems occur. 104 Ultimately, all stakeholders benefit from having access to a 360° understanding of all relevant data—clinical and nonclinical. 105

Generation & accessing of clinical and non-clinical data image adaption: DXC technology.
Connecting the dots to relate patients with organization
The implications discussed show the characteristics of open systems. They involve developing a design that effectively manages information exchanges in the form of data across different organizations through data interoperability and ensuring data security through proper surveillance and monitoring.
Healthcare Data interoperability is defined as the ability of different information technology systems and software applications to communicate, exchange data, and effectively allow patients and healthcare practitioners to use that information. 106
To survive and thrive, patients in organizations are conceived as customers of resources (availing healthcare services through the adoption of digital health), and resource exporters (producers of data) must adapt to the changing environment similar to open systems. 107
Various countries, such as the Global Digital Health Partnership (GDHP) and the EU EHR Exchange Format, have taken initiatives to exchange patient healthcare data to alleviate the first challenge. The eHealth Digital Service Infrastructure is ushering in an infrastructure of healthcare data continuity across borders, allowing the exchange of basic health information, such as e-Patient Outline and e-Prescriptions. Various European Union nations are using the X-load Platform to exchange e-patient summaries and e-prescriptions. 108
Finland and Estonia were the first to implement the infrastructure to exchange patient summaries, protecting privacy. Plans are underway to trade diagnostic tests in radiology and pathology. The European Commission laid out needs for the “2019-2024 EU Digital Strategy,” which included creating a European Health Data Space. Nordic countries have an integrated basic-level initiative of patient data exchange within their member countries to ensure seamless treatment. 106
In Asia and the South Pacific, numerous Asian nations also embrace advanced well-being methodologies to guarantee interoperability. The Ministry of Health and Family Welfare (MoHFW) of India has previously distributed Electronic Health Record norms and shaped a Center for Health Informatics under the aegis of their National Digital Healthcare Mission (NDHM). 109 New Zealand’s medical care offices, patients, and people marked a commitment to “New Zealand health interoperability” to diagram the orders to foster the reception of trade foundations and cycles in their well-being area.
Since open systems thinking aims to provide frictionless interaction with external factors, a common industry standard is required to unlock the data inside them. FHIR (fast healthcare interoperability resources) plays a critical function by facilitating communication with external programs. 110 Then, NIH (National Institutes of Health) researchers may encourage third-party apps to strip an FHIR API of sensitive clinical data to advance the field of wellness disclosures. 111
FHIR (fast healthcare interoperability resources) is crucial in interacting with third-party applications. An eBusiness-based Framework for eHealth is proposed to consolidate norms that are available to laypersons, such as the reception of customer-situated phrasings while planning them to clinical codes and the reception of an originally driven worldview of demonstrating data content in a particular and reusable manner. 110
Description of the subsystem akin to organizational subsystem:
FHIR workflow: There are 3 main functional blocks or components considered in the solution, as shown numbered in the diagram below:
FHIR API Convertor Historic health data come in various formats (JSON, PDF, Excel, Bio market Dataset) from different sources, including existing solutions linked to Social Media and Wearables, HIP, etc. The FHIR converter runs as a REST web service and can be deployed in the cloud. It takes the historical health data as input and converts it to FHIR bundles. These bundles can persist to an FHIR server such as the FHIR API. 112
AI/ML engine for prediction, diagnosis, and recommendation. This component accomplishes the following:
Feature Construction and Feature Selection are 2 components of predictive modeling. Feature Construction processes an element vector portrayal for each patient based on their EHR information, while Feature Selection extracts highlights for hazard forecasting. 113 Predictive Modeling Pipeline uses AI/ML techniques to empower secure and reliable division of wellbeing data among customers and suppliers, while also guaranteeing the nature of patient-situated eHealth frameworks and the constancy of their administrations. 114
FHIR Prediction Bundle to persist predictions.
The quality and reliability of patient-centered eHealth systems need the development of components at the framework and responsibility levels. It is important to develop strategies for compensating eHealth authorities for the services they provide. 115
Data security and surveillance
Blockchain—To ensure organizational (patient) data security
Healthcare data security is essential for digital health progress, and blockchain can play an important role in preventing a breach of healthcare data. The cloud has become increasingly important in healthcare due to convenience and savings, as it enables healthcare data management at an affordable cost. Interconnecting healthcare providers and their Patient Health Record solutions will help them take urgent or proactive action during any eventuality. Blockchain can play an indispensable role in preventing a breach of healthcare data, which can save millions of dollars. 116
Surveillance tool for organizational data (Biomets)
To survey more nuanced characteristics, like emotions and behavior, the organization (here, the human body) keeps tabs on clients’ qualities identified with conscious and unconscious changes in human attributes and body boundaries, like demeanor, inspiration, temperature, skin conductance, pose balance, mind action, pulse elements, and other crucial boundaries. With IoT technology, all biometric monitoring devices may wirelessly communicate with one another and transmit this data. Consequently, home care devices are now outfitted with technologies that allow physicians to remotely monitor and check patients at the push of a button, thanks to the proliferation of remote care technology. 117
BioMeT is a system that integrates software and hardware to improve medical applications. Confirmation and approval have always been integral parts of the board cycle for quality control in both software and hardware and their respective administrative parent companies. The IEEE Standard for System, Software, and Hardware Verification and Validation (IEEE 1012-2016) is used as a roadmap for testing the integrity of software and hardware in Internet-connected gadgets. 118
The patient is an individual—Can it be considered an organization?
Although it may seem counterintuitive to treat an individual patient as if they were an organization, this is necessary for a holistic, patient-centered approach.
In “Medicine as Culture: Illness, Disease, and the Body” by Deborah Lupton, it is stated, about the work of Deleuze and Guattari, that “the body, health, and identity” are inseparable and interdependent entities that constitute each other in a mutually dependent interchange of practice, meaning, social relations, and relations with objects, reinforced the idea of developing the Patient as an organization. 119
She also addressed the state’s role, which, as she put it, “executes supervisory action and controlling bodies” to establish guidelines for how people like patients “self-regulate and regulate their bodily deportment.”
According to Turner, “the body is a metaphor for social organization and social anxieties, the primary field of cultural and political activities.” Central to somatic society are the control, surveillance, and monitoring of bodies and the spaces between them. 120
Nancy Scheper-Hughes and Margaret Lock proposed a study on medical anthropology, focusing on the individual, social, and political bodies. This study returns to the “three bodies” notion, focusing on translational competency and fostering successful interactions between medical and non-medical practices. The first is each person’s unique perception of their own body, which may be distinguished from the perceptions of others. 121
Discourses that talk about a “sick society,” the “foot of the mountain,” or the “head of state” are examples of the second idea, the social body, or the symbolic representational uses of the body conceptualizing nature, society, and culture. 122
To keep societal “stability” at bay, the state controls, regulates, and surveys individual and group-level bodily behavior via biopolitics at the third level. 122
The medicalized body, the sexual body, the disciplined body, and the talking body are the 4 forms of physical selves that Frank outlines. The lines delineating these categories must be somewhat porous. Other sorts of bodies are also tied to the medical system, but the medicalized body is the most obviously linked to the medical care of sickness in its name. 123
The third level of biopolitics saw the emergence of a new dimension with the advent of digitization: the digital incarnation of the body or the virtual self in the form of data. Therefore, the state’s monitoring and surveillance included the patient’s virtual and physical selves. 124
Relevance
The research studies show that a new conceptualization is necessary for a patient-based healthcare model. Self-care, self-management, health literacy, resilience, and self-efficacy concepts are imperative to improving quality care, health, and well-being for all. 125
Accessibility to healthcare by overcoming barriers like cultural competence, age, gender, and psychosocial characteristics enables advocacy, acuity, engagement, and trust to improve patient-centered care. 126
Conceptualizing—“the patient as an organization” after exploring various attributes and the existing concepts leads to a new concept, redefining a new paradigm of patient approach toward a new healthcare model.
Further technological intervention can play a very important role in substantiating this new concept in various ways:
As a tool of patient engagement, advocacy, acuity, self-management, self-care, and self-efficacy.
Removing cultural competence, age, gender and language barriers.
Improving social factors, health literacy, trust, involvement, satisfaction.
It acts as a common thread to stitch these various attributes and concepts together, channeling them toward the birth of the “patient as an organization” concept.
As part of technology intervention, the Patient as an Organization concept can be applied to the 6D exponential growth model. 127
The 6D model is a framework that depicts the various phases of digital transformation, from early technology adoption to developing new business models. Digitization, deception, disruption, demonetization, dematerialization, and democratization comprise the 6Ds. 128
Digitization is the process of converting analog information into digital format. In healthcare, digitization can entail using electronic health records (EHRs), mobile health applications, and other digital tools to acquire, store, and analyze patient data. 129
The term deception refers to the fact that digitization’s initial impact may be minimal, but it can increase exponentially over time. As more data is collected and analyzed, the potential benefits of digitization become more apparent. 130
The term disruption refers to how digitization can disrupt conventional business models and methods of operation. 131 For instance, transitioning to patient-centered care and self-management may necessitate evaluating healthcare providers’ roles and responsibilities.
Demonetization is the process by which digitization can reduce or eliminate the costs associated with traditional healthcare practices. 132 Telemedicine, for instance, can reduce the need for costly in-person consultations.
Dematerialization describes how digitization can reduce the need for physical materials, such as paper documents and diagnostic apparatus. 133 For instance, wearable devices can monitor patient health without invasive procedures. 134
Digitization is the process by which patients can be empowered and granted greater control over their healthcare. For instance, patient portals and mobile health applications can facilitate patients’ access to their health information and communication with healthcare providers, ushering in an era of healthcare democratization. 135
Applying the 6D model to the concept of the Patient as an Organization, we can see how digitization can enable patients to take a more active role in administering their health, via patient portals, mobile health apps, and wearables. 136 As more data is collected and analyzed, the potential benefits of patient self-management become more evident, disrupting traditional healthcare models and resulting in cost savings and increased patient autonomy. 96 Hence adoption of digital health is an important factor toward achieving this goal.
The care model is meant to be patient-centric, with better coordination and integration of various care procedures and access. The patient’s emotional and psychological needs will be better met if the doctor takes more of an interest in them. 137
Encouraging self-management by monitoring will ensure better primary and preventive care. 138
Delivery of holistic care involves communication, measuring, diagnosing, and providing treatment with AI-embedded tools, that is, combining genomics with digitization. 139 will facilitate the active participation of patients as an organization.
Limitations
Digital health can potentially improve healthcare delivery, particularly in primary healthcare research. However, it faces several obstacles, including patients’ health literacy, cultural competency, and engagement. Patients may lack the skills necessary to use digital health technology efficiently, reducing their involvement and engagement in research. Cultural competency may also be a constraint, as diverse communities may not benefit from certain digital health technologies due to cultural differences. 140
Engagement is crucial for using digital health technologies, but patients may hesitate due to privacy, security, and treatment quality concerns. Advocacy is crucial for adopting digital health technology, as patients need access to advocates who can help navigate privacy and security concerns. 141
Acuity is another barrier to the widespread use of digital health solutions, as patients with complicated medical illnesses may not be able to benefit from digital health technology fully. 142 Addressing these restrictions and ensuring that digital health technologies can effectively improve primary healthcare outcomes for all patients is essential to ensuring the successful use of digital health technologies.
Conclusion
Global healthcare customers are now more aware that high-quality medical care is accessible. Patient preferences often include important aspects of patient-centered care, such as access to treatment, family and career participation, transition and continuity, physical comfort, emotional support, and respect. Meeting these aspirations via the coordinated efforts of all healthcare professionals may contribute to the success of the nation’s healthcare system. 143
It is important to note that the successful implementation of a patient-centered healthcare model, including the Patient as an Organization concept, requires not only the adoption of technology but also a cultural shift in healthcare organizations and the involvement of all stakeholders.
It involves fostering a collaborative and transparent relationship between patients and healthcare providers, integrating technology effectively into care delivery processes, and addressing any possible barriers or challenges. 144
Patient-generated data provides a concrete example of patients’ roles as resource creators. Patients are producing an immense amount of data on their health because of the proliferation of wearable gadgets and health apps. 145 This information may be used to understand better the patient’s health, habits, and response to therapy. Contributing to better healthcare practices, research, and resource allocation is voluntarily sharing patient data with healthcare professionals and researchers.
In conclusion, “Patient as an Organization” emphasizes the significance of patient participation in healthcare and the necessity of acknowledging patients’ rights as active healthcare stakeholders and data owners. Patients may not create resources in the conventional sense, but their contribution and input, especially in patient-generated data, may influence healthcare laws, policies, and procedures. It will lead from the exploitation to the ethical utilization.
Footnotes
Acknowledgements
I acknowledge Anusha Dasgupta’s contribution to formatting the figures.
Funding:
The author received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
I have conceived and researched the whole study.
Ethics Approval and Consent to Participate
The Central Drugs Standard Control Organization (CDSCO) under Directorate General of Health Services, Ministry of Health & Family Welfare, and Government of India is the National Regulatory Authority (NRA) and responsible for approval of Drugs/Device, Conduct of Clinical Trials and Clinical Investigation, laying down the standards, control over the quality of manufacturing and import of Drugs/Device in the country and coordination of the various activities with State Drug Control Organizations and uniform enforcement and implementation of the Drugs and Cosmetics Act and its provisions in country.
As per current regulation it is mandatory to take Ethical Committee clearance for a clinical trial or a study on human being for new drug/device or to modify and make to new claim which includes the indication, route of administration, dosage of existing approved drug/device from a registered ethical committee under Rule 122DD and informed consent according to Appendix VIII of Schedule Y of Drugs and Cosmetics Act, 1940 and Rules 1945 regulated by the Central Drug Standard Control Organization (CDSCO), Office of Drug Controller General India (DCGI), Directorate General of Health Services, and Ministry of Health and Family Welfare.
However, in the proposed survey article “Adoption of Digital Healthcare,” I wish to produce a few facts and points that will illuminate the article’s position and its non-applicability to the aforementioned regulation.
The Adoption of Digital Healthcare survey does not include any physical involvement of human being and not affecting their right, well-being, and safety.
The Adoption of Digital Healthcare survey is not being done for generating the data for discovering and/or verifying the clinical, pharmacological (including pharmacodynamics and pharmacokinetic), and/or adverse effects with the objective of determining safety and/or efficacy of the new drug or device.
The Adoption of Digital Healthcare survey not being performed in laboratory, clinic/hospital and therefore not attract any research protocol which required to be complied with Good Clinical Practice and then Ethical Committee approval.
The Adoption of Digital Healthcare survey is being done for Academic Purpose only and will not be used for any commercial or promotion of any product, or material in any manner.
Hence it is stated “where the results of such a trial are intended to be used only for academic or research purposes and not for seeking regulatory authority of any country for marketing or commercial purpose are referred to as Academic Trials and do not require permissions.
Please refer to the following links.
Therefore, in the light of given facts, we confirm that Adoption of Digital Healthcare survey is not fall under the scope of Ethical Committee clearance and purview of Appendix VIII of Schedule Y of Drugs and Cosmetics Act, 1940 and Rules 1945.
In order to support the aforementioned request, we are producing some links available in public domain for your reference and kind consideration as follows:
As the author, I am duly reporting that the questionnaire collected through Google Forms followed ethical norms, as respondent privacy has been maintained with the utmost care. Anonymized survey data has been used in this study following the ethical norms of the affiliated institution, MDI, Gurgaon.
The Helsinki Agreement has been fully followed in this study as no human element and data obtained from human subjects through monitoring, measuring, and diagnostic studies have been used in this manuscript.
As a Digital Health Drafting Committee member under NABH, I am fully aware of the data privacy and security policy.
The author’s reporting survey of human participants confirms that all methods were carried out according to relevant guidelines and regulations.
MDI CRE ( Comprehensive Research Evaluation) Committee has cleared this study.
Availability of Data and Materials
Will be provided when required. Primary data are available.
