Abstract
Digital twins (DT) technology has shown considerable growth in recent years. Previous studies have examined technologies in a variety of areas, including health care. However, limited studies have attempted to provide a thorough discussion of strategies for the seamless integration of DT into health care, particularly in the context of interoperability of heterogeneous medical data. This review examines the underlying concept of DT and its possible integration in healthcare, particularly in the context of healthcare interoperability. It also analyzes the main problems such as the lack of standardized protocols, the non-homogeneity of data formats and technical complexity. Finally, potential opportunities are highlighted such as standardized protocol, the creation of an open data platform and the empowerment of semantic interoperability. In conclusion, this review has provided valuable insights for many professionals, including researchers and healthcare providers, which will contribute to empowering patient-centered or personalized medicine and to the development of digital health.
Keywords
Introduction
In recent years, transformative shifts have been witnessed with the emergence of disruptive technologies through Industry 5.0. Alongside with the rise of artificial intelligence (AI), machine learning (ML), and data analytics, a new Internet of Things (IoT)-driven technology called digital twins (DTs) has gained traction across industries worldwide. 1 Since its introduction, various industries, and academic fields, including healthcare and biomedical engineering, have actively adopted and incorporated DT technology to increase productivity and capstone innovation. As of 2019, the Gartner Group, a leading research and advisory firm, has highlighted digital twin (DT) technology as one of the 10 most important strategic technological trends.2,3 At its core, the DT introduces physical system virtualization. This technology has an important role to play in promoting efficient use of information at both the physical and digital levels. The Digital Twin was first used in the lifecycle of project management in 2002. 4 Due to its invaluable benefits in data collection, processing, interpretation, and collaboration, DT has become an important integrated tool in wide range of areas, including smart cities and urban spaces, freight logistics, automotive, engineering and medical. 5
In healthcare, DT technology has been extended through the concept of the Medical Digital Twin (MDT). The MDT enables digital patient twinning to predict causes and effects of virtual models, thus advancing personalized medicine. Using these predictive capabilities, MDT is consistently used in clinical trials, research, and development in the medical and biomedical engineering fields, 6 facilitating refined therapeutic strategies and improving patient outcomes. Given its widespread adoption and the potential to improve the efficiency of care, reduce costs, and enable data-driven decision-making, MDT will benefit not only healthcare providers and patients but also other stakeholders, including insurers, through better risk assessment and policymakers, through well-designed healthcare policies.7,8
Despite their crucial importance for successful implementation, several studies have concentrated on significant challenges in digital twin technology, such as cybersecurity and data privacy, 9 enabling technologies, 10 and technological literacy. 11 Continuous efforts have been proposed and substantially deployed, as demonstrated in the previous studies, to address these challenges. 12 However, while these efforts are essential in all areas, there are specific challenges in integrating digital twins into the health sector, especially in terms of interoperability.
The digital twin is generally well known in pioneering industries sectors such as manufacturing and construction, where the implementation is usually based on structured and standardized data. Health interoperability, on the other hand, is a critical area where full implementation is very demanding and proving even more for the digital twins. This is mainly due to the sheer variety of health data formats, as illustrated by the fundamental difference between clinical reports and medical imaging. The ability of healthcare systems to exchange and interpret data seamlessly between different platforms remains a major barrier to the full potential of the digital twins in the sector.
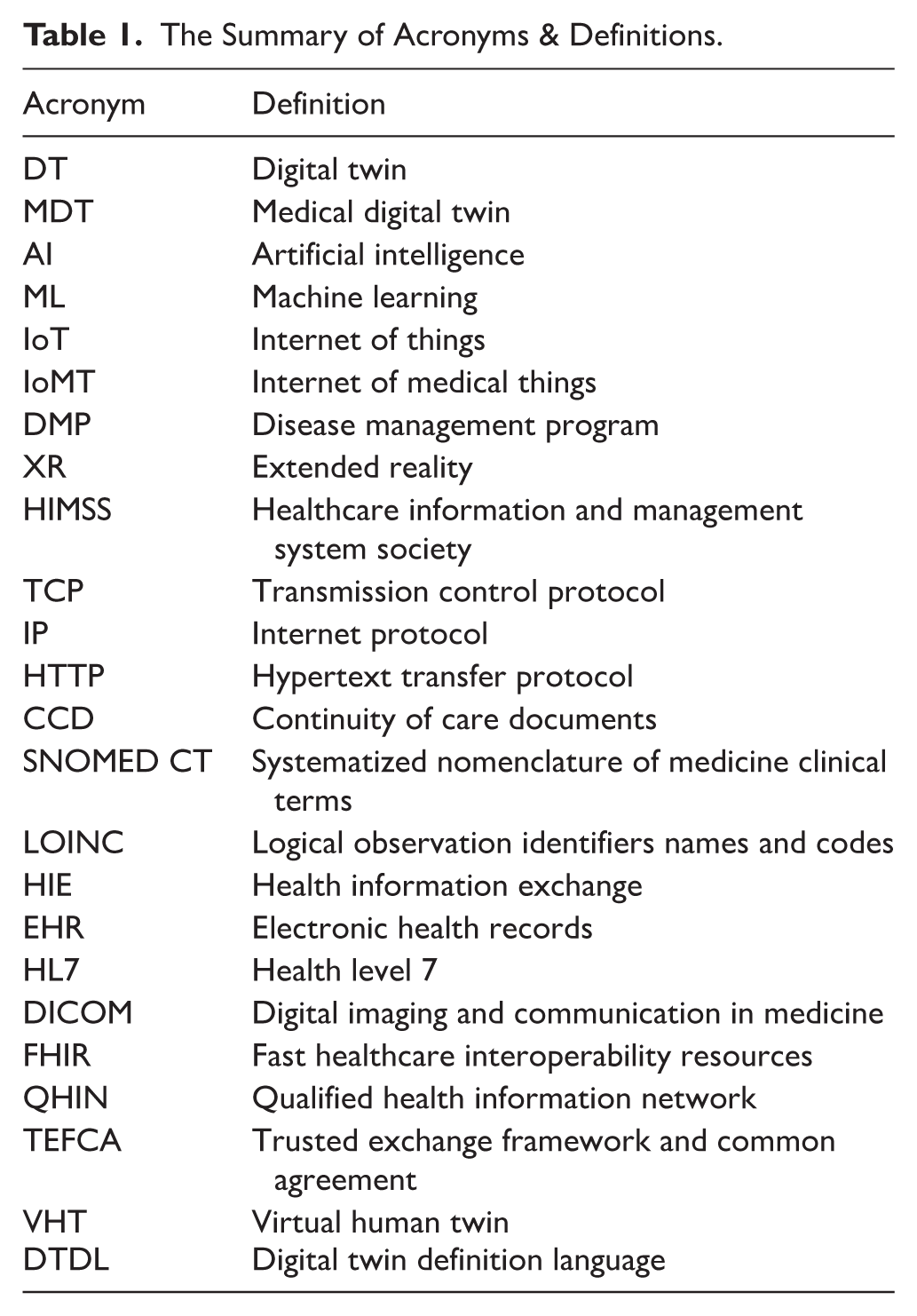
This review provides 3 key contributions. First, it introduces the fundamental concept of healthcare interoperability and its integration with MDT technology. Second, the study identifies the key challenges that hamper smooth interoperability practices using MDT. Finally, the paper highlights potential strategies to overcome these challenges, and highlights the importance of flexible integration approaches that can adapt to the evolving landscape of health technology. For a quick and convenient reference, the acronyms and their definitions are provided in Table 1.
The Summary of Acronyms & Definitions.

Search Strategy
To address the main conceptual gap identified above, this article establishes a middle ground between the IT-driven and health informatics perspectives. This approach offers a balanced yet tangible foundation for multiple disciplines, which examined in the narrative review focused on the integration of digital twinning and interoperability in healthcare. The literature search was designed to capture both peer-reviewed and gray literature relevant to the interdisciplinary subject. Selected conference proceedings were also included due to their high relevance and significant contribution to emerging themes in the field. Sources were retrieved from major scientific databases and repositories, including Google Scholar and IEEE Xplore, using keyword combinations such as “digital twin,” “healthcare,” “medical,” “interoperability,” and “facility.” To narrow down the search, these terms were linked together using Boolean operators (AND, OR). The review has been scoped to publications from 2019 to 2024 to ensure a focus on the latest trends and technologies.
Overview of the Digital Twin and Healthcare Interoperability
Digital Twin
The Digital Twin (DT) technology extends beyond simple computational modeling to encompass a wide range of applications. Given the diverse use cases, industrial and academic specialists define DTs differently across fields, highlighting the need for a universally applicable and accepted definition. 12 In general, DT refers to an accurate virtual representation of real-world physical entities (ie, objects, processes, services, and environments). These virtual models are seamlessly interconnected with their physical counterparts and synchronized at specified frequencies and fidelities. 13 The DT concept operates on 3 pillars: a physical entity, a digital entity, and a communication medium that ensures continuous data exchange between entities (Figure 1). Together, these components contribute to real-time monitoring, analysis, and optimization. 14

Digital twin system.
Ensuring real-time and synchronized (2-way sync) communication autonomously is a critical feature of DT technology to improve the efficiency and reduce downtime. DT communication model features 3 distinct phases, the digital model, the digital shadow, and the digital twin, which differ in terms of modes of bidirectional data exchange between the physical and digital entities.15,16 The digital model represents the primary level of interaction without unsupervised data exchange, 17 while the digital shadow model involves a 1-way data flow, with changes in the physical object being reflected in a digital replica. 18 On the other hand, the digital twin has a 2-way data flow, allowing changes in both physical and digital entities to identically reflect each other. 19 These features allow a wide range of applications across various industries.
Applications of the digital twin technology span various sectors, with key domains including urban spaces, manufacturing, engineering, automotive, and medicine. For example, in smart cities, the digital twins contribute to virtual modeling and infrastructure management, such as transportation networks, energy grids, and water systems, allowing real-time monitoring and better decision-making. 20 In manufacturing, the digital twins support predictive maintenance and process optimization by analyzing data from physical assets, reducing downtime and enhancing efficiency. 21 In the healthcare sector, digital twins are revolutionizing personalized medicine by simulating patient-specific conditions and predicting responses to treatments, leading to more accurate diagnoses and tailored therapies. 22 The diverse applications of digital twin technology across different sectors are discussed extensively in. 1 The significant role of digital twin technology in enhancing decision-making, improving performance, and efficiency is evident in every data-driven area.
The Value of Digital Twins in Healthcare
Professionals from academia and industry are actively working to effectively integrate digital twin (DT) technology in the healthcare industry. Since the introduction of healthcare 5.0, professionals such as clinical specialists, health informaticists, and IT experts have further engaged and accelerated the adoption of emerging technologies, including DT technology, in clinical practice. While successful implementations are still relatively rare, researchers and experts recognize the potential of digital twins to revolutionize technology-assisted medical training, healthcare delivery, and patient care, as well as medical research and development.
Previous studies have shown that the integration of digital twins benefits healthcare practitioners through risk-free preoperative planning.23 -26 This benefit is achieved through combination with enabling technologies such as extended reality (XR). For example, XR creates an immersive experience that allows surgeons as well as young medical students to practice procedures on a digital twin of the patient, offering realistic simulations with the ability for unlimited repetition before undertaking real simulations to enhance their skills. 27 This combination not only aids in mastery but also provides performance feedback and greater accessibility to advanced surgical training. 28
In addition, by simulating physiological processes and disease progression, MDTs support the creation of personalized treatment plans and early interventions.29 -31 A digital heart twin, for instance, continuously monitors real-time data from wearable or implanted devices. Artificial intelligence (AI) integrates cardiovascular data with other relevant information, such as laboratory results or medical imaging. 32 As it is both receptive and responsive, this technology can predict a patient’s condition, detect potential health issues, and assess medication effectiveness, which is particularly vital for critically ill patients. 33 The integration of digital heart twins can revolutionize patient care through dynamic pathways that are scalable, affordable, and feasible.34,35
Academics and industrial experts see opportunities in every challenge through research and development, and they can expand the value of digital twin technology. For example, in drug development, digital twins can model human responses to new medications, accelerating the discovery process and reducing the reliance on costly and time-consuming clinical trials. This not only enhances efficiency but also opens the possibilities for personalized medicine, where treatments are tailored to individual genetic profiles, potentially revolutionizing the management of rare diseases.
Digital twin technology has significantly advanced personalized medicine. Integrating it with the cutting-edge tools and technologies will further unlock its full potential. However, it should not be used in isolation. Rigorous data management and collaboration are essential for making unprecedented discoveries and improving healthcare outcomes.
Healthcare Interoperability
Personalized care enables patient-centric management and facilitates decision-making. Advancements in medical data communication technology have advanced not only in personalized care but also in connected care. These 2 components address healthcare interoperability. However, attaining full-scale healthcare interoperability remains challenging in many healthcare institutions.
According to the Healthcare Information and Management System Society (HIMSS), healthcare interoperability can be defined as "the ability of different information systems, devices, and applications to access, exchange, and cooperatively use data in a coordinated manner, within and across organizational, regional, and national boundaries, to provide timely and seamless portability of information and optimize the health of individuals and populations globally”. 36 Open data formats and shared standards are the key components of interoperability that allow seamless information exchange among healthcare providers, regardless of the disparate technological frameworks in particular healthcare institutions. Through the concepts of patient-centricity and personalized medicine, healthcare interoperability is dedicated to enhancing patient care and optimizing patient outcomes. 37
Healthcare system interoperability is essential for the seamless exchange of medical data and information. There are 4 key levels of interoperability, each representing a progressively deeper level of integration. A clear understanding of the role and interconnection of each level is crucial for the proper application of both theoretical and technical aspects. 38 Using a bottom-up approach in the pyramid model, the layers consist of foundational interoperability, syntactic interoperability, semantic interoperability, and organizational interoperability (Figure 2).
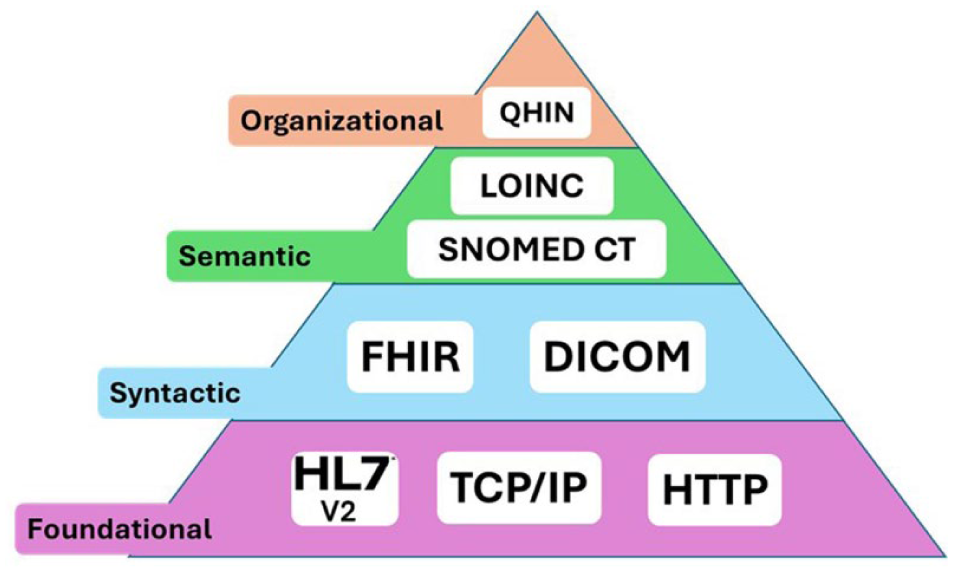
Levels of healthcare interoperability.
The first level, Foundational Interoperability, focuses on raw data communication, where different systems are able to securely exchange digital information through established communication protocols suitable for internet and network communication, such as TCP/IP and HTTP. 39 Securing data exchange is enabled through authenticated encryption applied to the data prior to transmission, where autopartitioning and reassembling took place in the transmission and reception phases. This level ensures that diverse infrastructures can connect, regardless of limitations or the absence of contextual understanding. 40
Advancing to the upper level, the syntactic interoperability layer ensures the compatibility of data exchanged between the system structurally and syntactically through a common standardized format. At this level, the data format and structure are defined, followed by the data being organized in a way that can be properly parsed and understood by the receiving system. This allows the systems to not only share data but also understand its structure, facilitating more meaningful exchanges. Common standards used at this level include Fast Healthcare Interoperability Resources (FHIRs) and Continuity of Care Documents (CCDs). 38
The next stack is occupied by semantic interoperability. At this level, systems are equipped with systematic item identification features that enable effective data exchange with meaningful interpretation. This can be achieved using common vocabularies and ontologies that provide context and definitions, allowing disparate systems to align with the interpretation of shared information. Standards such as the Systematized Nomenclature of Medicine Clinical Terms (SNOMED CT) and Logical Observation Identifiers Names and Codes (LOINC) are critical in achieving semantic interoperability. 41
Finally, the fourth level, organizational interoperability, encompasses collaboration at an institutional level, where policies, workflows, and practices are synchronized to enable comprehensive interoperability. This level cultivates a holistic ecosystem that integrates foundational, syntactic, and semantic capabilities with organizational frameworks. Each level serves as a building block, progressively increasing the potential for interoperability by leveraging mediation through standards and technologies, ultimately fostering a cohesive environment for diverse infrastructures. The technical framework known as the Qualified Health Information Network (QHIN), established under the Trusted Exchange Framework and Common Agreement (TEFCA), reflects a paramount effort by many agencies to realize organizational interoperability. 42
In essence, the notion of healthcare interoperability is composed of a syntactic and semantic perspective promoted through a global strategy that facilitate the management and exchange of information, driven by the Health Information Exchange (HIE) initiative. In a more explicit context, syntactic interoperability allows 2 or more systems to communicate and exchange data; however, the interface and programing languages are different. In contrast, semantic interoperability involves not only the exchange of data between 2 or more systems but also understood by each of them. In a larger context, HIE’s semantic approach should enable seamless electronic data sharing where standardized, structured, machine-readable data elements are transferred and integrated directly into the receiving organization’s electronic health records (EHRs). 43
Challenges
MDTs are keeping pace with other leading industries and hold promising potential that is yet to be unlocked. Prioritizing seamless medical data exchange across institutions requires the integration of interoperability within the Digital Twin. However, the adoption of MDTs presents numerous challenges, especially pertaining to healthcare interoperability.
Scarcity of Standardized Data Protocols
The first key challenge for interoperability in the MDT is the scarcity of standardized data protocols for medical data exchange. Currently, existing frameworks, such as Health Level 7 (HL7) and Digital Imaging and Communication in Medicine (DICOM), are essential for promoting medical data collaboration between health information systems. However, disparities in adoption practices across healthcare providers have hindered effective data sharing. This situation often influenced by several key factors including the financial constraints, vendor-specific customization, and a lack of enforced standardization.44,45
To address legacy system challenges, the healthcare industry is increasingly adopting modern, application programming interfaces (API)-driven solutions. For such purpose, the Fast Healthcare Interoperability Resources (FHIRs) have been proposed to overcome interoperability issues in health research, further enhance semantic interoperability through their “full-fledged” messaging standards. FHIR’s promising attribute facilitates effective data exchange and collaboration through its intermediary layers, thanks to its flexible and adaptable nature. While its implementation is not yet universal, the framework is increasingly adopted in many healthcare facilities, signifying its strong potential in mitigating the technical challenges, especially at the semantic level. 46 In a more recent study, a collaborative project has been initiated that led to the creation of a new modeling language known as Digital Twin Definition Language (DTDL) to meet the unique needs of digital twins. However, as the developed system is still in the early phase, it must achieve broader industry consensus to be effective. 47
Data Format Inhomogeneity
In addition to the lack of standardized protocols, data format inhomogeneity across different healthcare systems further restricts the potential of MDTs. Different systems may possess distinct data models, which leads to incoherency in digital twin representation. The key contributing factor to this issue stems from the poor integration of mixed forms of healthcare data, including structured (sensor-based data) and unstructured data (clinical reports). 48 Unfortunately, many existing implementations lack the advanced mapping and transformation techniques necessary to integrate these diverse data types into a unified digital twin framework. 47
To address the challenge of inconsistent data types, advanced data handling techniques are being employed, particularly using Artificial Intelligence (AI)-enabled tools. For instance, the Natural Language Processing (NLP) tool can effectively manage unstructured health data such as diagnostic reports, clinical notes, and prescriptions. The useful feature of NLP not only transform unstructured to structured data with ease, but also facilitates comprehensive analysis (syntactic) as well as collaborative data exchange (semantic). 49
Ethical Considerations in AI
Over the past decades, AI has played a pivotal role in shaping various industries, including healthcare. Consequently, its proven value has influenced industrial leaders to consider integrating AI-based elements into the MDT workflow. This is driven by the promise of creating more autonomous, adaptive, and resilient systems that significantly enhance decision-making. While companies have benefited from AI’s core values in their day-to-day operations, this adoption exposes them to the ethical dilemma including the algorithmic bias. 50
Digital heart twin, as mentioned in the earlier section, is an example of the AI-based digital twin which contributed to the personalized patient care. 32 However, the predictive features in the AI-driven models may pose ethical challenge, such as the algorithmic bias as highlighted in. 50 Algorithmic bias, which usually originates during the training phase, produces discriminatory outcomes due to limited variation in the training data. This led to the features misidentification that may negatively affecting the learning process or bias predictions. Mitigating this issue require the inclusion of diverse datasets from multiple population leading to reduced disparities in healthcare quality. Nevertheless, the challenges remain as the effort continues in finding the right balance between technological advancement with the responsibility to uphold human rights. 51
In summary, the technical complexity of healthcare environments poses additional hurdles. Digital twins must not only represent the individual patients (physical twins) but also account for the interactions between various healthcare entities, such as hospitals, clinics, and home care systems. This necessitates a robust interoperability framework that can accommodate the dynamic nature of healthcare delivery. 52 The challenge lies in ensuring that digital twins can effectively communicate and share data across these diverse entities while maintaining data integrity and security. 53
While digital twins hold great promise for enhancing healthcare interoperability, several challenges must be addressed. These include the need for standardized data exchange protocols, the integration of heterogeneous data formats, and the complexity of healthcare environments for implementing such systems. Overcoming these challenges and emphasizing their value delivery are essential for realizing the full potential of digital twins in improving patient care and operational efficiency in healthcare settings.
Potential Opportunities
Despite the key challenges highlighted, from an advantageous perspective, MDT technology offers numerous opportunities, especially in terms of healthcare interoperability. In this section, the key opportunities are discussed, with a focus on ensuring seamless healthcare interoperability as well as scalable implementation within the digital twin ecosystem. The insights offered highlight on the multiple contexts which cover the establishment of the standardized protocol, enabling an open data platform, and empowering semantic interoperability.
Establishing a Standardized Protocol
The colliding of different medical data formats, proprietary software, and inconsistencies in communication standards has created a demand for standardized protocols. The establishment of the standard, integrated with the digital twin, will further facilitate real-time monitoring and personalized care, particularly benefiting critical disease management in the hospital ward or at home. 54 This is particularly beneficial for managing critical diseases, both in hospital wards and at home.
A potentially specific explorable area is that integrating virtual twinning in the interoperability system is likely to increase accuracy in medical evaluation and facilitate healthcare providers in the decision-making process, as demonstrated through existing digitalized interventions.55,56 This will be particularly helpful for healthcare providers which currently facing difficulties in managing demanding care of the growing chronic diseases population.
MDT has the potential in shifting from the purely “healthcare” to the patient-empowered “self-care” for the patients with chronic diseases. Having said this, the adoption of MDT can be effectively implemented within the Disease Management Programs (DMP) at local, regional and global level.
Enabling an Open Data Platform
The combination of multiple types of medical information, both structured and unstructured, has pushed to make the open health data available. Although this may raise data privacy concerns, the advent of computational technology is potentially possible for data deidentification, such as data anonymization, pseudonymization, and crypto-secure authentication.53,57
Shareable open data can further pave the way for better and commendable FAIRification practices, which stand for “findable,” “accessible,” “interoperable,” and “reusable.” Proactive effort involving MDT implementation has been initiated; however, additional comprehensive evaluation of the deployed platform is needed. 58
Empowering Semantic Interoperability
Systematic data identification and interpretability are crucial for achieving semantic interoperability. Semantic interoperability facilitates organizational interoperability, which necessitates data consistency and accuracy. In this context, the integration of AI in the digital twin platform provides another potential opportunity: intelligently managing standardized terminologies and ontologies for effortless interoperable systems. 59
Throughout various sectors, AI has brought significant transformative changes especially through efficient data classification and prediction features. Often, organizations can benefit in many aspects through this efficient data-driven analysis and synthesization. With proper usage, this synergistic collaboration of human-AI interaction can further maximize the impact of health interoperability.
Enabling Scalable and Sustainable Growth
Despite persistent hurdles, ensuring access to key enabling technologies can catalyze the growth and widespread adoption of the Medical Digital Twin (MDT). Small-scale, practical solutions are key to realizing its personalized potential.
In this context, the nuanced adaptation of the Internet of Medical Things (IoMT) can serve as the primary tool for designing essential, cost-friendly, and scalable MDT infrastructure. For instance, patient-centric IoMT devices like smartwatches, smart rings, and other medical wearables hold strong potential for progressively enhancing active patient involvement. Their real-time monitoring, equipped with AI-driven personalized recommendations, can not only track patient health and fitness on a continuous basis but also provide comprehensive insights into overall physiological condition.
Ultimately, capitalizing on the MDT’s potential depends on the effective use of existing innovations and resources. This pragmatic approach makes the effort toward seamless, full-scale integration less daunting and more encouraging. 60
Conclusion
Despite the myriads of challenges for effective implementation, MDTs hold significant value. The regulatory framework and roadmap are important for the implementation of the technology to be scalable and sustainable over the long term. While the mainstream adoption approach may be found in the classroom, lab, and clinical setting, immediate next steps must actively incorporate more scalable research and development by integrating experts from academia, industry, and hospital practice. Alongside robust community engagement, responding to this call for a global initiative will accelerate the adoption and adaptation of the interoperable Medical Digital Twin, enabling higher quality healthcare.
The effective roadmap’s execution depends on the active and integrated collaboration of all stakeholders. Clinicians, biomedical engineers, and IT specialists should collaborate with regulatory bodies and policymakers through open, task-force-driven initiatives such as the European Union’s Virtual Human Twins (VHTs) program. This cooperation is essential for developing rapid yet sustainable strategies, supporting the technology’s full adoption. Combined and continuous efforts from various parties toward seamless healthcare interoperability could facilitate better personalized and precision medicine.
Footnotes
Author Contributions
TAITA: Writing – original draft, review & editing, conceptualization, visualization, and project administration; AMM: Writing - review & editing, supervision, conceptualization; YYLee: Writing - review & editing, supervision, and conceptualization; TST: Writing - review & editing, and conceptualization.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
