Abstract
Purpose:
Most of the breast cancer diagnoses are recommended for breast surgery. Unfortunately, many patients report preoperative anxiety, which can affect postoperative recovery. Preoperative teaching sessions have been shown to reduce anxiety and improve recovery for the patients with breast cancer. To better support the patients at our cancer center, a multidisciplinary preoperative teaching session was developed and delivered as a quality improvement initiative.
Methods:
Participants scheduled for breast surgery were invited to attend a group-delivered preoperative teaching session, either for breast-conserving surgery or mastectomy. The sessions were presented by a nurse, occupational therapist, and physiotherapist. Data were collected through a researcher-developed 2-item questionnaire administered before and after sessions to compare self-reported anxiety and knowledge levels, along with qualitative feedback.
Results:
A total of 94 participants attended the preoperative sessions, piloted over a year. The majority were scheduled for breast-conserving surgery. Wilcoxon signed rank tests showed that after session, self-reported levels of anxiety decreased, whereas levels of knowledge increased. Most participants found the session to be very helpful and would recommend it to other patients/families awaiting surgery.
Conclusions:
Patients awaiting surgery for breast cancer may be better supported through a multidisciplinary group teaching session by decreasing anxiety and improving knowledge related to the procedure. Future directions could explore the effect of specific session elements on anxiety, knowledge, and postoperative complications using psychometrically sound instruments and additional time points.
Implications for cancer survivors:
Standardization of these preoperative teaching sessions may enhance breast cancer care, reduce postoperative complications, and improve patient recovery.
Keywords
Introduction
Worldwide, breast cancer is the most prevalent cancer among women. 1 As throughout the rest of the world, the rate of breast cancer continues to rise in Canada with estimates that 1 in 8 women will develop breast cancer in their lifetime. 2 Earlier detection and advancements in cancer-related treatments have led to improvements in prognosis, however with this, welcomes new challenges of addressing the sequelae of the disease, its treatment-related side effects, complications, and long-term survivorship issues. Empirical evidence suggests that most of the women diagnosed with breast cancer are often recommended for breast surgery. 3 Persons undergoing surgical procedures often experience fear and anxiety preoperatively (ie, 60%-80% of older adults) in anticipation to the surgery.4,5 Similar findings were noted for patients undergoing cancer-related surgeries, 6 affecting postoperative recovery and increasing the risk for physiological complications (ie, pain and vomiting). 7
Preoperative teaching, that is, an interactive process of providing patients with information and explanations about surgical procedures, postoperative recovery processes, and psychosocial support,8,9 is beneficial to patients in reducing anxiety, length of hospital stay, postoperative physiological complications (ie, pain); improving knowledge6,10; and promoting self-care management, adherence, and postoperative recovery.11,12 Preoperative teaching is imperative and beneficial, as empirical evidence highlights the importance of identifying patients’ individual learning needs, styles, and preferences as it has the potential to affect patient’s information processing, retention, and application.13-15
In addition to providing preoperative teaching, appropriate and timely postoperative rehabilitation is important to ensure recovery from breast cancer surgeries (ie, segmental mastectomy, total mastectomy, axillary lymph node dissection, and breast reconstruction). 16 Upper extremity impairments following breast cancer treatment have been well-documented, with the majority presenting within 3 months and persisting longer than 2 years postoperatively. 17 Common sequelae following breast cancer–related surgeries include impaired shoulder range of motion, arm weakness, shoulder/arm pain, lymphedema, cellulitis, flap necrosis, abscess, dehiscence, hematoma, axillary web syndrome, seroma, pneumothorax, Mondor disease, brachial plexopathy, and nerve damage causing sensory disturbance.16,18-20
Prehabilitation takes place in the time between a patient’s cancer diagnosis and beginning of acute cancer treatment. Informed by physical and psychological assessments, prehabilitation identifies patient baseline needs and impairments, which in turn informs the delivery of appropriate interventions aimed to minimize posttreatment sequelae. 21 Examples of prehabilitation interventions include nutritional counseling and specialized physical therapy interventions that aim to improve physical functioning prior to starting cancer treatment. 21 Posttreatment benefits of prehabilitation include improved urinary continence, improved mood, physical well-being, and immune function in patients with prostate cancer and improved pulmonary/respiratory function and functional abilities in patients with lung cancer.21-24 Specifically, for the patients with breast cancer, prehabilitation has been shown to reduce shoulder pain, prevent shoulder impairments, 25 minimize range of motion deficits, 26 improve quality of life, as well as lower distress levels, depression, anxiety, and fatigue. 21
Multidisciplinary teams have been widely applied in the provision of cancer care.27,28 Through this strategy, health care providers from a range of professions (ie, nursing, rehabilitation, and medicine) collaborate to deliver comprehensive, complex, and patient-centered care through their respective expertise, perspectives, and knowledge. Empirical evidence indicates the benefits of multidisciplinary teams in improving coordination of patient care, care delivery, clinical decision making, and patient outcomes. 28 In addition, research supports the use of preoperative teaching for breast reconstruction surgery in terms of knowledge gains and decisional satisfaction. 29 In the oncology setting, preoperative teaching sessions have been shown to reduce anxiety and improve knowledge. 6 Because the patients with breast cancer can experience a multifaceted array of sequelae pre- and postoperatively, a multidisciplinary approach may be better suited to provide holistic care. As such, to better support the patients awaiting breast cancer surgery at our center, this quality improvement initiative sought to develop and deliver a multidisciplinary (ie, nursing, occupational therapy, and physiotherapy) preoperative teaching session.
Method
Preoperative breast cancer education sessions were delivered in group settings at the Segal Cancer Centre at the Jewish General Hospital in Montreal, Quebec. This quality improvement initiative took place under the hospital’s quality program. The data were collected through a researcher-developed 2-item questionnaire administered at 2 points in time: pre- and postteaching sessions to compare the anxiety and knowledge levels. Qualitative feedback for the improvement of future sessions was collected.
Sample
Eligibility criteria for participants were as follows: (1) a breast cancer diagnosis and scheduled to have either a lumpectomy (ie, partial and/or segmental mastectomy) or total mastectomy (with or without reconstruction) in the upcoming month, (2) outpatient; (3) able to read and write in either English or French, and (4) willing to physically attend a session at the hospital during clinic hours. Exclusion criteria included breast surgery for a reason other than breast cancer.
Development and implementation of the preoperative educational intervention
In line with the structured quality improvement model, 30 we developed and implemented the multidisciplinary preoperative session by (a) understanding the issues within the health care system, (b) creating a multidisciplinary improvement team, (c) enlisting all members to identify barriers to change and appropriate solutions, and (d) implementing a change in practice using the 4 E’s—engaging, educating, executing, and evaluating the session:
a. The current standard of care for patient awaiting breast cancer surgery is the provision of an information booklet entitled “What you should know about your Breast Surgery” by a nurse during the patient’s the routine preoperative assessment, which takes place days to weeks before the scheduled surgery. The booklet includes the following information: (1) a brief description on the surgery (not indicative of the type of surgical procedure); (2) precautions to take the morning of the surgery, immediately following surgery and at home; (3) a description of the Jackson-Pratt Drain and the steps to manage the drain effectively; (4) return to daily activities, load restrictions, and exercises to do postoperatively; (5) cautionary statement regarding reconstruction surgery and exercises, with a disclaimer outlining precautions of movements depending on plastic surgeon and the need to refer back to treating surgeon’s recommendations; and (6) contact information of the breast pivot nurse and lymphedema therapist. Generally, the booklet is not reviewed with the patient.
Despite the distribution of this booklet, allied health care professionals within the breast cancer department (ie, nurse navigators, physiotherapists, occupational therapists, breast surgeons, and oncologists) anecdotally expressed concern regarding patients’ understanding of their upcoming surgery, postoperative management, and side effects. In addition, patients verbally expressed anxiety and knowledge gaps related to their breast cancer surgeries. Together, this suggested a care-need gap for our patient population in the preoperative period.
b. A breast cancer nurse navigator, an occupational therapist, and a Hope & Cope physiotherapist in oncology came together to create a multidisciplinary team to develop a preoperative intervention to improve care for patients awaiting breast cancer surgery. Together, they proposed a preoperative teaching session with the aim to decrease participant’s anxiety levels, improve surgical knowledge, and potentially minimize the risk of postoperative sequelae.
c. Members of the team identified barriers that might impose difficulties to implement the preoperative teaching session, including and not limited to logistical challenges and resource constraints. Barriers were discussed and solutions were proposed for each. To reach the maximum number of patients and to provide the most poignant information, we developed a preoperative teaching session to be delivered by the multidisciplinary team (ie, breast cancer nurse navigator, occupational therapist, and Hope & Cope physiotherapist) to groups of patients and their caregivers. To ensure comprehensiveness and complementarity, education material delivered through the sessions was developed independently and reviewed collectively by the multidisciplinary team. Content was reviewed to improve delivery, readability, and relevance prior to delivering the session to patients. In addition, to ensure consistency, the same multidisciplinary members administered the intervention.
d. Implementation of the sessions involved engaging, educating, executing, and evaluating the session as follows 30 :
Engaging participants. A list of patients scheduled for a breast surgery in the upcoming month was obtained using the hospital electronic health record. A week to 10 days prior to the preoperative educational session, patients were telephoned and invited to the upcoming session. Patients were informed that the session was not mandatory but would be presented by a multidisciplinary team and would provide information regarding their surgery and recovery processes. The preoperative sessions were offered in addition to the provision of the standard of care booklet. Caregivers, family members, and/or friends were also invited.
Educating participants through the execution of the session. The preoperative teaching session scheduled for 60 minutes in duration was piloted over a 1-year period, taking place on the last Friday of each month for participants who were scheduled for surgery the subsequent month. Depending on the type of surgery scheduled, participants were invited to attend either the segmental mastectomy session (ie, breast-conserving surgery) or the total mastectomy session (with or without reconstruction). Education materials were tailored to the specific procedures as healing time, precautions, and complications vary. Each participant was provided a bilingual information package which was prepared by Hope & Cope volunteers with guidance from the preoperative team. Sessions were piloted in English and translated into French to meet the needs of the bilingual population. The packages provided in each preoperative session included the following: a calendar of events for Hope & Cope services (the hospital-affiliated wellness center designed for patients with cancer), information on a “newly diagnosed breast cancer support group,” a risk reduction brochure for lymphedema prevention (provided by the Lymphedema Association of Quebec), and a handout of the session slides and the postsurgical rehabilitation exercise program. Packages were designed for the participants to be able to take home and refer to them at any point pre- and postoperatively. Information was presented using visuals and a sixth-grade reading level to ensure accessibility to patients with limited literacy.
Evaluating the session. Prior to beginning the session, participants were asked to complete the prequestionnaire measuring their anxiety and knowledge levels. A question period with the multidisciplinary team was allocated at the end of the session to address concerns. The postquestionnaire was filled out after the question period by the participants, to capture their anxiety and knowledge levels after the session.
Variables and measures
Demographic and medical information was collected including age, sex, whether surgery was the first treatment for breast cancer, and types of treatments participants had previously undergone. Participants were asked to complete a researcher-developed nonvalidated questionnaire before and after session attendance. The questionnaire assessed participants’ (1) self-perceived anxiety levels (“I feel anxious . . .”), using a 10-point scale ranging from 0 (never) to 10 (always) and (2) self-perceived knowledge levels (“The level of my knowledge in regards to my surgery is . . .”), using a 10-point scale ranging from 0 (low) to 10 (high). The questionnaire also prompted for suggestions for future sessions using an open text box.
Analysis
The quantitative data were analyzed with Statistical Package for the Social Sciences Version 22.0 (SPSS 22.0). 31 The Shapiro-Wilk test showed that the data were not normally distributed. As such, difference between paired pre- and postcontinuous variables was tested for statistical significance (P value of ⩽.05 or less) through the nonparametric Wilcoxon tests. The qualitative data were analyzed using category schemes. 32 Independently, the first author (MI) and second author (GJL) read the participant feedback and suggestions from the questionnaire to identify underlying categories. The data were coded and the authors then met to discuss the emergent categories.
Results
During the period of August 2016 to August 2017, a preoperative session was given during the last Friday of each month for participants planned for their surgery the subsequent month. Two sessions were offered, one for breast-conserving surgery and the other for total mastectomy (with or without reconstruction). Approximately 6 to 25 patients per month were contacted and invited to attend the multidisciplinary preoperative teaching sessions. Each session was attended by 2 to 15 participants (along with family members). The contact information for members of the multidisciplinary team was provided to all participants should they have any issues or questions during their postoperative recovery process. The services at Hope & Cope, a non-for-profit organization, were provided for participants interested in receiving one-on-one peer counseling, self-help groups, physical activity classes, tailored exercise programs, public education, and awareness programs along with various other support groups. 33
Information covered in the preoperative teaching session was divided into 3 sections provided by the breast cancer nurse navigator in the Segal Cancer Centre, the occupational therapist in the Segal Cancer Centre, and the Hope & Cope physiotherapist.
The breast cancer nurse navigator explained the following: (1) the surgical procedures in detail along with the methods of sentinel and axillary lymph node dissection; (2) postoperative pain management; (3) dressing/wound care and Steri-Strip management; (4) bathing restrictions; (5) the Jackson-Pratt drain placement, fluid drainage, bulb suction mechanism, and care during period of usage; (6) specific mandates from surgeons; (7) postoperative complications (ie, hematoma, seroma, signs and symptoms of injection, and appropriate path of contact for medical management); and (8) the breast clinic hours and specific indications for emergency department visit during off hours.
The occupational therapist provided information on (1) the impact of the breast surgery on daily activities; (2) tips and ideas on how to prepare for the postoperative period before surgery (eg, preparing meals to reheat, completing any required heavy physical tasks, arranging additional help after surgery; (3) postoperative energy conservation; (4) fall risk reduction; (5) the importance of using the affected upper extremity postoperatively to engage in activities of daily living, such as grooming and eating as well as suggestions for comfort showering and transferring from bed; and (6) support groups and bringing any questions or concerns to their care team.
The physiotherapist provided education on (1) the goals of rehabilitation to regain shoulder range of motion and decrease risk of musculoskeletal sequelae; (2) lymphedema risk prevention and management; (3) postoperative home exercise program recommendations (eg, active assisted range of motion exercises for shoulder flexion, extension, abduction, external and internal rotation, and horizontal abduction) with the frequency, intensity, and duration; (4) movement precautions with a Jackson-Pratt drain; (5) scar tissue mobilization to decrease scar adhesion; (6) possible complications postoperatively (eg, axillary web syndrome); (7) precautions with a weighted load on affected surgical side was covered, with specific carrying restrictions, particularly for young mothers and their babies; and (8) the importance of asking the physiotherapist about any rehabilitative-related issues and needs if full range of motion was not attained by 6 weeks (for a breast-conserving surgery) and 8 weeks postoperatively (for a total mastectomy). Participants scheduled for a total mastectomy were immediately booked with a postoperative rehabilitation consult with the physiotherapist to ensure that a thorough evaluation was performed secondary to the extensiveness of these surgical procedures. Participants scheduled for lumpectomies were provided the option of booking with the physiotherapist. These consults provided an opportunity for women to ask questions and express concern about their recovery, provide education to address cancer-related bone loss, and exercise counseling to enhance bone density.
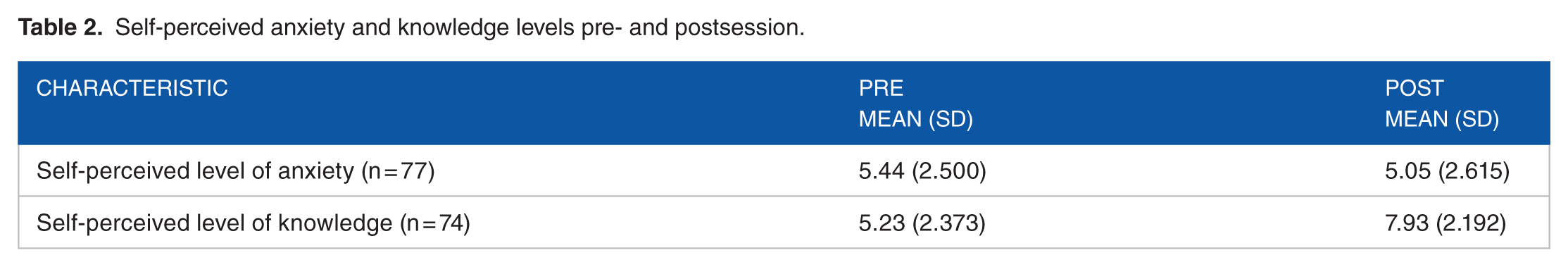
As per the participant characteristics outlined in Table 1, a total of 94 participants attended the sessions over the year. The mean age of the participants was 60.48 years, with a minimum age of 21 years and maximum age of 90 years. All participants were women except for 1 male. Most (74.47%) of the planned surgical interventions were breast-conserving surgery (n = 70), while unilateral and bilateral total mastectomies were less common (14.89%, n = 14 and 11.11%, n = 10, respectively). There was an 81% response rate for the attendees who completed the pre/postquestionnaire. The mean scores for the self-perceived levels of anxiety and knowledge pre- and postsession are outlined in Table 2. A Wilcoxon signed rank test showed that self-perceived level of anxiety was statistically significantly lower following the session in comparison with presession anxiety levels (z = −2.025, P < .05). Similarly, self-perceived level of knowledge was found to be significantly higher postsession (z = −6.422, P < .05). Most of the participants (n = 71) who completed the questionnaire found the session to be very helpful and would recommend the session to other patients/families awaiting surgery (n = 77). Immediately after the session, 29 participants booked for a postoperative physiotherapy consultation.
Participant characteristics.

Self-perceived anxiety and knowledge levels pre- and postsession.
When prompted for suggestions for future sessions, participants offered a variety of both positive and constructive feedback. The categories that emerged from the feedback are summarized in Table 3. Many patients offered commendations to the sessions, followed by suggestions to improve future sessions by adding an individualized session, adding more detailed information, including active participation of rehabilitation exercises and the translation of the session to other cancer sites that require surgical interventions.
Survey comments.

Discussion
A multidisciplinary team (ie, nursing, occupational therapy, and physiotherapy) preoperative teaching session was developed as a quality improvement initiative at our center, for patients awaiting breast cancer surgery. Relevant topics were presented during the session to multiple participants, using health care professional time more efficiently.
The results indicate that our preoperative teaching session may have reduced patient’s self-perceived anxiety levels and improved patients’ self-perceived knowledge levels, suggesting the benefits of offering preoperative teaching sessions. As anxiety has been found to be prevalent in women undergoing breast cancer treatment, 34 information provision has been shown to decrease anxiety levels. 6 By providing relevant and tailored information (such as potential side effects and approaches to minimize such complications) as well as outlining the clinical goals pre- and postoperatively, patients may be better equipped for surgical recovery. In addition, the simple act of offering contact information of the multidisciplinary team members may have reassured the patients and in turn possibly alleviated anxiety. As the literature outlines, interventions that encourage patients to be involved in their own care enable patients, ultimately empowering them with the skills, information, and resources necessary to tackle problems related to the care.34,35
Various teaching strategies and methods of delivery have been documented for patient education including traditional lectures, discussions, computer technology, written material, visual drawings, demonstrations, and repetition of information to facilitate retention. 36 The multidisciplinary team employed these evidence-based recommendations to meet the various learning needs and styles of patients. Session participants expressed appreciation for the simplicity yet comprehensive information provided during the sessions. The qualitative data also captured some of the recommended changes in the administration of the preoperative teaching session. The recommendations included more active participation and more detailed information of common comorbid conditions, specifically diabetes and how this may affect recovery postsurgery. Thus, future sessions may benefit from additional information on potential complications according to patients’ complexity of medical conditions (ie, cardiovascular, renal diseases, depression, and hypertension). Furthermore, participants recommended these preoperative sessions, not only to other patients awaiting surgery for breast cancer but also to patients of other tumor sites. The benefit of tailored information provision is echoed by other reports in which preoperative patient education may result in reduced pain, anxiety, recovery time and improves patient knowledge and satisfaction.11,36,37 As per the positive feedback received by patients, it should be noted that the sessions continue to be offered by the multidisciplinary team on a monthly basis. For patients who are unable to attend a session, they are referred to an uploaded recording of a previous presentation made available online for their convenience.
In addition, the physiotherapy rehabilitation information (eg, active exercises, lymphedema prevention, and shoulder impairment symptoms) that was provided as part of these sessions may have reduced postoperative sequelae and complications. Although these were not measured in this study, empirical evidence supports that early physiotherapy can minimize upper-limb dysfunctions, improve recovery of shoulder range of motion and strength, reduce postoperative pain, increase shoulder and arm use for daily activities, prevent lymphedema, and improve quality of life.17,38 Furthermore, sessions continue to be offered by the multidisciplinary team on a monthly basis.
Limitations
The study design precludes the identification of particular aspects of the session that may have played a more important role in reducing anxiety or increasing knowledge. The pre/postdesign does not allow for causal inferences. In addition, the use of nonvalidated tools to measure anxiety and actual knowledge levels coupled with a small sample size does not allow the generalizability of results to the patients with breast cancer beyond this study. The effectiveness of the session on either acute or long-term postoperative sequelae was not measured. Thus, further robust research and evaluation will be needed to determine the effectiveness of the developed approach.
Conclusions
Most patients diagnosed with breast cancer will be recommended for breast surgery. Our quality improvement initiative responded to the need in our cancer center for more comprehensive preoperative information. Our results suggest that a multidisciplinary group teaching session offered to patients awaiting surgery for breast cancer may decrease anxiety and improve level of knowledge related to the procedure. Standardization of these sessions may enhance breast cancer care, reduce postoperative complications, and improve patient recovery. Future directions could explore more robustly the effect of preoperative teaching session elements on anxiety, knowledge, and postoperative complications using psychometrically sound instruments and additional time points (ie, 1 week pre- and postsurgery).
Footnotes
Acknowledgements
The authors wish to thank Hope & Cope and the Segal Oncology Centre for their resources and support in this quality improvement initiative. In addition, the authors wish to acknowledge the Quebec Breast Cancer Foundation for a generous 3-year grant that made the Breast and Bone health program possible. Appreciation is extended to all the participants and caregivers who attended the preoperative sessions and provided valuable feedback. The research was performed at the Segal Cancer Centre at the Jewish General Hospital, Montreal, Quebec, Canada.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was made possible, in part by the Quebec Breast Cancer Foundation, which funded the Breast & Bone Health Program at Hope & Cope. Hope & Cope is a hospital-affiliated nonprofit organization funded by private donations to provide services and support to patients and caregivers affected by cancer.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
MI conceived and designed the intervention and planned it with GJL. MI conducted the intervention with GJL, NS, ATB, AC, KG and KJ. All authors discussed the results. MI wrote the manuscript with support from all authors.
Ethical approval
According to the policy activities that constitute research at the Jewish General Hospital in Montreal, Quebec, this work met criteria for quality improvement activities under the Quality Program. All participants were informed that they were participating in a quality improvement initiative. All questionnaires and feedback were collected anonymously. All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
